Revised 2015 Anemia Iron Deficiency Sickle Cell Anemia

















































![(From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles (From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles](https://slidetodoc.com/presentation_image/28add244b88aee85be26417e74622045/image-55.jpg)
















![(From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles (From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles](https://slidetodoc.com/presentation_image/28add244b88aee85be26417e74622045/image-76.jpg)








![(From Wong, D. L. [1997]. Whaley & Wong's essentials of pediatric nursing. [5 th (From Wong, D. L. [1997]. Whaley & Wong's essentials of pediatric nursing. [5 th](https://slidetodoc.com/presentation_image/28add244b88aee85be26417e74622045/image-88.jpg)





















- Slides: 109

Revised 2015

Anemia (Iron Deficiency) Sickle Cell Anemia Hemophilia ALL ( Acute Lymphobalstic Leukemia)

Insufficient dietary iron Maternal stored depleted at 6 mo. Inadequate iron intake

Hgb 6 -10 Irritability, weakness, decreased play activity Fatique Hgb <5 Anorexia Pale tachycardic

Iron replacement – ferrous sulfate Give with straw or syringe ^ citrus fruits or juices

Dietary instruction Teaching of long term complications of anemia Dark, tarry stools

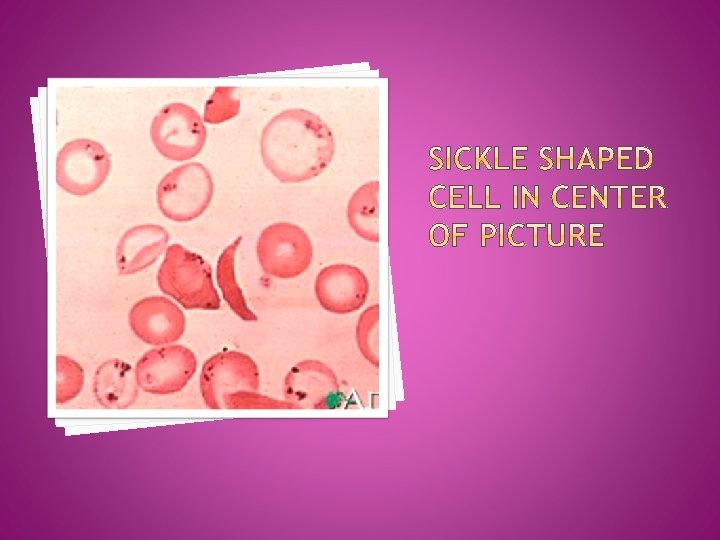
Inherited African-American / Mediteranian No cure

Sickling: Clumping of abnormal shaped cells Results in obstruction w/ severe tissue hypoxia

Severe sickling can lead to sickle cell crisis, an acutely painful period that occurs intermittent throughout life.

Infection Dehydration Cold Emotional stress

Hydration Analgesics O 2 Warm baths, local heat Avoid precipitating factors

Hemophilia Inherited – X linked Lack clotting factors: Factor VIII or Factor IX

Bleeding, bruising Hemarthrosis Bone deformities, contractures Hematomas Diag test: PTT

Replace clotting factors

What are your nrsg interventions? What is RICE? What are s/s of intracranial bleed?

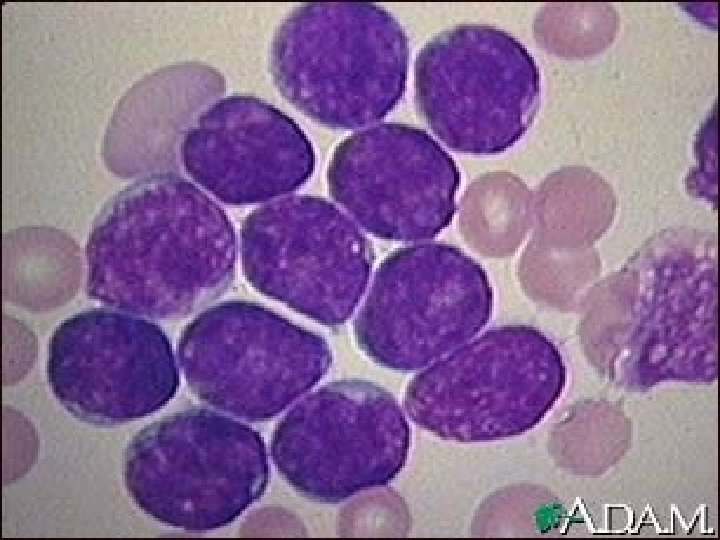
Acute Lymphoblastic Leukemia Most commom malignancy in children, ^ males Increased blast cells Decreased rbc’s and platelets Internal organs enlarge


