Respiratory Therapeutics Drug Therapy Antibiotics for Upper Respiratory

Respiratory Therapeutics

Drug Therapy Antibiotics for Upper Respiratory Tract Disease Antibiotics for Lower Respiratory Tract Disease Antifungal Therapy Antiviral Therapy Glucocorticoids Bronchodilators Mucolytics Antihistamines Antitussive Agents Nutrition and fluid therapy

Antibiotics for Upper Respiratory Tract Disease o Empiric antibiotic therapy is often used in animals with presumed respiratory infection prior to obtaining definitive information on the bacteria involved because susceptibility results take 2– 5 days to become available or because of an inability to obtain an appropriate sample. o In kittens with acute (likely viral) upper respiratory disease, flora of the upper respiratory tract (Staphylococcus, Streptococcus, Pasteurella, Bordetella, Mycoplasma, and anaerobes) may overwhelm local defenses and colonize the nasal cavity, leading to clinical signs of sneezing and mucopurulent nasal discharge. o Antibiotics are commonly administered for 1– 2 weeks to kittens with acute upper respiratory infection to reduce bacterial numbers and decrease bacterial invasion of epithelium damaged by viral infection.

o. Fortunately, many commonly encountered bacterial strains remain susceptible to amoxicillin–clavulanic acid or to fluoroquinolones, Azithromycin also has clinical efficacy for acute feline upper respiratory tract infection. o It is important to remember that penicillin derivatives are ineffective against Mycoplasma spp. , a cell-wall deficient bacteria. Because this organism can be found in acute feline upper respiratory disease, use of doxycycline or a fluoroquinolone would be appropriate

o In chronic upper respiratory tract disease in the cat, aerobic bacterial infection is a common complication. o The chronic disease is typically characterized by devitalization of tissue with accumulation of inflammatory products Doxycycline and azithromycin are attractive drugs to use in such cases because they possess anti-inflammatory effects as well as antimicrobial action. o Newer fluoroquinolones (pradofloxacin and premafloxacin) also have some efficacy against anaerobic organisms. For cats with underlying osteomyelitis or suspected anaerobic infections, a drug such as clindamycin could be more effective in controlling clinical signs since it penetrates bone tissue.

o When treating the bacterial component of feline upper respiratory tract disease, consideration should be given to using a long course (4– 6 weeks) of antibiotics to achieve maximal control of bacterial numbers. o Bacterial involvement in canine inflammatory rhinitis appears to be less prominent than in the feline syndrome Secondary bacterial infection can develop in dogs that have been treated for nasal aspergillosis infections because of destruction of turbinates and loss of normal nasal defense mechanisms. In those cases, 7– 10 days of any broad spectrum antibiotic (e. g. , amoxicillin-clavulanic acid) can help alleviate nasal discharge.

Antibiotics for Lower Respiratory Tract Disease o Appropriate therapy for bacterial respiratory infection often requires antibiotics directed at Gram-negative and -positive aerobes, and Mycoplasma organisms(before final culture results are available ) would include enrofloxacin with a penicillin derivative drug, metronidazole, or clindamycin. o Ticarcillin, a carboxypenicillin formulated only for intravenous use, is a valuable drug to employ in early treatment of pneumonia. It has improved efficacy in treatment of Pseudomonas infection as well as anaerobic infections; however, it is ineffective against Mycoplasma.

q Lower respiratory tract infections require 2– 6 weeks of antibiotic treatment. q Azalides (azithromycin and clarithromycin) have efficacy against Gram-positive and Gram-negative organisms and Mycoplasma. These drugs have the advantage of producing high and prolonged tissue levels, typically resulting in enhanced bacterial killing. 8
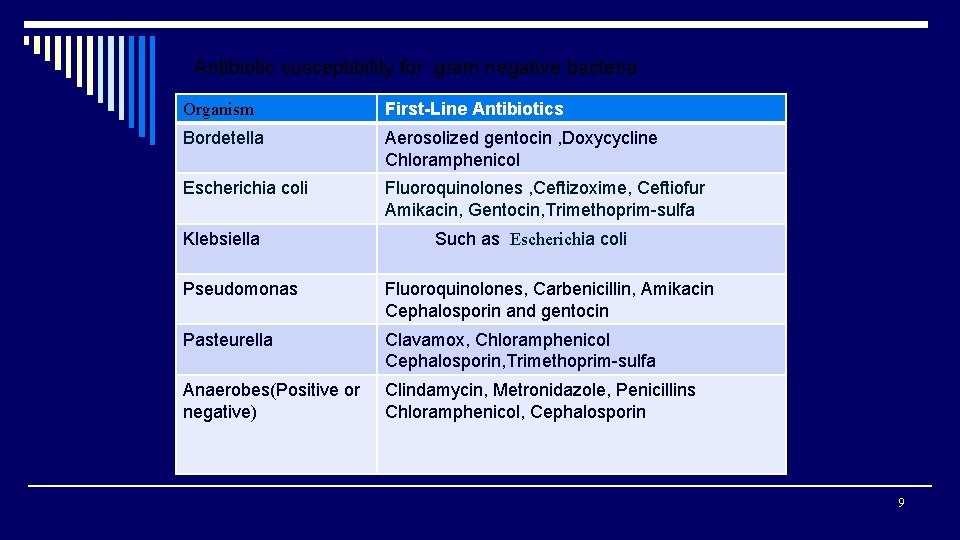
Antibiotic susceptibility for gram negative bacteria Organism First-Line Antibiotics Bordetella Aerosolized gentocin , Doxycycline Chloramphenicol Escherichia coli Fluoroquinolones , Ceftizoxime, Ceftiofur Amikacin, Gentocin, Trimethoprim-sulfa Klebsiella Such as Escherichia coli Pseudomonas Fluoroquinolones, Carbenicillin, Amikacin Cephalosporin and gentocin Pasteurella Clavamox, Chloramphenicol Cephalosporin, Trimethoprim-sulfa Anaerobes(Positive or negative) Clindamycin, Metronidazole, Penicillins Chloramphenicol, Cephalosporin 9
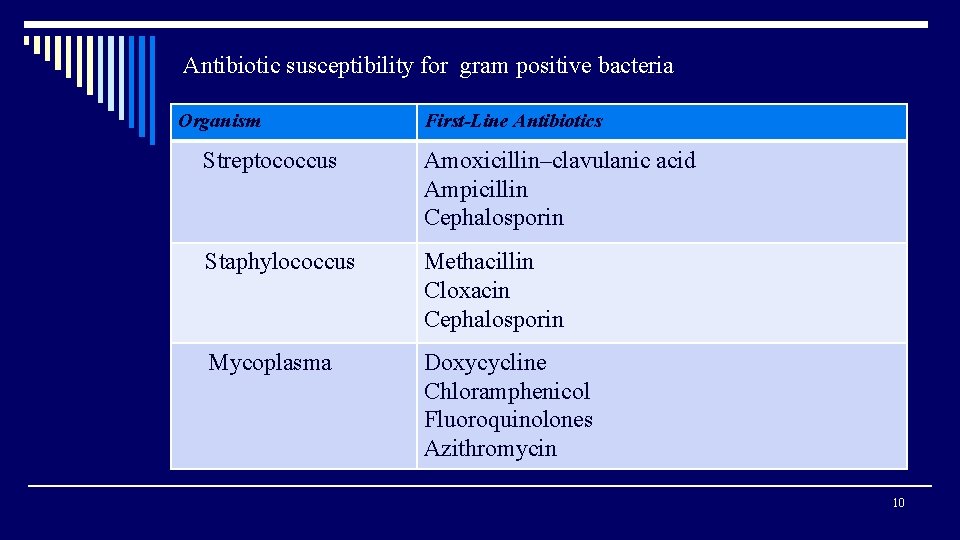

