Retroviruses Retroviruses Probably the most studied group of

Retroviruses

Retroviruses Probably the most studied group of viruses in molecular biology!!! n Enveloped, positive-strand RNA viruses n Unique morphology and replication n Replicate through a DNA intermediate by reverse transcriptase (RT) n

Retroviruses n n n Baltimore and Temin in 1970 RNA-dependent DNA polymerase (reverse transcriptase ) encoded by retroviruses Retroviruses replicate through an DNA intermediate This DNA copy of viral genome integrates into host chromosome This discovery earned the Nobel prize: contradicted the central dogma of molecular biology-genetic information passed from DNA to RNA and then to protein n Here: from RNA to DNA

History Rous sarcoma virus: solid tumors in chicken n Other cancer causing retroviruses from other animal species (oncogenes) n 1981: first human retrovirus: Human Tlymphotropic virus (HTLV-1) n 1983: Human immunodeficiency virus (HIV) n
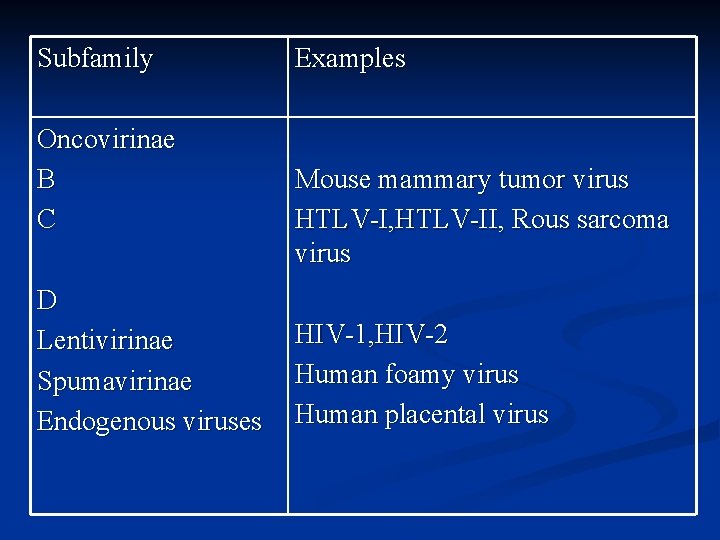
Subfamily Oncovirinae B C D Lentivirinae Spumavirinae Endogenous viruses Examples Mouse mammary tumor virus HTLV-I, HTLV-II, Rous sarcoma virus HIV-1, HIV-2 Human foamy virus Human placental virus

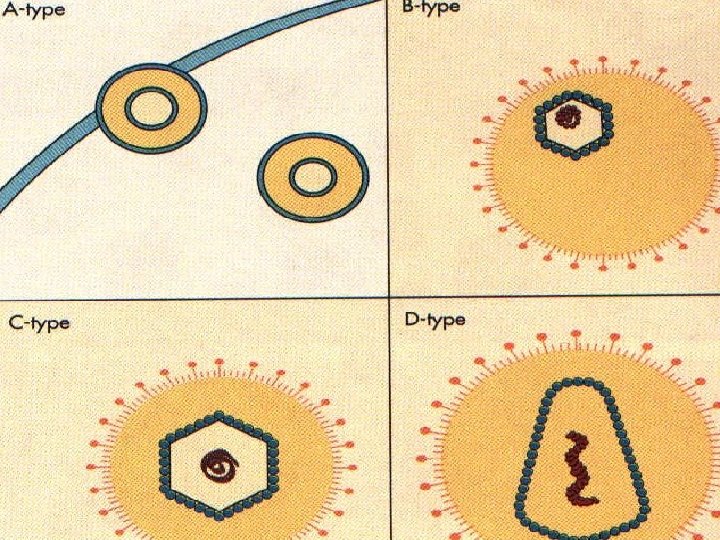
n Oncoviruses: immortalize or transform target cells, A, B, C, D type according to their core and capsid n Lentiviruses: slow viruses associated with neurologic and immunosuppresive disease Spumaviruses: no disease n Endogenous viruses: transmitted vertically, 1% of n human chromosome, in many animal species and humans, one detected in placental tissue which facilitates placental function

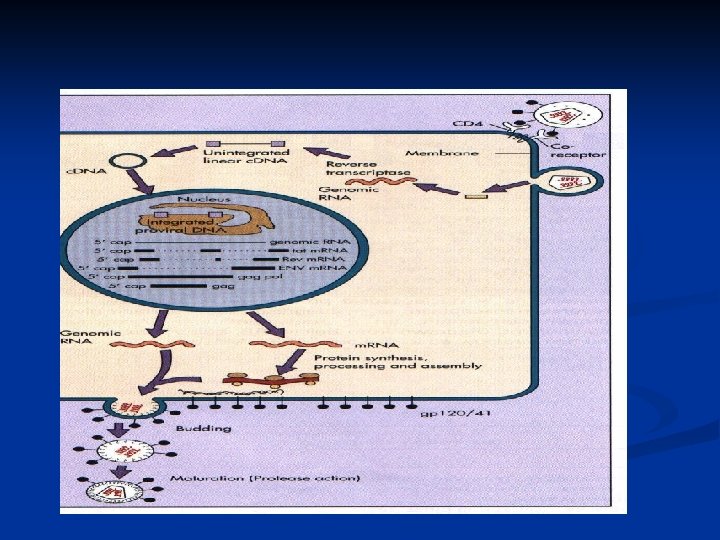
Retroviruses n n n Enveloped sperical virion Two copies of positive-strand RNA genome RT Provirus integrates randomly into host chromosome Transcription of the genome is regulated by the interaction of host transcription factors with promoter and enchancer elements in the long-terminal repeat portion (LTR) of the genome

