Rome III based IBS and female FullYoung Chang

Rome III based IBS and female Full-Young Chang GI Division Feb. 7, 2007 at the Dept of GYN


Dr. G (GI & GYN)? 1971



Hospital of the University of Pennsylvania (HUP) 美國費城賓州大學附屬醫院(1989年 7月至 1990年 7月)

IBS, an example of FGID l l l IBS cardinal symptoms description: pain, derangement of …. digestion, and flatulence l Powell R. Med Trans Royal Coll Phys 1818; 6: 106 -17. The bowels are at one time constipated and at another lax in the same person-----how the disease has two such different symptoms I do not propose to explain l Cumming W. London Med Gazette 1849; NS 9: 969 -73. Separated IBS from functional diarrhea, began with an enteric infection l Chaudhary NA, et al. Q J Med 1962; 31; 307 -22. Thompson WG. Gastroenterology 2006; 130: 1552 -6.

Lecture contents l FGID disease model l Visceral pain pathophysiology l Rome III classification l IBS knowledge l Represented IBS reports in Taiwan

FGID, 2006 l Nonstructural symptoms l l From single biological etiology to integrated biopsychosocial model of illness/disease l l l Mind amenable to scientific study, playing role in illness Link of mind & body dysregulation illness AGA 704 member survey of FGID l l Enigmatic, less amenable to explain or effective treatment Problems of living: physiological, intrapsychiatric, and sociocultural impacts on daily life activities There is no evidence of an inflammatory, anatomic, metabolic or neoplastic process that explains the patient’s symptoms No known structural: 81% Stress disorder: 57% practitioners, 34% academicians/ trainees Motility disorders: 43% practitioners, 26% academicians/ trainees Physicians deny FGID existence or unneeded studies Drossman DA. Gastroenterology 2006; 130: 1377 -90.
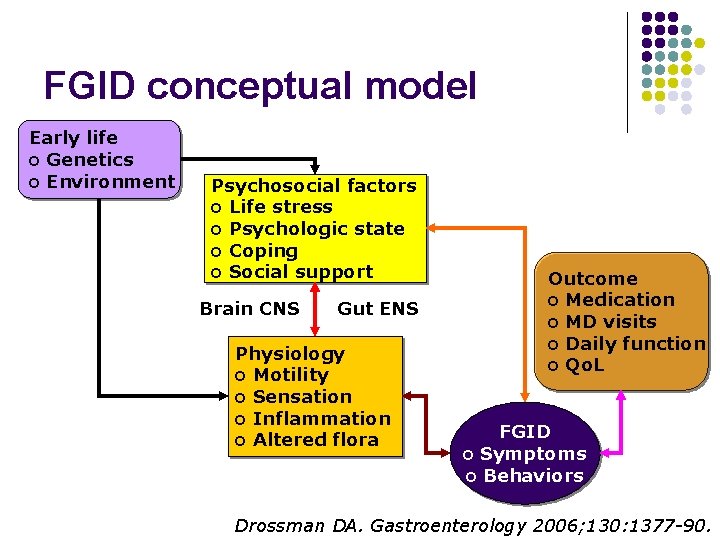
FGID conceptual model Early life o Genetics o Environment Psychosocial factors o Life stress o Psychologic state o Coping o Social support Brain CNS Gut ENS Physiology o Motility o Sensation o Inflammation o Altered flora Outcome o Medication o MD visits o Daily function o Qo. L FGID o Symptoms o Behaviors Drossman DA. Gastroenterology 2006; 130: 1377 -90.
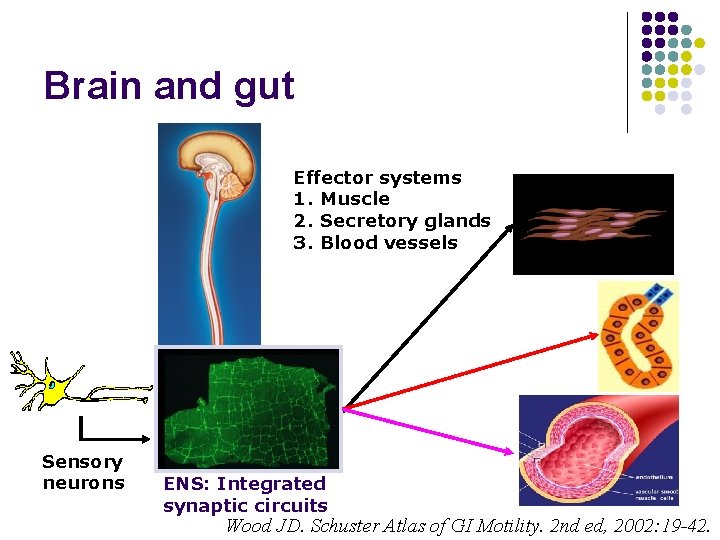
Brain and gut Effector systems 1. Muscle 2. Secretory glands 3. Blood vessels Sensory neurons ENS: Integrated synaptic circuits Wood JD. Schuster Atlas of GI Motility. 2 nd ed, 2002: 19 -42.
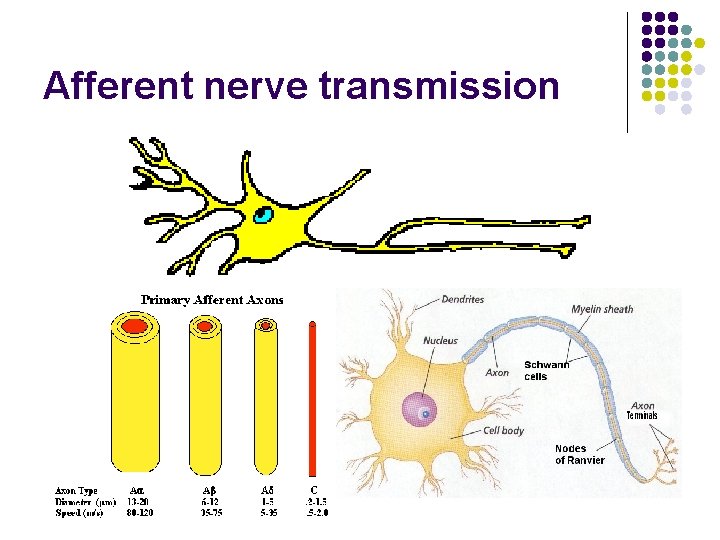
Afferent nerve transmission
Classic afferent pain pathway l First order: viscera to spinal cord l Pass through autonomic nerve plexus (nerve web to major artery supply) l Run within regional splanchnic nerves l l l Vagal afferents: mainly autonomic functions, but also with pain conduction Sympathetic chain (thoraco-lumbar) Enter spinal cord white ramus, synapsed in dorsal horn (laminae I, II, V) 1 st order neuron body: dorsal root ganglia Second order: spinal cord to brain stem Third order: brain stem to higher levels of cortex Michael D, et al. Schuster Atlas of GI Motility. 2 nd ed, 2002: 43 -55.

