Review of PICC Lines Kelly Mc Cormick RN

























- Slides: 31

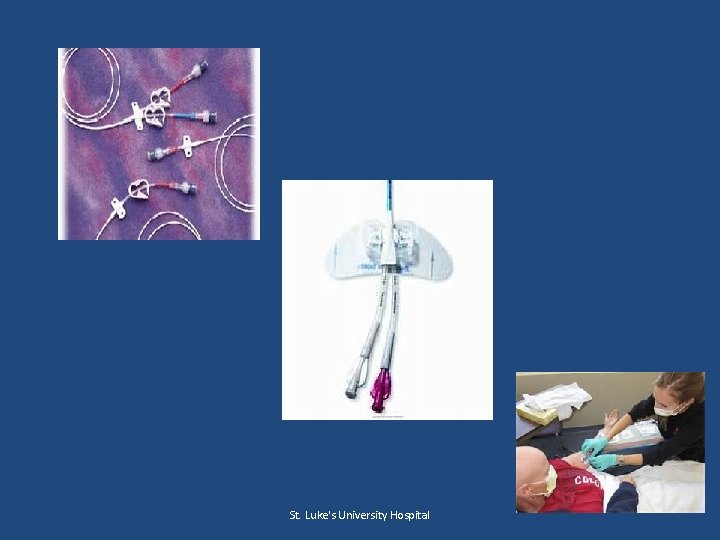
Review of PICC Lines Kelly Mc. Cormick RN, BSN, OCN Infusion/PICC Team St. Luke’s University Hospital Rev. 12 12 13 St. Luke's University Hospital

Instructions • • Before proceeding to the Posttest, be sure you have completely reviewed the following Power. Point© program. Completion of this program will award 0. 5 CE. This program is a required educational review for RNs at the Bethlehem Campus who care for patients with PICCs due to new technology available – completion is required by August 31, 2013.

Objectives The purpose of this program is to review key points related to PICC lines. At the conclusion of the program, the RN will be able to: • List the purpose of PICC lines and the medications for which they are appropriate/required. • Discuss the process for ordering a PICC insertion. • Describe the acceptable processes for confirming PICC placement. • Incorporate care and maintenance guidelines for PICCs into practice.

St. Luke's University Hospital

What are PICC Lines? PICC = Peripheral Inserted Central Catheter Reminders: • PICC lines require a physician order • Inserted at bedside or Interventional Radiology • Used in patients receiving medications where peripheral vein administration is contraindicated • May be beneficial to patients who are extremely difficult IV sticks • May be used for longer term access, can stay in place up to 1 year • Often used in the home or extended care facilities

Medications that Require Central Line Administration § Antineoplastic (chemotherapy) § TPN § Pressors ( i. e. Dopamine, Levophed) § Irritant or vesicant (i. e. Potassium - high concentration) § Long-term and/or caustic antibiotics (i. e. Vancomycin, Amphotericin B) § Any medication with a p. H below 5 or greater than 9 or osmolarity more than 600 Osm/L (i. e. Amiodarone, Ganciclovir Sodium)

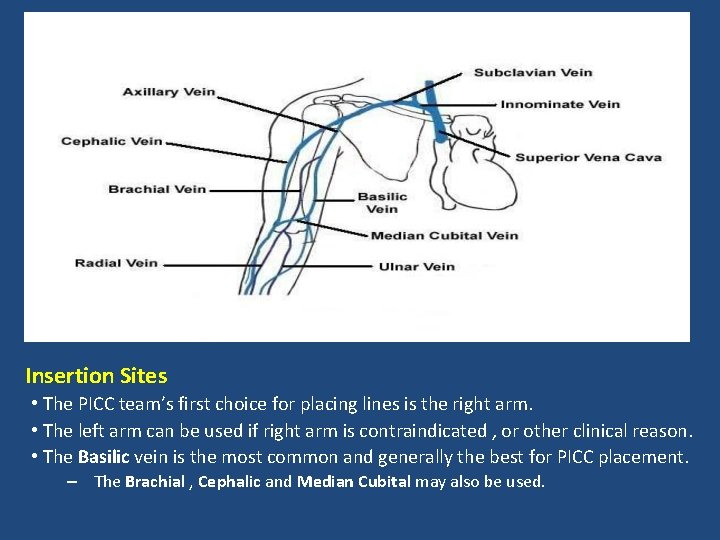
Insertion Sites • The PICC team’s first choice for placing lines is the right arm. • The left arm can be used if right arm is contraindicated , or other clinical reason. • The Basilic vein is the most common and generally the best for PICC placement. – The Brachial , Cephalic and Median Cubital may also be used.

