Rh Incompatability Rh Isoimmunization The Rh factor is

Rh- Incompatability Rh- Isoimmunization

The Rh factor is : An antigen that present in the surface of the RBC’s Was discovered 1 st on monkeys

Definition Is an immunologic disorder that occurs in a pregnant Rh-negative pt carrying an Rh-positive fetus.

PATHOPHYSIOLOGY Person who lacks Rh antigen on the surface of RBC is called Rh- negative And an individual with antigen is Rh-positive
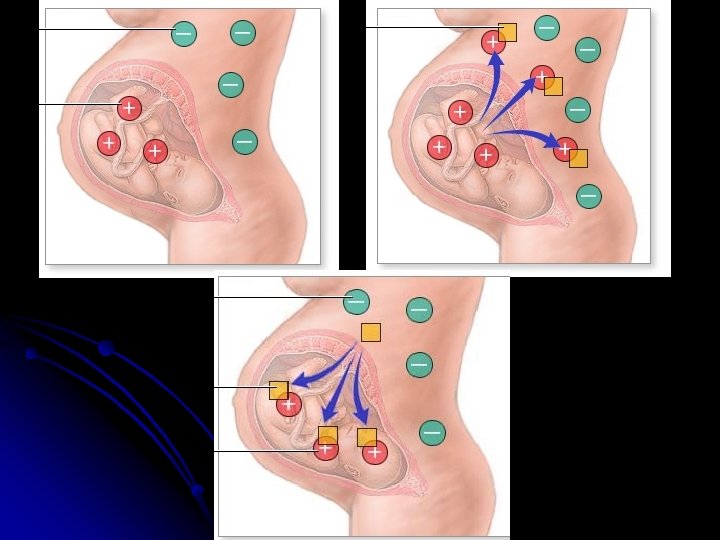

Antigens that make up the Rh complex CDE ( Cc. DEe) N. B : more than 90% of Rh Incompatibility are due to D antigens

Two mechanism are proposed for sensitization : *sensitization ? ? Rh –ve patient are exposed to Rh-Ag 1 - Occurrence of undetected placental leak of fetal RBCs into the maternal circulation During pregnancy 2 - “ Grandmother theory “

*In general two exposures to Rh antigen Are required to produce any significant sensitization unless the first exposure is massive. *The initial response to exposure to Rh antigen is production of Ig. M for short period of time

Pathogenesis Of Rh Isoimmunisation Rh Negative Women Rh -ve Fetus No problem Man Rh positive (Homo/Hetero) Fetus Mother previously sensitized Secondary immune response ? Iso-antibody (Ig. G) Fetus Haemolysis Rh positive Fetus Rh+ve R. B. C. s enter Maternal circulation Non sensitized Mother ? Primary immune response Fetus unaffected, 1 st Baby usually escapes. Mother gets sensitised?
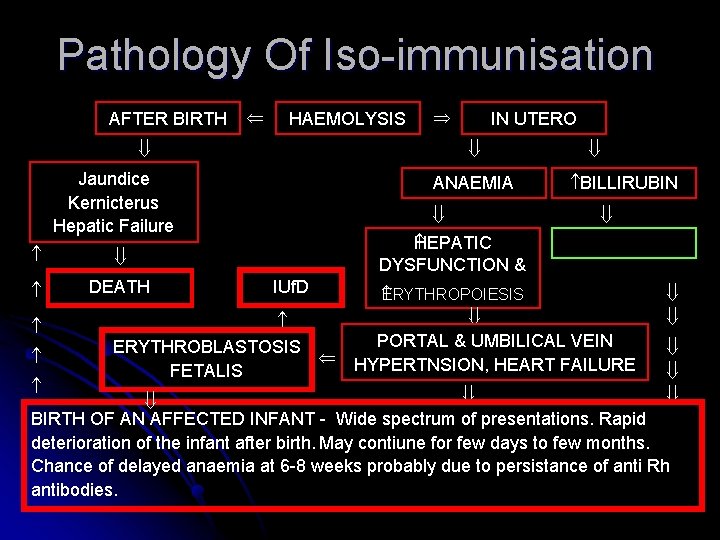
Pathology Of Iso-immunisation AFTER BIRTH HAEMOLYSIS Jaundice Kernicterus Hepatic Failure DEATH ANAEMIA BILLIRUBIN EPATIC H DYSFUNCTION & IUf. D ERYTHROBLASTOSIS FETALIS IN UTERO ERYTHROPOIESIS PORTAL & UMBILICAL VEIN HYPERTNSION, HEART FAILURE BIRTH OF AN AFFECTED INFANT - Wide spectrum of presentations. Rapid deterioration of the infant after birth. May contiune for few days to few months. Chance of delayed anaemia at 6 -8 weeks probably due to persistance of anti Rh antibodies.

