Respiratory System Gas Exchange and Oxygenation Gas Exchange
























- Slides: 34

Respiratory System Gas Exchange and Oxygenation

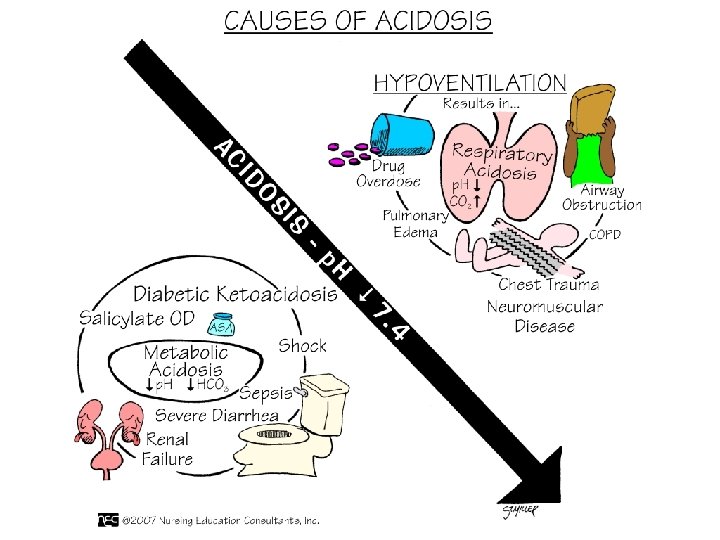
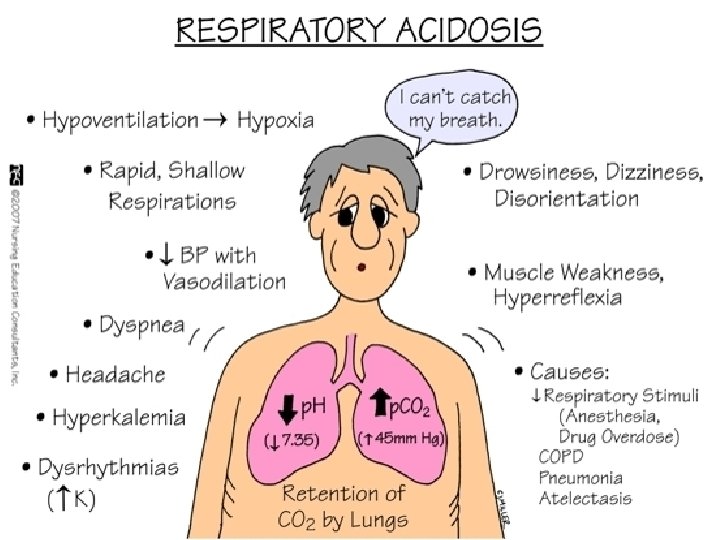
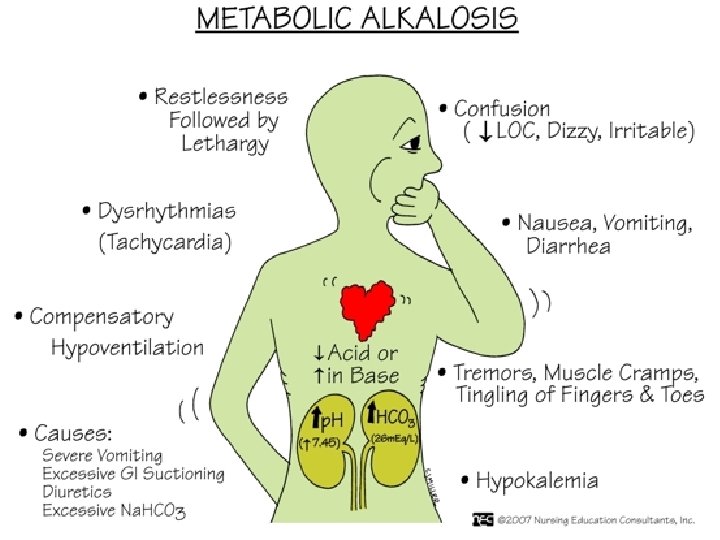
Gas Exchange • ABG interpretation done in NURE 131 • Reread chapter 18 • Focus on 2 aspects of acid/base balance • Respiratory alterations • Respiratory acidosis • Respiratory alkalosis • Focus on oxygenation • Hypoxemia

ABG Interpretation Review • Acid/Base balance • Regulation of p. H • Normal p. H required for normal cellular function • Controlled by respiratory system and renal system ACIDOTIC p. H 7. 35 – p. H 7. 45 ALKALOTIC








ABG Interpretation Normal Values • p. H • CO 2 • PO 2 • Sat • HCO 3 • 7. 35 - 7. 45 • 35 - 45 • 80 - 120 • > 95% • 22 - 26

