Rickets Metabolic Bone Diseases Physiology Calcium Phosphate PTH

Rickets & Metabolic Bone Diseases

Physiology Calcium Phosphate PTH Vitamin D Calcitonin

Calcium > 99% in bone Muscle and nerve function Clotting mechanisms Free plasma Ca = Bound plasma Ca Active transport absorption in the duodenum and passive diffusion in the jejunum 98% reabsorption in the kidney

Calcium Requirement 600 mg/day in children 1300 mg/day in adolescents and young adults 750 mg/day in adults 1500 mg/day in pregnant women 2000 mg/day in lactating women 1500 mg/day in postmenopausal women and patients with fractures

Phosphate Key component of bone mineral Enzyme systems and molecular interactions 85% in bone Plasma Phosphate is mostly unbound 1000 -1500 mg/day
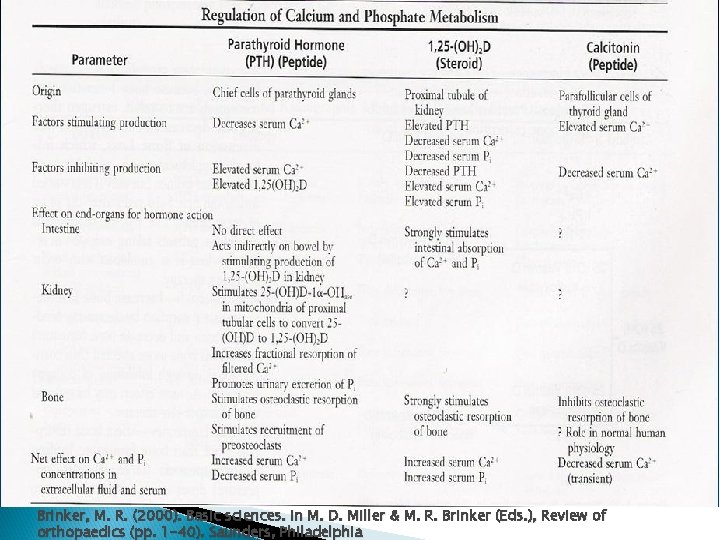

Brinker, M. R. (2000). Basic sciences. In M. D. Miller & M. R. Brinker (Eds. ), Review of orthopaedics (pp. 1 -40). Saunders, Philadelphia
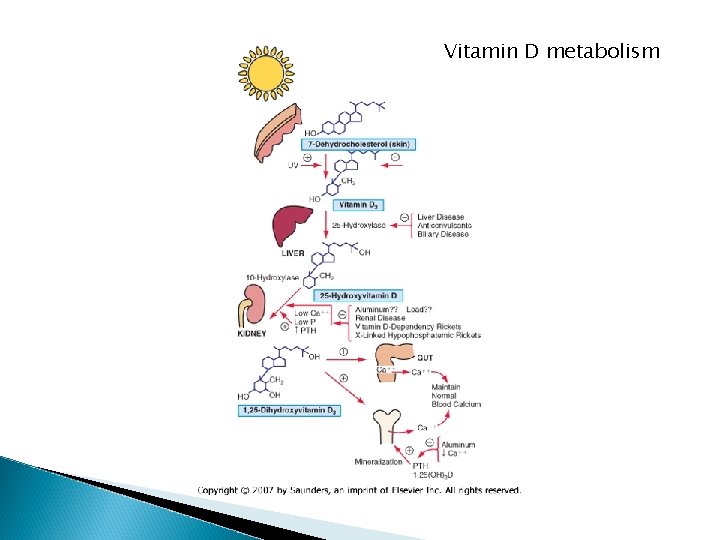
Vitamin D metabolism

Secondary role Other Hormones - Estrogen - Corticosteroids - Thyroxin Non-hormonal Factors - Mechanical stress - Prostaglandin E - Acid-base balance

Rickets

Introduction Normal bone growth & mineralization require adequate availability of calcium & phosphate. Deficient mineralization can result in rickets and/or osteomalacia. Rickets refers to the changes caused by deficient mineralization at the growth plate. Osteomalacia refers to impaired mineralization of the bone matrix. Rickets & osteomalacia usually occur together as long as the growth plates are open; only osteomalacia occurs after the growth plates have fused.

Causes of Rickets Vitamin D disorders ◦ Nutritional vitamin D deficiency; Congenital vitamin D deficiency; Secondary vitamin D deficiency; Malabsorption ; Increased degradation; Decreased liver 25 -hydroxylase; Vitamin D-dependent rickets type 1; Vitamin D-dependent rickets type 2; Chronic renal failure. Calcium deficiency ◦ Low intake, Calcium deficient Diet, Premature infants (rickets of prematurity), Malabsorption, Dietary inhibitors of calcium absorption Phosphorus deficiency ◦ Inadequate intake, Premature infants (rickets of prematurity), Aluminum-containing antacids

Causes of Rickets RENAL LOSSES ◦ X-linked hypophosphatemic rickets; Autosomal dominant hypophosphatemic rickets; Hereditary hypophosphatemic rickets with hypercalciuria; Overproduction of phosphatonin (Tumorinduced rickets, Mc. Cune-Albright syndrome, Epidermal nevus syndrome, Neurofibromatosis), Fanconi syndrome, Dent disease DISTAL RENAL TUBULAR ACIDOSIS

