Respiratory disease Liu lin xiang Radiology school 6222136







































- Slides: 92

Respiratory disease Liu lin xiang, Radiology school, 6222136 lxliu@tsmc. edu. cn 1

Bronchiectasis Ø Chronic irreversible dilatation of bronchi Ø Major cause of morbidity in less developed countries Ø Causes: Ø Postinfectious Ø Mechanical obstruction Ø Congenital Ø Granulomas and fibrosis 2

Bronchiectasis: Clinical features w Large volumes of purulent sputum w Finger clubbing w Frequent infective exacerbation w Recurrent hemoptysis w Mild bronchiectasis: few physical signs 3

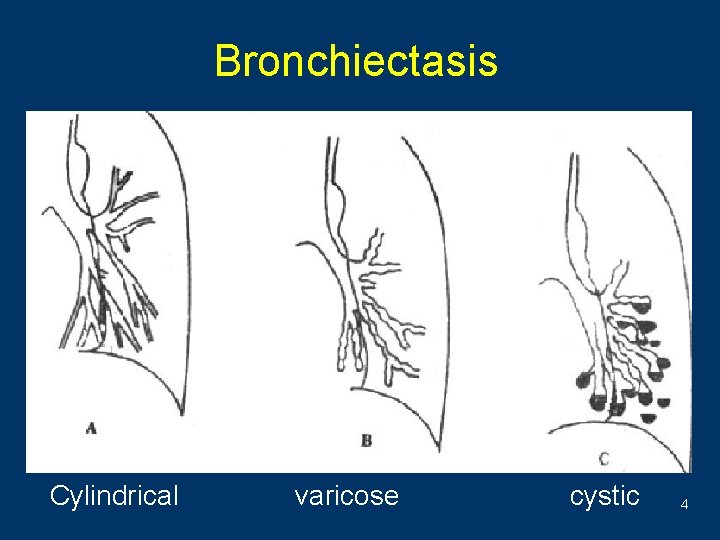
Bronchiectasis Cylindrical varicose cystic 4

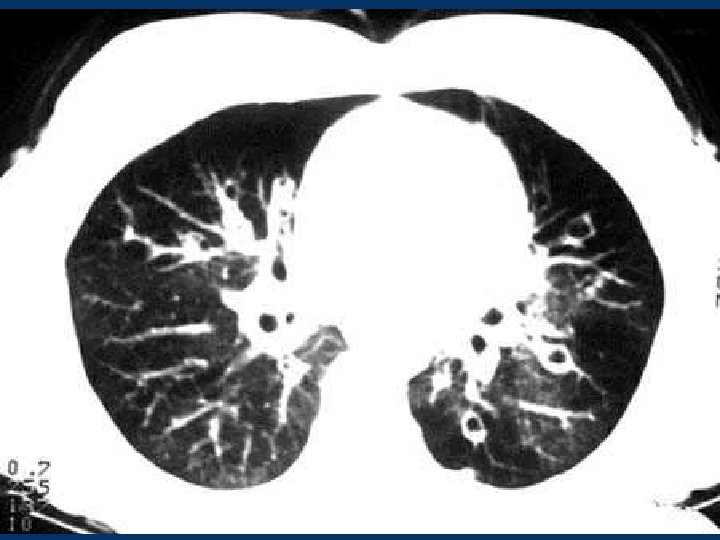
Radiological findings l Margins of pulmonary vessels indistinct l Tramlines, ill-defined ring opacities l Filled with pus and mucus lead to tubular and ovoid opacities l Cystic: multiple thin-walled ring opacities and contain fluid levels l Coarse honeycombing pattern l Patchy peribronchial consolidation and focal areas of subsegmental collapse in diffuse disease l Affected lobe overinflated or relatively collapsed 5

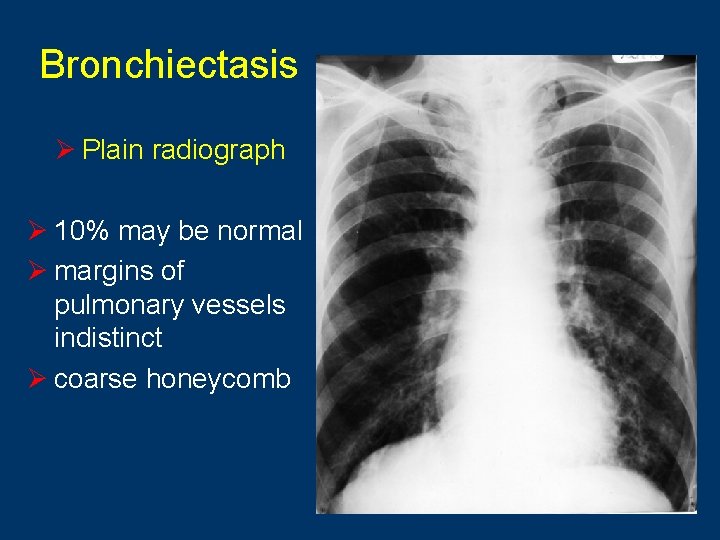
Bronchiectasis Ø Plain radiograph Ø 10% may be normal Ø margins of pulmonary vessels indistinct Ø coarse honeycomb 6