Ordering a PICC Line PICC lines are NOT considered emergent. If a patient is unstable, alternate methods of access should be considered Refer to NPPM Peripherally Inserted Central Catheters-Insertion and Maintenance [D-28] for specific entity/campus ordering information.

PICC Questions? Questions/Problems related to PICC lines can be directed to a PICC nurse: • Allentown Campus – page the PICC Nurse • Anderson Campus – notify Interventional Radiology • Bethlehem Campus – notify the Infusion Center • Miners Campus – call the PICC Team • Quakertown Campus – call your manager/ supervisor • Warren Campus – notify Interventional Radiology

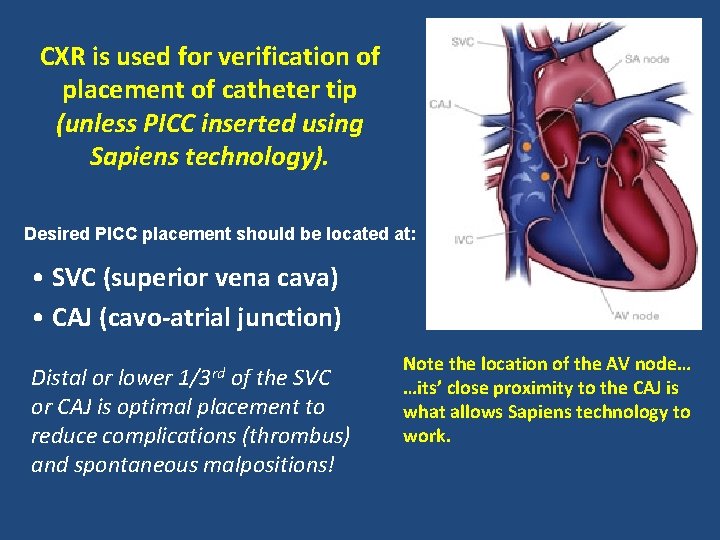
CXR is used for verification of placement of catheter tip (unless PICC inserted using Sapiens technology). Desired PICC placement should be located at: • SVC (superior vena cava) • CAJ (cavo-atrial junction) 1/3 rd Distal or lower of the SVC or CAJ is optimal placement to reduce complications (thrombus) and spontaneous malpositions! Note the location of the AV node… …its’ close proximity to the CAJ is what allows Sapiens technology to work.

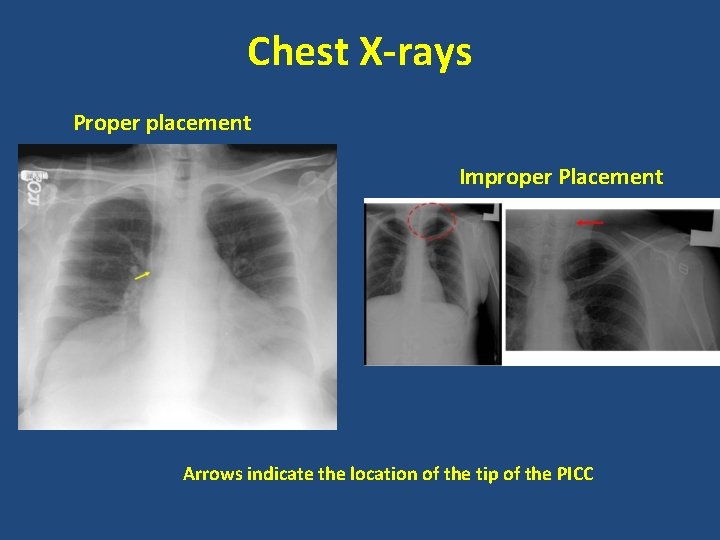
Chest X-rays Proper placement Improper Placement Arrows indicate the location of the tip of the PICC

Radiology Reports Documentation by the radiologist as to the location of the tip of the PICC line must appear in the medical record prior to use of the catheter. The RN caring for the patient reviews the Radiology report prior to use. If tip placement is confirmed in the SVC/CAJ, per documentation by the radiologist, the PICC line may be used (no physician order is needed to use).

Radiology Reports • An attending or resident should not give an “okay to use” without a formal radiology reading. • The radiologist should specifically state “pull back ‘x’ cm” if necessary. If the report is not specific, call the Radiology reading room to clarify. • Staff nurses (after appropriate training) may pull back to reposition the PICC according to the radiologist’s instructions. • A repeat CXR is required after any catheter manipulation. • After repositioning the PICC line, the RN should complete appropriate documentation in the patient’s medical record.