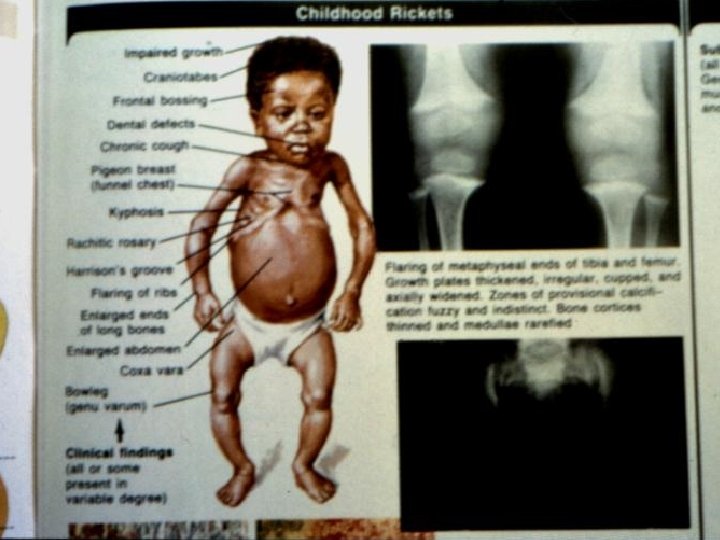
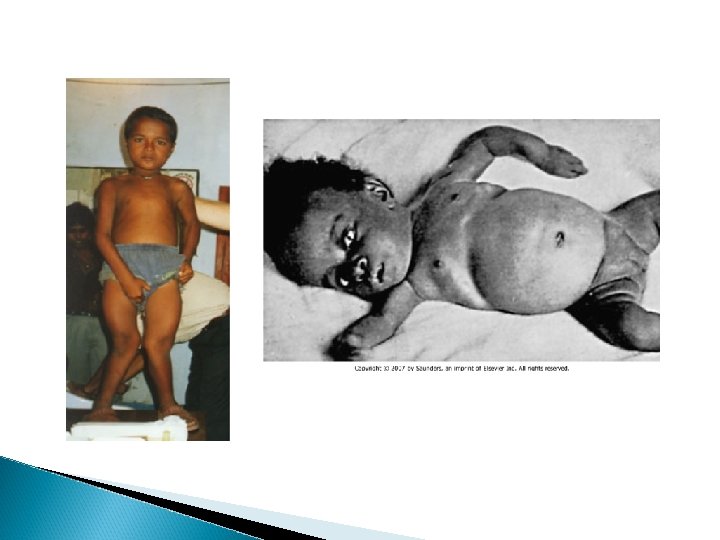
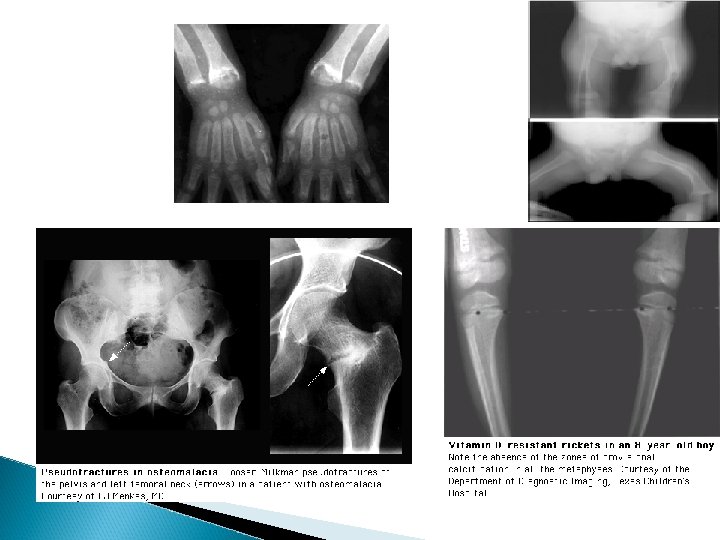
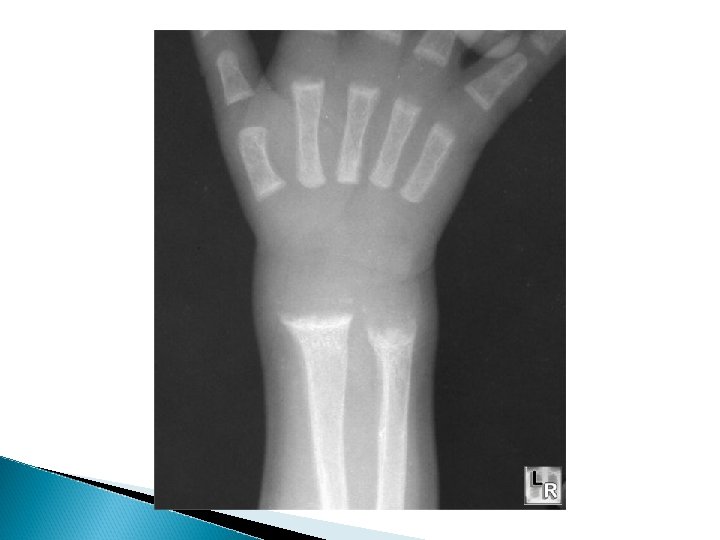
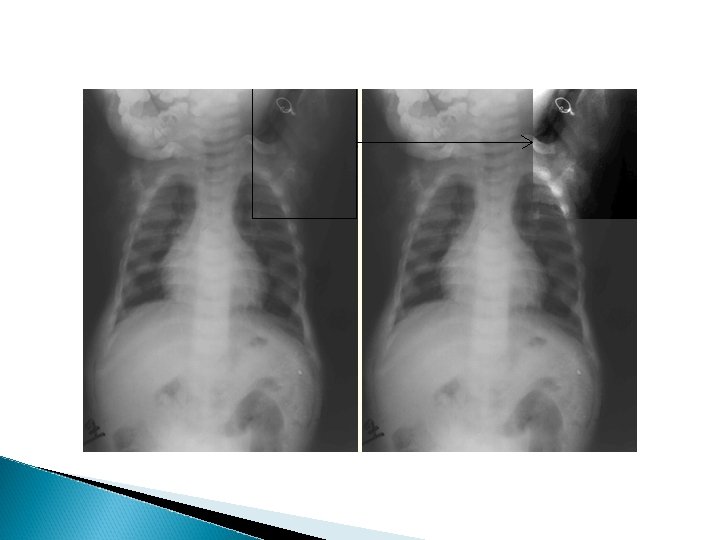
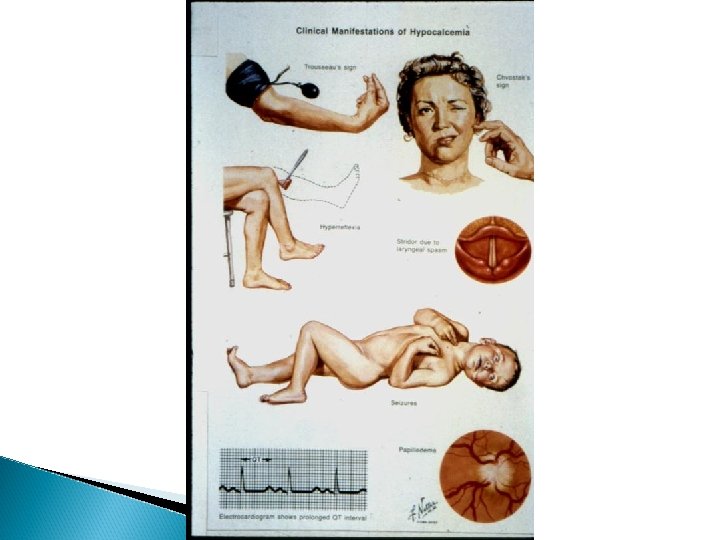
Clinical features of Rickets GENERAL Failure to thrive; Listlessness; Protuding abdomen; Muscle weakness (especially proximal); Fractures. HEAD Craniotabes; Frontal bossing; Delayed fontanelle closure; Delayed dentition; caries; Craniosynostosis CHEST Rachitic rosary; Harrison groove; Respiratory infections and atelectasis BACK Scoliosis , Kyphosis , Lordosis EXTREMITIES Enlargement of wrists and ankles; Valgus or varus deformities Windswept deformity (combination of valgus deformity of 1 leg with varus deformity of the other leg); Anterior bowing of the tibia and femur; Coxa vara; Leg pain. HYPOCALCEMIC SYMPTOMS Tetany ; Seizures; Stridor due to laryngeal spasm

