Respiratory Distress in Newborn Eko Sulistijono Siti Lintang

Respiratory Distress in Newborn Eko Sulistijono, Siti Lintang K Perinatology Division Pediatric Medical Faculty-Saiful Anwar Hospital

Respiratory Distress in Newborn • Normal infants/asphyxia with successful resuscitation – may have respiratory distress: • Infant’s respiratory rate more than 60 times/minute, may show one or more additional signs of respiratory problem • Infant’s respiratory rate less than 30 times/minute • Infant with central cyanosis (bluish at the tongue and lips) • Infant with apnea (breathing stops for more than 20 seconds)

Causes of Respiratory Distress • Pulmonary disorders: Pneumonia • Cardiologic disorders: Congenital Heart Disease, Myocardium dysfunction • Central nervous system disorders caused by: Asphyxia, Cerebral hemorrhage • Metabolic disorders: Hypoglycemia, Metabolic acidosis • Surgical diseases: Pneumothorax, Tracheoesophageal fistula, Diaphragmatic hernia • Others: Meconeum Aspiration Syndrome, Transient Tachypnea of the Newborn, Hyaline Membrane Disease

Causes of Respiratory Distress Based on Gestational Age • In Preterm Infants: – – Hyaline Membrane Disease Pneumonia Asphyxia Congenital Anomaly or Malformation • In Aterm Infants: – – – Meconeum Aspiration Syndrome Pneumonia Transient Tachypnea of the Newborn Acidosis Congenital Anomaly or Malformation

Diagnosis of Respiratory Distress History taking: • The Time of Respiratory Distress’s Manifestation • Gestational Age • Antenatal Steroid Therapy • Predisposition Factors: PROM (Premature Rupture of the Membrane), Fever in mothers before delivery • History of Asphyxia and Delivery with Intervention • History of Aspiration

Diagnosis of Respiratory Distress (Cont’d) Clinical Features of Respiratory Distress • Clinical Syndrome consisting of these following symptoms: – Infant’s respiratory rate more than 60 times/minute or infant’s respiratory rate less than 30 times/minute and may show one or more additional signs of respiratory problem as such: – Infant with cyanosis (blueness at the tongue and lips) – Chest wall retraction – Grunting – Infant with apnea (breathing stops for more than 20 seconds)

Clinical Classification of Respiratory Distress § § § Severe respiratory distress Moderate respiratory distress Mild respiratory distress
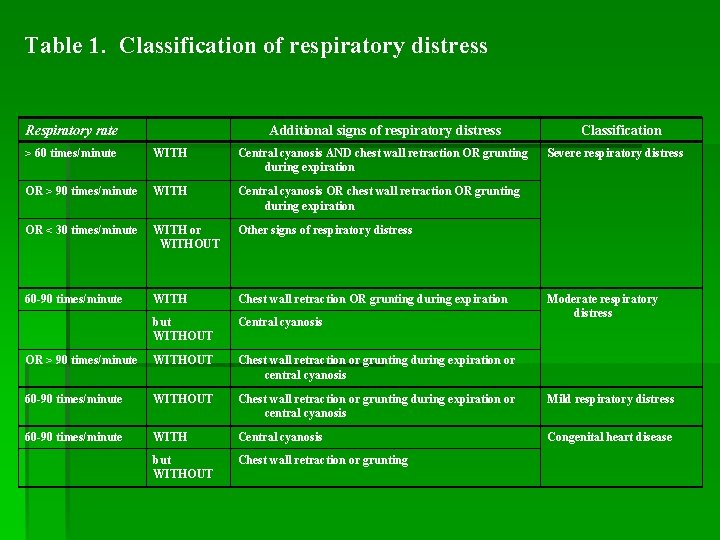
Table 1. Classification of respiratory distress Respiratory rate Additional signs of respiratory distress Classification > 60 times/minute WITH Central cyanosis AND chest wall retraction OR grunting during expiration Severe respiratory distress OR > 90 times/minute WITH Central cyanosis OR chest wall retraction OR grunting during expiration OR < 30 times/minute WITH or WITHOUT Other signs of respiratory distress 60 -90 times/minute WITH Chest wall retraction OR grunting during expiration but WITHOUT Central cyanosis OR > 90 times/minute WITHOUT Chest wall retraction or grunting during expiration or central cyanosis 60 -90 times/minute WITHOUT Chest wall retraction or grunting during expiration or central cyanosis Mild respiratory distress 60 -90 times/minute WITH Central cyanosis Congenital heart disease but WITHOUT Chest wall retraction or grunting Moderate respiratory distress

