Respiratory Medicine Alice HartGeorge Contents ABCDE symptoms SOB

Respiratory Medicine Alice Hart-George

Contents • ABCDE & symptoms: SOB, chest pain, cough/haemoptysis • 1. Respiratory Failure • 2. Asthma & COPD • 3. Bronchietctasis • 4. Granulomatous & Vasculitic Lung Disease - TB, Sarcoidosis, Wegener’s, Churg Strauss, Hypersensitivity pneumonitis (EAA) • 5. Infections • 6. Restrictive Lung Disease (Intrinsic v Extrinsic) • 7. Lung Cancer

A. . B. . CDE • A: Is the patient talking? Airway patent. - Brief PC/PMH/Drugs&Allergy • B: Look: Colour, SOB, Accessory Muscles, RR, Sp. O 2. Listen: Auscultate, Percuss. Cough, Wheeze, Silent. Feel: Trachea, Equal chest expansion • OXYGEN on (COPD: Venturi 24% Sp. O 2 88 -92%) - Sit them up • Peak flow, ABG, CXR, Temperature (+/- Blood culture), Sputum sample

Classic OSCE Presentations Condition Signs & Sounds Pulmonary fibrosis Gradual onset SOB, dry cough, fine bibasal inspiratory crackles, clubbing in up to 50% COPD SOB, productive cough, air entry Wheeze, hyperexpanded/barrel chest, prolonged expiratory time/pursed lips Pneumonia SOB, productive cough, bronchial breathing, end expiratory crackles, fever, pleuritic chest pain. Non-specific in elderly. Pulmonary oedema SOB, fine end-inspiratory crackles, productive cough (frothy pink), orthopnea/PND, JVP, 3 rd heart sound. Pleural effusion SOB, dry cough, pleuritic chest pain, reduced air entry, reduced vocal resonance, stony dull to percussion. PJP/PCP Dry cough, fever, malaise, perihilar shadowing, immunocompromised (HIV, RA). Desaturation on mobilizing. Pneumonectomy Scar, reduced/absent breath sounds. Lung Ca/old Rx for TB. Pleural rub: non-specific sign occurring with pleural inflammation of any cause
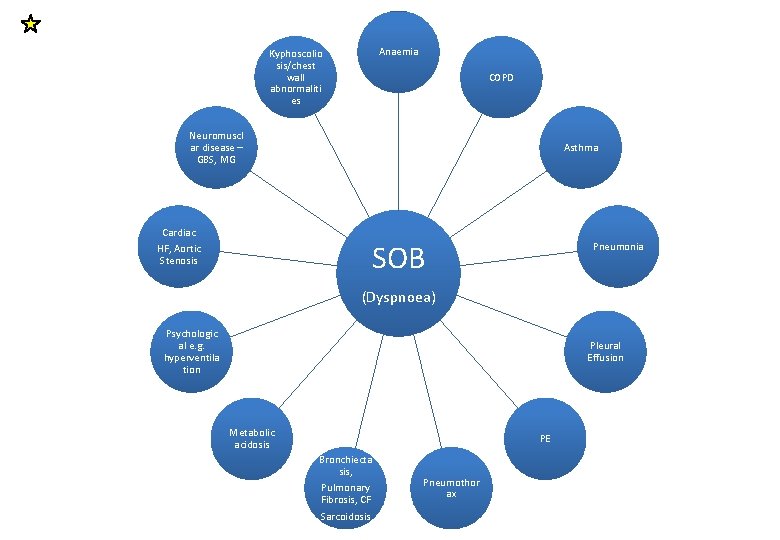
Anaemia Kyphoscolio sis/chest wall abnormaliti es COPD Neuromuscl ar disease – GBS, MG Cardiac HF, Aortic Stenosis Asthma SOB Pneumonia (Dyspnoea) Psychologic al e. g. hyperventila tion Pleural Effusion Metabolic acidosis PE Bronchiecta sis, Pulmonary Fibrosis, CF Sarcoidosis Pneumothor ax
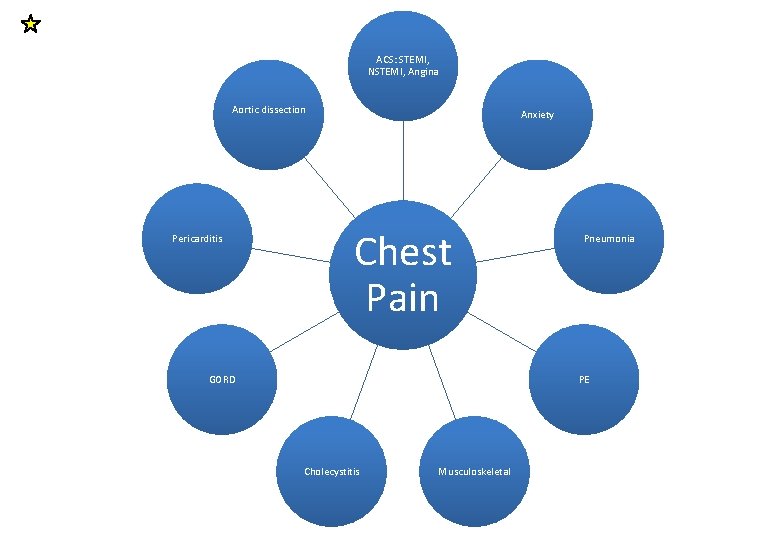
ACS: STEMI, NSTEMI, Angina Aortic dissection Pericarditis Anxiety Chest Pain GORD Pneumonia PE Cholecystitis Musculoskeletal
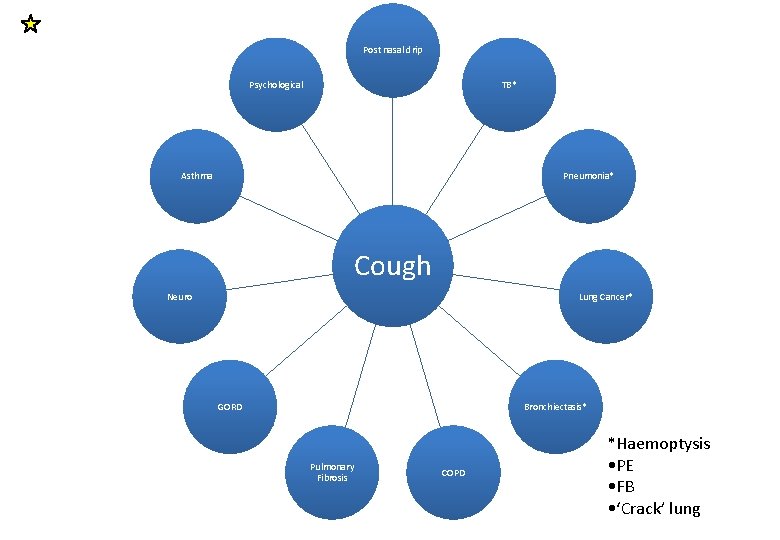
Post nasal drip Psychological TB* Asthma Pneumonia* Cough Neuro Lung Cancer* GORD Bronchiectasis* Pulmonary Fibrosis COPD *Haemoptysis • PE • FB • ‘Crack’ lung
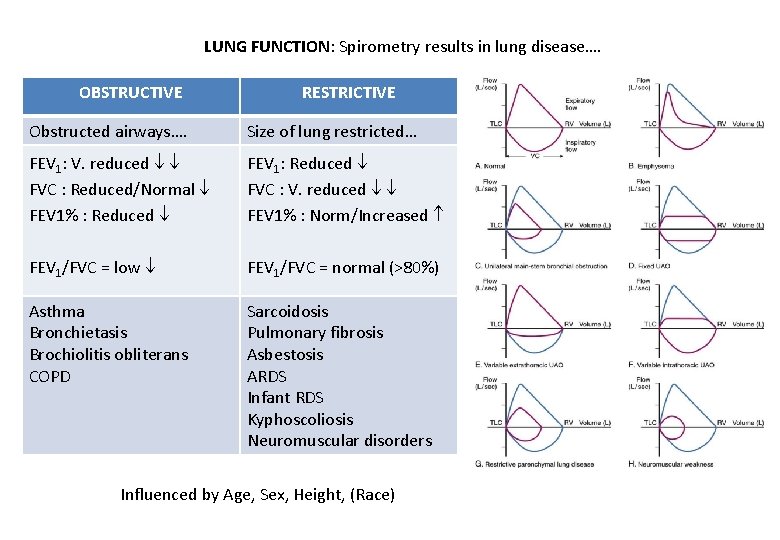
LUNG FUNCTION: Spirometry results in lung disease…. OBSTRUCTIVE RESTRICTIVE Obstructed airways…. Size of lung restricted… FEV 1: V. reduced FVC : Reduced/Normal FEV 1% : Reduced FEV 1: Reduced FVC : V. reduced FEV 1% : Norm/Increased FEV 1/FVC = low FEV 1/FVC = normal (>80%) Asthma Bronchietasis Brochiolitis obliterans COPD Sarcoidosis Pulmonary fibrosis Asbestosis ARDS Infant RDS Kyphoscoliosis Neuromuscular disorders Influenced by Age, Sex, Height, (Race)

