Rheumatic Heart Disease in Pregnancy Dr Jane Thorn
















- Slides: 20

Rheumatic Heart Disease in Pregnancy Dr Jane Thorn Obstetrician and Gynaecologist Royal Darwin Hospital October 2016

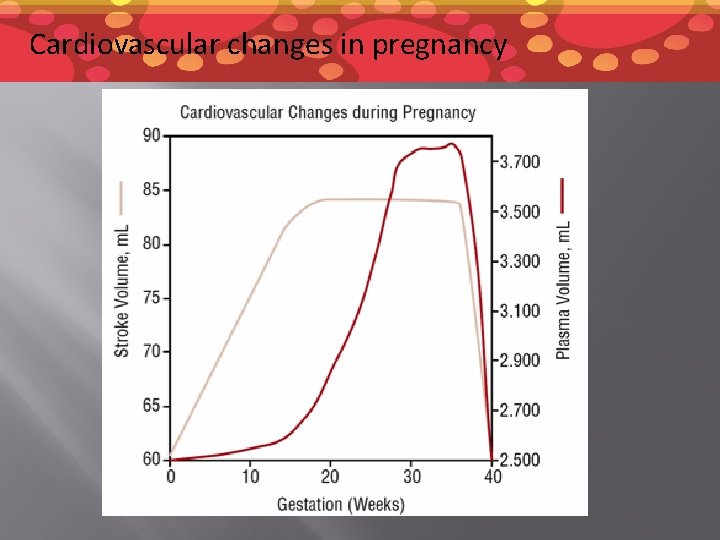
Cardiac Output in Pregnancy � � Increases by 30 – 40% by around 27 weeks gestation then drops dramatically toward term (37 – 41 weeks) Blood volume increases 1000 – 2000 mls � ~625 mls in the maternal circulation of the placenta

Cardiovascular changes in pregnancy

Labour and Birth � First Stage � Labour Uterine contractions Pain � Second Stage � Birth of the baby Active descent of the baby (pushing) � Third Stage � Delivery of the placenta Associated maternal blood loss (up to 500 mls considered normal)

Cardiac Impact of Labour and Birth � Cardiac output rises progressively from the first stage of labour to an additional 50% in late second stage � An � � increase of >7 litres per minute Birth causes a dramatic shift of fluid with a sharp rise in left atrial pressure. This can be exacerbated by post-partum haemorrhage Epidural and general anaesthetics cause acute changes in cardiac output

Why are we interested in RHD in Pregnancy � Cardiac disease is one of the major causes of maternal mortality in Australia � Pregnant women with mitral stenosis have a mortality risk of up to 1% � Pregnant women with mitral stenosis and atrial fibrillation have a mortality risk of up to 15% � Pregnant women with pulmonary hypertension have a mortality risk of up to 50%

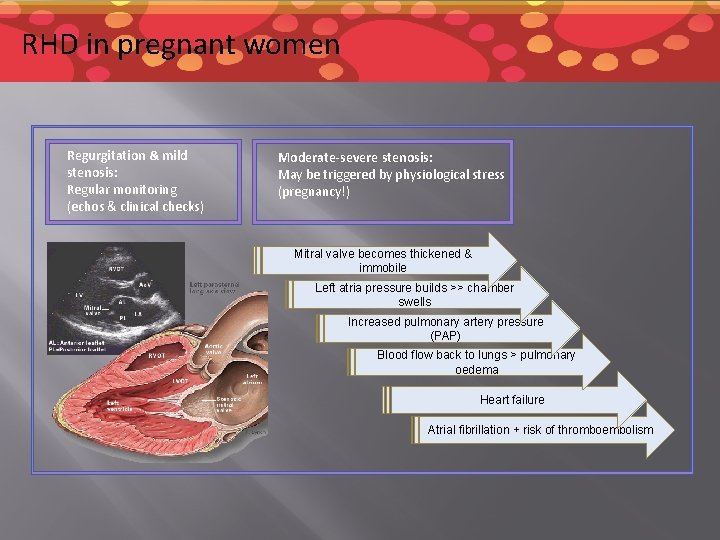
RHD in pregnant women Regurgitation & mild stenosis: Regular monitoring (echos & clinical checks) Moderate-severe stenosis: May be triggered by physiological stress (pregnancy!) Mitral valve becomes thickened & immobile Left atria pressure builds >> chamber swells Increased pulmonary artery pressure (PAP) Blood flow back to lungs > pulmonary oedema Heart failure Atrial fibrillation + risk of thromboembolism

• 180 women giving birth with RHD • Australia • 190 pregnancies • • • 10 women had two or more pregnancies during the study 79% Aboriginal &/or Torres Strait Islander 187 liveborn babies 60 women resident in the Northern Territory • www. amoss. com. au Preliminary data 3 of 30 inpatients at RDH on 16/10/16 RHD

