RHEUMATOID ARTHRITIS Dr Mge Bakgil Kalayc RHEUMATOID ARTHRITIS

RHEUMATOID ARTHRITIS Dr. Müge Bıçakçıgil Kalaycı

RHEUMATOID ARTHRITIS (RA) Second most common form of chronic arthritis Chronic, insidious, autoimmune inflammatory disorder Symmetric polyarthritis affecting mainly small joints in the hand feet, as well as larger joints such as the wrist and shoulders

Characteristic deformities include subluxations, dislocations, rheumatoid nodules, and joint contractures. Crippling disease Shortens survival quality of life

Twin and family studies demonstrate a heritability of 60%; approximately 30% of genetic risk is attributed to the shared epitope encoded on the human leukocyte antigen molecules. Patients with HLA-DRB 1 alleles may have a poorer prognosis

Hormonal and reproductive factors contribute to the female excess and parity, breast feeding, and exogenous hormones are modifiers of risk. Smoking is the strongest known environmental risk factor for RA

ETIOLOGY The cause of rheumatoid arthritis is unknown Genetic predisposition Enviromental event (such as infection) inappropriate self-directed immune response

ENVIROMENTAL FACTORS Infectious agents, Immunoregulatory and hormonal irregularities Immune mediated chronic inflammation Genetic (30%) Environmental Trigger: Self Antigen T cell activation Chronic Inflammation Lymphoid cells infiltrate synovium New blood vessels form in synovium Synovial proliferation Joint destruction
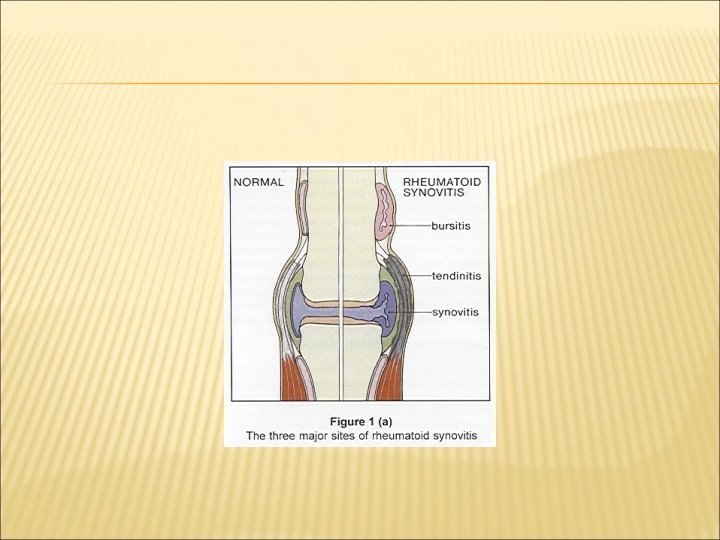

MECHANISMS OF JOINT DAMAGE Synovial mass stretches joint capsule and ligaments: joint swelling, instability & deformity Cytokine and proteolytic enzyme rich synovial fluid destroys cartilage joint space narrowing on X-rays Infiltration of cartilage and later bone by invading synovium (pannus) marginal erosions

EPİDEMIOLOGY Prevalence 0. 05 -0. 15/1000 in developed nations. Disease onset most common at 25 -55 years of age Incidence rises with age Women: men 2. 5: 1

SYMPTOMPS AND SIGNS

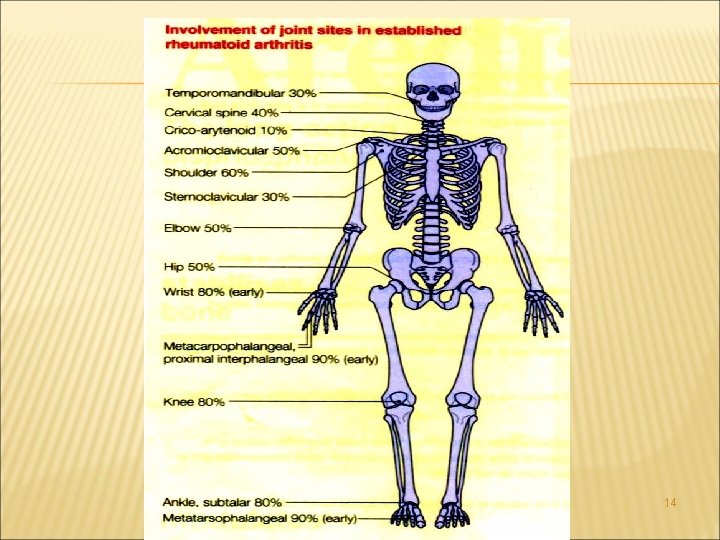
ARTICULAR MANIFESTATIONS The distribution of involved joint is a critical clue to the underlying diagnosis. RA can effect any of the synovial joints. The disease starts in the MCF, PIP, MTF joints Followed by the wrist, knees, elbows, ankles, hips, and shoulders