Antibiotic susceptibility for gram positive bacteria Organism First-Line Antibiotics Streptococcus Amoxicillin–clavulanic acid Ampicillin Cephalosporin Staphylococcus Methacillin Cloxacin Cephalosporin Mycoplasma Doxycycline Chloramphenicol Fluoroquinolones Azithromycin 10
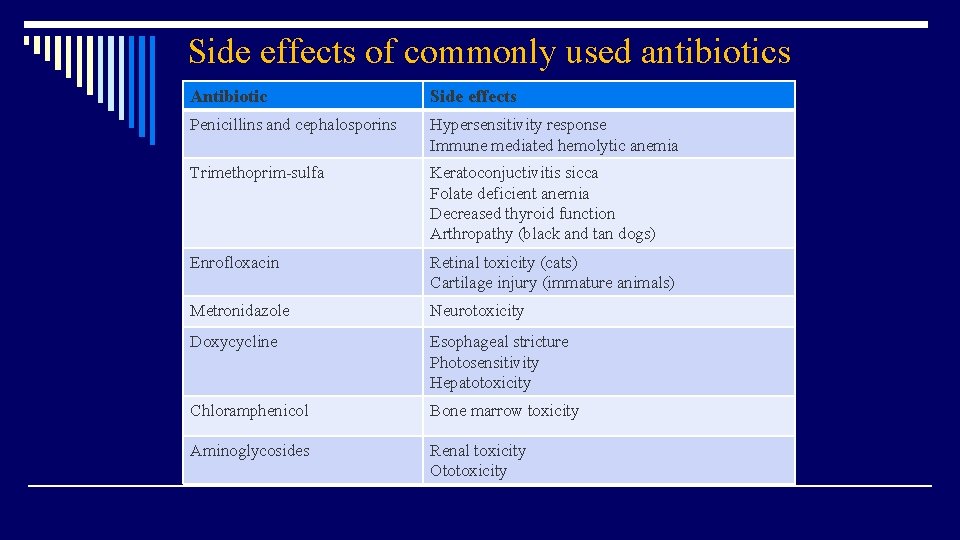

Side effects of commonly used antibiotics Antibiotic Side effects Penicillins and cephalosporins Hypersensitivity response Immune mediated hemolytic anemia Trimethoprim-sulfa Keratoconjuctivitis sicca Folate deficient anemia Decreased thyroid function Arthropathy (black and tan dogs) Enrofloxacin Retinal toxicity (cats) Cartilage injury (immature animals) Metronidazole Neurotoxicity Doxycycline Esophageal stricture Photosensitivity Hepatotoxicity Chloramphenicol Bone marrow toxicity Aminoglycosides Renal toxicity Ototoxicity

Antifungal Therapy o. Fungal infection in the respiratory tract most commonly involves Cryptococcus neoformans or Aspergillus fumigatus in the nasal cavity of cats or dogs, respectively, and Histoplasma capsulatum, Blastomyces dermatitidis, or Coccidioides immitis organisms in the lower respiratory tract. Nasal aspergillosis is a special condition, which appears to respond best to extensive debridement of fungal plaques and topical antifungal therapy , long -term therapy (6 weeks to over 12 months) must be anticipated. fungistatic or fungicidal agents administered orally or parenterally should be chosen.

o The azoles (itraconazole, fluconazole, voriconazole, posaconazole) are fungistatic agents that inhibit P 450 enzymes involved in synthesis of ergosterol, a key component of the fungal cell wall. o Itraconazole can be used as sole therapy for nasal or pulmonary fungal infection or can be used following amphotericin B for sustained control of disease. o Itraconazole is excreted by the liver, and side effects of therapy include hepatic toxicity, dermatotoxicity, and anorexia. o Fluconazole is renally excreted thus a reduced dosage is recommended for animals with renal insufficiency.

o Terbinafine is an allylamine fungistatic agent that is thought to act through inhibition of epoxidase during the synthesis of ergosterol for the fungal cell membrane. Side effects are apparently rare. o Flucytosine is a pyrimidine analog and a fungistatic drug It is used only in combination with other antifungal agents because it is a relatively weak antifungal and because of rapid development of resistance.

o Amphotericin B is a fungicidal drug that creates breaks in the fungal cell membrane. o Because it is highly nephrotoxic, aggressive diuresis with 0. 9% saline (20– 40 ml/kg over 1 hours) is recommended prior to administration. o After saline diuresis, the infusion line is flushed with 5% dextrose to avoid precipitation of the amphotericin in saline, drug should be protected from light during administration. o A test dose of 0. 5 mg/kg in 5% dextrose solution is administered intravenously over 5– 6 hours on the first day of therapy. Body temperature is continually measured during the infusion because of the likelihood of a drug fever.

