SAFE CARE TRANSITIONS BRIDGING SILOS OF CARE AGS

SAFE CARE TRANSITIONS: BRIDGING SILOS OF CARE AGS Karin Ouchida, MD Assistant Professor of Medicine Division of Geriatrics Montefiore Medical Center/AECOM Medical Director Montefiore Home Health Agency November 14, 2009 THE AMERICAN GERIATRICS SOCIETY Geriatrics Health Professionals. Leading change. Improving care for older adults.

OBJECTIVES • Identify complications of poor transitions • List key components of safe transitions • Distinguish different discharge services and settings • Appreciate the physician’s role Slide 2

WHY SHOULD YOU CARE ABOUT THIS? • Patient safety Ø The Joint Commission • Health care reform Ø Reduce avoidable re-hospitalizations Ø Increase accountability + transparency Slide 3
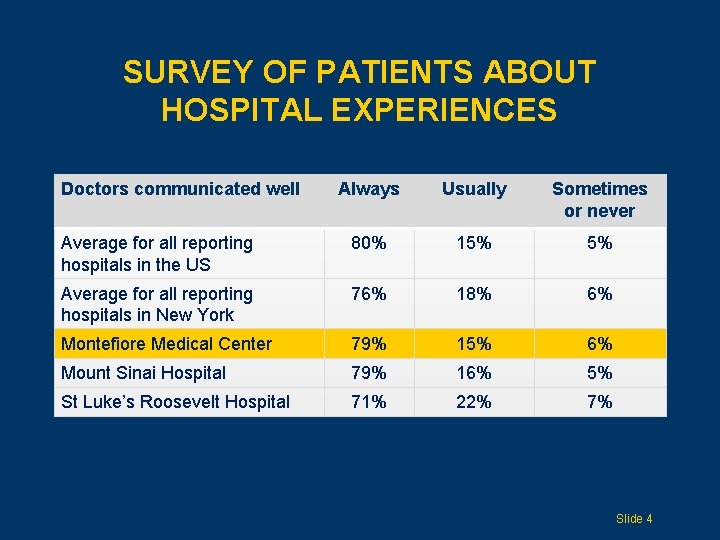
SURVEY OF PATIENTS ABOUT HOSPITAL EXPERIENCES Doctors communicated well Always Usually Sometimes or never Average for all reporting hospitals in the US 80% 15% 5% Average for all reporting hospitals in New York 76% 18% 6% Montefiore Medical Center 79% 15% 6% Mount Sinai Hospital 79% 16% 5% St Luke’s Roosevelt Hospital 71% 22% 7% Slide 4

HOW OFTEN DO TRANSITIONS OCCUR? • After hip fracture, pts underwent an average of 3. 5 “relocations” • Between Thurs and Mon morning, 6 7 “handoffs” may occur • Medicare beneficiaries see a median of 2 PCPs and 5 specialists yearly! Boockvar et al. JAGS. 2004; 52: 1826 -1831. Horwitz et al. Arch Intern Med. 2006; 166: 1173 -1177. Hoangmai et al. N Engl J Med. 2007; 356: 1130 -1139. Slide 5

DEFINITION OF TRANSITIONAL CARE The set of actions necessary to ensure the coordination and continuity of health care as patients transfer between different health care settings or levels of care Coleman and Berenson. Ann Intern Med. 2004; 140: 533 -536. Slide 6

COMPLICATIONS OF POOR TRANSITIONS • Adverse events • Increased health care utilization • Patient dissatisfaction • Provider dissatisfaction Slide 7

ADVERSE EVENTS • Injury resulting from medical management vs. underlying disease • 1 in 5 patients experiences an adverse event during the hospital-to-home transition Ø 1/3 are preventable Ø 1/4 of patients are re-admitted to the hospital Forster et al. Ann Intern Med. 2003; 138: 161 -167. Slide 8