Extra skeletal findings in Rickets Extraskeletal manifestation of rickets vary depending upon the mineral deficiency. Hypoplasia of the dental enamel is typical for hypocalcemic rickets, whereas abscesses of the teeth occur more often in phosphopenic rickets. Hypocalcemic seizures, decreased muscle tone leading to delayed motor milestones, recurrent infections, increased sweating.
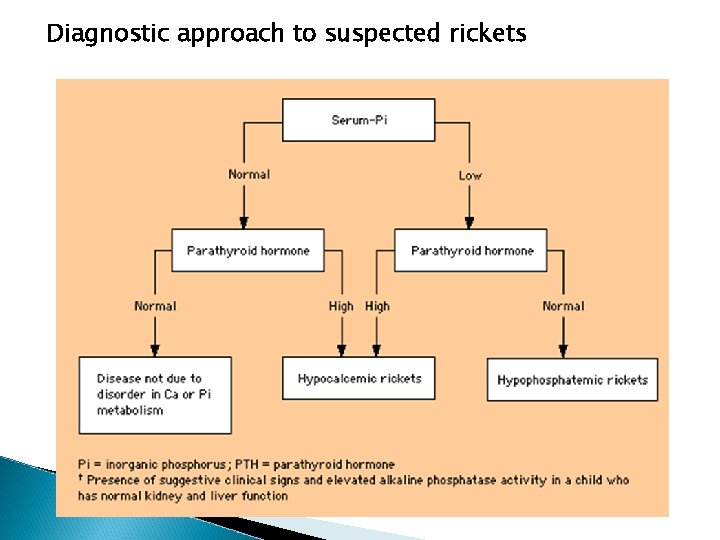
Diagnostic approach to suspected rickets
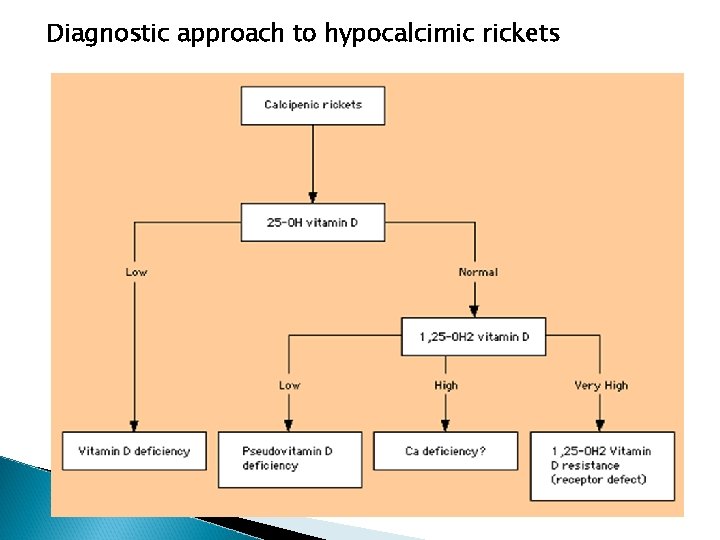
Diagnostic approach to hypocalcimic rickets
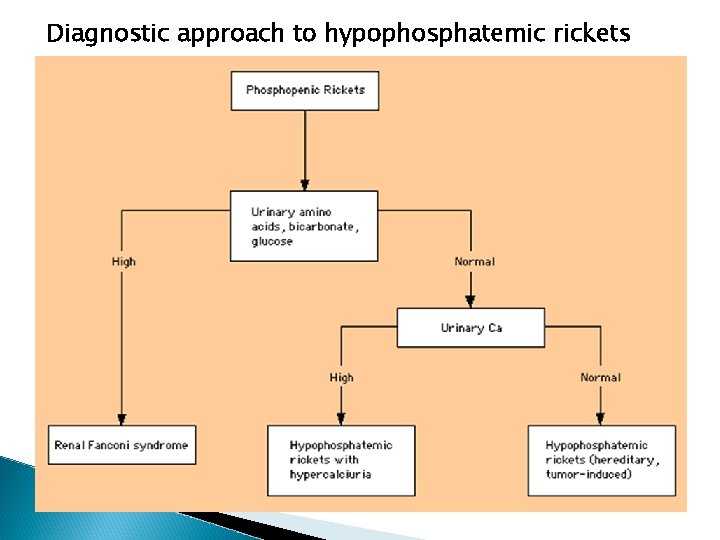
Diagnostic approach to hypophosphatemic rickets
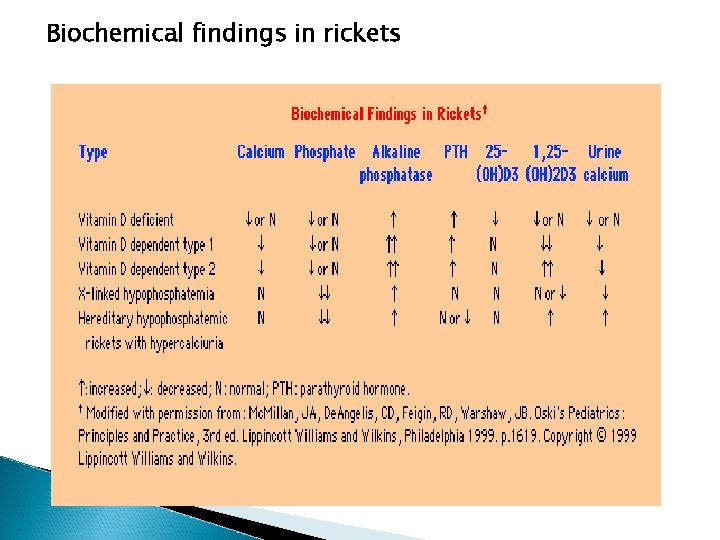
Biochemical findings in rickets