o On the day after administration, renal parameters are measured, and if values are within normal limits, a dose of 1. 0 mg/kg can be administered on the following days. o Amphotericin B can also be used SC in animals that cannot be hospitalized, or cannot be treated with oral medications. Amphotericin B at a dose of 0. 5– 0. 8 mg/kg is diluted in 400– 500 m. L of 0. 45% Na. Cl/2. 5% dextrose and administered subcutaneously two to three times weekly until disease has resolved

o To reduce the likelihood of renal insufficiency, administration of amphotericin B lipid complex is recommended. The drug is given as a 20– 30 -minute infusion of 0. 5– 1. 0 mg/kg and pretreatment with saline diuresis is not a requirement.
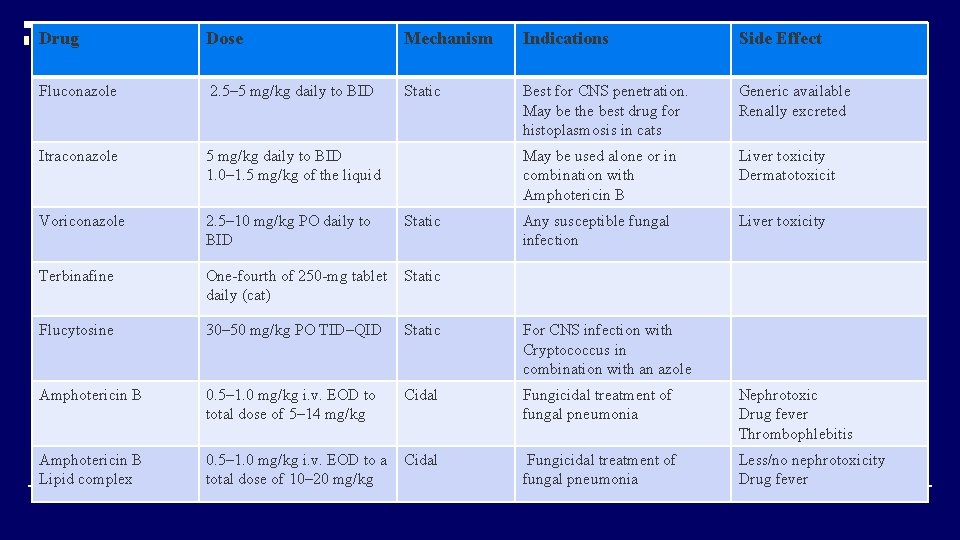
Drug Dose Mechanism Indications Side Effect Fluconazole 2. 5– 5 mg/kg daily to BID Static Best for CNS penetration. May be the best drug for histoplasmosis in cats Generic available Renally excreted Itraconazole 5 mg/kg daily to BID 1. 0– 1. 5 mg/kg of the liquid May be used alone or in combination with Amphotericin B Liver toxicity Dermatotoxicit Voriconazole 2. 5– 10 mg/kg PO daily to BID Static Any susceptible fungal infection Liver toxicity Terbinafine One-fourth of 250 -mg tablet daily (cat) Static Flucytosine 30– 50 mg/kg PO TID–QID Static For CNS infection with Cryptococcus in combination with an azole Amphotericin B 0. 5– 1. 0 mg/kg i. v. EOD to total dose of 5– 14 mg/kg Cidal Fungicidal treatment of fungal pneumonia Nephrotoxic Drug fever Thrombophlebitis Amphotericin B Lipid complex 0. 5– 1. 0 mg/kg i. v. EOD to a total dose of 10– 20 mg/kg Cidal Fungicidal treatment of fungal pneumonia Less/no nephrotoxicity Drug fever

Antiviral Therapy o Viruses (feline herpes virus-1: FHV-1; feline calicivirus: FCV) have been implicated as major etiologic agents in acute feline upper respiratory disease. o Generally self-limiting, and antiviral therapy is rarely used. o In the chronic disease syndrome, Clinical signs may be due to direct cytopathic effects mediated by the virus or due to the host’s immunologic response to infection.

o Lower respiratory tract disease due to viral infection is less common but may occur with some upper respiratory tract viruses or due to infection with the mutated coronavirus(feline infectious peritonitis virus: FIP) o Many respiratory manifestations of feline infectious peritonitis virus are related to the host’s immunologic response and subsequent vasculitis. o definitive diagnosis of FIP remains difficult. o Antiviral therapy is NOT RECOMMENDED in suspect cases. 20

o Acyclovir and valacyclovir, a prodrug of acyclovir, are not recommended o o because of poor efficacy against FHV-1 and unacceptable toxicity. The most promising drug for use against FHV-1 -related ocular disease is famcyclovir although this drug has not been evaluated specifically for chronic nasal disease in the cat. Oral lysine (250– 500 mg PO BID) might be helpful in kittens or cats with upper respiratory disease that is presumed to be viral in origin. Lysine competes with arginine in FHV-1 protein synthesis, and inhibition of synthetic activity decreases replication of the virus. Supplementation does not result in systemic arginine depletion and no side effects have been reported.