Chemo & steroids Intrathecal drugs Goal is remission

Pallor, fatigue Fever, ^ infections Bleeding, bone pain Limping s/s of ICP

Monitor s/s infection & reduce risk Oral care Enc. Nutrition

AIDS RHEUMATOID ARTHRITIS

Chronic, usually fatal Perinatal infection, 91% Blood & bodily fluids Sexual abuse Adolescents have ^ risk d/t risky behaviors

Keep viral load low Prev. infections Restore normal G & D Improve quality of life Box 31 -2 drugs

Prevent infection Nutrition / meds Family support

Chronic inflammatory autoimmune connective tissue disease Destroys cartilage, affects joints & tissues Occuring bet. 1 -3 & 8 -10 yrs old

Stiffness, edema Loss of motion Warm to touch Increase temp Macula rash

Clinical findings No specific tests ESR X-rays

Preserve joint function NSAIDS DMARDS Moist heat - PT

Manage pain, educate Support groups to express fears & concerns Balance rest/exercise

Acute respiratory infections are common in infancts & children. They range from minor to life threatening illnesses.

Lack surfactant to keep lungs expanded Gestational age at birth influences severity #1 s/s respiratory distress

Exogenous Surfactant O 2 therapy Parenteral therapy

Inflammation of lung tissue Common cause RSV Viral more common than bacterial

See Box 31 -3 Dx x-ray Tx O 2, fluids, nebulizers, antx if bacterial cause

Resp & CV assessmt Infection control Hydration, IV fluids O 2 & antx as ordered

No cause Occurs during sleep 3 rd leading cau of death betw. 2 -4 mos. Diagnosed on autopsy

Family grief support Allay feelings of guilt and blame Teach “back to sleep”

“sore throat” 80% viral 20% strep H-influenza in children , 3 yrs s/s: Fever Sore throat White exudate

S/S same as pharyngitis Treatment : 1)Same as pharyngitis 2) Tonsillectomy

Pre-op Notify MD of temp Post-op Monitor for bleeding, no straws, analgesics

Acute viral disease marked by resonant barking cough, difficult breathing & laryngeal spasm.

LTB = most common form of Croup Follows an URI s/s: barking cough, tachypnea retractions

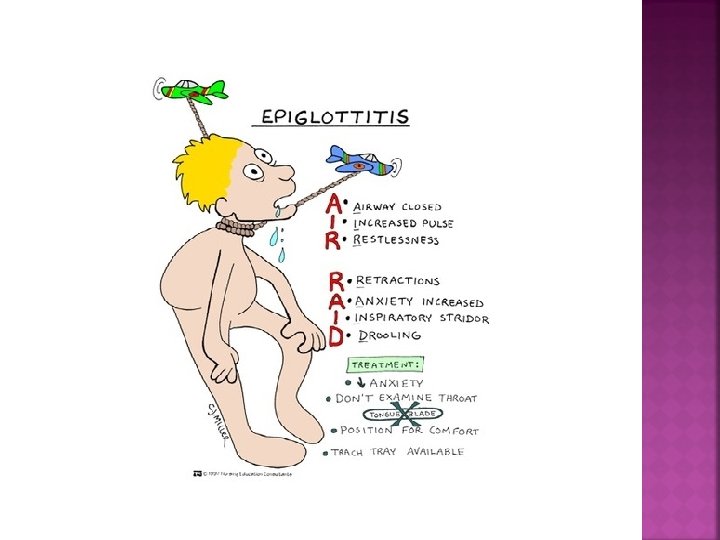
Cause: H influenzae bacteria Life threatening airway obstruction


Drooling High Fever Resp distress Muffled voice Progressive resp. distress Anxiety Fear

Check for the 4 “D’s” 1) Drooling 2) Dyspnea 3) Dysphonia 4) Dysphagia

Maintain airway Cool mist NPO – IV fluids Epinephrine, Antx

^ HOB Assess resp. status Freq. VS Trach tray @ bedside

Usually viral s/s: same as with URI + cough Common during winter months Children < 4 y. o.