INCREASED HEALTH CARE UTILIZATION • 16% of Medicare beneficiaries are re-hospitalized within 30 days of discharge after a surgical admission Ø Vascular surgery 24% Ø Major bowel surgery 17% Ø 20% 40% are re-admitted to a different hospital • Readmission is associated with increased mortality, impaired function, and nursing home placement • Cost of unplanned re-hospitalizations in 2004: estimated at $17. 4 billion Jencks et at. N Engl J Med. 2009; 360: 1418 -1428. Boockvar et al. J Am Geriatr Soc. 2003; 51: 399 -403. Slide 9

4 CRITICAL COMPONENTS OF SAFE TRANSITIONS 1. Medication reconciliation 2. Patient education ü Red flags ü Who to call 3. Communication between sending and receiving providers 4. Timely follow-up Slide 10

CASE 1 • A 78 -year-old woman with a history of atrial fibrillation, CVA, and newly diagnosed breast cancer is admitted for mastectomy • Warfarin is held for surgery • The hospital course is complicated by delirium and UTI • The patient is discharged to subacute rehab • She is re-admitted after 5 days with rapid a-fib and sudden dysarthria/facial droop Slide 11

CASE 1: MEDICATIONS HOME • Atenolol 50 mg qd • Metformin 850 mg BID • Glucotrol 10 mg qd • Warfarin 3 mg q. HS • Prevacid 30 mg qd • Calcium/vitamin D 600/400 IU BID • Alendronate 70 mg weekly HOSPITAL • NPH 8 units q. AM • Protonix 40 mg daily • Keflex 500 mg BID • Colace 300 mg qd • Senna 2 tabs q. HS DISCHARGE • NPH 8 units q. AM • Protonix 40 mg daily • Keflex 500 mg BID Slide 12

COMPONENT 1: MEDICATION RECONCILIATION • How: Start with an accurate pre-admission list • When: “Across the continuum of care” • Why: Most adverse events are medicationrelated (66%) Forster et al. 2003 Ann Intern Med. 2003; 138: 161 -167. Slide 13

CASE 2 • A 78 -year-old woman with mild dementia, CAD, and DM is admitted with fever and abdominal pain • She is found to have acute cholecystitis and undergoes open cholecystectomy • The post-op course is complicated by mild cellulitis at the incision site • She is discharged on Keflex and Percocet for pain but not educated about warning signs/symptoms • She is re-admitted 7 days later with wound abscess and fecal impaction Slide 14

COMPONENT 2: COACHING PATIENTS TO ACHIEVE SKILL TRANSFER • Care Transitions Intervention® www. caretransitions. org • Subjects: 65+ admitted with multiple chronic conditions Transitions Coach (APN, RN, MSW) simulates common transition challenges and coaches them to adopt effective strategies to respond: Ø Resolving confusion over medications Ø Scheduling and preparation for follow-up visits Ø Identifying indicators of worsening condition (“red flags”) and knowing how to respond Coleman et al. Arch Intern Med. 2006; 166: 1822 -1828. Slide 15
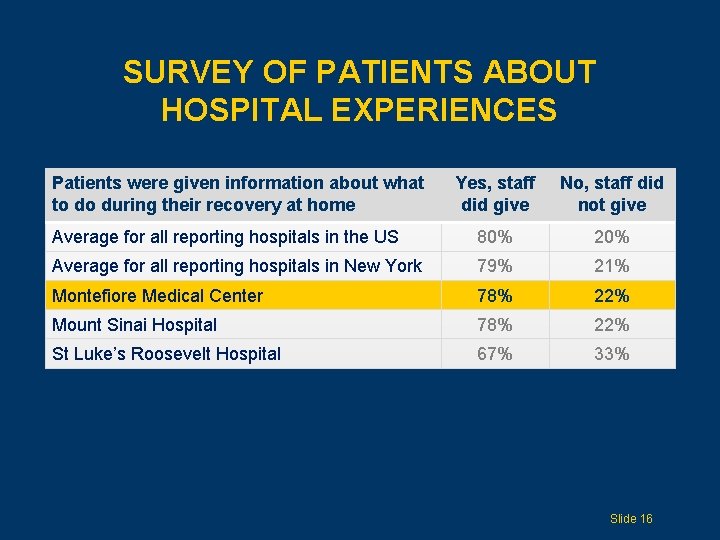
SURVEY OF PATIENTS ABOUT HOSPITAL EXPERIENCES Patients were given information about what to do during their recovery at home Yes, staff did give No, staff did not give Average for all reporting hospitals in the US 80% 20% Average for all reporting hospitals in New York 79% 21% Montefiore Medical Center 78% 22% Mount Sinai Hospital 78% 22% St Luke’s Roosevelt Hospital 67% 33% Slide 16

