RESPIRATORY STRESSORS Pritam Pandit RN BSN CCRN ASTHMA
RESPIRATORY STRESSORS Pritam Pandit, RN, BSN, CCRN
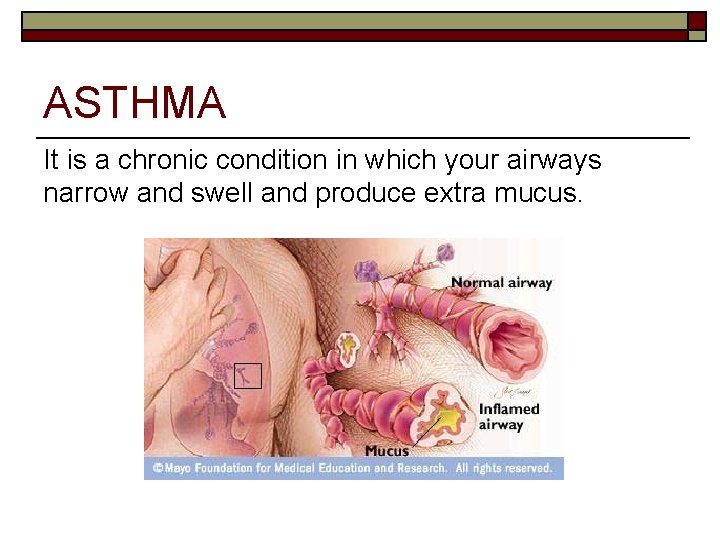
ASTHMA It is a chronic condition in which your airways narrow and swell and produce extra mucus.
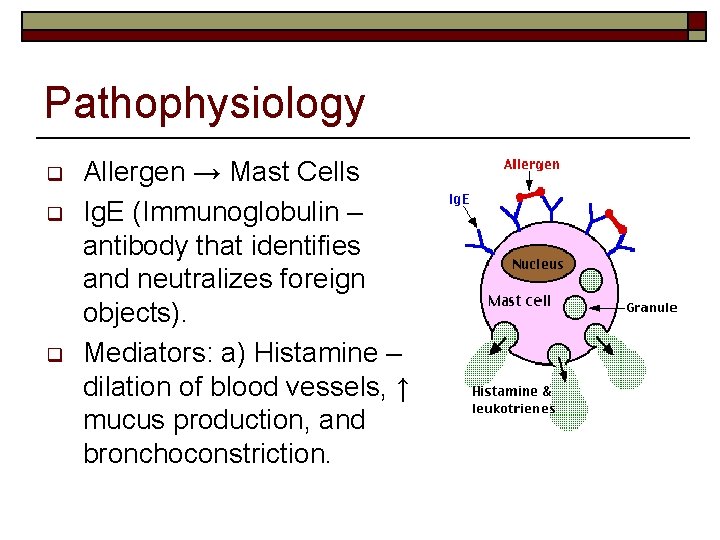
Pathophysiology q q q Allergen → Mast Cells Ig. E (Immunoglobulin – antibody that identifies and neutralizes foreign objects). Mediators: a) Histamine – dilation of blood vessels, ↑ mucus production, and bronchoconstriction.
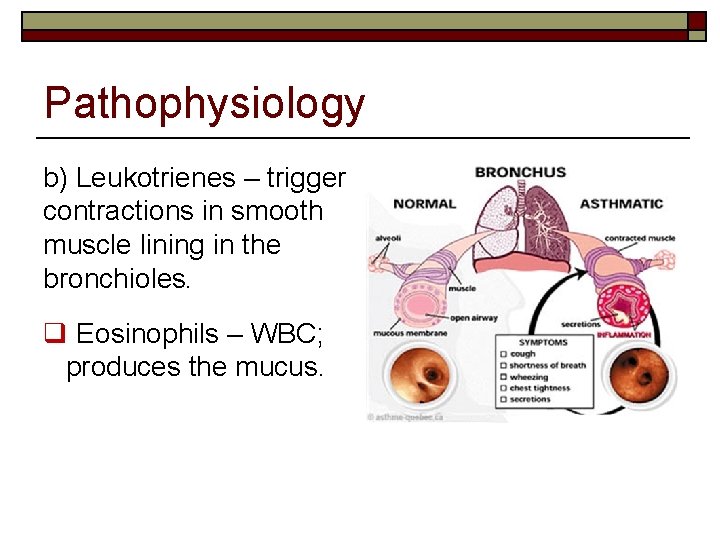
Pathophysiology b) Leukotrienes – trigger contractions in smooth muscle lining in the bronchioles. q Eosinophils – WBC; produces the mucus.
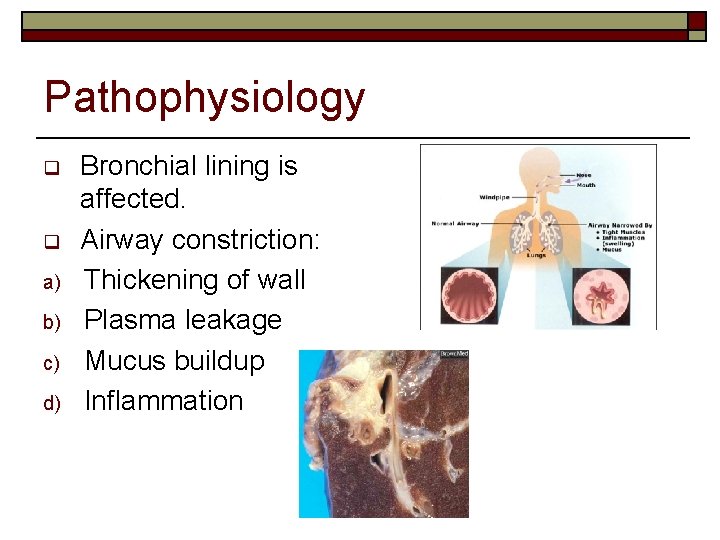
Pathophysiology q q a) b) c) d) Bronchial lining is affected. Airway constriction: Thickening of wall Plasma leakage Mucus buildup Inflammation

