Respiratory Diseases Pathophysiology and Medical Treatments Respiratory System












































- Slides: 47

Respiratory Diseases Pathophysiology and Medical Treatments

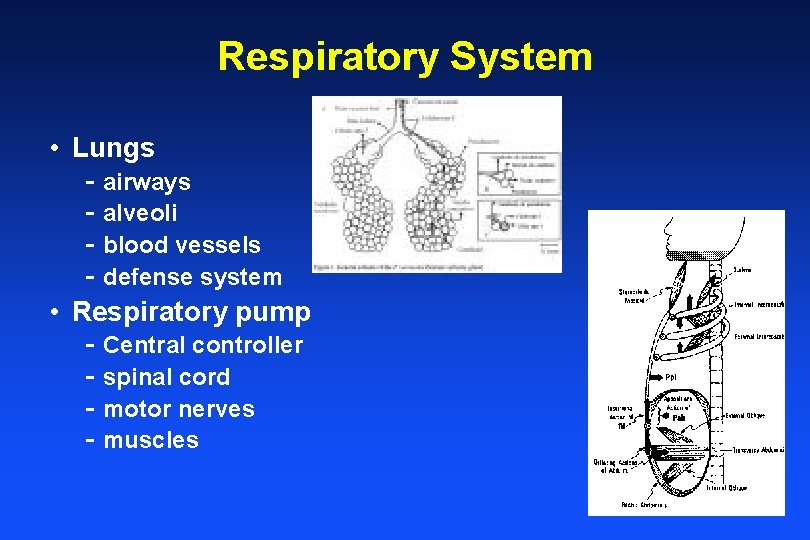
Respiratory System • Lungs - airways - alveoli - blood vessels - defense system • Respiratory pump - Central controller - spinal cord - motor nerves - muscles

Respiratory Diseases • Lungs - airways-asthma - alveoli-COPD, pulmonary fibrosis - blood vessels-pulmonary hypertension - defense system- inadequate cough, aspiration, immune dysfunction • Respiratory pump - Central controller-central alveolar hypoventilation - spinal cord- SCI - motor nerves- ALS - muscles- muscular dystrophy

Discussion Topics • Lung diseases - Asthma - COPD - Pulmonary fibrosis - Lung Transplant - Pneumonia • Respiratory Pump Diseases - Muscular Dystrophy - Spinal Cord Injury

Asthma • Defined as reversible obstruction or narrowing of the airways - between episodes patients feel normal and have normal pulmonary function tests • If you were to see the asthmatic airway under the microscope you would see: - narrowed, edematous airways - inflammation in the airway walls - excess mucous secretion and plugging

Asthmatic Airway

Asthma • Allergy Related (extrinsic) - Immunoglobulin E (Ig. E) - Pollens, and animal danders, etc. - Seasonal - Younger individuals • Unrelated to allergy (intrinsic) - Aspirin sensitivity - Not seasonal

Asthma- Symptoms • • • Shortness of breath (dyspnea) Wheezing Chest tightness “Feeling of suffocating” Cough Exercise induced

Asthma- Physical Findings • Rapid breathing (tachypnea) • Perspiring • Using “accessory” muscles of respiration - sternoclydomastoid, platysma, pectoralis major and minor • cyanosis • tachycardia • pulsus paradoxus

Asthma- Acute Treatment • Bronchodilation (opening the airways) - inhaled B-agonists (B 2 receptors bronchodilate) - • albuterol, salmeterol, pirbuterol, bronkosol parenteral B-agonists • epinephrine, terbutaline, isoproterenol inhaled anticholinergics (cholinergic receptors constrict) • ipatroprium bromide, glycopyrrolate Theophylline

Asthma Treatment-Acute • Anti-inflammatory - parenteral steroids • Artificial ventilation - Noninvasive-facemask - Invasive-endotracheal tube • High risk