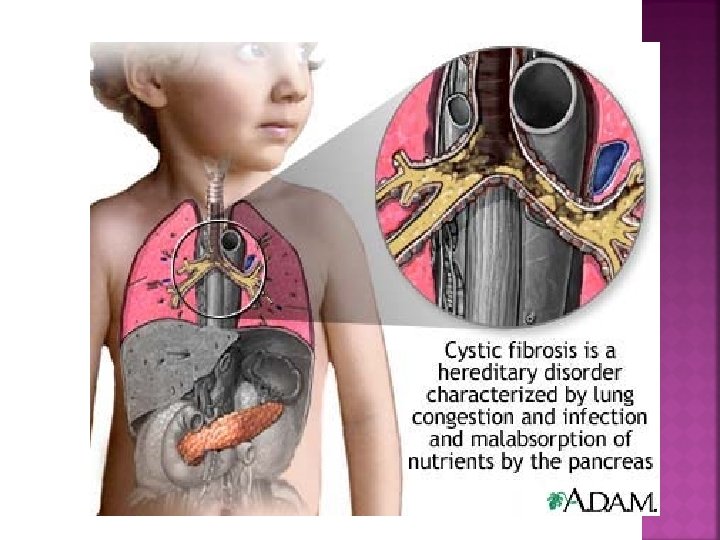
Inherited, No defective gene cure Excessive thick mucus produced Obstructs lungs & GI system


steatorrhea Barrel chest Increased Na. Cl in sweat & saliva

^ nutrition Pancreatic enzymes CPT / postural drainage

Common chronic childhood illness Obstructive resp. disorder, familial tendency
![From Ashwill J W Droske S C 1997 Nursing care of children principles (From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles](https://slidetodoc.com/presentation_image/28add244b88aee85be26417e74622045/image-55.jpg)
(From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles and practice. Philadelphia: Saunders. ) Comparison of a normal bronchial tube and a bronchial tube during an asthma episode.

Bronchospasm Bronchial edema s/s: SOB Expiratory wheeze

Quick relief meds Long term meds Allergen testing

^HOB Meds, hydration Rest, breathing exercises Avoid triggers Teach self-care

An 8 -year-old child has a history of asthma and lives with her mother and younger sister. In assessing the home environment, the nurse learns that the family lives in a townhouse and has one cat and two dogs. The mother smokes two packs of cigarettes a day, the child shares a room with her younger sister, and the house is carpeted. How could the mother modify the home environment to better control her daughter’s asthma?

Any alteration in GI function has the potential to affect other bodily systems.

Facial malformation during fetal development Assoc. w/ folic acid deficiency, ETOH & smoking

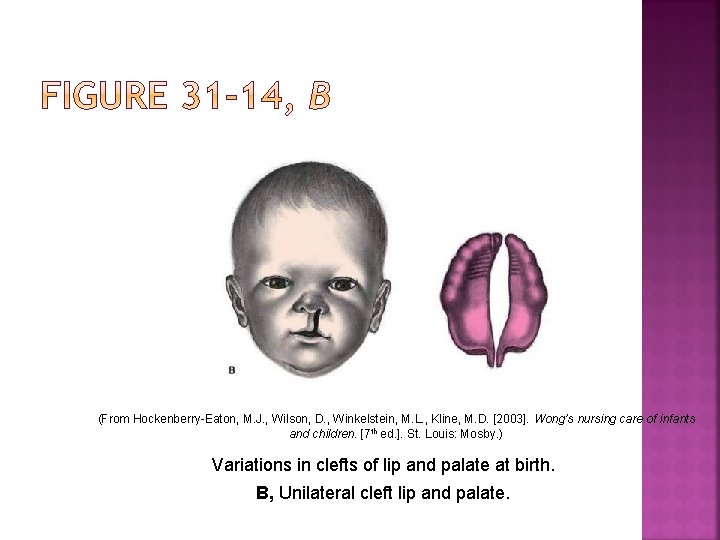
(From Hockenberry-Eaton, M. J. , Wilson, D. , Winkelstein, M. L. , Kline, M. D. [2003]. Wong’s nursing care of infants and children. [7 th ed. ]. St. Louis: Mosby. ) Variations in clefts of lip and palate at birth. B, Unilateral cleft lip and palate.