Classic afferent pain pathway (2) l Second order: spinal cord to brain stem l l Postsynaptic neurons: superficial laminae of dorsal horn cross to contralateral side cephalad within ventrolateral quadrant of spinal cord (tracts) synapse within thalamic and reticular formation nuclei of pons and medulla Spinothalamic tract Spinoreticular tract Third order: brain stem to higher levels of cortex l l l Widely distributed in brain Spinothalamic tract: somatosensory cortex for pain perception, quality and localization Spinoreticular tract: limbic system, frontal cortex, motivationaffective pain perception (unpleasant) Michael D, et al. Schuster Atlas of GI Motility. 2 nd ed, 2002: 43 -55.
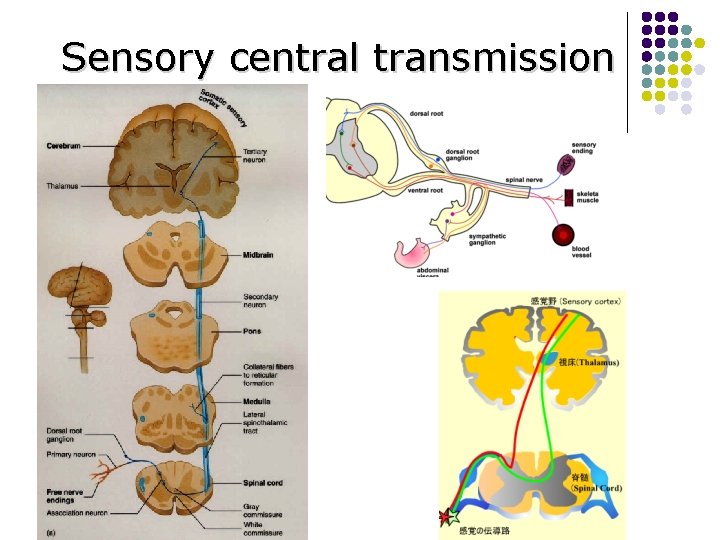
Sensory central transmission
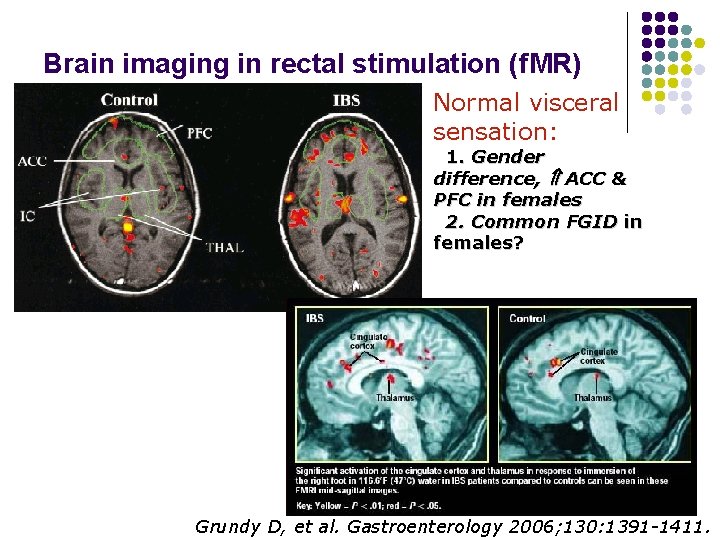
Brain imaging in rectal stimulation (f. MR) Normal visceral sensation: 1. Gender difference, ACC & PFC in females 2. Common FGID in females? Grundy D, et al. Gastroenterology 2006; 130: 1391 -1411.

Psychological factors l Strong emotion, stress: motility l l Modulators of experience, behavior, clinical outcomes l l motor response to stressors, partially correlated with symptoms Not necessary to diagnose FGID Evidence l l l Stress GI symptoms Modifying experience, behaviors & seeking care of illness FGID with psychosocial consequences on general wellbeing, daily function status, sense, future functioning at work or at home Drossman DA. Gastroenterology 2006; 130: 1377 -90.

History of the Rome diagnostic criteria 1978: the Manning criteria for IBS 1984: the Kruis criteria for IBS 1989: the Rome guidelines for IBS 1990: the Rome classification system for FGIDs (Rome-1) 1992: the Rome criteria for IBS and the FGIDs (1994) 1999: the Rome II criteria for IBS and the FGIDs 2006: the Rome III criteria Thompson WG. Gastroenterology 2006; 130: 1552 -6.

