RSI Rapid Sequence Intubation What When Where Why

RSI: Rapid Sequence Intubation What, When, Where, Why & How Michael T. Czarnecki, MD 265

Objective What is RSI? Discuss the “ 7 P’s” of RSI Review RSI pharmacologic agents Highlight current controversies with RSI 1/17/2022 2

RSI Defined “Virtually simultaneous administration of a potent sedative agent and a neuromuscular blocking agent to induce unconsciousness and motor paralysis for tracheal intubation” 1/17/2022 3

Why Bother with RSI? Rapid airway control Less risk of aspiration Highest success rates/lowest complications – More controlled Optimal intubating conditions 1/17/2022 4

What are The Problems Inherent to Intubation? Laryngoscopy and Intubation – Increased bronchospasm – Increased ICP – Increased catecholamine release 1/17/2022 5

Beneficial Effects of RSI “Tight Heads” – Intracranial pathology “Tight Hearts” or “Tight Vessels” – Cardiovascular disease “Tight Lungs” – Reactive airway disease 1/17/2022 6

Assumptions in Airway Management Pt. has a full stomach Pt. is preoxygenated Pts. do not receive BVM ventilation unless necessary to keep O 2 sat. over 90% Sellick’s maneuver always used 1/17/2022 7

RSI: “ 7 P’s” 1. 2. 3. 4. 5. 6. 7. 1/17/2022 P = Preparation P = Preoxygenation P = Pretreatment P = Paralysis with induction P = Protection P = Placement of the tube P = Post-Intubation management 8

RSI: Timeline T – 10 minutes T – 5 minutes T – 3 minutes T=0 T + 30 seconds T + 45 seconds T + 90 seconds 1/17/2022 Prepare Preoxygenate Pretreat Paralysis with induction Protection Placement Post-Intubation management 9

Preparation: T – 10 minutes Prepare the patient – Monitoring/access – Positioning – Assess for difficult airway • “ 4 D’s”, “LEMON”, “BONES”, “SHORT” • Mallampati Prepare your equipment Prepare yourself (mental checklist) Prepare your personnel 1/17/2022 10

Difficult Airway Assessment 4 D’s – Distortion, Disproportion, Dysmobility, Dentition BONES – Beard, Obese, No teeth, Elderly, Snores (sleep apnea) SHORT – Surgery (head/neck/jaw), Hematoma, Obese, Radiation, Tumor LEMON MALLAMPATI Always have a “Rescue Airway” technique ready JUMP AHEAD 1/17/2022 11
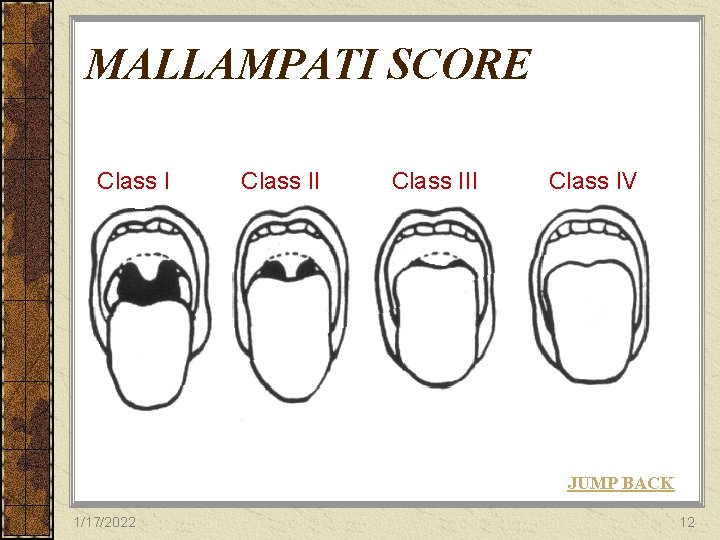
MALLAMPATI SCORE Class III Class IV JUMP BACK 1/17/2022 12

60 -SECOND EXAM “LEMON” Look for external difficulty Evaluate using 3=3=2 rule 3 fingers fit II) in mouth Mallampatiü(Class I& ü 3 fingers fit from mentum Obstruction to hyoid cartilage ü 2 fingers fit from mandible Neck Mobility to top of thyroid cartilage JUMP BACK 1/17/2022 13
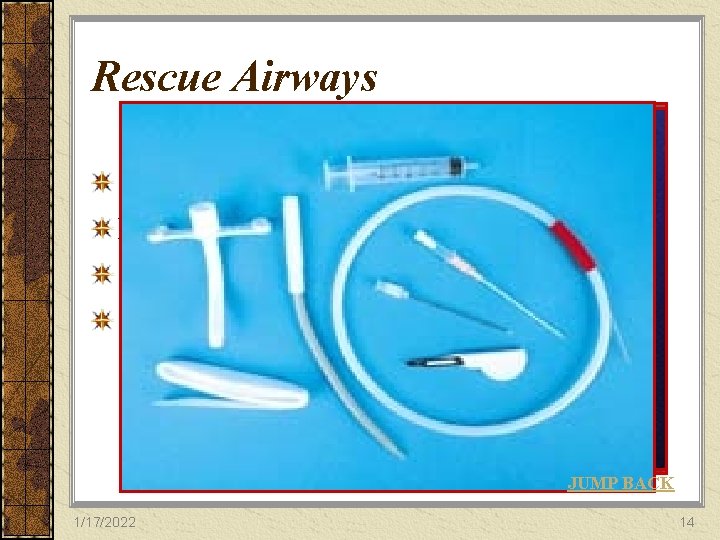
Rescue Airways Gum Elastic Bougie (GEB) Laryngeal Mask Airway (LMA/ILMA) Combitube Surgical Cricothyrotomy JUMP BACK 1/17/2022 14