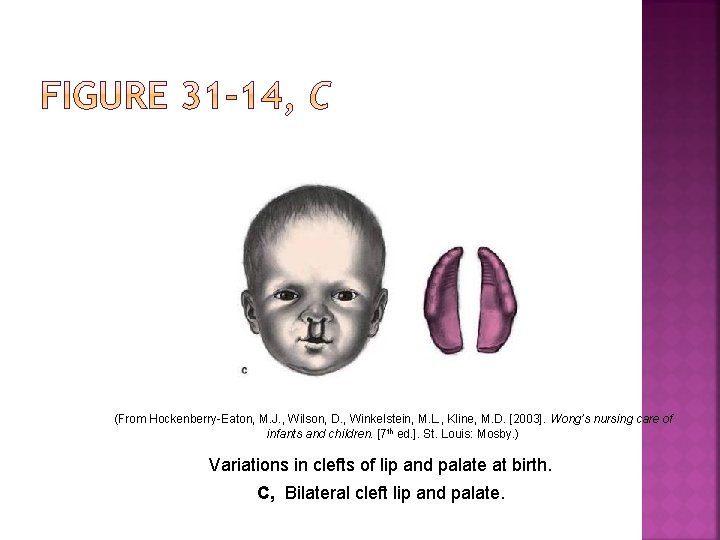
(From Hockenberry-Eaton, M. J. , Wilson, D. , Winkelstein, M. L. , Kline, M. D. [2003]. Wong’s nursing care of infants and children. [7 th ed. ]. St. Louis: Mosby. ) Variations in clefts of lip and palate at birth. C, Bilateral cleft lip and palate.

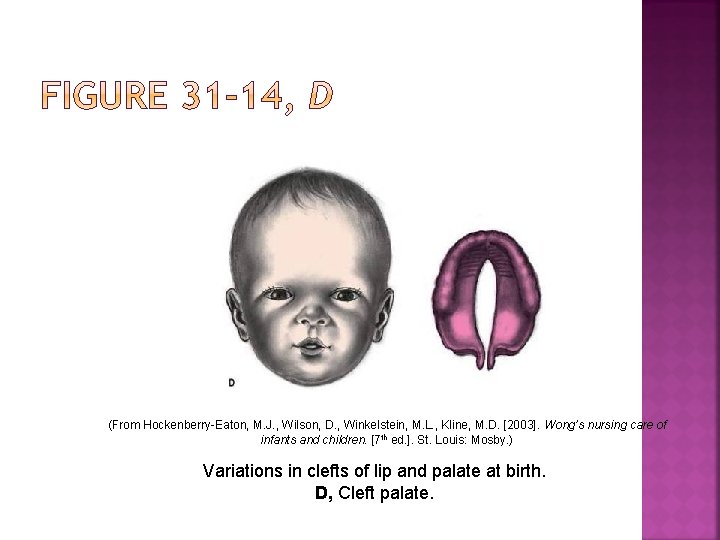
(From Hockenberry-Eaton, M. J. , Wilson, D. , Winkelstein, M. L. , Kline, M. D. [2003]. Wong’s nursing care of infants and children. [7 th ed. ]. St. Louis: Mosby. ) Variations in clefts of lip and palate at birth. D, Cleft palate.

Cleft lip little feeding diff. Extensive cleft lip & palate dif. Feeding & speech

Lip repaired at 1 -2 mo. Palate repaired by 1 yr. Multidisciplinary hlth care approach

Parental support Assistive feeding devices ESSR feeding techniques Freq. burping

Maintain integrity of suture line Adv. Diet as tol Soft rubber tipped feeder, no breast Back or side lying only


Intake less then output Determined by change in wt. Infants and young children more easily effected

§Increased frequency, fluid content & volume of stools

Treat cause Restore fluids and electrolytes Modified BRAT diet, Pedialyte, Rehydralyte, Infalyte

I&O Infection control Nutrition, rehydrate Daily weights

Passage of hard infrequent stool Structural disorders Diet, meds Repressed urge to defecate

Hypertrophied pyloric muscle obstructs gastric outlet Unknown etiology Fig. 31 -16 pg. 1022
![From Ashwill J W Droske S C 1997 Nursing care of children principles (From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles](https://slidetodoc.com/presentation_image/28add244b88aee85be26417e74622045/image-76.jpg)
(From Ashwill, J. W. , Droske, S. C. [1997]. Nursing care of children: principles and practice. Philadelphia: Saunders. ) Comparison of normal pyloric opening with evidence of pyloric stenosis.