Signs/Symptoms o o o o Wheezing Cough Tightness in chest SOB Intensifies at night Sweating Orthopnea
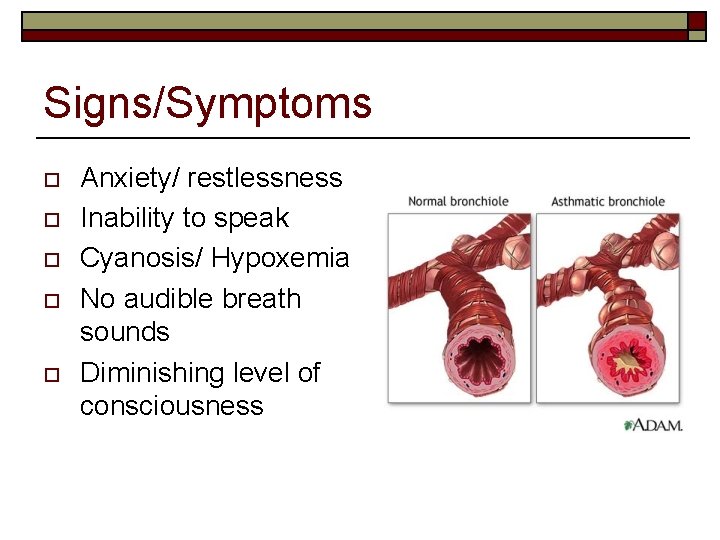
Signs/Symptoms o o o Anxiety/ restlessness Inability to speak Cyanosis/ Hypoxemia No audible breath sounds Diminishing level of consciousness

Breath sounds o o Dependent on degree of bronchospasm Audible Diminished Absent
Vital Signs o o o Tachypnea Tachycardia Hypoxia

Asthma Attack Triggers o o o Specific allergens Pollen Mold Dust Animal dander

Asthma Attack Triggers o o o o Chemicals Forestry – Foliage Fishing Cigarette smoke Medications – beta blockers Pregnancy Exposure to cold

Asthma Attack Triggers o o Smoke Food Sudden changes in the weather Environment

Classes of Asthma 1. Mild Intermittent q Symptoms < 2/week q Brief exacerbations q Night symptoms < 2/mo q Asymptomatic with normal function between exacerbations

Classes of Asthma 2. Mild Persistent o Symptoms > 2/week, < 1/day o Exacerbation affects ADLs o Night symptoms > 2/mo

Classes of Asthma 3. Moderate Persistent o Daily symptoms o Exacerbations >2 or more/week o Exacerbations affects ADLs o Night symptoms > 1/week o Daily use of short term beta-agonists
Classes of Asthma 4. Severe Persistent o Continuous symptoms o Frequent exacerbations o Frequent night symptoms o Activity limited
Status Asthmaticus o Severe episode of bronchospasm that does not respond to standard treatment
Adult Onset – Risk Factors o o Obesity Allergies Exposure to latex Occupational hazards

Exercise Induced Asthma o o o Strenuous activity Decreased heat and moisture in lungs Inhaling large amounts cold, dry air

Strenuous activities o o o Playing in the cold Hyperventilating Laughing Crying Exercise requiring breathing through the mouth

Signs/Symptoms o o o Usually occurs 5 -20 min into activity Tightness in chest Coughing Wheezing SOB or rapid shallow breaths

Prevention o o Warm up exercise Meds prior to activity Cooling down post exertion Limit participation during high trigger days

Occupational Asthma o o o o Triggers in the job Chemicals Vapors Allergens in the environment People Higher during “flu” season Bacteria & viruses

Nocturnal Asthma o o Defined - as asthma from 12 midnight till 8 am Wheezing SOB when lying down Usually awaken 2 am-4 am

Miscellaneous Asthma o o o Cough variant (chronic cough) Seasonal Aspirin induced (overproduction of leukotrienes)