1. Respiratory Failure • Failure of Gas Exchange (O 2 in, CO 2 out) • Need blood (perfusion, Q) to come into close proximity to air (ventilation, V) • 2 Types: – Hypoxaemic Type I – low oxygen levels (ABG Sa. O 2 <8 k. Pa) – Hypercapnic Type II – low oxygen levels and high CO 2 levels (ABG Sa. CO 2 >6. 7 k. Pa)

Hypoxaemic (Type I) • Causes: – V/Q mismatch, the air isn’t going to the same bits as the blood. E. g. Pneumonia, PE, Asthma, Pulmonary oedema. – Shunting of blood from pulmonary to systemic circulation, blood bypasses the lungs. – Hypercapnea. O 2 and CO 2 levels in alveoli interrelated. The more CO 2, the less space for O 2 – High altitude. Less O 2 in the air. • Management: – Give more. High flow O 2. Make sure it’s not Type II! – CPAP – Continuous Positive Airway Pressure – Reverse underlying cause. Treat the infection, break the clot

Hypercapnic (Type II) • Causes: – Ventilation. Either total ventilation (i. e. resp rate) or in dead space of lung. COPD, opiates, respiratory exhaustion – Inspired CO 2. Only really an issue in intubated patients rebreathing their own CO 2 • Management: – Natural Ventilation. Reverse sedating drugs, Give O 2 – COPD: Restrict O 2 Venturi 24% Sp. O 2 88 -92%, Neb Salbut. & Ipatrop Br. – Assisted Ventilation • Invasive – Intubate and give positive pressure ventilation to keep alveoli open and better ventilated. • Non Invasive (NIV) – Bi. PAP. Two different pressures, one for inhalation, one for exhalation. Bi PAP for type II.
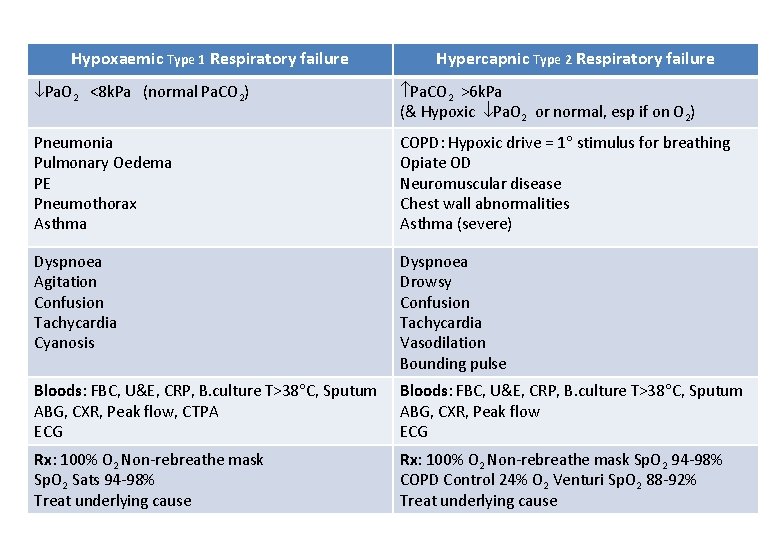
Hypoxaemic Type 1 Respiratory failure Hypercapnic Type 2 Respiratory failure Pa. O 2 <8 k. Pa (normal Pa. CO 2) Pa. CO 2 >6 k. Pa (& Hypoxic Pa. O 2 or normal, esp if on O 2) Pneumonia Pulmonary Oedema PE Pneumothorax Asthma COPD: Hypoxic drive = 1 stimulus for breathing Opiate OD Neuromuscular disease Chest wall abnormalities Asthma (severe) Dyspnoea Agitation Confusion Tachycardia Cyanosis Dyspnoea Drowsy Confusion Tachycardia Vasodilation Bounding pulse Bloods: FBC, U&E, CRP, B. culture T>38 C, Sputum ABG, CXR, Peak flow, CTPA ECG Bloods: FBC, U&E, CRP, B. culture T>38 C, Sputum ABG, CXR, Peak flow ECG Rx: 100% O 2 Non-rebreathe mask Sp. O 2 Sats 94 -98% Treat underlying cause Rx: 100% O 2 Non-rebreathe mask Sp. O 2 94 -98% COPD Control 24% O 2 Venturi Sp. O 2 88 -92% Treat underlying cause

2. Asthma • Common chronic disease characterised by reversible expiratory airflow limitation, cough, SOB, wheeze, chest tightness, especially at night/with exercise. • Hx Atopy (Eczema, Asthma, Hay fever, Allergies, Ig. E) • Diurnal variation in symptoms (& peak flow) • Examination can be normal. • Very common; 5 -10% of population. Causes 2000 deaths/year, prevalence increasing in West.

