Rheumatoid Arthritis Dr M C du Plooy The



































- Slides: 44

Rheumatoid Arthritis Dr M C du Plooy The Wits University DGMC

Introduction - Systemic disease - Progressive inflammatory immune mediated disorder. - Affects articular and extra articular structures - Joints pathology characterised by proliferation of synovial membrane - Chronic destructive polyarthritis

Epidemiology • • • Worldwide distribution Incidence : 4 per 10, 000 Prevalence : 1 -3 % Female : Male ratio - 3: 1 Older age groups - equal Children (UK) prevalence 1 per 1000 Incidence 1 per 10, 000

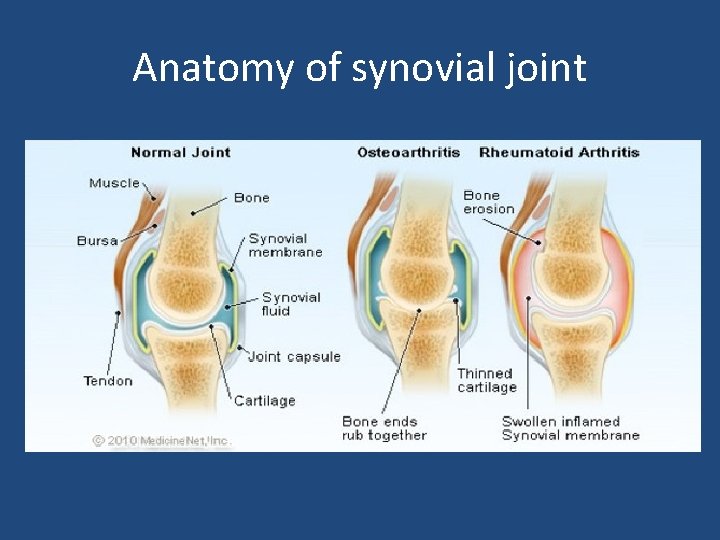
Anatomy of synovial joint

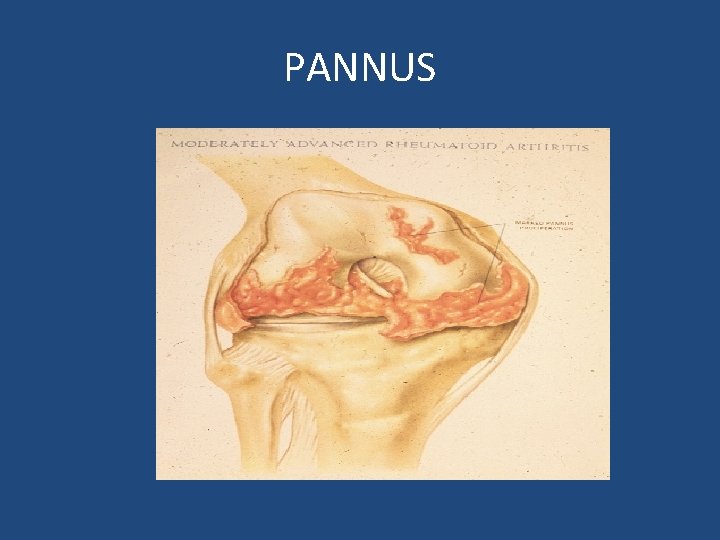
Pathogenesis • Synovial joints affected • Synovial membrane -1 to 3 cells thick • RA- proliferation of synovium - expanding layer of synovial cells - pannus formation ( granulation tissue )

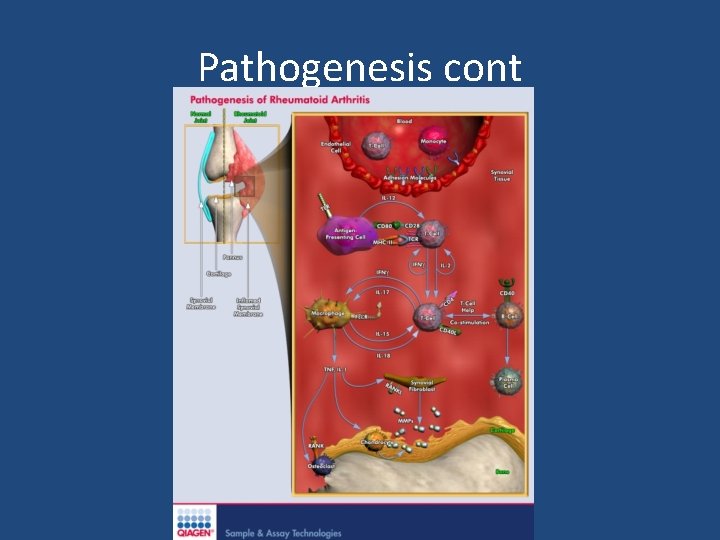
Pathogenesis cont

PANNUS

Clinical Picture Systemic disease • Articular features • Extra articular features