Retroviruses n n Simple retroviruses encode gag, pol and env genes Complex viruses also encode accessory –regulatory genes (tat, rev, nef, vif, vpu for HIV) Assembles and buds from the plasma membrane Final morphogenesis requires protease cleavage of gag and gag-pol polypeptides after envelopment.
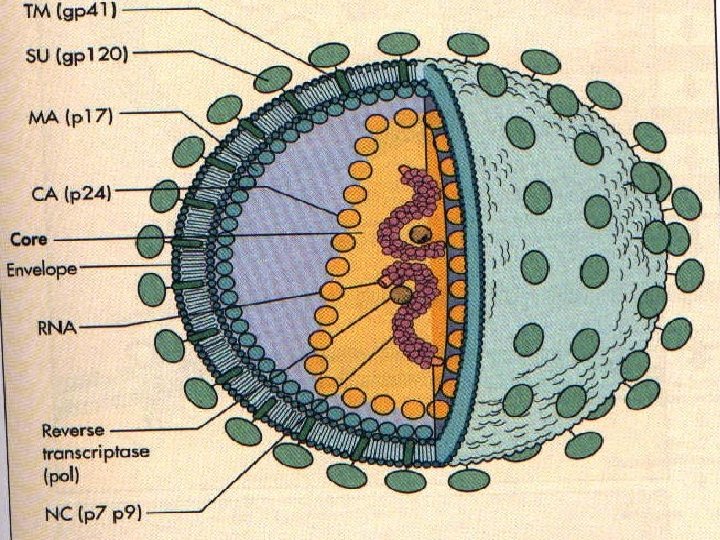
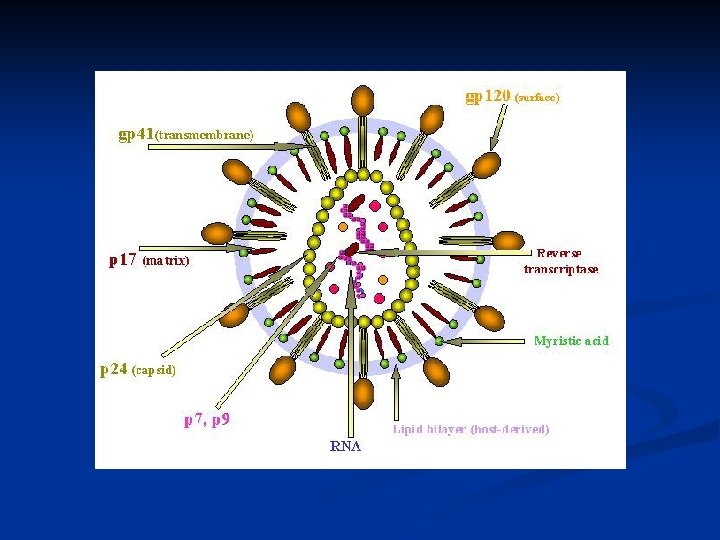
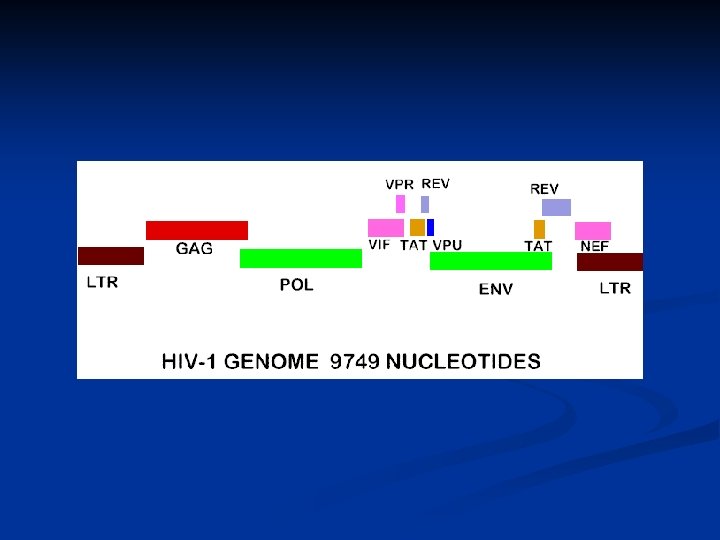
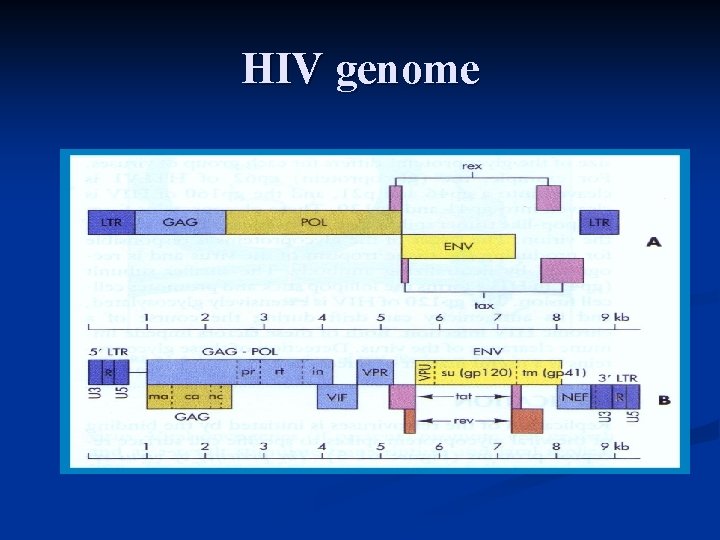
HIV genome