CASE 3 • A 75 -year-old man is admitted for elective hernia repair • He is given Ancef preoperatively and develops a rash, although he has no previous history of medication allergy • Post-op, he has hematuria, which resolves spontaneously; a UA/urine culture and urine cytopathology are sent • When he is discharged to home, the discharge summary does not list Ancef allergy or note pending urine cytology Slide 17

COMPONENT 3: COMMUNICATION • System problems contributed to all preventable and ameliorable adverse events • Most common reason for failed transition = poor communication between inpatient MD and patient or PCP (59%) • Direct communication between inpatient MD and PCP occurred in only 3%-20% of cases Forster et al. Ann Intern Med. 2003; 138: 161 -167. Kripalani et al. JAMA. 2007; 297: 831 -841. Slide 18

WAYS TO COMMUNICATE üDischarge summary üPatient üProprietary software üE-mail üPhone Slide 19

DISCHARGE SUMMARIES • Key information is often missing: Ø Ø Ø Responsible hospital MD (25%) Main diagnosis (18%) Discharge medications (20%) Specific follow-up plans (14%) Diagnostic test results (38%) Tests pending at discharge (65%) • Available at follow-up visit only 12% 34% of the time Kripalani et al. JAMA. 2007; 297: 831 -841. Kripalani et al. J Hosp Med. 2007; 2: 314 -323. Slide 20

THE “IDEAL” DISCHARGE FORM • • Presenting problem Key findings and test results Final diagnoses Condition at discharge (including functional and cognitive status if relevant) • Discharge destination • Discharge medications (purpose, cautions, changes in dose or frequency, meds that should be stopped) • • Follow-up appointments Pending labs/tests Specialist recommendations Documentation of patient education/understanding Anticipated problems or suggestions 24/7 call-back number Referring/receiving providers Advanced directives/code status Halasyamani et al. J Hosp Med 2006; 1: 354 -360. Slide 21

PENDING TEST RESULTS • 2600 patients discharged from hospitalist services at 2 academic hospitals Ø 40% had test results returned after discharge Ø 10% required some action • Hospitalists and PCPs surveyed about 155 results Ø Unaware of 60% Ø 40% were actionable, 13% urgent Roy et al. Ann Intern Med. 2005; 143: 121 -128. Slide 22

RECOMMENDATIONS FOR OUTPATIENT WORKUP • Of 700 discharges, 30% had outpatient work-up recommended Ø Diagnostic procedure (48%) Ø Subspecialty referrals (35%) Ø Laboratory tests (17%) • 36% of work-ups were not completed Ø Availability of discharge summary increased likelihood that post-discharge work-up would be completed (OR = 2. 35) Moore et al. Arch Intern Med. 2007; 167: 1305 -1311. Slide 23

CASE 4 • An 80 -year-old woman is admitted with fever, vomiting, and abdominal pain • She is found to have acute appendicitis and undergoes laparoscopic appendectomy • She is discharged home with instructions to follow-up in the surgery clinic in 4 weeks • She is re-admitted 2 weeks later with fever, altered mental status after a fall at home • The port sites are grossly infected Slide 24

