Respiratory Support options BY NICOLE STEVENS CPAP is

Respiratory Support options BY: NICOLE STEVENS

CPAP is “Continuous Positive Airway Pressure”, it is a gas pressure higher than atmospheric pressure, continuously applied to the airway during spontaneous breathing. It is provided to help maintain functional residual capacity (FRC) and prevent airway collapse, thereby reducing work of breathing and improving gas exchange. Ø CPAP can be delivered by a neopuff (mask or cut down ETT), through a ventilator or via a bubbler system Ø

CPAP Equipment Ø Most centres use the Fisher and Paykel ventilator and CPAP circuits. The interfacing connected to this varies from centre to centre. Ø 2 most common are the Hudson prongs and the F&P midline mask or prongs.

CPAP equipment Ø With both the Hudson prongs and the F&P systems other equipment is also required. Ø Both systems have a particular hat that is placed on the baby and used to hold the tubing/prongs in the correct position. Ø When caring for a baby on CPAP it is important to have a neopuff at hand, suction equipment and appropriate monitoring in place.
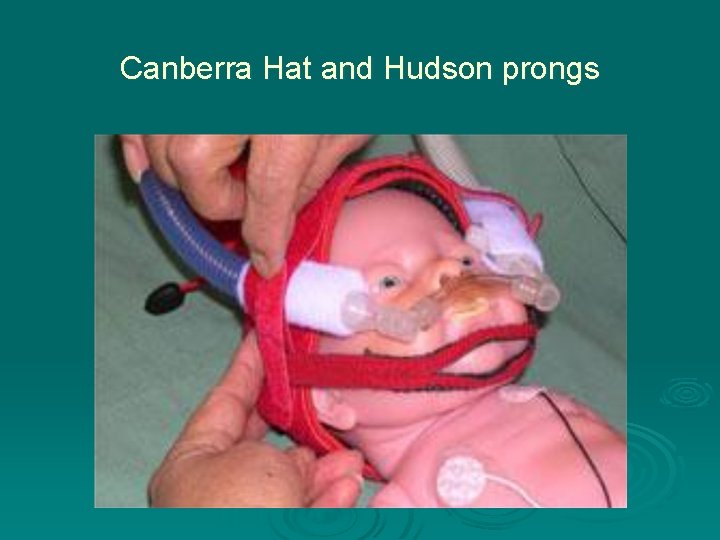
Canberra Hat and Hudson prongs

CPAP Settings Set gas flow for ventilator at 6 -8 litres/min Ø Set gas flow for bubble circuit at 5 -10 litres/min (aiming for a flow that achieves a moderate ‘boil’ in the water chamber) Ø PEEP is ordered by a medical officer and will usually be between 5 – 8 cm/H 2 O (occassionally PEEPs as high as 10 cm/H 2 O may be used in a tertiary hospital in extreme cases where reintubation is very undesirable). Ø

CPAP Setup Ø Measure head for hat size Ø Measure nares for prong/mask size if using F&P; examine nares and judge by weight if using Hudson prongs Ø Put equipment together, test circuit for leaks by turning on, occlude prongs (to close the circuit) and observe if the chamber bubbles, if not trouble shoot the circuit to look for breaks in the circuit

Process cont… Ø Ø Ø Position baby on the back Apply hat Insert prongs/position mask Secure tubing/prongs Using 2 people turn babies head to the side and hold in position ensuring prongs and tubing stay straight; other person rotates body and pulls arm through on underside. Baby will now be prone with one hand up to the mouth and the other lying down beside the body. Use gel pillows and neck rolls (cloth nappies) to assist with comfortable positioning.