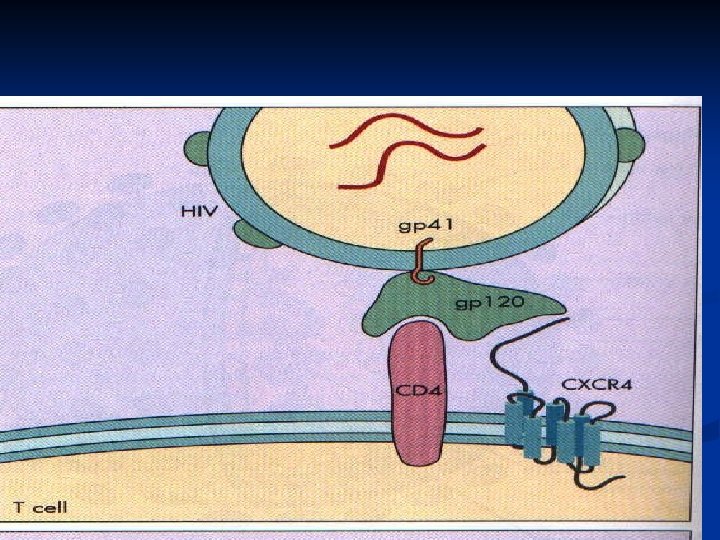
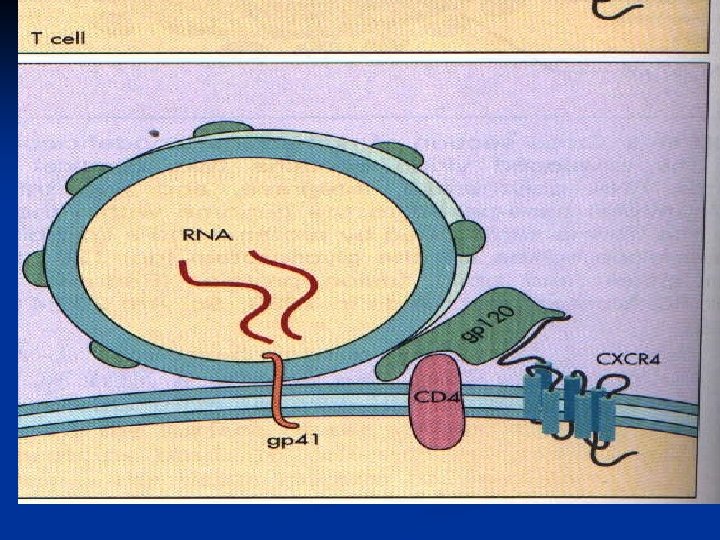
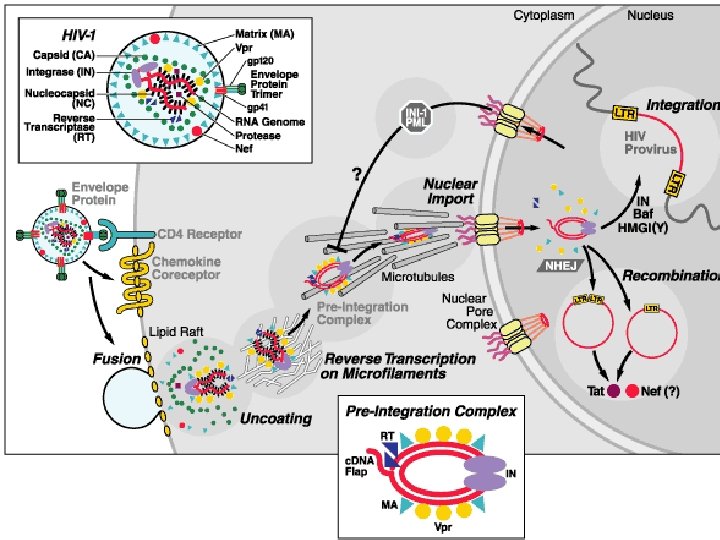
Gp 120 CD 4 surface receptor protein n Initially expressed on cells of the macrophage lineage (macrophage, dendritic cells, microglial cells) (M-tropic)+ second receptor CCR 5 n Later on helper T cells (T-tropic) +fusin (CXCR 4) n

Chemokine receptors n CCR 5: binds macrophage-tropic, non-syncytium-inducing (R 5) viruses mucosal and intravenous transmission of HIV infection. n CXCR 4: T-cell-tropic, syncytium-inducing (X 4) viruses, which are frequently found during the later stages of disease. n In up to 13% of individuals of northern European descent, a naturally occurring deletion of 32 base pairs in the CCR 5 gene results in a mutant CCR 5 receptor that never reaches the cell surface. Individuals homozygous for this mutation (1 -2% of the Caucasian population) are almost completely resistant to HIV infection.

Transmission *Blood, semen, vaginal secretions n Sexual contact n Exposure to contaminated blood and blood products n From infected mother to her baby perinatally

HIV is not transmitted Casual contact n Touching, hugging, kissing, coughing, sneezing, insect bites, water, food, utensils, toilets, swimming pools, public baths n
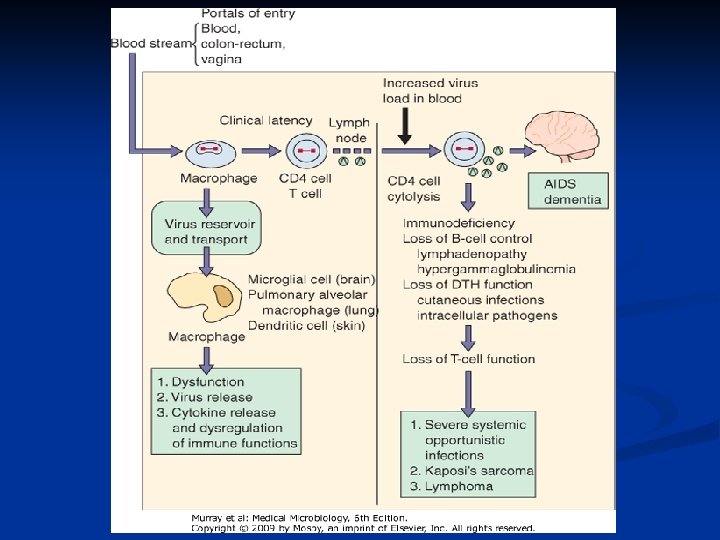

Transmission Inoculation of blood: Transfusion, needlesharing among intravenous drug abusers, needlestick, open wound, mucous membrane exposure, tattoo needles n Sexual trasmission: anal and vaginal intercourse n Perinatal transmission: Intrauterine, peripartum and breast milk n

