Revisited imaging findings and pathophysiology of abusive head

Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (e. Ed. E-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki, T. Moritani *islam-elhelf@uiowa. edu

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma Disclosures: § The authors having no disclosures.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma Purpose: § To provide an update on the pathophysiology and MRI findings of abusive head trauma (AHT), with emphasis on diffusion imaging. Approach: § We conducted literature review of recent publications regarding AHT, focusing on pathophysiology and imaging findings. We then reviewed our institutional database for representative cases. § This presentation is divided into four main sections: First, we explain the mechanisms of AHT. Second, we give an update about pathophysiology of AHT. Third, we discuss the imaging findings of AHT. Finally, we focus on the important role of DWI in AHT.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 1 - Mechanisms of AHT: § It is important to understand the mechanisms of trauma associated with AHT. This helps to understand the pathophysiology of intracranial injuries. § Common mechanisms of AHT include: 1. Blunt impact. 2. Shaking injury 3. Whiplash injury. 4. Manual strangulation. 5. Stabbing injury.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 1 - Mechanisms of AHT: • Blunt impact: § Refers to localized dynamic force delivered at a point of time. This is also known as impact loading (Fig. 1). § Injuries commonly seen with this kind of trauma include skull fractures (with or without scalp hematoma), cerebral contusions and extra-axial bleeding. • Shaking injury: § Refers to the kind of trauma when the child is grasped from the chest and shacked vigorously. This results in transmitted impulsive force to the baby's head causing linear and rotational shear forces on intracranial contents. This is also known as impulsive loading (Fig. 2). § Injuries commonly associated include subdural hemorrhage, retinal hemorrhage, DAI and parenchymal tears.

Fig. 1: Impact loading Fig. 2: Impulsive loading http: //drjosephtm. blogspot. com/2015/04/head-injuries-part-1 -general-principles. html https: //www. youtube. com/watch? v=dlvpyuke. WVM

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 1 - Mechanisms of AHT: • Whiplash injury: § Refers to injury at the cranio-cervical junction as a result of shaking. The weak soft tissue neck support, combined with relative large sized head, causes impulsive forces to be easily transmitted from torso to the skull. The cranio-cervical junction acts as a fulcrum of motion and is exposed to significant impulsive forces (Fig. 3). § This leads to spinal cord and soft tissue injuries at the cranio-cervical junction (1, 67). • Manual Strangulation: § This causes acute compromise of carotid blood flow resulting in brain ischemia and HII pattern. Hemorrhagic laminar necrosis has been reported 7 -10 days after strangulation. • Stabbing injury: § This is less common mechanism of AHT. This usually results in serious brain injury with characteristic injuries like carotid-cavernous fistula and infection.
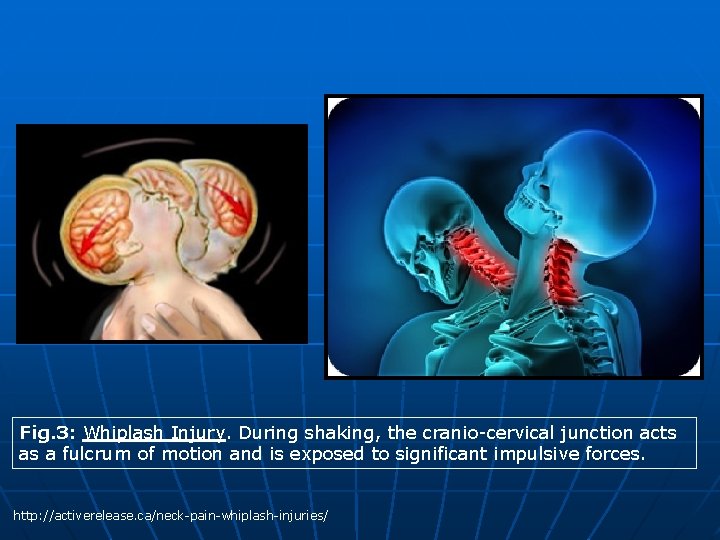
Fig. 3: Whiplash Injury. During shaking, the cranio-cervical junction acts as a fulcrum of motion and is exposed to significant impulsive forces. http: //activerelease. ca/neck-pain-whiplash-injuries/

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT: Injury patterns associated with AHT are usually classified into primary and secondary injuries. § Primary injuries occur at the time of trauma and are directly related to the impact. This includes extra-axial bleeding, cerebral contusions/clefts, cranio-cervical injury, retinal hemorrhage and skull fracture § Secondary injuries develop over time as a result of sequential biochemical and physiological cascades in response to primary brain injury. This includes hypoxic ischemic injury (HII) and diffuse axonal Injury (DAI).