*Most immunization occur at the time of delivery and Ab appear either during the postpartum period or following exposure to the antigen in the next pregnancy *If a women has hx of fetal hydrops with a previous pregnancy , the risk of hydrops with a subsequent pregnancy is about 90%

Incidence - Although the transplacental hemorrhage is very common, the incidence of Rh immunization within 6 months of delivery of the 1 st Rh-positive , ABO-compatible infant is only about 8%

Incidence -The overall risk of immunization for the 2 nd fullterm, Rh-positive , ABO-compatible pregnancy is about 1 in 6 pregnancies -The risk of Rh sensitization following ABOincompatible Rh-positive pregnancy is 2% WHY? ! The protection against immunization in ABOincompatible is Due to the destruction of the ABO incompatible cells in the maternal circulation and removal of the RBCs debris by the liver

Incidence -The incidence of immunization following spontaneous abortion is 3. 5%, whereas following induced abortion is 5. 5%

Incidence -All Rh-negative patients at 8 weeks’ or more gestation should receive prophylactic Rho D-immune globulin (Rho-GAM) following spontaneous or induced abortion , invasive gynecologic procedure, or abdominal trauma.

Recognition of the pregnancy at risk

History: A history suggesting the presence of any of the following factors should trigger an extensive diagnostic study: Maternal history Rh negative (d; d) blood type Known presence of isoimmune blood group antibodies Prior administration of blood products Risks of illicit drug use Collagen disease Thyroid disease or diabetes Organ transplant (liver, kidney) Blunt abdominal trauma (abuse, auto accident) Coagulopathy Use of indomethacin, sodium diclofenac, or potentially teratogenic drugs during pregnancy Younger (<16 y) or older (>35 y) maternal age Risk factors for sexually transmitted diseases Hemoglobinopathy (especially with Asian or Mediterranean ethnicity) Occupational exposure to infants or young children Pet cat Current or recent community epidemic of viral illness

Family history Jaundice in other family members or in previous child Family history of twinning (specifically, monozygotic) Family history of genetic disorders, chromosomal abnormalities, or metabolic diseases Congenital malformation(s) in previous child Previous fetal death(s) Hydramnios in earlier pregnancies Prior hydrops fetalis Previous fetomaternal transfusion Congenital heart disease in previous child

Physical: The presence of any of the following physical findings should prompt further diagnostic evaluation: Twinning Hydramnios Exanthem or other evidence of intercurrent viral illness Herpetic lesion(s) or chancre(s) Decrease in fetal movements

- By blood sample from each pregnant woman 1 st visit to determine blood group and Rh type. - In Rh-negative Rh status of the father should be determined.

- If the father is Rh-positive , his Rh genotype and ABO status should be determined. -The can be done by testing his RBCs by reagent for antigens D, E , C, e &c. - If he is homozygous for D antigen? ? -Heterozygous? ?

-the Rh-negative woman whose partner is Rh-positive and whose initial antibody test is negative should repeat it again at 28 week prior to receive the Rho-GAM prophylactic.