EVALUATION OF RESPIRATORY DISTRESS WITH DOWN SCORE 0 1 2 Respiratory rate < 60 x/minute 60 -80 x/minute > 80 x/minute Retraction No Mild Severe Cyanosis No Disappear with O 2 Cyanosis with O 2 Air Entry Positive Slightly decrease No Grunting No Audible with stethoscope Audible without tool Score < 4 Score 4 – 7 Score > 7 be taken) : No respiratory distress : Respiratory distress : Impending respiratory failure (Blood gas analysis must

Test Public health care is usually not provided with the facility to perform test, therefore: improving observation or clinical examination is the main concern § Laboratory testing: § Routine blood test and blood smear to diagnosis the possibility of infection or neonatal sepsis § Blood glucose level

General Management • • • Obtain intravenous line If the infant is not dehydrated, administer Dextrose 5% IV Monitor vital signs Maintain airway patency Give oxygen (2 -3 liter/minute with nasal catheter) If the infant has apnea: – Resuscitate according to the phase needed – Further evaluate • If seizure occurs, treat it • Immediately check blood glucose level (if the facility is available) • Administer adequate nutrition

Specific Or Advance Management • MODERATE RESPIRATORY DISTRESS: – Continue oxygenation 2 -3 liter/minute with nasal catheter, if dyspnea persist give O 2 4 -5 liter/minute with mask – Do not give fluid to the infant – Administer antibiotic (ampicillin and gentamicin) to treat sepsis possibility: • • • Axillary temperature < 340 C atau > 390 C Meconeal amniotic fluid History of intrauterine infection, suspect severe infection if fever is present or premature rupture of the membrane (>18 hours)

§ If axillary temperature is 34 – 36, 50 C or 37, 5 – 390 C, treat the temperature abnormality and reevaluate after 2 hours § If the temperature is still unstable or respiratory distress is not improving, administer antibiotic to treat sepsis possibility § If the temperature is normal, continue to observe infant. If the temperature becomes unstable again, repeat the steps above

• MILD RESPIRATORY DISTRESS: – Transient Tachypnea of the Newborn (TTN), • Especially after caesarian surgery, aterm infant • Usually this condition improves and is alleviated without treatment – Observe infant’s breathing every 2 hour for the next 6 hours – If during observation respiratory distress worsen or other sepsis symptoms appear, treat for sepsis possibility and manage the moderate respiratory distress and immediately refer to Referral Hospital – Give breast milk if infant could feed. If not, then give breast milk with one of the fluid administration alternatives

§ Reduce oxygenation periodically when respiratory distress improves. Stop oxygenation when respiratory rate is between 30 – 60 times/minute § Observe infant for the next 24 hours, when respiratory rate is stable between 30 – 60 times/minute, no sign of sepsis, and no other problem needing treatment, infant could be discharged

§ SEVERE RESPIRATORY DISTRESS: § Prepare to refer to Referral Hospital § Stabilize before referring § Refer with resuscitation-skilled personnel § Maintain airway and oxygenation during transportation

NEONATAL PNEUMONIA

Introduction Pneumonia § is an important cause of neonatal infection § Accounts morbidity and mortality aspecialy in developing country

Pathogenesis Routes of acquisition: Varies in part with the time of onset of pneumonia § Early – onset pneumonia § Late - onset pneumonia

