Restrictive and Interstitial Lung Disease J B Handler

Restrictive and Interstitial Lung Disease J. B. Handler, M. D. Physician Assistant Program University of New England 1

Abbreviations n n n SLE- systemic lupus erythematosis DLCO- diffusing capacity for carbon monoxide HRCT- high resolution computed tomography ALS- Amyotrophic Lateral Sclerosis RR- respiratory rate IFIP- idiopathic fibrosing interstitial pneumonia n RA- rheumatoid arthritis 2

Restrictive Disease and Dysfunction n Collection of diseases that are characterized by reduction in volume of air within the lung parenchyma. n n n Abnormal reduction in pulmonary ventilation. Restrictive pattern on PFT’s. Compensated by RR. Multiple etiologies: Most common are forms of interstitial lung disease. Some diseases have both obstructive and restrictive components: Cystic fibrosis, others. 3

Interstitial Lung Disease n n Heterogeneous group of diseases (>180) with common response to lung injury. Idiopathic fibrosing interstitial pneumonia (IFIP), formerly called Idiopathic (primary) Pulmonary Fibrosis: Classic example of restrictive lung disease. Multiple secondary etiologies- see below. Pathology is similar, regardless of etiology. 4

Secondary Etiologies n n n Drug related: Amiodarone (potent antiarrhythmic), bleomycin (tx cancer), some antibiotics (sulfonamides), others. Occupational inhalation: Silica, asbestos, beryllium, others. Connective tissue disorders: SLE, Polymyositis, RA, scleroderma. Others: Radiation, amyloidosis, sarcoidosis. Infections: Fungal (Coccoidiomycosis, Pneumocystis), Mycobacterium, some 5 viruses.

IFIP n n Diagnosis of exclusion Must exclude other etiologies (via biopsy) before saying “idiopathic”. n n n Variations of IFIP exist, with varying response to therapy. Characteristic clinical, radiographic, PFT and other findings. Poor prognosis as with many other etiologies of interstitial lung disease. 6
Pathology n Inflammatory infiltrate in lung parenchyma/interstitium: n n n Inflammation of alveolar epithelium and capillary endothelium followed by: Fibrosis of the alveoli and interalveolar septum Inflammation can include the respiratory bronchioles. Thickening of alveolar-capillary membrane by collagen and fibrous tissue. Over time Fibrosis throughout lung parenchyma. 7
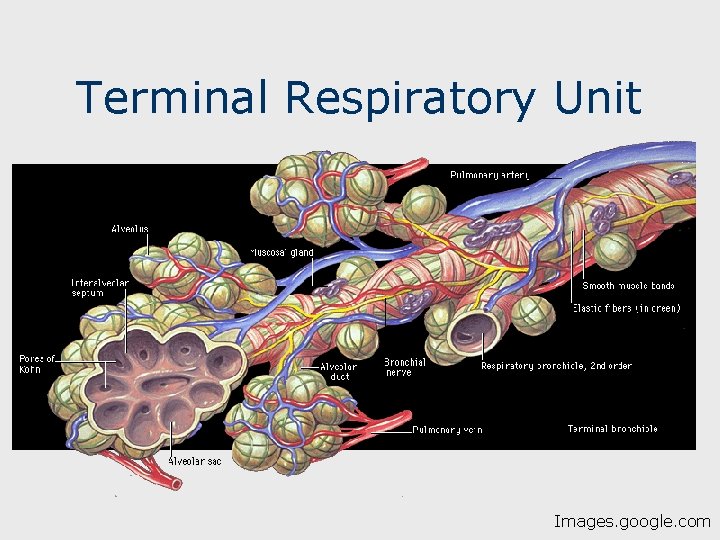
Terminal Respiratory Unit Images. google. com
Pathology/Pathophysiology n n Inflammatory cellular and fibrotic response. Inflammatory cells release chemical mediators activation of fibroblasts collagen deposition. Tissue injury, vascular injury and permeability. Epithelial injury thickens/breaks alveolarcapillary membrane impaired diffusion of gas ( DLCO). 9