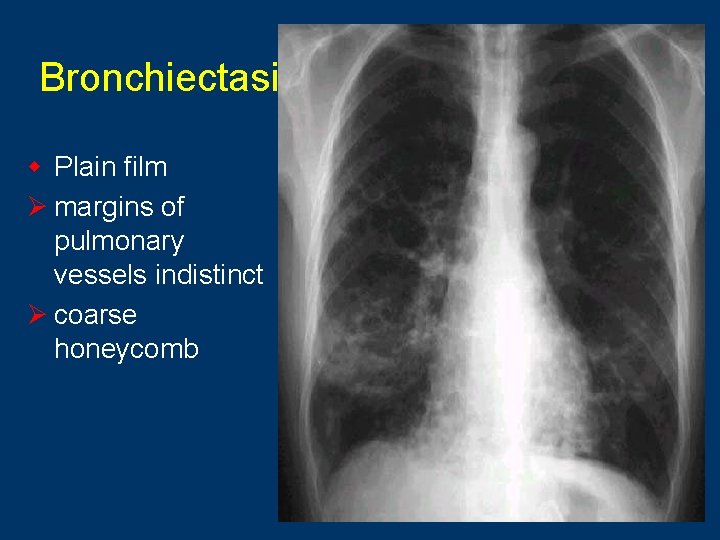
Bronchiectasis w Plain film Ø margins of pulmonary vessels indistinct Ø coarse honeycomb 7

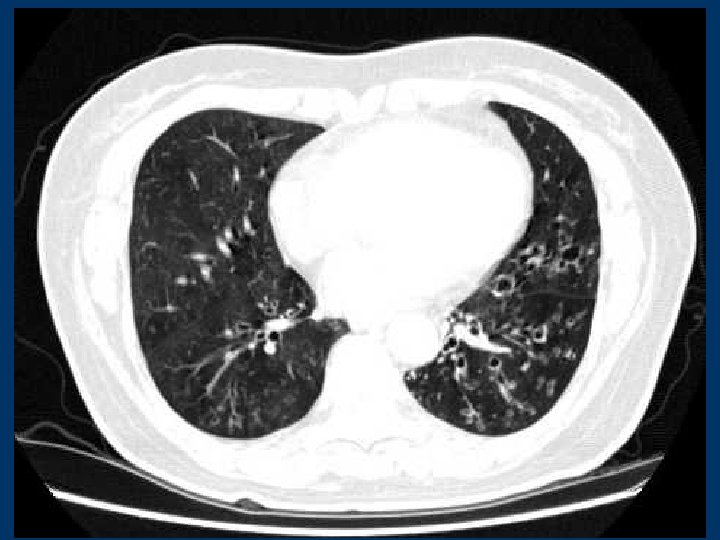
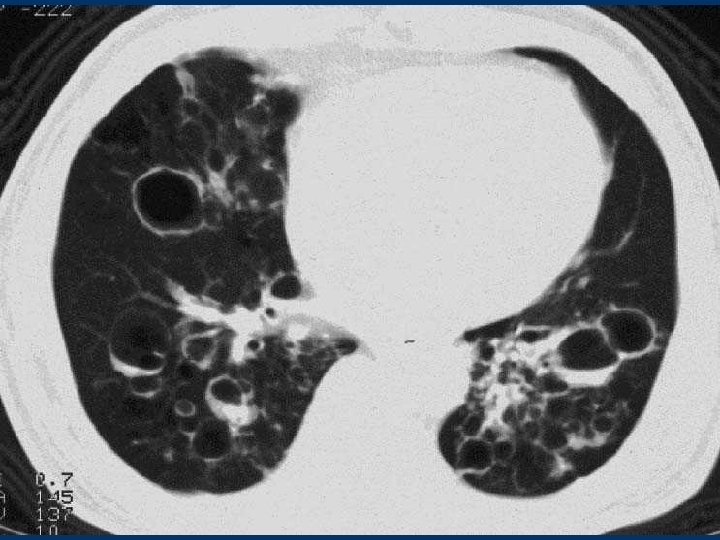
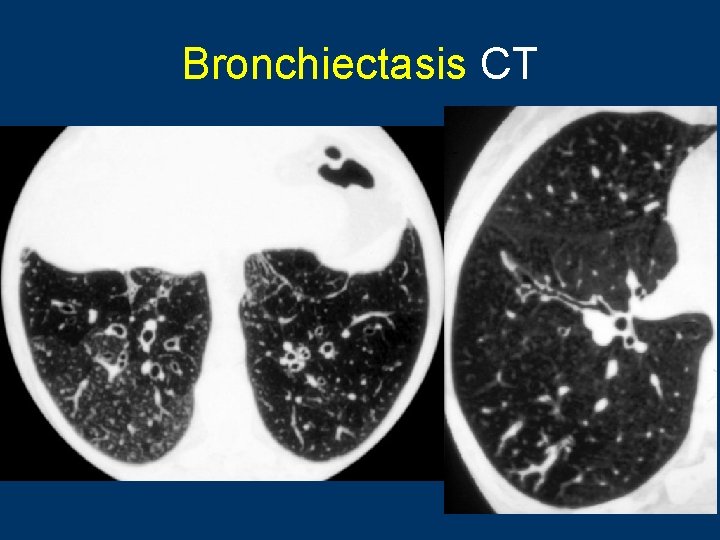
Bronchiectasis CT , Dilatation of bronchi wo bronchial wall thickening , Bronchial dilatation in isolate cystic spaces grouped along a fissure or mediastinal pleura , Volume loss of lung associated crowding of mildly dilated airways and displaced fissure , Accumulation of secretions easily recognizable as lobulated glove-finger, V or Y densities , Bronchiolitis may present in the same areas 8

Bronchiectasis CT w Cylindrical: smooth dilatation of the affected bronchi, not taper normally towards the periphery, but no actual loss of bronchi w Varicose: irregularity and beading of the affected bronchi. destruction and loss of the bronchial lumen peripherally w Saccular: increasing dilatation of bronchi towards the periphery, with ballooning, and a loss of bronchial subdivisions 9

Bronchiectasis CT w Define the extent, severity and location w Thick-walled dilated bronchi, with a diameter greater w w w than their accompanying pulmonary artery In cross-section, ring-shaped, "signet ring" In long axis, bronchi look like tramlines Associated: air-fluid levels in dilated bronchi, cystic spaces, and occasional ectatic beaded bronchi Bronchi visible in peripheral half of lung Focal volume loss, hyperlucency or oligaemia 10

