Respiratory Physiology Revision Breathing why bother Supply of

Respiratory Physiology Revision

Breathing – why bother? • Supply of energy is fundamental to all living processes • Aerobic respiration produces more ATP per molecule of glucose than anaerobic • Need substrate for aerobic respiration (O 2) • Need to remove by-product of aerobic respiration (CO 2)

Summary of steps involved in respiration The steps involved in respiration are • ventilation, • gas exchange between alveolar air and lung capillaries, • bulk transport via the circulation, • gas exchange between capillaries and tissue cells, and • cellular utilization of O 2 and production of CO 2. In the steady state, the net volumes of oxygen and carbon dioxide exchanged in the lungs per unit time are equal to the net volumes exchanged in the tissues. Typical volumes per minute are 250 ml for oxygen consumption and 200 ml for carbon dioxide production.
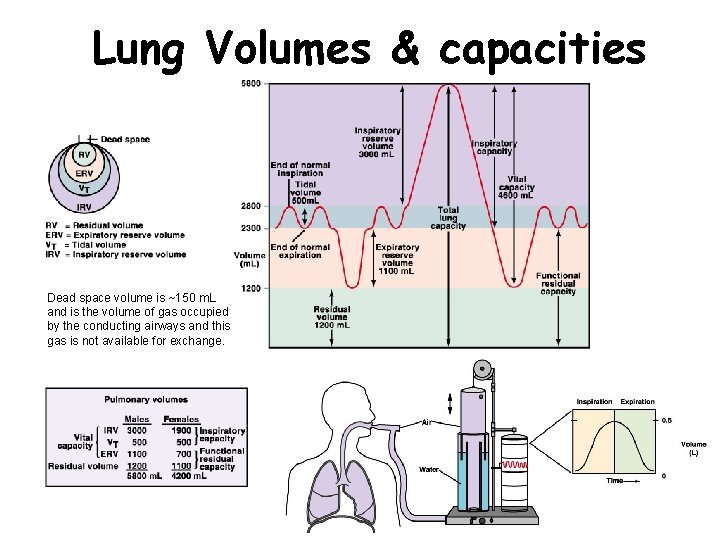
Lung Volumes & capacities Dead space volume is ~150 m. L and is the volume of gas occupied by the conducting airways and this gas is not available for exchange.