Rome III l Rome board l l 2002, London: 7 -member coordinating committee Validation, promotion of evidence l l Encouraging “developing world” participation l l l Gender, society, patient, social issues China, Brazil, Chile, Venezuela, Hungary, Romania 87 participants from 18 countries in 14 committees, Nov/Dec 2004: culminated meeting in Rome Prepared drafts, published and reported: May 2006 Preliminary discussion for Rome IV Thompson WG. Gastroenterology 2006; 130: 1552 -6.

Rome III classification of FGIDs l 28 adults, 17 pediatric l l l 6 domains in adults l l l Symptom-based, motor/sensory/CNS relationship Symptoms may be overlapped Esophageal, gastroduodenal, bowel, functional abdominal pain syndrome (FAPS), biliary, anorectal Bowel: IBS, FD, FC, functional bloating Pediatric; age category l Neonate/toddler, child/adolescent Drossman DA. Gastroenterology 2006; 130: 1377 -90.

FGID (bowel & pain) l Functional bowel disorders l l l C 1: IBS C 2: Functional bloating C 3: Functional constipation C 4: Functional diarrhea C 5: Unspecified functional bowel disorder D: Functional abdominal pain syndrome Drossman DA. Gastroenterology 2006; 130: 1377 -90.

Irritable bowel syndrome (IBS) l IBS is a functional bowel disorder in which abdominal pain or discomfort is associated with defecation or a change in bowel habit, and with features of disordered defecation l l l 10 -20% adults in world, female predominant Come and go over time, overlap with other FGID Poor Qo. L, high heath care costs Longstreth GF, et al. Gastroenterology 2006; 130: 1480 -91.

Diagnostic criteria for IBS, C 1 l Recurrent abdominal pain or discomfort at least 3 days per month in the last 3 months associated with 2 or more of the following: l l Improvement with defecation Onset associated with a change in frequency of stool Onset associated with a change in form (appearance) of stool Criteria fulfilled for the last 3 months with symptom onset at least 6 months prior to diagnosis l Discomfort: uncomfortable sensation not described as pain Longstreth GF, et al. Gastroenterology 2006; 130: 1480 -91.

Sub-typing IBS by predominant stool pattern l Subtype (absent use of antidiarrheals or laxatives) l l l IBS-C (IBS with constipation): hard or lumpy stools >25% and loose (mushy) or watery stools <25% of BMs IBS-D (IBS with diarrhea): loose (mushy) or watery stools >25% and hard or lumpy stool <25% of BMs IBS-M (mixed IBS): hard or lump stools >25% and loose (mushy) or watery stools > 25% of BMs IBS-U (unsubtyped IBS): insufficient abnormality of stool consistency to meet criteria for IBS-C, D, or M Stool form: Bristol scale Longstreth GF, et al. Gastroenterology 2006; 130: 1480 -91.
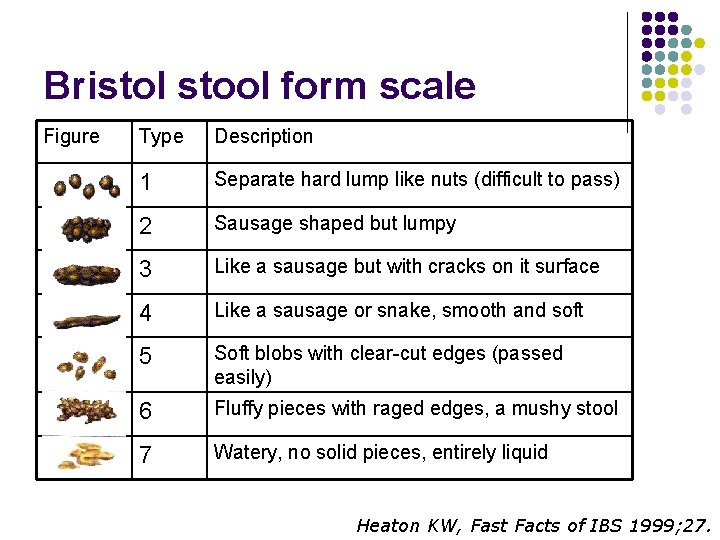

Bristol stool form scale Figure Type Description 1 Separate hard lump like nuts (difficult to pass) 2 Sausage shaped but lumpy 3 Like a sausage but with cracks on it surface 4 Like a sausage or snake, smooth and soft 5 Soft blobs with clear-cut edges (passed easily) 6 Fluffy pieces with raged edges, a mushy stool 7 Watery, no solid pieces, entirely liquid Heaton KW, Fast Facts of IBS 1999; 27.
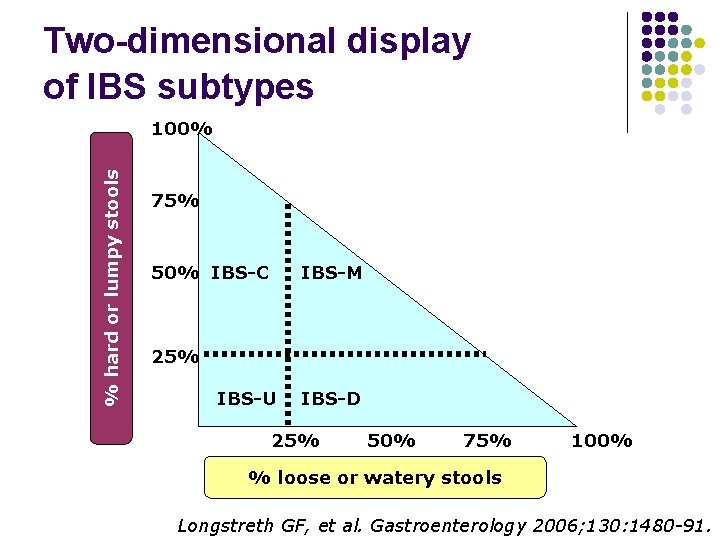
Two-dimensional display of IBS subtypes % hard or lumpy stools 100% 75% 50% IBS-C IBS-M 25% IBS-U IBS-D 25% 50% 75% 100% % loose or watery stools Longstreth GF, et al. Gastroenterology 2006; 130: 1480 -91.

