S 1 Secretion Reabsorption Filtration S 2 Circulatory
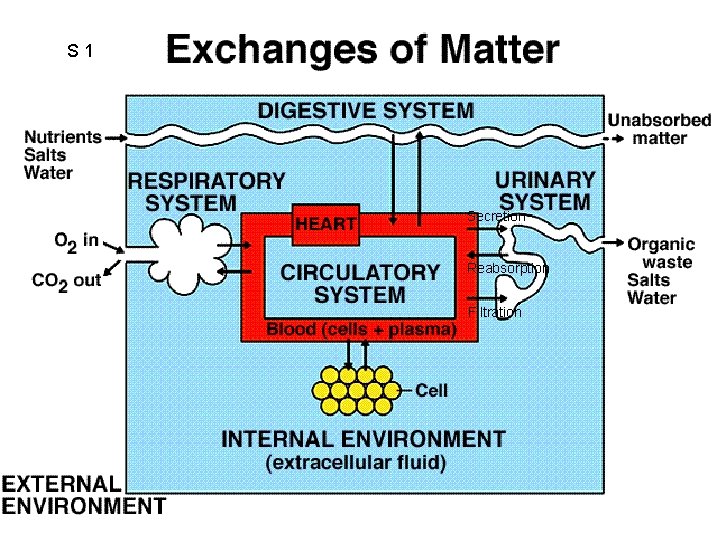
S 1 Secretion Reabsorption Filtration

S 2 • • • Circulatory System Circulates Nutrients: glucose, amino acids, fatty acids, ketones, etc Wastes: Hormones: bound & free Gases: CO 2 and O 2 Formed Elements: Cells and Cell Fragments – Erythrocytes, Leukocytes, Thrombocytes = Platelets Other roles of the Cardiovascular System Thermoregulation Blood Clotting Reproduction (ex: penile erection)
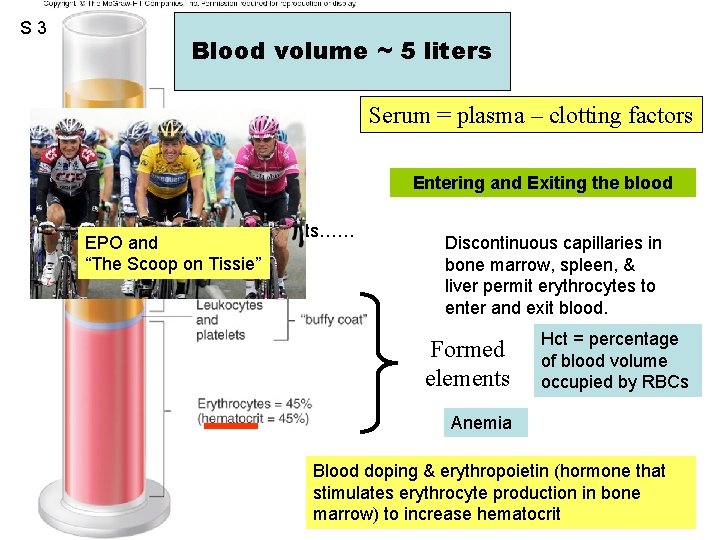
S 3 Blood volume ~ 5 liters Figure 12. 01 Serum = plasma – clotting factors Entering and Exiting the blood Components…… EPO and “The Scoop on Tissie” Discontinuous capillaries in bone marrow, spleen, & liver permit erythrocytes to enter and exit blood. Formed elements Hct = percentage of blood volume occupied by RBCs Anemia Blood doping & erythropoietin (hormone that stimulates erythrocyte production in bone marrow) to increase hematocrit
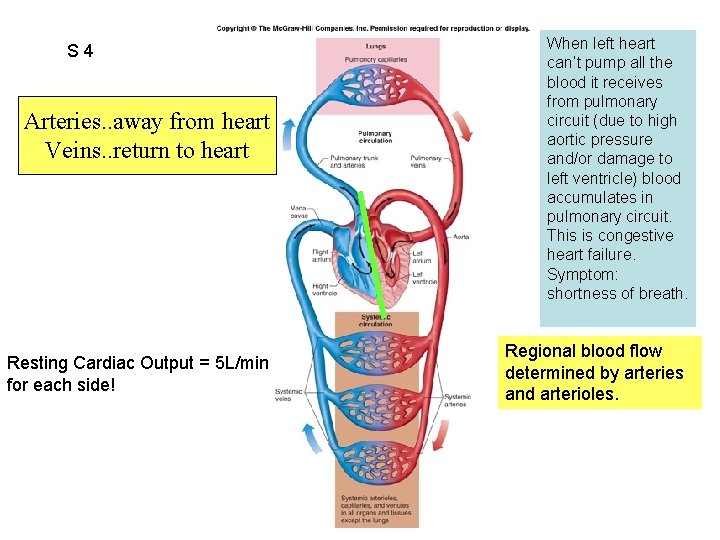
S 4 Fig. 12. 02 Arteries. . away from heart Veins. . return to heart Resting Cardiac Output = 5 L/min for each side! When left heart can’t pump all the blood it receives from pulmonary circuit (due to high aortic pressure and/or damage to left ventricle) blood accumulates in pulmonary circuit. This is congestive heart failure. Symptom: shortness of breath. Regional blood flow determined by arteries and arterioles.
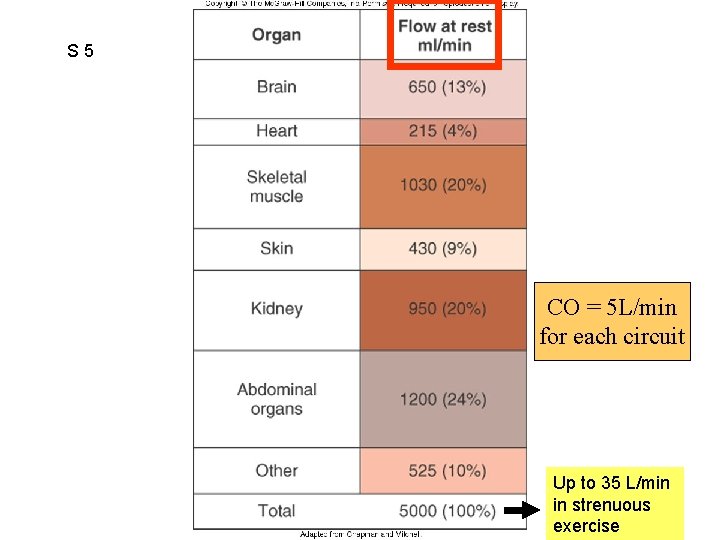
S 5 Figure 12. 04 CO = 5 L/min for each circuit Up to 35 L/min in strenuous exercise
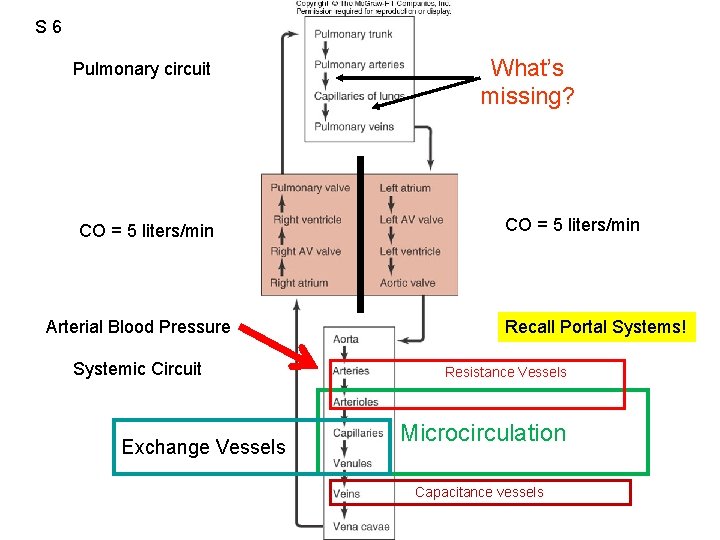
S 6 Pulmonary circuit CO = 5 liters/min Arterial Blood Pressure Systemic Circuit Exchange Vessels What’s missing? CO = 5 liters/min Recall Portal Systems! Resistance Vessels Microcirculation Capacitance vessels
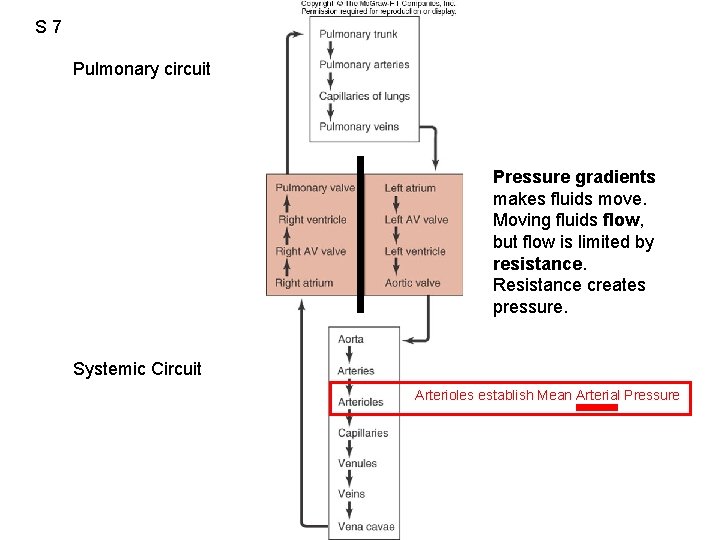
S 7 Pulmonary circuit Pressure gradients makes fluids move. Moving fluids flow, but flow is limited by resistance. Resistance creates pressure. Systemic Circuit Arterioles establish Mean Arterial Pressure
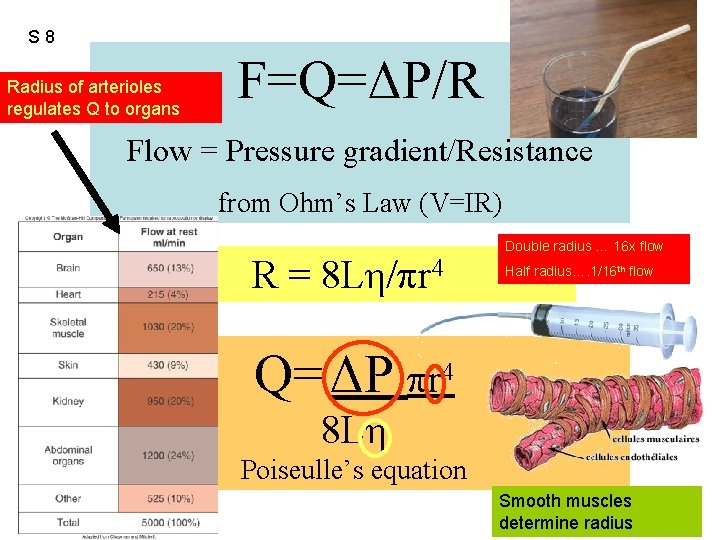