Asthma - Chronic. Treatment • anti-inflammatories are key to prevent exacerbations - inhaled steroids at high dose - • triamcinalone, budesonide, fluticasone, beclomethasone mast cell stabilizing drugs • nedocromil, cromolyn • B-agonists and anticholinergics as needed • Leukotriene inhibitors - zafirleukast (zyflo) - Montelukast (singulair_ • “Stepped care” - Gradual addition of medications

Chronic Obstructive Pulmonary Disease (COPD) • Is a general term for patients with chronic airflow obstruction that may be due a number of causes - emphysema - chronic bronchitis - chronic severe asthma • > 90% of cases are due to smoking • Lungs are obstructed and overinflated

Physiologic Derangements in COPD • Destruction of Alveolar Tissue • Loss of lung elastic recoil • Airway obstruction

Chronic Obstructive Pulmonary Disease (COPD) • Functional consequences of airway disease and chronic lung injury - Obstruction to airflow - Hyperinflation of the chest - Improper respiratory muscle function - Increase work of breathing

COPD- Symptoms • gradually progressive shortness of breath (over years) - may end up disabled with dyspnea at rest - may require oxygen • cough frequently productive of sputum • leg swelling • anxiety

COPD- Physical Signs • • • Barrel chest Tachypnea “Pursed-lip” breathing Use of accessory muscles Diaphragm dysfunction - Hoover sign - lack of outward movement of abdomen • Reduced and prolonged expiratory airflow


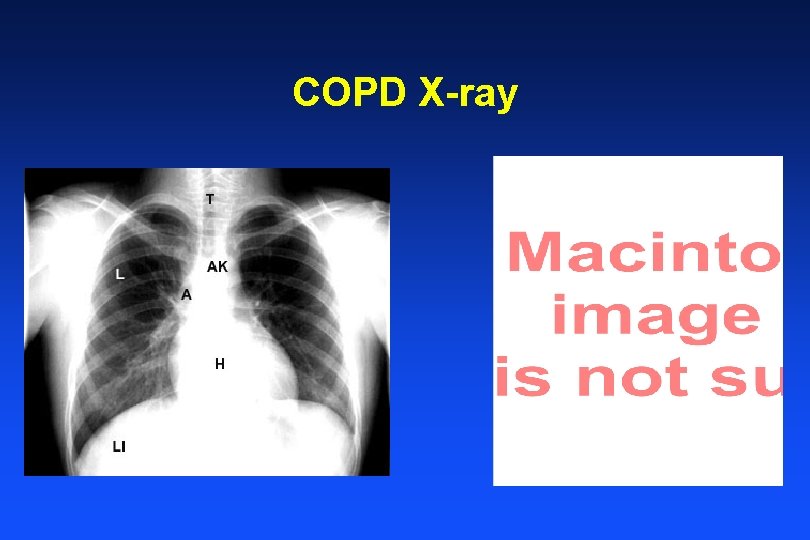
COPD X-ray

COPD- Treatment • • B-agonists Anticholinergics Theophylline Steroids - only 20 % of patients are steroid responsive

COPD Treatment • Pulmonary Rehabilitation • Lung Transplant • Lung Volume Reduction Surgery (LVRS)

Pulmonary Rehabilitation Exercise

Pulmonary Rehabilitation Breathing Re-training

Pulmonary Rehabilitation Teaching • • • Biology of disease Medications Oxygen Travel Minimizing energy expenditure Interpersonal relationships

Break

COPD-Surgical interventions • Lung volume reduction surgery (LVRS) • Lung transplantation

LVRS • Hypothesis: Hyperinflation of the lungs in COPD is the primary cause of dyspnea. Reducing the sized of the lungs will reduce dyspnea and increase expiratory airflow • Procedure: Sternotomy with resection of 25 to 30% of each lung

Lung Volume Reduction Surgery

Lung Transplantation • • For very advanced disease Age < 65 years No other major medical problems Post transplant immunosupression - 15 -20 medications

Pulmonary Fibrosis • Scarring of the lung tissue due to inflammation • Lungs become too small- “restricted” • Due to a wide range of causes: - drugs - toxic exposures - rheumatologic diseases - idiopathic- “IPF”