COMPONENT 4: TIMELY FOLLOW-UP • 50% of patients re-hospitalized within 30 days of discharge did not have an outpatient MD visit billed to Medicare • Benefits of timely follow-up: Ø Ø Lab monitoring Reconcile medications Check on home supports Reinforce knowledge of red flags and emergency contact information Jencks et al. N Engl J Med. 2009; 360: 1418 -1428. Forster et al. Ann Intern Med. 2003; 138: 161 -167. Slide 25

CHALLENGES TO IMPROVING TRANSITIONAL CARE • Physicians Ø Awareness Ø Multiple providers Ø Time • Patients Ø Ø Health illiteracy Cognitive impairment Language barriers Lack of social support • Systems Slide 26

DO WE NEED “TRANSITIONALISTS”? Slide 27

TRIAL OF DISCHARGE SERVICES (1 OF 5) • Subjects: Adults admitted to medicine teaching service, discharged home • Design: Randomized trial with block randomization • Intervention: Nursing discharge advocate visit plus pharmacist phone call • Follow-up: 30 days • Primary endpoint: Number of ED visits and readmissions • Secondary endpoints: Patient knowledge of diagnosis, PCP name, follow-up, preparedness for discharge Jack et al. Ann Intern Med. 2009; 150: 178 -187. Slide 28

TRIAL OF DISCHARGE SERVICES (2 OF 5) • Nursing discharge advocate Ø Educated patient re: dx, meds, follow-up Ø Arranged follow-up appointments Ø Set up post-discharge services Ø Reviewed and transmitted discharge summary to PCP Ø Provided pt with “after-care plan” • Pharmacist phone call 2 4 days post-discharge to review medications Jack et al. Ann Intern Med. 2009; 150: 178 -187. Slide 29
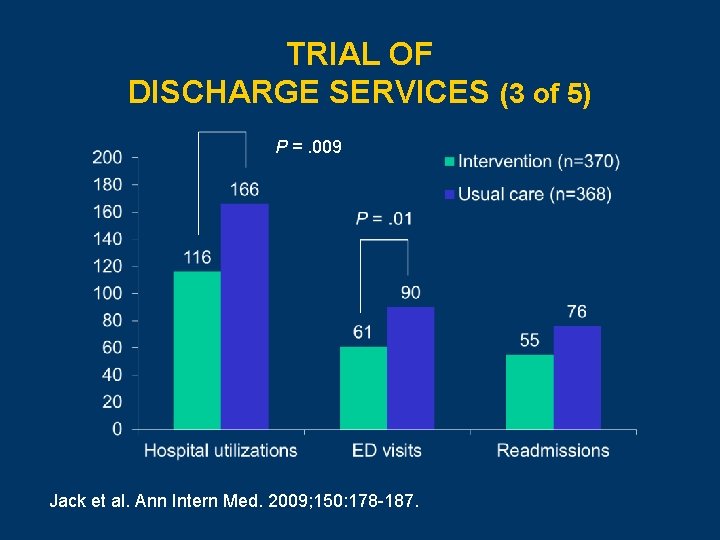
TRIAL OF DISCHARGE SERVICES (3 of 5) P =. 009 Jack et al. Ann Intern Med. 2009; 150: 178 -187.
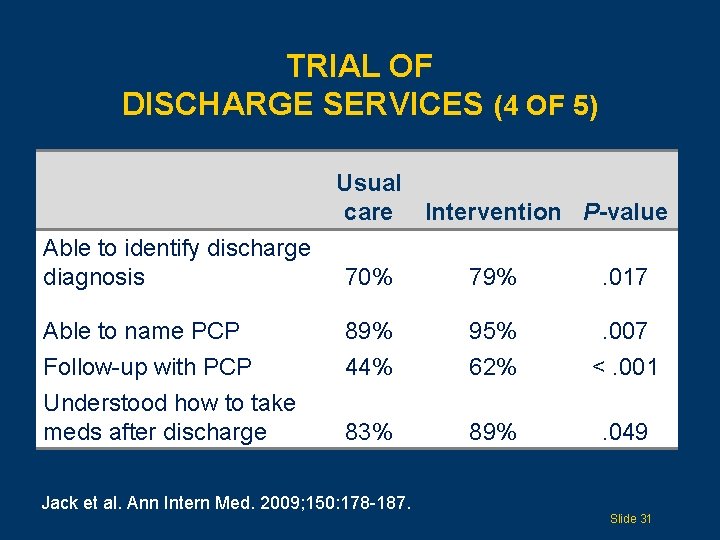