Diagnostics o o o PFT – pulmonary function test CXR – chest x-ray Peak flow measurement n Measures highest airflow during forced expiration
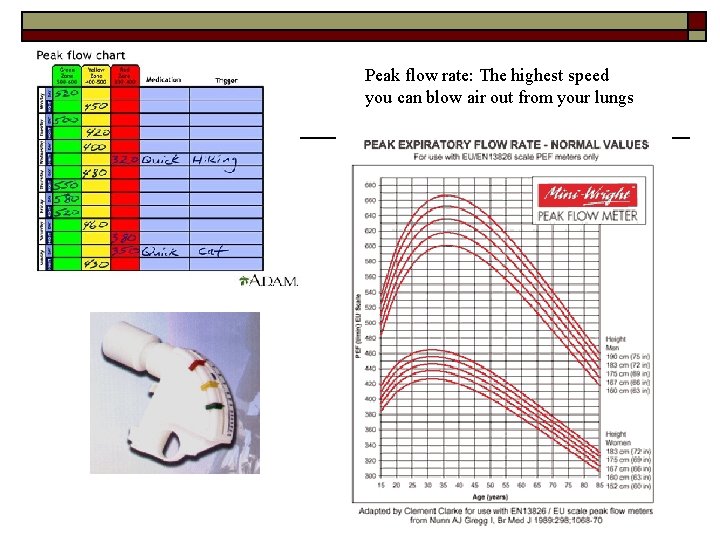
Peak flow rate: The highest speed you can blow air out from your lungs
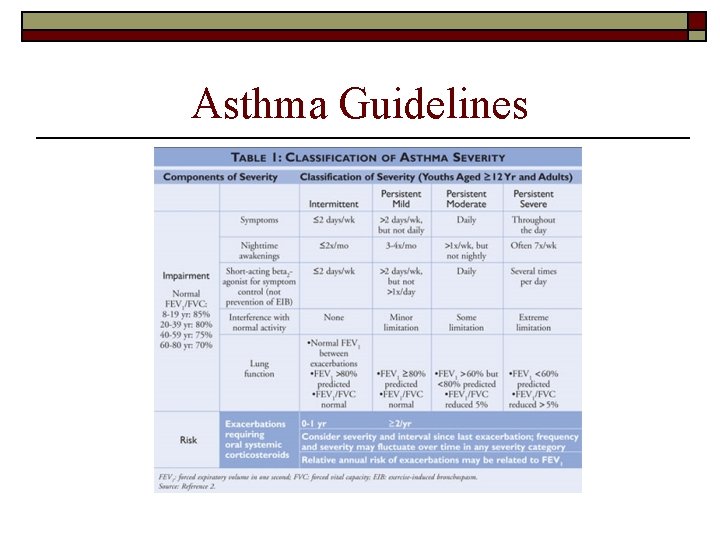
Asthma Guidelines

Asthma Guidelines

Treatment – Quick-Relief o Short-acting beta 2 adrenergics n n n o Proventil Xopenex Maxair Anticholinergics n Atrovent
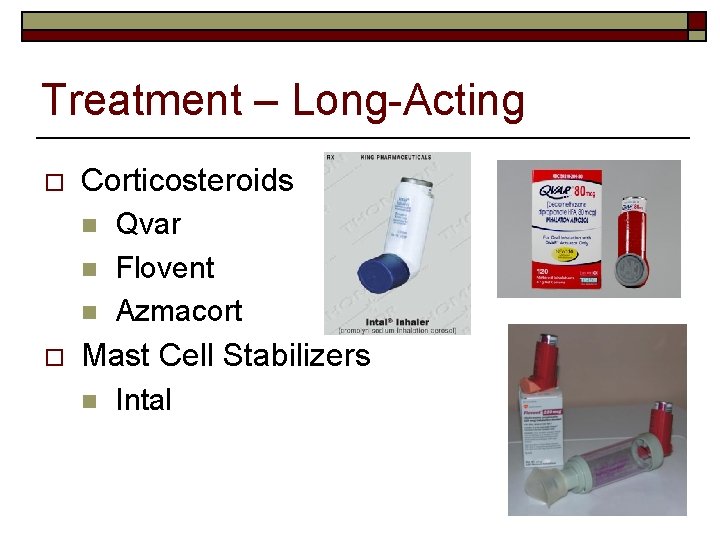
Treatment – Long-Acting o Corticosteroids n n n o Qvar Flovent Azmacort Mast Cell Stabilizers n Intal

Treatment – Long-Acting o Long-acting beta 2 -adrenergics n n o Serevent Foradil Xanthine derivatives n n Slo-bid Theodur

Treatment – Long-Acting o Leukotriene modifiers (inhibitors) n n o Accolate Singulair Combination products n n n Symbicort Advair Diskus Dulera

Nursing o o o Depends on severity of symptoms – use of quick relief meds Educate on use of inhalers (spacers, etc. ) Breath sounds Pulse oximetry Vital signs Peak flow