Population at high risk Intravenous drug abusers, sexually active people with many partners (homosexual, heterosexual), prostitutes, newborns of HIV infected mothers n Blood and organ recipients and hemophiliacs: before 1985 (pre-screening programs) n

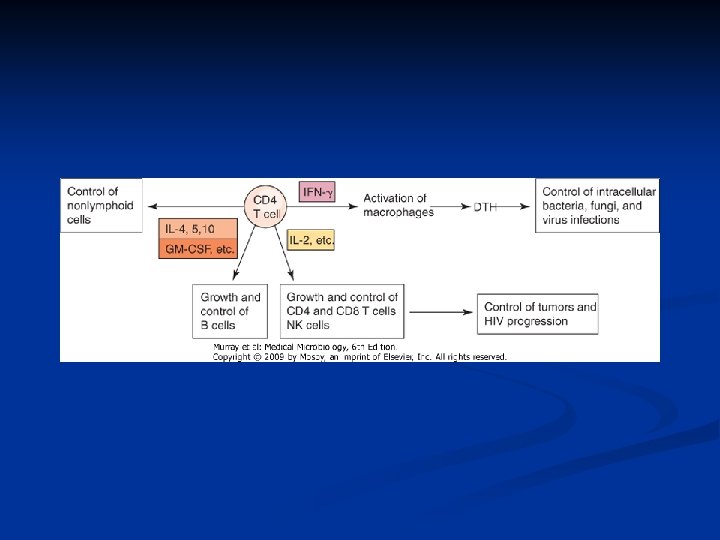

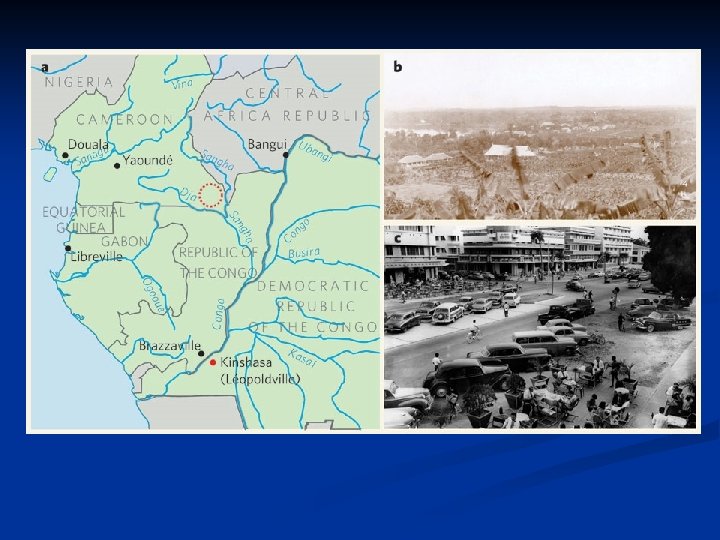
Epidemiology n n Late 1970 s-early 1980 s Young homosexual men, Haitians, heroin addicts, hemophiliacs were noted to be dying of normally benign opportunistic infections HIV appears to have evolved since 1930 s from a simian virus and then rapidly spread Africa and the world by an increasinly mobile population. There is an expanding epidemic worldwide.
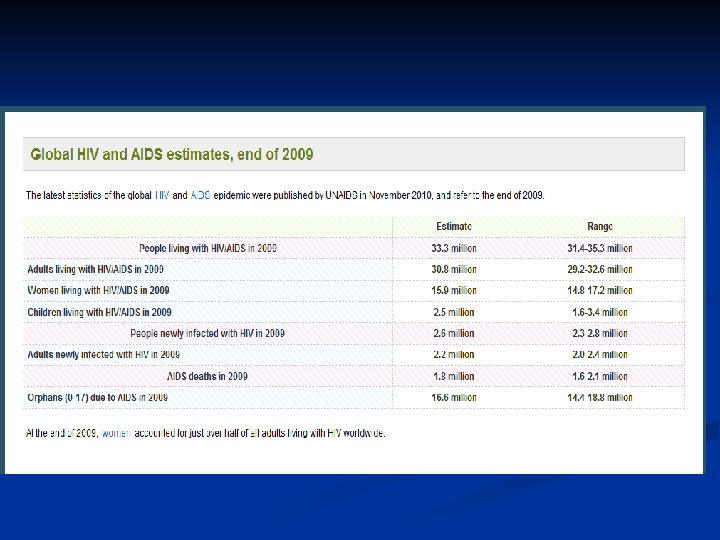

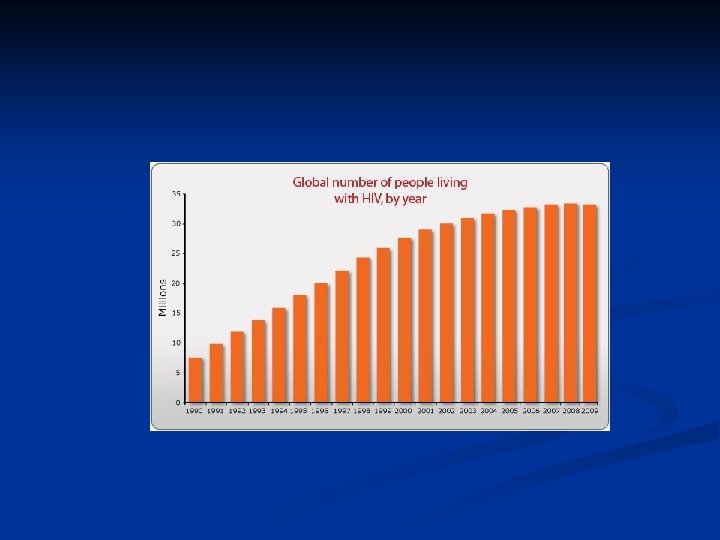
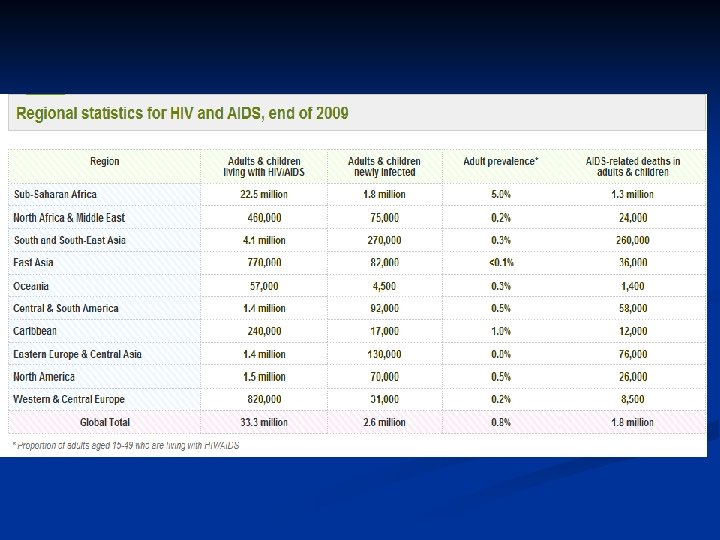