Pathophysiology n n n Destruction of alveoli/capillaries V/Q mismatch; both shunting and increased dead space. Ongoing repair/re-injury cycle; nonhomogeneous scarring throughout lung. Lung compliance. 10
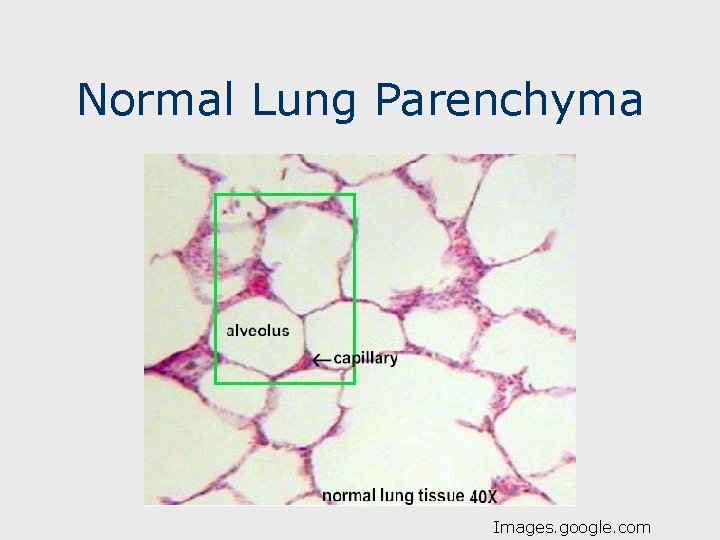
Normal Lung Parenchyma Images. google. com
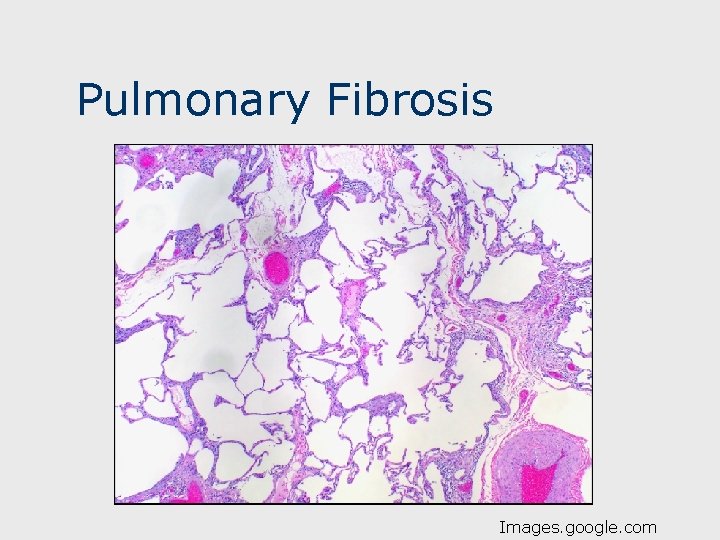
Pulmonary Fibrosis Images. google. com

Clinical Presentation (IFIP) n Insidious onset most often with gradual development of shortness of breath; initially exertional, then at rest. n n Other etiologies may have acute chronic presentation. History: Occupational exposure? Smoker? n n Travel history (parasitic infections) Risk factors for HIV 13

Clinical Presentation Decreased activity tolerance n Dry, non-productive cough n +/- fever; depends on etiology n Presentation may vary depending on etiology n 14