Asthma • Can be classified as: – Extrinsic. Positive Ig. E, (‘allergic’). Occurs in childhood, response to environmental irritants, often associated with atopy. Often remits during teens, but may recur in later life. – Intrinsic. Normal Ig. E (‘non-allergic’), Develops later in life or post URTI. More progressive and less responsive to treatment.

Pathophysiology • Irritants cause bronchospasm and inflammation. Inflammation leads to oedema, mucus secretion, smooth muscle hypertrophy and fibrosis. • Stimuli : House dust mite, pollen, cat hair, viral infection, cold air, cigarette smoke, exercise, emotional stress. • Drugs contraindicated: BB, NSAIDs.
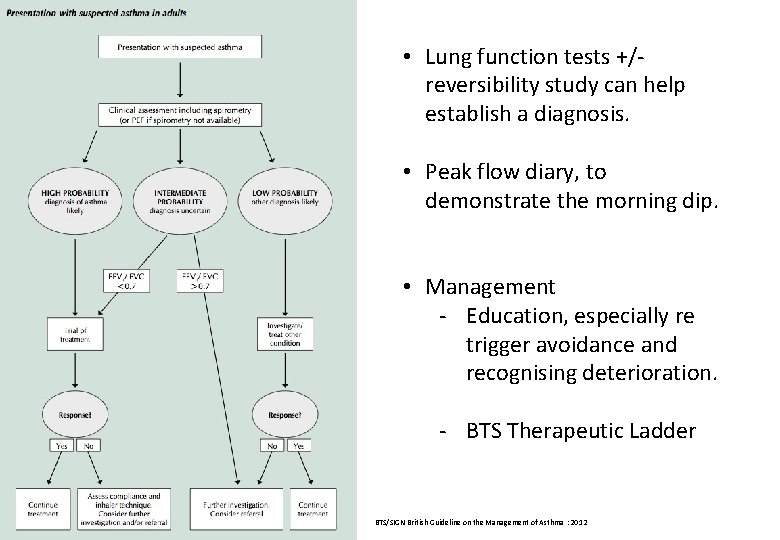
• Lung function tests +/- reversibility study can help establish a diagnosis. • Peak flow diary, to demonstrate the morning dip. • Management - Education, especially re trigger avoidance and recognising deterioration. - BTS Therapeutic Ladder BTS/SIGN British Guideline on the Management of Asthma : 2012
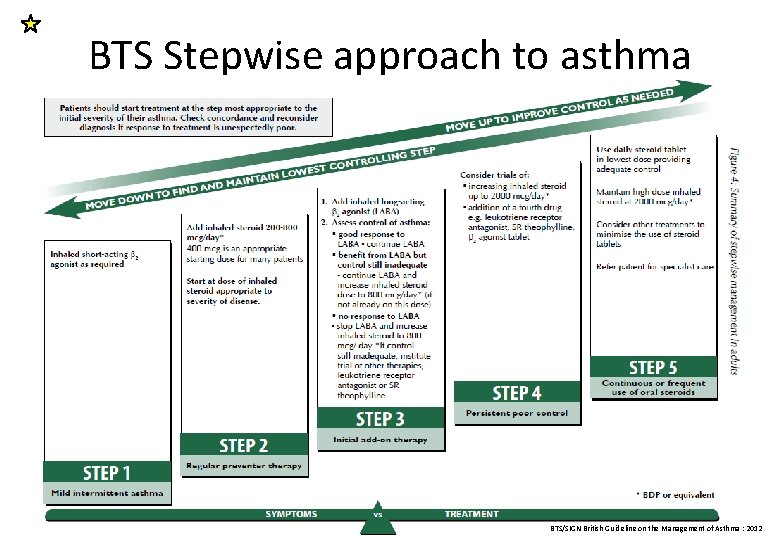
BTS Stepwise approach to asthma BTS/SIGN British Guideline on the Management of Asthma : 2012

COPD • Chronic, progressive respiratory disorder characterised by airflow limitation of only limited reversibility • Very common, kills >20, 000 people per year in UK • Risk factors: Smoking, smoking, atmospheric pollutants, alpha 1 antitrypsin deficiency. • Chronic productive cough for 3 months each year for 2 consecutive years, or abnormal permanent dilatation of terminal air spaces.

COPD • Smoking causes inflammation, mucus gland hypertrophy and mucus production. Airflow limitation in small airways. • Destruction of lung tissue and dilatation of distal airspaces which collapse. • Lungs lose pliability, loss of elastic recoil and gain more dead air space/trapping (hence hyperinflation), increasing the work of breathing and causing SOB. • As disease progresses, the poorly ventilated lung tendency to accumulate CO 2, so to compensate, the respiratory centres become tolerant to high blood CO 2 and focus shifts to respiratory drive on hypoxaemia; ‘hypoxic drive’.