Nursing o o o May need hospitalizations for severe exacerbations Educate on self-care and follow-up Importance of adhering to regime and preventative measures
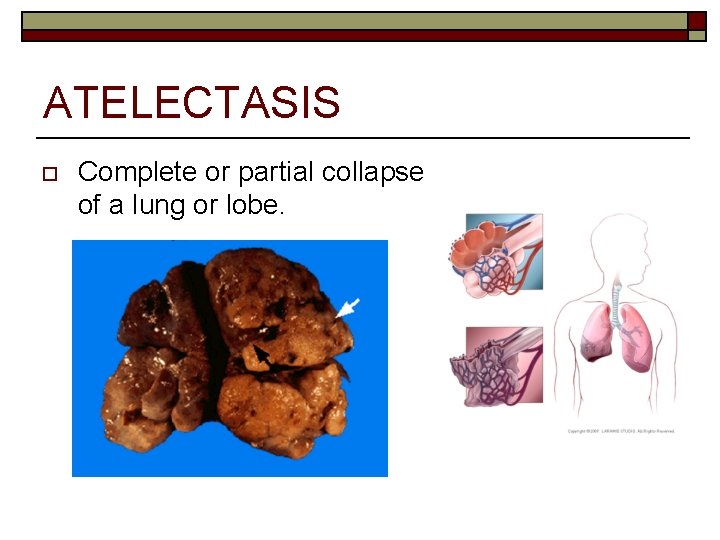
ATELECTASIS o Complete or partial collapse of a lung or lobe.
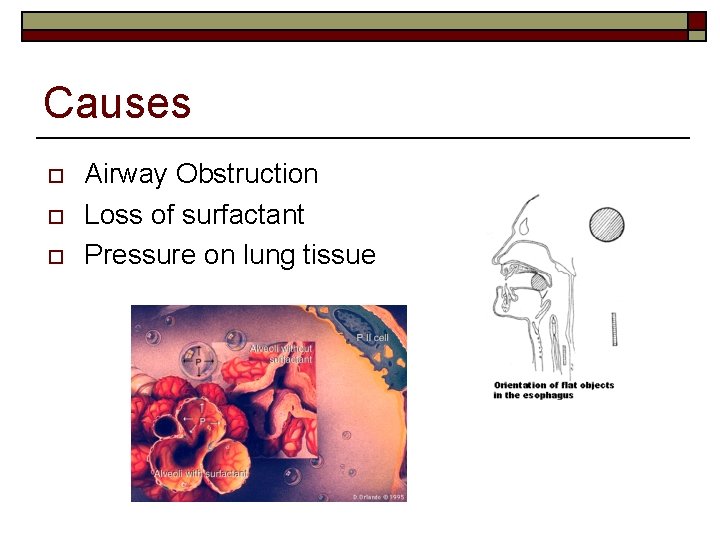
Causes o o o Airway Obstruction Loss of surfactant Pressure on lung tissue

Signs/Symptoms o o SOB/dyspnea/ tachypnea Tachycardia Anxiety Fever - not r/t infection but reaction to injury
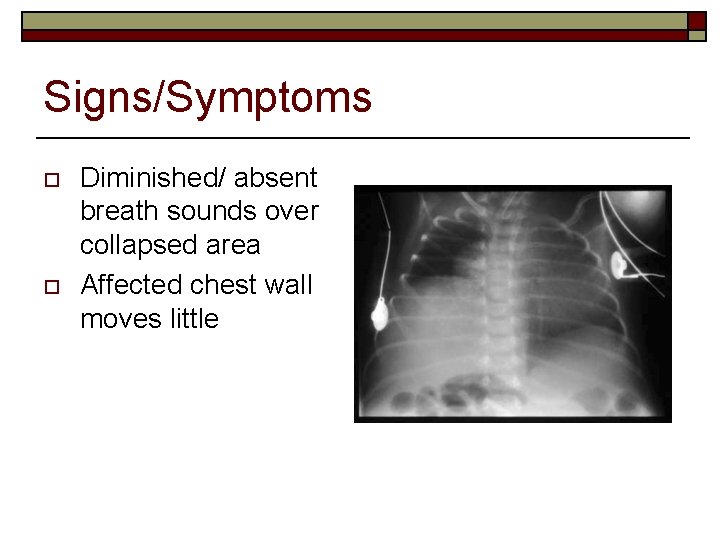
Signs/Symptoms o o Diminished/ absent breath sounds over collapsed area Affected chest wall moves little
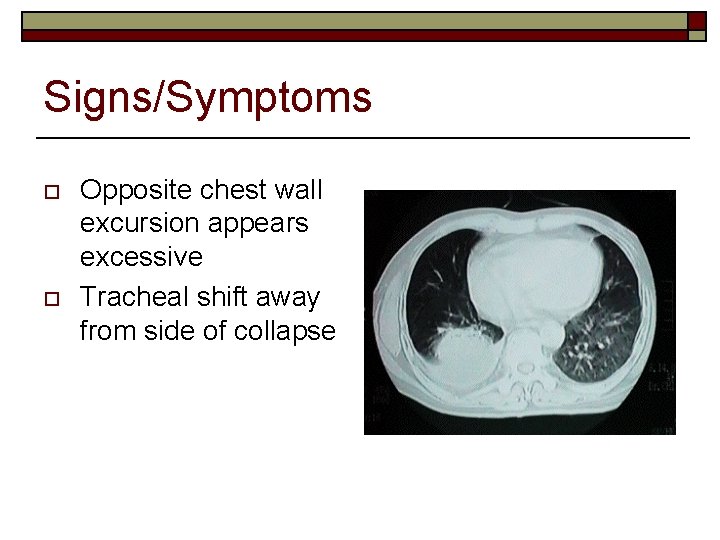
Signs/Symptoms o o Opposite chest wall excursion appears excessive Tracheal shift away from side of collapse
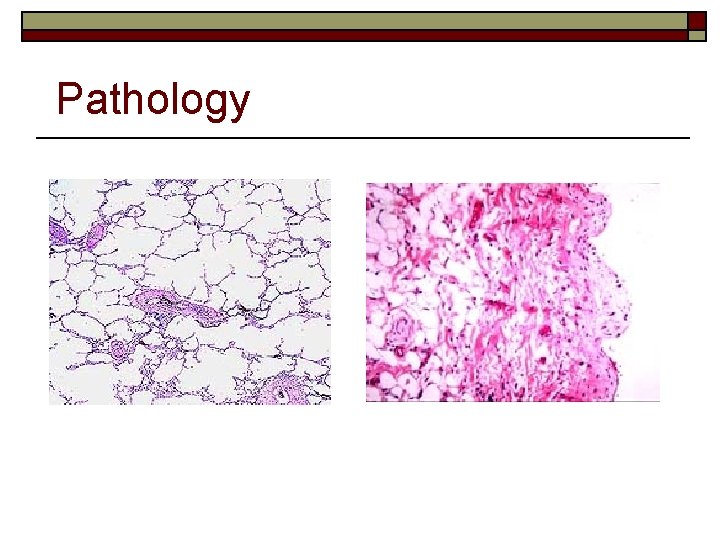
Pathology