Question #1 • Interpret the following ABG result: p. H 7. 32 CO 2 50 PO 2 62 Sat 91% HCO 3 28 a. b. c. d. Compensated respiratory acidosis Uncompensated respiratory acidosis Compensated metabolic acidosis Uncompensated metabolic acidosis

Question #2 • Interpret the following ABG: p. H 7. 49 CO 2 32 PO 2 78 Sat 98% HCO 3 24 a. b. c. d. Compensated respiratory alkalosis Uncompensated respiratory alkalosis Compensated metabolic alkalosis Uncompensated metabolic alkalosis

Question #3 • Which of the following ABG results would the nurse expect to see on a client with stable, chronic, hypercapnic COPD? a. b. c. d. p. H 7. 31 p. H 7. 40 p. H 7. 35 p. H 7. 49 CO 2 52 38 50 33 PO 2 68 PO 2 78 PO 2 62 PO 2 88 Sat Sat 93% 98% 91% 99% HCO 3 26 24 28 25

Question #4 A nurse receives the following ABG results on a client with pneumonia (p. H 7. 37 CO 2 35 PO 2 50 Sat 86% HCO 3 26), the priority nursing action at this time would be to: a. Administer 2 liters oxygen to the client immediately and call Rapid Response STAT b. Call the physician’s office to report the results c. Raise the HOB and take vital signs d. Apply a pulse oximeter for continuous readings •

Oxygen Administration • Purpose: treat hypoxia, deliver increased oxygen to tissues, maintain adequate oxygenation • Indications: reduced arterial O 2 noted in ABG • PO 2 less than 60 • Sat less than 90% • PO 2 should be 80 -100 • S/S respiratory distress caused by hypoxia: change in mental status, restlessness, agitation, respiratory rate increases, use of accessory muscles, diaphoresis, cyanosis (late stage)

Oxygen Administration: Potential Complication in Select Patients • Normal breathing is controlled by Medulla and Pons • Stimulated by increased CO 2 levels to maintain normal CO 2 level and normal p. H • COPD patients with hypercapnea (retainers) have higher CO 2 levels and over time their body adjusts to this level • They are stimulated to breath due to decreased oxygen levels instead of carbon dioxide • If oxygen given to them at high dose it depresses the breathing stimulation that they are depending on, which can potentially result in apnea

Oxygen Administration: Potential Complication in Select Patients • In this patient population be cautious giving oxygen • Give oxygen 1 -2 liters • Have MD order • There are going to be times that these patients require higher levels of oxygen • Must maintain cerebral oxygenation • Can tolerate Sa. O 2 around 88% with confirmation by MD • Many end up requiring mechanical ventilation at these points

Oxygen • Nasal cannula • Simple face mask • Venti mask • Face tent • Partial rebreather • 100% rebreather

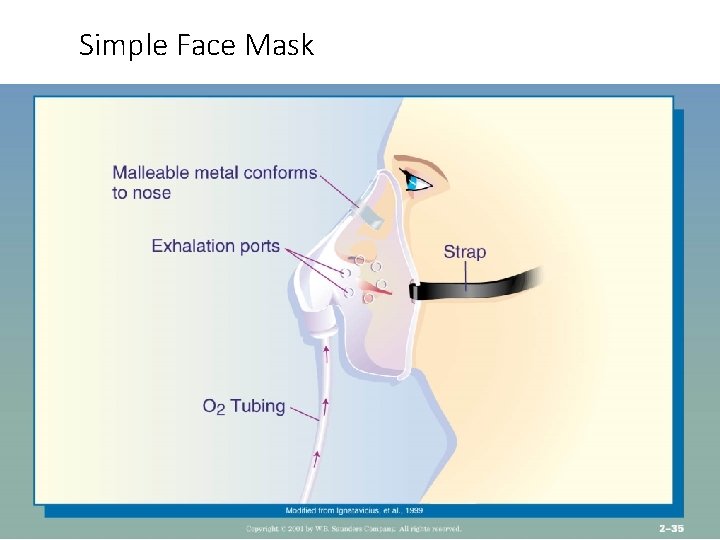
Oxygen Delivery Systems • Each liter of oxygen delivers approximately 3%. When you add that to the amount in room air (21%) you have the total • Low flow-delivered by nasal cannula 1 - 6 L • Simple face mask 5 - 10 l/min • Venturi system determine by adapters used • Colored adapters allow a mixture of room air and oxygen • Also need to follow directions for amount of l/min • Face tent- at 4 -8 L/min • Non-rebreather- rebreather mask-10 -15 l/min deliver 80 -100% oxygen Brunner p. 637, 275 -1