-At delivery , cord RBCs must be sent to determine fetal blood group , Rh type. and direct coomb’s test. - If a transplacental hemorrhage of greater than 30 ml of blood is suspected, a Kleihauer-betke test is helpful to detemine the volume of hemorrhage.

Betke -Kleihauer test: In this test, by acid elution mother's RBC’s very pale fetal cells remain stained. Simple comparative counts allow an estimate of whether a significant fetal-maternal transfusion occurred

Maternal Rh-antibody titer -Anti-D antibody titers generally provide limited information regarding the severity of fetal hemolysis in Rh disease. -But it can be used to guide the decision regarding initiating other procedure.

-In initially immunized pregnancy , the fetus is NOT at risk if the titer remains below 1: 16. -in patient with a positive titer less than 1: 16 repeat titer should be obtained every 2 to 4 weeks. - If the titer rises to 1. 16 or more , invasive testing should be considered. -

Amniotic fluid spectrophotometer used for: severity of fetal hemolysis

Amniotic fluid spectrophotometer There is excellant correlation between the amount of biliary pigment in amniotic fluid and fetal hematocrit, beginning at 27 weeks’ gestation. -the most common source of bilirubin is tracheal and pulmonary efflux and transudate from the umbilical and placental vessel. -
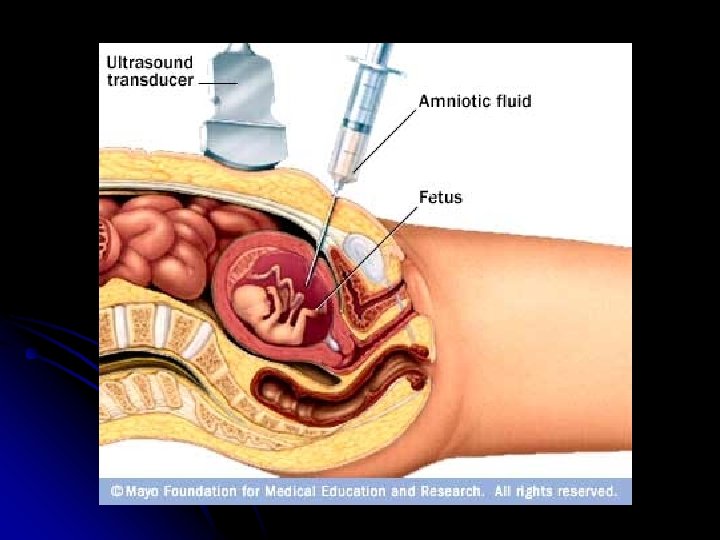