S 8 Radius of arterioles regulates Q to organs F=Q=ΔP/R Flow = Pressure gradient/Resistance from Ohm’s Law (V=IR) R= 8 Lη/πr 4 Double radius … 16 x flow Half radius…. 1/16 th flow Q= ΔP πr 4 8 Lη Poiseulle’s equation Smooth muscles determine radius
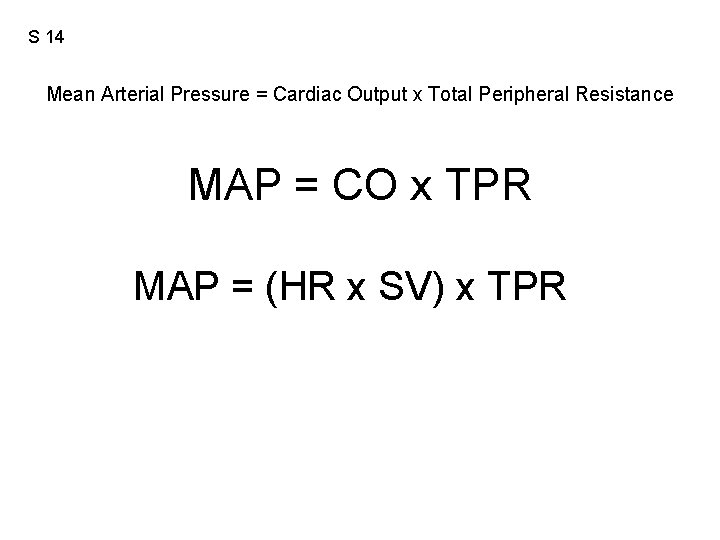
S 14 Mean Arterial Pressure = Cardiac Output x Total Peripheral Resistance MAP = CO x TPR MAP = (HR x SV) x TPR

S 1 Cardiac Output = Heart Rate X Stroke Volume What regulates heart rate? What regulates Stroke Volume? CO = HR x SV 5 L/min = 72 beat/min x 70 ml/beat The Cardiac Cycle animation
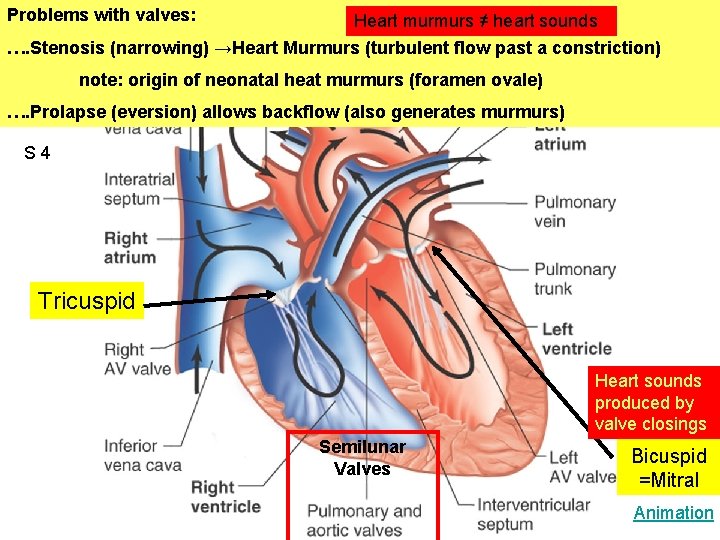
Problems with valves: Heart murmurs ≠ heart sounds …. Stenosis (narrowing) →Heart Murmurs (turbulent flow past a constriction) Figure 12. 07 note: origin of neonatal heat murmurs (foramen ovale) …. Prolapse (eversion) allows backflow (also generates murmurs) S 4 Tricuspid Heart sounds produced by valve closings Semilunar Valves Bicuspid =Mitral Animation
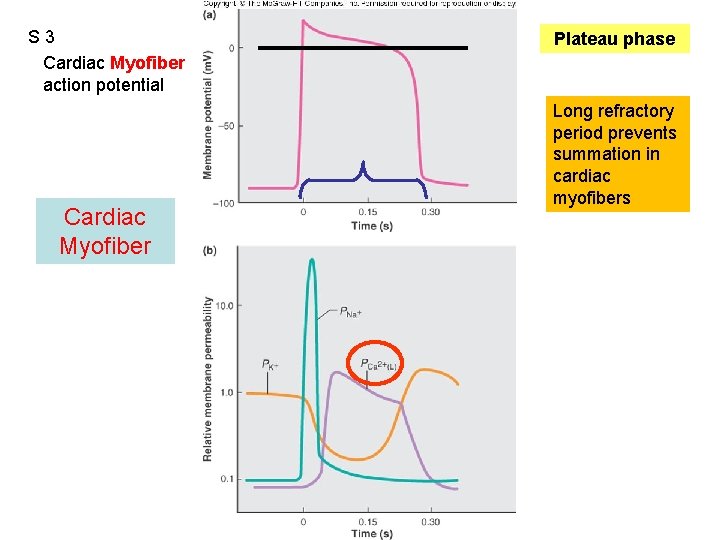
S 3 Cardiac Myofiber action potential Cardiac Myofiber Figure 12. 13 Plateau phase Long refractory period prevents summation in cardiac myofibers
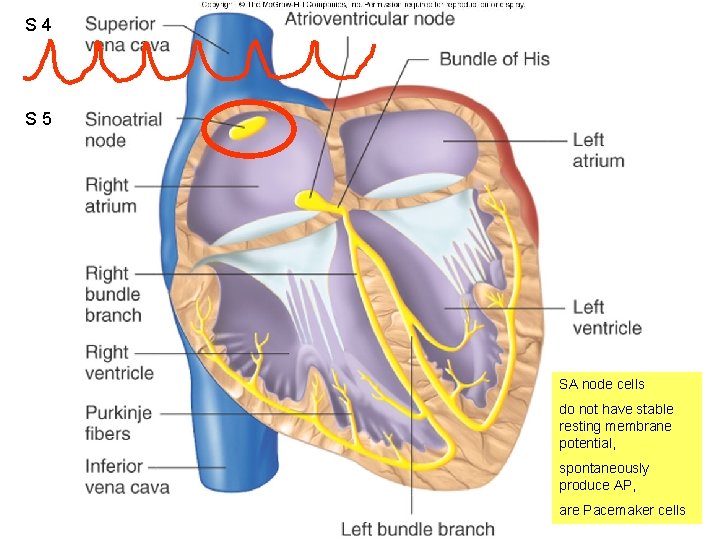
S 4 Figure 12. 11 S 5 SA node cells do not have stable resting membrane potential, spontaneously produce AP, are Pacemaker cells
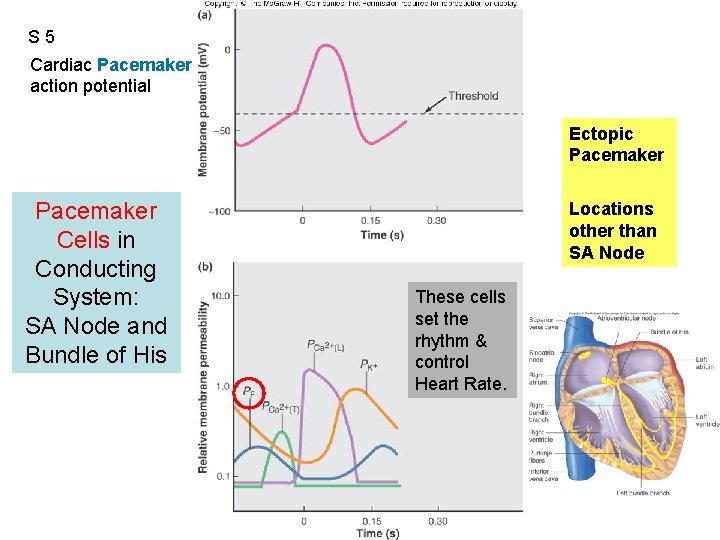
S 5 Cardiac Pacemaker action potential Figure 12. 14 Ectopic Pacemaker Cells in Conducting System: SA Node and Bundle of His Locations other than SA Node These cells set the rhythm & control Heart Rate.

1 QQ # 14: Answer one. 1. A) Which vessels are classified as exchange vessels? B) Why are they called exchange vessels? 2. A) What produces a heart sound? B) What produces a heart murmur? 3. With all other factors held constant, how would blood flow be affected by a doubling of the pressure gradient? 4. A) Explain how a heart can continue to beat even if the SA node is not functioning. B) Would this heart rate be faster or slower than the rate produced by the SA node?