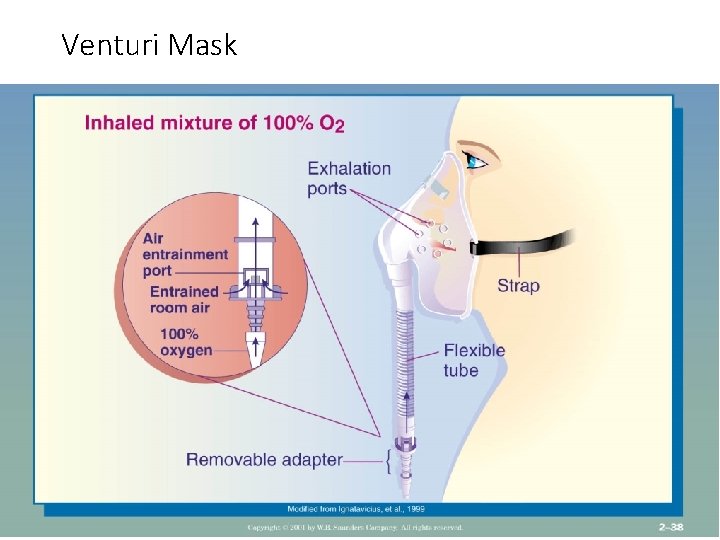
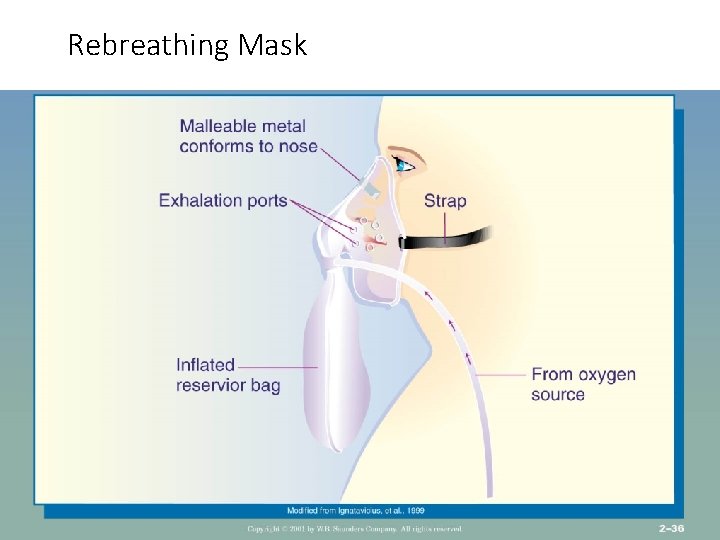
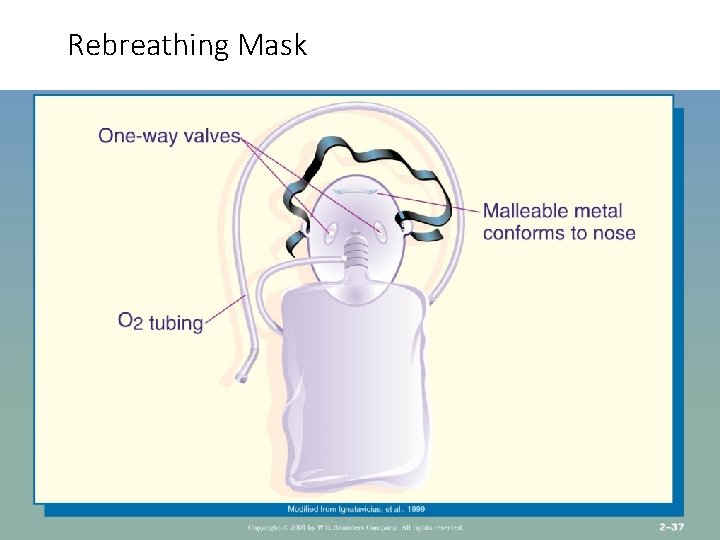
High Flow Delivery • Venturi Mask-or Venti Mask – 4 -15 L/Min 24 -50% O 2, delivers the most precise O 2 concentration • Non rebreather mask- mask with reservoir and one way valve. Used when O 2 concentration >60% is required. Mask must be snug • High need and use of mask interfere with oral intake • Both need humidification-decrease dryness to mucosa. Prevents thickening of secretions, loosens secretions, prevents mucus plugs