FYI Any patient admitted to the hospital with a PICC line in place, should have a CXR to confirm placement!

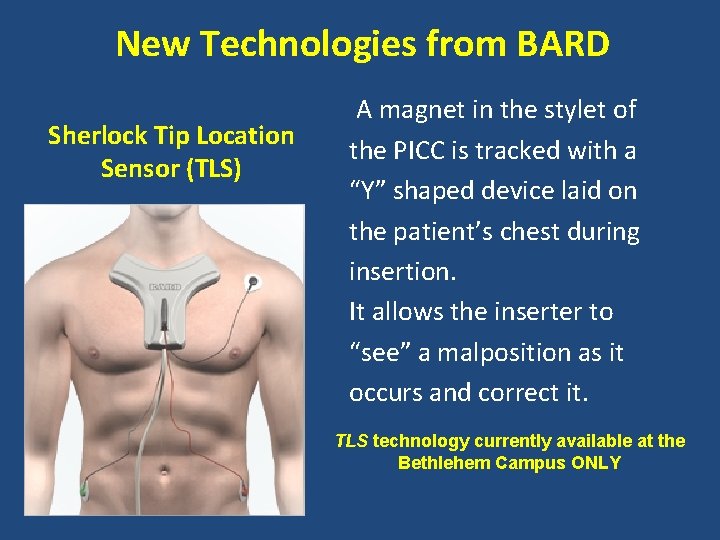
New Technologies from BARD Sherlock Tip Location Sensor (TLS) A magnet in the stylet of the PICC is tracked with a “Y” shaped device laid on the patient’s chest during insertion. It allows the inserter to “see” a malposition as it occurs and correct it. TLS technology currently available at the Bethlehem Campus ONLY

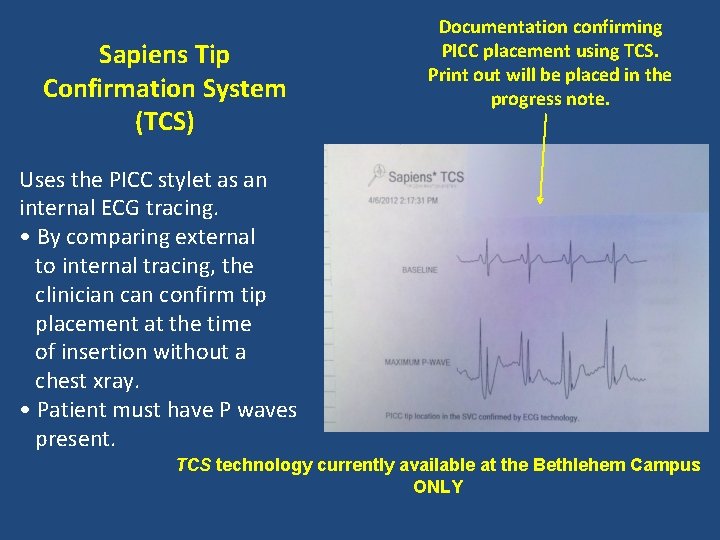
Sapiens Tip Confirmation System (TCS) Documentation confirming PICC placement using TCS. Print out will be placed in the progress note. Uses the PICC stylet as an internal ECG tracing. • By comparing external to internal tracing, the clinician confirm tip placement at the time of insertion without a chest xray. • Patient must have P waves present. TCS technology currently available at the Bethlehem Campus ONLY

With Sapiens Technology, is a Chest X-ray Needed? Communication is the key! • After the PICC is inserted, the PICC nurse will inform the patient’s RN whether or not placement is confirmed. • The Sapiens ECG strip will be placed in the progress note if placement is confirmed! • If placement is confirmed, there is NO need for an x-ray or order to use PICC. – Per Protocol it is “okay to use. ” This communication method is currently used at the Bethlehem Campus ONLY Pink stickers will be placed on the caps of a PICC line which needs a chest xray to confirm placement. - The patient’s RN should remove the pink sticker once placement is confirmed.

Questions? Any questions regarding a chest xray reading and/or PICC placement can be directed to a PICC nurse or appropriate Radiologist.