Symptoms include pain , swelling, and stiffness Stiffness often predominating in the mornings Early treatment helps limit the number of joints involved RA almost always spares DIP joints
14

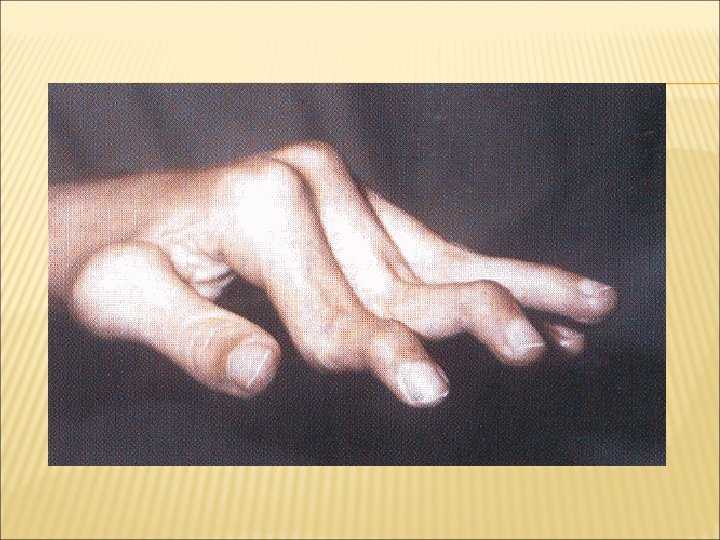
HAND MCP joints PIP joints Synovitis Swan neck deformity Boutonniere deformity Z-deformity of thumb Tendons Synovitis Ulnar deviation Flexor tenosynovitis Extensor tenosynovitis Poor grip: power and pinch





Wrist Synovitis Subluxation Radial deviation Ankylosis Carpal tunnel syndrome


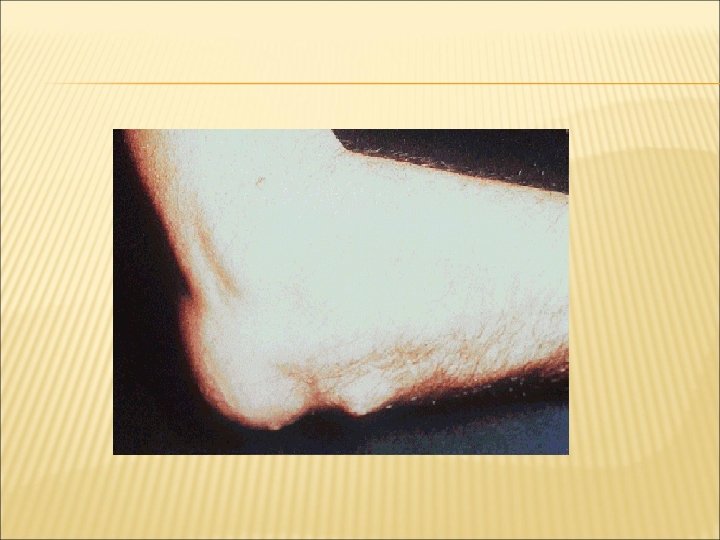
ELBOW Synovitis Flexion contracture Decreased, painful pronation and supination Olecranon bursitis RA nodules

FOOT MTP Synovitis Subluxation with hammer toe and metatarsalgia Toe deviation/overriding Collapse of medial arch of foot


ANKLE/HINDFOOT Ankle Synovitis Retrocalcaneal bursitis Tenosynovitis/rupture Peroneal tendons Tibialis posterior Subtalar arthritis Reduced and painful movement