Presentation • Progressive productive cough (yellow/white), SOB, often over many years. Strong smoking history. Be aware of ‘asthma’ in older adults! Get a smoking hx! • Often exercise tolerance and wheeze • O/E: Hyperinflation, coarse crackles, wheeze, breath sounds, hyperresonance on percussion. Prolonged expiration, pursed lips, rail grabbing. • Spirometry helps confirm disease and assess severity. FEV 1/FVC <70% (FEV 180% predicted) • (Post nebs PEF can help differentiate from asthma if doubtful)
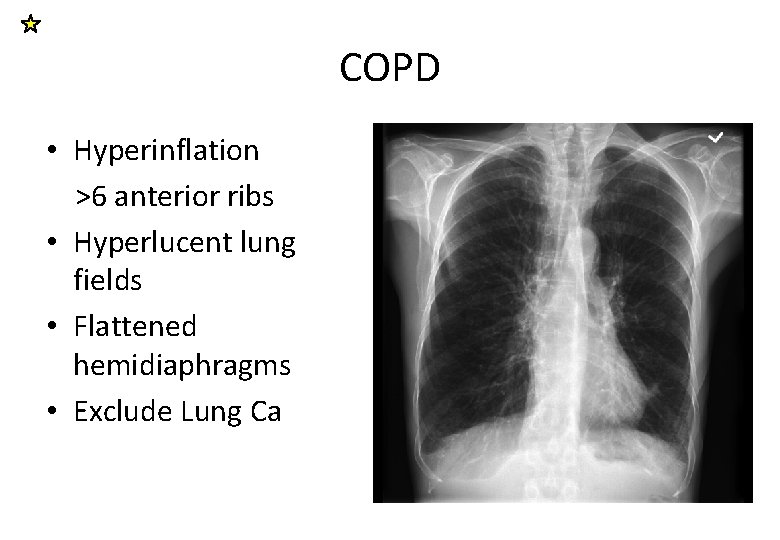
COPD • Hyperinflation >6 anterior ribs • Hyperlucent lung fields • Flattened hemidiaphragms • Exclude Lung Ca

Management • STOP SMOKING! • Short acting B 2 Agonists, LAB 2 A, LAmuscarinic antagonist, Inhaled Corticosteroids, Anticholinergics. • Influenza & Pneumococcal vaccines • Pulmonary Rehab, especially if recent exacerbation • Complications: Respiratory failure, Cor Pulmonale, Pneumothorax, Polycythemia. • Discuss ceilings of treatment sooner rather than later. • Home O 2 (24 -28% Venturi: 88 -92%)

Acute exacerbation of COPD • • • Like Pneumonia but NO CONSOLIDATION on CXR Different Abx to CAP/HAP Often worsening symptoms & purulent sputum Ix: Basic obs, Sp. O 2, Peak flow, ABG, CXR, Bloods (FBC, U&E), Sputum, Urine, Blood culture if febrile. Rx: O 2 Venturi 24 -28% Sp. O 2 88 -92% Neb Salbutamol 5 mg & Ipatropium bromide 500 mcg Oral/IV steroid (Prednisolone 30 mg PO 14/7) Abx trust guidelines e. g. Amox 500 mg TDS/ Doxy 200 mg OD Non invasive ventilation (NIV aka Bi. PAP) for ACIDOTIC CO 2 retainers, during hypercapnoeic exacerbations Pa. CO 2 ≥ 6 / p. H ≤ 7. 35 to acidosis mortality

3. Bronchiectasis • Abnormal and Permanent dilatation of bronchi • Focal or diffuse impaired clearance of bronchial secretions 2 infection (chronic, recurrent). • Cough, Purulent sputum, Haemoptysis, Wheeze, SOB, Clubbing, Coarse inspiratory creps at bases. Aetiology Congenital Acquired 1 ciliary dyskinesia Post-infective (Measles, Pertussus, Klebsiella, TB, HIV, Pneumonia) Kartagener’s Obstruction (Tumour, Inhaled FB) Young’s Allergic (Aspergilosis) CF Other (RA, UC, ideopathic, hypogammaglobulinaemia)

Bronchiectasis • Ix: Sputum, Spirometry (Obstructive), CXR, HRCT (thick large airways larger than blood vessels), Blood Immunoglobulins, Sweat test. • Rx: Physio, bronchodilator, steroids, Abx if 2 infection. High resolution CT • Bronchial wall thickening • Dilated bronchi appear ‘beaded’ • Signet ring sign
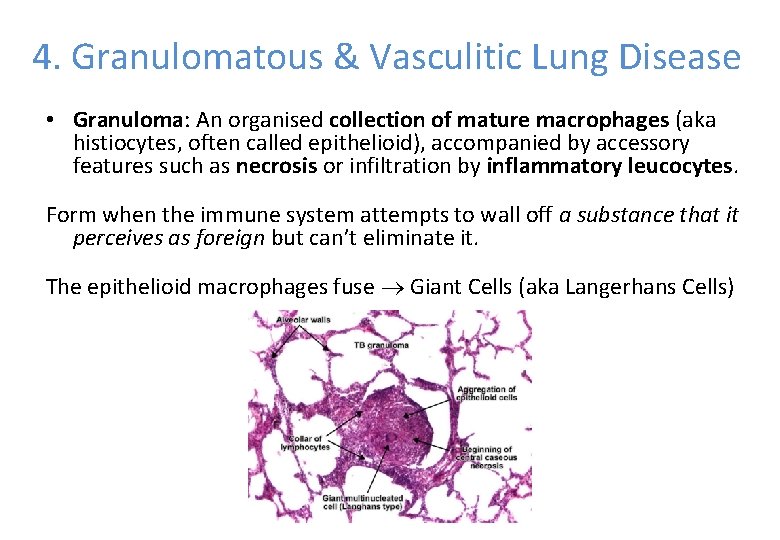
4. Granulomatous & Vasculitic Lung Disease • Granuloma: An organised collection of mature macrophages (aka histiocytes, often called epithelioid), accompanied by accessory features such as necrosis or infiltration by inflammatory leucocytes. Form when the immune system attempts to wall off a substance that it perceives as foreign but can’t eliminate it. The epithelioid macrophages fuse Giant Cells (aka Langerhans Cells)

Granulomatous & Vasculitic Lung Disease • Many causes, differentiated by clinical phenotype/accessory features. – Infection: • TB • PCP/PJP – Autoimmune: • Sarcoidosis • Wegener’s Granulomatosis • Churg Strauss – Inflammation from foreign substance: Hypersensitivity Pneumonitis (aka EAA: extrinsic allergic alveolitis) • Bird fancier’s lung • Farmer’s lung • Mushroom Picker’s lung

TB Most common ID killer worldwide 1. 4 million deaths 2010 M tuberculosis, Acid-Fast Bacilli smear and culture. Slow growing, obligate aerobic, intracellular parasite. Non spore forming, non-motile, only living in humans. • Recognised by time of Hippocrates as infectious, termed phthisis (wasting disease), used to be called consumption in Europe for same reason. • Rare in West unless risk factor present • •

TB • Mycobacteria are highly antigenic, promote vigorous non specific response, which is exactly what they need to do to get into phagocytes, where they set up home. Also provides means of spread via lymph nodes. • Extrapulmonary disease is rare except in immunocompromised, who get disease in Liver, Bone marrow, spleen, kidneys, bones (Pott’s Disease), and Brain. • Typical lesions are granulomas with epithelioid macrophages and Langerhans cells with central caseation and necrosis with a rim of fibrosis. • Initial lesions may heal and develop latent infection, before reactivating as pulmonary or generalised disease (anti TNF drugs CXR) • If unable to halt the initial infection, pt develops primary progressive TB, rapid onset of tuberculous pneumonia with purulent exudate.