Glucocorticoids o Glucocorticoids and nonsteroidal anti-inflammatory agents (NSAIAs) are commonly used classes of drugs that provide potent anti-inflammatory actions to treat a variety of conditions. o The major anti-inflammatory actions of these drug classes include suppression of pro-inflammatory cytokines and other mediators. o Glucocorticoids are less specific in their actions compared to NSAIAs, influencing metabolic and immune system functions. .

o Glucocorticoids enter cells largely through passive diffusion and bind to cytosolic receptors. Receptor number and type vary between tissues. Upon binding, receptors rapidly move into the nucleus where they exert molecular effects. o All types of inflammation, including those arising from infectious, traumatic, hypersensitivity or other immune response, and neoplastic etiologies, can be impacted by glucocorticoids o Effects of glucocorticoids are dosage-dependent, and can vary among species. Dosages should be titrated to maximize therapeutic benefit while minimizing adverse effects. 23

Selected Actions of Glucocorticoids o Anti-Inflammatory Effects o o o o • Suppression of pro-inflammatory cytokines and chemokines (e. g. , interleukin [IL]-1, IL-2, IL- 6, IL-8, tumor necrosis factor [TNF]-alpha) • Diminished inflammatory enzyme activity (e. g. , cyclooxygenase [COX]-2, phospholipase [PL] A 2) • Suppression of T-cell proliferation • Inhibition of mononuclear phagocytosis and of chemotaxis • Apoptosis of activated lymphocytes • Induction of anti-inflammatory cytokines (e. g. , IL-10, transforming growth factor [TGF]-beta) • Stabilization of lysosomal membranes 24

o Endocrine Effects o Suppression of adrenocorticotropic hormone production and decrease in thyroid stimulating hormone and thyroid hormone production. o Neurologic and Muscular Effects o Behavior change and muscle weakness o Renal Effects o o o Increase in glomerular filtration rate Inhibition of antidiuretic response in renal tubules Proteinuria Retention of water, sodium, and chloride Excretion of potassium and calcium 25
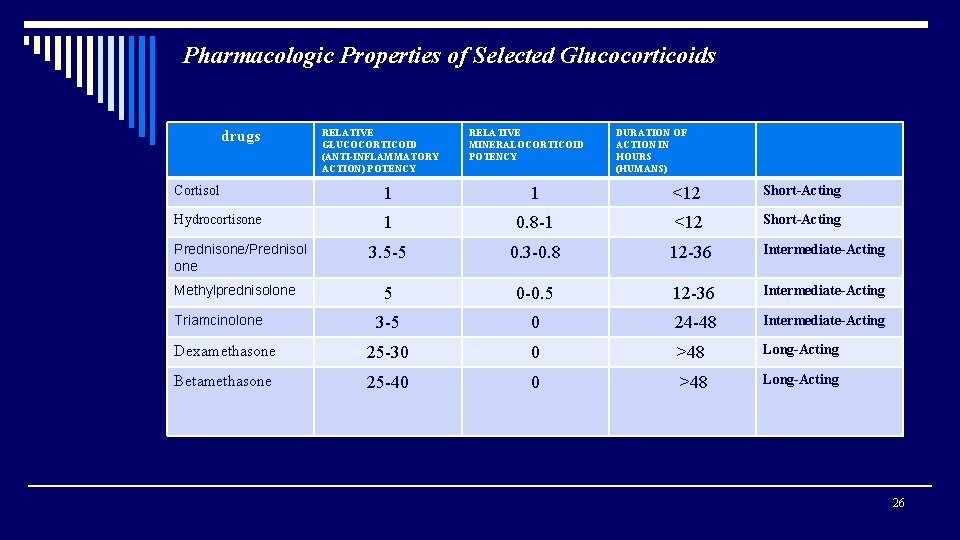
Pharmacologic Properties of Selected Glucocorticoids drugs RELATIVE GLUCOCORTICOID (ANTI-INFLAMMATORY ACTION) POTENCY RELATIVE MINERALOCORTICOID POTENCY DURATION OF ACTION IN HOURS (HUMANS) Cortisol 1 1 <12 Short-Acting Hydrocortisone 1 0. 8 -1 <12 Short-Acting 3. 5 -5 0. 3 -0. 8 12 -36 Intermediate-Acting 5 0 -0. 5 12 -36 Intermediate-Acting 3 -5 0 24 -48 Intermediate-Acting Dexamethasone 25 -30 0 >48 Long-Acting Betamethasone 25 -40 0 >48 Long-Acting Prednisone/Prednisol one Methylprednisolone Triamcinolone 26

o Hematopoietic Effects o • Increase in circulating neutrophils, monocytes o • Decrease in circulating lymphocytes, eosinophils o • Sequestration of lymphocytes; involution of lymphoid tissue o • Increase in circulating red blood cells, platelets o Metabolic Effects o • Increase in hepatic gluconeogenesis o • Increase in protein catabolism o • Mobilization of free fatty acids o • Antagonism of insulin activity 27

o Prednisone, prednisolone, and dexamethasone are commonly used systemic glucocorticoids in dogs and cats. o Cats might be more resistant to the effects of glucocorticoids and require relatively higher dosages than dogs. cats also are more sensitive to serious glucocorticoid adverse effects such as diabetes and congestive heart failure. o Unfortunately, scientific evidence for glucocorticoid dosing regimens in dogs and cats is lacking. o A common initial anti-inflammatory dosage of predniso(lo)ne is 0. 5 - 1 mg/kg/day (dogs) or 1 -2 mg/kg/day (cats). Immunosuppressive dosages range from 2 -4 mg/kg/day in dogs and 2 -8 mg/kg/day in cats.

o Several considerations should be weighed when choosing among the many options for anti-inflammatory glucocorticoid therapy, including desired rapidity of onset, site of activity, and duration of treatment. o In cases when rapid onset of activity is needed (e. g. , respiratory inflammation leading to airway obstruction), injectable succinate or phosphate salts of glucocorticoids are recommended. o The duration and dose of corticosteroid therapy will depend upon the severity and chronicity of respiratory signs, the extent of the infiltrates on radiographs, and the degree of inflammation on cytology. o The length of therapy required to alleviate signs , long-term therapy (2– 3 months for dogs with chronic bronchitis and 4– 5 months for dogs with eosinophilic disease) can be anticipated in most cases.