IBS clinical manifestations l Abdominal pain l l l Others l l l l Bloating, distension, mucus, urgency, incomplete defecation Changed frequency and consistency of BM No unique etiology to explain clinical disorders l l Generalized or lower abdomen Relieved by defecation, strongly associated with stress Motor, sensory disorders Local inflammation Central, peripheral mechanisms Psychological No universally effective therapy Symptom based therapy: subgroups of IBS Bueno L. Curr Opin Pharmacol 2005; 5: 583 -8.
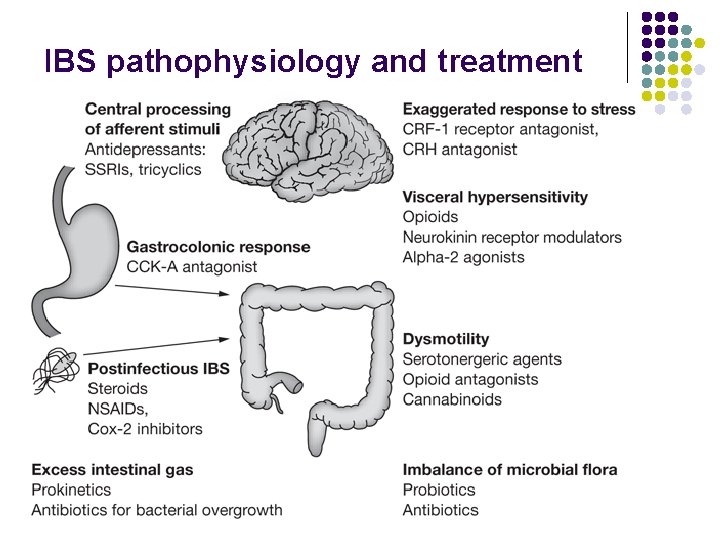
IBS pathophysiology and treatment

Extra-colonic symptoms in IBS l l More physician visits: X 3 Undergoing more abdominal/GYN surgeries l l GU/GYN dysfunctions l l Dysmenorrhea, dyspareunia, impotence, urinary frequency, nocturia, incomplete bladder emptying Fibromylagia: 2/3 reported rheuma sx l l l More chronic pelvic pain Associated with IBS severity 63% chronic fatigue with IBS Others: headaches, back pain, HCVD? PU? Skin rash, insomnia, palpitation, loss of concentration, unpleasant taste Hasler WL, et al. Yamada T, Textbook of Gastroenterol 4 th ed, 2003: 1817 -42.
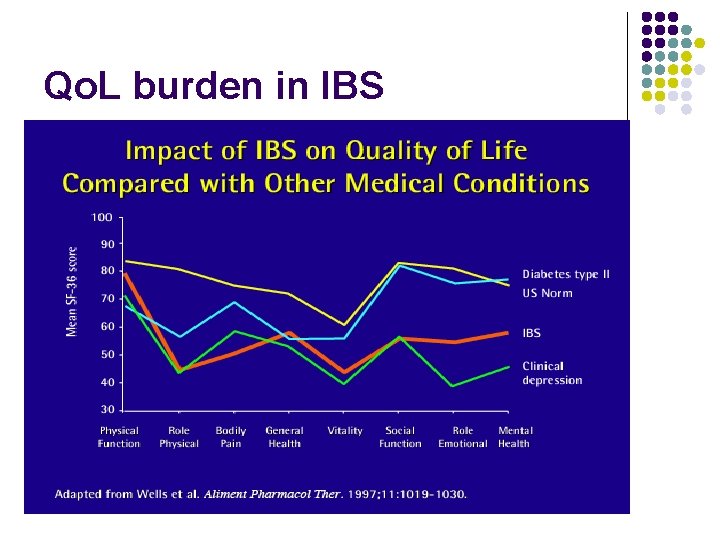
Qo. L burden in IBS

IBS social cost, USA (1998)

Alarm symptoms in IBS diagnosis l l l l l Age of onset over 50 yrs Progressive or very severe non-fluctuating symptoms Nocturnal symptoms waking from sleep Persisted diarrhea, recurrent vomiting Rectal bleeding, anemia Unexplained BW loss Family history of colon cancer Fever Abnormal physical examinations Talley NJ, et al. Lancet 2002; 360: 555 -564.

Natural history of IBS l l l l A safe diagnosis Chronic disorder with extremely variable Fluctuated symptoms Stable prevalence in community over 12 -20 months Repeated investigations: reinforce illness behavior Considering alarming factors No to other organic disorders Camilleri M. Management of the IBS. Gastroenterology 2001; 120: 652 -68.

