Royal Oldham Hospital Emergency Medicine Induction Programme Oxygen




















- Slides: 26

Royal Oldham Hospital Emergency Medicine Induction Programme Oxygen delivery

Case 1 n n A 64 year old woman 3 days difficulty in breathing Much worse over last 12 hours On examination n sitting bolt upright n very anxious n n Her observations are n Pulse 134/min n BP 112/62 n RR 40/min n Sa. O 2 92% n GCS 15/15 sweaty Thoughts?

Case 1 n What more would you like to know? • PMH - Nil • SH -Gave up smoking 12 years ago • Temperature 37. 9 • ABGs on air p. H 7. 36 p. O 2 7. 2 p. CO 2 5. 1

Case 1 n How much oxygen should we give her? n 21% n 24% n 28% n 35% n 40% n 60% n Maximal

Guidelines for the use of oxygen in the ED Breathless patient prior to medical review COPD, previous Bi. PAP, Home oxygen, Alert on A&E card • Continuous sats monitoring • Use Venturi mask 24 -28% to maintain sats 88 -92% • Nebulise on air • Use nasal prongs 1 -4 L/min to provide O 2 during nebs only • Review O 2 therapy after medical review Asthma, LVF, major trauma, Pneumothorax, unwell child • Continuous sats monitoring • Provide O 2 via non-rebreathe mask at 15 L/min • Review O 2 requirements after medical review

Oxygen delivery n What oxygen delivery devices do you know? n How much oxygen do they deliver?

Nasal Cannulae n n n n Recommended in the Guideline as suitable for most patients with both type I and II respiratory failure. 2 -6 L/min gives approx 24 -50% FIO 2 depends on oxygen flow rate and patient’s minute volume and inspiratory flow and pattern of breathing. Comfortable and easily tolerated No re-breathing Low cost product Preferred by patients (Vs simple mask)

Simple face mask/Hudson (Medium concentration, variable performance) n n Used for patients with type I respiratory failure. Delivers variable O 2 concentration between 35% & 60%. Low cost product. Flow 5 -10 L/min Flow must be at least 5 L/min to avoid CO 2 build up and resistance to breathing (although packaging may say 2 -10 L)

Venturi or Fixed Performance Masks Aim to deliver constant oxygen concentration within and between breaths. 24 -40% Venturi Masks operate accurately A 60% Venturi mask gives ~50% FIO 2 With TACHYPNOEA (RR >30/min) the oxygen supply should be increased by 50% Increasing flow does not increase oxygen concentration


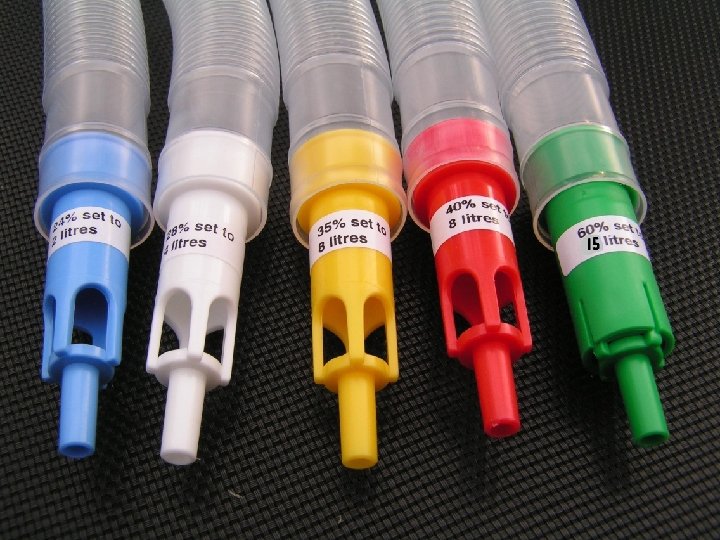
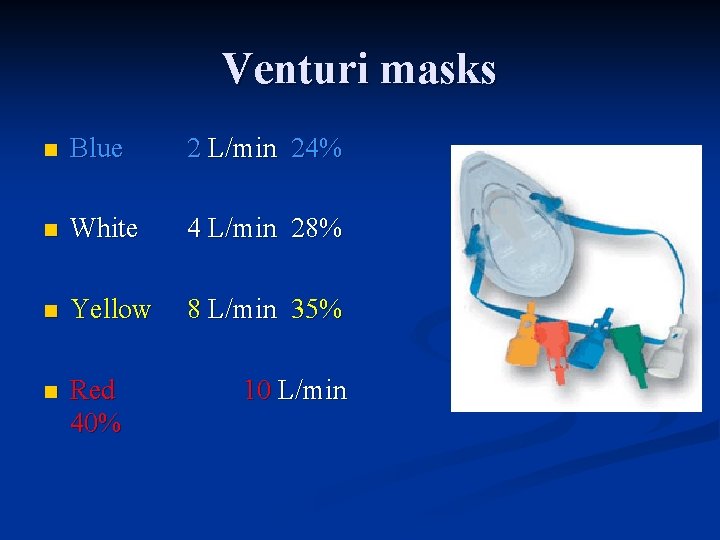
Venturi masks n Blue 2 L/min 24% n White 4 L/min 28% n Yellow 8 L/min 35% n Red 40% 10 L/min

