RISPACS Descriptors and Coding Dr Keith Foord Consultant




















- Slides: 29

RIS-PACS Descriptors and Coding Dr Keith Foord Consultant Radiologist, East Sussex Hospitals

A national system of RIS coding and descriptors ? Why? Must be as intuitive and easy to use as possible Should have national acceptance q q q q Relates to needs of request/entry systems within NCRS – pre. RIS - SNOMED match to record request to Spine Consistency and uniqueness in requesting terminology – pre. RIS and within RIS Consistency in activity measurement - RIS Consistency in clinical coding of events – RIS - SNOMED match For accurate communication of results data between hospitals – post RIS results reporting, cluster stores and national spine - SNOMED match to ‘performed examination code’ to Spine For ‘Payment by results’ – accurate records of same patient activity – national tariffs - SNOMED match / accurate HRGs DICOM Structured Reporting

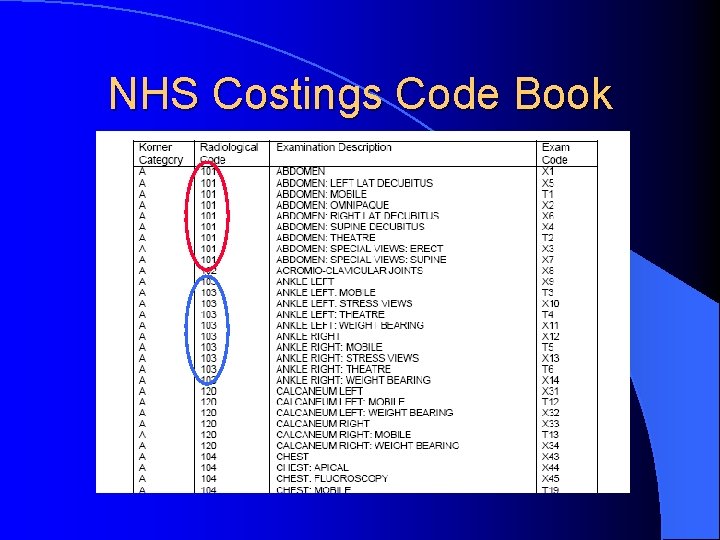
NHS Costings Code Book

Descriptors need to be UNIQUE in NCRS FOOT LEFT not unique When a user searches all of the examinations available for ‘Foot Left’ the search may return: FOOT LEFT, FOOT LEFT Swab, FOOT LEFT Physiotherapy, FOOT LEFT Dressing, etc. But XR FOOT LEFT is unique

Radiology Short Codes Used in RIS as shortcuts For bookings For internal communications within Radiology To help group procedures For internal management / audit / activity For common use need a structure, ideally short (max. 6 letters/digits) and logical

Radiological Short Codes 1 2 3 4 5 6 Modality X – X-ray Three or four letter body part F – Fluoro / function code I – Interventional/ Fluoro C – CT 4 th letter reserved M – MRI for R, L, B or W U – U’sound N – Radionuclide if procedure R or L lateralisable, Imaging Both or Whole body, P – PET otherwise can be used for any E- Endoscopy letter or number Z- Image analysis or review Postqualifier (Extra or subdescriptor)

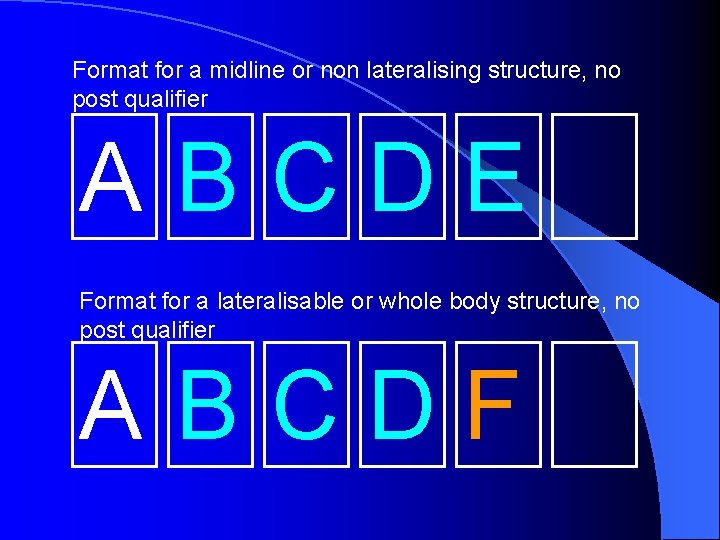
Format for a midline or non lateralising structure, no post qualifier ABCDE Format for a lateralisable or whole body structure, no post qualifier ABCDF