IBS treatment l Positive clinical diagnosis l l Reassurance, explanation, advice precipitating factors Targeting on major symptoms Follow up in treatment response l l l Good doctor-patient relationship visits Subgroup based treatment on bowel habit Unsatisfactory in medicine l l l Exclude other organic disorders Poorly understood High placebo effect: 30%~80% in short-term trials and with time Targeting new receptors Talley NJ. Lancet 2001; 358: 2061 -8.
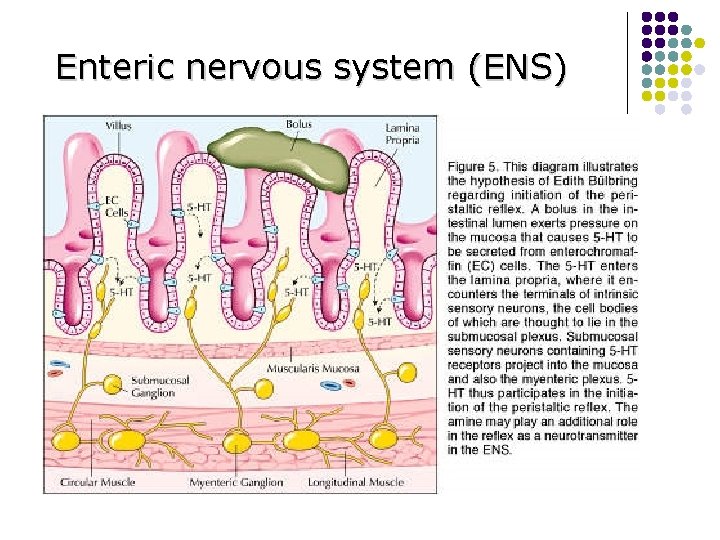
Enteric nervous system (ENS)
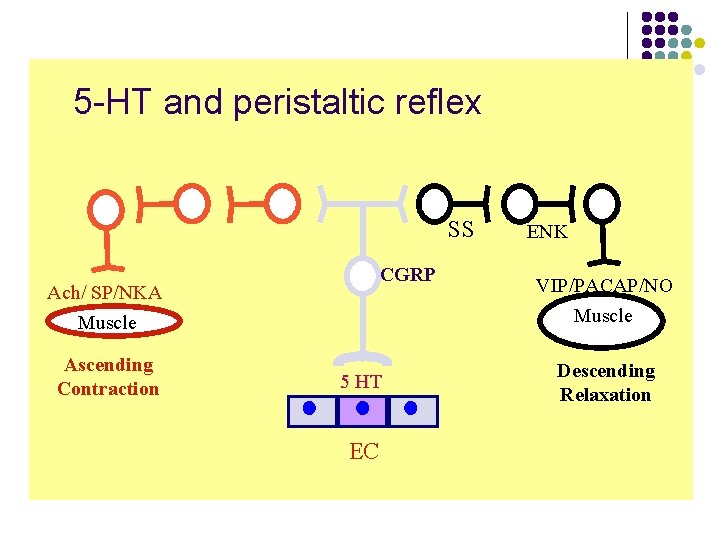
5 -HT and peristaltic reflex SS CGRP Ach/ SP/NKA Muscle Ascending Contraction 5 HT ENK VIP/PACAP/NO Muscle Descending Relaxation EC Yamada T: Textbook of Gastroenterology 3 rd ed, 1999: 100

Tegaserod treatment l l Partial 5 -HT 4 agonist (also blocking 5 -HT 2 B) Approved, female C-IBS (2004 review) l l overall symptoms, BM no BM days No effect: abdomen pain/discomfort Potential indications: GE, stomach compliance l l UGI: dyspepsia, gastroparesis Intestinal pseudo-obstruction? Galligan JJ, et al. Neurogastroenterol Motil 2005; 17: 643 -653.
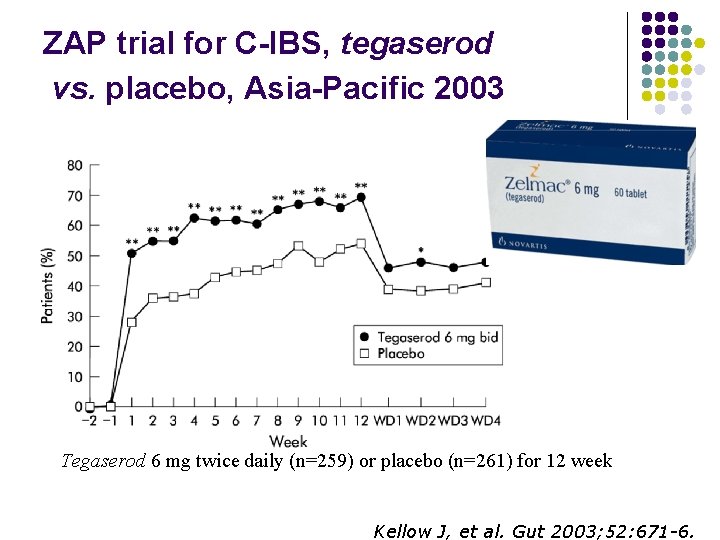
ZAP trial for C-IBS, tegaserod vs. placebo, Asia-Pacific 2003 Tegaserod 6 mg twice daily (n=259) or placebo (n=261) for 12 week Kellow J, et al. Gut 2003; 52: 671 -6.

Alternative therapies l l l Replaced colon flora: in controlled trial, efficacy, safety? Local action of antibiotics: effect in some, need rigorous test Probiotics: flatulence in IBS Peppermint oil: no convincing data Chinese herb drug: significant in a trial l l Mixture, true action? Need other trials to confirm Acupuncture: uncertain benefit Talley NJ. Am J Gastroenterol 2003; 98: 750 -8.

Alternative therapy for IBS Hussain Z, et al. APT 2006: 23: 465 -71.