§ Early – onset pneumonia § Generally within three days of birth § Aquired from the mother by one of three routes § Intra uteri aspiration of infected amniotic fluid § Transplacental tranmision of organisms from the mother to the fetus § Aspiration during or after birth of infected amniotic fluid or vaginal organisms

§ Late - onset pneumonia § Occures during hospitalization or after discharge § Nosocomial acquired from § Infected individuals § Contaminated equipment § Microorganisms can invide through § injury tracheal § bronchoia mucosa § bloodstream

Mechanisms of injury in GBS pneumonia § In GBS pneumonia, § the level of beta – hemolysin expression correlate directly with the abilility of the organism to injure of epithelial cell § Hemolysin act as pore forming cytolysis alveolar edema and hemorrhage § Surfactant phospholipid inhibits beta- hemolysisassociated lung epithelial cell injury premature infants more severelly affected

Pathology (The patologic changes very with type of organisms) Bacteria : § Inflammation of pleura § infiltration / distruction of brochopulmonary tissue § leukocyte and fibrious exudate within alveoli and bronchi/ bronchioles § Bacteria are seen within interstitial spaces, alveoli, bronci/bronchioles

§ Virus § Cause an interstitial pneumonia § Infiltration of mononuclear cell and lympocytes hyalin membrane formation - interstitial fibrosis and scarring
Microbiology Cause : § Bacterial § Viral § Spirochetal § Protozoan § Fungal pathogens

Early- onset pneumonia 1. Bacterial infections 1. 2. 3. 4. 5. 6. Escherichia coli Group B streptococcus Kleibsiella spp Staphylococcus aureus Streptococcus pneumonia Mycobacterium tuberculosis transplacentally 7. Listeria monocytogenes

2. Viral infections 1. 2. 3. 4. 5. 6. Herpes simplex virus ( HSV) Adenovirus Enteroviruses Mumps Rubella Cytomegalovirus 3. Fungal infections 1. Candida sp 4. Other patogens 1. Toxoplasma 2. Syphilis

Late – onset pneumonia 1. Bacterial infections 1. 2. 3. 4. 5. 6. 7. Staphylococcus Kleibsiella Escheichia coli Enterobacter cloacae Streptococcus pneumoniae Pseuodomonas aeroginosa Serratia marcescens

2. Viral infections 1. 2. 3. 4. 5. 6. Adenovirus Parainfluenza virus Rhinovirus Enteroviruses Influenza RSV 3. Fungal infections 1. Candida sp

Risk factors § Early – onset pneumonia § PRM > 18 hours § Maternal amnionitis § Premature delevery § Fetal tachycardia § Maternal intrapartum fever § Late – onset pneumonia § Assisted ventilation

§ Other factors § Anomaly of the airway (choanal atresia, tracheoesophageal fistule) § Severe underlying disease § Prolonge hospitalization § Neurologic empairment aspiration gastroentestinal contents § Poor hand washing § Overcrowding

Clinical manifestation Early- onset pneumonia § Respiratory distress beginning at / soon after birth § May have associated § § § Lethagy Apnea Tachycardia Poor perfusion Septic Shock § Other sign § § § Temperature instability Metabolic acidosis Abdominal distentions

Late – onset pneumonia § Respiratory distress § Apnea § Tachycardia § Poor feeding § Abdominal distention § Jaundice § Emesis § Circulatory collapse

Diagnosis § Sudden onset of respiratory distress or other sign of illness should be evaluated for pneumonia / sepsis § culture: Blood, cerebrospinal fluid, pleural fluid § Chest radiography Bilaterall alveolar densities + air bronchograms Irregular patchy infiltrates Normal pattern

Treatment § Early- onset pneumonia § Ampicillin + gentamycin § Cephalosphorin § Late - onset pneumonia § Vancomycin + aminoglycoside § viral infection § Acylovir

Outcome § Predicted § Severity disease § Gestational age § Underlying medical conditions § Infecting organism § Increased mortality : § preterm birth § chronic lung disease § immune deficiencies
- Slides: 36