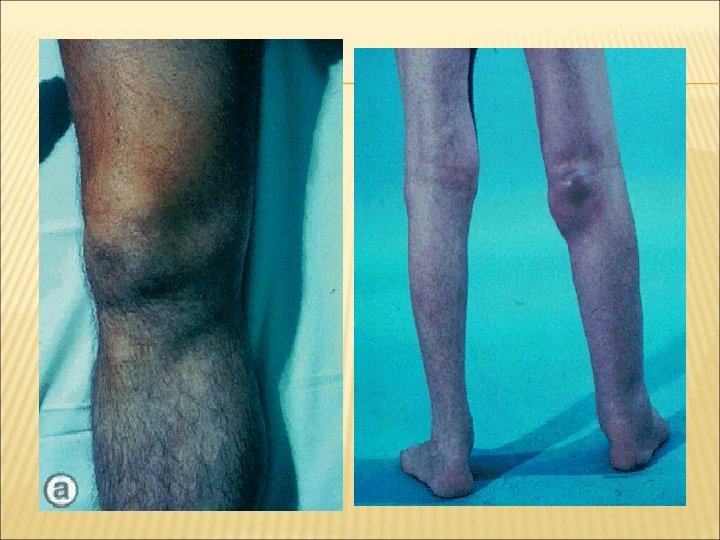
KNEE Synovitis Effusions Baker’s cyst +/- rupture Instability/ deformity eg valgus deformity Flexion contracture
HIP Arthritis (usually late) Pain especially on weight bearing Reduced movement Trochanteric bursitis SHOULDER Subacromial bursitis Rotator cuff tendinitis Glenohumeral joint arthritis Acromio-clavicular arthritis

CERVICAL SPINE Involved in 70% patients with longstanding RA Occipital pain made worse by movement Subluxation of C 1 -2 with compression of spinal cord during neck flexion Significant if >10 mm instability on flexion Usually slowly developing myelopathy

OTHER JOINTS TMJ: reduced mouth opening Sternoclavicular Crico-arytenoid Ossicles of ears

EXTRA-ARTICULAR MANIFESTATIONS OF RHEUMATOID ARTHRTITIS

EXTRA-ARTICULAR MANIFESTATIONS Systemic features; -fatigue, -weight loss, and -low grade fevers (≤ 38 ⁰C) -more common in those patients with rheumatoid factor (seropositive)

SUBCUTANEOUS NODULES Approximately one –quarter of patients In patients who are seropositive for rheumatoid factor. Nodules may ocur almost anywhere lungs, heart, and eye, Most commonly occur subcutaneously on extensor surfaces particullary forearms , over joints or pressure points

SUBCUTANEOUS NODULES Firm on examination Usually nontender( unless traumatized) Tought to be triggered by small vessel vasculitis.
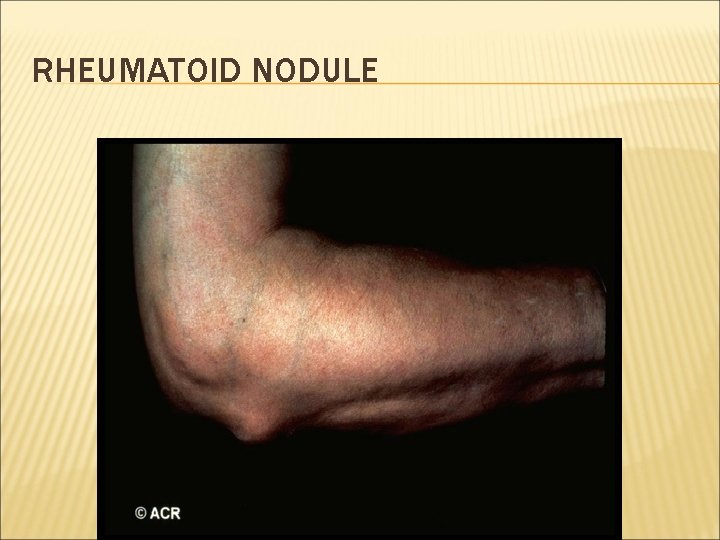
RHEUMATOID NODULE

LUNGS Lungs Pleurisy Pleural effusions ( exudate!) RA nodules single/multiple (Caplan syndrome if huge nodules in coal miners) Lung fibrosis