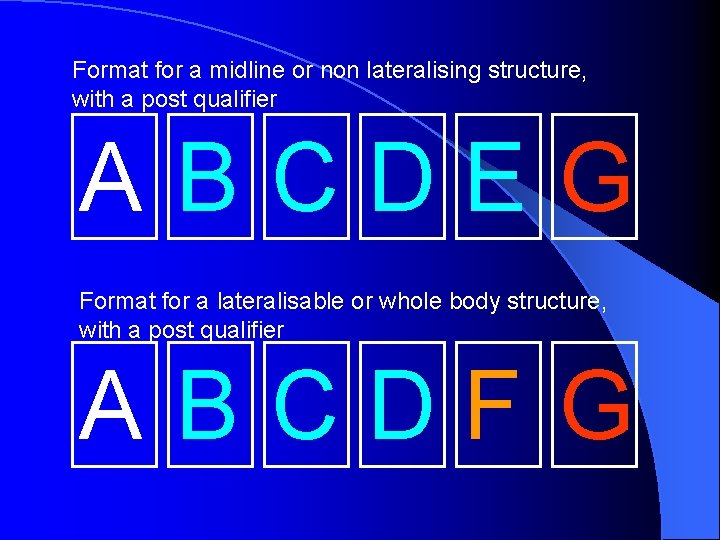
Format for a midline or non lateralising structure, with a post qualifier ABCDEG Format for a lateralisable or whole body structure, with a post qualifier ABCDF G

Extra qualifiers (6 th letter/number = G) q A B D E I J q M q O q P R S T X q q q q q 1 q 2 q 3 q 4 q Ablation Biopsy (Core or FNA) Drainage or Aspiration of fluid Embolisation Insertion of device in. Jection - as an objective of the procedure, not as part of the preliminary to this objective Mobile - for any modality, but particularly for 'portable' plain films and use of mobile image intensifiers t. Omography in its wider sense. O may be added to any plain film examination to define planar tomography - or postcoordinated Plasty - as in angio. Plasty or dacrocysto. Plasty - ie balloon dilatation for Radiotherapy planning Stent Use of intra. Thecal contrast e. Xtraction - eg in retrieval of intravascular foreign bodies or removal of temporary IVC filter First part of study Second part of study Third part of study Fourth visit etc. – 5, 6, 7, 8, 9 – 10 th = 0

Eg CT guided PELVic Biopsy CPEL VB Eg Interventional (Fluoroscopic) Right SFA Angioplasty I ASF RP

Pre and Post Co-ordination (1) In order to group procedures many old RIS systems lack the ability to post co-ordinate procedures together under one accession number. l Particular examples are for 'both' plain film exams eg 'both ankles' and in CT where examinations often combine e. g. CT Chest, Abdomen, Pelvis. l Pre co-ordination or grouping of these procedures is therefore required in advance. l Pre co-ordination should not be used in RIS-PACS systems capable of full post co-ordination as within these individual procedure codes will be automatically or manually grouped prior to archiving and reporting l

Eg CT guided PELVic Biopsy CPEL VB This is pre-coordinated with the whole process described in the code

Pre and Post Co-ordination (2) l l l In modern RIS systems post co-ordination can be applied to group related procedures together. All RIS systems supplied via LSPs should do this. Some procedure codes such as 'U/S biopsy' by themselves do not define precisely what has happened although it would define the activity of “Performing a biopsy under ultrasound control and the consumables/activity associated with this. ” Such codes need post co-ordinating with the relevant body part to fully inform activity statistics Similarly separate CT body part examinations can be post co-ordinated together to enable the multiple examinations to be reported together as one report. The advantage is a more sophisticated approach to audit, activity measurement and stocktaking

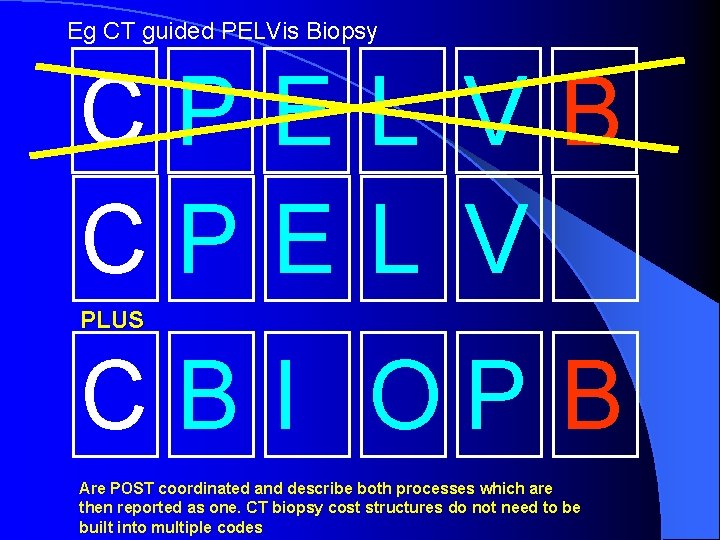
Eg CT guided PELVis Biopsy CPEL VB CPEL V PLUS CB I OP B Are POST coordinated and describe both processes which are then reported as one. CT biopsy cost structures do not need to be built into multiple codes

Eg PET/CT for Chest CCHES PLUS P GE NW Are POST coordinated and describe both processes which are then reported as one.