Presentation • Cough, haemoptysis, weight loss, fever, night sweats • Risk: HIV, Exposure, Endemic area, Homeless/Prison, Overcrowding, Malnutrition, Immunocompromised. • Elderly can just present with non resolving lung symptoms. • CXR: Consolidation, Apical cavitation/granuloma (Ghon focus), Hilar lymphadenopathy, fibrosis, calcification • • TB meningitis: 2 -3/52 headache, change mental state Coma Pott’s disease: Spinal lesions, pain, weakness GU TB: UTI Sx or PID Sx/Epididymitis Sx GI TB: Non healing ulcers, pain, malabsorption, diarrhoea, PR blood.
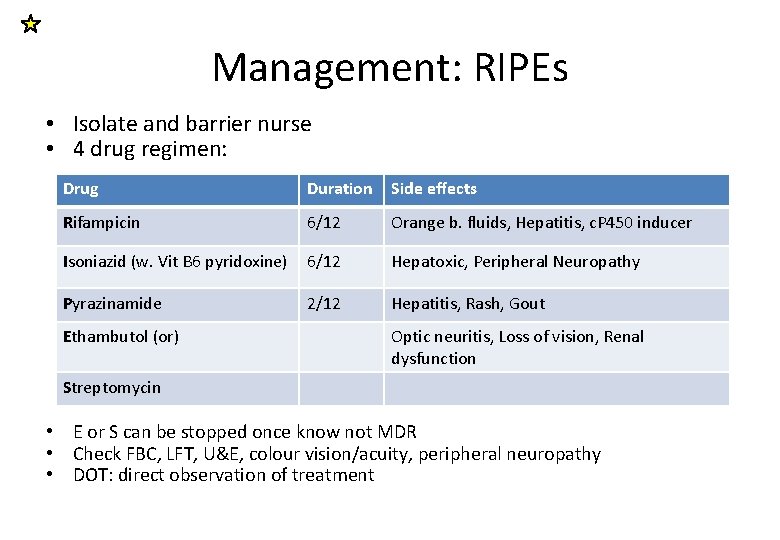
Management: RIPEs • Isolate and barrier nurse • 4 drug regimen: Drug Duration Side effects Rifampicin 6/12 Orange b. fluids, Hepatitis, c. P 450 inducer Isoniazid (w. Vit B 6 pyridoxine) 6/12 Hepatoxic, Peripheral Neuropathy Pyrazinamide 2/12 Hepatitis, Rash, Gout Ethambutol (or) Optic neuritis, Loss of vision, Renal dysfunction Streptomycin • E or S can be stopped once know not MDR • Check FBC, LFT, U&E, colour vision/acuity, peripheral neuropathy • DOT: direct observation of treatment

Sarcoidosis • • Granulomas form in multiple organs, cause unknown. ? changes in immune system following exposure to an agent. Usually affects lungs or lymph nodes, but can affect any organ, generally gradual onset. Women slightly > Men, > African descent, in whom disease is both more prevalent and more likely to be symptomatic. 2/3 people with radiological signs of Sarcoid are asymptomatic. Acute presentation Chronic presentation Fatigue, weight loss, arthritis, fever, dry eyes, dry cough, SOB. Fibrotic lung disease (lymphocytic alveolitis) Hilar lymphadenopathy Anterior Uveitis/ chorioretinitis Dactilitis Parotitis Facial nerve palsy Hypercalcaemia (hydroxlation of vit. D by sarcoid macrophages) Erythema nodosum (red itchy painful lower leg rash) Lupus pernio (facial/arms rash) Hepato-Splenomegaly Inspiratory crackles = rare Restrictive Lung FT volume & compliance, FEV 1/FVC= 90% Serum ACE and ESR = high Deranged LFTs, Ig CXR: reticulo-nodular shadowing
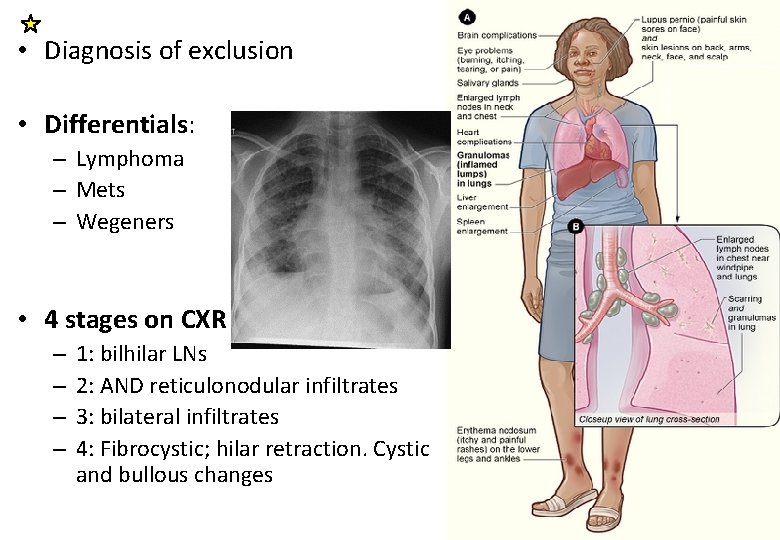
• Diagnosis of exclusion • Differentials: – Lymphoma – Mets – Wegeners • 4 stages on CXR – – 1: bilhilar LNs 2: AND reticulonodular infiltrates 3: bilateral infiltrates 4: Fibrocystic; hilar retraction. Cystic and bullous changes

Sarcoidosis Mangement • NSAIDs – in mild disease • Steroids • Common steroid alternatives (Methotrexate, azathioprine) • Hydroxychloroquine (for bone involvement)