Ultrasonic detection of Rh sensitization -Serial ultrasonic examination for placental size and thickness and hepatic size. -Fetal hydrops diagnosed by; -asictes -pleural effusion -pericrdial effusion -Skin edema
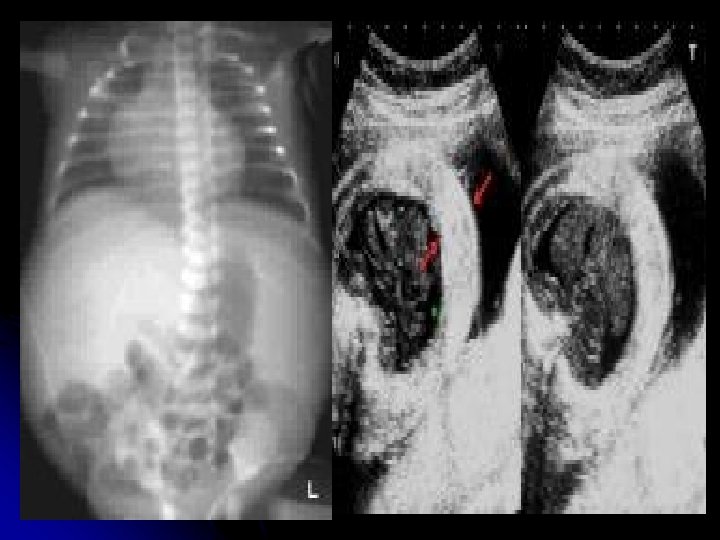
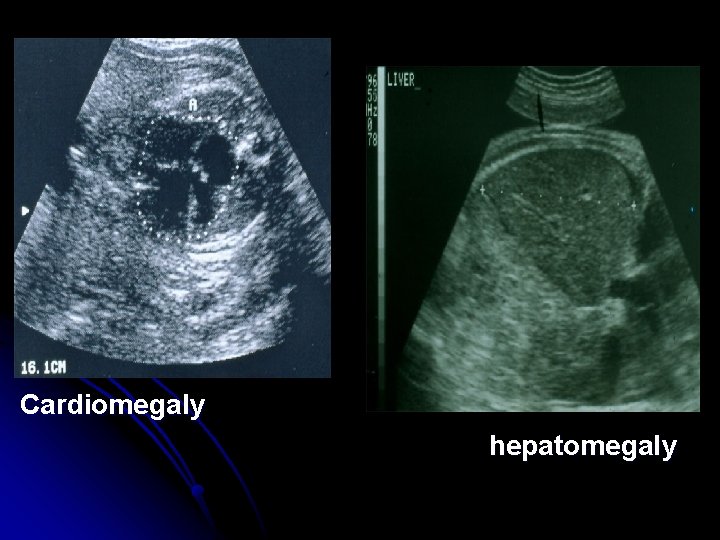
Cardiomegaly hepatomegaly

-Doppler assessment of peak velocity in the fetal middle cerebral artery MCA may prove to be the most valuable ultrasonic tool for detecting fetal anemia. - After 35 week gestation , this test may produce a higher false-positive rate.
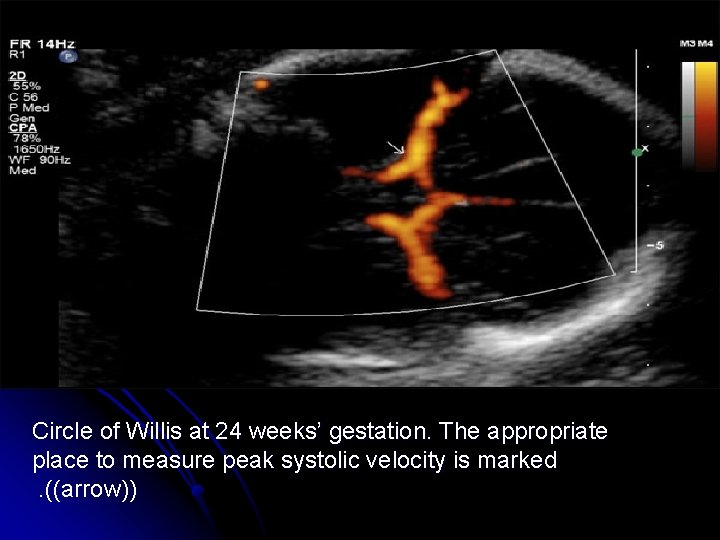
Circle of Willis at 24 weeks’ gestation. The appropriate place to measure peak systolic velocity is marked. ((arrow))

Percutaneous umbilical blood sampling Allow measurement of fetal; Hemoglobin Hematocrit Blood gases p. H Bilirubin level
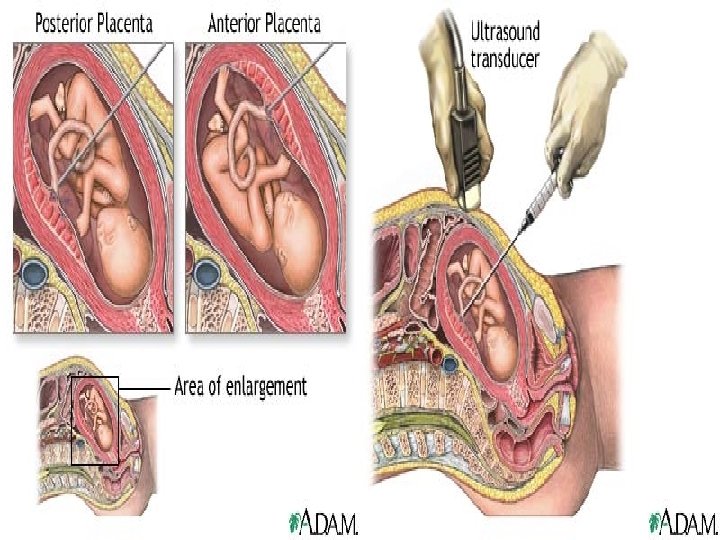
Risk from PUBS: -Fetal exsanguination from placental vessels tear -fetomaternal hemorrhage 40%