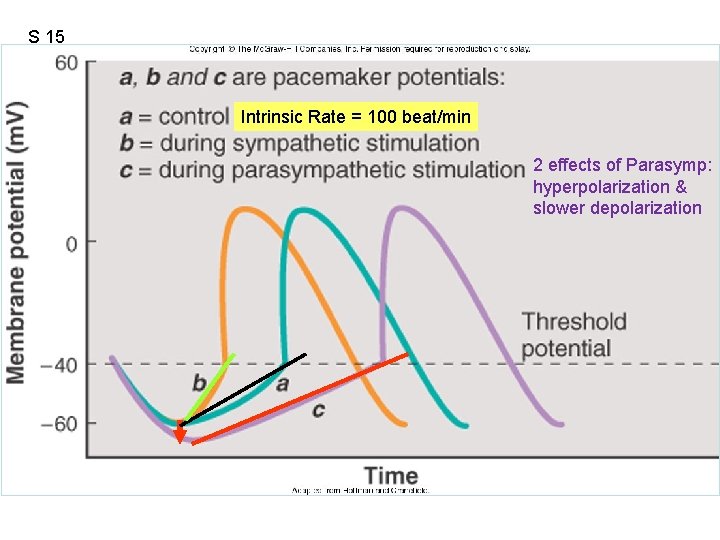
S 15 Figure 12. 22 Intrinsic Rate = 100 beat/min 2 effects of Parasymp: hyperpolarization & slower depolarization
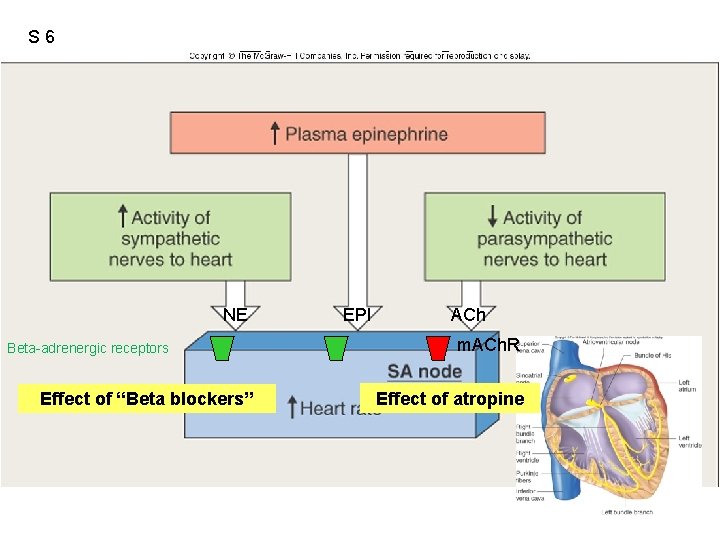
S 6 Figure 12. 23 NE Beta-adrenergic receptors Effect of “Beta blockers” EPI ACh m. ACh. R Effect of atropine
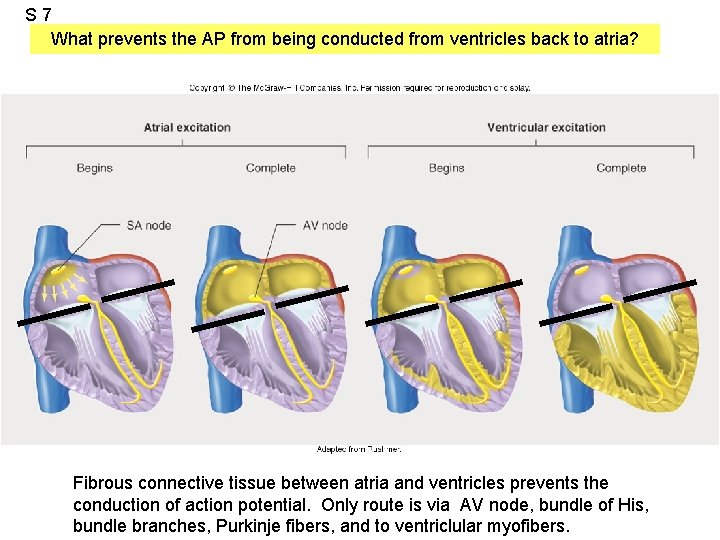
S 7 What prevents the AP from being conducted from ventricles back to atria? Fibrous connective tissue between atria and ventricles prevents the conduction of action potential. Only route is via AV node, bundle of His, bundle branches, Purkinje fibers, and to ventriclular myofibers.
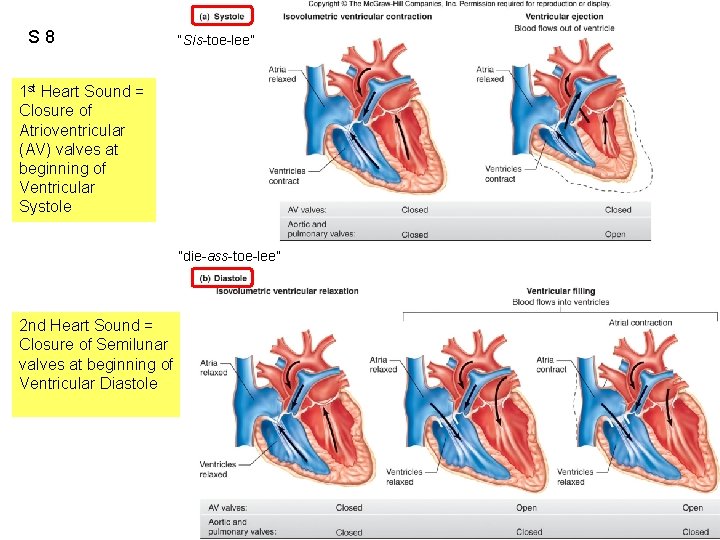
S 8 “Sis-toe-lee” 1 st Heart Sound = Closure of Atrioventricular (AV) valves at beginning of Ventricular Systole “die-ass-toe-lee” 2 nd Heart Sound = Closure of Semilunar valves at beginning of Ventricular Diastole
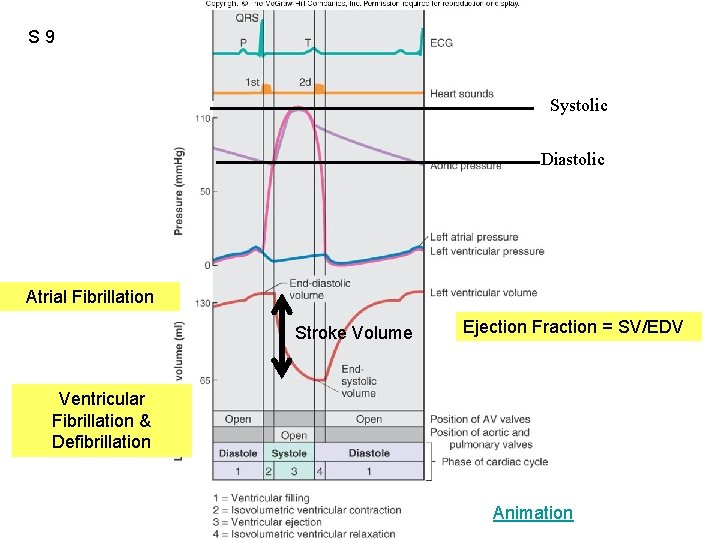
S 9 Figure 12. 20 Systolic Diastolic Atrial Fibrillation Stroke Volume Ejection Fraction = SV/EDV Ventricular Fibrillation & Defibrillation Animation
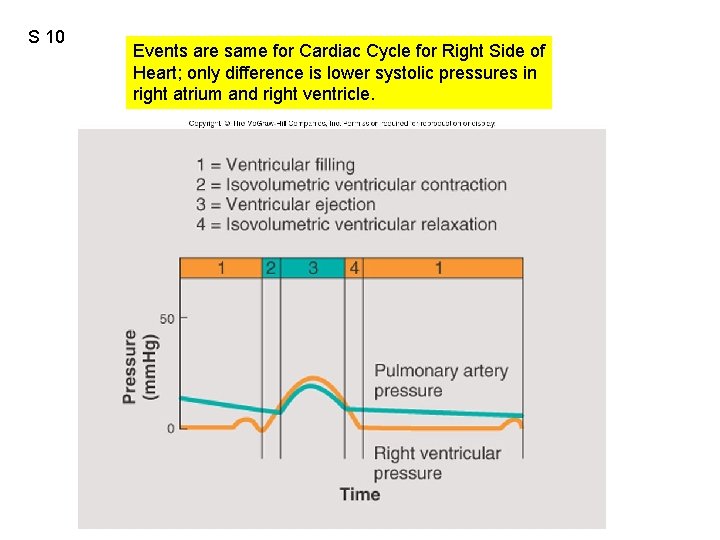
S 10 Events are same for Cardiac Cycle for Right Side of Heart; only difference is lower systolic pressures in right atrium and right ventricle.