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT: • Extra-axial bleeding/ fluid collections: § Subdural hematoma (SDH) is the most common encountered imaging findings in AHT. When SDH is seen in association with retinal hemorrhage and parenchyma injury the specificity for AHT is notably increased. § A well established theory to explain SDH in the setting of AHT is rupture of the bridging veins in the subdural space due to shear forces. This is more pronounced with impulsive loading. The infants' brain is relatively soft and small with prominent extra-axial CSF space. This causes increased brain shaking within the skull exposing bridging veins to significant shear forces. § Some recent studies proposed additional theories to explain SDH in AHT. In these studies, bridging vein thrombosis was demonstrated in approximately 45% of SDH cases. Some other studies attributes SDH to rupture of an intradural vascular plexus that was found to be prominent in young children.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT: • Extra-axial bleeding/ fluid collections: § Subdural hygromas may also be associated with AHT, and it is commonly confused with SDH in the setting of AHT. Hygromas may develop acutely as a result of meningeal tear or CSF transudation secondary to acute SDH. Hygromas may also reflect expected evolution of chronic SDH. § Epidural and subarachnoid hemorrhage (SAH) can also be seen, however they are less associated with AHT compared to SDH. SAH is caused by tearing of tiny vessels in the arachnoid space. § It 's noteworthy to mention that specific anatomic features in infants’ brain decrease the risk of epidural hematoma compared to adults. In infants, the inner table groove for the middle meningeal artery is less prominent allowing for some mobility of the artery, and the pediatric durra is more firmly adherent to the calvarial bone as well.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT: • Cerebral contusions/Contusional clefts: § Cerebral contusions usually develop due to transmitted forces to the cerebral mantle on impact loading (Fig. 4). Contusions may be less common than in adults due to the fact that the skull inner table is more smooth than in adults, and the brain tissue in children is more viscous due to increased water content. § Contusional clefts, also known as parenchymal lacerations, usually develop at younger children and are commonly related to impulsive loading. Shear forces at the level of gray-white matter interface can result in parenchymal laceration/cleft. § Contusional clefts commonly occur in children under 6 months, however some reports showed parenchymal lacerations up to 11 months of age.

Fig. 4: Cerebral contusions. Impact loading may cause brain contusion at the impact side or on the opposite side (counter-coup). https: //userscontent 2. emaze. com/images/2 b 77 d 3 ba-8689 -4 f 7 b-a 451 -bc 23 a 2 d 64281/6 a 111 dfe 8 e 7 cd 99 effd 4217 cba 164 cc 6. png