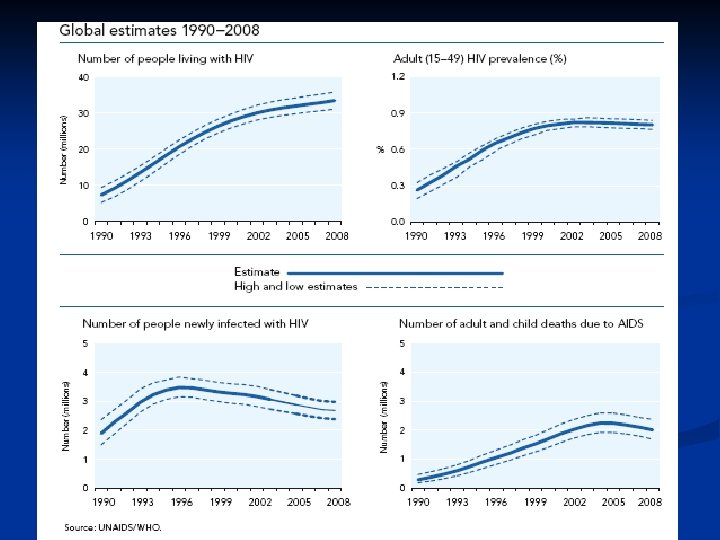
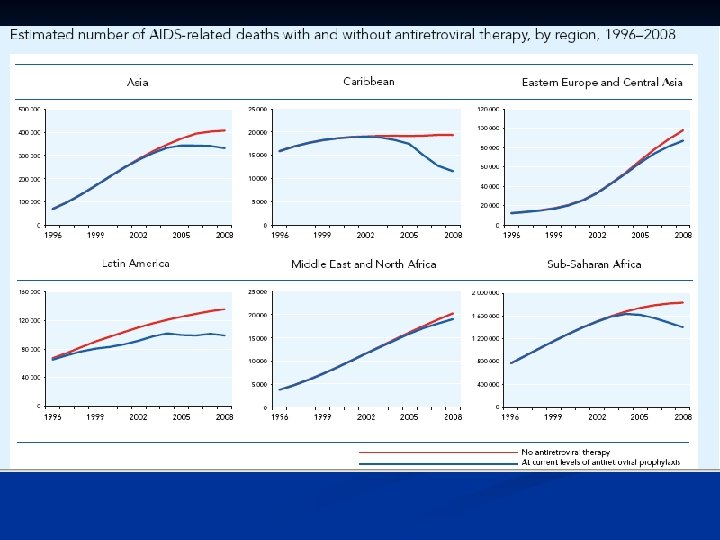
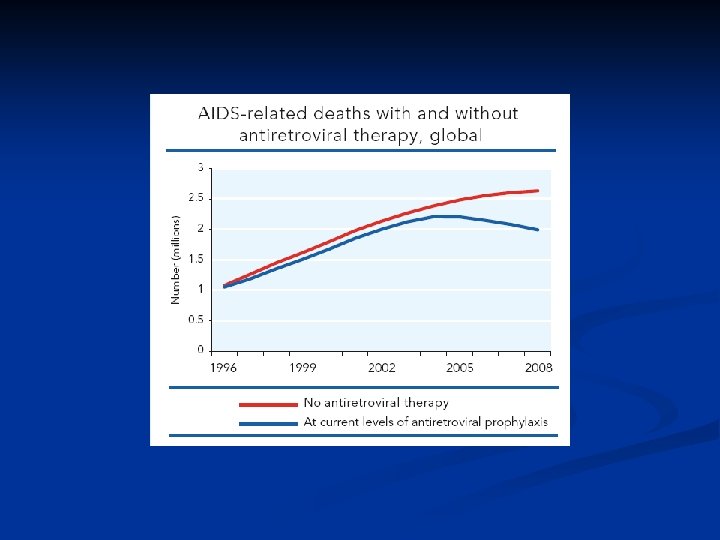
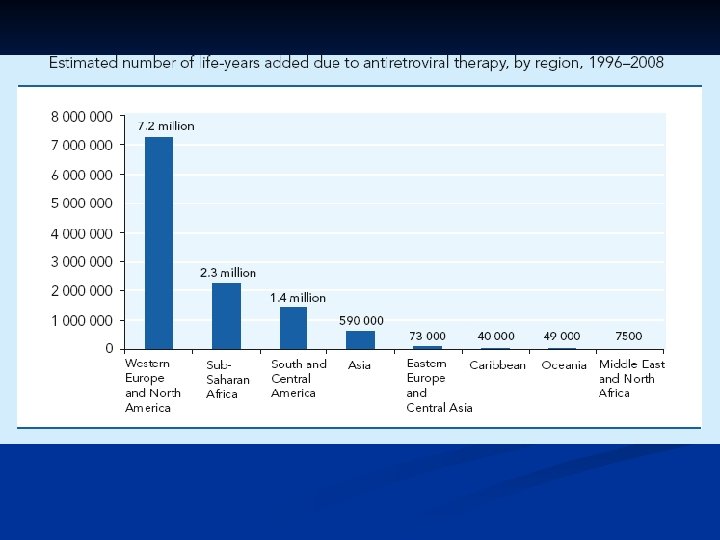
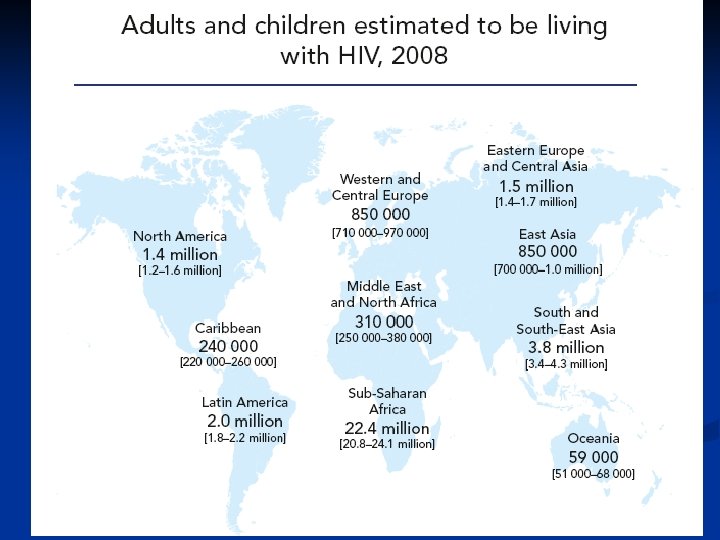