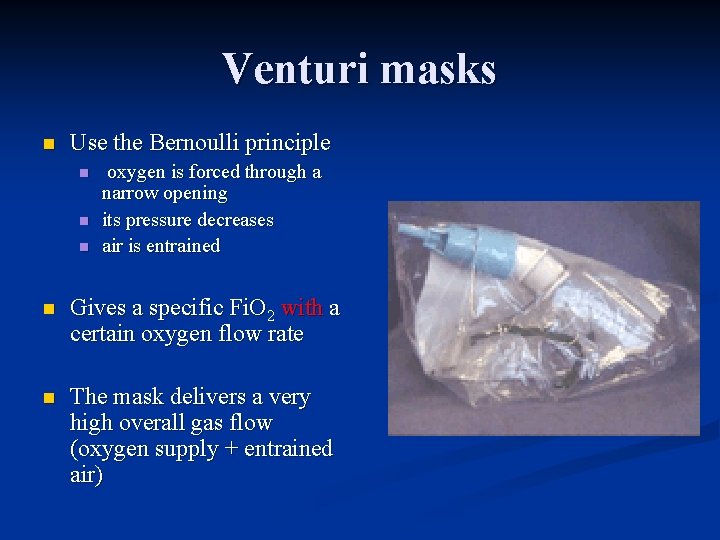
Venturi masks n Use the Bernoulli principle n n n oxygen is forced through a narrow opening its pressure decreases air is entrained n Gives a specific Fi. O 2 with a certain oxygen flow rate n The mask delivers a very high overall gas flow (oxygen supply + entrained air)

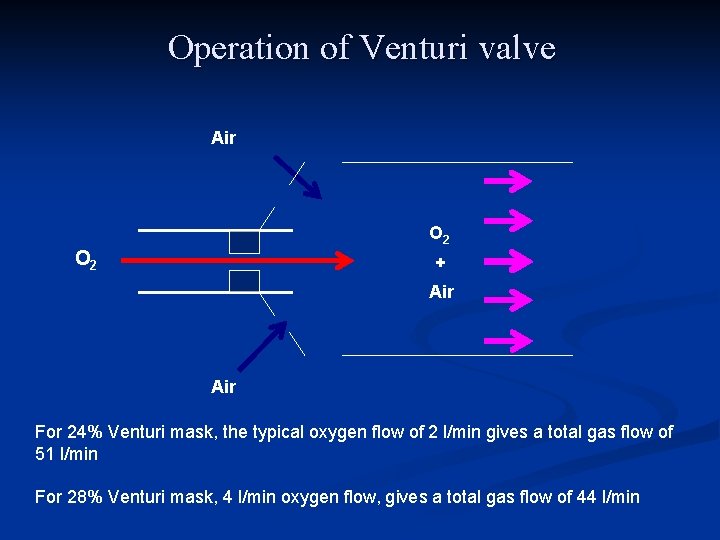
Operation of Venturi valve Air O 2 + Air For 24% Venturi mask, the typical oxygen flow of 2 l/min gives a total gas flow of 51 l/min For 28% Venturi mask, 4 l/min oxygen flow, gives a total gas flow of 44 l/min

Non-rebreathing mask n Cheap, available everywhere n Can cause claustrophobia n May cause CO 2 rebreathing if low oxygen flows used n Will take high (>15 l/min) oxygen flow rate n Max Fi. O 2 60% n Needs correct set-up

Non-rebreathing mask n High flow (15 l/min) oxygen MUST be used n Occlude the valve to fill the bag first, mould the metal strip onto the patient’s nose and tighten the straps to reduce leak The bag must fill and empty with each breath n If it doesn’t, the Fi. O 2 = 40% n