11

12

13

Bronchiectasis CT 14

Bronchiectasis 15

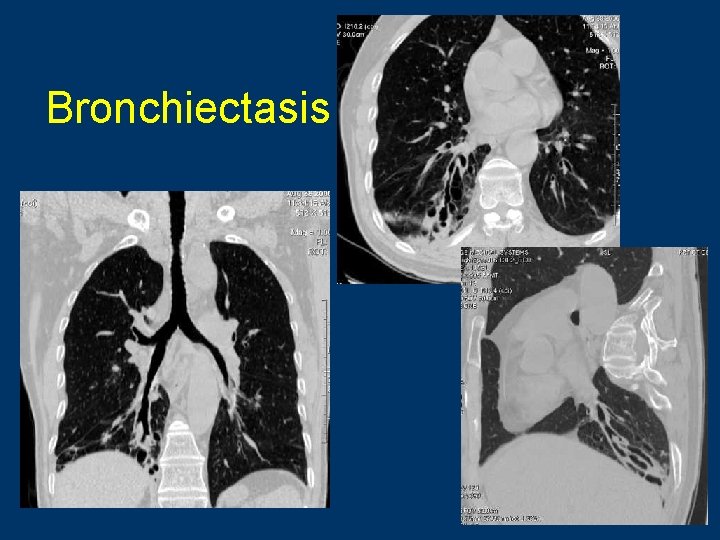
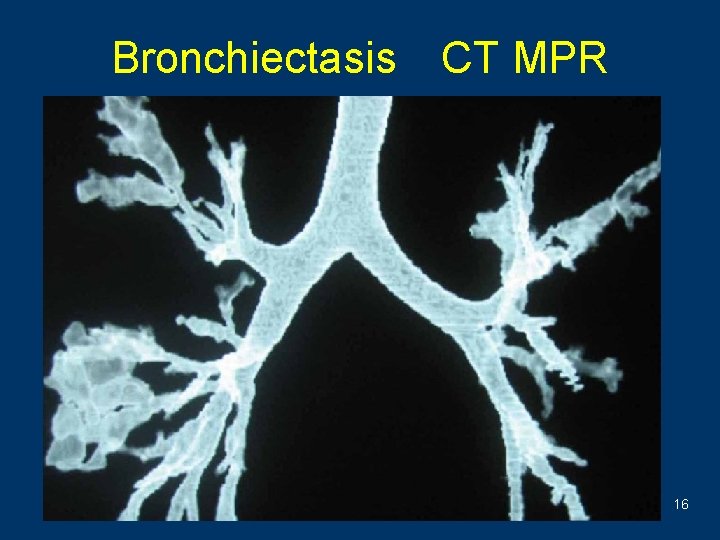
Bronchiectasis CT MPR 16

Lobar pneumonia ¦ Result of alveolar wall injury with severe hemorrhagic edema induced by inhaled infectious organisms that reach the subpleural zone of the lung ¦ Rapid multiplication of organisms and invasion of the infected edematous fluid by polynuclear leukocytes ¦ Spreads rapidly through the pores of Kohn leading to a consolidation of an entire lobe or segment ¦ The most common causes are streptococcus pneumonia, klebsiella pneumonial infection, legionella infection and mycoplasma pneumonia infection 17

Radiological findings l Air space consolidation involving an entire lobe containing air bronchograms l Because of antibiotics, the pneumonia is limited to one or more segments within a lobe l Sometimes, voluminous edema may result in expansion of the lobe recognized radiographically by bulging of the fissures l Necrosis and cavitation represent the potential complication of lobar pneumonia 18

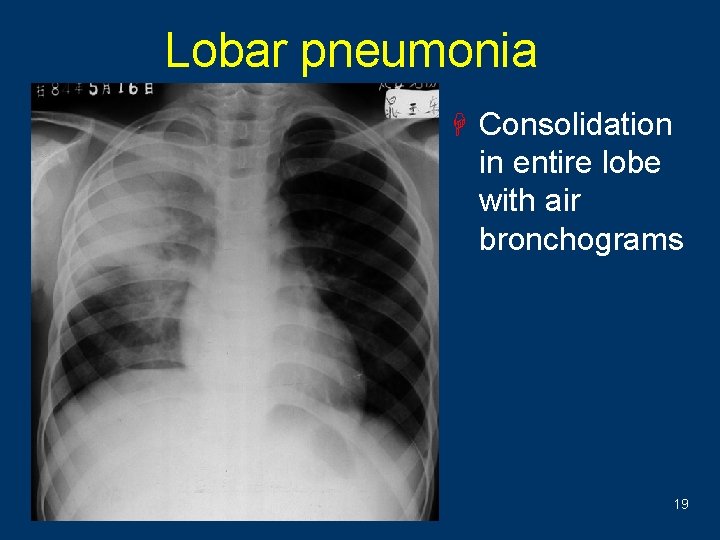
Lobar pneumonia H Consolidation in entire lobe with air bronchograms 19

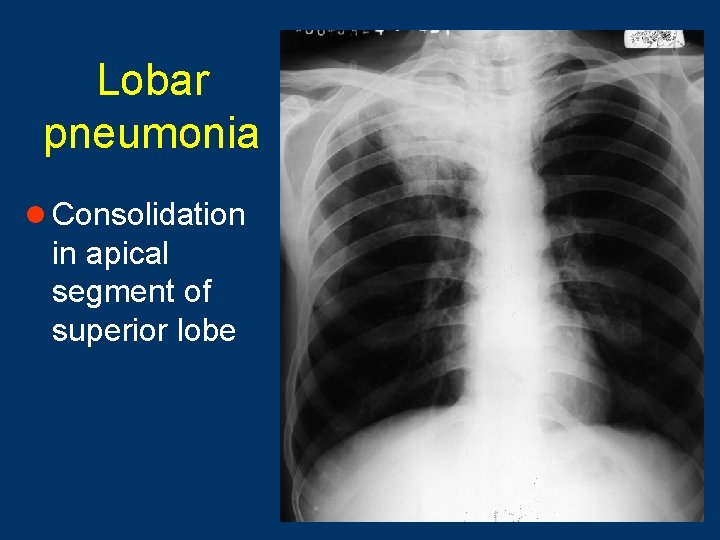
Lobar pneumonia l Consolidation in apical segment of superior lobe 20