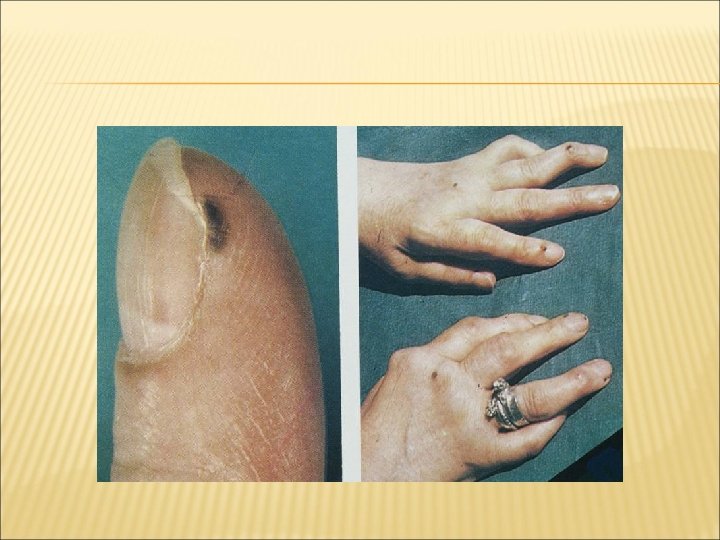
VASCULITIS RA associated small vessel vasculitis Digital infarcts Leukocytoclastic vasculitis should prompt more aggressive treatment with disease – modifying antirheumatic drugs (DMARDs). Pyoderma gangrenosum

CARDIAC INVOLVEMENT Patients with RA have significantly increased morbidity and mortality from coronary artery disease. chronic inflammation, some of medications used, and sedantary lifestyle may be significant risk factors.

CARDIAC INVOLVEMENT Pericardial effusions common (detected in up to 50 % of patients by echocardiography) usually asymptomatic. Rarely, may result in a fibrinous pericarditis, and constrictive pericarditis Uncommonly, rheumatoid nodules may occur in the conduction system and cause heart block.

EYES Secondary Sjögren syndrome Episcleritis Scleromalacia perforans
NEUROLOGIC MANIFESTATIONS Peripheral nerve entrapment syndromes Carpal tunel syndrome Tarsal tunel syndrome Vasculitis - monoeuritis multiplex Subluxations at C 1 -C 2 -myelopati. Rheumatoid nodules in the central nervous system usually asymptomatic

FELTY SYNDROME The triad of RA, Splenomegaly, and Neutropenia. In patients with severe , seropositive disease May be accompanied by hepatomegaly, thrombocytopenia, lympadenopathy and fevers

FELTY SYNDROME Most patients -do not require specific therapy Treatment should be focused on severe RA. Splenectomy -if severe neutropenia exists (<500 cells/µL) a - recurrent bacterial infections

COMPLICATIONS Infections More susceptible to any infection (RA, steroids, MTX) ESPECIALLY susceptible to joint infections Always suspect septic arthritis if sudden increase in symptoms in one joint

COMPLICATIONS Osteoporosis and fractures RA Immobility Steroids Amyloidosis Rare Longstanding disease Proteinuria/decreased renal function Lymphoma

DIAGNOSIS & EVALUATION

BASELINE EVALUATION OF P’T WITH RA Laboratory ESR/ CRP Rheumatoid factor: performed only at baseline to establish the dx; may be repeated 6 -12 ms after disease onset if negative initially ANA Anti-CCP (anti-cyclic citrullinated peptide) 51

CBC, electrolyte, Cr, hepatic panel, U/A, : performed at baseline to assess organ dysfunction due to comorbid diseases, before starting medications SF analysis: performed at baseline if necessary, to rule out other disease; may be repeated during disease flares to rule out septic arthritis

BASELINE EVALUATION OF P’T WITH RA Radiography of selected involved joints May have limited diagnostic value early in the disease, but helps to establish a baseline for periodically monitoring disease progression and response to treatment bone scan, MRI 53

DIFFERENTIAL DIAGNOSIS Post viral (parvo, rubella) Reactive arthritis SLE Polyarticular Gout Polyarticular OA