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma: 2 - Pathophysiology of Injuries associated with AHT: • Skull Fractures: Calvarial bones in children are more pliable when compared to the more rigid adult skull. On impact injury, skull bones can deform to absorb the direct trauma. This may result in brain injury without definite fractures on imaging. However, above certain threshold the calvarium is no more able to absorb the impact force and it fractures. Growing skull fracture refers to widening of fracture lines over time. Meningeal tear result in a lepto-meningeal cyst that insinuates itself between the fracture edges. Transmitted CSF pulsations cause progressive widening of the calvarial defect. • Retinal hemorrhage (RH): RH is strongly associated with, yet not diagnostic of, AHT. Specially with impulsive loading, transmitted shear forces can result in retinal separation & hemorrhage. Another contributing factor is sudden increased intracranial venous pressure due to chest compression in shaking injury.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma: 2 - Pathophysiology of Injuries associated with AHT • Cranio-cervical Injury (CCI): § CCI is commonly encountered in the context of whiplash injury. § The younger the child the weaker the cervical muscles and ligaments will be. The weak neck support in infants causes extensive rotational movement of the relatively heavy head along the fulcrum of the cranio-cervical junction. This results in vertebral subluxation with consequent soft tissue injury but with less frequent osseous injuries. § Different injury patterns have been reported, the most common of which is ligamentous injury. However the most serious injury is cervico-medullary contusion/ axonal injury. This carries the risk of damage to brain stem respiratory centers with ensuing apnea and possible HII.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT • Hypoxic ischemic injury: § Different theories have been hypothesized to explain HII. A well accepted theory is that HII develop as a result of acute hypoxia due to apnea. Specially with whiplash mechanism of injury, cervico-medullary axonal injury develops with consequent dysfunction of the brain stem respiratory centers causing apnea. In cases of strangulation, acute compromise of the carotid arterial flow causes acute profound ischemia resulting in HII. § Another theory linked development of HII to disturbances in cerebral vascular autoregulation. The exact mechanism is unknown, however suggested explanations include exaggerated inflammatory response and increased permeability of the blood brain barrier in developing brain. These factors, together with the known low mean arterial blood pressure in infants, cause rapid deterioration of cerebral blood supply.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT • Hypoxic ischemic injury: § Unilateral HII brain pattern has been frequently reported in AHT. This is particularly observed underlying unilateral SDH. Some studies have documented altered brain metabolism in areas adjacent to SDH, raising the possibility that SDH itself may initiate, or exaggerate, some neuroexcitatory pathways that end up into HII. § Excitotoxic brain injury refers to a kind of brain response to injurious events (e. g: Trauma, seizures). Brain metabolism shifts form aerobic to anaerobic metabolism. This causes rapid depletion of ATP and accumulation of lactate within the pre-synaptic neurons, leading to cell membrane dysfunction and release of excitatory neurotransmitters, like glutamate. Released glutamate binds to post synaptic N-methyl-D-aspartate (NMDA) receptors (abundant in immature brains). Activation of NMDA receptors causes influx of Ca into the post-synaptic neurons and release of oxygen free radicals, like nitric oxide, that eventually lead to neuronal death. Glutamate binding to non NMDA receptors causes cytotoxic brain edema (Fig. 5).
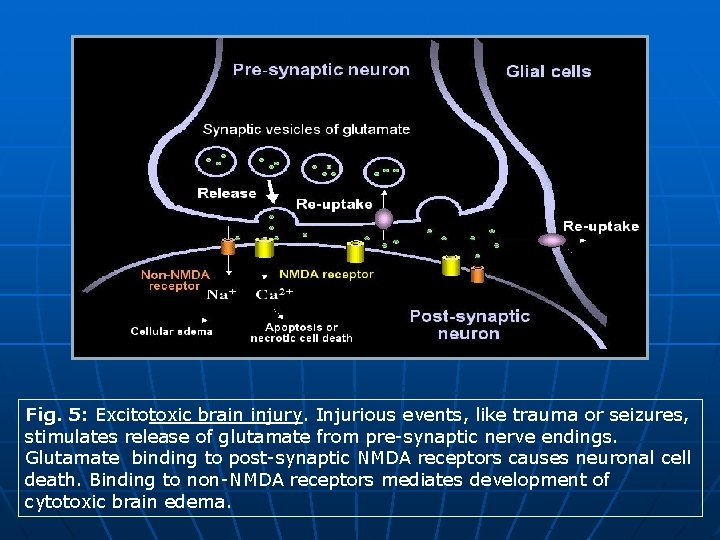
Fig. 5: Excitotoxic brain injury. Injurious events, like trauma or seizures, stimulates release of glutamate from pre-synaptic nerve endings. Glutamate binding to post-synaptic NMDA receptors causes neuronal cell death. Binding to non-NMDA receptors mediates development of cytotoxic brain edema.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 2 - Pathophysiology of Injuries associated with AHT • Diffuse axonal injury: § DAI refers to cerebral injury on the axonal level that develops in response to shaking-impact loading. DAI has been reported in a relatively older group than that of cerebral contusions/clefts. This can be explained by the changes in brain viscosity with progressive myelination. § It is known that infants' brain have increased water content and smaller axonal size compared to adults. This renders white matter axons more susceptible to micro-trauma when exposed to rotational shear forces of impulsive loading. This may trigger excitotoxic cascade due to leakage of glutamate at the node of Ranvier (Fig. 6). § Common locations of DAI include gray-white matte interface (specially frontal and para-falcine regions), corpus callosum, dorsal brain stem and internal capsule.
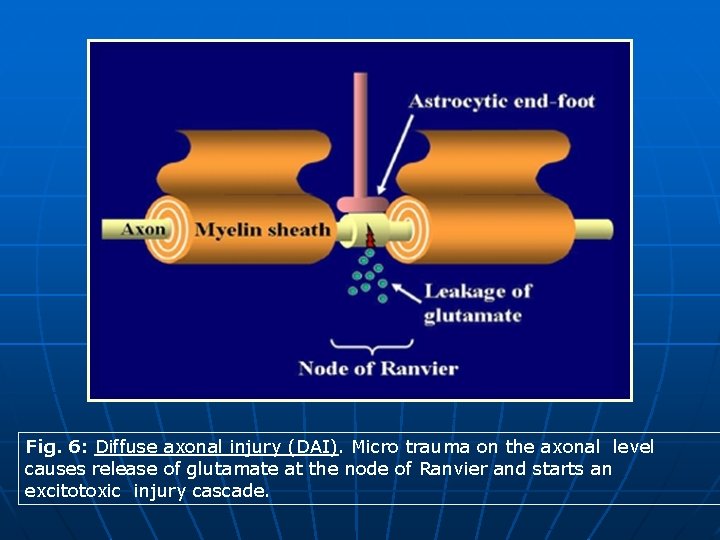
Fig. 6: Diffuse axonal injury (DAI). Micro trauma on the axonal level causes release of glutamate at the node of Ranvier and starts an excitotoxic injury cascade.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: § The only available imaging guidelines in inflicted neurotrauma was issued by the Royal College of Radiologists and the Royal College of Pediatrics and Child Abuse (RCR/RCPCA). Per these guidelines, CT and MRI are considered complimentary imaging modalities. CT scan is recommended in any child under the age of one year where there is evidence of physical abuse. § There is no single imaging finding that is considered diagnostic of AHT. Classic findings in the context of AHT secondary to impulsive loading include a triad of retinal hemorrhage, subdural hemorrhage and diffuse parenchymal injury(HII pattern). It should be noted that this triad may be characteristic, but not diagnostic, of AHT. Diagnosis of AHT usually necessitates a multi-disciplinary approach.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Extra-axial bleeding/ fluid collections : § Classically, SDH appears as a crescent shape extra-axial collection. SDH in AHT is commonly bilateral over cerebral convexities with extension along the inter-hemispheric fissure and posterior fossa but without significant mass effect (Fig. 7). § Not all subdural fluid collections are SDH. Subdural hygromas can develop in the setting of AHT in an acute or chronic setting (Fig. 8). Differentiation of SDH from hygromas can be challenging, specially on CT. Pure hygromas appear as hypodese subdural fluid collection without significant mass effect. Thus they can mimic chronic SDH. Hemato-hygromas appear on CT as subdural fluid collection with different densities mimicking the appearance of acute on top of chronic SDH. § On MRI, signal changes of SDH is usually altered due to mixing with the high oxygen content CSF in infants. Chronic SDH may not show the hypointense T 1 and T 2 signal characteristic of hemosiderin due to the paucity of phagocytes in the subdural space.
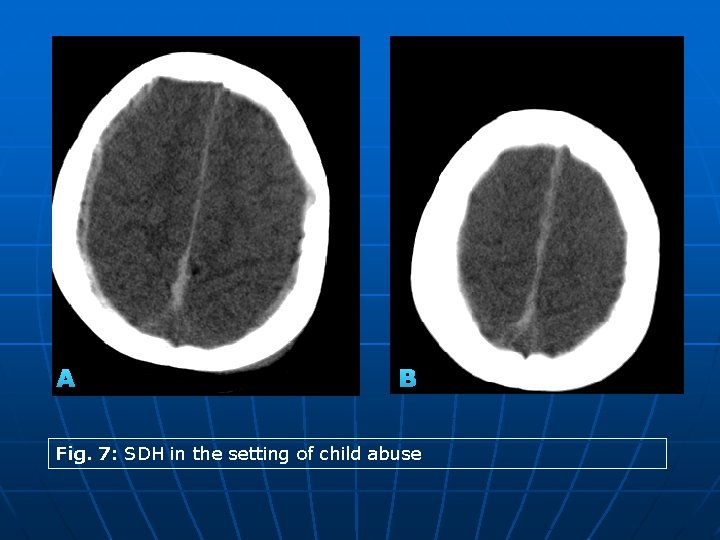
A B Fig. 7: SDH in the setting of child abuse