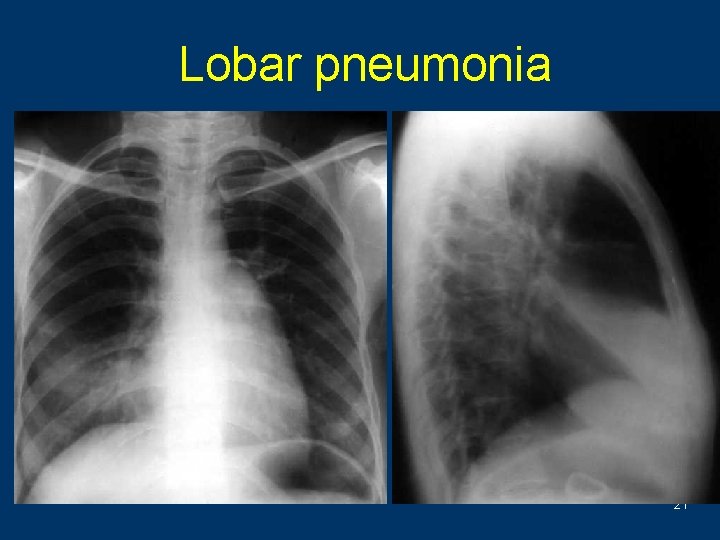
Lobar pneumonia 21

Lung abscess w Certain virulent bacteria create focal areas of necrosis or lung abscess w Abscess may not be recognized on chest films because of surrounding lung consolidation or no communication with a conducting airway and thus no cavitation is appreciated w Abscess formation is most likely with anerobic and Gramnegative bacteria w Lung abscess may occur because of inflammatory necrosis of otherwise normal lung or occasionally secondary to vascular involvement leading to ischemic necrosis and death of lung 22

Lung abscess w Radiographically, a lung abscess may be difficult to appreciate secondary to surrounding lung consolidation w but will be recognized when air enters the abscess cavity creating either a large single abscess or multiple smaller microabscesses w With the larger abscess cavities the inner walls are thick and irregular 23

Lung abscess w Resolution of an abscess is recognized when abscess cavity decreases in size or amount of fluid within an abscess fluctuates w This is not related to healing necessarily but instead to ease of communication between abscess cavity and a conducting airway w Fluid levels will rise in cavity if exit is blocked and will fall if opening remains patent 24

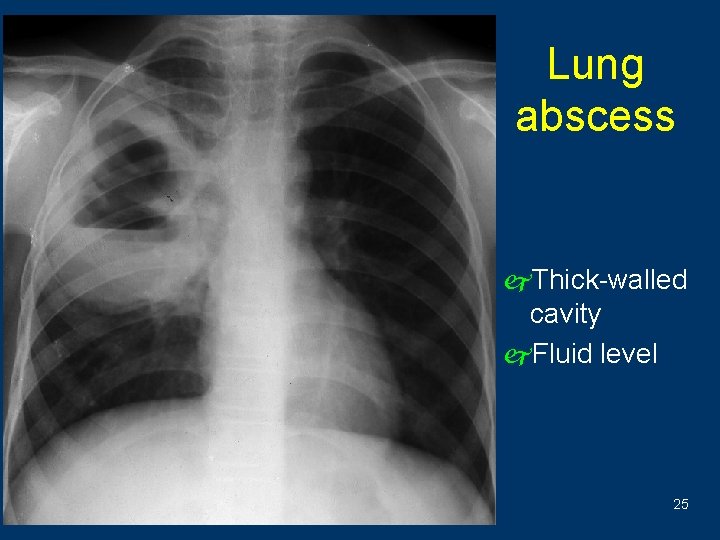
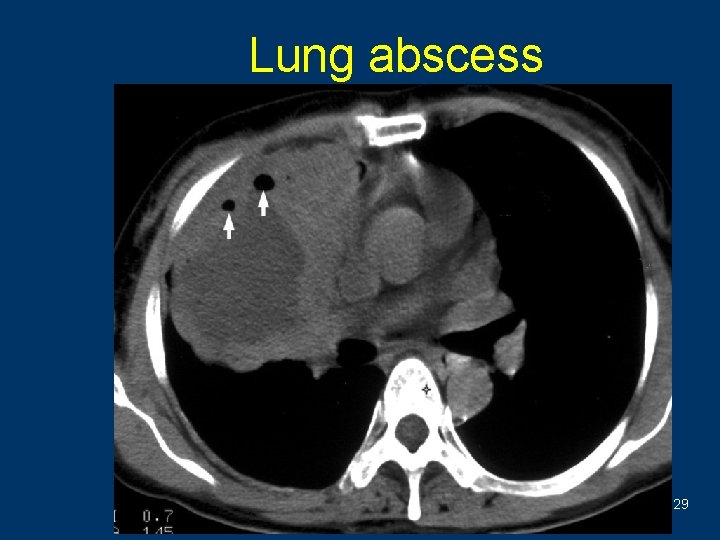
Lung abscess j. Thick-walled cavity j. Fluid level 25