Requestable procedures Full list incl multis Post co-ord list

Unique codes for requestor, reporter, Trust, ward and unique ‘Accession numbers’ related to examination modality. Requestor and reporter NCRS National code related to GMC/GDC/SR no. or cross match to this via look up table. May not be a doctor. Trust 3 character NCRS codes eg RPX Ward 3 character prefix eg RPXBaird Accession No. 3 character prefix RPX 123456. Needed as same model machines might generate identical numbers and no process between manufacturers to coordinate these.


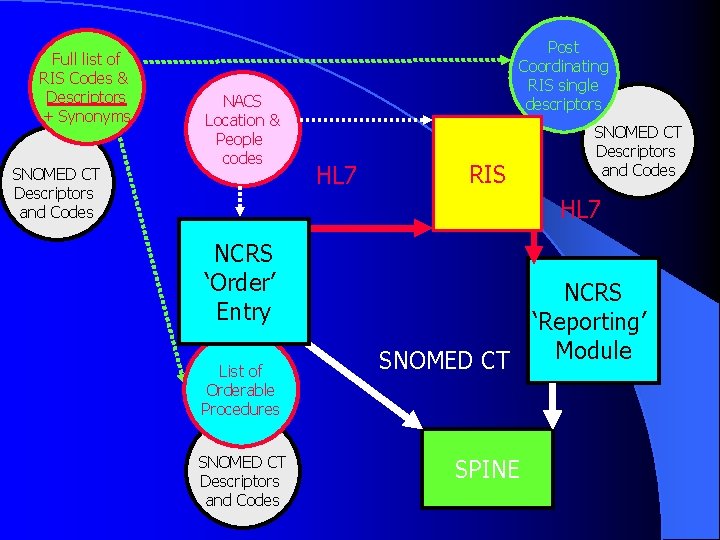
Full list of RIS Codes & Descriptors + Synonyms SNOMED CT Descriptors and Codes NACS Location & People codes Post Coordinating RIS single descriptors HL 7 RIS SNOMED CT Descriptors and Codes HL 7 NCRS ‘Order’ Entry List of Orderable Procedures SNOMED CT Descriptors and Codes NCRS ‘Reporting’ Module SNOMED CT SPINE

Sub-Descriptors / Codes l l l REQUESTING Layer (1 st order) Right Oblique QR Left Oblique QL Right Lateral LR Left Lateral LL Weight Bearing WB Standing ST Axial AX AP 20 o 20 Judet’s JU Stryker’s SY Etc… l l l l l IN RADIOLOGY (RIS) Layer (2 nd order) Same list + Supine SU Prone PR Decubitus DE Complex Oblique QC Angled Oblique 22, 30, 45 Frog laterals FR May need to combine together or with 1 st order list eg DELR

SNOMED CT NCRS provides support for clinical coding using the SNOMED CT nomenclature for diagnosis and procedure codes. SNOMED CT codes will be applied to the patients record through manual selection by users, as well as an integrated bi -product of clinical processes (i. e. orders, assessments). SNOMED CT clinical coding is supported for inpatient and outpatient encounters.

SNOMED CT At the end of an episode / encounter of care, SNOMED CT codes are recorded in NCRS via the Discharge Summary / Encounter diagnosis and procedure codes. The SNOMED codes recorded in NCRS are sent to the 3 M clinical encoder where clinical coding is completed in SNOMED CT, ICD 10, Read, and OPCS 4. Codes will be transferred back to NCRS and will update, not replace, the patient diagnosis and procedure codes. A full audit trail is available.

SNOMED CT Within NCRS P 1 R 2, users will have the ability to manually record SNOMED CT codes within the following areas: § Discharge Summary / Encounter § Problems / Provisional Diagnoses Within NCRS P 1 R 2, SNOMED CT codes will be recorded against the patients record, as a by-product of clinical processes, in the following clinical areas: § Assessments § Findings / Flowsheets § Orders (viz. the code for the request) § Results (viz. the code for the procedure(s) performed, not the radiological diagnosis or report which will be transferred via HL 7 messaging)

Orders and Results in Radiology SNOMED CT Order codes can be derived from Order/Entry systems, but will be MUCH MORE ACCURATE if derived from the accepted and if required modified final RIS procedure entry with SNOMED CT matching. SNOMED CT Results codes from Radiology are a dilemma. This does not apply to ‘Procedure performed’ , but to a provisional radiological diagnosis which may be a list of differential diagnoses which could be entered by a reporter (ie manually). Unlikely to happen given pressures of work! The use of DICOM structured reporting may give the possibility of automatically constructing radiological diagnosis codes from the structured report