A B C Fig. 8: Development of acute subdural hygroma. (A) On arrival, (B) and (C) at 8 h and 24 h, respectively.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Extra-axial bleeding/ fluid collections: § As SDH evolves, it shows a layering sediment level at its dependent part. The upper serous fraction of the collection can elicit a signal close to simple fluid, like in hygromas (Fig. 9). It is always recommended to look for the dependent portion of any subdural fluid collection. Identification of blood signal within the dependent part implies that this collection is not a simple hygroma. § Hygromas can appear as simple collections in the acute phase, however as they evolve they tend to loculate and develop enhancing neomembranes along the outer followed by inner margin. Hematohygromas show blood component from acute bleeding, however identifying enhancing neomembranes (develop within 10 -21 days after injury) indicate chronic nature. § Classic imaging appearance of epidural hematoma is lentifom extra-axial bleeding usually seen near calvarial fracture. SAH appears as blood smearing the cortical sulci and basal cisterns. FLAIR sequence is highly sensitive for detection of SAH compared to conventional T 2 imaging (Fig. 10).
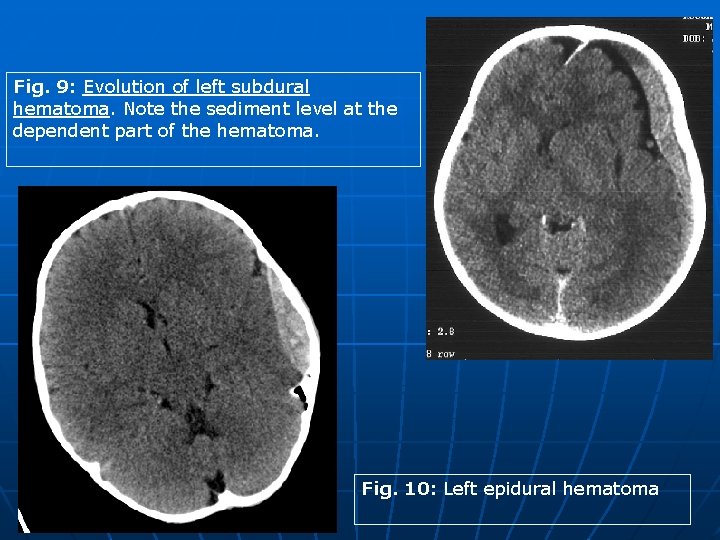
Fig. 9: Evolution of left subdural hematoma. Note the sediment level at the dependent part of the hematoma. Fig. 10: Left epidural hematoma