Mechanics of Breathing • Occurs because thoracic cavity changes volume • Inspiration uses external intercostals and diaphragm • Expiration is passive at rest, but uses internal intercostals and abdominals during severe respiratory load • Breathing rate is 10 -20 breaths / minute at rest, 40 - 45 at maximum exercise in adults

Gas laws summary • • Charles Law states that the volume occupied by a gas is directly related to the absolute temperature (v a T) Henry’s Law states that the amount of gas dissolved in a liquid is determined by the pressure of the gas and it’s solubility in the liquid. Dalton’s Law states that the total pressure of a gas mixture is the sum of the pressures of the individual gases. Boyle’s Law states that the pressure exerted by a gas is inversely proportional to to its volume (P a 1/V) Note that gases (singly or in mixtures) move from areas of high pressure to areas of low pressure.
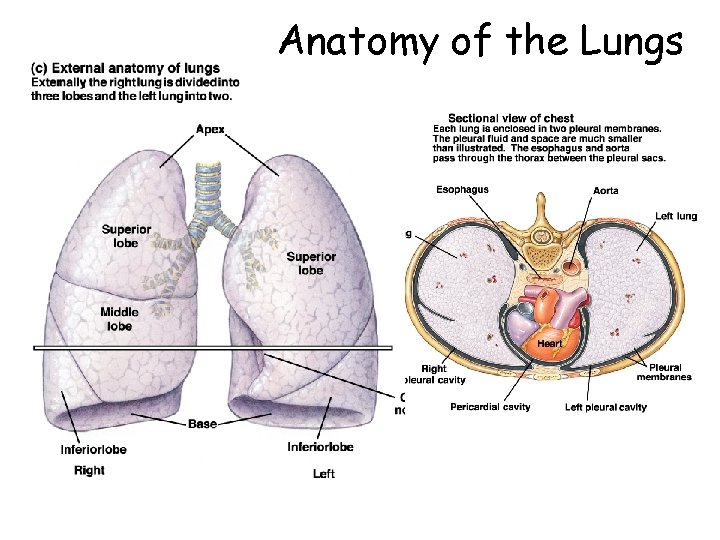
Anatomy of the Lungs
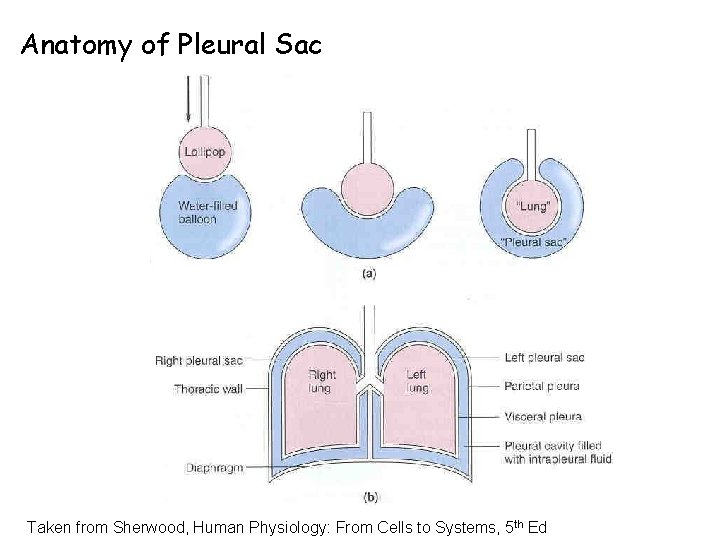
Anatomy of Pleural Sac Taken from Sherwood, Human Physiology: From Cells to Systems, 5 th Ed
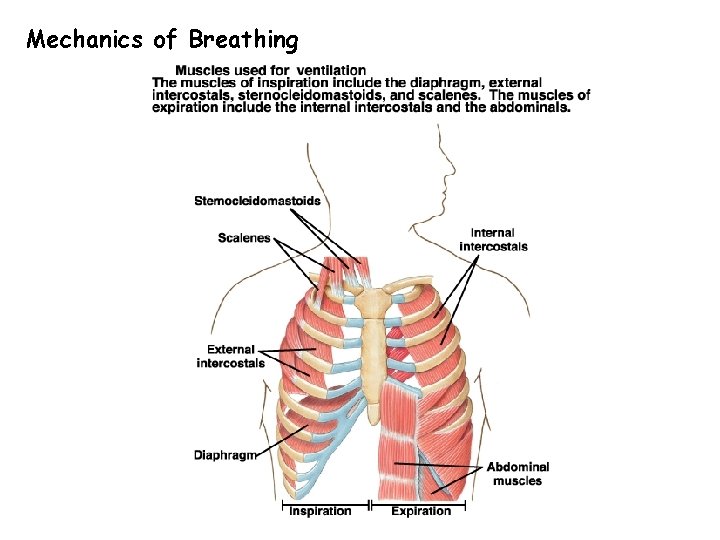
Mechanics of Breathing
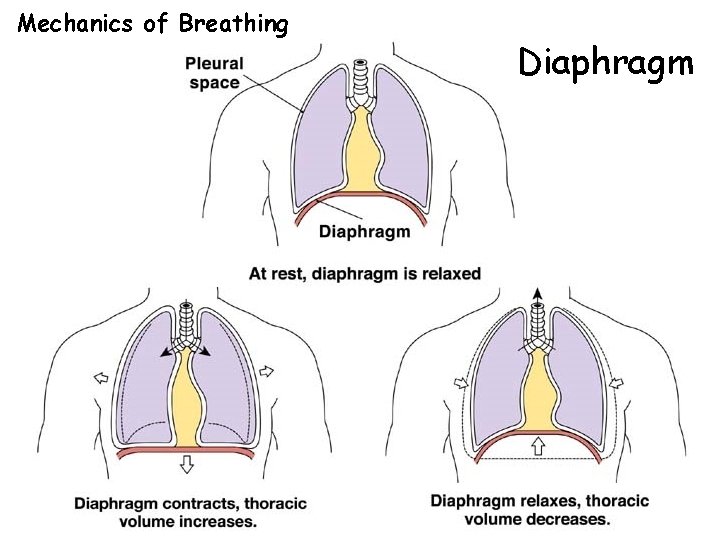