Adverse Effects and Contraindications for the Use of Glucocorticoids o Adverse effects of glucocorticoid therapy result frequently from prolonged use of high dosages. o Exogenous glucocorticoids can suppress the HPAA and cause iatrogenic hyperadrenocorticism. Clinical signs are similar including polyuria, polydipsia, pendulous abdomen, and dermatologic change. o Other adverse effects include : muscle wasting, weakness, ligament rupture, obesity, hypercoagulability, insulin resistance and diabetes, a wide range of GI effects, from subclinical gastric mucosal injury to GI ulceration and perforation at high dosages.

o Glucocorticoids should not be used concurrently with NSAIA therapy due to the increased risk of GI ulceration. o Because glucocorticoids may affect cardiac muscle function and cause water retention, cautious use is recommended in patients with heart disease as congestive heart failure is a potential risk, especially in cat. o Topical ocular glucocorticoids should not be used in patients with corneal ulceration or infection, as ulcers can worsen and stromal melting can occur. 31

Corticosteroids (Cont’d) Drug Formulation Beclomethasone Inhaler 50 mcg / dose (BID) Inhaler 250 mcg / dose (BID) 32

Corticosteroids (Cont’d) Drug (Cont’d) Formulation Budesonide Inhaler 50 mcg / dose (BID) Inhaler 200 mcg / dose (BID) Inhaler 100 mcg / dose (BID) Inhaler 200 mcg / dose (BID) Inhaler 400 mcg / dose (BID) 33

Corticosteroids (Cont’d) Drug (Cont’d) Formulation Fluticasone Inhaler 25 mcg / dose (MDI) Inhaler 50 mcg / dose (MDI) Inhaler 125 mcg / dose (MDI) Inhaler 250 mcg / dose (MDI) Inhaler 50 mcg / dose (Accuhaler) Inhaler 100 mcg / dose (Accuhaler) Inhaler 250 mcg / dose (Accuhaler) 34

Corticosteroids (Cont’d) o Nursing alerts n n Rinse mouth with water without swallowing after administration to reduce the risk of candidiasis If taking bronchodilators by inhalation, use bronchodilators several minutes before the corticosteroid to enhance application of the corticosteroid into the bronchial tract 35

Bronchodilators o The two main classes of bronchodilators used in veterinary medicine are methylxanthine derivatives (theophylline) and beta-agonists, these agents provide only mild relaxation of airway smooth muscle and bronchodilation. o Methylxanthine agents such as theophylline and aminophylline are used clinically as bronchodilators. o Theophylline may provide other beneficial effects by increasing diaphragmatic muscle strength, improving pulmonary perfusion, reducing respiratory effort, and stimulating mucociliary clearance (in dogs, but not in cats). o dose of 10 mg/kg PO every 12 hours in a dog and 15 or 19 mg/kg once daily in the evening for the cat.

Adverse effects of methylxanthines o Include gastrointestinal upset, tachycardia, and hyperexcitability. o Theophylline metabolism is influenced by many factors, including fiber in the diet, smoke in the environment, congestive heart failure, and the use of other drugs. a reduced dosage can be considered initially (5 mg/kg every 12 hours in a dog and 5– 10 mg/kg once daily in the cat). o Methylxanthines are relatively weak bronchodilators and while they may be beneficial for adjunctive therapy in control of clinical signs, they are not recommended for use in an acute or emergency situation.
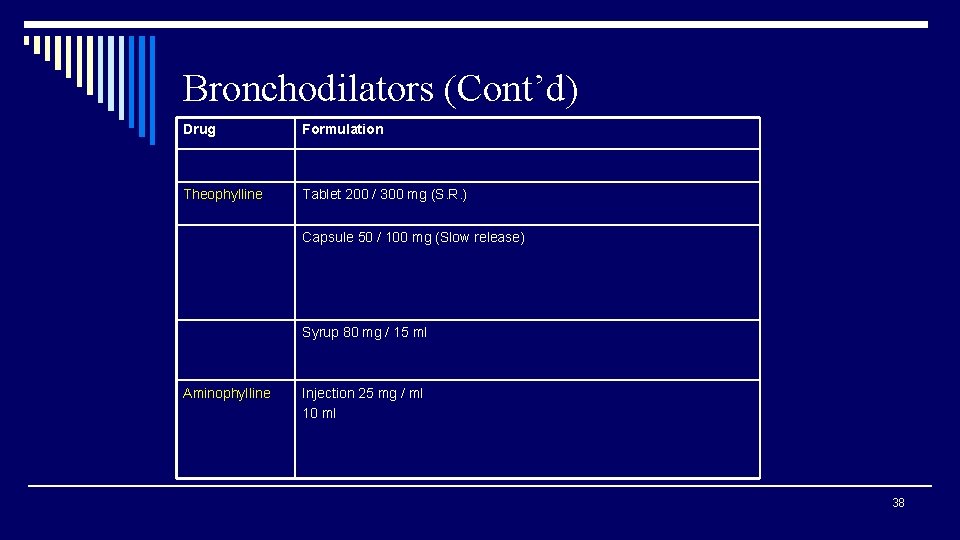

Bronchodilators (Cont’d) Drug Formulation Theophylline Tablet 200 / 300 mg (S. R. ) Capsule 50 / 100 mg (Slow release) Syrup 80 mg / 15 ml Aminophylline Injection 25 mg / ml 10 ml 38

ü Beta-agonists o Administration of a beta-2 agonist (terbutaline or albuterol) results in o o o bronchodilation due to direct relaxation of airway smooth muscle. The recommended dose is 0. 01 mg/kg parenterally or 0. 625 mg/cat PO BID. Dogs can receive 0. 625– 5 mg PO every 12 hours These bronchodilators also resulted in a reduction in the severity of the pulmonary infiltrate. Chronic use of a beta-agonist can result in downregulation of beta-receptor density and decreased efficacy of the drug. Methylxanthines and beta-agonists may result in excitability or tremors during initial therapy, but animals usually become accustomed to the drug.
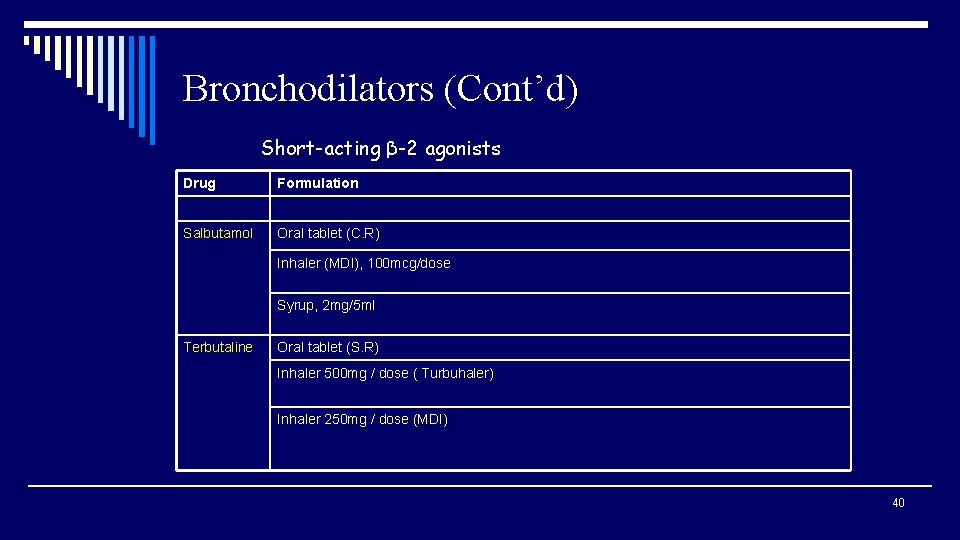