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Cerebral contusions/ Contusional clefts: § Non hemorrhagic cerebral contusions usually appear as focal areas of hypodensity. However, this is difficult to detect in the relatively hypodense brain parenchymal in young children. Hemorrhagic contusions are seen as focal areas of hyperdense bleeding , usually cortical in location and adjacent to skull fractures (Fig. 11). § On MRI imaging, non hemorrhagic contusions may be difficult to detect on T 2 WI due to increased brain water content. On FLAIR sequence, these lesions can show subtle high signal intensity. DWI may show restricted diffusion due to focal cytotoxic edema. Contusional clefts appear as linear abnormal signal at the gray white matter interface that may extend to the cortex. Common locations are the frontal and temporal lobes. Contusional clefts are commonly hemorrhagic resulting in a sedimentation level at their dependent extension. This is seen on MRI as a dependent blood signal within the cleft, most appreciated on GRE and SWI sequences (Fig. 12).
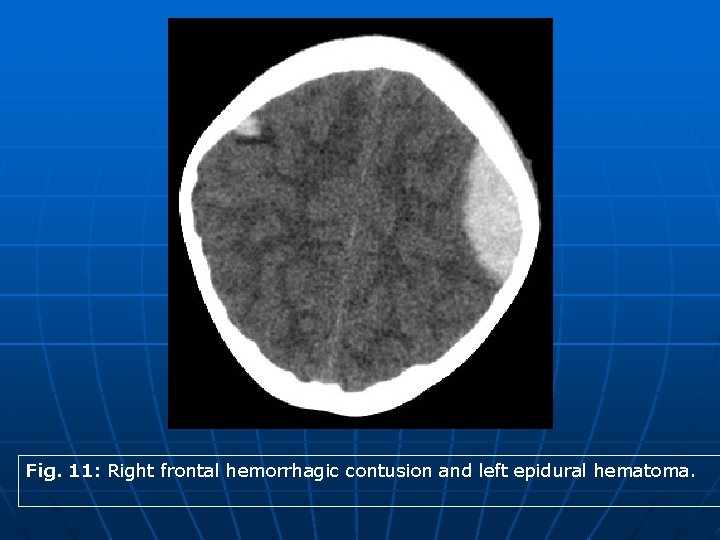
Fig. 11: Right frontal hemorrhagic contusion and left epidural hematoma.
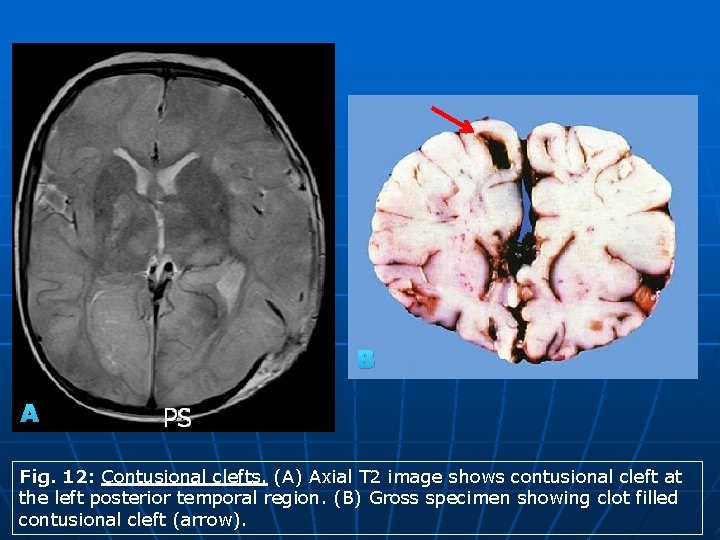
B A Fig. 12: Contusional clefts. (A) Axial T 2 image shows contusional cleft at the left posterior temporal region. (B) Gross specimen showing clot filled contusional cleft (arrow).