Articular features • Symmetrical • Small joints hands and feet PIPJ MCPJ Wrists • Elbows • Shoulders • Not DIPJ

Articular features cont Lower limbs • • Knees Ankles Midfoot – midtarsal joints Hip Other : • Sternoclacicular joint • TM Joint

Articular features -cont • Cervical Spine esp C 1 and C 2 - radiculopathy - spinal cord involvement • NOT thoracic or lumbar spine • Cricoarytenoid joints : - throat pain - Hoarseness - Stridor

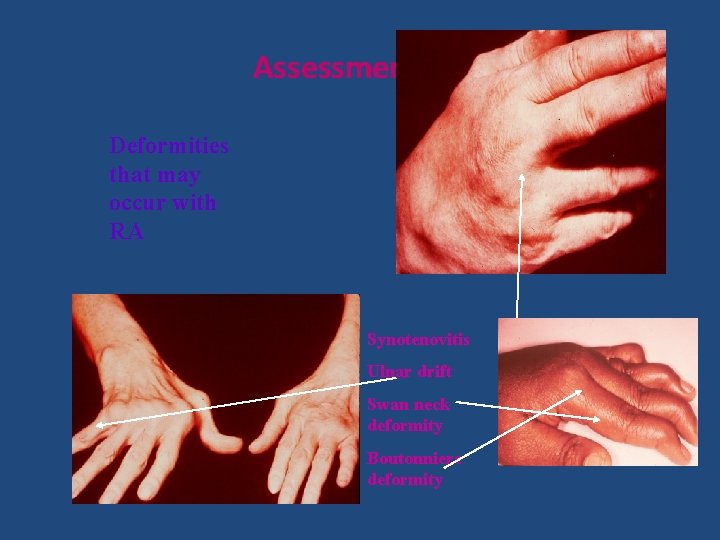
Typical deformities Hands : • Swan neck deformities • Boutonniere • Z deformities thumb • bent fork deformities Feet : • • • Hallux valgus Cock up toes / hammer toes Overriding toes Subluxation of MTPJ Pes planus

Assessment RA Deformities that may occur with RA Synotenovitis Ulnar drift Swan neck deformity Boutonniere deformity

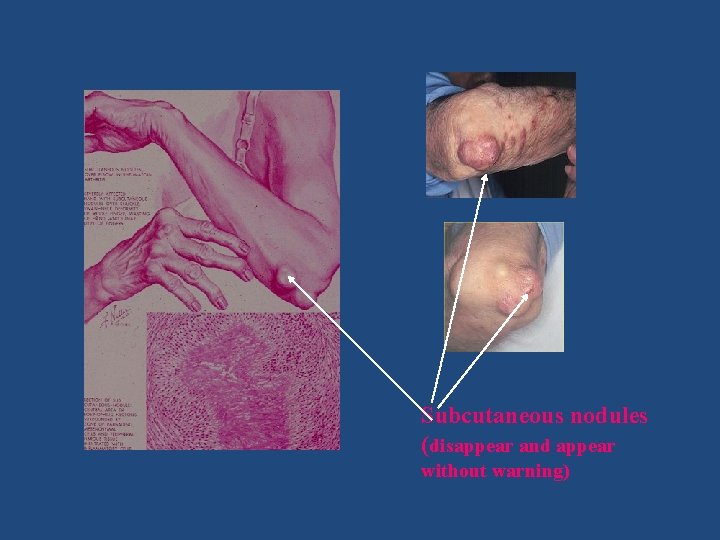
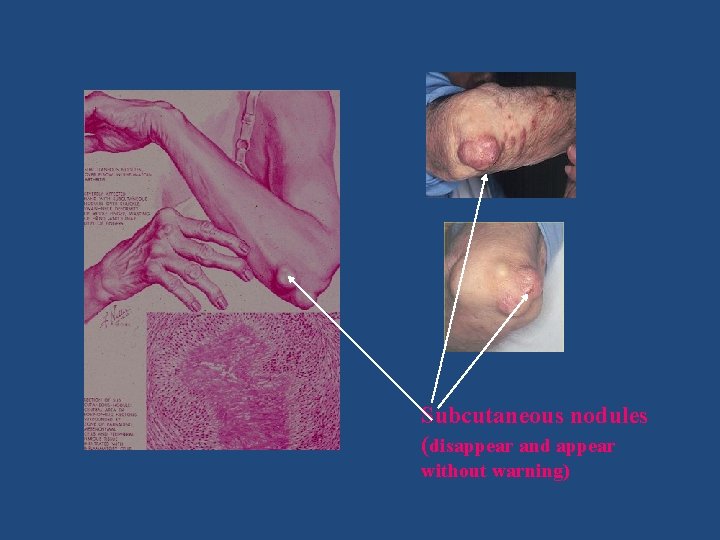
Subcutaneous nodules (disappear and appear without warning)