Diagnostics o o o ABG’s/ O 2 therapy prn Pulse oximetry Elevate HOB
Interventions o o Turn q 2 h or ambulate TCDB and use IS Treat cause Primary/Tertiary prevention
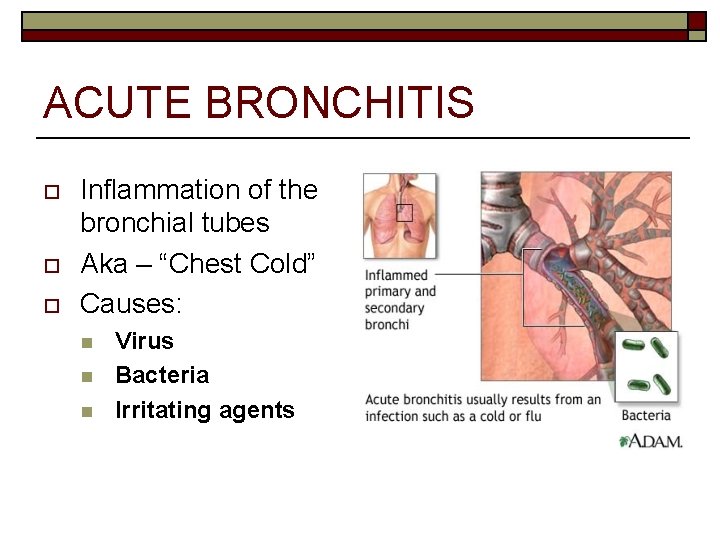
ACUTE BRONCHITIS o o o Inflammation of the bronchial tubes Aka – “Chest Cold” Causes: n n n Virus Bacteria Irritating agents
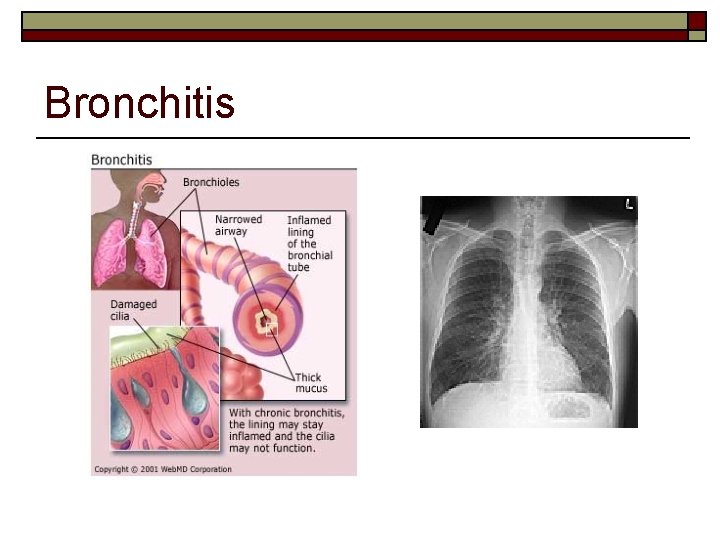
Bronchitis
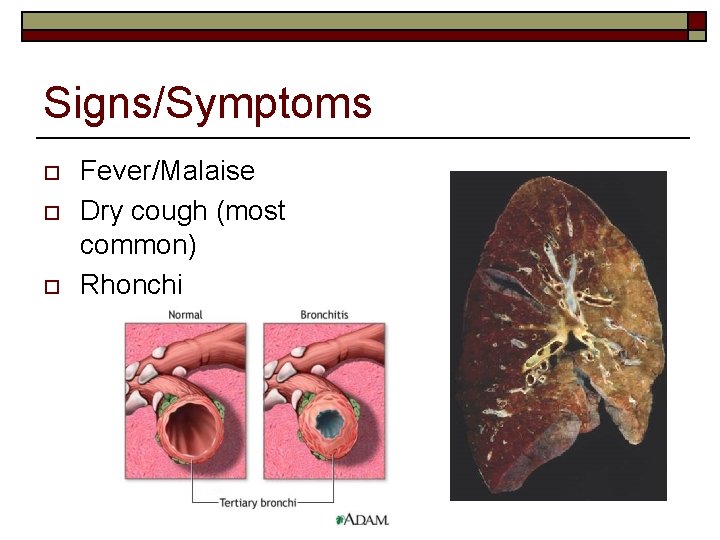
Signs/Symptoms o o o Fever/Malaise Dry cough (most common) Rhonchi
Interventions o o o Maintain hydration Prevent pooling of secretions (TCDB) Rest ASA/Tylenol to ↓ fever/malaise Expectorants vs cough suppressants
Interventions o o o Inhaled bronchodilators In hospital: sputum C&S Treat with antibiotic CXR to r/o pneumonia Decongestant/ Antihistamine