VS IBS in females

IBS characters in Asian large scale studies l IBS in Japan (Kumano H. Am J Gastroenterol 2004; 99: 370 -6) l 4000 (M: 50%) subjects, national wide random questionnaire Rome II: 6. 1% Highly associated morbidity, agoraphobia l M/F: 4. 5%/7. 8%, p<0. 001 Female: higher morbidity No different in consulters or non-consulters IBS in Southern China (Xiong LS, et al. Aliment Pharmacol Ther 2004; 19: 1217 -1224) l 4178 (M: 45. 6%), face to face interview, random cluster sampling Guangzhou Manning: 11. 5%; Rome II: 5. 7% Female predominance: Manning (1: 1. 34), Rome II (1: 1. 25) Risk factors: NSAID using, food allergy, psychological distress, life event stress, dysentery, negative copying style, health related Qo. L
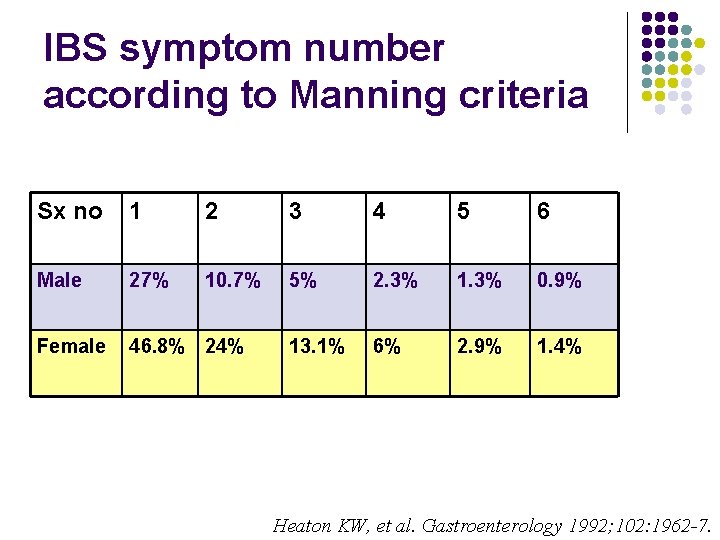
IBS symptom number according to Manning criteria Sx no 1 2 3 4 5 6 Male 27% 10. 7% 5% 2. 3% 1. 3% 0. 9% Female 46. 8% 24% 13. 1% 6% 2. 9% 1. 4% Heaton KW, et al. Gastroenterology 1992; 102: 1962 -7.

Gender factor on IBS symptoms, Taiwan 2005 BM type Male, n=266 Female, n=181 P value <3/wk 5. 6% 14. 9% 0. 001 >3/day 31. 6% 17. 7% 0. 001 Hard, lump 8. 6% 18. 8% 0. 002 Loose, mush 44. 4% 29. 8% 0. 002 Social impact GI consultation 56% 54. 1% NS Absenteeism 20. 7% 32. 6% 0. 006 Total days/yr 0. 7± 3. 1 2. 3± 6. 4 0. 01 Sleep disturbance 35. 3% 50. 3% 0. 002 Lu CL, et al. Aliment Pharmacol Ther 2005; 21: 1497 -505.
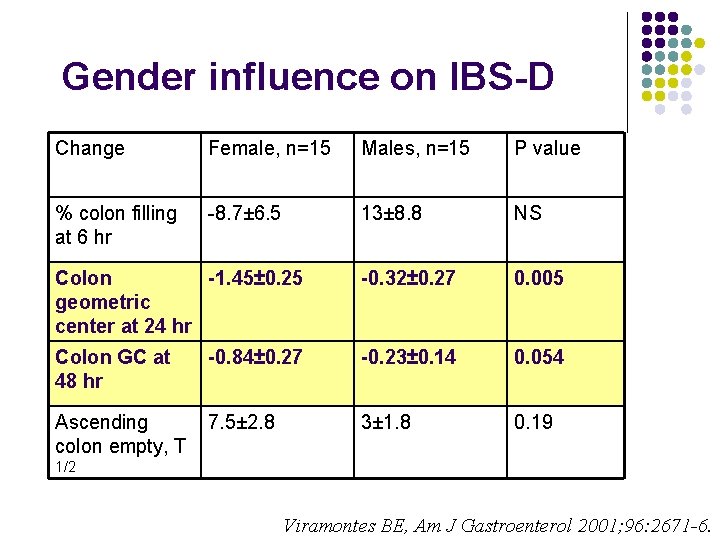
Gender influence on IBS-D Change Female, n=15 Males, n=15 P value % colon filling at 6 hr -8. 7± 6. 5 13± 8. 8 NS Colon -1. 45± 0. 25 geometric center at 24 hr -0. 32± 0. 27 0. 005 Colon GC at 48 hr -0. 84± 0. 27 -0. 23± 0. 14 0. 054 Ascending colon empty, T 7. 5± 2. 8 3± 1. 8 0. 19 1/2 Viramontes BE, Am J Gastroenterol 2001; 96: 2671 -6.
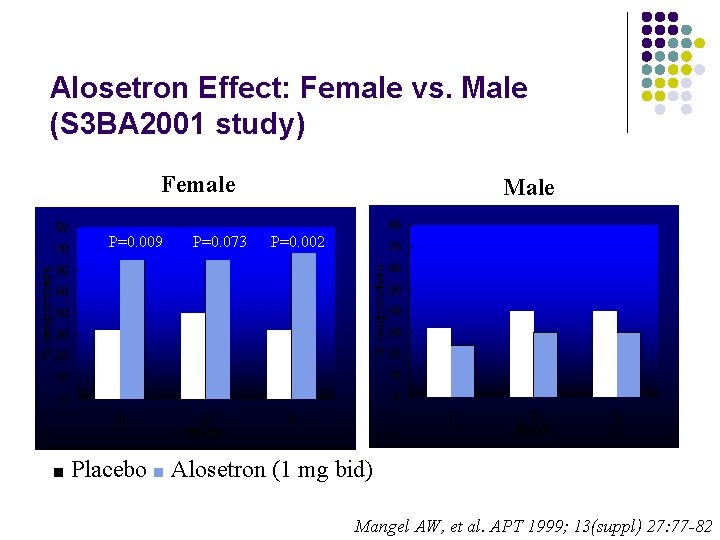
Alosetron Effect: Female vs. Male (S 3 BA 2001 study) Female P=0. 009 ■ P=0. 073 Male P=0. 002 ** * Placebo ■ Alosetron (1 mg bid) Mangel AW, et al. APT 1999; 13(suppl) 27: 77 -82

Sex hormones or gender impacts on brain-gut axis l Animals l l Drugs: estrogen/progesteron on P-450 system l l Low threshold for visceromotor response in rat proestrus vs estrus phase potency of opiates to visceromotor response in male rats Modulation of response in afferent neurons of male GP CYP 3 A 4: women clearing drugs quickly Humans l l Slow GE in women Women experience greater pain to most stimuli Different areas of brain activation: males vs females Different polymorphism of 5 -HT transporter promoter: males vs females Ouyang A, et al. Am J Gastroenterol 2006; 101: S 602 -9.