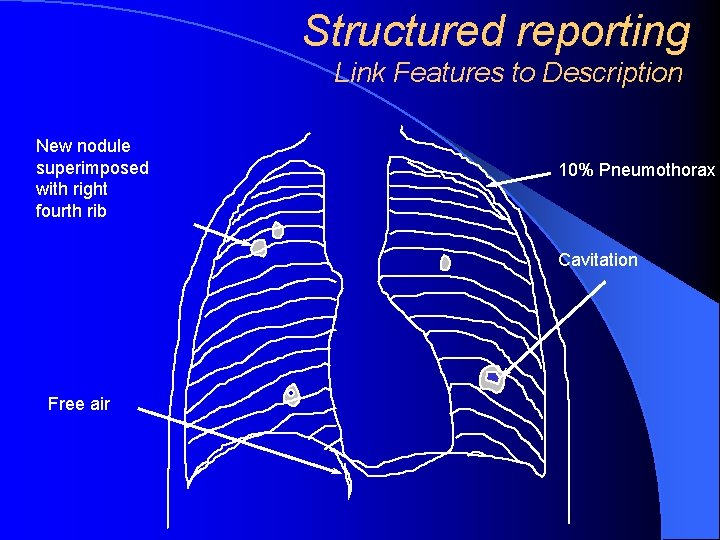
Structured reporting DICOM SR – is an ‘envelope’, but within this useful structure is available. User decides how much structure to use and controls with templates the type of content, if it is mandatory or optional and modes of expression Incorporated into the report are captured images of key findings (which can be exploded to full screen presentation), structured diagnosis information, recorded audio, the ability to sort findings by anatomy or priority, to view prior findings associated with the corresponding patient and hyperlinks to related information.

Structured reporting Link Features to Description New nodule superimposed with right fourth rib 10% Pneumothorax Cavitation Free air

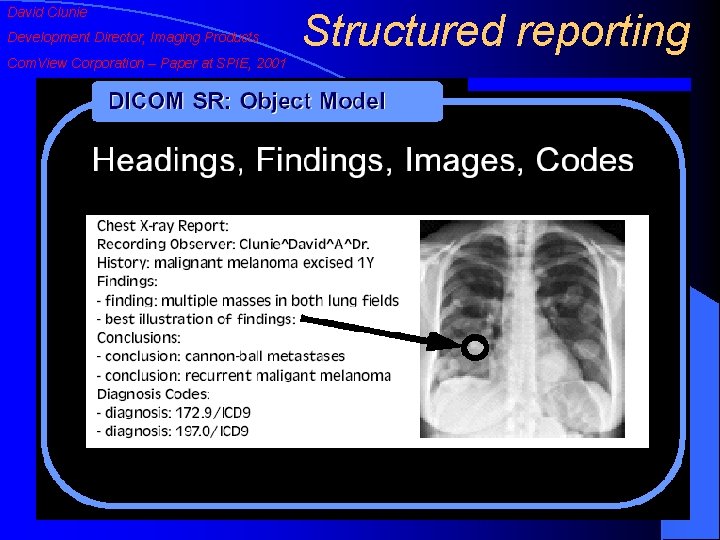
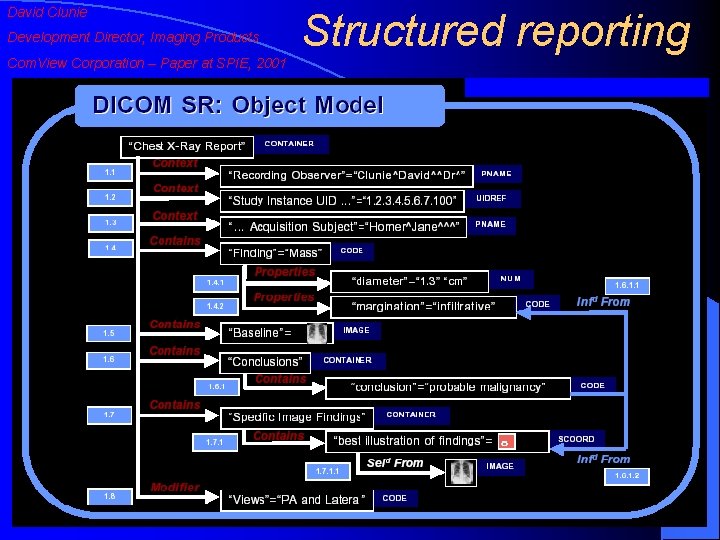
David Clunie Development Director, Imaging Products Com. View Corporation – Paper at SPIE, 2001 Structured reporting

David Clunie Development Director, Imaging Products Com. View Corporation – Paper at SPIE, 2001 Structured reporting