Wegener’s Granulomatosis (aka Granulomatosis with polyangiitis aka ANCA-associated granulomatous vasculitis) • Systemic Necrotizing Vasculitis • Autoimmune attack of small/medium vessels • via Anti-neutrophil cytoplasmic antibodies (c-ANCA+ 75 -90%) either Cytoplasmic or Perinuclear activate neutrophils in affected tissues, targeting vessel endothelium Vasculitis and granuloma formation. • Unknown aetiology • Affects URT, nose, LRT, lungs, kidneys • Rare (10 : 1, 000) M=F > N Europeans (Caucasian 90%). Symptoms: Respiratory: Recurrent LRTI, Cough, SOB, Haemoptysis, nasal congestion, epistaxis, ulcerated mucosa, otitis media, saddle nose = late presentation Renal: Haematuria, fever, night sweat, weight loss Eyes: Episcleritis, Uveitis, Optic nerve vasculitis
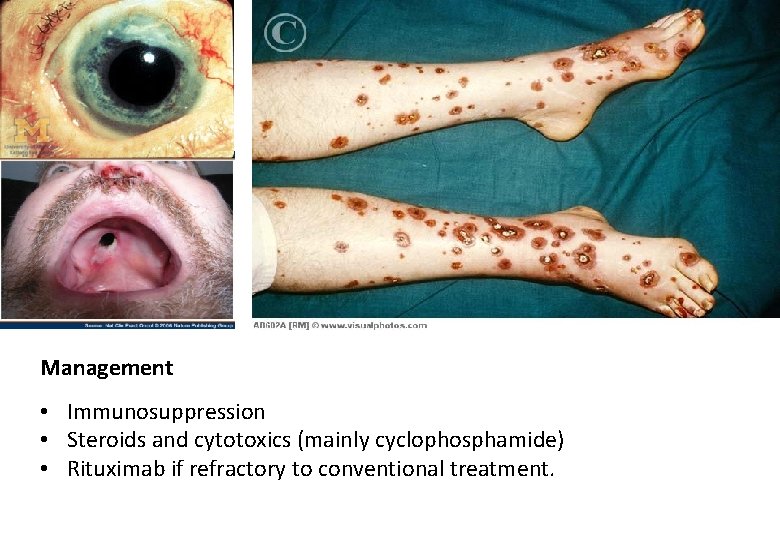
Management • Immunosuppression • Steroids and cytotoxics (mainly cyclophosphamide) • Rituximab if refractory to conventional treatment.

Churg Strauss syndrome (aka allergic granulomatous angiitis) • • • Systemic Necrotizing Vasculitis Autoimmune attack of small/medium vessels via Anti-neutrophil cytoplasmic antibodies (p. ANCA+ 75%) Eosinophilic infiltrative disease and Granulomatous inflammation Rare. Unknown cause Key features/stages: 1. Allergies (new) 2. Asthma (esp mature onset) and Allergic rhinitis 3. Organ involvement - Sinusitis Eosinophilic pneumonia Mononeuritis multiplex (vasculitic neuropathy) Gastroenteritis and necrotised intestines Systemic small vessel vasculitis and granulomatosis, with pulmonary, cardiac, derm, renal and peripheral nerve involvement, causing sx related to those systems. Progresses to a coronary arteritis and MI.

Churg Strauss syndrome Management • Specialist involvement for each organ system affected, resp cardio derm etc. • Immunosuppression via Steroids • Cytotoxics, esp Cyclophosphamide or azathioprine. • Life long follow up, with monitoring of ESR and degree of eosinophilia. • 5 year survival with treatment approx 60%, with death due to MI, CRF, GI bleed, Cerebral Haemorrhage or Respiratory failure

Hypersensitivity pneumonitis aka EAA Extrinsic Allergic Alveolitis • Inflammation within the alveoli due to hypersensitivity to inhaled allergens, often occupational exposure. • Combination of type III (immune complex) and type IV (cell mediated) hypersensitivity • More of a syndrome, a clinical phenotype with lots of causes • Famous examples include farmer’s lung, mushroom picker’s lung or pigeon fancier’s lung

Hypersensitivity pneumonitis • Diffuse inflammation of lung parenchyma, characterised by poorly formed non -caseating granuloma with Langerhans cells and interstitial fibrosis. • Can progress to alveolar destruction; ‘Honeycombing’ • The condition where granuloma meets fibrosis • Ig. G mediated, patients have high levels. • 3 ways to present: – Acute: 4 -6 hours post heavy exposure to agent, with chills, malaise, cough, SOB and headache. Resolves on cessation of exposure – Subacute: Intermittent episodes of mini version of above, with fatigue and weight loss – Chronic: Often no history of above episodes, present with insidious onset cough, SOB and weight loss. Removing agent gives only partial relief.

Hypersensitivity pneumonitis Management • Cease exposing yourself to pigeons, no matter how much you fancy them. No mushroom picking, even if it’s magical. • Steroids if severe

5. Infections • Pneumonia • Aspergillosis
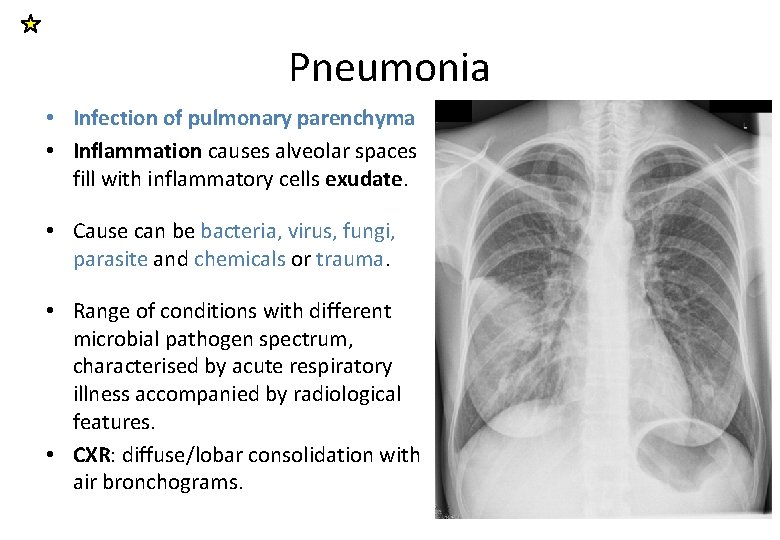
Pneumonia • Infection of pulmonary parenchyma • Inflammation causes alveolar spaces fill with inflammatory cells exudate. • Cause can be bacteria, virus, fungi, parasite and chemicals or trauma. • Range of conditions with different microbial pathogen spectrum, characterised by acute respiratory illness accompanied by radiological features. • CXR: diffuse/lobar consolidation with air bronchograms.