Preoxygenate: T – 5 minutes Provides reservoir of oxygen during apnea If pt. spont. breathing – then NRB for 5’ – Provides maximum of 70% Fi. O 2 Avoid bagging the spont. breathing patient – If needed, use sellick & airway adjunct – 8 effective Vital Capacity breaths provides best preoxygenation 1/17/2022 15

Pretreat: T – 3 minutes L - Lidocaine O - Opiates A - Atropine D – Defasiculating Agent 1/17/2022 16

Lidocaine (1. 5 mg/kg) Consider in “Tight Head” or “Tight Lungs” – Blunts ICP rise (? ? ) – Suppress cough response • may blunt bronchospasm • may blunt sympathetic response Does Lido help in head trauma? – No clinical trials have answered question – Not proven to change outcome – Little downside in using Robinson, Emeg Med J 2001; 18: 453 1/17/2022 17

Opioids Fentanyl (3 mcg/kg slow IV over 3’) – Consider in “Tight Heads”, “Tight Heart”, & “Tight Vessels” – Beware: cautious use in pt’s dependent on sympathetic drive (aka, trauma) 1/17/2022 18

Atropine Only needed in: – Children under 10 y. o. – Adults receiving 2 nd dose of succinylcholine 0. 01 mg/kg IV push – Minumum dose: 0. 1 mg 1/17/2022 19

Defasiculating Agent Use any paralytic at 10% paralyzing dose Consider in “Tight Heads” Beware: may cause hypoventilation and frank paralysis – be prepared Who needs defasiculation? – Helps mitigate ICP rise with succinylcholine – Not really useful in any other ICU situation 1/17/2022 20

Paralysis with Induction: T = 0 Tailor inducing agent to specific needs – Barbituates – Etomidate – Midazolam – Ketamine – Propofol JUMP AHEAD 1/17/2022 21

Barbituates Decreases GABA dissociation at receptor Rapid onset sedation Decreases ICP Hypotension (especially in hypovolemia) Choices: – Thiopental, pentobarbital, methohexital Overall – Etomidate is better that Barbs JUMP BACK 1/17/2022 22

Thiopental Onset 15 seconds, duration 3 -5 minutes Cardiac depressant, venodilator – Hypotension Dose depedent on pt. profile – Euvolemic adult (3 -5 mg/kg IV) – Hypovolemic adult (1 -3 mg/kg IV) JUMP BACK 1/17/2022 23

Etomidate Nonnarcotic, nonbarbituate, nonanalgesic Minimal cardio effects, lowers ICP Is it the ideal agent for RSI? – May cause critical adrenal suppression • Inhibits adrenal mitochondrial hydroxylase activity • Occurs after both single bolus and infusions • Infusions incr. ICU death rate & incr. infections – Clinical significance is unclear • Randomized, controlled trials on outcomes needed Malerba, et al: Intensive Care Med 2005 1/17/2022 24
Etomidate (con’t) Induction dose: 0. 2 – 0. 3 mg/kg IV Onset: 20 – 30 seconds Duration: 7 – 15 minutes May cause myoclonic jerking, hiccups, injection pain, N/V (also on emergence) Risk for adrenal insufficiency incr. 12 -fold Jackson, Chest 2005 Mar Murray, Chest 2005 Mar; 127: 707 -709 1/17/2022 JUMP BACK 25

Midazolam Nonanalgesic sedative, anxiolytic, amnestic Respiratory depressant and hypotension – Give slow IV – Give ½ the dose in elderly or COPD Rapid onset (< 1 minute) Induction dose (0. 1 - 0. 3 mg/kg) DIFFERENT than sedation dose (0. 01 – 0. 03 mg/kg) – In RSI, 92% of adults are underdosed Sagarin, et al: Acad Emerg Med 2003 Apr; 10: 329 -38 1/17/2022 JUMP BACK 26

Ketamine (1 – 2 mg/kg) Dissociative, analgesic, amnestic Causes catecholamine release – Incr. BP, HR, ICP, Laryngospasm risk Bronchodilator → induction agent in asthma Onset: 15 – 30 seconds Duration: 10 – 15 minutes JUMP BACK 1/17/2022 27

Propofol (0. 5 – 1. 2 mg/kg) (white magic, milk of amnesia) Sedative-hypnotic Cardiac depressant, venodilator – Hypotension – Decr. ICP at expense of CPP JUMP BACK 1/17/2022 28