Mechanics of Breathing Diaphragm
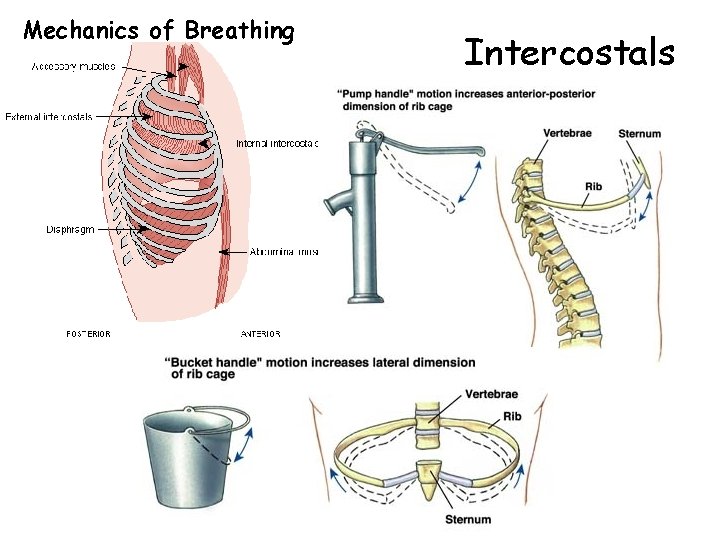
Mechanics of Breathing Intercostals
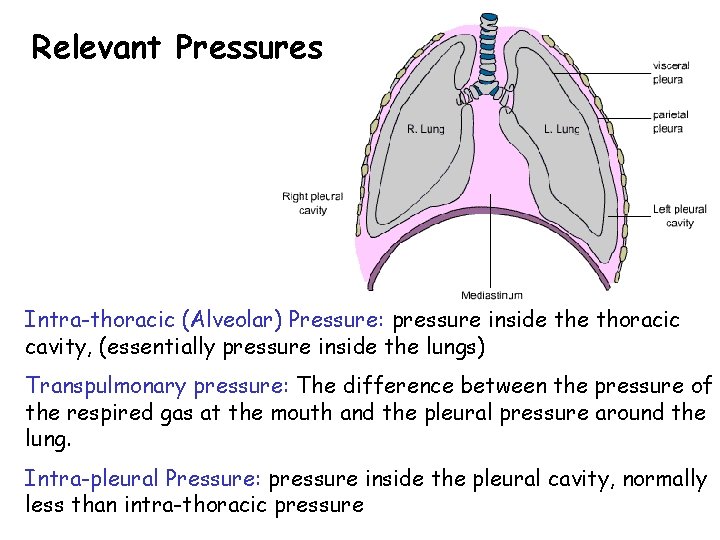
Relevant Pressures Intra-thoracic (Alveolar) Pressure: pressure inside thoracic cavity, (essentially pressure inside the lungs) Transpulmonary pressure: The difference between the pressure of the respired gas at the mouth and the pleural pressure around the lung. Intra-pleural Pressure: pressure inside the pleural cavity, normally less than intra-thoracic pressure
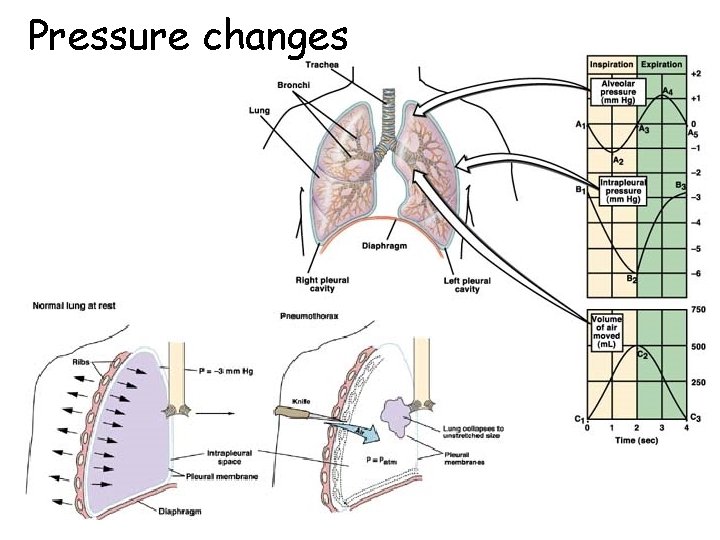
Pressure changes

Surfactant • Detergent like fluid produced by Type II Alveolar cells • Reduces surface tension on alveolar surface membrane thus reducing tendency for alveoli to collapse • Increases lung compliance (distensibilty) • Reduces lung’s tendency to recoil • Makes work of breathing easier • Is more effective in small alveoli than large
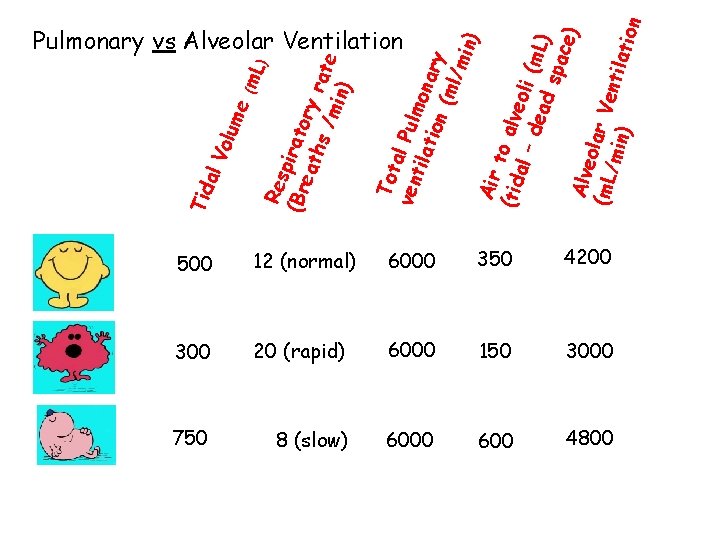
L) (m 500 12 (normal) 6000 350 4200 300 20 (rapid) 6000 150 3000 750 8 (slow) 6000 600 4800 Tot ven al Pulm tila tion onary (ml /mi n) Air (tid to alve al – o dea li (m. L) d s pac e) Alve o (m. L lar Ve /min ntila ) tion me olu Res (Br pirato eat r hs y rat e /mi n) al V Tid Pulmonary vs Alveolar Ventilation