Interstitial Lung Disease

Pulmonary Fibrosis. Symptoms • • Dyspnea Exercise intolerance Cough Symptoms associated with systemic disease

Pulmonary Fibrosis- Exam Findings • • • Rapid, shallow breathing clubbing of the fingers “velcro” rales or crackles in the lungs cyanosis findings associated with systemic disease

Pulmonary Fibrosis. Treatment • Steroids • Cytotoxic agents - imuran - cyclophosphamide • Lung Transplant

Pneumonia • Common pulmonary disease • Usually there is an associated host defense problem - aspiration - foreign body - immune suppression - • recent viral illness • More global immune problem Ciliary problem • smoking • Cystic Fibrosis

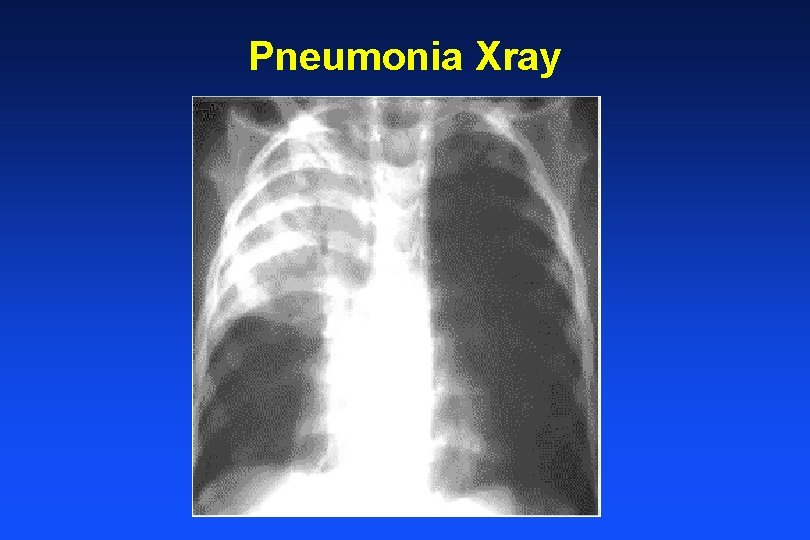
Pneumonia Xray

Pneumonia- Symptoms and Physical Findings • • • Cough Chest pain Fever, chills Dyspnea Evidence of consolidation on lung exam - “bronchial breath sounds” - egophony - dullness to percussion

Pneumonia- Treatment • One or more antibiotics • Choice will depend on patients age, immune status, seriousness of clinical condition • Sputum sample with Gram’s stain can be helpful

Spinal Cord Injury • Level of spinal cord injury is critical • C 2 or above clearly ventilator dependent • C 3 -C 5 - likely ventilator dependent at least partially • C 5 and below usually ventilator independent but cough and secretion clearance is a problem • Lung volumes appear “restricted” • Cough and expiratory flow always an issue

Spinal Cord Injury. Respiratory Treatment • Will depend entirely on level of injury • Maintaining adequate ventilation is of utmost importance, almost all patients will initially be on a mechanical ventilator • Clearance of secretions and prevention of pneumonia is also of critical importance - The leading cause of death in the first year following injury is pneumonia • Techniques of Secretion Management - Chest physical therapy, assisted cough - Tracheal suctioning - In-exsufflator

Spinal Cord Injury. Respiratory Treatment • Some patients may need only partial ventilation at night • Non-invasive ventilation may be an option - No tracheostomy - Less complications

Muscular Dystophy • Many varieties - Frequently genetic • • Muscle and not nerves are affected Progressive loss of function over years Primary cause of death is pneumonia Currently no medical treatment - Future: ? Gene therapy

Muscular Dystrophy • Often associated with scoliosis • Patients will be short of breath • Patients will often breath less well at night and have associated sleep apnea • Treatment will be aimed at relieving symptoms and prolonging life • Noninvasive ventilation is a definite option

Mouthpiece Ventilation”SIP”

Nocturnal Ventilation

Cough-Assist Device

Noninvasive Ventilation