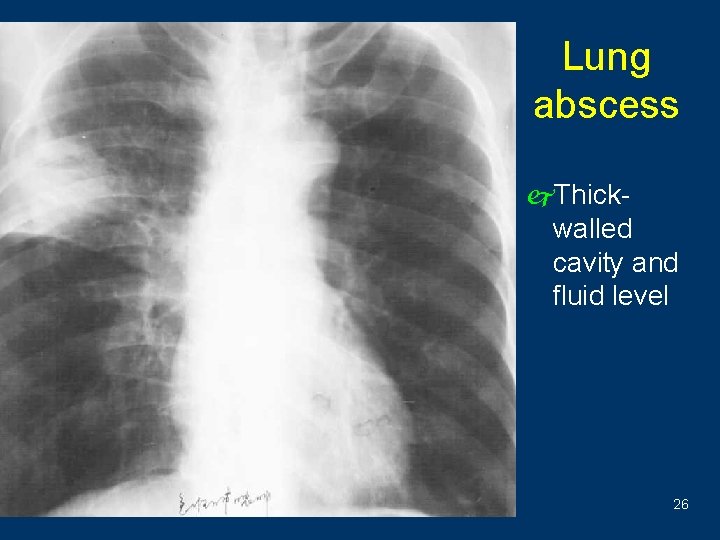
Lung abscess j. Thickwalled cavity and fluid level 26

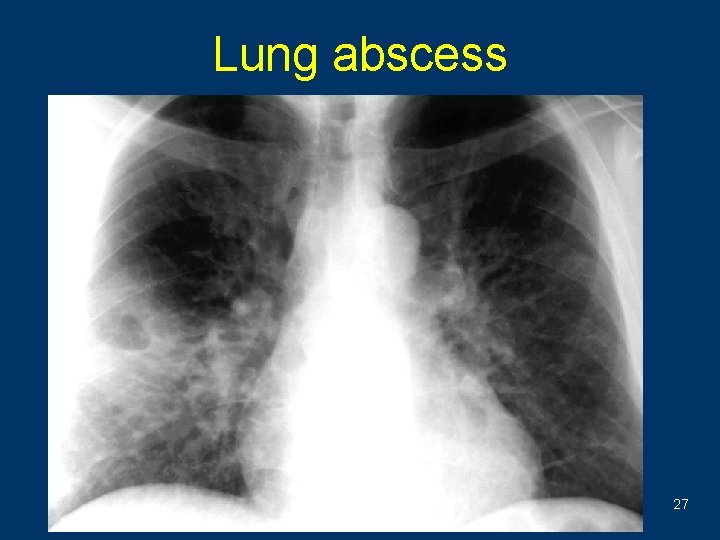
Lung abscess 27

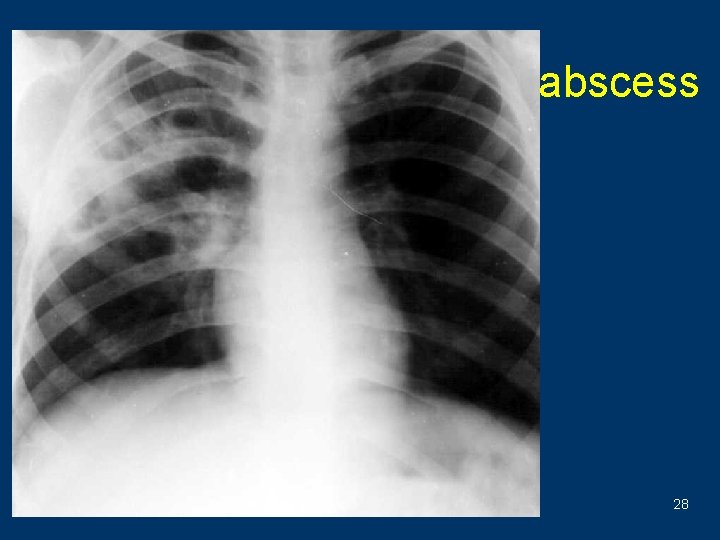
abscess 28

Lung abscess 29

Pulmonary tuberculosis l Infection by Mycobacterium tuberculosis bacillus by respiratory inhalation, with the organism multiplying in the alveolar walls l Primary tuberculosis represents the development of a positive reaction to tubercle bacilli following the first exposure l Often subclinical, but in infants or those with impaired defence due to poor nutrition or underlying illness, may be present clinically 30

Pulmonary tuberculosis w As the immune system develops a positive reaction to the bacillus, the multiplication of the organism is halted w Localized inflammatory response in the lung parenchyma and the draining lymph nodes w Central necrosis within this area, later heals by fibrosis and calcification 31

Pulmonary tuberculosis w If response is delayed, organisms may spread from draining lymph nodes into regional nodes and, via thoracic duct into circulation to pass by hematogenous spread throughout the body. This can also give rise to tuberculous meningitis and miliary tuberculosis w Bronchogenic spread of tuberculosis occurs following poor containment of the original infection, with pulmonary consolidation w Spread can occur as infected material expectorated and enters other non-affected bronchi 32

Primary tuberculosis w Reaction to the tubercle bacillus following first w w exposure to the organism, typically by inhalation presence of primary tuberculosis in childhood varies from subclinical to overwhelming and lifethreatening In healthy child, should be a self-limiting condition, lasting at most a few weeks. If there are clinical symptoms there is fever, loss of appetite, general malaise and, possibly, a skin rash Inspired bacilli lodge on the alveolar walls and multiply. A localized, mainly histiocytic, inflammatory reaction is set up Draining lymph nodes may enlarge as part of this sensitivity reaction 33

Primary tuberculosis w Usually, the immune response is sufficient to contain the initial infection, which heals as a small granuloma. The granuloma may show associated lymph node calcification. There may be central necrosis within this area, which later heals by fibrosis and calcification, which may take 6 months or more to appear w In infants, this process may not be adequate and pulmonary consolidation may occur as part of the primary infection. Bronchogenic spread may then cause widespread pulmonary infection, while hematogenous spread may cause a miliary pattern of pulmonary infection. Once it is in the circulation, the child is at risk from hepatic and meningeal infection. This bacteremia is also the source of miliary tuberculosis 34