PNEUMONIA o o Infection that inflames the air sacs in one or both lungs. Fluid fills. Causes: n Bacteria, Viruses, Fungi n Food/Fluid aspiration, or Emesis n Toxic/caustic chemical inhalation

Signs/Symptoms o o Fever/ Chills/ Sweats/ Headache Pleuritic chest pain Cough/Sputum production Rales/ Crackles

Signs/Symptoms o o Dsypnea/ Tachypnea Increase tactile fremitus Dull percussion Unequal Chest Expansion
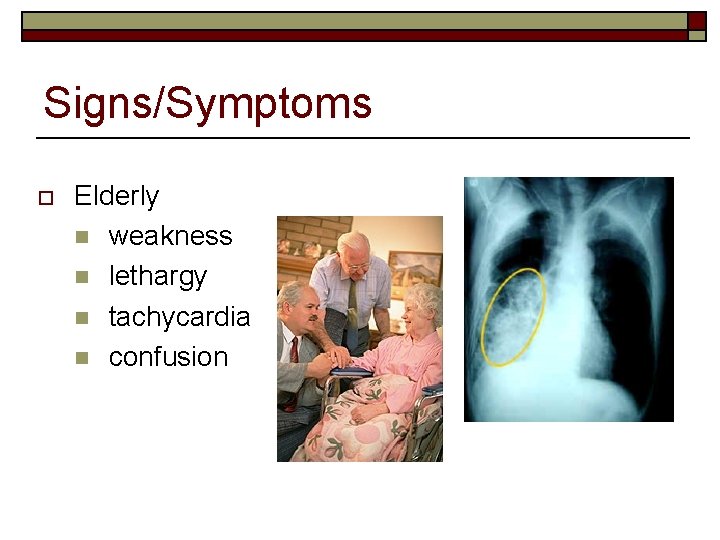
Signs/Symptoms o Elderly n weakness n lethargy n tachycardia n confusion
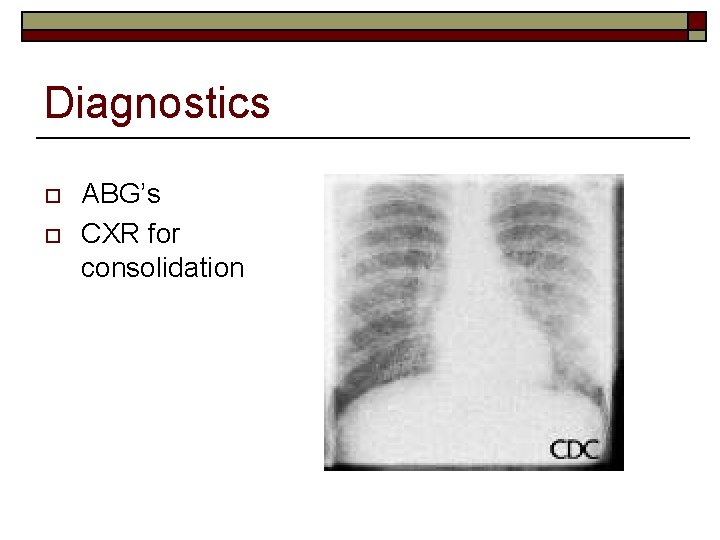
Diagnostics o o ABG’s CXR for consolidation
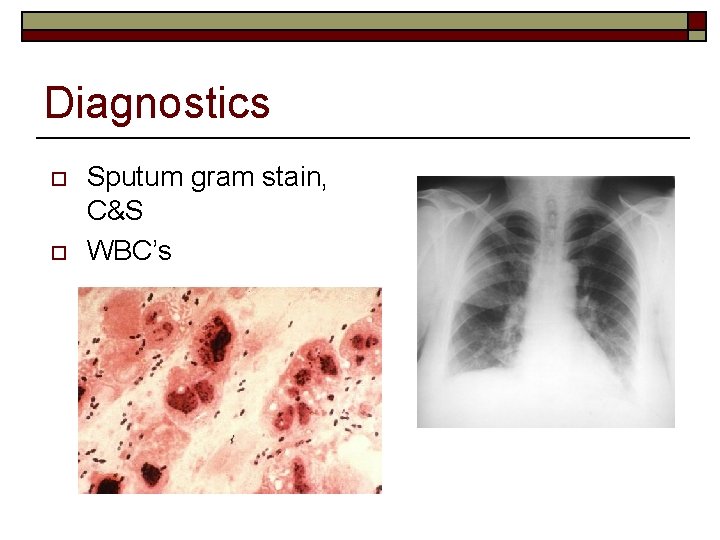
Diagnostics o o Sputum gram stain, C&S WBC’s