Bronchodilators (Cont’d) Short-acting β-2 agonists Drug Formulation Salbutamol Oral tablet (C. R) Inhaler (MDI), 100 mcg/dose Syrup, 2 mg/5 ml Terbutaline Oral tablet (S. R) Inhaler 500 mg / dose ( Turbuhaler) Inhaler 250 mg / dose (MDI) 40
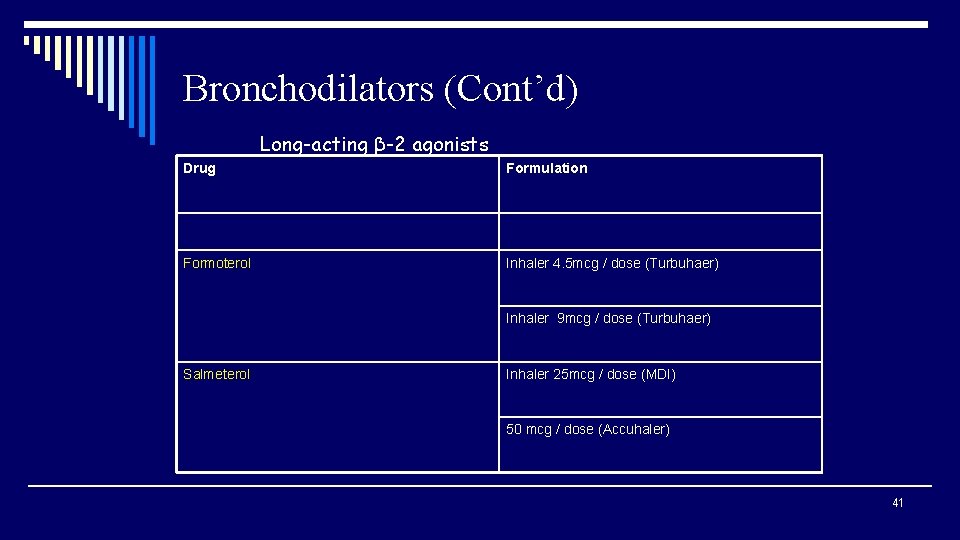

Bronchodilators (Cont’d) Long-acting β-2 agonists Drug Formulation Formoterol Inhaler 4. 5 mcg / dose (Turbuhaer) Inhaler 9 mcg / dose (Turbuhaer) Salmeterol Inhaler 25 mcg / dose (MDI) 50 mcg / dose (Accuhaler) 41

Bronchodilators (Cont’d) n Other adrenoceptor agonists p Less suitable & less safe for use as bronchodilators because they are more likely to cause arrhythmias & other side effects n Ephedrine p Adrenaline (epinephrine) injection is used in the emergency treatment of acute allergic and anaphylactic reactions 42

Bronchodilators (Cont’d) o Antimuscarinic bronchodilators n n Blocks the action of acetylcholine in bronchial smooth muscle, this reduces intracellular GMP, a bronchoconstrictive substance Used for maintenance therapy of bronchoconstriction associated with chronic bronchitis & emphysema 43

Bronchodilators (Cont’d) Drug Formulation Ipratropium Inhaler 20 mcg / dose (MDI) Tiotropium Inhaler 18 mcg /dose 44

Bronchodilators (Cont’d) o Adverse effects: n n n Dry mouth Nausea Constipation 45

Mucolytics o Marked controversy exists concerning the utility of mucolytic agents in human medicine, and there is little information on the use or efficacy of these preparations in veterinary patients. o Conditions that might respond to mucolytic agents include feline chronic rhinosinusitis, canine rhinitis, chronic bronchitis, bronchiectasis, and pneumonia-associated with production of viscous secretions(e. g. , Mycoplasma). o Mucolytic/expectorant agents such as N-acetylcysteine, bromhexine, Scarboxymethylcysteine, ambroxol, guaifenesin, and iodinated glycerol can thin the viscosity of mucin-containing secretions.

Mucolytics o These drugs act by a variety of mechanisms including breakage of disulfide bonds in airway mucoproteins, stimulation of serous airway secretions. o Nbulization with N-acetylcysteine result in bronchoconstriction or epithelial injury and this route is not recommended. o N-acetylcysteine is reported to provide a variety of antioxidant effects that might prove beneficial in respiratory patients. dose of 30– 60 mg/kg (not to exceed 600 mg) PO BID–TID 47