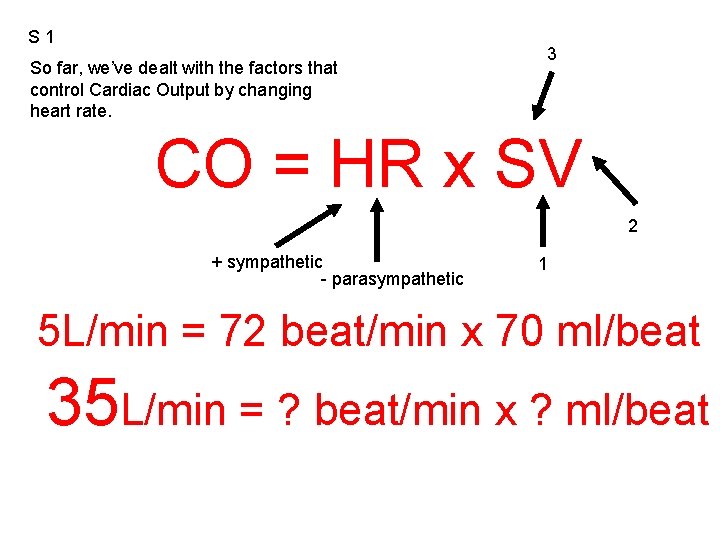
S 1 So far, we’ve dealt with the factors that control Cardiac Output by changing heart rate. 3 CO = HR x SV 2 + sympathetic - parasympathetic 1 5 L/min = 72 beat/min x 70 ml/beat 35 L/min = ? beat/min x ? ml/beat
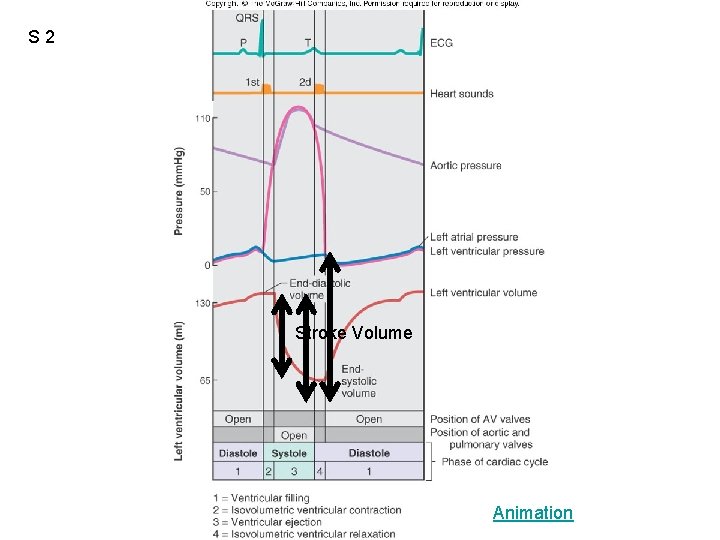
S 2 Figure 12. 20 Stroke Volume Animation
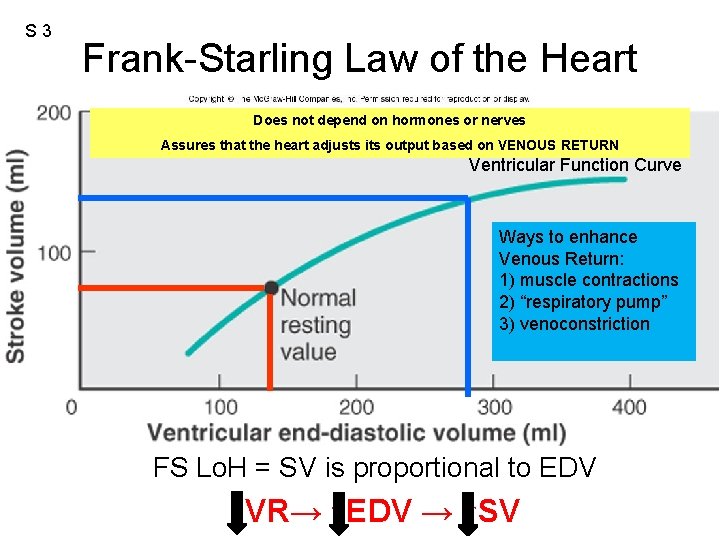
S 3 Frank-Starling Law of the Heart Does not depend on hormones or nerves Assures that the heart adjusts its output based on VENOUS RETURN Ventricular Function Curve Ways to enhance Venous Return: 1) muscle contractions 2) “respiratory pump” 3) venoconstriction FS Lo. H = SV is proportional to EDV ↑VR→ ↑EDV → ↑SV
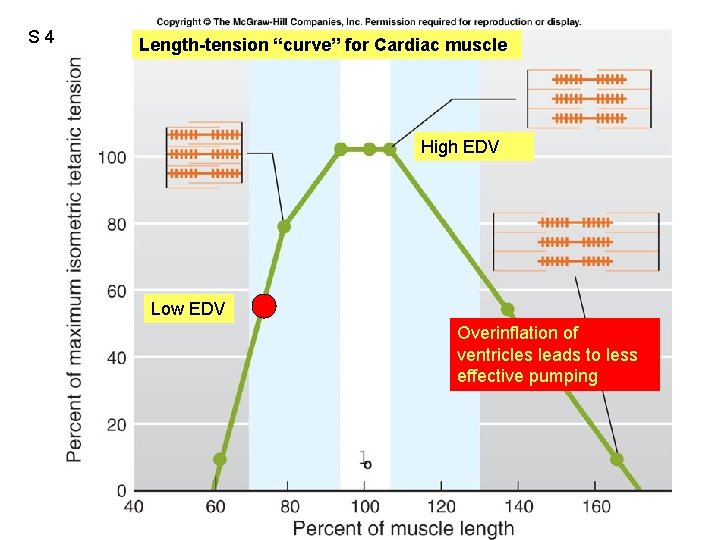
S 4 Length-tension “curve” for Cardiac muscle Fig. 09. 21 High EDV Low EDV Overinflation of ventricles leads to less effective pumping
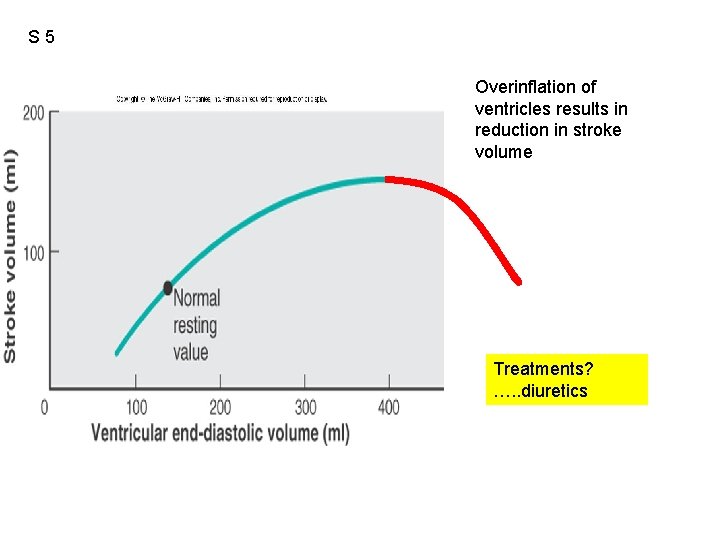
S 5 Overinflation of ventricles results in reduction in stroke volume Treatments? …. . diuretics
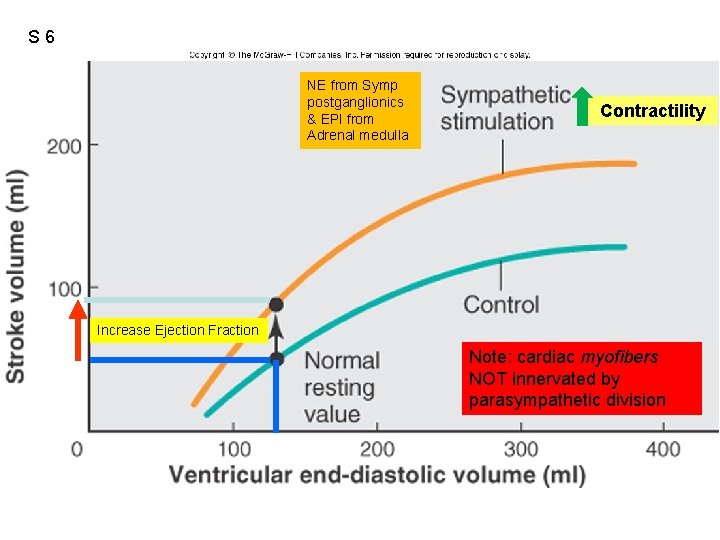
S 6 NE from Symp postganglionics & EPI from Adrenal medulla Contractility Increase Ejection Fraction Note: cardiac myofibers NOT innervated by parasympathetic division
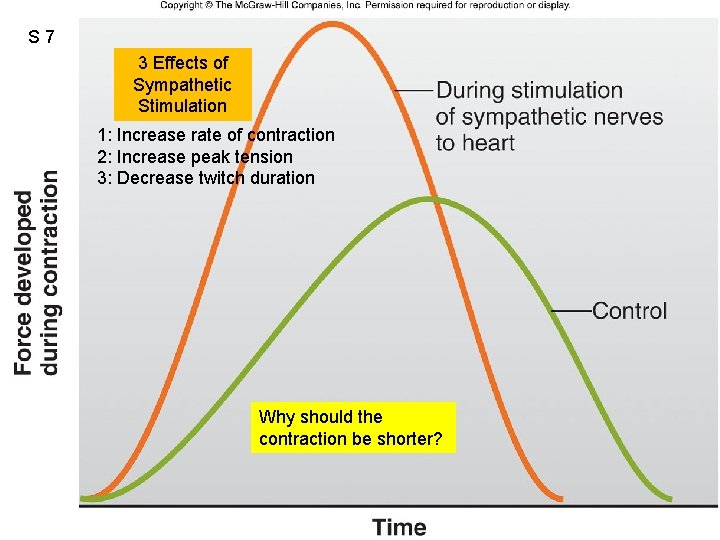
S 7 3 Effects of Sympathetic Stimulation 1: Increase rate of contraction 2: Increase peak tension 3: Decrease twitch duration Why should the contraction be shorter?