Physical Exam, Testing n n Lungs: Fine, inspiratory crackles (like velcro) at lung bases. RR late. Clubbing of fingers: bony growth and enlargement of terminal phalange; present 25 -50% of cases. Chest x-ray (see below): May appear normal until advanced disease. HRCT- may be useful- confirms “honeycomb pattern”. 15
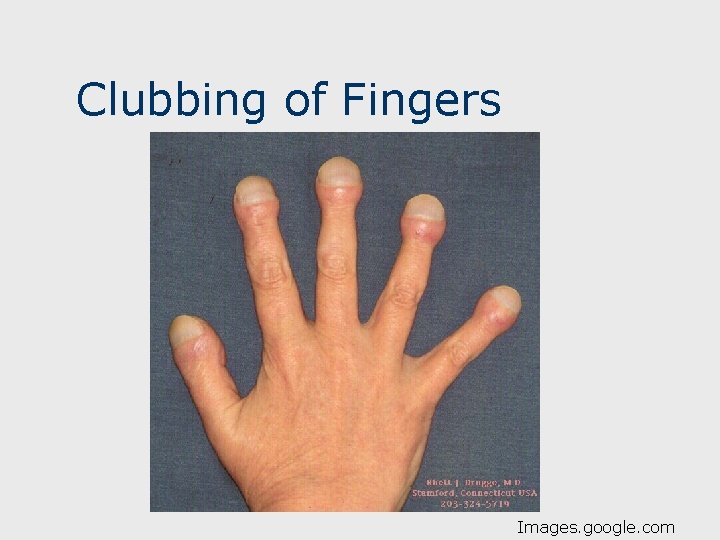
Clubbing of Fingers Images. google. com
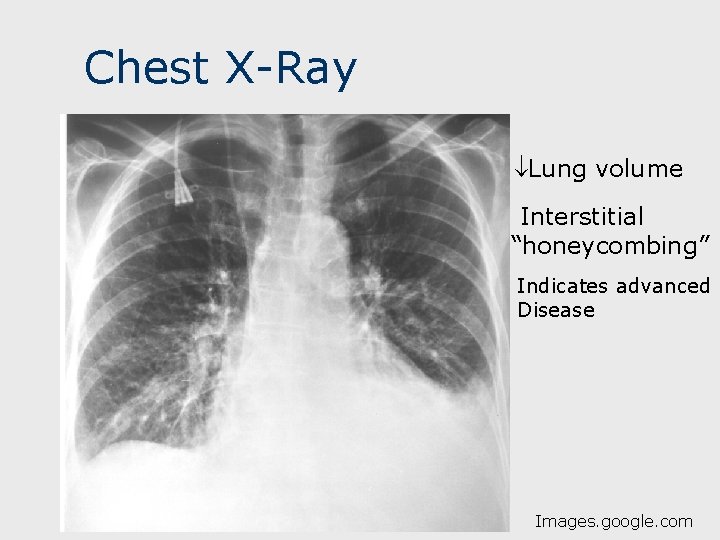
Chest X-Ray Lung volume Interstitial “honeycombing” Indicates advanced Disease Images. google. com

PFT’s and ABG n n n Marked reduction in all lung volumes. FVC, FEV 1, both often markedly Normal FEV 1/FVC (or ) DLCO ABG: progressive hypoxemia due to both DLCO and V/Q mismatch. Worse with exercise. PCO 2 reflects increased respiratory rate to accommodate hypoxemia. PCO 2 levels rare except with end stage disease. 18

Lung Biopsy n Most important tool to confirm diagnosis and sort out underlying etiologies. n n n Trans bronchial biopsy- least invasive, but sample size to small in most cases. Thoracoscopic biopsy- less invasive than open thoracotomy but still requires small incisions into thorax. Open lung biopsy- requires thoracotomy; multiple samples obtained from different areas of lung. 19

Treatment n n No data to show that any treatment improves survival or quality of life of in patients with IFIP. Progressive disease in most patients death in 3 -5 years. Other etiologies sometimes respond to systemic corticosteroids (prednisone, et al) or immunosuppressive agents with varying degrees of improvement. 20

Restrictive Disease: Others n Neuromuscular diseases: ALS, Muscular Dystrophy, Polio, etc. n n n Impair lung inflation; restrictive pattern on PFT’s. Kyphoscoliosis: Decrease lung volume; restrictive pattern on PFT’s. – abnl forward bending puts pressure on lungs Pleural diseases: prevent lung expansion; restrictive pattern on PFT’s. 21
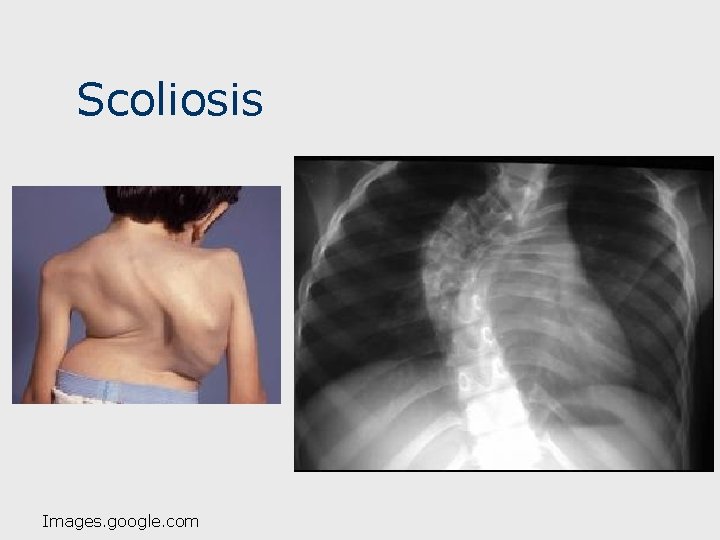
Scoliosis Images. google. com
- Slides: 22