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Skull fractures: § Diastatic and complex depressed fractures are suspicious of AHT specially in absence of clinical history of high impact trauma. Common locations are parietal and occipital bones (Fig. 13). § CT is sensitive for detection of skull fractures, specially non-displaced fissure fractures. 3 D reformatted images and volume rendering should be routinely used to avoid missing fractures and to evaluate the full extent of calvarial injury. • Retinal hemorrhage: § On CT, RH appears as hyperdense signal in the posterior globe. If retinal detachment is evident, it shows as folded membranes in the posterior globe that converge posteriorly towards the optic disc and are limited anteriorly by the ora serrata. § MRI shows the same features as CT. GRE (T 2*) and SWI sequences have the highest sensitivity for detection of RH.
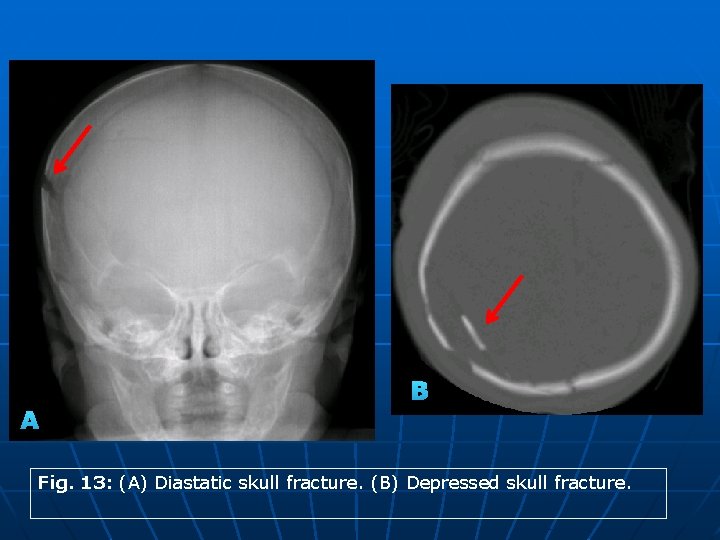
B A Fig. 13: (A) Diastatic skull fracture. (B) Depressed skull fracture.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Cranio-cervical injury (CCI): § MRI is superior for evaluation of cord contusions and ligamentous injuries in addition to extra-axial spinal bleed. Fat saturation sequences, like STIR sequence, significantly increases detection of CCI. Most common detected CCI is ligamentous injury. This shows as abnormal high T 2 and STIR signal along known anatomical course of cervical ligaments. § Another finding in the context of CCI is retro-clival hematoma, reported in about third of cases with AHT. Retro-clival epidural hematoma appears as blood intensity anterior to the tectorial membrane. § Cervico-medullary injury can happen without corresponding osseous abnormality. This is particularly true in the first year of life, and is known as spinal cord injury without osseous abnormalities (SCIWORA).