Management ACCORDING TO GESTATIONAL AGE

vaginal delivery at or near term is the goal of mangement, after 34 weeks determine the fetal lung maturity by L: S ratio or phosphatidylglycerol PG level to determine the optimum time of delivery, before 34 weeks try to avoid delivery.

Liley chart Originated by liley in 1961, he compared ∆OD 450 measurements with fetal outcome in 101 isoimmunized pregnancies and showed that Mild, Moderate, or Sever fetal anemia could be predicted according to which of three zones the bilirubin level was plotted into ∆OD 450 = optical density deviation.
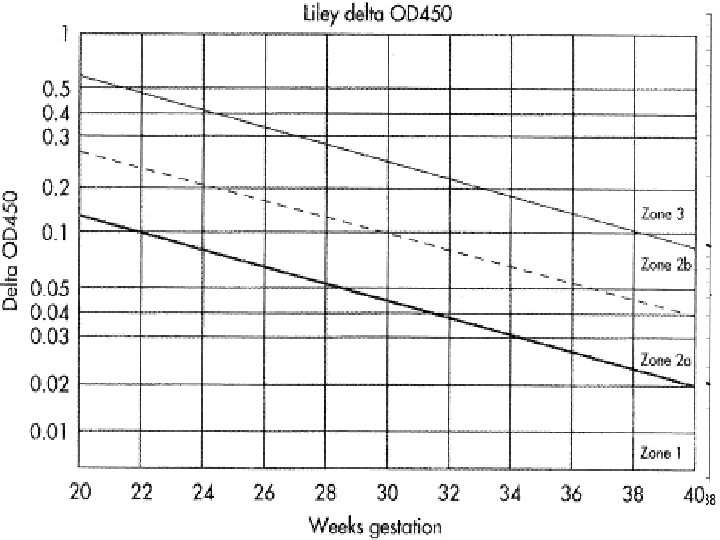
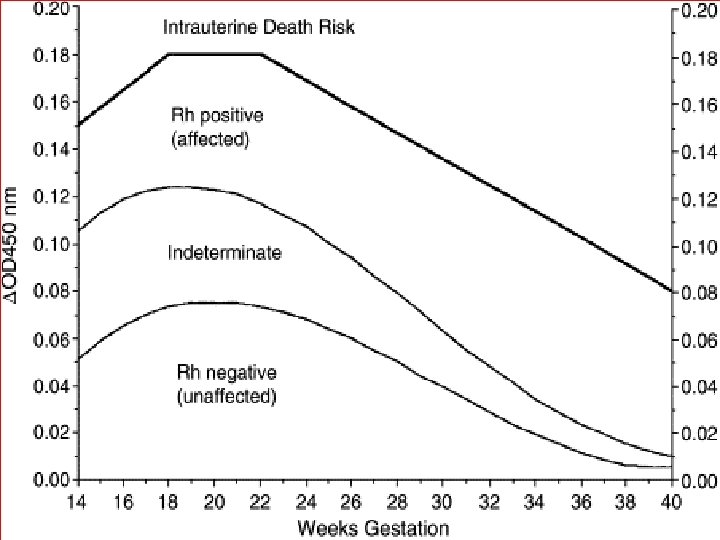
Queenan curve (Deviation in amniotic fluid optical density at a wavelength of 450 nm in Rh-immunized pregnancies from 14 to 40 weeks' gestation)

Zone 1 →fetus unaffected (Rh negative) or have only mild disease →repeat sampling in 2 to 3 weeks Zone 2→ if in lower part→ fetus at moderate risk→ HB level between 11 to 13 g/dl whereas in the upper part HB level between 8 to 10. 9 g/dl → repeat sampling within 1 to 2 weeks if in lower part, if in upper part delivery is indicated.