Biochemical findings in rickets Alkaline phosphatase usually is ↑in all forms of rickets. Serum phosphorus concentrations usually are↓ in both hypocalcemic and hypophosphatemic rickets. Serum Ca is ↓only in hypocalcemic rickets. Serum parathyroid hormone typically is ↑in hypocalcemic rickets, in contrast it is N in hypophosphatemic rickets. 25 -OH vitamin D reflect the amount of vitamin D stored in the body, and is ↓in vit D deficiency. 1, 25 -OH 2 vitamin D can be↓, N or ↑in hypocalcemic rickets and usually is N or slightly ↑in hypophosphatemic rickets.

Treatment of Rickets Vitamin D. Stoss therapy: 300, 000 -600, 000 IU orally or IM in 2 -4 divided doses over one day. High dose vit D 2000 -5000 IU orally for 4 -6 wks followed by 400 IU daily orally as maintenance. Adequate dietary Calcium & phosphorus provided by milk, formula & other dairy products. Symptomatic hypocalcaemia need IV Cacl as 20 mg/kg or Ca gluconate as 100 mg/kg as a bolus, followed by oral calcium tapered over 2 -6 weeks.

Other Metabolic Bone Diseases
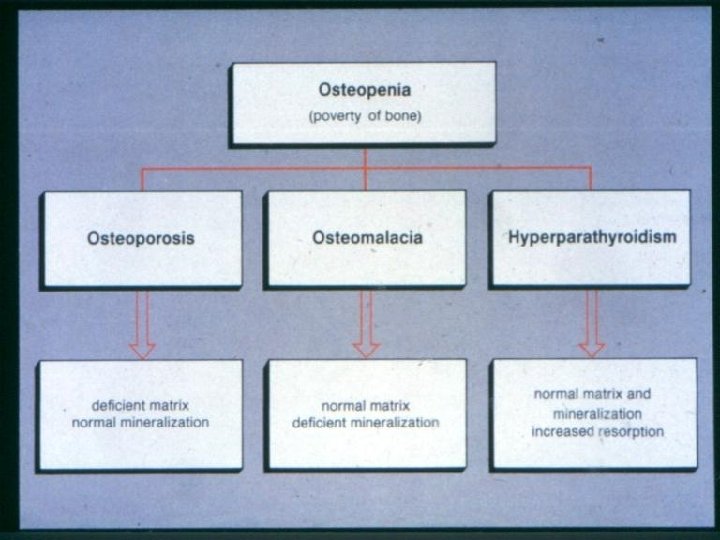

Hyperparathyroidism *Primary hyperplasia - adenoma - carcinoma *Secondary persistent hypocalcaemia *Tertiary secondary leads to hyperplasia

Hyperparathyroidism Pathology - PTH overproduction - Increased renal tubular absorption , intestinal absorption and bone resorption of Ca - Hypercalcaemia and hypercalciuria - Suppressed phosphate tubular reabsorption - Hypophosphataemia and hyperphosphaturia

Hyperparathyroidism Pathology *Hypercalcaemia calcinosis , stone formation , recurrent infection and soft tissue calcification *Bone resorption loss of bone substance , subperiosteal erosion osteitis fibrosa cystica and brown tumors

Hyperparathyroidism Symptoms & Signs *Hypercalcaemia anorexia , nausea , depression and polyuria *Bone rarefaction pain , pathological fractures and deformities *Biochemistry hypercalcaemia , hypophosphataemia , high alk. Phosphatase and serum PTH