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Hypoxic ischemic injury (HII) : § CT scan is not sensitive for detection of early HII and may be normal in the first 24 hours after insult. When seen on CT, HII appear as hypodense region with mass effect in the form of effacement of the cortical sulci. HII may show different patterns including bilateral (Fig 14), unilateral (Fig 15), or watershed distribution in addition to diffuse HII. § There may be early sparing of the cerebellum, brain stem and thalamus that appear relatively hyperdense (reversal sign) (Fig 14). The flax and tentorium leaflets may appear relatively hyperdense and should not be confused with subarachnoid hemorrhage (pseudo-subarachnoid hemorrhage sign). § DWI is much more sensitive for early detection and delineation of the extent HII. This appears as areas of restricted diffusion with high DWI and low ADC values. DWI shows bright signal intensity within the first 12 -24 hours after insult. The posterolateral lentiform nuclie is one of the earliest regions to show abnormal signal intensity.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Hypoxic ischemic injury (HII) : § In the next 48 hours, restricted diffusion signal progress to the typical diffuse form of HII (Fig 14). Of note, changes in DWI beak at about 3 -5 days and then "pseudonormalizes" by the end of the first week. On the other hand, hyper intense T 2 signal starts to be evident after 48 hours and becomes most evident after 7 -10 days. Thus, altered T 2 signal intensity is particularly important by the end of the first week when DWI has pseudonormalized. § Most research suggest b values of 700 -100 sec/mm 2, however some authors suggested higher b values up to 1500 sec/mm 2. § MRS is also used for diagnosis of HII (Fig 16). Common findings include reduced NAA values, elevation of lactate peaks (reflecting tissue hypoxia/ischemia), and elevated glutamine-glutamate peak (reflecting excitotoxic release of glutamate). NAA is usually normal in the first 48 hours following acute HII, and normal values don't exclude HII. Voxels are usually positioned at the basal ganglia and centrum semiovale.
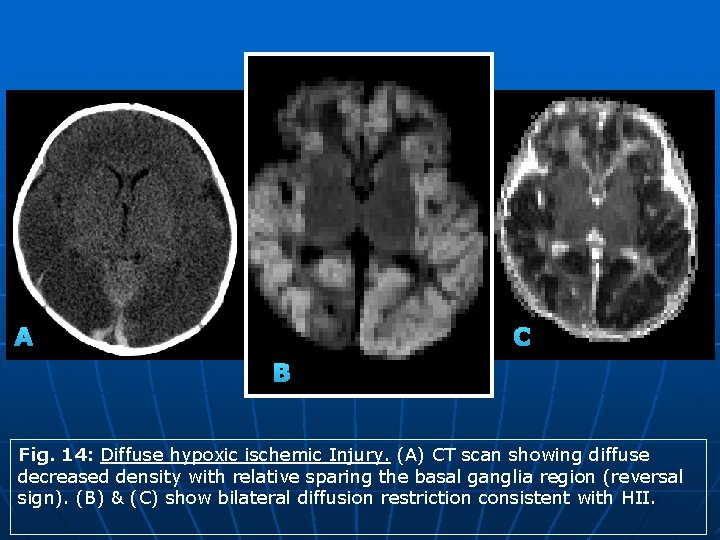
A C B Fig. 14: Diffuse hypoxic ischemic Injury. (A) CT scan showing diffuse decreased density with relative sparing the basal ganglia region (reversal sign). (B) & (C) show bilateral diffusion restriction consistent with HII.
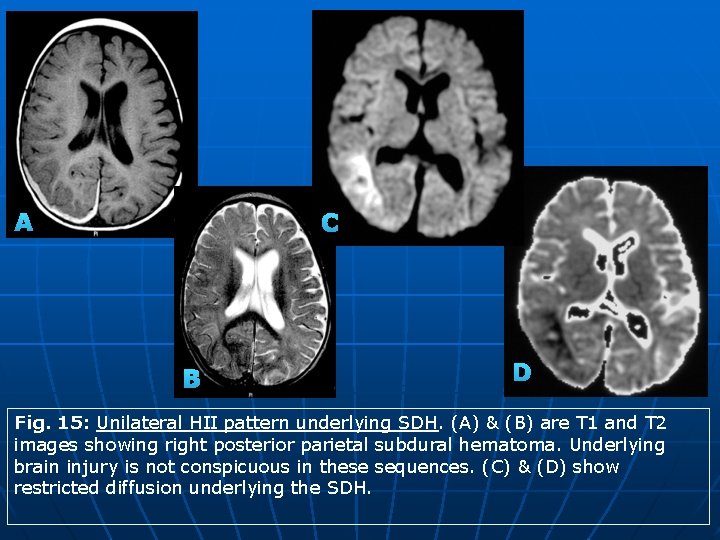
A C B D Fig. 15: Unilateral HII pattern underlying SDH. (A) & (B) are T 1 and T 2 images showing right posterior parietal subdural hematoma. Underlying brain injury is not conspicuous in these sequences. (C) & (D) show restricted diffusion underlying the SDH.
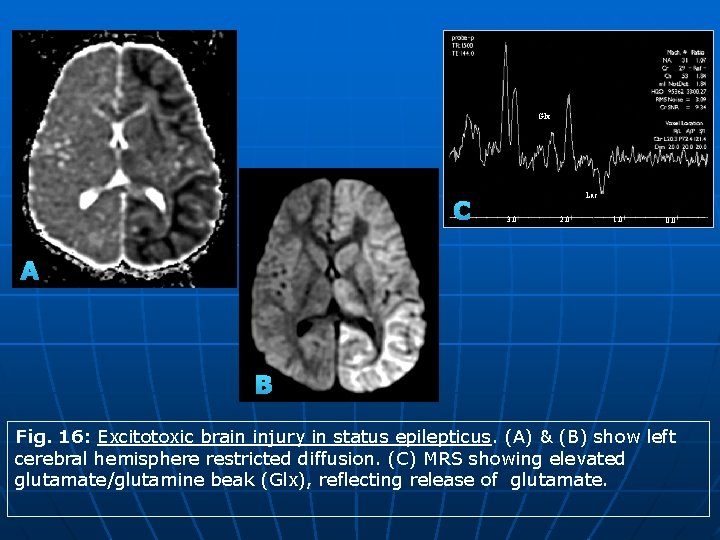
Glx C Lac 3. 0 2. 0 1. 0 0. 0 A B Fig. 16: Excitotoxic brain injury in status epilepticus. (A) & (B) show left cerebral hemisphere restricted diffusion. (C) MRS showing elevated glutamate/glutamine beak (Glx), reflecting release of glutamate.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 3 - Imaging of AHT: • Diffuse Axonal Injury (DAI): § Non hemorrhagic DAI is difficult to detect on CT. Hemorrhagic DAI appear as punctuate hyperdense hemorrhagic foci at the aforementioned characteristic locations. § MRI is more sensitive for detection of DAI. FLAIR sequence is more sensitive than T 2 signal in detection of the focal hyperintense signal of DAI. DWI is highly sensitive in detection of DAI, whether hemorrhagic or non hemorrhagic, will show restricted diffusion that reflects as hyperintense signal intensity on DWI (Fig. 18). GRE and SWI is very sensitive for detection of hemorrhagic DAI, showing blooming signal. § Diffusion-tensor imaging (DTI) can be used to assess the integrity of white matter tracts based on fractional anisotropy. Some studies showed reduced fractional anisotropy and mean diffusivity values in patients exposed to multiple subconcusive head trauma. Reduced values reflect damage to white matter tracts. These results need further validation in the setting of AHT.
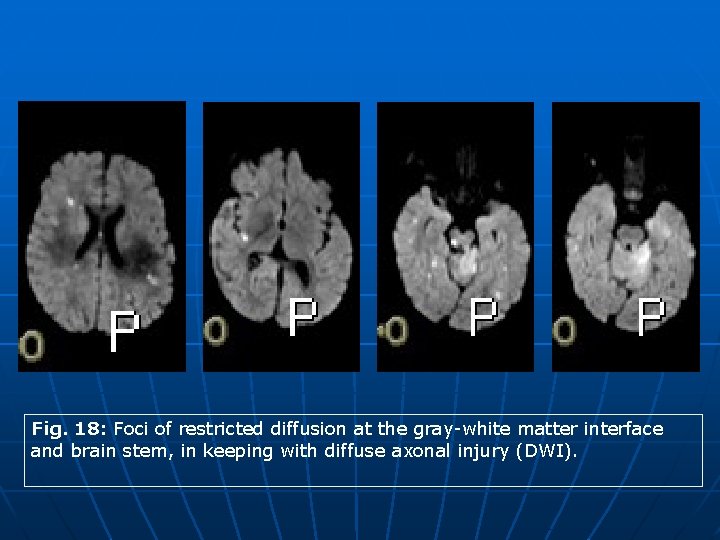
Fig. 18: Foci of restricted diffusion at the gray-white matter interface and brain stem, in keeping with diffuse axonal injury (DWI).