Zone 3→ severely affected fetus with HB level of less than 8 g/dl and without therapy death is predicted within 7 to 10 days immediate fetal red blood cell transfusion or delivery ACCORDING TO GESTATIONAL AGE l

Neonatal care and out come Cord blood is obtained for HB concentration measurement and direct coombs test. If the infant is anemic → initial exchange transfusion. If the infant is not anemic→ the need for transfusion is determined by the rate of increase in bilirubin concentration, the maturity of the infant and the presence of other complication.

Clinical management of the sensitized patient With serial sampling we either get: -Falling OD 450 values fetus Rhnegative if mildly affected: NO intervention is required !

-if the OD 450 is either stable or rising serial sampling is required. -If the OD 450 enters zone II or III -AFTER 34 weeks determination of lung maturity delivery -BEFORE 34 weeks delivery is best avoided intrauterine transfusion is recommended.

Intrauterine Transfusion -The goal is to transfuse fresh group O, Rhnegative packed RBCs. -The blood for transfusion require; -routine blood screening. -irradiation. - washing and processing through leukocytepoor filter. - screen for cytomegalovirus.

-The procedure ; -The repeated transfusion are generally scheduled at 1 to 3 week interval. -The final transfusion is typically performed at 34 to 35 weeks’ gestation. - the overall survival rate following intrauterine transfusion is about 85%
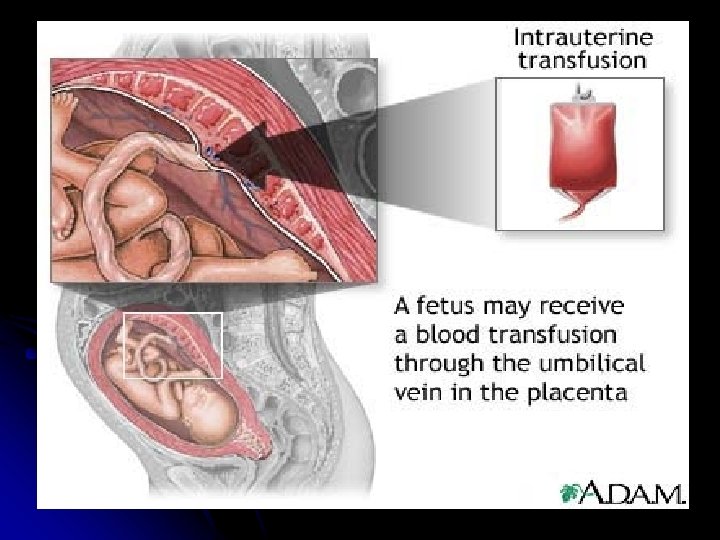

Other modes of therapy - Maternal plasmapheresis: - Phenobarbital

Prevention of Rh incompatibility -Administration of anti-D immune globulin (Rh-GAM) to Rh-negative women. -The recommended dosage is 300 mg of D-immunoglobulin at 28 wk. of gestation and following delivery (within 72 hr. ) of a D-positive infant.

Other situations might Rh-GAM be used -After induced or spontaneous abortion (50 mg less than 13 wk. of gestation , 300 mg after 13 wk. ) -Ectopic pregnancy (same dosing as for abortion) -Aminocentesis. (300 mg) -percutaneous umbilical blood sampling. -External cephalic version. -Any other case where feto-maternal hemorrhage is suspected.

THANK YOU ALL
- Slides: 54