REVIEW OF EVIDENCEBASED PRACTICE AND DETERMINING CLINICAL QUESTIONS

REVIEW OF EVIDENCE-BASED PRACTICE AND DETERMINING CLINICAL QUESTIONS TO ADDRESS

DEFINITION OF EBP (MELNYK & FINEOUT-OVERHOLT 2011) Problem-solving approach to clinical practice that integrates: External Evidence: Internal Evidence: Search, critical appraisal, & synthesis of most relevant & best research Via own clinical expertise, generated from outcomes management or QI projects, patient assessment, and evaluation Considers patient preferences and values

EVIDENCE-BASED PRACTICE (EBP) Crucial to: deliver quality healthcare ensure best patient outcome Under utilized: Not the norm in many healthcare systems in US and elsewhere (Melnyk & Fineout-Overholt, 2011)

WHY EBP? Best patient outcomes Reduced: healthcare costs geographic variations in care Retention of healthcare workers (Melnyk & Fineout-Overholt, 2011)

YOUR EXPERIENCES IN EBP?
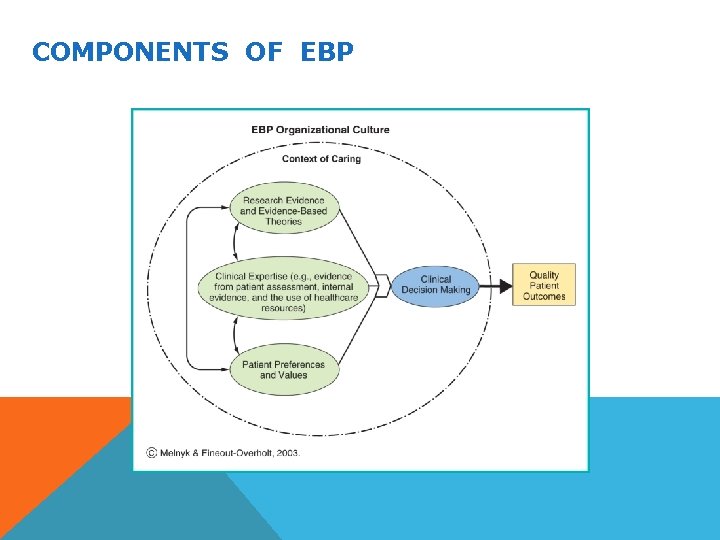
COMPONENTS OF EBP

INITIATIVES TO ADVANCE EBP Institute of Medicine’s Roundtable on Evidence-Based Medicine United States Preventive Services Task Force (USPSTF) Agency for Healthcare Research and Quality (AHRQ) National Consortium for the Advancement of Pediatric and Adolescent Evidence-Based Practice (NCPAEP) Magnet Recognition Program by the ANA Credentialing Center (Melnyk & Fineout-Overholt, 2011)

OTHER DISCIPLINES THAT USE EBP?

Medicine (really began here in the 90’s) Cochrane Physical Therapy Dentistry Psychology Speech Therapy Etc.

STEPS OF THE EBP PROCESS (MELNYK & FINEOUT-OVERHOLT, 2011) 0. Cultivate a spirit of inquiry. 1. Ask the burning clinical question in PICOT format. 2. Search for and collect the most relevant best evidence. 3. Critically appraise the evidence (i. e. , rapid critical appraisal, evaluation, and synthesis).

STEPS OF THE EBP PROCESS (CONT’D) 4. Integrate the best evidence with one’s clinical expertise and patient preferences and values in making a practice decision or change. 5. Evaluate outcomes of the practice decision or change based on evidence. 6. Disseminate the outcomes of the EBP decision or change. (Melnyk & Fineout-Overholt, 2011) * For our class we go through Step 4. The DNP program continues through Steps 5 & 6

STEP 1: ASK THE CLINICAL QUESTION IN PICOT FORMAT Patient population Intervention or issue of interest Comparison intervention or group Outcome Time frame

STEP 2: SEARCH FOR/COLLECT THE MOST RELEVANT BEST EVIDENCE – HIERARCHY OF EVIDENCE (MELNYK & FINEOUT-OVERHOLT, 2011) Level I: Systematic reviews or meta-analyses of RCTs Level II: RCTs Level III: Controlled trials without randomization Level IV: Case-control and cohort studies Level V: Systematic reviews of descriptive and qualitative studies Level VI: Single descriptive or qualitative studies Level VII: Opinion of authorities and/or reports of expert committees

STEP 3: CRITICALLY APPRAISE THE EVIDENCE Appraise: Validity Reliability Applicability

STEP 4: INTEGRATE THE BEST EVIDENCE WITH CLINICAL EXPERTISE AND PATIENT PREFERENCES This is the “implementation” step EBP is not based solely on research and published evidence Patients’ hx/circumstances have a significant bearing on choice of intervention Availability of resources also considered Melnyk & Fineout-Overholt, 2011)

STEP 5: EVALUATE OUTCOMES OF THE PRACTICE DECISION OR CHANGE BASED ON EVIDENCE Measurement of outcomes to determine and document impact of the EBP change on healthcare quality and/or patient outcomes Essential in determining whether the change based on evidence resulted in the expected outcomes when implemented in the real-world clinical practice setting (Melnyk & Fineout-Overholt, 2011)

STEP 6: DISSEMINATE OUTCOMES OF EBP DECISION OR CHANGE positive and negative outcomes Via various methods personal communication to conference presentation (Melynk & Fineout-Overholt, 2011)
- Slides: 17