Afterload is analogous to trying to pump more air into a tire that is already fully inflated (heart contracting to overcome diastolic pressure. ) S 9 High blood pressure increases the workload of the heart…. . Cardiac hypertrophy…. increase chance of irregular conduction of AP through heart Hypertrophic cardiomyopathy

S 8 Summary: Control of Stroke Volume FS Lo. H • End diastolic volume (preload) • Contractility (strength of ventricular contraction due to adrenergic stimulation) • Pressure in arteries that must be overcome = Afterload
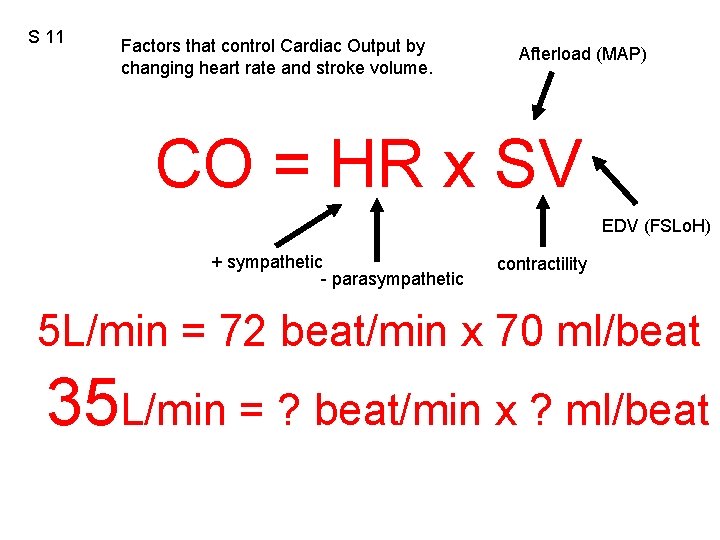
S 11 Factors that control Cardiac Output by changing heart rate and stroke volume. Afterload (MAP) CO = HR x SV EDV (FSLo. H) + sympathetic - parasympathetic contractility 5 L/min = 72 beat/min x 70 ml/beat 35 L/min = ? beat/min x ? ml/beat
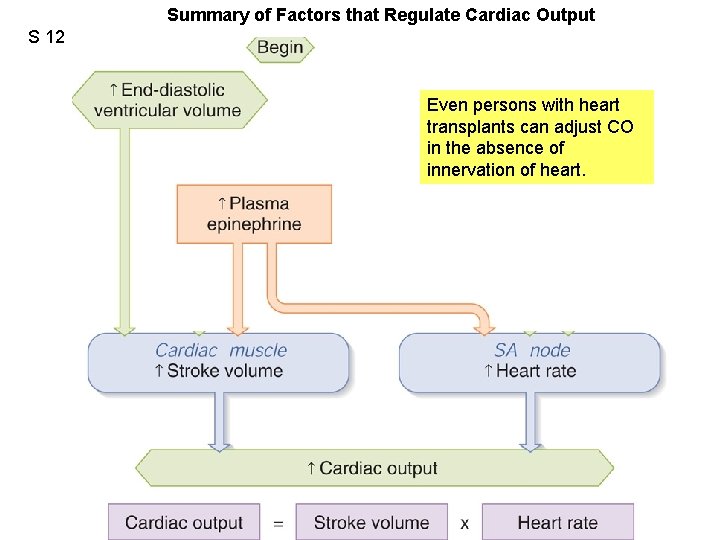
Summary of Factors that Regulate Cardiac Output S 12 Fig. 12. 28 Even persons with heart transplants can adjust CO in the absence of innervation of heart.
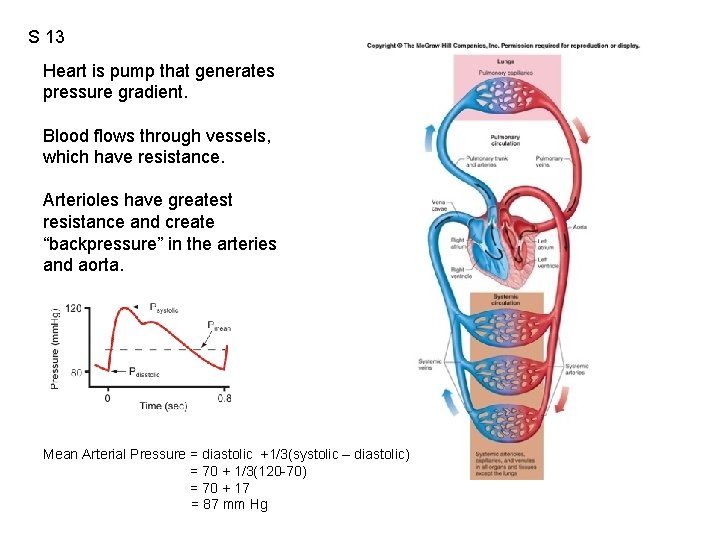
S 13 Heart is pump that generates pressure gradient. Blood flows through vessels, which have resistance. Arterioles have greatest resistance and create “backpressure” in the arteries and aorta. Mean Arterial Pressure = diastolic +1/3(systolic – diastolic) = 70 + 1/3(120 -70) = 70 + 17 = 87 mm Hg
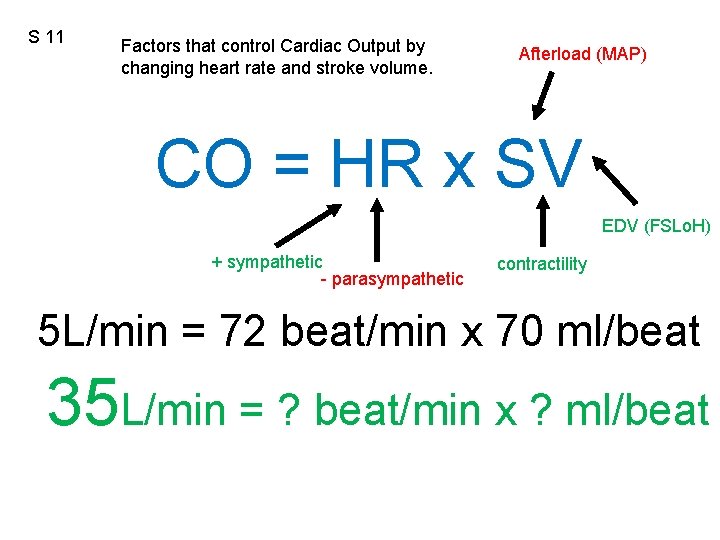
S 11 Factors that control Cardiac Output by changing heart rate and stroke volume. Afterload (MAP) CO = HR x SV EDV (FSLo. H) + sympathetic - parasympathetic contractility 5 L/min = 72 beat/min x 70 ml/beat 35 L/min = ? beat/min x ? ml/beat

S 1 Properties of Blood Vessels All vessels and heart chambers lined with ENDOTHELIAL cells (simple squamous) • Arteries • Arterioles Variable Resistance vessels • Capillaries Exchange • Venules Capacitance vessels, high • Veins compliance, low pressure, Elastic, low compliance, large diameter, low resistance vessels Wall = simple squamous endothelium No smooth muscle; cannot change diameter valves for unidirectional flow
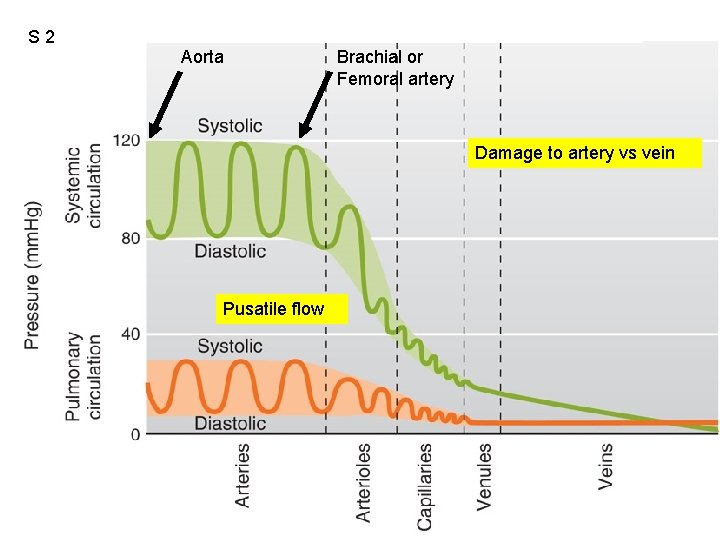
S 2 Aorta Fig. 12. 29 Brachial or Femoral artery Damage to artery vs vein Pusatile flow
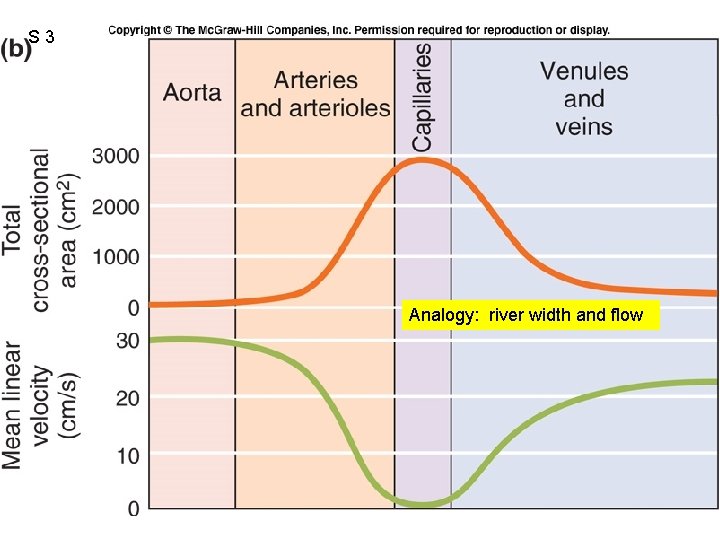
S 3 Fig. 12. 39 b Analogy: river width and flow
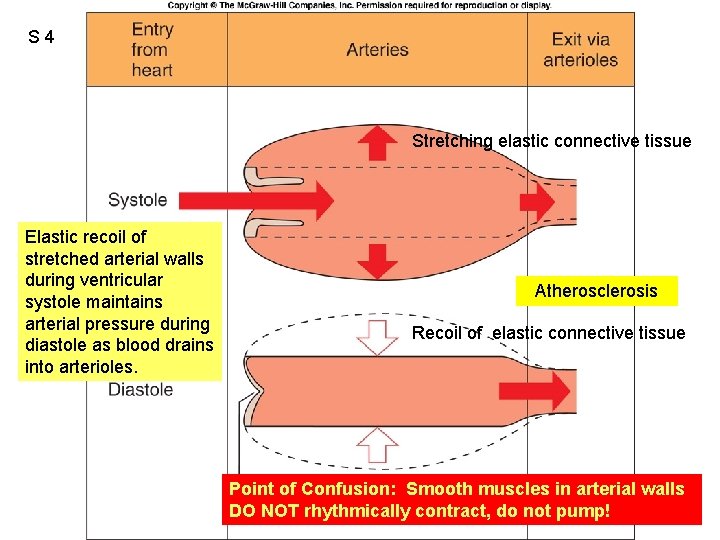
S 4 Fig. 12. 30 Stretching elastic connective tissue Elastic recoil of stretched arterial walls during ventricular systole maintains arterial pressure during diastole as blood drains into arterioles. Atherosclerosis Recoil of elastic connective tissue Point of Confusion: Smooth muscles in arterial walls DO NOT rhythmically contract, do not pump!