Interventions o o Raise HOB Maintain hydration Prevent pooling Chest PT/Postural draining
Interventions o o Adequate rest Good Nutrition Mild analgesics (nonopiod) Inhaled bronchodilators

TUBERCULOSIS o o o Potentially serious infection of the lungs. Caused by acid-fast bacillus Mycobacterium tuberculosis Must be reported to Health Department Agencies

Communicability o o Transmitted by aerosolization only Infectious, but brief exposure doesn’t cause infection Risk of transmitting TB reduced within 2 -3 weeks after chemo Inflammatory disease may occur in any part of the body

Pathophysiology o o o Inhaled organism gets past defense mechanism and implants in lung tissue. Immune system triggers formation of “tubercles” around phagocytized bacilli and forms a protective wall. Forms into “hard” or “soft” tubercles.

Pathophysiology o Hard tubercles (primary infection) n Tubercles calcify and keep bacilli in check. n Client is infected, but does not have active disease n Will have positive TB skin test, but can’t give to anyone
Pathophysiology o Soft tubercules n Bacilli multiply n Caseation: necrosis into cheese-like mass n Inflammation subsides, lesions heal to calcified areas OR erode to bronchus n Liquefied caseous material coughed up (full-blown disease)

Factors That Lower Resistance o o o Advanced age/very young Immunodeficiency Hormonal changes Malnutrition Alcoholism

Factors That Lower Resistance o o o Presence of other disease states Poverty (malnutrition and overcrowding) Certain ethnic groups – ex: Native Americans, Eskimos, immigrants from Southeast Asia, Mexico, Ethiopia, Latin America

Assessment o History n Recent/Past exposure to TB n Occupation n Previous TB skin test n Received BCG vaccine

Assessment: Systemic o o o Fatigue Anorexia Weight loss Persistent low-grade fever (afternoon temp up) Chills and sweats (often at NIGHT)
Assessment: Respiratory o o o Dyspnea (usually in advanced cases) Persistent cough, initially dry then productive Hemoptysis Chest pain: dull, aching, chest tightness Non-resolving bronchopneumonia
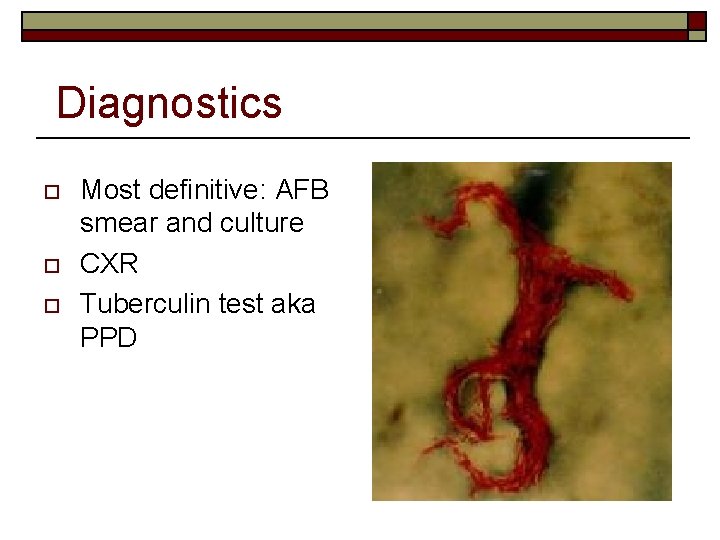
Diagnostics o o o Most definitive: AFB smear and culture CXR Tuberculin test aka PPD
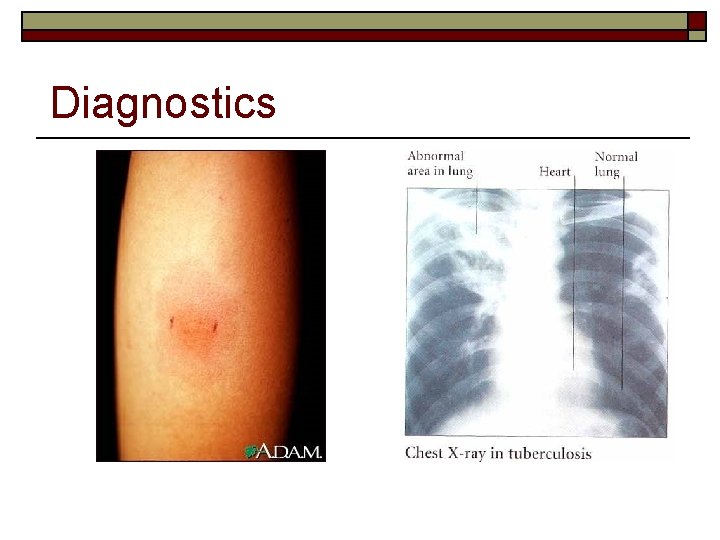
Diagnostics
Interventions o o Chemotherapy First line drugs RIPES
Side Effects o o o Baseline studies prior to start of RIPE Liver - INH, pyrazinamide Kidney – Streptomycin