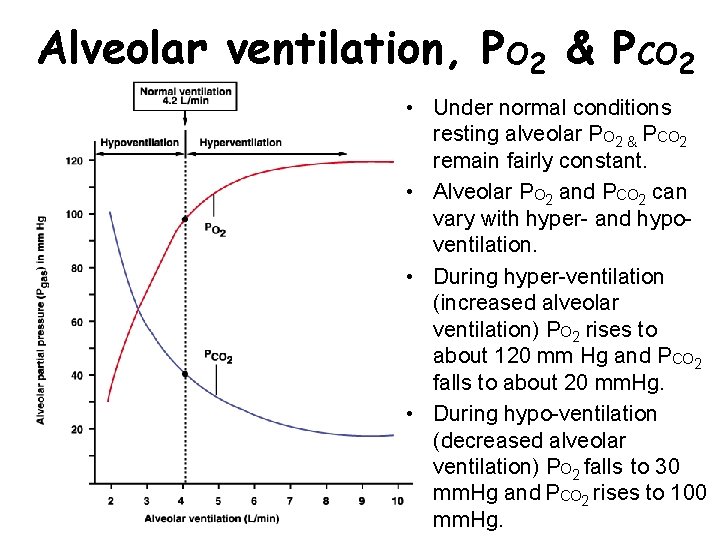
Alveolar ventilation, PO 2 & PCO 2 • Under normal conditions resting alveolar PO 2 & PCO 2 remain fairly constant. • Alveolar PO 2 and PCO 2 can vary with hyper- and hypoventilation. • During hyper-ventilation (increased alveolar ventilation) PO 2 rises to about 120 mm Hg and PCO 2 falls to about 20 mm. Hg. • During hypo-ventilation (decreased alveolar ventilation) PO 2 falls to 30 mm. Hg and PCO 2 rises to 100 mm. Hg.

Compliance Definition: change in volume relative to change in pressure i. e. how much does volume change for any given change in pressure It represents the stretchability of the lungs HIGH COMPLIANCE = large increase in lung volume for small decrease in ip pressure LOW COMPLIANCE = small increase in lung volume for large decrease in ip pressure Changes in disease states/age
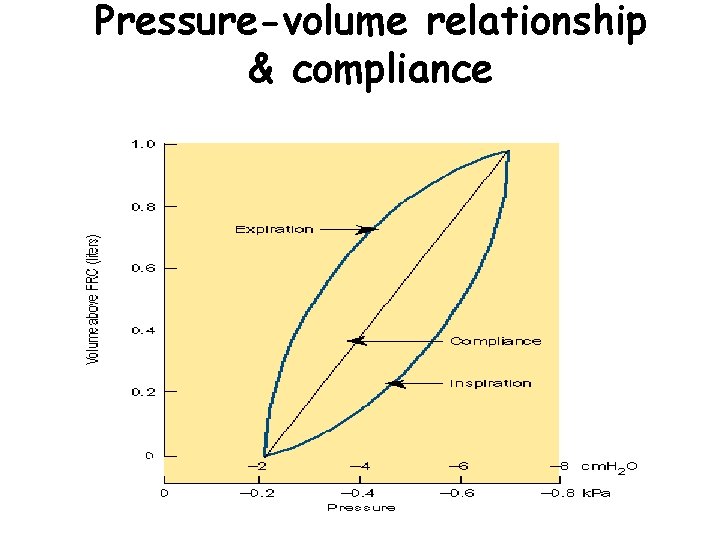
Pressure-volume relationship & compliance
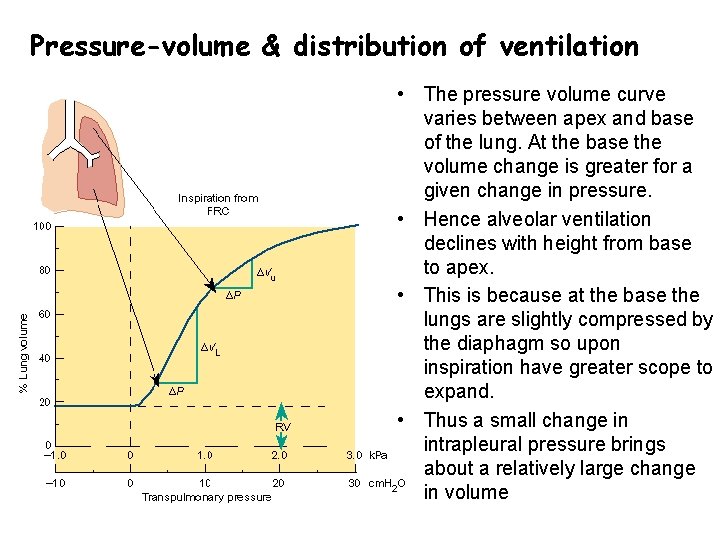