Antitussive Agents o The cough reflex is of major importance in animals because it serves the essential function of clearing secretions from the airway. Suppression of this reflex before resolution of inflammation can be deleterious because mucus can become trapped in small airways. o When clinical signs suggest that inflammation is resolving yet the cough persists, cough suppression is desirable because chronic coughing can lead to repeated airway injury and syncopal events. o Over-the-counter cough suppressants rarely are effective in dogs, and narcotic cough suppressants are most effective. o Butorphanol can be prescribed, a couple of drops of injectable solution deposited on the tongue can be effective, but neither the dosage needed nor the dose-effect relationship has been studied.
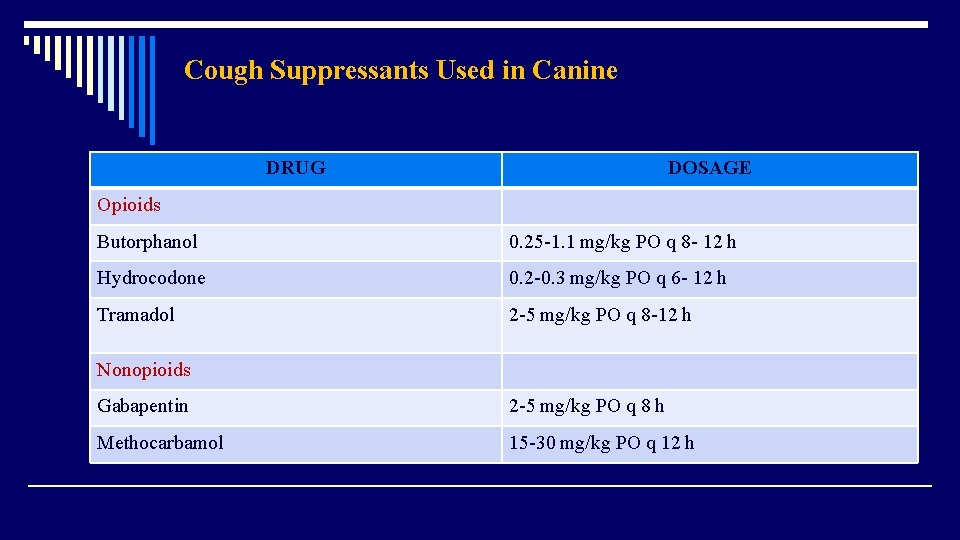
Cough Suppressants Used in Canine DRUG DOSAGE Opioids Butorphanol 0. 25 -1. 1 mg/kg PO q 8 - 12 h Hydrocodone 0. 2 -0. 3 mg/kg PO q 6 - 12 h Tramadol 2 -5 mg/kg PO q 8 -12 h Nonopioids Gabapentin 2 -5 mg/kg PO q 8 h Methocarbamol 15 -30 mg/kg PO q 12 h

Antihistamines o H 1 receptor antagonists Inhibit smooth muscle constriction in blood vessels & respiratory & GI tracts n Decrease capillary permeability n Decrease salivation & tear formation o Used for variety of allergic disorders to prevent or reverse target organ inflammation n 50

Antihistamines (Cont’d) o First-generation H 1 receptor antagonists n Non-selective/sedating n Bind to both central & peripheral H 1 receptors n Usually cause CNS depression (drowsiness, sedation) but may cause CNS stimulation (anxiety, agitation), especially in cats n Also have substantial anticholinergic effects 51
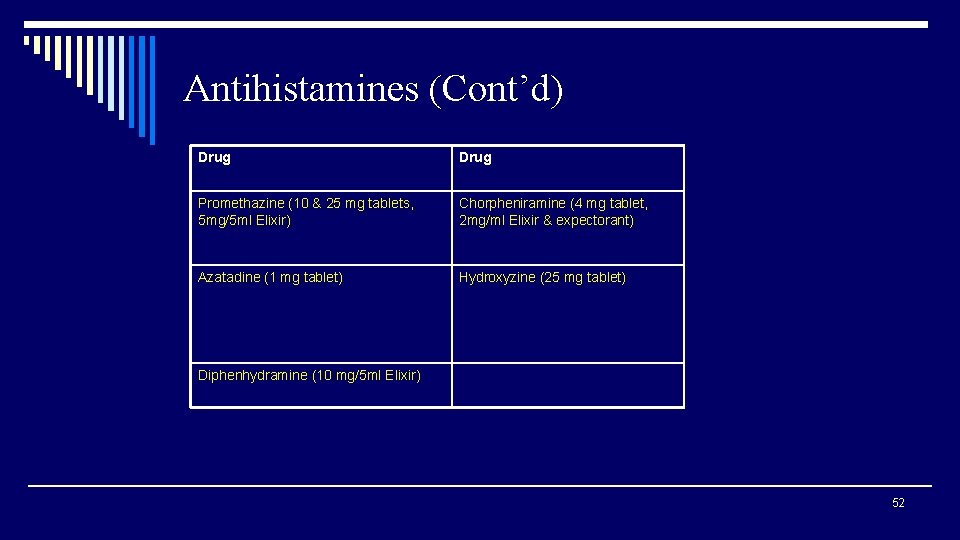

Antihistamines (Cont’d) Drug Promethazine (10 & 25 mg tablets, 5 mg/5 ml Elixir) Chorpheniramine (4 mg tablet, 2 mg/ml Elixir & expectorant) Azatadine (1 mg tablet) Hydroxyzine (25 mg tablet) Diphenhydramine (10 mg/5 ml Elixir) 52

Antihistamines (Cont’d) o Adverse effects: n n Sedation Dry mouth GI disturbances Urinary retention 53

Antihistamines (Cont’d) o Second-generation H 1 receptor antagonists n n n Selective/non-sedating Cause less CNS depression because they are selective for peripheral H 1 receptors & do not cross blood-brain barrier Longer-acting compared to first-generation antihistamines 54

Antihistamines (Cont’d) Drug Acrivastine (Semprex) Cetirizine (Zyrtec) Desloratadine (Aerius) Fexofenadine (Telfast) Loratadine (Clarityne) 55

Antihistamines (Cont’d) o Adverse effects: n n May cause slight sedation Terfenadine may interact with, ketoconazo erythromycin, cisapride or grapefruit juice, leading to potentially serious ECG changes e. g. 56

Leukotriene receptor antagonists o Act by suppressing the effects of leukotrienes, compounds that promote bronchoconstriction as well as eosinophil infiltration, mucus productions, & airway edema. o Help to prevent acute asthma attacks induced by allergens & other stimuli. o Indicated for long-term treatment of asthma. o Leukotriene modifiers are not effective for use in acute episodes of acute bronchial asthma because their effects are not rapidly observed in patients. 57

Leukotriene receptor antagonists (Cont’d) o Dosage: n n n Montelukast (0. 25– 0. 50 mg/kg/day PO) Zafirlukast (1– 2 mg/kg PO q 24 h bid) Zileuton (5 -lipoxygenase inhibitor, unknown dosage ) 58