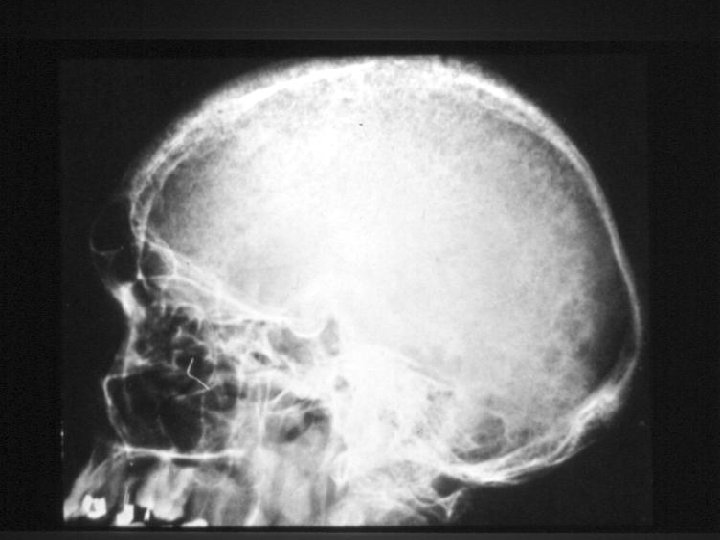
Hyperparathyroidism X-rays - Subperiosteal bone resorption - Generalized decrease in bone density - Brown tumors - Chondrocalcinosis knee , wrist and shoulder
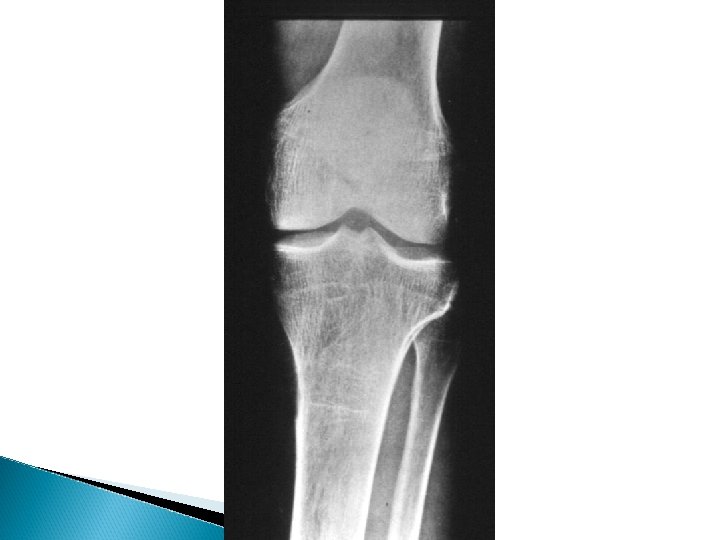
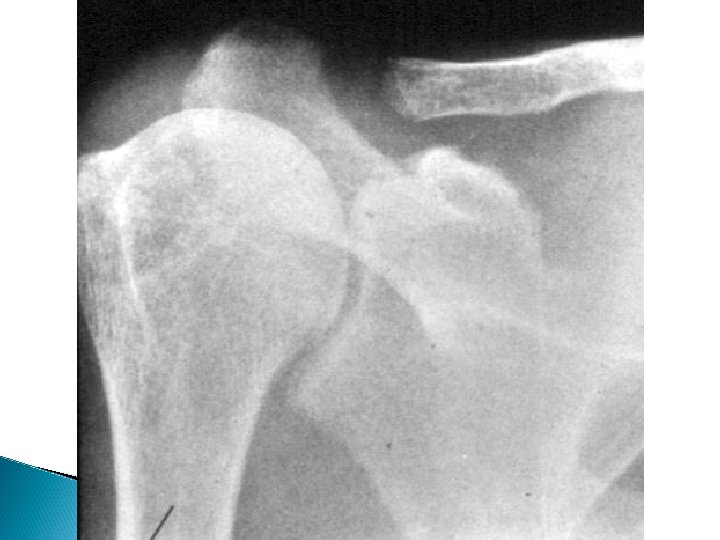
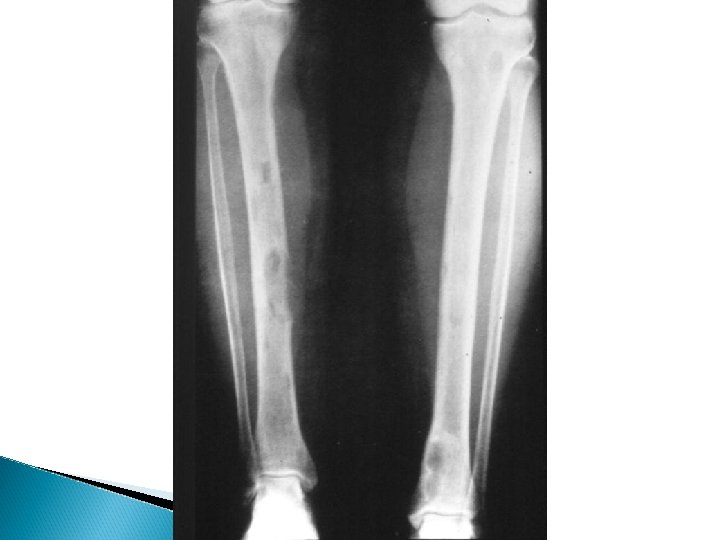
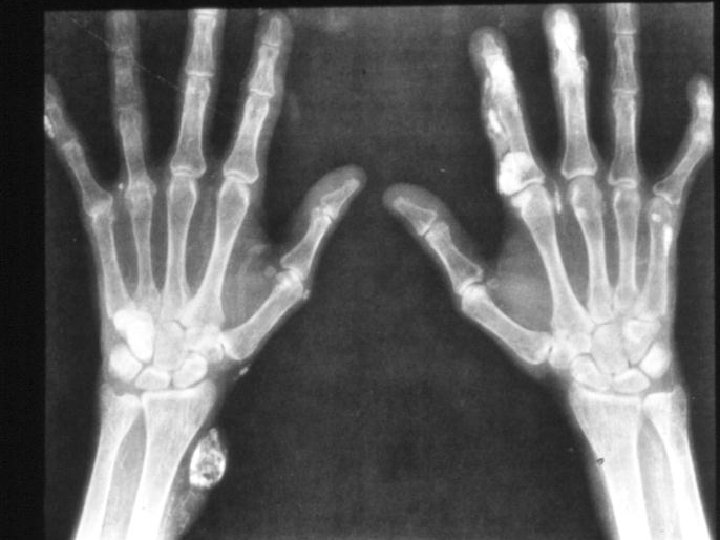
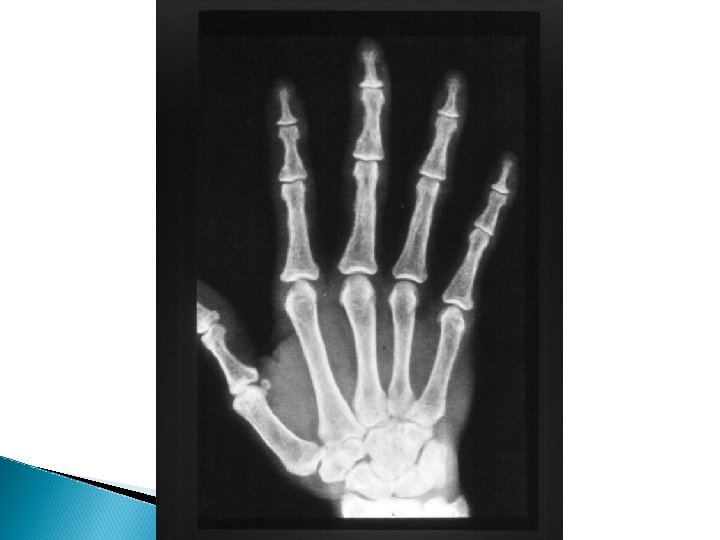