Pressure-volume & distribution of ventilation • The pressure volume curve varies between apex and base of the lung. At the base the volume change is greater for a given change in pressure. • Hence alveolar ventilation declines with height from base to apex. • This is because at the base the lungs are slightly compressed by the diaphagm so upon inspiration have greater scope to expand. • Thus a small change in intrapleural pressure brings about a relatively large change in volume
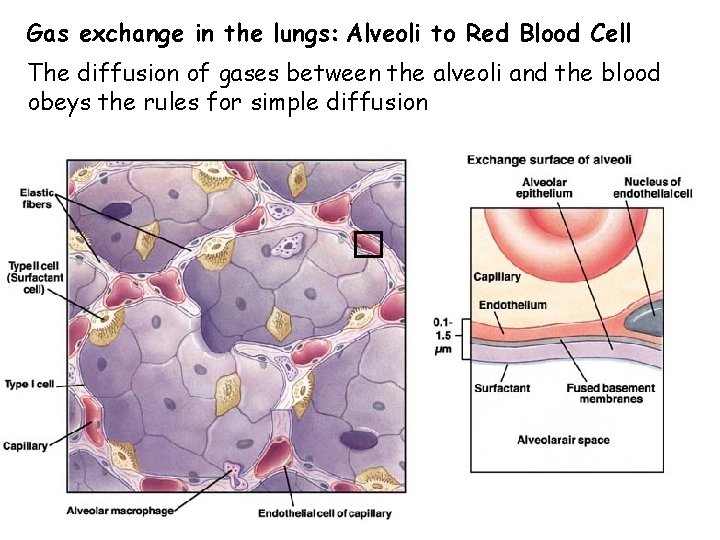
Gas exchange in the lungs: Alveoli to Red Blood Cell The diffusion of gases between the alveoli and the blood obeys the rules for simple diffusion
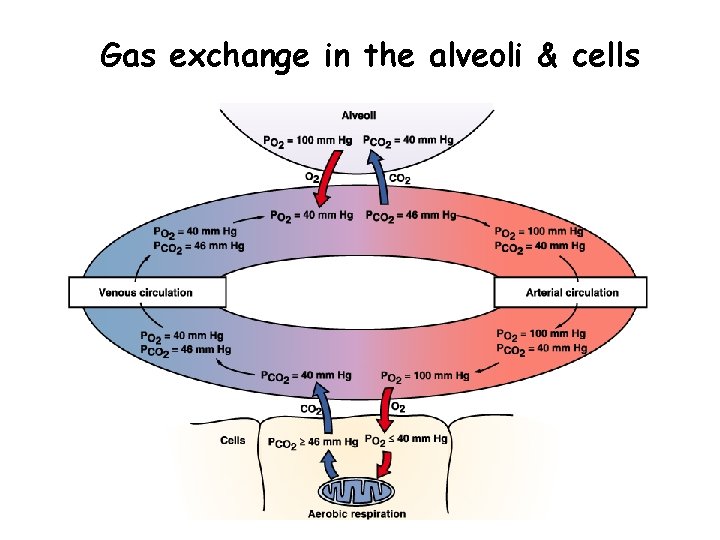
Gas exchange in the alveoli & cells
Ventilation-Perfusion Relationship Ventilation (air getting to alveoli) Ideally match (compliment) each other Perfusion (local blood flow)
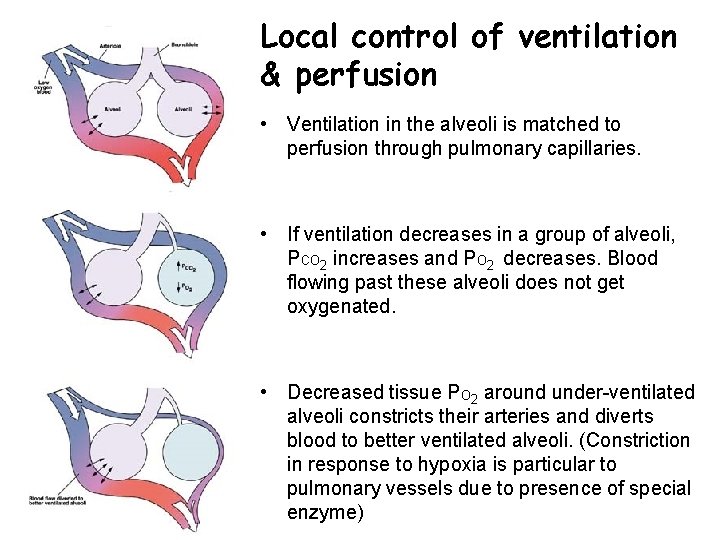
Local control of ventilation & perfusion • Ventilation in the alveoli is matched to perfusion through pulmonary capillaries. • If ventilation decreases in a group of alveoli, PCO 2 increases and PO 2 decreases. Blood flowing past these alveoli does not get oxygenated. • Decreased tissue PO 2 around under-ventilated