AIDS cause by HIV Retroviridae family n Lentivirinae genus n Enveloped, positive strand RNA virus n 2 identical 9 -10 kb RNA n

AIDS n Human immunodeficiency virus type 1 and 2 (HIV-1, HIV-2)

HIV HIV-1: isolated in 1983 n Responsible from AIDS pandemic n HIV-2: isolated in 1986 n HIV-2 less pathogenic slow progression to AIDS n

HIV group and subtypes Rapid mutation and recombination HIV-1 n Group M (major): A-J n Group O n Group N HIV-2 n A-E subtypes n
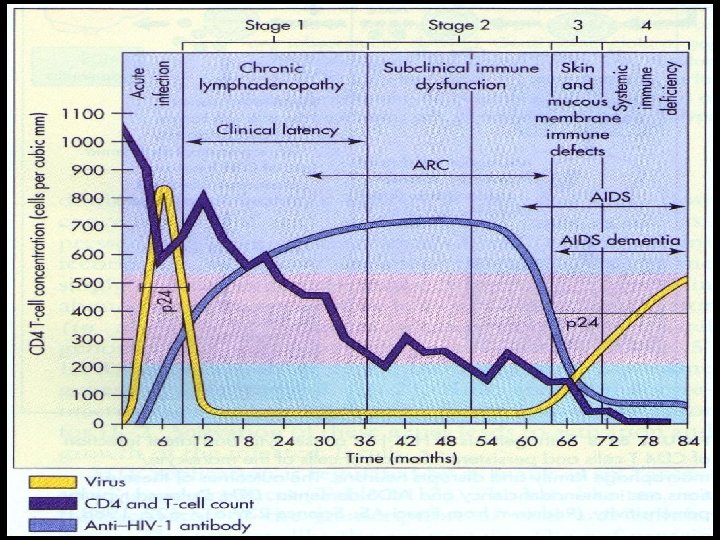
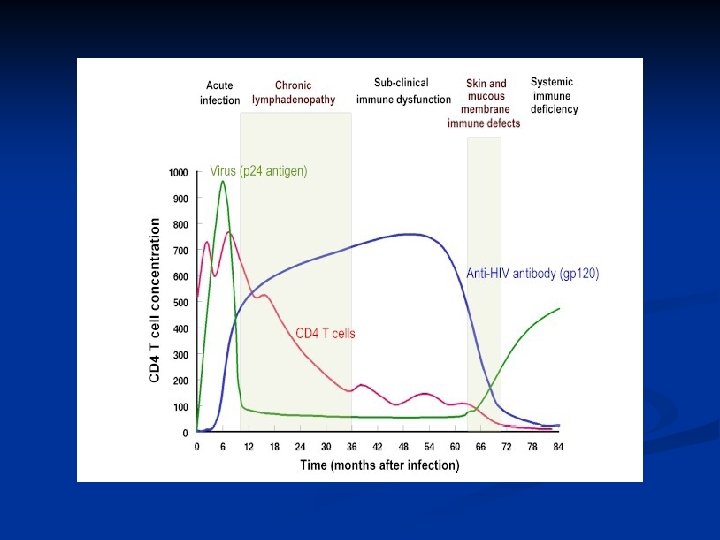
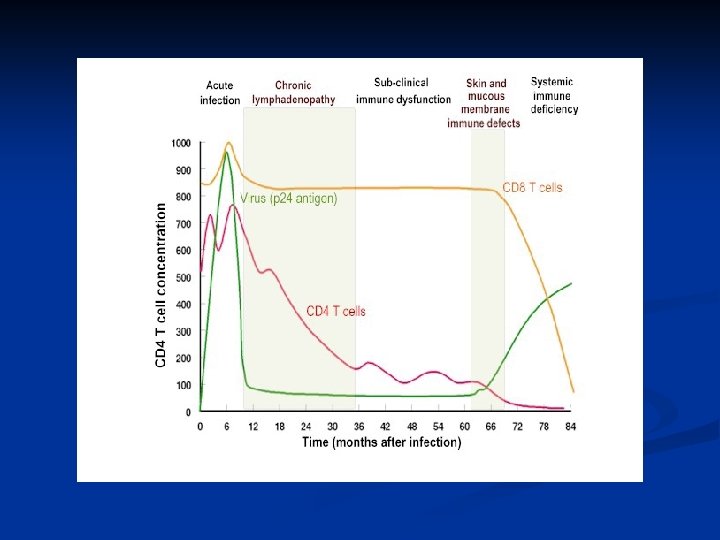

