Rh Blood Grouping Rh antigens Rh antigens were


Rh Blood Grouping

Rh antigens • Rh antigens were originally discovered in the RBCs of Rhesus Monkey- Named as ‘Rh antigens’ or ‘Rh Factor’ • Later on Rh antigens were also detected in most of the human beings • The people having Rh antigen or factor are called ‘Rh Positive’

Rhesus Blood Group System • First demonstrated by testing human blood with rabbit anti sera against red cells of Rhesus monkey & classifying Rh negative & Rh positive.

Rhesus Blood Group System • The genotype is determined by the inheritance of 3 pairs of (SIX) closely linked allelic genes situated on chromosome 9 • Six common type of Rh antigens in human beings C, D, E, c, d, & e. • Person having C cannot have c antigen • Same is true for D-d & E-e groups

Rhesus Blood Group System • The gene ‘d’ has no antigenic expression. So there are only five effective antigens. • The foetus inherits one gene from each group as a set of Cde, cde etc from each parent • Subsequently less common antigens Cw, Du, Es have also been found.

Rhesus Blood Group System • C/c & E/e are weak antigens and impractical to match. • ‘D’ antigen is by far the most immunogenic in the Rh system.

Rh antigens • Antigen D is most widely present antigen • The persons having either of C, D, E antigens are Rh Positive • The persons having either of c, d, e antigens are Rh negative

Rhesus Blood Group System • 78 genotypes are possible. Most frequent genotypes are – – Cde/cde – Cde/c. DE – c. DE/cde – cde/cde – cd. E/cde – Cde/cde (33%) (18%) (12%) (11%) (15%) (1%)

Rhesus Blood Group System • For clinical & all practical purposes it is enough to know whether one is Rh POSITIVE or NEGATIVE against anti D sera. • Rh positive 85% • Rh negative 15%

Rhesus Blood Group System • Incidence of Rh negative varies in different races: – Mongoloids- nil, – Chinese & Japanese- 1 -2%, – Indians-5%, – Africans-5 -8%, – Causcasians-15 -17% – Basques-30 -35%.

Antibodies for Rh factor • ABO system antibodies are spontaneously formed (Landsteiner law) • Anti Rh antibodies are normally not present in Rh+ or Rh – person

Formation of anti Rh- antibodies: § RBCs containing Rh factor injected into Rh Negative person. § Anti Rh antibodies develop slowly, § Maximum conc 2 to 4 months later. § Multiple exposures to Rh factor result in Rh negative person being strongly “sensitized”to Rh factor.

Characteristics of the transfusion reactions: • Rh negative never exposed to Rh positive blood—no immediate reaction. • Anti Rh antibodies formed in sufficient quantities during the next 2 -4 weeks. • Agglutination of transfused cells. • RBCs hemolyzed by the tissue macrophage system. • Mild delayed transfusion reaction occurs.

• Subsequent exposure to Rh positive blood into the Rh negative person, transfusion reaction is greatly enhanced and can be immediate and severe.

• • • Erythroblastosis Fetalis Hemolytic disease of the new born Icterus Neonatorum Rh- mother Rh+ Fetus due to Rh+ father No reaction in first pregnancy Rh+ cells of baby may enter maternal blood during labor • Mother will develop Anti D • Next pregnancy with Rh+ baby will cause the disease

Pathogenesis Rh Negative Women Man Rh positive (Homo/Hetero) Rh Neg Fetus No problem Fetus Mother previously sensitized Secondary immune response antibody (Ig. G) Fetus Haemolysis Rh positive Fetus Rh+ve R. B. C. s enter Maternal circulation Non sensitized Mother ? Primary immune response Fetus unaffected, 1 st Baby usually escapes. Mother gets sensitized?

Erythroblastosis Fetalis • Anti D cross placental barrier • Rh+ cells of baby react • Characterised by Agglutination and phagocytosis of the fetal RBCs. • Hemolysis, Hb released into blood. • Fetus macrophages convert Hb into bilirubin. ↑Bilirubin→ Jaundice.