alveoli constricts their arteries and diverts blood to better ventilated alveoli. (Constriction in response to hypoxia is particular to pulmonary vessels due to presence of special enzyme)
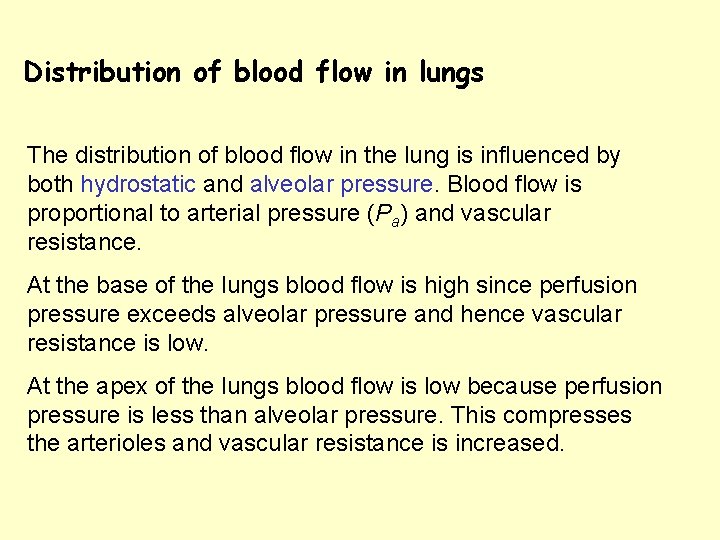
Distribution of blood flow in lungs The distribution of blood flow in the lung is influenced by both hydrostatic and alveolar pressure. Blood flow is proportional to arterial pressure (Pa) and vascular resistance. At the base of the lungs blood flow is high since perfusion pressure exceeds alveolar pressure and hence vascular resistance is low. At the apex of the lungs blood flow is low because perfusion pressure is less than alveolar pressure. This compresses the arterioles and vascular resistance is increased.
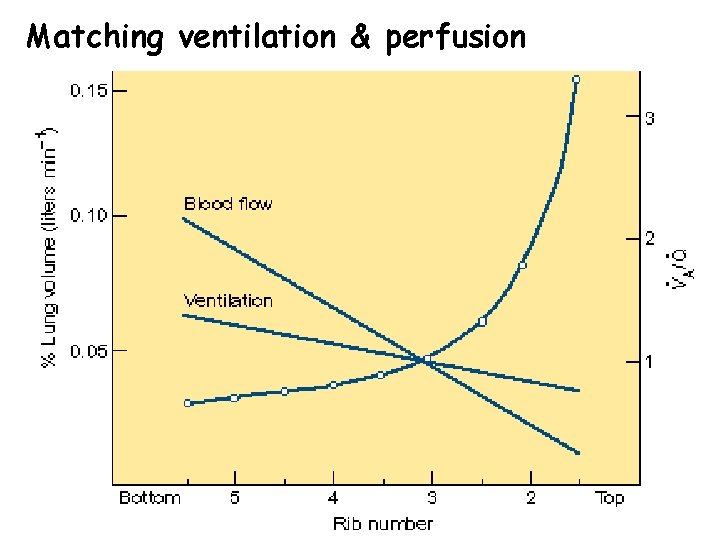
Matching ventilation & perfusion
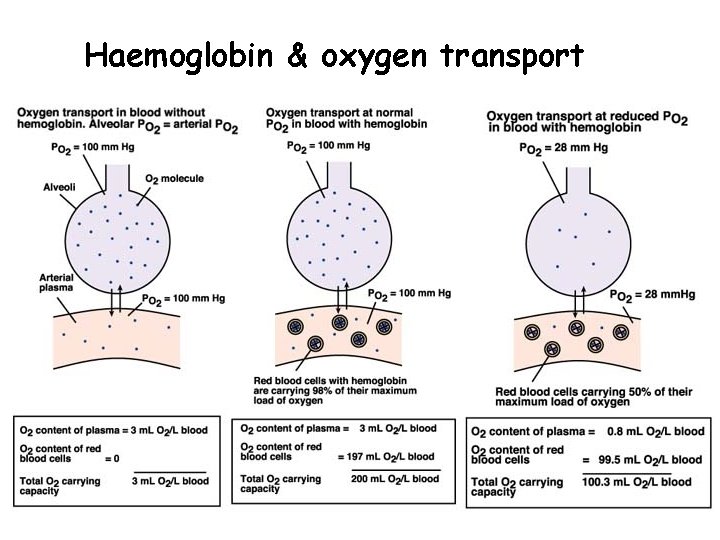
Haemoglobin & oxygen transport
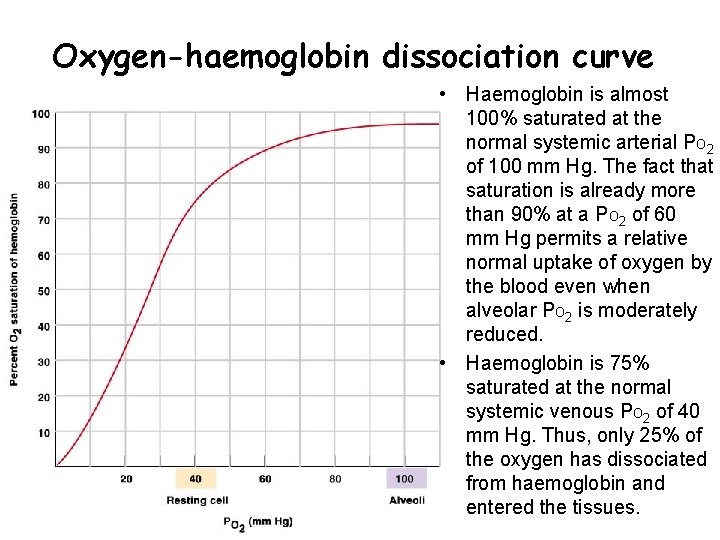
Oxygen-haemoglobin dissociation curve • Haemoglobin is almost 100% saturated at the normal systemic arterial PO 2 of 100 mm Hg. The fact that saturation is already more than 90% at a PO 2 of 60 mm Hg permits a relative normal uptake