Hyperparathyroidism Treatment Surgical excision of adenoma or hyperplastic parathyroid tissue Hungry bone syndrome ◦ Treated by vitamin D

Osteoporosis * Normal mineralization * Decrease bone mass (amount of bone per unit volume) * Age related * Associated or manifestation of other conditions

Osteoporosis Causes * Idiopathic * Nutritional * Endocrine disorders * Drug induced * Malignant diseases * Miscellaneous
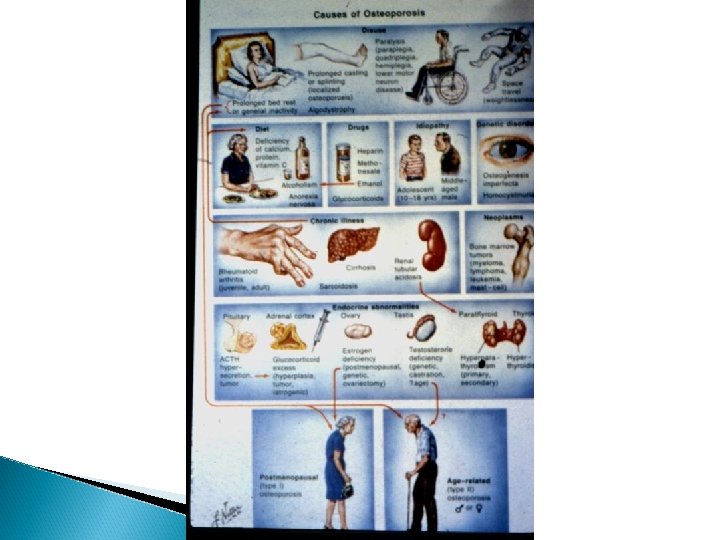