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 4. Role of Diffusion imaging in Abusive head trauma: § The role of DWI in non-accidental trauma is crucial, given its sensitivity for early manifestations of cytotoxic edema. DWI is probably the most sensitive and spcific imaging technique in the evaluation of brain damage in AHI. DWI can detect cytotoxic edema within few minutes of the onset of symptoms, when conventional sequences such as T 2 and FLAIR are still normal. § DWI plays an important role in determining the extent of the brain injury which correlates with the clinical outcome. Tanoue et al demonstrated that the ADC values during the acute phase of AHI are associated with poor long-term neuro developmental outcome. Bilateral posterior watershed infarcts may signify a higher risk for visual loss.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma 4. Role of Diffusion imaging in Abusive head trauma: § Diffusion Tensor Imaging (DTI) can be used to detect microstructural white matter abnormalities in the setting of AHI. Metrics such as mean diffusivity, axial diffusivity, and radial diffusivity, and fractional anisotropy can be calculated from DTI. § Children affected by abuse frequently experience significant psychiatric sequelae, such as PTSD. It was found that children affected by abuse have reduced FA in the medial and posterior regions of the corpus callosum. The proposed mechanism is reduced myelination or subtle change in the axonal structure. The corpus callosum is known to have projections from brain parts responsible for emotional and memory processing, such as those experienced with abuse.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma Conclusion: § Neuroradiology plays an important role in evaluation of AHT. Recent research links imaging findings to the more detailed diagnosis and clinical outcomes of AHT. Neuroradiologists need to be familiar with imaging findings of AHT and prognostic imaging features when caring for these patients. § DWI is sensitive for detection of most imaging findings associated with AHI. DWI better delineates the extent of brain injury and can have an important prognostic value when evaluating possible consequences of AHT.

Revisited Imaging Findings and Pathophysiology of Abusive Head Trauma Selected references: n n n n Utsunomiya H. Diffusion MRI abnormalities in pediatric neurological disorders. Brain Dev. 2011; 33 : 235 -42. K. N. Aida and K. Matsui. Apparent diffusion coefficient values predict outcomes of abusive head trauma. Acta Paediatr. 2013; 102: 805 -8. Zimmerman R. A. , L. T. Bilaniuk, and L. Farina. Non-accidental brain trauma in infants: diffusion imaging, contributions to understanding the injury process. J Neuroradiol. 2007; 34 : 109 -14. Hsieh KL, Zimmerman RA, Kao HW, et al. Revisiting neuroimaging of abusive head trauma in infants and young children. AJR 2015; 2014: 944 -52. Dremmen MH, Huisman TA. Non-accidental injury of the pediatric central nervous system. In: Diseases of the brain, head and neck, spine 2016 -2017. Springer International Publishing; 2016: 307 -16. Nixon JN, Soares BP. Imaging of Abusive Head Trauma: A Review and Update. Curr Radiol Rep http: //dx. doi. org/10. 1007/s 40134 -015 -0136 -6. Pfeifer CM, Hammer MR, Mangona KL, et al. Non-accidental trauma: The role of radiology. Emerg Radiol. 2016 Nov 10. [Epub ahead of print] Huang BY, Castillo M. Hypoxic-ischemic brain injury: Imaging findings from birth to adulthood. Radiographics. 2008 ; 28 : 417 -39.

- Slides: 44