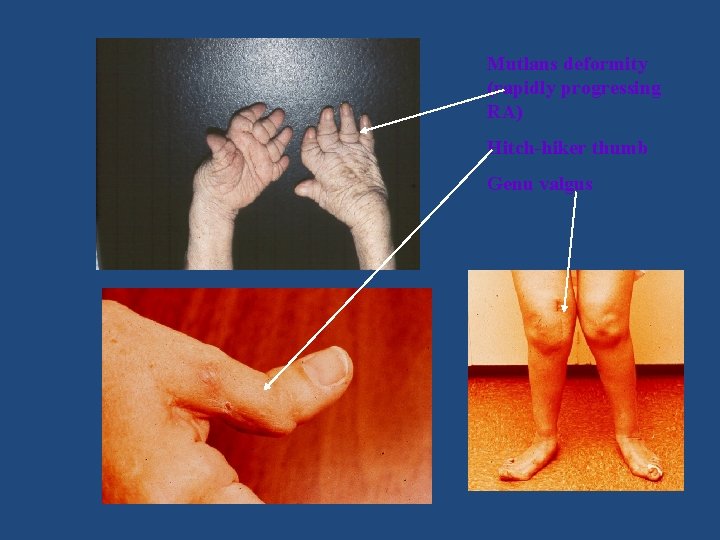
Mutlans deformity (rapidly progressing RA) Hitch-hiker thumb Genu valgus

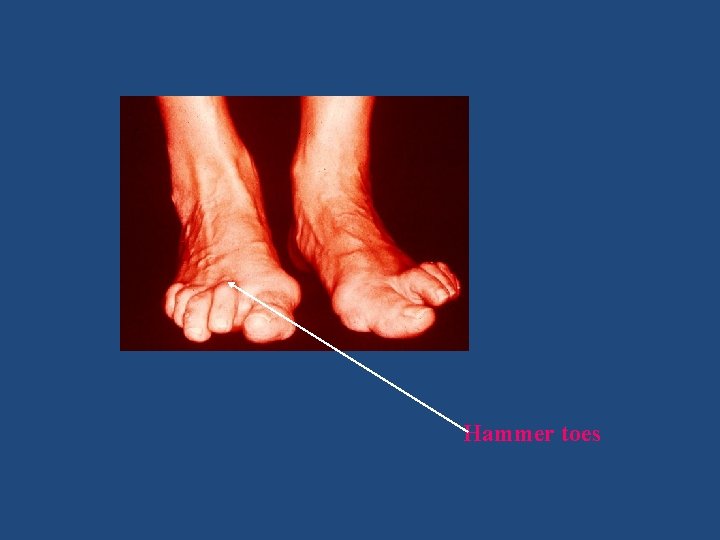
Hammer toes

Extra articular features • Constitutional: - Fever / Weight loss / fatigue • Skin ; - SC Nodules - Vasculitis - Palmar erythema • Pulmonary : - Pleuritis - Pulm nodules - ILD - Bronciolitis obliterans - Pulmonary HPT : ILD / vasculitis of pulmonary vessels

cont • Eyes : - Sjogrens syndrome - Episcleritis - Scleritis - scleromalacia perforans • Haematological: - Anaemia : ACD / Fe deficiency / Folate def - Leucocytosis - Thrombocytosis

cont Renal : - Rarely directly - Amyloidosis or drugs CVS : Increased risk of IHD - Accelerated atherosclerosis - Corticosteroids - Vasculitis Other : MR / AR / TR RA is Independent risk factor for IHD