Clinical differences of IBS: males vs females l l l Motility: no confirmed data Autonomic system: sympathetic/ vagal activity to colorectal distension in men Afferent sensory pathways: threshold to rectal distension in women IBS Female: easily developing PI-IBS Psychological status: depression, anxiety, somatization in women Drug response: efficacy of 5 -HT 3 antagonists, 5 HT 4 agonists Ouyang A, et al. Am J Gastroenterol 2006; 101: S 602 -9.
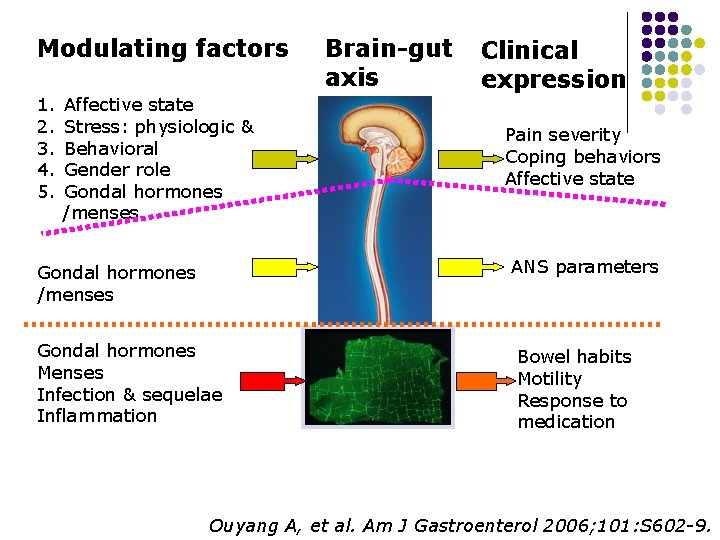
Modulating factors 1. 2. 3. 4. 5. Affective state Stress: physiologic & Behavioral Gender role Gondal hormones /menses Brain-gut axis Clinical expression Pain severity Coping behaviors Affective state ANS parameters Gondal hormones /menses Gondal hormones Menses Infection & sequelae Inflammation Bowel habits Motility Response to medication Ouyang A, et al. Am J Gastroenterol 2006; 101: S 602 -9.

IBS in Taiwan, 2003 l l 2, 018 (M: 60. 2%), paid physical check up, selfadministered questionnaire Prevalence: l l Rome II: 22. 1% Rome I: 17. 5% ( =0. 73) No gender difference but younger, decreasing with age IBS subjects l l l Absenteeism, physician visits (GI, non-GI) More chance with cholecystectomy l not with appendectomy / hysterectomy Sleep disturbance Lu CL, et al. Aliment Pharmacol Ther 2003; 18: 1159 -69.
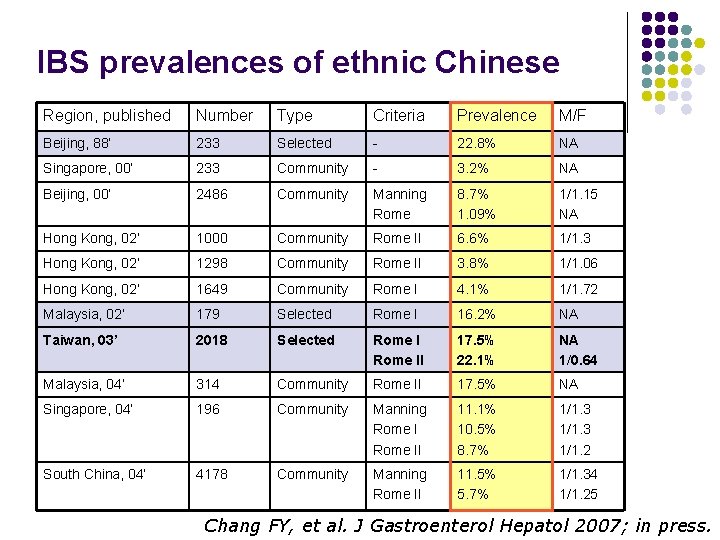
IBS prevalences of ethnic Chinese Region, published Number Type Criteria Prevalence M/F Beijing, 88’ 233 Selected - 22. 8% NA Singapore, 00’ 233 Community - 3. 2% NA Beijing, 00’ 2486 Community Manning Rome 8. 7% 1. 09% 1/1. 15 NA Hong Kong, 02’ 1000 Community Rome II 6. 6% 1/1. 3 Hong Kong, 02’ 1298 Community Rome II 3. 8% 1/1. 06 Hong Kong, 02’ 1649 Community Rome I 4. 1% 1/1. 72 Malaysia, 02’ 179 Selected Rome I 16. 2% NA Taiwan, 03’ 2018 Selected Rome II 17. 5% 22. 1% NA 1/0. 64 Malaysia, 04’ 314 Community Rome II 17. 5% NA Singapore, 04’ 196 Community Manning Rome II 11. 1% 10. 5% 8. 7% 1/1. 3 1/1. 2 South China, 04’ 4178 Community Manning Rome II 11. 5% 5. 7% 1/1. 34 1/1. 25 Chang FY, et al. J Gastroenterol Hepatol 2007; in press.