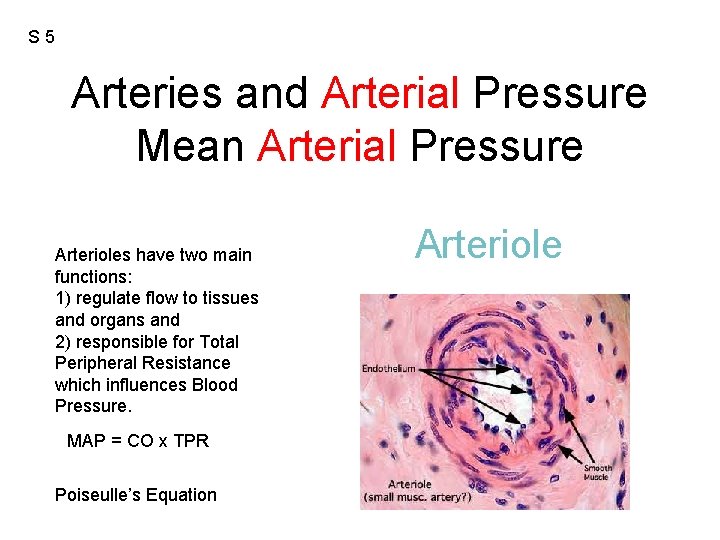
S 5 Arteries and Arterial Pressure Mean Arterial Pressure Arterioles have two main functions: 1) regulate flow to tissues and organs and 2) responsible for Total Peripheral Resistance which influences Blood Pressure. MAP = CO x TPR Poiseulle’s Equation Arteriole
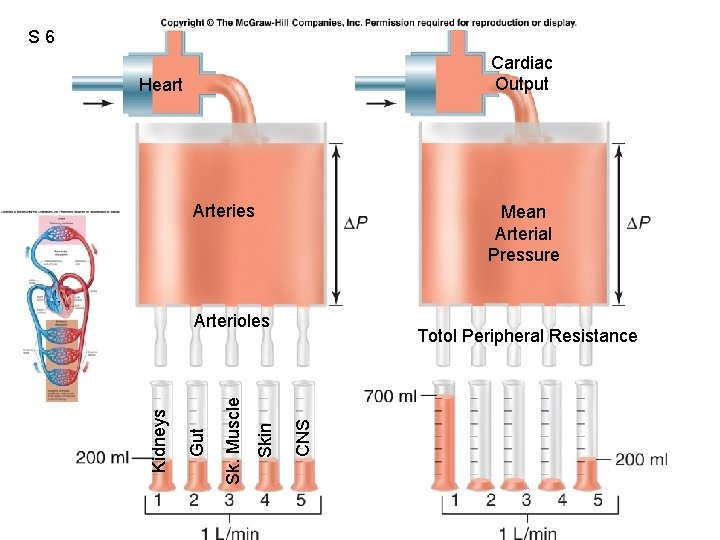
S 6 Fig. 12. 50 Heart Arteries Mean Arterial Pressure Totol Peripheral Resistance CNS Skin Sk. Muscle Gut Arterioles Kidneys Cardiac Output
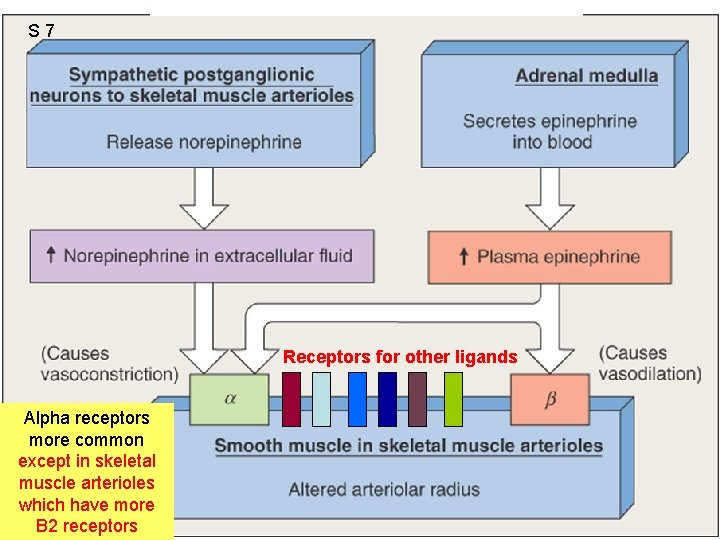
S 7 Receptors for other ligands Alpha receptors more common except in skeletal muscle arterioles which have more B 2 receptors
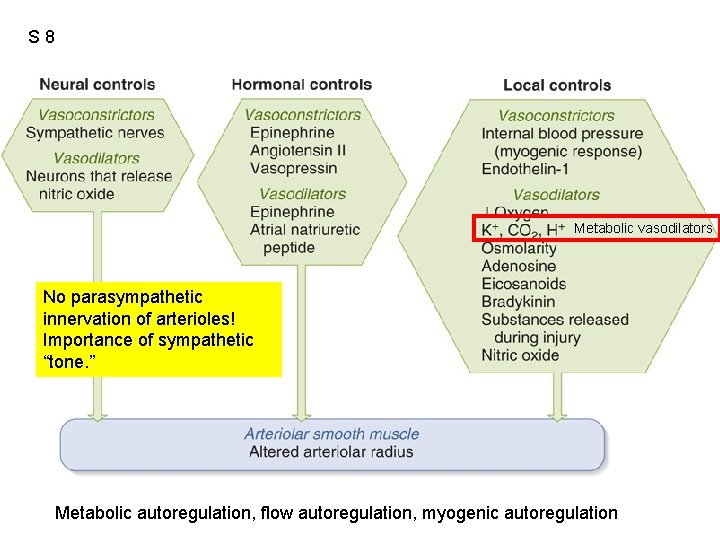
S 8 Fig. 12. 36 Metabolic vasodilators No parasympathetic innervation of arterioles! Importance of sympathetic “tone. ” Metabolic autoregulation, flow autoregulation, myogenic autoregulation
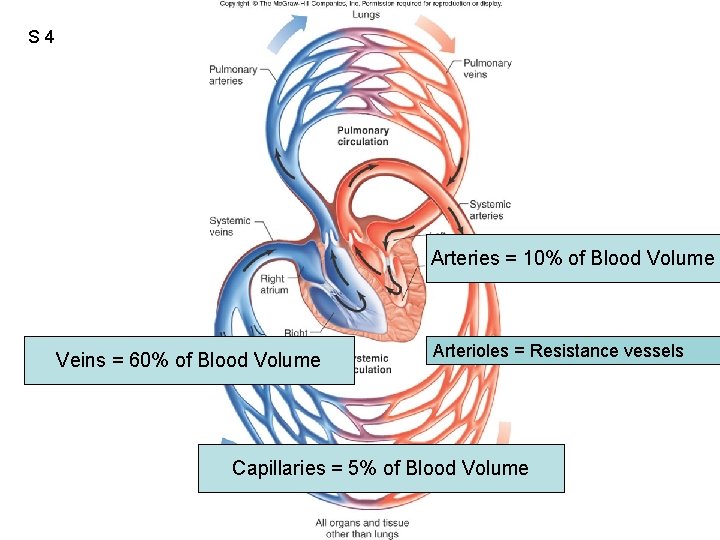
S 4 Figure 12. 02 Arteries = 10% of Blood Volume Veins = 60% of Blood Volume Arterioles = Resistance vessels Capillaries = 5% of Blood Volume
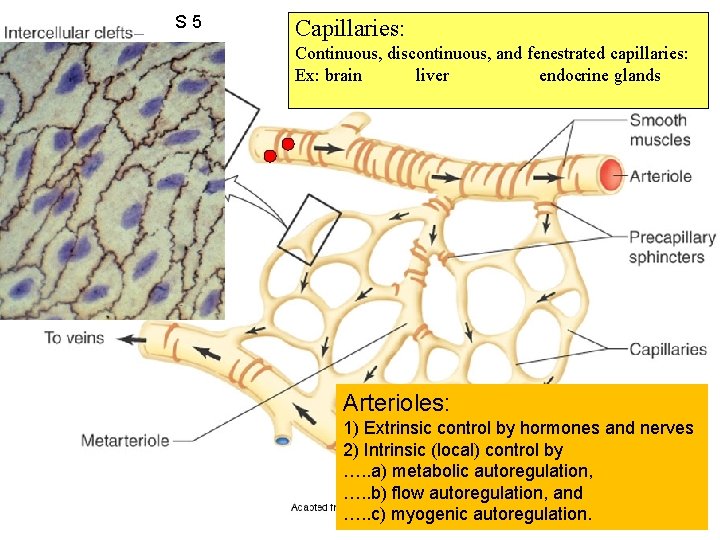
S 5 Capillaries: Figure 12. 38 Continuous, discontinuous, and fenestrated capillaries: Ex: brain liver endocrine glands Generate vasodilators and vasoconstrictors Arterioles: 1) Extrinsic control by hormones and nerves 2) Intrinsic (local) control by …. . a) metabolic autoregulation, …. . b) flow autoregulation, and …. . c) myogenic autoregulation.