Primary tuberculosis w Radiography of the chest in primary tuberculosis varies from a small subpleural exudative reaction, wo unilateral hilar lymphadenopathy, to more extensive disease such as multifocal pneumonic change or a diffuse interstitial nodularity w Enlarged lymph nodes cause distal atelectasis w Pleural effusion is not an unusual feature w Lung changes take months or years to clear, and any calcified lesions persist indefinitely 35

Primary tuberculosis w In children without tuberculous consolidation, the radiographic changes represent the development of the immune reaction to the infection w Main reason for regular radiography is to allow early diagnosis of miliary tuberculosis, which may be visible before there is any clinical suspicion w As this is a manifestation of hematogenous spread, meningitis is also a very likely complication w Radiographic changes in uncomplicated primary tuberculosis are not visible until after the immune response has developed, so skin testing is a more sensitive method of diagnosis 36

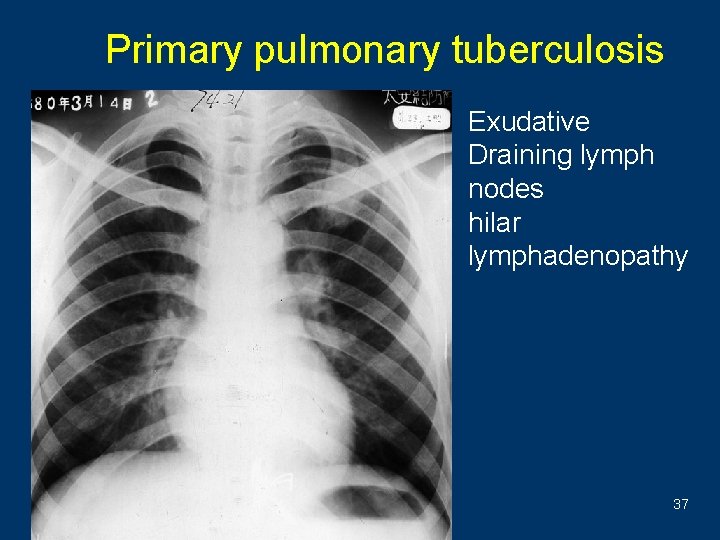
Primary pulmonary tuberculosis • Exudative • Draining lymph nodes • hilar lymphadenopathy 37

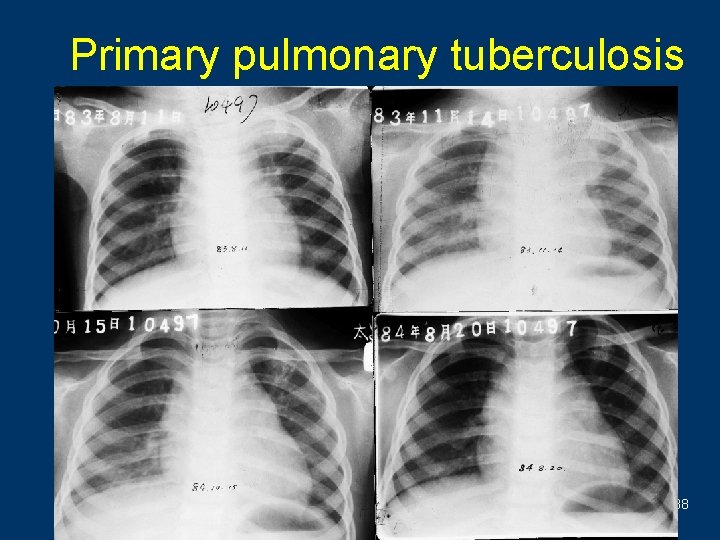
Primary pulmonary tuberculosis 38

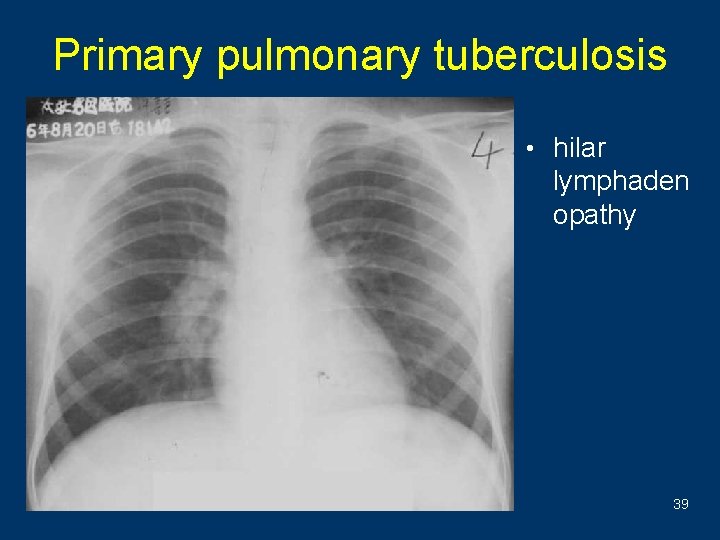
Primary pulmonary tuberculosis • hilar lymphaden opathy 39

Miliary tuberculosis w Clinical presentation is variable, with infants being relatively asymptomatic w Seen some time following a bacteraemia w Usually occurs during the incubation period, when the tubercle bacilli are deposited throughout the lungs w Patients are generally very ill with respiratory failure, fever and malaise at the time of diagnosis 40