Care of a PICC Line Test your current knowledge by answering the following… At what point after insertion is the first PICC dressing change to occur? Answer: within 24 hours After the initial dressing change, how often are PICC dressing changes done? Answer: every 7 days & prn Exception: Warren Campus where Biopatch is used

How often does a PICC need to be flushed and with what? Answer: flush each lumen of the PICC after each use and, if inactive, every 12 hours - see Flush Protocol for details How often should a PICC site assessment be done? Answer: at least every shift

List the PICC site assessments that should be reported immediately to the physician… Answer: The following should be reported immediately to the physician: • • pain redness warmth swelling blood pulsing leakage subjective patient complaints

A patient with a PICC line who states: “It feels like something is crawling in my neck” is likely experiencing which of the following: • • Hallucinations Bed bugs Medication reaction A migrating PICC line

Reminders: Care of a PICC Line • Arm circumference is measured 3 cm above insertion site on insertion – The RN caring for the patient needs to re-measure the arm circumference with any patient complaint or abnormal assessment finding, and prn • Use only 10 m. L syringes (or larger) to flush PICCs • All infusions administered through the PICC are to be given via an infusion pump • When using the B. Braun CARESITE® Luer Access Device (needlefree valve) with positive displacement feature, clamping the line is only required when removing/changing the valve. – When flushing valve with syringe, do not clamp until the syringe is removed (may negate positive pressure).

Care of a PICC Line Reminders: • If a patient with a PICC line is confused or considered to be at risk for self-discontinuing the PICC, the RN should wrap the PICC line with Kling to protect the site. – Keep in mind, the site still needs to be assessed every shift!

PICC Lines: Helpful Hints & Other Reminders • According to the current SLUHN Central Line policy, new needle-free valves should be applied with: – every blood draw – every dressing change – if compromise and/or residual blood remains in the needle-free valve • If a PICC catheter is occluded, obtain a physician’s order for TPA/Cathflo – RN then follows hospital/entity protocol/package insert • DO NOT draw blood cultures from the PICC line – unless specifically ordered • DO NOT draw blood from a line with TPN infusing or while TPN is running via the other port • 5 m. L waste per protocol for blood draws

Potential Complications • • • Air embolus Infection Phlebitis Malposition Blockage Infiltration/Extravasation • • • Thrombus Difficult removal Nerve injury/irritation Leakage Malfunction of catheter In the event of catheter breakage, clamp the line, wrap the end with a sterile 4 x 4, and notify the physician immediately.

Blood Draws from a PICC Line • Always use a 10 m. L syringe (or larger) • Discard 5 m. L blood (waste) • Withdraw sample using: – a Vacutainer blood leur adapter & blood collection tubes – a syringe & transfer device • Flush with 20 m. L NSS after blood specimen obtained (see Flush Protocol)

Things to Keep in Mind • All IV’s infusing into a port of a central line, should be stopped one minute prior to specimen collection. • Vasoactive solutions should not be stopped therefore, blood specimens should be drawn from another site. • Blood samples should not be drawn from a line being used for TPN. • Blood samples for coagulation studies should not be drawn from a line containing Heparin, unless a physician's order is obtained.

PICC Removal • A physician’s order is needed for removal of a PICC. • RNs who have been instructed & validated on PICC line removal may remove PICCs • PICC Removal = using sterile technique – Place the patient in position for comfort with arm extended at 45 -90 angle – The site should be covered with gauze and an occlusive dressing – The patient should be monitored for up to 30 minutes for any adverse reactions to the PICC line removal – The dressing should be left in place for 24 hours – The RN must inspect the catheter tip for intactness • Refer to the NPPM D-28 Peripherally Inserted Central Catheters-Insertion and Maintenance for documentation requirements

References St. Luke’s University Hospital Network Nursing Policy and Procedure Manuals. Peripherally Inserted Central Catheter-Insertion and Maintenance [D-28] St. Luke’s University Hospital Network Nursing Policy and Procedure Manuals. IV Therapy Policy [D-16] St. Luke’s University Hospital Network Nursing Policy and Procedure Manuals. Central Venous Access Devices – Care and Maintenance, Blood Collection & Removal of [D-04] Infusion Nurses Society. (2011). Infusion Nursing Standards of Practice. Journal of Infusion Nursing 34(1 S)

The End • Exit this Power. Point© program. • Click on “Take Test” which is final step of this education. • Remember, no attendance record is needed. Completion of the posttest will be sent electronically to your Edu-Tracker record once a 100% is achieved. • Print the Certificate of Completion for your records if desired. • Comments, question, or suggestions can be directed to your entity PICC nurse or Kelly Mc. Cormick/Donna Bydlon at 484 -526 - 4333.