1 QQ # 15 Answer one. 1. Describe metabolic autoregulation and list four substances that are classified as metabolic vasodilators. 2. What is the main difference between flow autoregulation and metabolic autoregulation? 3. Explain why the pressure in a major artery doesn’t fall to 0 during ventricular diastole.
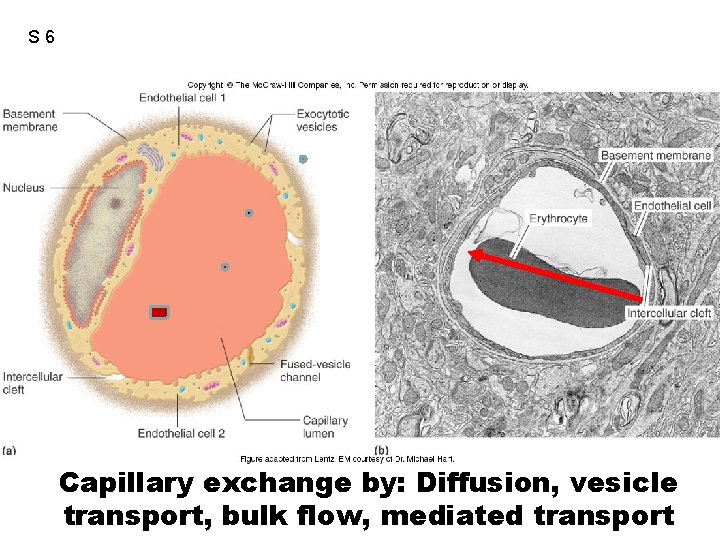
S 6 Capillary exchange by: Diffusion, vesicle transport, bulk flow, mediated transport
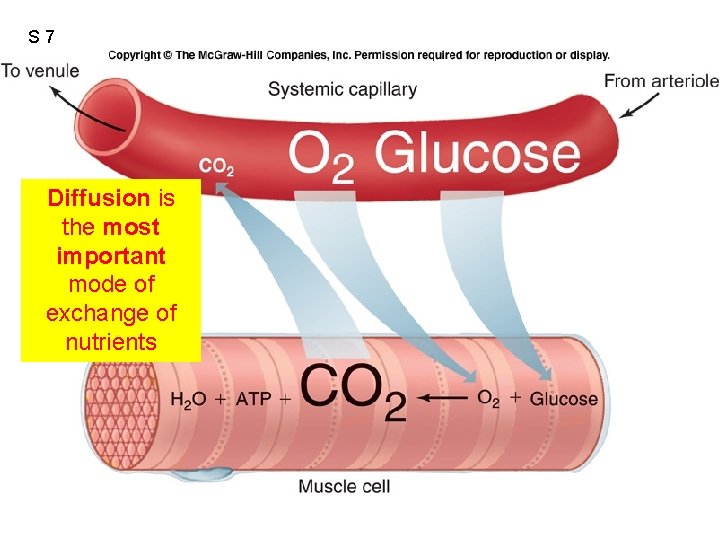
S 7 Diffusion is the most important mode of exchange of nutrients Fig. 12. 40
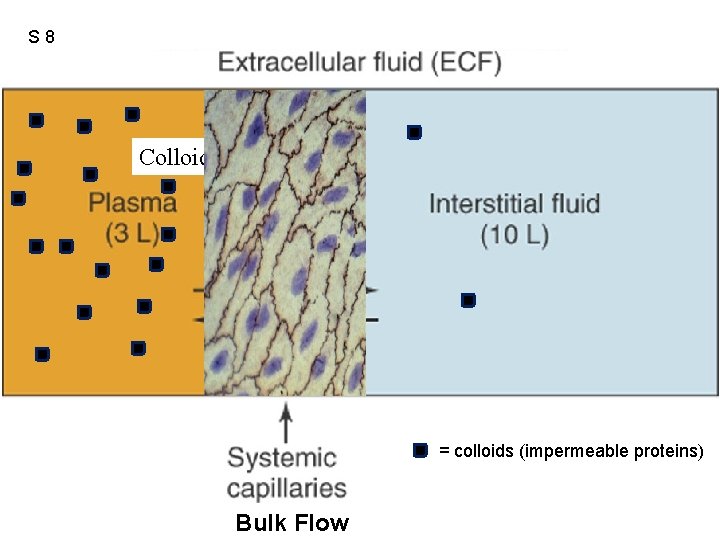
S 8 Figure 12. 41 Colloids Crystalloids = colloids (impermeable proteins) Bulk Flow
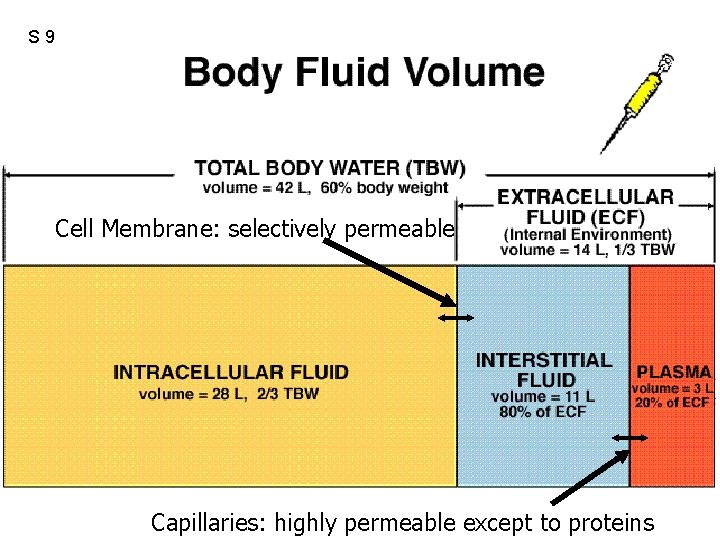
S 9 Cell Membrane: selectively permeable Capillaries: highly permeable except to proteins
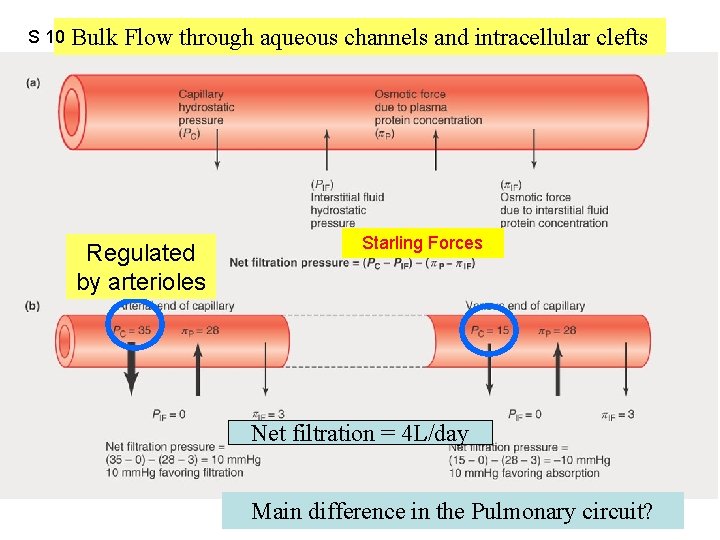
S 10 Bulk Flow through aqueous channels and intracellular clefts Figure 12. 42 Regulated by arterioles Starling Forces Net filtration = 4 L/day Main difference in the Pulmonary circuit?