Leukotriene receptor antagonists (Cont’d) o Adverse effects: n n n GI disturbances Hypersensitivity reactions Restlessness 59

Cromoglycates o Stabilise mast cells & prevent the release of bronchoconstrictive & inflammatory substances when mast cells are confronted with allergens & other stimuli o Only for prophylaxis of acute asthma attacks 60

Cromoglycates (Cont’d) Drug Formulation Cromoglycate Na Inhaler (1 mg & 5 mg/dose) four times daily, may be increased to six to eight times daily Nedocromil Sodium Inhaler 2 mg / dose, four times daily 61

Cromoglycates (Cont’d) Adverse effects Nursing Alerts Transient Bronchospasm , coughing, throat irritation , A selective β 2 agonist such as salbutamol or terbutaline may be inhaled a few minutes beforehand 62

Cromoglycates (Cont’d) o Nursing Alerts (Cont’d) n Cromoglycates are for long-term prophylaxis, patients should administer on a regular schedule & the full therapeutic effects may take several weeks to develop some animals are hypersensitive to this drugs 63

Nutritional Therapy o Obesity is a common finding in the pet population. o Obesity results in poor lung expansion, Increasing abdominal pressure on the diaphragm, reduced thoracic volume, or increased work of breathing and decreasing thoracic wall compliance , o Improvements in exercise tolerance and arterial oxygenation can be seen with weight loss alone. o A 1– 2% weight loss per week is desirable but difficult to achieve (German et al. 2007). o Marked energy restriction and rigorous owner cooperation is required. 64

Routes of Administration o Parenteral administration of drugs is indicated for any animal with swallowing disorders, vomiting, or malabsorptive intestinal disease. o For treatment of life-threatening disease, parenteral administration of a microbiocidal agent rather than a static drug provides optimal therapy. o An exception to this might be the animal with severe pulmonary infiltrates associated with fungal pneumonia. Rapid killing of large numbers of organisms can lead to acute respiratory distress syndrome when an exuberant inflammatory response damages the alveolocapillary membrane, resulting in noncardiogenic pulmonary edema.

Cont… ü Nebulization: o Nebulization creates extremely small fluid particles for inhalation. The o o site of deposition of these particles depends on their size, charge , and other parameters. Humidifiers create larger droplets that do not reach lower airways. Nebulizers create smaller particles (0. 5 to 3 micrometers) that penetrate more deeply into the respiratory tract. Nebulized liquids can be delivered to dogs and cats via face mask, or the animal can be placed in a closed tent or aquarium-type container. Tent/tank nebulization could be adequate for saline nebulization, medications should be administered via mask. 66

Cont… o Simple saline nebulization improve mucus fluidity and therefore function of the mucociliary escalator. o Treat animals with pneumonia with saline nebulization from one to four times daily. o Nebulization also can be used for delivering medications including antimicrobial drugs bronchodilators, glucocorticoids, or mucolytics agents (caution—not all liquid drug forms are suitable for nebulization). o Administration of drugs not specifically developed for inhalational delivery can be associated with adverse reactions including severe bronchoconstriction and with damage to the equipment.
![o Antimicrobials designed for inhalational delivery (e. g. , Tobramycin [Tobi]) are prohibitively expensive o Antimicrobials designed for inhalational delivery (e. g. , Tobramycin [Tobi]) are prohibitively expensive](http://slidetodoc.com/presentation_image_h/1a37aed958bb84799307520380a33fff/image-68.jpg)
o Antimicrobials designed for inhalational delivery (e. g. , Tobramycin [Tobi]) are prohibitively expensive for veterinary use. o Aminoglycosides designed for intravenous administration often are used instead. gentamicin 6 to 8 mg/kg, qs 5 to 10 m. L in saline, via nebulization for animals with susceptible airway pathogens once daily as an adjunct to systemic antimicrobial administration. o Nebulization of mucolytic agents results in bronchoconstriction and thus is not routinely advocated. (such as acetylcystein).

FLUID THERAPY IN PULMONARY DISEASE o When considering patients with pulmonary disease, it seems more sensible not to question what fluid to use but rather how much. o A limited fluid therapy strategy that ensures euvolemia is advisable in patients with pulmonary dysfunction. Fluid restriction could increase the risk of ARDS and multiorgan failure. o Experimental studies on dogs subjected to pulmonary contusions and hemorrhagic shock have shown no difference in EVLW (extravascular lung water) between volume resuscitation with plasma or moderates of crystalloid fluid administration. o Faster rates (> 30 m. L/kg/h) of isotonic crystalloid fluid infusion were associated with increases in EVLW and histologic evidence of worsening of pulmonary contusions. o The available evidence suggest that patients with pulmonary contusions after trauma should be resuscitated conservatively by maintaining mean arterial blood pressure of more than 70 mm Hg to ensure adequate tissue perfusion.

FLUID THERAPY IN ACUTE RESPIRATORY DISTRESS SYNDROME(ARDS) o o o Patients who have acute lung injury and ARDS have increased permeability of the alveolar-capillary barrier as a result of inflammation. Increased permeability results in loss of the colloid osmotic pressure differential between the capillary and interstitium. In these situations, increases in capillary hydrostatic pressure could result in fluid exudation into the interstitium. In patients with early ARDS, colloid infusion such as albumin and dextran-40 improves hemodynamic and oxygen transport variables more effectively and is not associated with deleterious pulmonary effects. In the terminal stages of ARDS, any fluid administered worsens pulmonary function and the patient’s condition

o Maintaining intravascular volume at the lowest level consistent with adequate o o o systemic perfusion remains a reasonable objective in ARDS patients. If systemic perfusion cannot be maintained after restoration of intravascular volume, treatment with vasopressors or positive inotropes should be initiated immediately. When managing these challenging cases, clinicians should remember that pulmonary function may deteriorate with any type of fluid administration. In hypovolemic or hypotensive patients, small boluses of isotonic crystalloids or colloids should be given to restore perfusion, Avoiding rates of more than 30 m. L/kg for isotonic crystalloids. If perfusion is not restored by adequate volume resuscitation, vasopressors or positive inotropes should be administered 71
- Slides: 71