TRIAL OF DISCHARGE SERVICES (4 OF 5) Usual care Intervention P-value Able to identify discharge diagnosis 70% 79% . 017 Able to name PCP 89% 95% . 007 Follow-up with PCP Understood how to take meds after discharge 44% 62% <. 001 83% 89% . 049 Jack et al. Ann Intern Med. 2009; 150: 178 -187. Slide 31

TRIAL OF DISCHARGE SERVICES (5 OF 5) In the intervention group: • Follow-up with PCP made prior to discharge: 94% (vs. 35% in usual care) • D/C summary sent to PCP within 24 hours: 90% • Pharmacist reviewed meds with 50% Ø 65% had at least 1 medication problem Ø 50% needed corrective action by pharmacist Slide 32

A STRATEGY FOR EFFECTING SAFE TRANSITIONS If you don’t have a transitionalist, identify and involve interdisciplinary team members who can help you with: • Med reconciliation • Patient education • Communication • Follow-up Slide 33

A TEAM APPROACH Inpatient Outpatient/Home • • • Nurse Social worker Pharmacist PT/OT Medical students Caregivers Home care nurse Home care SW Pharmacist Home care PT/OT Case managers Caregivers Slide 34

IDENTIFYING THE MOST APPROPRIATE DISCHARGE SETTING Functional assessment: • Activities of daily living and instrumental activities of daily living • Ambulation • Cognitive status • Home environment • Caregiver support Slide 35

SHORT-TERM HOME HEALTH CARE • Skilled need: RN, PT and/or speech therapy • Homebound: assistance for person/device to leave the home • Intermittent care: part-time, intermittent needs • Physician supervision: must have outpatient MD to sign orders, address concerns • If the patient needs assistance with activities of daily living (ADLs) or instrumental ADLs, there must be sufficient/willing caregiver(s) Slide 36

REHABILITATION SETTINGS HOME SUBACUTE • Can tolerate PT for • Aggressive 30 60 min/day PT/OT/ST 3 h/day • Medical and/or • Medical needs and/or • Great potential to personal care needs achieve functional needs can be met exceed what family goals by short-term aide can provide (eg, needs • Impairment + family support help getting to subject to serious (eg, needs help bathroom and/or decline if with shopping, administering meds, aggressive tx is picking up meds) and is at high risk for not immediate falls) Slide 37

HOME VS. INPATIENT REHABILITATION • 234 patients randomized to home-based vs. inpatient rehab after total joint replacement; followed for 1 year • Average stay in inpatient rehab = 18 days • Number of home rehab visits = 8 • Functional outcomes equal • No significant difference in infection, DVT, infection, patient satisfaction • Lower cost for home-based rehab (~$3000) Mahomed et al. J Bone Joint Surg Am. 2008; 90: 1673 -1680. Slide 38

SKILLED NURSING FACILITY • Skilled need for RN, PT/OT, or speech therapy Ø IV antibiotics Ø Wound care Ø Rehab • Medical or personal care needs exceed home supports Slide 39

SUMMARY • Care transitions are associated with increased adverse events and health care utilization • Safe transitions require medication reconciliation, patient education, provider communication, and timely follow-up • Functional assessment helps identify the most appropriate discharge setting • Physicians are responsible for ensuring safe transitions Slide 40

THANK YOU FOR YOUR TIME! Visit us at: www. americangeriatrics. org Facebook. com/American. Geriatrics. Society Twitter. com/Amer. Geriatrics linkedin. com/company/american-geriatricssociety Slide 41
- Slides: 41