NMBs: Neuromuscular Blocking Agents Depolarizing – Succinylcholine Non-Depolarizing – Pan/Vec/Atra/Rocuronium Potential Problems – Inadequate pre-intubation neuro exam – Failure to sedate – Inadequate pre-treatment or inadequate dosing – Aspiration and Dysrhythmias – Failed intubation → surgical airway needed 1/17/2022 29

Succinylcholine (1. 5 – 2. 0 mg/kg) Onset: 15 – 30 sec; Duration: 5 – 12 min Contraindications: – FHx malignant hyperthermia, burns, crush injuries, progressing neuromuscular disease Side Effects: – Brady, hyper-K+, fasciculations, MH • ↓HR: pretreat all kids; adults 2 nd dose with atropine • ↑K+: peaks in 5’, resolves in 15’ – Treat like any hyperkalemia case Use actual-body weight for dose Rose, et al: Anesth Analg 2000 1/17/2022 30
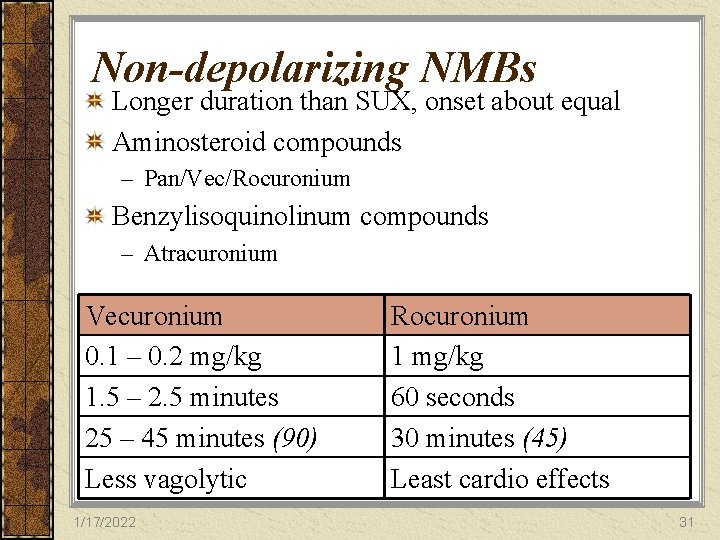
Non-depolarizing NMBs Longer duration than SUX, onset about equal Aminosteroid compounds – Pan/Vec/Rocuronium Benzylisoquinolinum compounds – Atracuronium Vecuronium 0. 1 – 0. 2 mg/kg 1. 5 – 2. 5 minutes 25 – 45 minutes (90) Less vagolytic 1/17/2022 Rocuronium 1 mg/kg 60 seconds 30 minutes (45) Least cardio effects 31

Rocuronium Is it equivalent to SUX? – Meta-analysis 1600 pts → equivalent in: • Acceptable conditions for intubation • Rates of intubation success – But SUX is BEST at creating EXCELLENT conditions Perry, AEM 2002 1/17/2022 32

RSI: Timeline T – 10 minutes T – 5 minutes T – 3 minutes T=0 T + 30 seconds T + 45 seconds T + 90 seconds 1/17/2022 Prepare Preoxygenate Pretreat Paralysis with induction Protection Placement Post-Intubation management 33
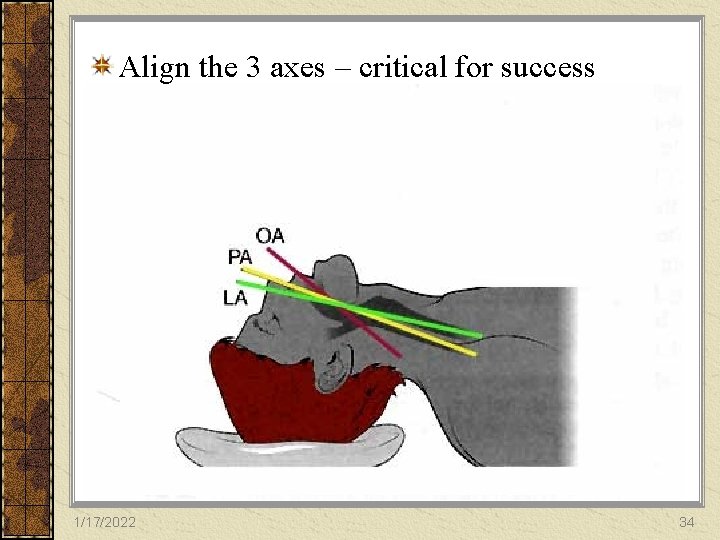
Align the 3 axes – critical for success Sellick’s maneuver 1/17/2022 34

Confirm placement/review CXR Secure tube Vent Settings Administer sedation Maintain paralysis if indicated And…. . 1/17/2022 35

Don’t Ever Forget the “ 7 Ps” P = Preparation P = Preoxygenation P = Pretreatment P = Paralysis with induction P = Protection P = Placement of the tube P = Post-Intubation management 1/17/2022 36
WHEN IN DOUBT, PULL IT OUT! 1/17/2022 37
- Slides: 37