Acute retroviral syndrome n n n n First signs occur in days to several weeks Transient %50 -70 Activation of immune system Multisystem dysfunction Flu or infectious mononucleosis sydrome like findings Then a latent period

AIDS Continuous viral replication n Immune system dysfunction n

CD 4 T lymphocyes n > 500 /µl (> %29) 1 n 200 -499 (% 14 -28) 2 n < 200 /µl (< %14) 3 n

Incubation n Adults with no treatment: 10 -11 years n ‘rapid progressors’ : 2 -3 years n ‘non-progressor’ Stable CD 4 cell count : 7 -10 years

HIV genome Structural genes: gag/env n Pol: enzymes -reverse transcriptase -protease -integrase Tat and Rev: necessary for replication Accessory genes: Vif, Vpr(HIV-1), Vpu, Nef Vpx(HIV-2) n

HIV Viral RNA (in free Virion ) n Viral DNA: integrated in host cell DNA (Provirus) n

Seroconversion Usually 3 weeks n 1. 5, 3, 6, 12 months n
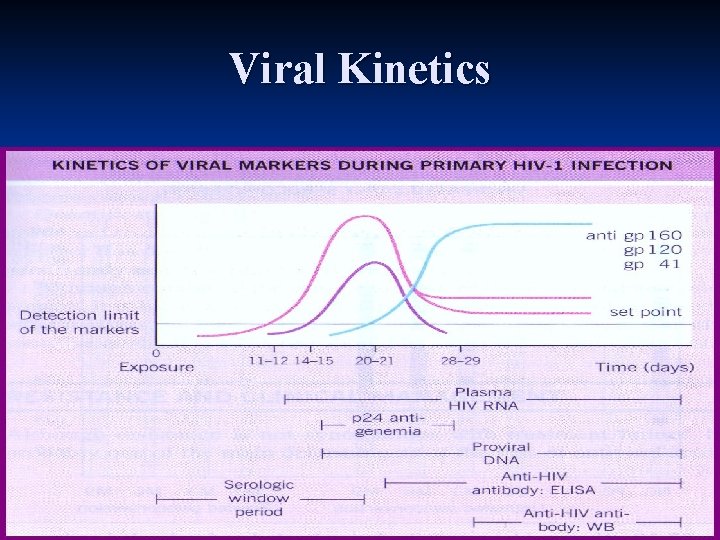
Viral Kinetics

Laboratory diagnosis Serology: Adults and children older than 15 months: n Initial screening: ELISA, latex agglutination n Confirmation: Western-blot Molecular techniques: -qualitative DNA detection: babies younger than 15 months -quantitative RNA: follow up of HIV infected people who are on therapy
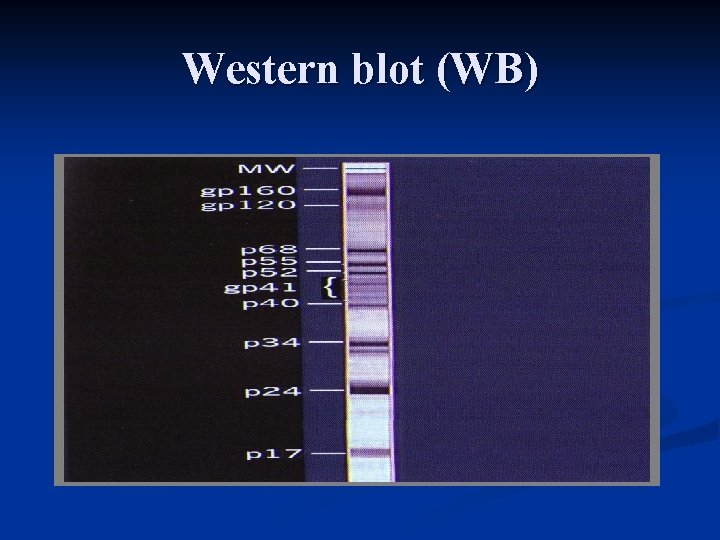
Western blot (WB)

Other tests Immunologic status: CD 4: CD 8 ratio Low n Antiretroviral resistance tests n
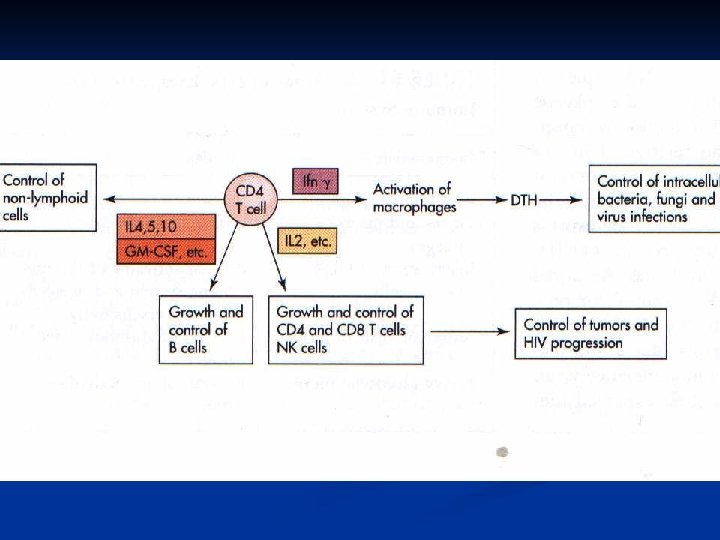