Projectile vomiting Olive shaped mass, R. abd Wt loss, poor skin turgor dehydration

Pyloromyotomy ( Fredet-Ranstedt procedure)

One part of intestine telescopes into another S/S currant – jelly like stool Abd. pain

Barium enema Tx: barium enema Surgical repair

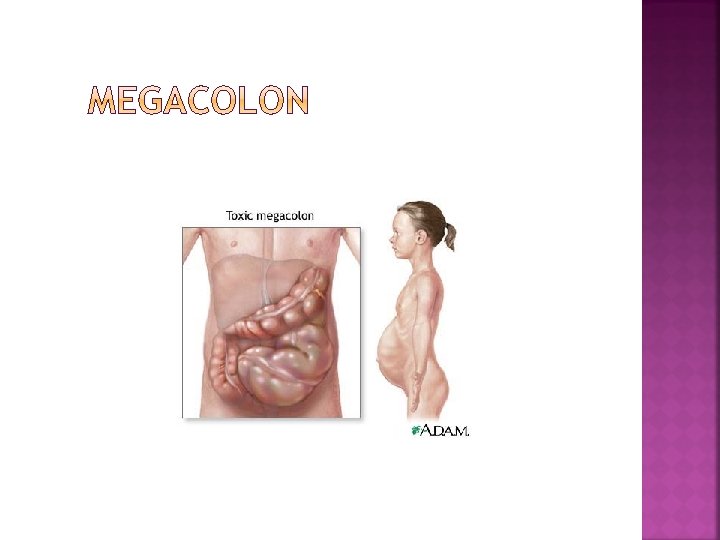
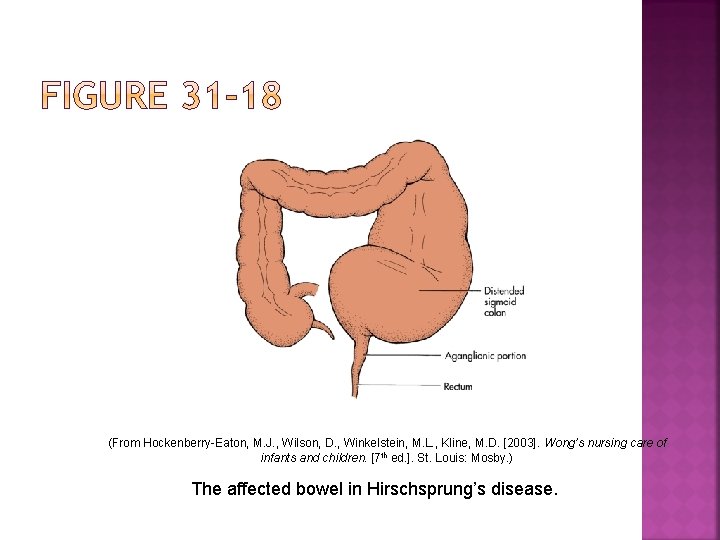
Presents as Megacolon Hirschsprung's disease is a condition that affects the large intestine (colon) and causes problems with passing stool. It's present when a baby is born (congenital) and results from missing nerve cells in the muscles of a portion of the baby's colon.


(From Hockenberry-Eaton, M. J. , Wilson, D. , Winkelstein, M. L. , Kline, M. D. [2003]. Wong’s nursing care of infants and children. [7 th ed. ]. St. Louis: Mosby. ) The affected bowel in Hirschsprung’s disease.

Temporary colostomy Endo-rectal pull through

Pre-Op Care? ? Post-Op Care ? ?