Osteoporosis - Idiopathic osteoporosis - normal investigations - In old patients we have to role out malignancy and multiple myeloma - Younger patients must be fully investigated - Several causes may be involved - Osteoporosis can be associated with osteomalacia

Osteoporosis Symptoms & Signs - Bony aches - Easy fractures spine - lower radius - femoral neck - Rib fracture , chest pain - Normal biochemistry
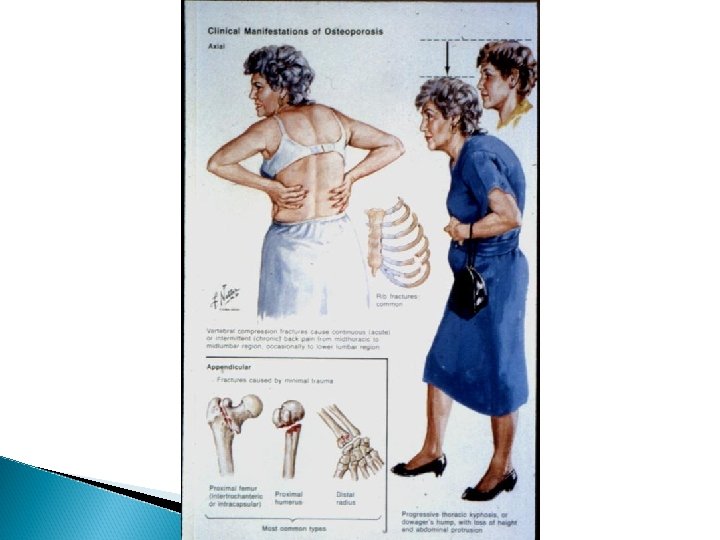