Setup cont…. NGT or OGT required to be in place; for smaller/premature babies always use an OGT when babies are on CPAP; if it is a larger/term baby may be able to use a NGT (it is about the size of the nares and ability to comfortably fit prongs and gastric tube in the one nare). Ø Tube needs to be opened to air, to allow excess air to ‘vent’ out; in addition aspirate tube at least 6 hrly and discard excess air. Ø

CPAP CARES Ø Ø Ø Cluster cares (6 – 8 hrly); coordinate with any procedures that may need to happen (eg. CXR, blood tests, IV resites) Cares consists of a nappy change, temperature taking, removal of hat and prongs/mask to inspect for pressure areas, suction nares/mouth if required, reapply hat and prongs and reposition If baby very dependent on PEEP can use the neopuff and mask during cares; if baby on oxygen can use cot oxygen to deliver same Fi. O 2 via ambient cot O 2 while CPAP is off. Depends on the baby as to how much time you can take Preferable to use 2 people if you are not feeling 100% confident or if the baby is quite unstable

Cares cont… Ø Visually check position of prongs at least hourly, ensuring the nose is not distorted and no pressure is being applied to the nasal septum by the prongs; maintain a small gap between the prongs and the septum; if using a mask inspect for pressure areas across the nasal bridge Ø Use a skin/nasal integrity chart to record shift by shift observations

CPAP Observations Record hrly: PEEP, flow, Fi. O 2, humidifier temperature, Sa. O 2, HR, RR Ø Check temperature hrly for 4 hours when starting or stopping CPAP (because of additional heat created by hat and humidified tubing), otherwise check temp 4 – 6 hourly if stable Ø Measure blood pressure initially and then at least daily while on CPAP Ø Nasal integrity chart each shift Ø Record any apnoeic episodes, desaturations and/or bradycardias requiring intervention Ø

When to increase PEEP Increasing: if a baby is on a CPAP of 5, has significant work of breathing and has an increasing oxygen requirement (greater than 30%) increase the PEEP to 6. Same for steps up to PEEPs of 7 and 8. Ø Baby in a PEEP of 8 still with significant work of breathing and oxygen requirement may require intubation and surfactant administration Ø Always be aware of risk of air leak and consider CXR if baby clinically deteriorating. Ø

When to decrease PEEP Depends on the gestation of the baby as to how quick the weaning process happens Ø PEEP is decreased by 1 cm at a time Ø Decision to do this is based on oxygen requirement (<30%), WOB, and how the baby manages with cares Ø In a preterm baby it is usual to only decrease the PEEP once (maybe twice) in the day Ø Feeds (via gastric tube) can be slowly introduced while the baby is on CPAP, once WOB/tachypnoea has settled Ø

HI - FLOW Can be used in neonates and paediatrics Ø Trials have been done in recent times comparing Hi-Flow to CPAP in neonates (hiperspace trial RWH) Ø Both modes of respiratory support being used in NICU’s in Melbourne Ø New CPG just being ratified for its use in paediatrics at BHS (particularly aiming at the population that presents to ED during winter) Ø

Hi-Flow in Neonates Ø Used in the same circumstances as CPAP: Newborns with respiratory distress 2. Babies being extubated, but likely to still need some degree of pressure support +/ -supplemental oxygen Ø Flows used: 2 Litres to 6 Litres/min; increased or decreased by 1 L at a time as you would PEEP with CPAP 1.

Hi Flow in Paediatrics Equipment: Ø F&P prongs (multiple sizes available); stand; airvo system; 2 L bag of water for irrigation; oxygen tubing; 15 L flow meter To Commence: Ø Need paediatric registrar or consultant review; registrar must discuss with consultant Ø Consider CXR, blood gases, septic workup Ø Consider IV fluids (2/3 maintenance) Ø Discuss with PIPER decision to commence

Hi Flow in Paediatrics Nursing roles: Ø Set up airvo system Ø Select prong size Ø Record baseline observations (HR, RR, Sp. O 2, WOB, BP, Conscious level, Fi. O 2) Ø Suction nares before commencing and PRN

Hi Flow in Paediatrics Management: Ø Start at 1 L/kg/min (round down to whole number); commence Fi. O 2 at 30% Ø Titrate Fi. O 2 to achieve target Sp. O 2 92 – 97% Ø If > 50% required, notify paed, reduce O 2 to 30% and increase flow to 2 L/kg/min, titrate O 2 again to achieve target Sp. O 2 Ø If more than 2 L/kg/min required consider transfer to tertiary centre, and need for invasive ventilation