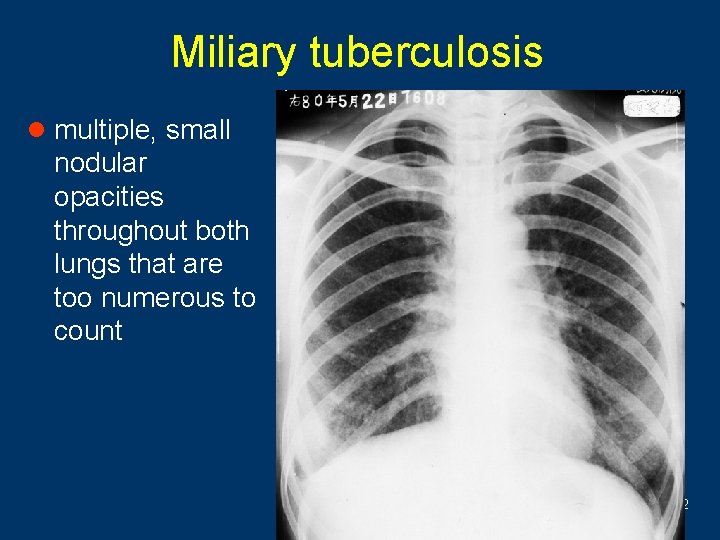
Miliary tuberculosis w Chest film demonstrates multiple, small nodular w w opacities throughout both lungs that are too numerous to count Untreated disease results in steady enlargement of these nodules until death of the patient ensues Lymphadenopathy and pleural fluid or other evidence of primary tuberculosis may not be present on chest film Diagnosis may require transbronchial biopsy to identify acid-fast bacilli When treated the miliary pattern gradually disappears leaving a normal chest film within several weeks to months 41

Miliary tuberculosis l multiple, small nodular opacities throughout both lungs that are too numerous to count 42

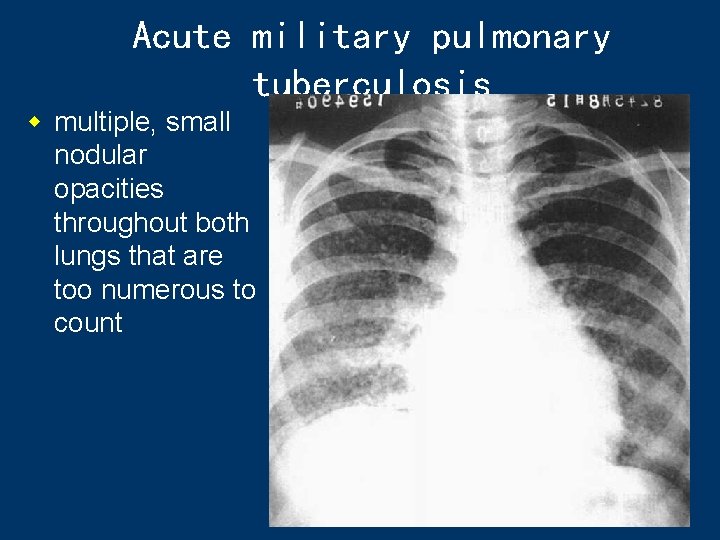
Acute military pulmonary tuberculosis w multiple, small nodular opacities throughout both lungs that are too numerous to count 43

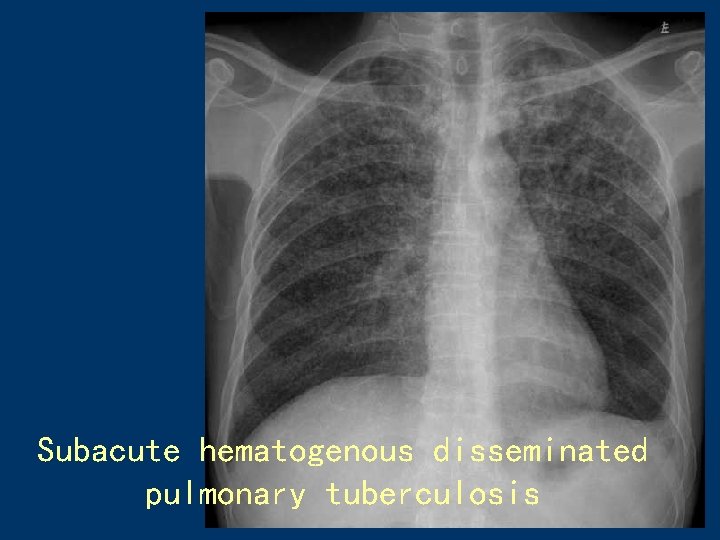
Subacute hematogenous disseminated pulmonary tuberculosis 44

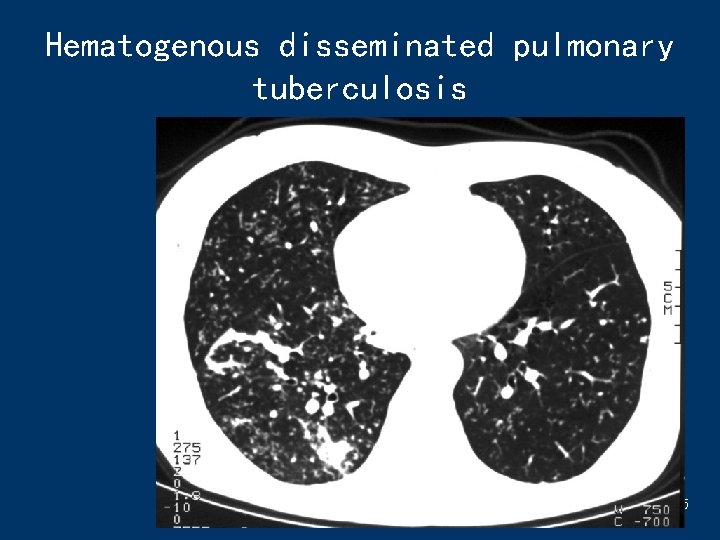
Hematogenous disseminated pulmonary tuberculosis 45