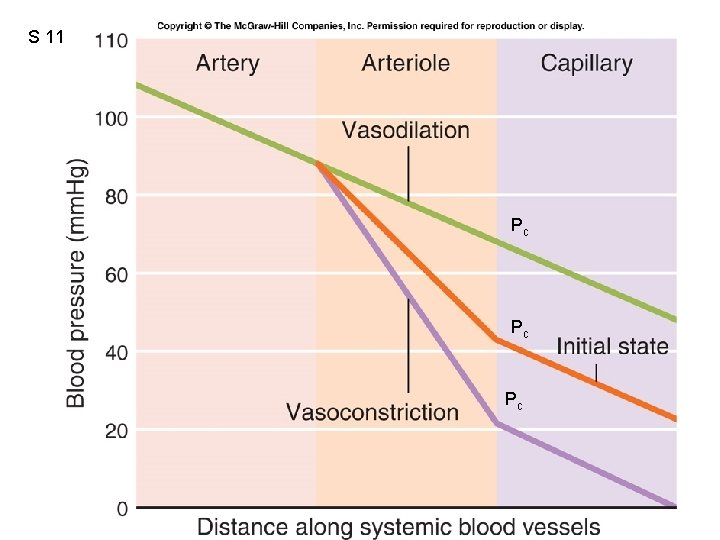
S 11 Fig. 12. 43 Pc Pc Pc

S 12 Who Cares? Aunt Esther Cancer of the liver; Failure of hepatocytes to produce plasma colloids
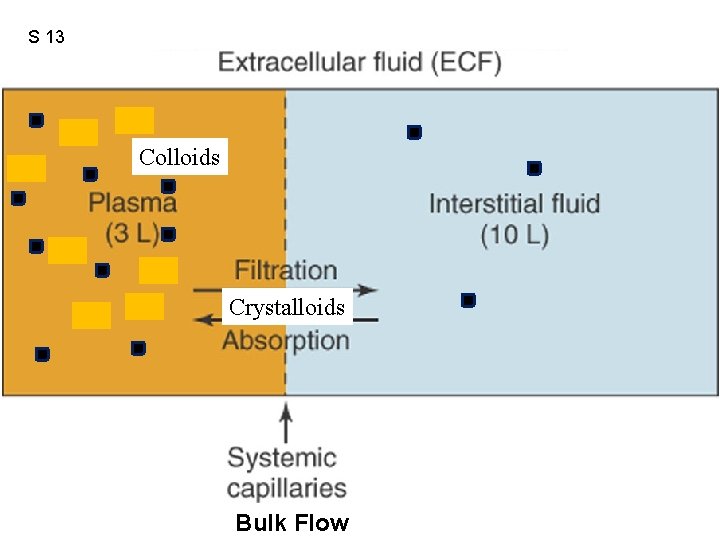
S 13 Figure 12. 41 Colloids Crystalloids Bulk Flow
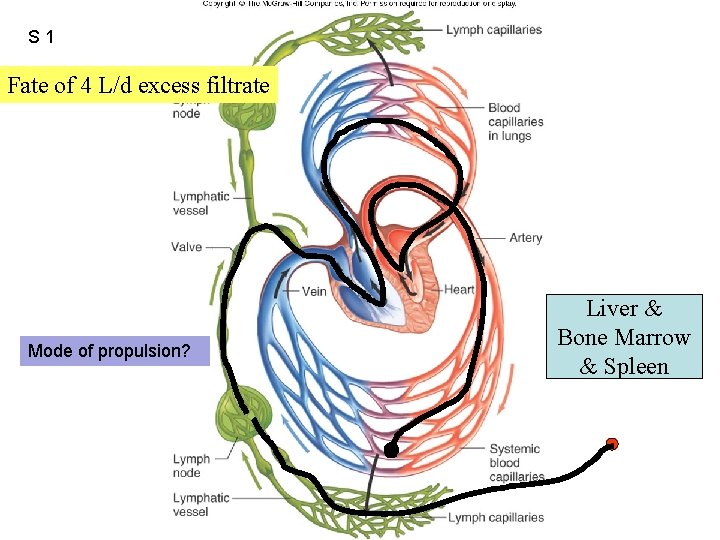
S 1 Figure 12. 47 Fate of 4 L/d excess filtrate Mode of propulsion? Liver & Bone Marrow & Spleen
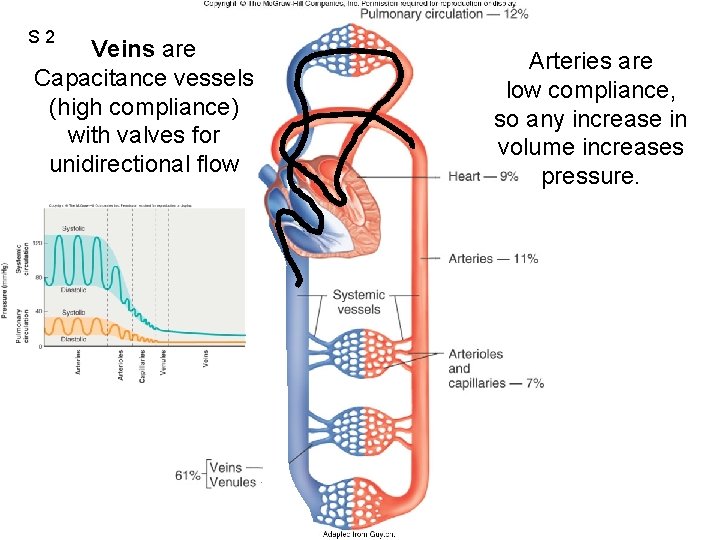
S 2 Veins are Capacitance vessels (high compliance) with valves for unidirectional flow Figure 12. 44 Arteries are low compliance, so any increase in volume increases pressure.
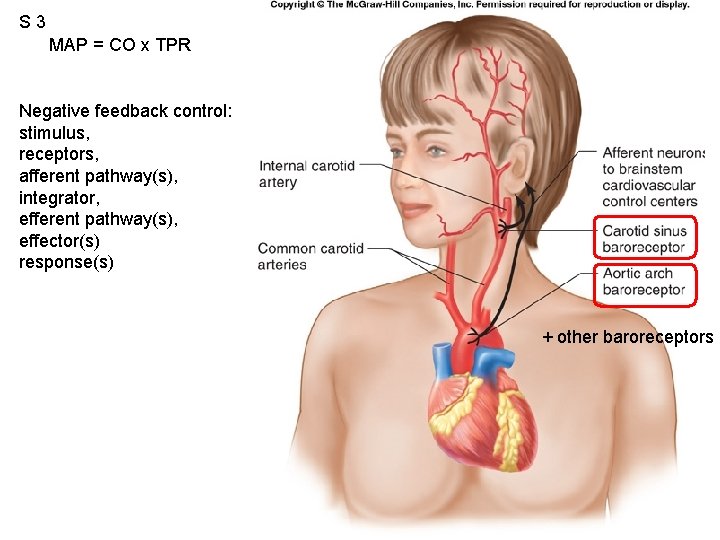
S 3 MAP = CO x TPR Fig. 12. 53 Negative feedback control: stimulus, receptors, afferent pathway(s), integrator, efferent pathway(s), effector(s) response(s) + other baroreceptors
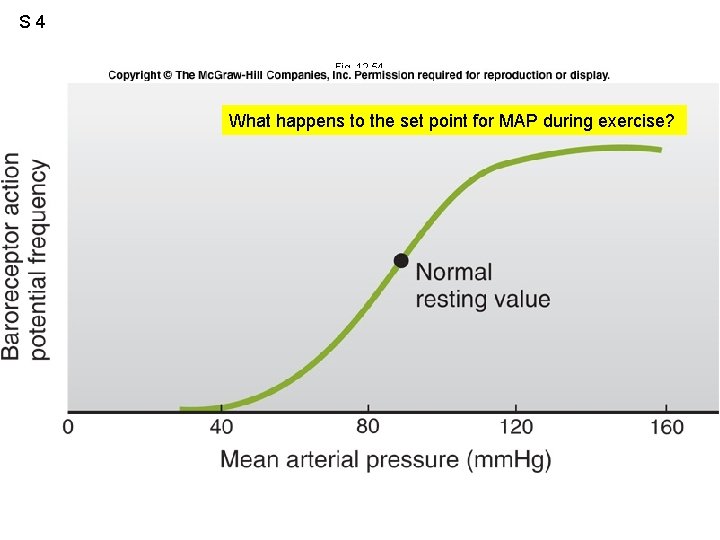
S 4 Fig. 12. 54 What happens to the set point for MAP during exercise?
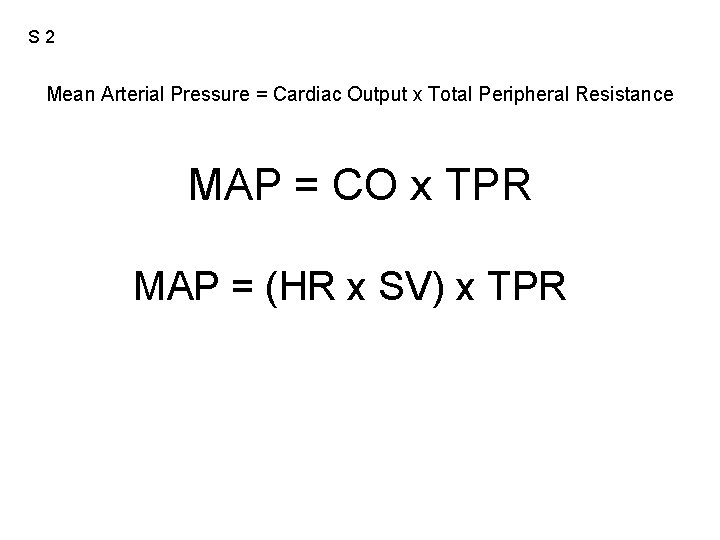
S 2 Mean Arterial Pressure = Cardiac Output x Total Peripheral Resistance MAP = CO x TPR MAP = (HR x SV) x TPR

S 6 Test 3 Hemorrhage Diagram On one page, create a well-organized diagram for the following. Beginning with a loss of about 1 liter of blood from a vein, diagram the early events associated with hemorrhage and the negative feedback responses to hemorrhage in a well-organized diagram. Write legibly! Completeness, accuracy, and detail, together with the proper sequence earn maximal points. The following abbreviations can be used: ACE, AII, Aldo (aldosterone), JGA, m. ACh. R, Hct, Q, SV, EF (ejection fraction), RBC, HR, EDV, ACh, ANH, ADH, CO, TPR, EPO, VR, MAP, EPI, NE, SAN (SA Node), a. Ad. R , b. Ad. R, Symp (sympathetic), Parasymp (parasympathetic), PV (plasma volume), r (radius), Pc, f. AP (frequency of action potentials. ) Any other abbreviations must be defined. "If in doubt, write it out!" Use single headed arrows (→) to indicate sequential relationships and doubled-stemmed arrows to indicate increases or decreases.
- Slides: 59