Hi Flow in Paediatrics When to consider escalating treatment: Ø No improvement after 90 mins on 2 L/kg/min Ø If >60% O 2 on 2 L/kg/min is needed to keep Sp. O 2 >92% Ø Recurrent apnoea, desaturation and/or bradycardic episodes Ø Worsening acidosis or hypercarbia on blood gases

Hi Flow in Paediatrics When to consider weaning: Ø When vital signs are stabilised, and after review by paediatric consultant or registrar Ø Reduce Fi. O 2 by 5% and reassess hourly Ø Continue this process aiming to maintain target Sp. O 2 Ø Once Fi. O 2 is back to 30%, flow can be weaned, decrease flow rate by 0. 25 L/kg/min and reassess after 2 hours Ø Continue process Ø Once at 2 Lpm, if remains stable, change to LFNP

Hi Flow in Paediatrics Documentation: Ø Continuous monitoring required Ø During initial hours of stabilising document 30 minutely obs, and with changes Ø Once stable document observations hourly (HR, RR, WOB, Sp. O 2, Fi. O 2, flow rate Ø Check temperature hourly until stable, then with cares (4 – 6 hrly) Ø BP as ordered Ø Record all observations on age appropriate chart

Ventilation in Neonates Ø Commence in birth room with neopuff device if required Ø If intubation is required in the birth room, the baby can be manually ventilated using the neopuff attached to the ETT until a ventilator is available Ø Intubation may be required because of no, or insufficient, respiratory effort at birth despite adequate initial resuscitation

Ventilation in Neonates cont… Profound hypoxia or hypercarbia is also an indication to intubate Ø Modes of ventilation to choose from will depend on the ventilator available Ventilation Modes: Ø CMV (continuous mandatory ventilation) Ø SIPPV (sychronised intermittent positive pressure ventilation) Ø SIMV (sychronised intermittent mandatory ventilation) Ø PSV (pressure support ventilation) Ø High Frequency (Oscillation or Jet) Ø

Ventilation ETT size selection (2. 5 – 4. 0 mm), rough guide, divide gestational age by 10 Ø Orally tape at weight + 6 cm (eg. 3. 5 kg baby, tape at 9. 5 cm) Ø Nasal tape at weight x 1. 5 + 6 cm Ø Once secured confirm position with Xray, adjust in or out if required, and re-secure Ø Leukoplast 2. 5 cm tape for securing (cut to size), multiple options for style of taping; trouser leg style easiest, and can be used orally or nasally, for intubation, or cut down ETT for CPAP Ø Hydrocolloid to protect skin on both sides of face Ø

Observations Ø As per CPAP and Hi Flow Ø In addition: PEEP, PIP, Mean, Flow, IT, rate (set and actual), Volume Guarantee, if using, (set and actual). Ø Urine output (weigh nappies) Ø Each shift: ETT size, position, tape integrity Ø PRN suction, measure length to end of tube on suction catheter, disconnect venitlator, suction, and reconnect

Volume Guarantee Based on weight of baby, calculated as m. Ls/kg Ø Usually start at 4 m. Ls/kg Ø This is the tidal volume you are wanting the baby to have going through their lungs with each breath. PIP will be set at a maximum. The ventilator will allow the baby to use their own respiratory effort and will add in extra PIP if required to achieve the target VG. Ø Generally range between 2 -5 m. Ls/kg, changed in response to blood gases; to clear excess CO 2 increase VG, if over ventilated decrease VG. Ø Increments usually in 0. 5 m. Ls/kg at a time Ø

Ways to deliver Oxygen Facial Ø LFNP or HFNP Ø Cot oxygen Ø Head box Ø Neopuff Ø Bubble or ventilator CPAP Ø Intubated and ventilated General rule: if there is an increasing oxygen requirement of 30% or above, whatever support is in place is likely not adequate, so increase support Ø

QUESTIONS? ? ?
- Slides: 29