Indicators of disease Opportunistic infections: n Protozoal: Toxoplasmosis n Fungal: Candidiasis, Pneumocystis carinii n Viral : Cytomegalovirus, HSV n Bacterial: Mycobacterium avium-intracellulare Opportunistic neoplasias: Kaposi’s sarcoma
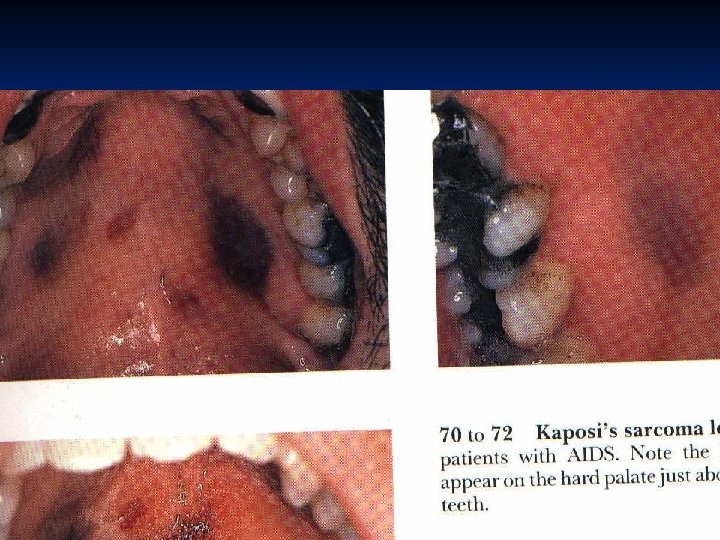
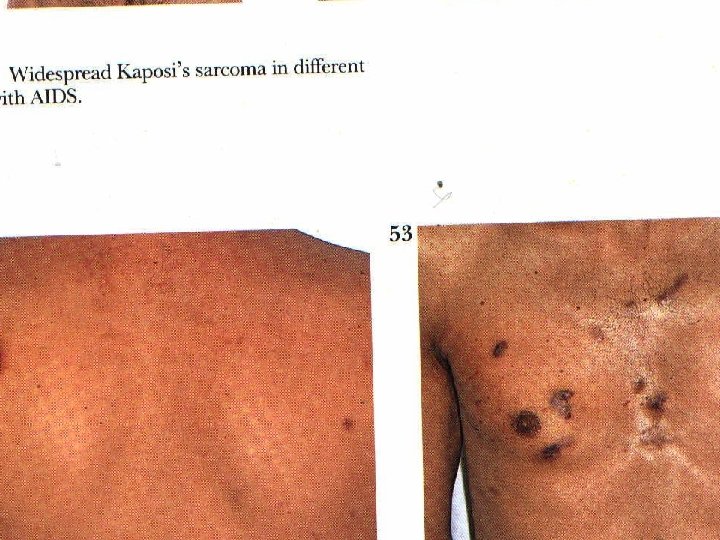


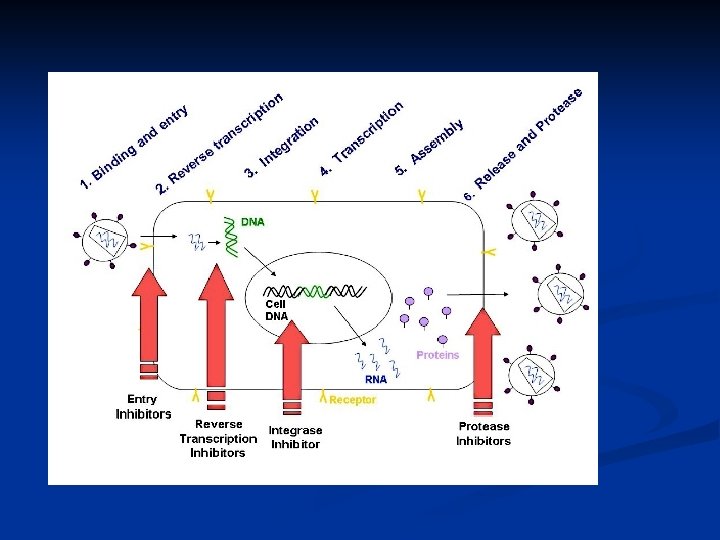
CCR 5 Antagonist Maravirıoc (MVC) – Selzentry n Integrase inhibitor Raltegravir (RAL)/ Isentress n


Prevention and control Education n Blood and blood product screening n Infection control: ‘Universal Blood and body fluid precautions’: All patients may be infectious for HIV and other bloodborn infections: -wear protective clothing(gloves, masks, gown) and other barriers to prevent exposure to blood products n

Prevention and control n 10% household bleach(% 0. 5 chlorine, 5 g/litre 5000 ppm n 70% ethanol 2% glutaraldehyde 4% formaldehyde 6% Hydrogen peroxide Washing laundry in hot water with detergent is sufficient to inactivate HIV. n n

Modes of control n n n Antiviral drugs limit progression of disease Vaccines for prevention and treatment are in trials Safe(Condom!) monogamous sex helps limit spread. Sterile injection neeedles should be used Large scale screening programs for blood transfusion, organs for transplants, clotting factors

Oncovirinae RNA tumor viruses n Associated with leukemias, sarcomas and lymphomas in many animals n Not cytolytic n Distinquished by the mechanism of cell transformation and length of latency period between infection and the development of disease n

Oncovirinae Sarcoma and acute leukemia viruses: n Protooncogenes(at least 35) n Highly oncogenic, direct effect n No human virus Leukemia viruses: n No oncogene n Long latency period n HTLV-I, HTLV-II, HTLV-5

Human T lymphotropic virus type 1( HTLV-I) Adult acute T-cell lymphocytic leukemia (ATLL) n HTLV-associated myelopathy (tropical spastic paraparesis) n Blood transfusion, sexual intercourse, breast feeding n Long latency period: approximately 30 years n

Human T lymphotropic virus type 1( HTLV-I) Endemic in southern Japan n ATLL (1 in 20 people over a 30 -50 years n Diagnosis: ELISA+WB n Viral RNA by RT-PCR n
HTLV-2: Hairy cell leukemia n HTLV-5: malignant cutaneous lymphoma n
- Slides: 78