RA CLASSIFICATION CRITERIA – 1987 AMERICAN COLLEGE OF RHEUMATOLOGY 1. 2. 3. 4. 5. 6. 7. Morning stiffness in and around the joints lasting at least 1 hour At least 3 joint areas simultaneously have had soft tissue swelling or fluid (PIP, MCP, wrist, elbow, knee, ankle, and MTP) At least 1 area swollen (as defined above) in a wrist, MCP, or PIP joint Symmetical involvement of the same joint areas (as defined in 2) Subcutaneous nodules over bony prominences, extensor surfaces, or in juxta-articular regions Postive serum Rheumatoid Factor Radiographic changes typical of rheumatoid arthritis on hand wrist radiographs (must include erosions ) Need 4 of 7 for Diagnosis
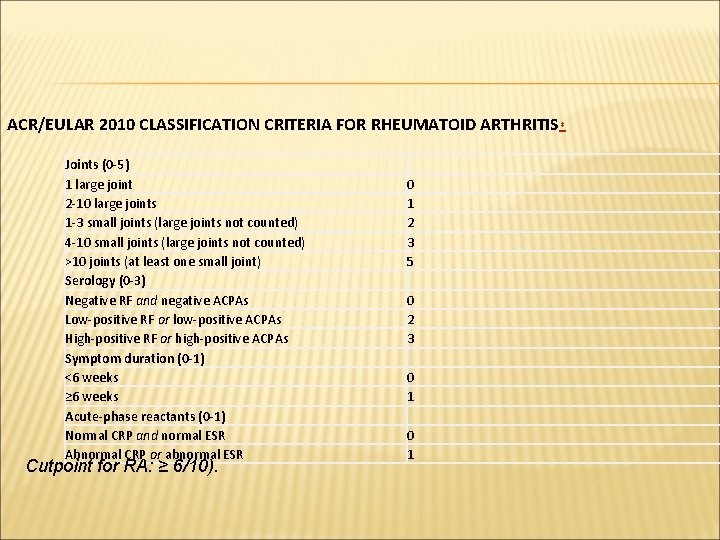
ACR/EULAR 2010 CLASSIFICATION CRITERIA FOR RHEUMATOID ARTHRITIS * Joints (0 -5) 1 large joint 2 -10 large joints 1 -3 small joints (large joints not counted) 4 -10 small joints (large joints not counted) >10 joints (at least one small joint) Serology (0 -3) Negative RF and negative ACPAs Low-positive RF or low-positive ACPAs High-positive RF or high-positive ACPAs Symptom duration (0 -1) <6 weeks ≥ 6 weeks Acute-phase reactants (0 -1) Normal CRP and normal ESR Abnormal CRP or abnormal ESR Cutpoint for RA: ≥ 6/10). 0 1 2 3 5 0 2 3 0 1

RHEUMATOID FACTOR (RF) RFs are human auto-Abs that react with the Fc portion of normal polyclonal Ig. G. Named thus because their first description was in patients with rheumatoid arthritis RF test is approximately 65%-75% sensitive for the diagnosis The presence of RF, even in high titers or large amounts, is not specific for RA

CONDITIONS ASSOC. WITH (+) TESTS FOR RHEUMATOID FACTOR Rheumatologic Diseases Rheumatoid arthritis (~70%) Sjögren’s syndrome (~90%) Lupus (~20%) Cryoglobulinemia syndrome (90%) Lung Diseases Interstitial fibrosis Silicosis Infections Hepatitis C virus Acute viral infections Endocarditis Tuberculosis Miscellaneous Sarcoidosis Malignancies Aging