Cont Vasculitis - Leucocytoclastic vasculitis - Non healing ulcers eg Pyoderma gangrenosa - Neuropathy

cont Nervous system: • Central NS: - brain not affected - spinal cord compression C/Spine • Peripheral NS: - Peripheral neuropathy - Compression neuropathy eg CTS, TTS - Mononeuritis multiples eg wrist or foot drop

COMPLICATIONS MALIGNANCIES: • Increased risk : - Altered immuno surveilance - Immunosuppressive drugs • Types: - NHL - Nonmelanomatous skin cancers • Lower risk: - Breast CA - Colon cancer • ? NSAID Rx

cont INFECTIONS : Increased risk multifactorial : - Activity and severity of RA - GC use - Comorbidities eg DM, CCF - Joint replacement surgery

Investigations Blood tests • • RF Anti CCP ab FBC LFT ESR CRP ANA

Investigations - cont • Imaging : - Xray : hands – AP only C/Spine - Ultrasound - MRI - Bone density • Urine dipstix

Diagnosis • ACR criteria 1987: - EMS > 1 hr Arthritis in > joint areas Small joints : PIPJ / MCPJ /wrists Symmetric Nodules RF and/or Anti CCP positive Xray changes eg typical erosions , PAOP 4/7 present > 6 weeks

Eular –ACR criteria 2010

Subcutaneous nodules (disappear and appear without warning)

Poor prognostic features • • • Smoking Number of swollen joints Socioeconomic status Level of education Lag time from onset sx to diagnosis to initiation of DMARD’s Sustained elevated acute phase reactants Anti CCP positivity High titers of RF and anti CCP ab Genetic background Erosions esp < 2 yrs

Management Non pharmacological : Pharmacological Surgical

Non Pharmacological - Multi disciplinary team • • • OT PT Podiatry Biokinetics Psychologist Social worker

Joint Protection: Do’s and Don’t’s

Management -cont Pharmacological: Pain Relief : - Analgesics : - NSAIDS DMARD’s - Synthetic - Biologic

Mx -cont Synthetic DMARD’s • • • Anti malarials Methotrexate Sulfasalazine Leflunomide Corticosteroids

Mx -cont Biologic DMARD’s: • Cytokine Inhibitors : - Anti –TNF inhibitors : Infliximab; Adalumimab; Etanercept; Golimumab - Anti IL 6 ab ( Actemra ) • T cell co stimulatory pathway modulator: Abatacept – Orencia • B Cell inhibitors Anti CD 20 inhibitor ( Rituximab ) • Intracellular : Small molecules kinase inhibitors eg JAK kinase inhibitors

Management -cont DMARD’s - SLOW ACTING drugs - Explain to patients re A/E - Regular blood tests Corticosteroids: - Bridging period - Beneficial in first 6 months - Vit D and Ca prophylactically with CS > 1/12

Mx -cont • Comorbid diseases: • Depression • Osteoporosis • Traditional risk factors for IHD HPT; Dislipidaemia ; Smoking ; DM

Pregnancy • Which drugs are safe to use ? • • Salazopyrin Hydroxycloroquin Azathioprine Prednisone

Mx - cont Surgical : • • Joint replacement Tenosynovectomy for nerve entrapment Decompression carpal tunnel Corrective arthrotomies of MTJ Stabilisation of C/Spine Tendon release and transfer Arthrodesis of esp ankle joint

Outcome measures • Treat to target : • What is the target ? - Remission (goal) Clinical remission Serological remission Radiographic remission - Low disease activity

cont • How to measure ? Various tools : - SDAI - CDAI - DAS 28 score - HAQ

cont • What parameter to be measured ? • • Duration of EMS Number of tender joints Number of swollen joints Patient global assessment Physicians global assessment Acute phase reactants Ultrasonography

Mortality and Morbidity • Morbidity: Disease of > 10 yrs – 50 -80% unable to work • Mortality: • Causes of death : - IHD - Infections - Fractures with post op complications - Malignancies

THANK YOU