Osteoporosis X-rays - Decrease bone density - Wedging or biconcave vertebrae - Thin cortex and deformities - Dexa Scan - Biopsy
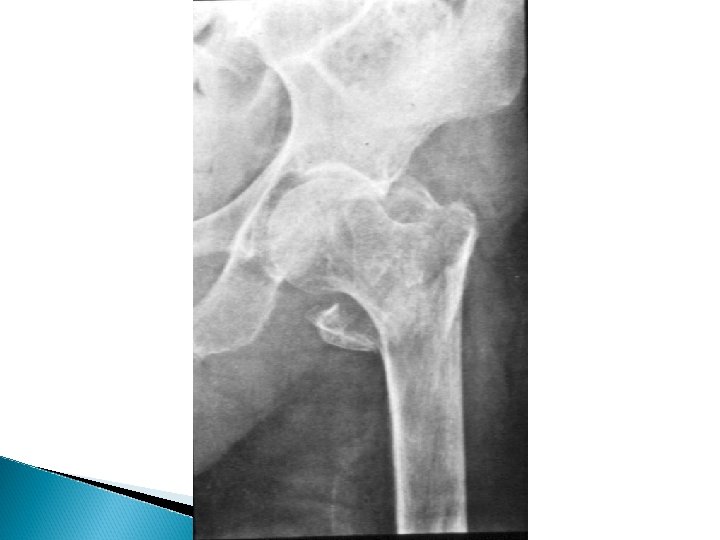
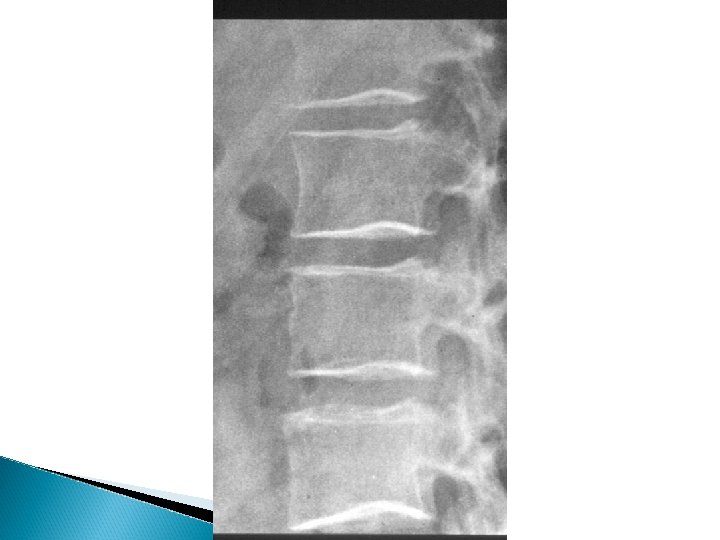
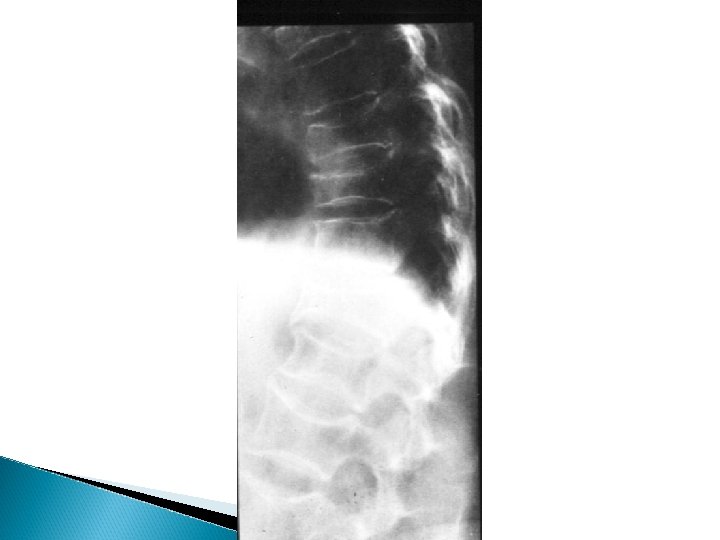
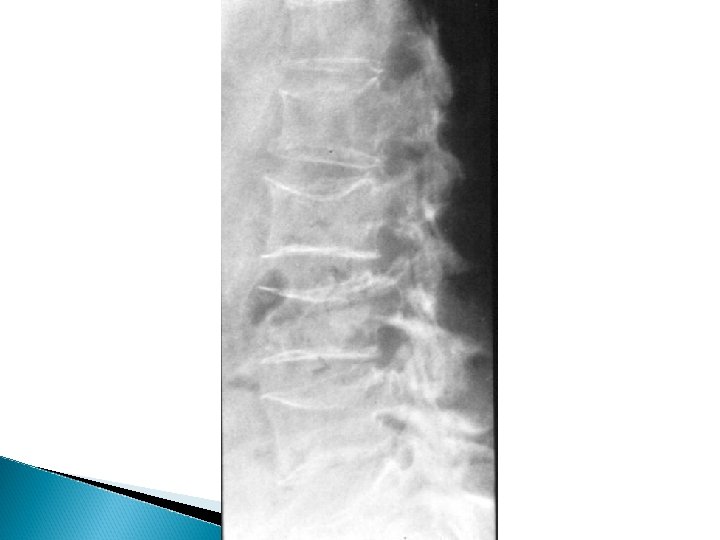
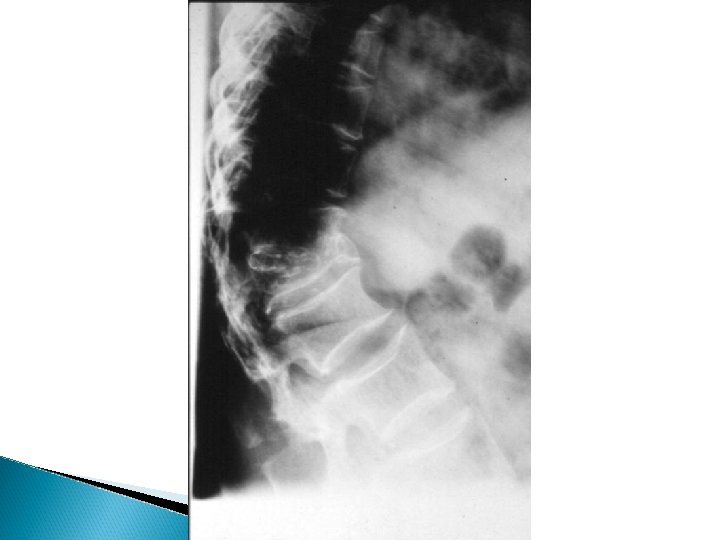


Osteoporosis Treatment - Treat underlying cause - Idiopathic , extremely difficult - Calcium and vitamin D - Fluoride and triple therapy - Calcitonin , Diphosphonate - Treat fractures


Osteoporosis Prevention * Good diet * Exercise * Exposure to sun light * Ca supplement * Hormone therapy

Renal Osteodystrophy Diminished renal P excretion Increased Ca excretion Impaired synthesis of Vit D Toxicity e. g. Aluminum and amyloidosis
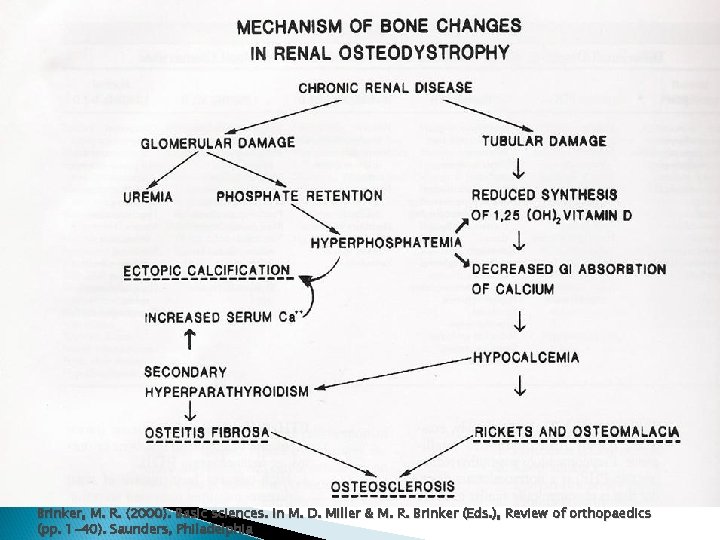
Brinker, M. R. (2000). Basic sciences. In M. D. Miller & M. R. Brinker (Eds. ), Review of orthopaedics (pp. 1 -40). Saunders, Philadelphia

Thank You
- Slides: 61