Oxygen Flow Meter The centre of the ball indicates the correct flow rate. This diagram illustrates the correct setting of the flow meter to deliver a flow of 2 litres per minute

Nebuliser n Basically a Hudson mask with an attachment n Max Fi. O 2 = 40%

Bag/valve/mask n Self inflating bag will work even without gas flow n Delivers Fi. O 2 close to 100% when reservoir fitted n High resistance to spontaneous ventilation due to valves – don’t use if pt breathing (work of breathing ↑) n Excellent for augmenting patients’ own efforts

Mapleson C circuit n Delivers Fi. O 2 close to 100% n Ideal for patients breathing spontaneously n Needs continuous gas flow (unlike BVM) n Difficult to use, experience needed

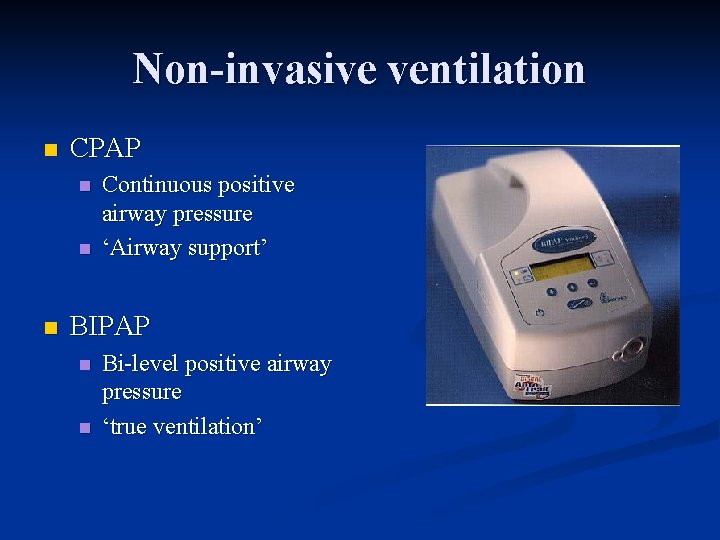
Non-invasive ventilation n CPAP n n n Continuous positive airway pressure ‘Airway support’ BIPAP n n Bi-level positive airway pressure ‘true ventilation’

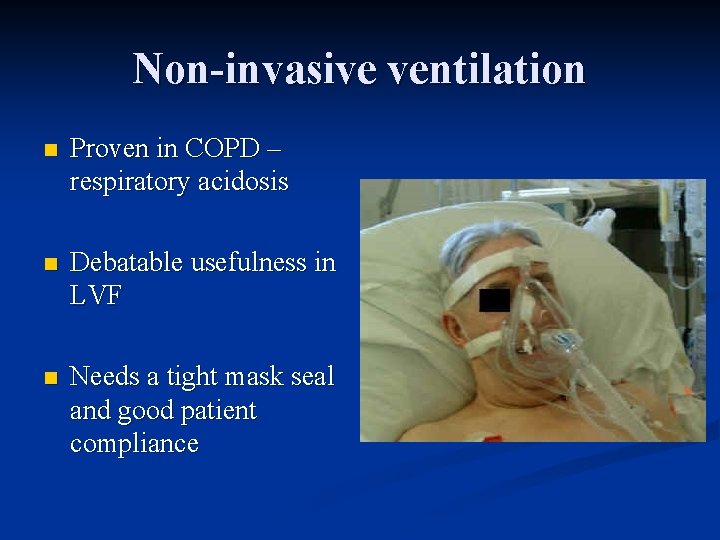
Non-invasive ventilation n Proven in COPD – respiratory acidosis n Debatable usefulness in LVF n Needs a tight mask seal and good patient compliance

What device and flow rate should you use in each situation?

Oxygen therapy 2008 onwards – Follow Trust policy Selected COPD patients Critical illness Most patients

Pitfalls n Don’t be scared to give high Fi. O 2 to anyone in respiratory distress n Some patients will need limited oxygen n n reassessment is the key The OXYGEN outlet looks very similar to the AIR outlet. n Make sure you are giving the correct gas! n No flow meter should be attached to the air outlets but may have been accidently left if used in a previous patient

Key point Hypoxia Kills Excess Carbon Dioxide can be Treated Follow Trust Guidelines on Prescription and Delivery

Any questions