Side Effects o o Hearing – Streptomycin Visual acuity (can’t differentiate between red/green) Ethambutol

Side Effects o o o Nausea - may need antinausea drugs Anorexia – qhs Peripheral neuropathies (INH) n r/t vit. B 6 deficiency n may need concurrent use of PYRIDOXINE (vit. B 6)

Interventions o o Check hospital protocols: treatment usually continues for 6 -9 months Social Service Referral or Public Health Department follow-up at home for regiment compliance

Interventions o o o Hospitalization = 1 -2 weeks Respiratory isolation Fitted masks Negative pressure room ventilation UV - germicidal effect

Interventions o Pt. no longer considered a Health Hazard: n n after 2 -3 weeks of chemo improvement in s/s 3 consecutive negative smears collected on different days maintenance of medication compliance at home

Patient/Family Education o o Education assists with compliance Cover mouth No need to wash clothes/ dishes separately Handle used tissues carefully

Prevention o o TB screening of at-risk populations Early ID and treatment of active cases Report to Public Health Department Increase public awareness
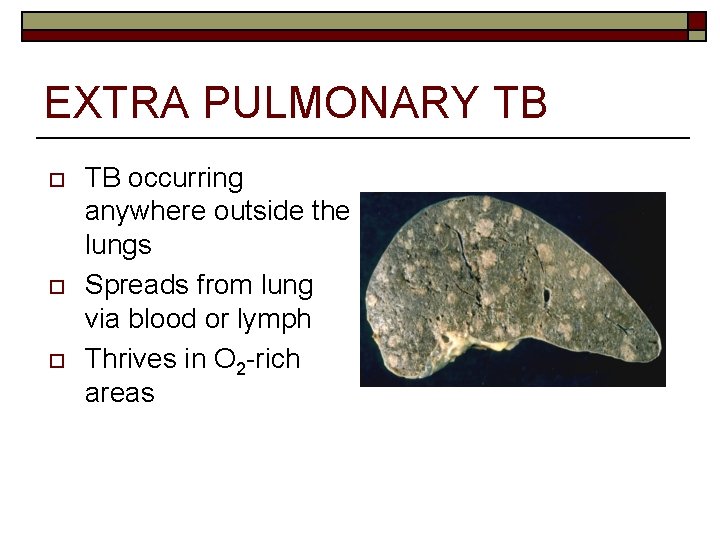
EXTRA PULMONARY TB o o o TB occurring anywhere outside the lungs Spreads from lung via blood or lymph Thrives in O 2 -rich areas

Common Sites o o o Renal cortex Bone growth plates Meninges Disseminated TB Larynx/Mouth

Questions 1. Which of the following pathophysiological mechanisms that occurs in the lung parenchyma allows pneumonia to develop? a) Atelectasis b) Bronchiectasis c) Effusion d) Inflammation

Questions 2. A 24 -year-old client comes into the clinic complaining of right-sided chest pain and shortness of breath. He reports that it started suddenly. The assessment should include which of the following interventions? a) Auscultation of breath sounds b) Chest x-ray c) Echocardiogram d) Electrocardiogram (ECG)

Questions 3. A client with pneumonia has a temperature ranging between 101* and 102*F and periods of diaphoresis. Based on this information, which of the following nursing interventions would be a priority? a) Maintain complete bedrest b) Administer oxygen therapy c) Provide frequent linen changes d) Provide fluid intake of 3 L/day

Questions 4. A client with acute asthma is prescribed shortterm corticosteroid therapy. What is the rationale for the use of steroids in clients with asthma? a) Corticosteroids promote bronchodilation b) Corticosteroids act as an expectorant c) Corticosteroids have an anti-inflammatory effect d) Corticosteroids prevent development of respiratory infections

Questions 5. Basilar crackles are present in a client’s lungs on auscultation. The nurse knows that these are discrete, non continuous sounds that are: a) Caused by the sudden opening of alveoli b) Usually more prominent during expiration c) Produced by airflow across passages narrowed by secretions d) Found primarily in the pleura

- Slides: 85