ANTI-CCP There are other RA-associated auto-Abs known to be specific for rheumatoid arthritis Perinuclear factor Antikeratin antibodies
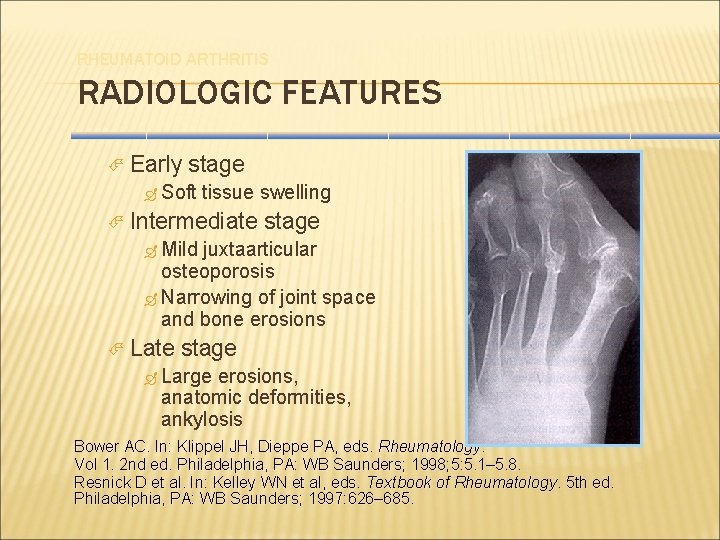
RHEUMATOID ARTHRITIS RADIOLOGIC FEATURES Early stage Soft tissue swelling Intermediate stage Mild juxtaarticular osteoporosis Narrowing of joint space and bone erosions Late stage Large erosions, anatomic deformities, ankylosis Bower AC. In: Klippel JH, Dieppe PA, eds. Rheumatology. Vol 1. 2 nd ed. Philadelphia, PA: WB Saunders; 1998; 5: 5. 1– 5. 8. Resnick D et al. In: Kelley WN et al, eds. Textbook of Rheumatology. 5 th ed. Philadelphia, PA: WB Saunders; 1997: 626– 685.
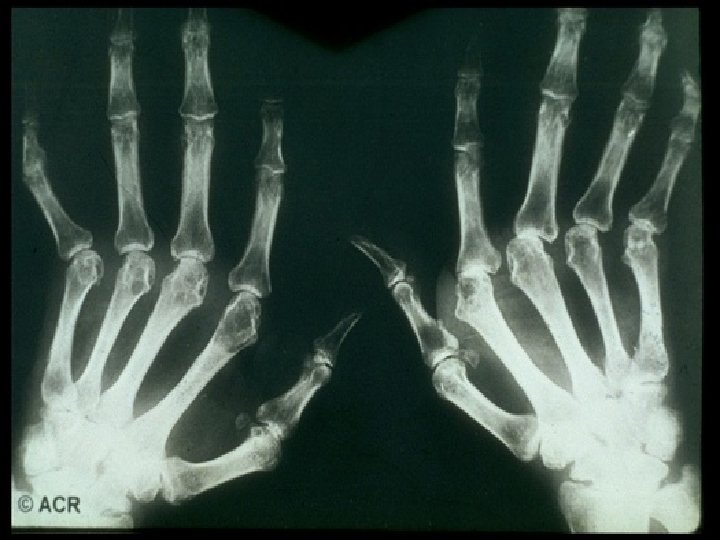
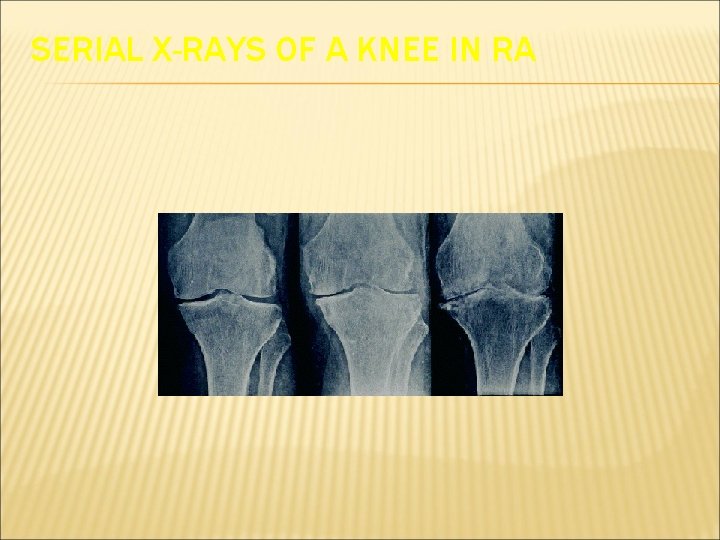
SERIAL X-RAYS OF A KNEE IN RA

MANAGEMENT & THERAPY

RA - MANAGEMENT Nonpharmacologic rest fatigue, splinting pain relief cold, ultrasound, massage physical therapy occupational therapy Patient education

RA - MANAGEMENT Pharmacologic analgesics NSAIDs - full dose corticosteroids prednisone at low dose - “bridge”, “burst” intra-articular steroids

DISEASE MODIFYING AGENTS every patient should be considered for at least one modifying agent limitations may not prevent damage may not be tolerated due to toxicity

DMARD’S (1950’S-1990) Methotrexate Sulfasalazine Antimalarials Gold Salts Penicillamine Cyclophosphamide Azathioprin

DMARDS hydroxychloroquine mild non-erosive disease combinations 200 mg bid eye exams

DMARDS Sulfasalazine 1 gm bid - tid CBC, LFTs onset 1 - 2 months Methotrexate most commonly used drug fast acting (4 -6 weeks) po, SQ - weekly CBC, LFTs

NEW THERAPIES FOR RA Leflunomide (Arava) Tumor Necrosing Factor Inhibitors Etanercept (Enbrel) Infliximab (Remicade) Adalimumab (Humira) Interleukin – 1 Receptor Antagonists

SURGICAL TREATMENT Soft tissue: Carpal tunnel release Synovectomy Tendon transfers Joint replacement Arthodesis

PROGNOSIS Life expectancy reduced by 7 years in men 3 years in women Severe morbidity sudden onset do better than gradual early knee involvement bad Bad RA has a worse prognosis than Hodgkins disease
- Slides: 72