IBS is an independent factor in predicting negative-appendectomy 430 patients with emergent appendectomy 68 (15. 8%): negative exploration, 2003 -05 Adjusted Odds Ratio 95% Confidence interval p value Rome-II IBS 2. 17 1. 14 – 4. 24 0. 02 Degree of Anxiety 1. 12 1. 02 – 1. 49 0. 04 Absence of migrating pain 3. 43 1. 90 – 5. 95 <0. 001 Absence of muscle guarding 3. 72 2. 07 – 6. 70 <0. 001 PMNC (<75%) 3. 05 1. 69 – 5. 51 <0. 001 No use of CT scan 2. 32 1. 27 – 4. 26 <0. 01 Lu CL, et al. Gut 2007; in press.
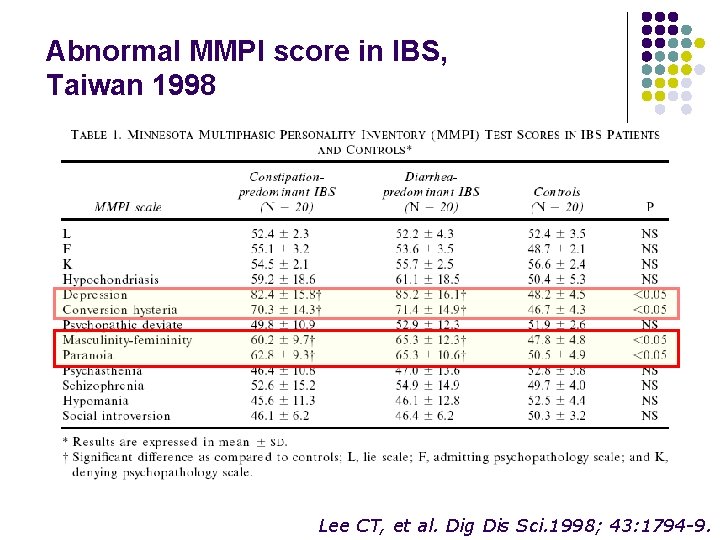
Abnormal MMPI score in IBS, Taiwan 1998 Lee CT, et al. Dig Dis Sci. 1998; 43: 1794 -9.
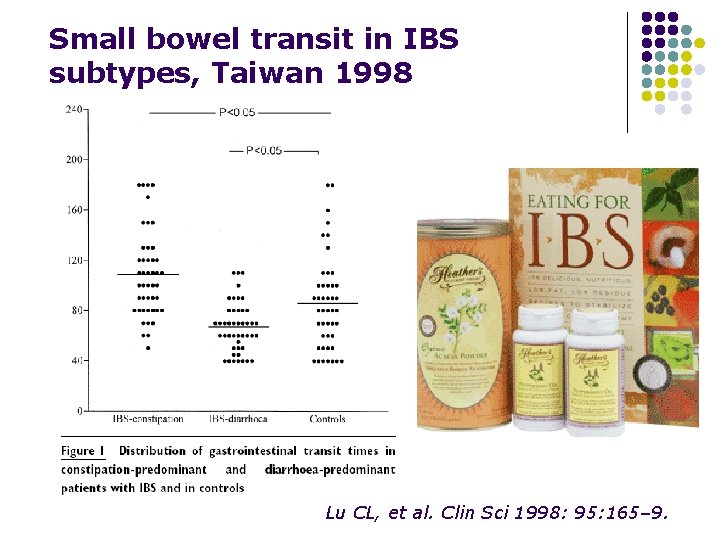
Small bowel transit in IBS subtypes, Taiwan 1998 Lu CL, et al. Clin Sci 1998: 95: 165– 9.
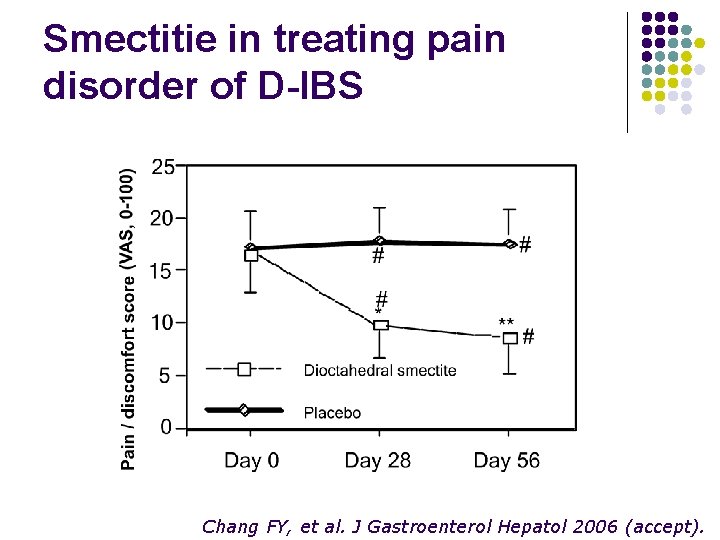
Smectitie in treating pain disorder of D-IBS Chang FY, et al. J Gastroenterol Hepatol 2006 (accept).

Nurses’ knowledge in caring IBS patients, Taiwan 2001 l 120 RN in a tertiary acute care facility, 46 -item questionnaire, filled voluntarily l l l Categories: demography, IBS information source, nurses’ IBS knowledge, perception, beliefs, learning requirement 92. 5%: agree or strongly agree having limited IBS knowledge 53. 3%: cannot explain IBS well to patients 10. 8%: able to recognize IBS symptoms Little specific IBS knowledge of Taiwan nurses Chen H, et al. Nur Health Sci 2001; 3: 173 -7.

Conclusions l l FGID has been a problem of living, it means biopsychosocial disorder Current Rome III clearly addresses IBS and its subtypes IBS treatments based on main symptoms Gender effect on IBS manifestations but no recommended different treatments
- Slides: 57