• Severe Anemia → ↑↑Erythropoiesis → Appearance of immature, even nucleated cells (Blast cells) in the blood • Hematopoietic tissues, liver and spleen get enlarged and produce RBCs trying to replace for the hemolyzed RBCs. • Because of rapid production, early forms of RBCs including nucleated blastic forms of RBCs are released into circulation.
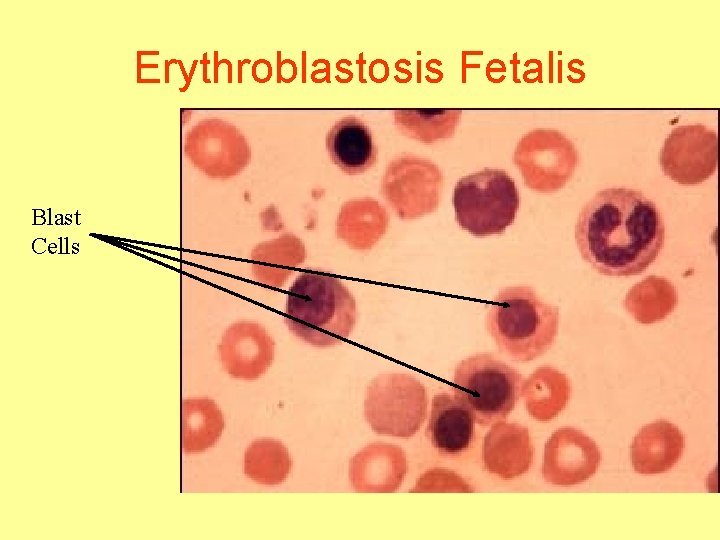
Erythroblastosis Fetalis Blast Cells

Erythroblastosis Fetalis • Death very common • Permanent mental impairment if the baby survives • Damaged motor area of brain due to precipitation of bilirubin in neurons (Kernicterus) • Exchange transfusion with Rh- blood just after birth is the only treatment • Prevention- Injection of anti D antibody to Rhmother in the first gestation after delivery for immediate destruction of Rh+ cells of the baby

Treatment of erythroblastosis fetalis: EXCHANGE TRANSFUSION: • 400 ml of Rh negative blood is infused over a period of 1. 5 or more hours while the neonate’s own Rh positive blood is being removed. • This is done several times to keep bilirubin level low and prevent kernicterus. • By the time these transfused Rh negative cells are replaced by infant’s own Rh positive cells (6 weeks), anti Rh antibodies

that have come from the mother have been destroyed.
Prevention • Rho. GAM® • Contains Ig. G anti-D (anti-Rh) • Prevents Rh immunization • Manufactured from human plasma that contains anti-D • A single 300 mcg dose will suppress the immune response to 15 ml of Rhpositive RBCs (approx 30 m. L whole blood)

Mechanism of Action • Suppresses the immune response of Rhnegative individuals to Rh-positive RBC’s • Is not effective once Rh immunization has occurred

Prevention of Rh Incompatibility • Premarital counseling? • Proper matching of blood in transfusions particularly in women before childbearing. • Blood grouping must for every woman, before 1 st pregnancy. • On exposure to Rh +ve Blood Anti Rh Immunoglobulin should be given as early as possible • Proper management of unsensitised Rh negative pregnancies.

POSSIBLE MECHANISM OF ACTION OF ANTI –D ANTIBODY: Anti-D antibody attaches to D antigen sites on Rh positive fetal red blood cells that may cross the placenta and enter the mother’s circulation thereby interfering with the immune response to the D antigen.
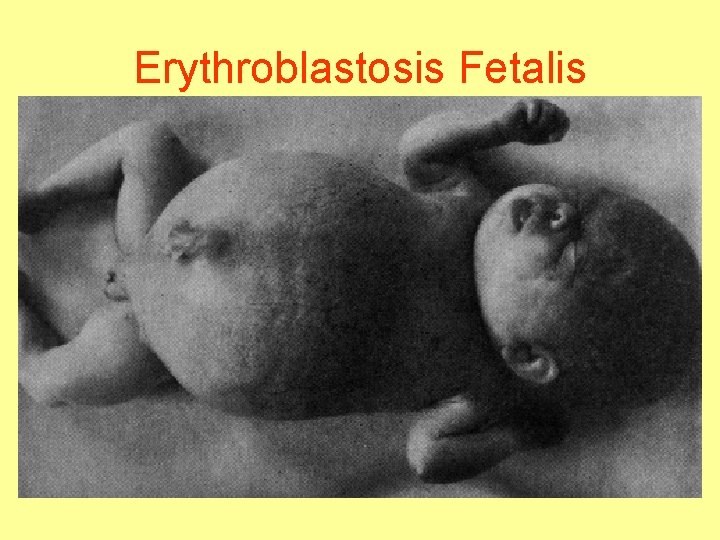
Erythroblastosis Fetalis

Thank-you Questions ? ?
- Slides: 29