Pneumonia • Generally classified by the context in which it develops – – Community Acquired (CAP): Includes within 48 hours admission Hospital Acquired (HAP): Occuring >48 hrs of admission Aspiration Pneumonia of Immunocompromise • Alternatively, by anatomic distribution of disease – Lobar – Bronchopneumonia – Interstitial
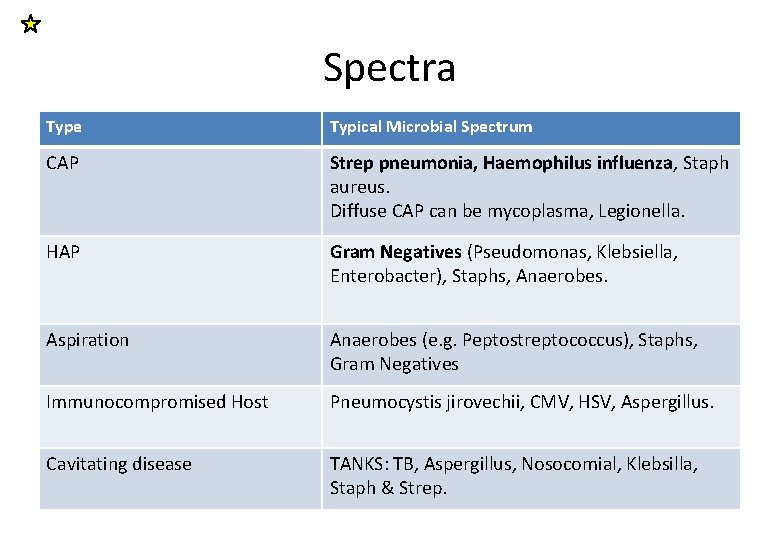
Spectra Type Typical Microbial Spectrum CAP Strep pneumonia, Haemophilus influenza, Staph aureus. Diffuse CAP can be mycoplasma, Legionella. HAP Gram Negatives (Pseudomonas, Klebsiella, Enterobacter), Staphs, Anaerobes. Aspiration Anaerobes (e. g. Peptostreptococcus), Staphs, Gram Negatives Immunocompromised Host Pneumocystis jirovechii, CMV, HSV, Aspergillus. Cavitating disease TANKS: TB, Aspergillus, Nosocomial, Klebsilla, Staph & Strep.

Medically important bacteria Gram positive cocci Staphylococci S. aureus Coagulase negative staphylococci Streptococci Group A streptococcus (S. pyogenes) Group B Group C and G Group D = enterococcus S. pneumoniae Viridans type streptococci Peptococcus / Peptostreptococcus Gram positive rods (bacilli) Bacillus e. g. B. cerus and B. anthracis Corynebacterium Propionibacterium Listeria monocytogenes Clostridium e. g. C. difficile Mod 302 ID session 1 2009: Dr Martin Llewelyn Gram negative cocci Neisseria N. meningitidis N. gonorrhoea Moraxella (Branhamella) catarrhalis Gram negative rods Haemophilus influenzae Enterobacteriaciae Salmonella & Shigella Eschericia coli Klebsiella and Enterobacter Proteus Pseudomonas e. g P. aeruginosa Bacteroides e. g. B. fragilis Campylobacter and Helicobacter Vibrio cholerae Bordetella pertussis Legionella Anaerobes shown in green

Pneumonia Symptoms: • Cough, SOB +/- purulent sputum. • Fever, Pleuritic chest pain, haemoptysis • Headaches, confusion, myalgia, malaise • May be vague presentation in immunocompromised or elderly. O/E: • Crackles, bronchial breathing, pleural rub • ↑ RR, Hypotension, Confusion Ix: • Bloods – FBC, CRP, U&E (Urea & CURB 65) • CXR, Sputum culture, VBG Rx: • Supportive – IV Fluids, O 2, Chest physio. • Antibiotics – Local guidelines, pending culture
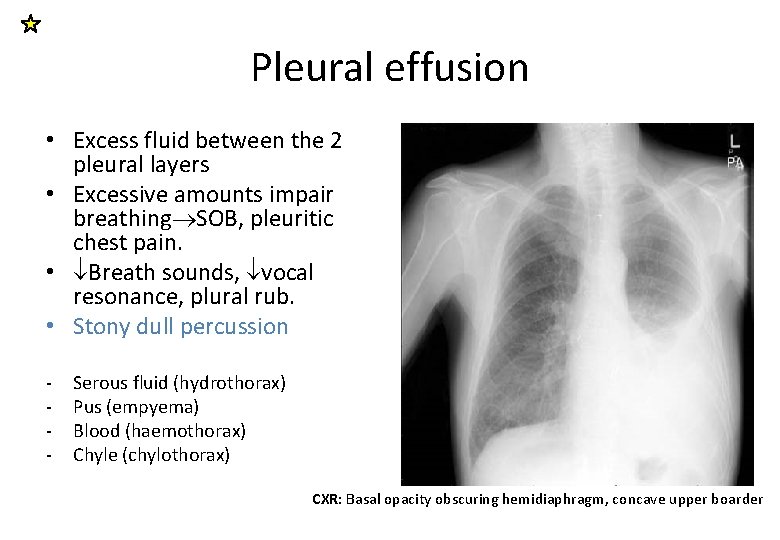
Pleural effusion • Excess fluid between the 2 pleural layers • Excessive amounts impair breathing SOB, pleuritic chest pain. • Breath sounds, vocal resonance, plural rub. • Stony dull percussion - Serous fluid (hydrothorax) Pus (empyema) Blood (haemothorax) Chyle (chylothorax) CXR: Basal opacity obscuring hemidiaphragm, concave upper boarder

Transudate v Exudate Transudate <30 g/L Exudate >30 g/L Systemic Local Cardiac (e. g. LVF – common, restrictive pericarditis) Renal (e. g. Nephrotic syndrome) Liver (e. g. Cirrhosis, Budd Chiari) Endocrine (e. g. Hypothyroid) Nutritional (e. g. Hypoalbumin) Carcinoma (e. g. bronchus) Infection (e. g. lobar pneumonia) Inflammation (e. g. TB) RA PE Surgical ward – pancreatitis, post-CABG