of oxygen by the blood even when alveolar PO 2 is moderately reduced. • Haemoglobin is 75% saturated at the normal systemic venous PO 2 of 40 mm Hg. Thus, only 25% of the oxygen has dissociated from haemoglobin and entered the tissues.
![Alkalosis. Acidosis, exercising muscle p. H PCO 2 Temp. [DPG] Alkalosis. Acidosis, exercising muscle p. H PCO 2 Temp. [DPG]](http://slidetodoc.com/presentation_image/94fd35ccaa03abaec084a20b49f42822/image-28.jpg)
Alkalosis. Acidosis, exercising muscle p. H PCO 2 Temp. [DPG]
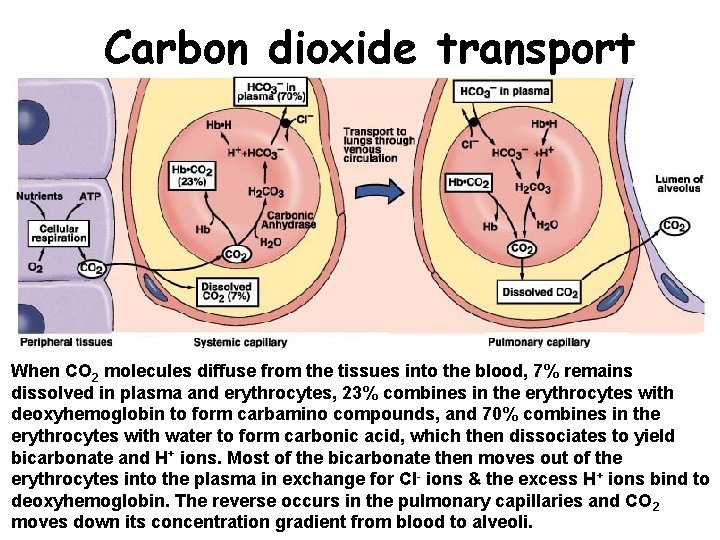
Carbon dioxide transport When CO 2 molecules diffuse from the tissues into the blood, 7% remains dissolved in plasma and erythrocytes, 23% combines in the erythrocytes with deoxyhemoglobin to form carbamino compounds, and 70% combines in the erythrocytes with water to form carbonic acid, which then dissociates to yield bicarbonate and H+ ions. Most of the bicarbonate then moves out of the erythrocytes into the plasma in exchange for Cl- ions & the excess H+ ions bind to deoxyhemoglobin. The reverse occurs in the pulmonary capillaries and CO 2 moves down its concentration gradient from blood to alveoli.