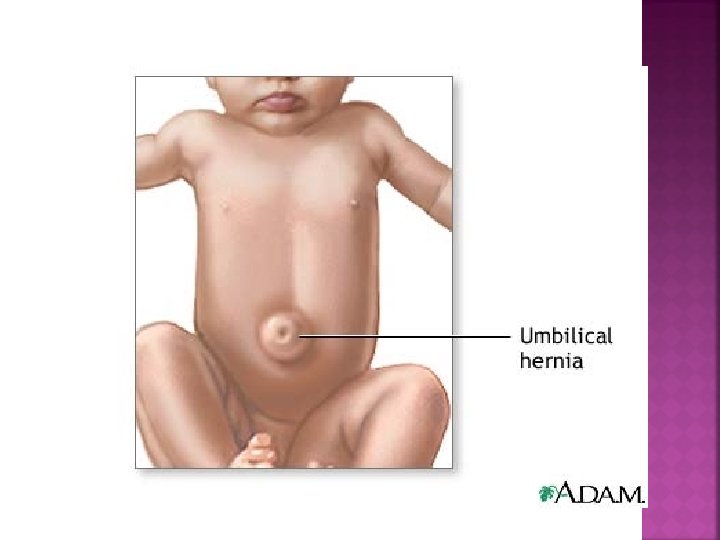
Organ protrudes through weakened muscle wall

![From Wong D L 1997 Whaley Wongs essentials of pediatric nursing 5 th (From Wong, D. L. [1997]. Whaley & Wong's essentials of pediatric nursing. [5 th](https://slidetodoc.com/presentation_image/28add244b88aee85be26417e74622045/image-88.jpg)
(From Wong, D. L. [1997]. Whaley & Wong's essentials of pediatric nursing. [5 th ed. ]. St. Louis: Mosby. ) Location of hernias.

Inflammation of appendix s/s rebound tenderness Elevated WBC Pain @ Mc. Burneys point

Regurgitation of gastric contents Vomiting/spitting up/choking/gagging Esophageal ulceration Heme. + stool

Small frequent thickened feedings Pepcid, Zantac, Tagamet Surgical repair

Disorders of the GU Syst. alter the delicate balance of fluid & electrolytes in the body and may be life threatening

Proteinuria Edema Hypoproteinemia hyperlipidemia

Peri-orbital edema Ascites Generalized edema

I&O Skin care ^pro. diet

Inflammation of glomerulus Strep is most common cause s/s proteinuria tea colored urine HTN ( idiopathic )

CRITICAL THINKING QUESTION The nurse has admitted a 7 year-old male to the pediatric unit with a diagnosis of acute glomerulonephritis. The nurse informs the mother that a urine specimen is needed and gives the patient a urinal. The mother states, “I don’t understand why he is having kidney problems. He had bronchitis a week ago and was feeling better. ” How should the nurse manage this situation?

Guidelines: The nurse should inform the mother that occasionally an upper respiratory infection can lead to acute glomerulonephritis. The nurse should explain to the mother that for her son to heal, he must have his fluids restricted, strict bed rest, and eat a balanced diet.

Bedrest Restrict fluids & Na + I&O Diuretics and antihypertensive

Most common malignant tumor of childhood Develops from immature kidney cells Prognosis greatly improved in recent decades

Large, firm, asymptomatic abd mass Do not palpate abd

Pre/post op care Family support Surgery Nephrectomy

Disorders are usually from over or under production of hormones. Can affect all aspects of body function including appearance, G & D and psychologic well being.

Lack thyroid hormones Tx. Thyroid hormone replacement

Teach parents importance of med administration to prevent cognitive & growth impairment

Type I Diabetes (IDDM) Lack of insulin TX exogenous insulin, diet & exercise

Family teaching is paramount What topics would be included in your teaching?

Question: A pediatric nurse is caring for an infant who has been diagnosed with GERD. The nurse places infant cereal into the bottle with formula for the mother to feed the infant. The mother asks why she placed cereal in the bottle when her pediatrician has instructed her not to feed the infant foods until he is 6 months of age. How should the nurse manage this situation?

Question: A 2 -month-old infant, with failure to thrive and projectile vomiting, is scheduled for surgery to repair the hypertrophic pyloric stenosis. The mother does not understand why her daughter cannot receive medication to treat this disorder. How can the nurse manage this situation?