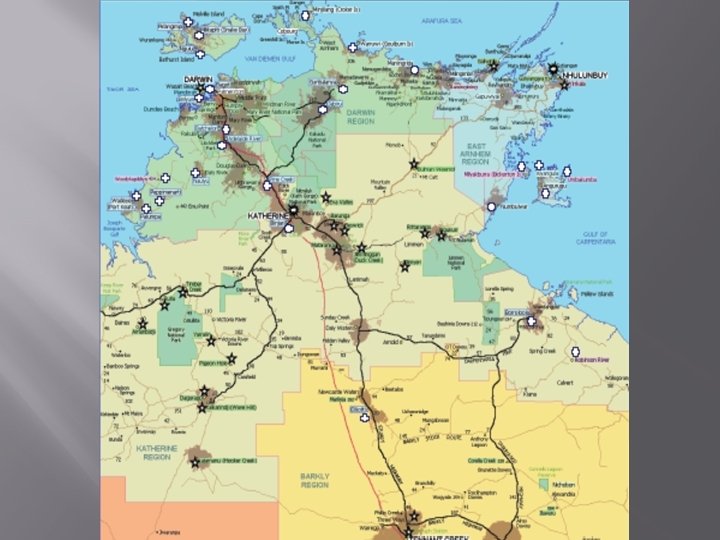
Antenatal care and transfer Antenatal Care • 36% women 1 st antenatal visit >20 weeks • 56% women transferred care during pregnancy • 2/3 due to high-risk status &/or to access facilities due to their RHD • 9 women transferred interstate; & significant number travelled distances >1800 km to a referral hospital • All women residing in remote communities in the NT must give birth in one of 4 hospitals • RDH, ASH, Gove, Katherine • Women from North East Arnhem and the Barkley region considered high risk must give birth at Royal Darwin Hospital health. uts. edu. au


Case Study CB � 27 year old woman � Living � between Katherine and Minyerri G 6 P 3 � NVB x 3 1 in WA 2 at Katherine Hospital � PPH � � 700 mls last baby This pregnancy dated on 8/40 scan RHD diagnosed May 2015 P 2/3 � Mild mitral stenosis and regurgitation � Mild aortic regurgitation � Commenced on LA Bicillin at diagnosis � No echocardiogram performed this pregnancy

CB � Syphilis +ve � 1: 18 in early pregnancy � Treated appropriately � Baby to receive treatment at birth � Anaemic � Hb � � 97 Did not have OGTT Heavy tobacco smoker Non-drinker Domestic violence

CB � At least 7 antenatal visits � Antenatal care between Minyerri (Sunrise Health Service) and Katherine (Wurli-Wurlinjang Health Service and Katherine Hospital) � Obstetric ultrasound at 36/40 � Oligohydramnios and raised umbilical artery dopplers � Induction of labour started but abandoned � Repeat ultrasound considered normal � No documented follow-up plan

CB � Presented to KH at 38/40 with SROM � Duration of ROM > 24 hours � Started on IV benzyl penicillin � Induction of labour � Normal vaginal birth � Retained placenta with 2000 ml PPH necessitating manual removal in OT (general anaesthetic) � Retrieved to RDH for ongoing care

How would I have liked this case managed? � Pre-pregnancy planning � Effective contraception to allow for: Review of cardiac status and education around risks associated with pregnancy and birth Change of medication if on ACE inhibitors, warfarin etc Review of diabetic and renal status and BGL stabilisation and optimisation Treatment of STIs Correction of anaemia Education around engaging in antenatal care and need for early pregnancy diagnosis

How would I have liked this case managed? � Regular antenatal visits � From pregnancy diagnosis (preferably in first trimester) � Opportunity to offer aneuploidy screening � Allows time for appropriate referral and multidisciplinary management and planning for delivery � Collaborative care with both community clinics and obstetricians

How would I have liked this case managed? � � � Echo and cardiac review in third trimester with recommendation regarding ability to tolerate normal labour Anaesthetic review (after Echo) Delivery in a hospital with appropriate level of obstetric, anaesthetic and cardiac expertise

Challenges of Care � � Access to services and expertise in regional and remote areas Disconnected health information services Awareness: Untold stories – under-reporting. (Generally) good awareness in high-prevalence regions… but diagnosis is still ‘missed’. Low awareness where RHD is overall rare Conflicting priorities for women – how important is sub-clinical RHD when there’s no food in the home?

A taxi to get to the ferry to get to the plane to get to the cardiac centre … for an echocardiogram … when you don’t know if your kids are going to be all right …