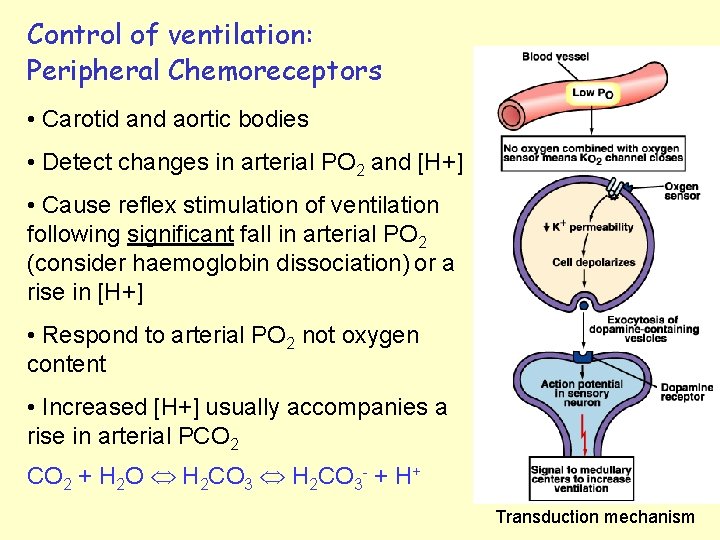
Control of ventilation: Peripheral Chemoreceptors • Carotid and aortic bodies • Detect changes in arterial PO 2 and [H+] • Cause reflex stimulation of ventilation following significant fall in arterial PO 2 (consider haemoglobin dissociation) or a rise in [H+] • Respond to arterial PO 2 not oxygen content • Increased [H+] usually accompanies a rise in arterial PCO 2 + H 2 O H 2 CO 3 - + H+ Transduction mechanism
![Control of Ventilation: Central Chemoreceptors • Medulla • Detect changes in [H+] in CSF Control of Ventilation: Central Chemoreceptors • Medulla • Detect changes in [H+] in CSF](http://slidetodoc.com/presentation_image/94fd35ccaa03abaec084a20b49f42822/image-31.jpg)
Control of Ventilation: Central Chemoreceptors • Medulla • Detect changes in [H+] in CSF around brain • Cause reflex stimulation of ventilation following rise in [H+] (PCO 2) Ventilation is reflexly inhibited by an increase in arterial PO 2 or a decrease in arterial PCO 2/[H+] (hyperventilation)
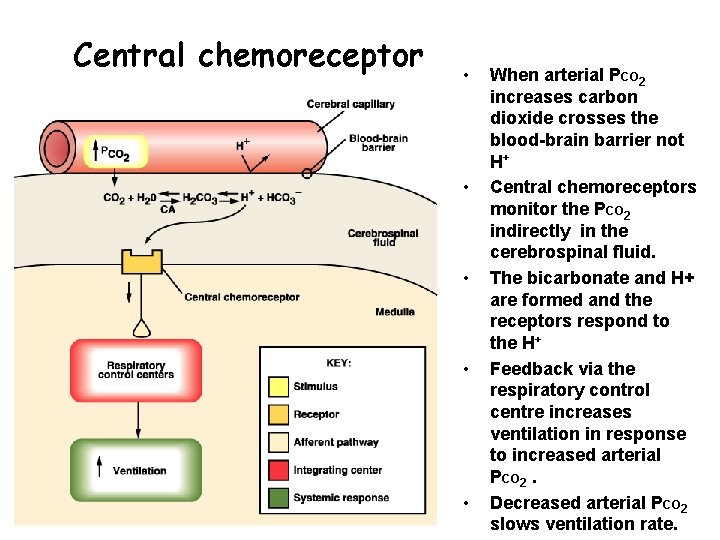
Central chemoreceptor • • • When arterial PCO 2 increases carbon dioxide crosses the blood-brain barrier not H+ Central chemoreceptors monitor the PCO 2 indirectly in the cerebrospinal fluid. The bicarbonate and H+ are formed and the receptors respond to the H+ Feedback via the respiratory control centre increases ventilation in response to increased arterial PCO 2. Decreased arterial PCO 2 slows ventilation rate.
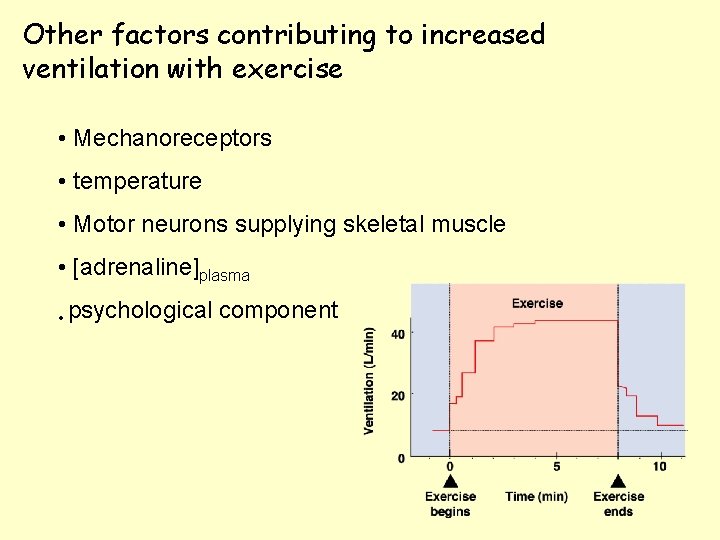
Other factors contributing to increased ventilation with exercise • Mechanoreceptors • temperature • Motor neurons supplying skeletal muscle • [adrenaline]plasma • psychological component

Voluntary Control of Breathing • Descending neural pathways from cerebral cortex to respiratory motor neurons • Cannot over ride involuntary stimuli such as arterial PCO 2 or [H+] • Breath-holding • Hyperventilation
- Slides: 34