Simple Face Mask

Venturi Mask

Rebreathing Mask

Rebreathing Mask

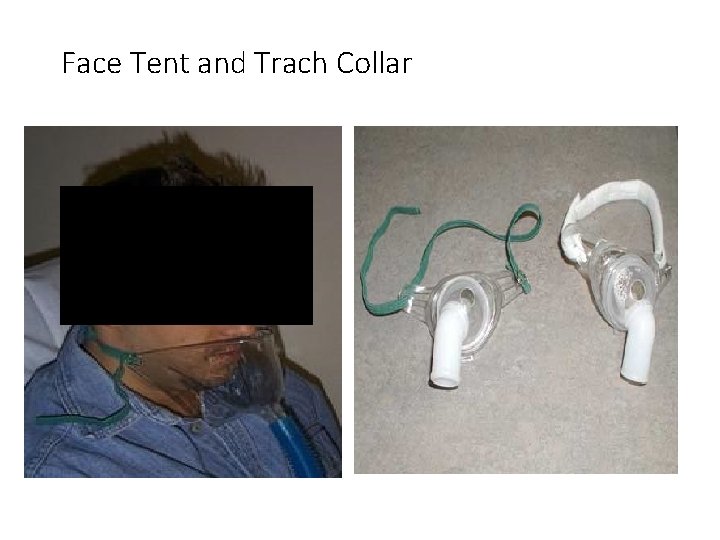
Face Tent and Trach Collar

Oxygen With Artificial Airway • Require humidification to the airway • Bypasses normal filtering of nose • Tracheostomy collar and T-tube used to deliver oxygen to trach or endotracheal tube • Recommended flow rate is 10 l/min. with nebulizer set to inspired O 2 concentration

Other Devices • BIPAP Machine – bi-level positive airway • Used with patients who oriented (COPD, Asthma, PN) o. Delivers a set Inspiratory airway pressure (when pt inspires) o. Delivers a LOWER set end expiratory pressure as the patient exhales o. Both pressures increase tidal volume and may relieve dyspnea • CPAP Machine – continuous positive airway pressure o. Delivers set positive airway pressure for both inhalation and exhalation o. Used with obstructive sleep apnea to keep airway open longer

Complications of Oxygen • Atelectasis-alveoli may collapse due to high O 2 concentration due to nitrogen elimination from the lungs – diinished BS or crackles • With increase inspired O 2 nitrogen replaced and O 2 molecules rapidly absorbed into blood • Leaves alveoli relatively empty and predisposed to collapse

Ocular Damage-O 2 Administration • Common in neonates requiring high amounts of oxygen • Ocular damage-retinal injury can also occur in adults when exposed to 100% O 2 • Pa. O 2 of 150 mm/hg or more for 4 hours can result in retinal fibroplasia • Persons with previous retinal disease (detachment) are at high risk • Toxic effects: tearing, edema, visual impairment

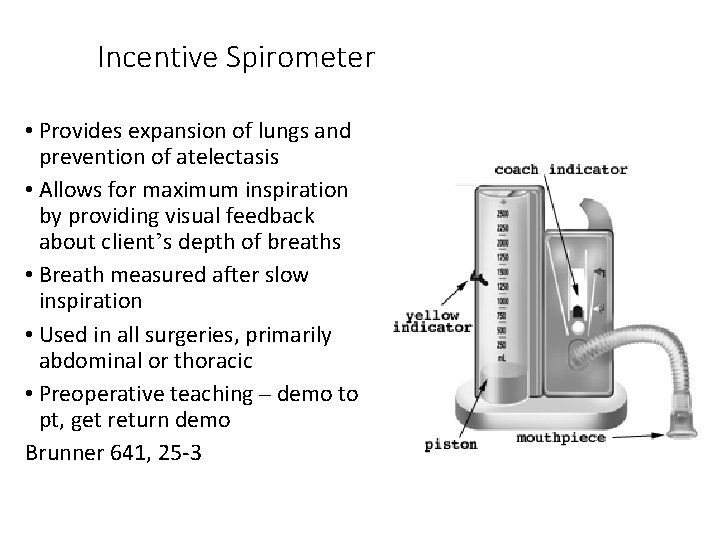
Incentive Spirometer • Provides expansion of lungs and prevention of atelectasis • Allows for maximum inspiration by providing visual feedback about client’s depth of breaths • Breath measured after slow inspiration • Used in all surgeries, primarily abdominal or thoracic • Preoperative teaching – demo to pt, get return demo Brunner 641, 25 -3

Chest Physiotherapy • Consists of physical chest wall maneuvers • Percussion (clapping or cupping) • Vibration • Postural drainage • Cough • Goals of therapy: clear airways of excessive secretions to reduce breathing effort • Facilitate the client’s ability to cough up or expectorate

PATIENT EDUCATION Breathing Exercises: p. 641, 25 -4 • General instructions • Diaphragmatic breathing • Pursed-lip breathing • Effective coughing technique p. 642, 25 -5

Question The nurse is caring for a client post hip repair. The client suddenly becomes SOB, very anxious with a bluish color to the face and chest. Vital signs are: RR 42, HR 110, Posat 87% and dropping. Which type of oxygen should the nurse consider administering? a. Nasal cannula b. Venturi mask c. Face tent d. 100% rebreather mask