6. Restrictive Lung Disease (RLD) (aka restrictive ventilatory defects) • Essentially effects due to reduced lung volume, TLC, VC, without changes to airway resistance. • Can be divided anatomically into: – Intrinsic. Parenchymal Disease. Inflammation and scarring of lung tissue (Interstitial lung disease), or filling of airspaces with exudate and debris (pneumonitis). Impairs gas exchange (Exercise O 2) – Extrinsic. Extraparenchymal. Diseases affecting the bits that work outside the organ e. g. neuro, leading to inadequate ventilation and respiratory failure.
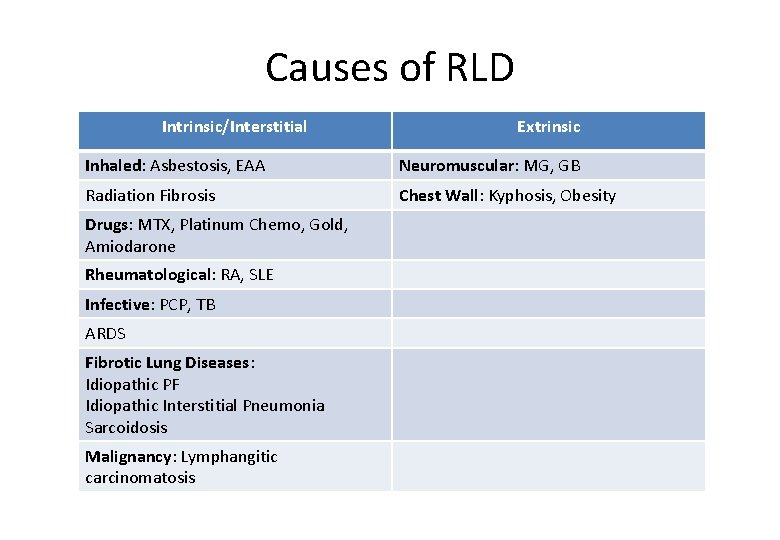
Causes of RLD Intrinsic/Interstitial Extrinsic Inhaled: Asbestosis, EAA Neuromuscular: MG, GB Radiation Fibrosis Chest Wall: Kyphosis, Obesity Drugs: MTX, Platinum Chemo, Gold, Amiodarone Rheumatological: RA, SLE Infective: PCP, TB ARDS Fibrotic Lung Diseases: Idiopathic PF Idiopathic Interstitial Pneumonia Sarcoidosis Malignancy: Lymphangitic carcinomatosis

Intrinsic RLDs • Inhaled substances – Inorganic • • Silicosis Asbestosis Berylliosis Coal – Organic – Systemic lupus erythematosus – Rheumatoid arthritis – Ankylosing spondylitis • • Hypersensitivity pneumonitis. Farmers, Mushrooms, Pigeons • Drug induced – Antibiotics. Nitrofurantoin – Chemotherapeutic drugs – Antiproliferatives. Cyclophosphamide, MTX, • Sulfasalazine – Gold – Antiarrhythmic agents. Phenytoin, amiodarone – Statins • Connective tissue disease – Systemic sclerosis – Polymyositis – Dermatomyositis • Infection – – – Atypical pneumonia Pneumocystis pneumonia (PCP) Tuberculosis Chlamydia trachomatis Respiratory Syncytial Virus Idiopathic – – – Sarcoidosis Vasculitides Idiopathic pulmonary fibrosis Hamman-Rich syndrome Antisynthetase Syndrome Malignancy – Lymphangitic carcinomatosis

Symptoms of RLD Intrinsic • SOB on exertion. Due to gas exchange • Dry Cough • Haemoptysis in vasculitic types • Wheeze = rare but happens • Chest pain uncommon Extrinsic • SOB, Exercise tolerance, Recurrent Infection • Often associated spinal deformity, muscle weakness

Signs of RLD • • Clubbing – IPF, Asbestosis Fine crackles – Any interstitial Chest wall disorders/Obesity – Extrinsic disorder Extrapulmonary findings: – Erythema nodosum: Sarcoid – Maculopapular rash: SLE – Telangectasia: Scleroderma/CREST – Joint involvement: RA • Cor pulmonale – Pulmonary HTN R heart failure, ankle swelling, ascites, loud P 2

History in RLD • Thorough history, need to elicit which exposures and for how long. Travel, Social and Drug History all important. • Duration can give a clue: – Acute: EAA, Acute interstitial pneumonitis, eosinophilic pneumonia – Subacute: EAA, Sarcoid, Drug induced, Rheum – Chronic: EAA, IPF, Sarcoid, Pulmonary Histiocytosis • Smoking History • Some types familial, e. g. IPF, Sarcoid

Investigations in RLD • Bloods. Can give clue to underlying cause, polycythaemia RBC/Hct indicates hypoxia and WCC pneumonitis. • Rheum Bloods, Serum ACE, CK. • CXR – Reticular pattern. High Res-CT to follow. Reticular pattern indicative, fibrosis=honeycombing • Lung Function tests to stage severity

Management of RLD • Depends on Cause • Include Steroids, immunosupressives and cytotoxics • May have little effect • Lung Transplant

7. Lung cancer • Most common malignancy in West • 40, 000 new cases in UK/year • More deaths than colon, prostate and breast combined • 95% are attributable to smoking • 1 Smoker: Squamous cell carcinoma • 1 Non smoker: Adenocarcinoma • Symptoms: none, cough, SOB, haemoptysis, chest pain, anorexia, weight loss, dysphagia, hoarse voice (Right Laryngeal Nerve)
Lung cancer Small cell (oat cell) Non small cell (NSCLC) Share common prognoses/treatment 15 -20% central airways, grows rapidly, spreads early Sqaumous cell: 35 -40% large airways, grows slowly, spreads late Adenocarcinoma: 20 -30% peripheral, more common in nonsmokers Large cell (anaplastic): 5 -10% heterogeneous undifferentiated tumours Other: Undifferentiated, Carcinoid. . rare

Lung cancer • - Investigations: Bloods: FBC, LFT, U&E/Creatinine, Calcium CXR: solid masses visible/nodes Biopsy (histology) CT & staging (TNM- Curative/Palliative? ) • Treatment: Chemotherapy, Radiotherapy, Surgery.

Lung cancer • Pancoast tumour: Lung apex- brachial plexus. Shoulder pain, ulnar distribution. 1 st-2 nd ribs. • Horner’s syndrome (Horny PAMELa)- sympathetic nerve supply Ptosis, Anhydrosis (ipsilateral loss of sweating), Miosis (constricted pupil), Enopthalmos, Loss of ciliospinal reflex (dilation of the ipsilateral pupil in response to pain applied to the neck, face, and upper trunk). • Phrenic nerve: elevation of hemidiaphragm/SOB

The End!
- Slides: 62