Lung cancer w Also called bronchogenic carcinoma w The most common fatal malignant neoplasm in men and it has now surpassed breast cancer as the leading cause of cancer death in women w The risk of lung cancer occurrence is related to the number of cigarettes smoked, the number of smoking years, the age at which smoking began, and the depth of inhalation w The risk decreases with cessation of smoking but never completely disappears 46

Lung cancer w Most patients with lung cancer present with clinical symptoms, and only a minority are asymptomatic w Patients with central tumors obstructing a major bronchus may present with cough, wheezing, hemoptysis and lung infection w Local intrathoracic spread result in left laryngeal nerve paralysis, pleural or chest wall pain, symptoms related to SVC obstruction or Pancoasts neoplasm w Sometimes symptoms resulting from distant metastases may reveal the lung cancer 47

Lung cancer w A large variety of paraneoplastic syndromes may also be associated with lung cancer w Include skeletal abnormalities such as clubbing, hypertrophic pulmonary osteoarthropathy and osteomalacia or endocrine and metabolic disorders such as Cushing's syndrome from adenocorticotrophic hormone production, hyponatraemia associated with inappropriate antidiuretic hormone syndrome production, and insulin-like activity 48

Histological type w The common types include adenocarcinoma, squamous cell carcinoma, small cell carcinoma and large cell undifferentiated carcinoma w Multidifferentiated carcinomas may also occur (adenosquamous carcinoma) w Giant cell carcinoma is a subset of large-cell undifferentiated carcinoma w Bronchioalveolar cell carcinomatosis is a subset of adenocarcinoma 49

Squamous cell carcinoma w A frequent type representing about one third of all lung cancers, associating with smoking w Pathologically, often arise in squamous metaplasia commonly seen in the bronchial mucosa of cigarette smokers w Centrally located involving the proximal bronchi and growth is mainly endobronchial w Extension through the bronchial walls and along the bronchial mucosa 50

Squamous cell carcinoma w Central necrosis is a frequent feature w Involvement of regional lymph nodes is common, occurring by direct extension or by means of lymphatic metastases w Grow rapidly, but distant metastases occur relatively late w Associated with the best prognosis 51

Squamous cell carcinoma w May associated with hypercalcaemia due to ectopic parathormone production w Most common cause of Pancoast neoplasm w Radiological features vary with location of tumor w Central and endobronchial produce a hilar or perihilar mass. Atelectasis or obstructive pneomonitis present distal to bronchial obstruction w When small, bronchial wall abnormalities can be missed on standard radiography but are well depicted on CT 52

Squamous cell carcinoma w When the tumor is more peripheral (one third of cases) it manifests characteristically as a thick-walled cavitary mass with or without an airfluid level w Such a lesion may be indistinguishable radiographically from primary lung w A solitary pulmonary nodule or mass is also a possible radiological manifestation 53

Lung cancer Macro-pathology X Central type: main bronchus, lober bronchiel and segmental bronchiel X Peripheral type: from segmental bronchiel to terminal bronchiole X Alveolar type: bronchioalveole 54

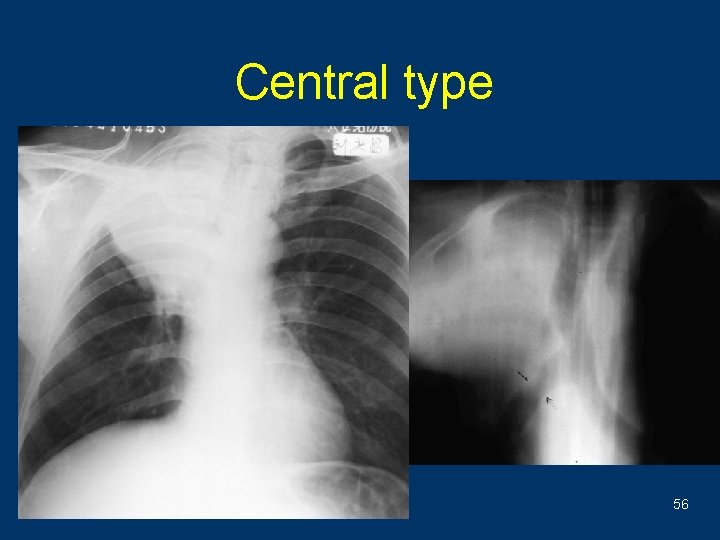
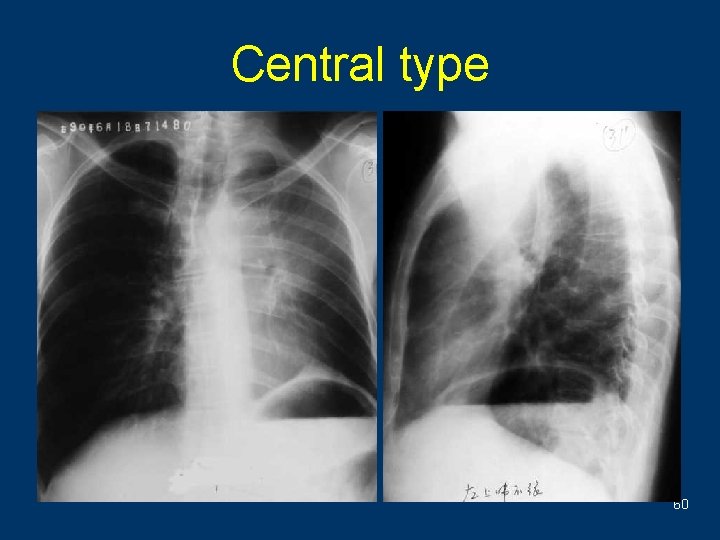
Central type w Direct signs ªhilar or perihilar mass ªNerrow or obstruction of bronchiel w Indirect signs ªAtelectasis ªObstructive pneomonitis 55

Central type 56

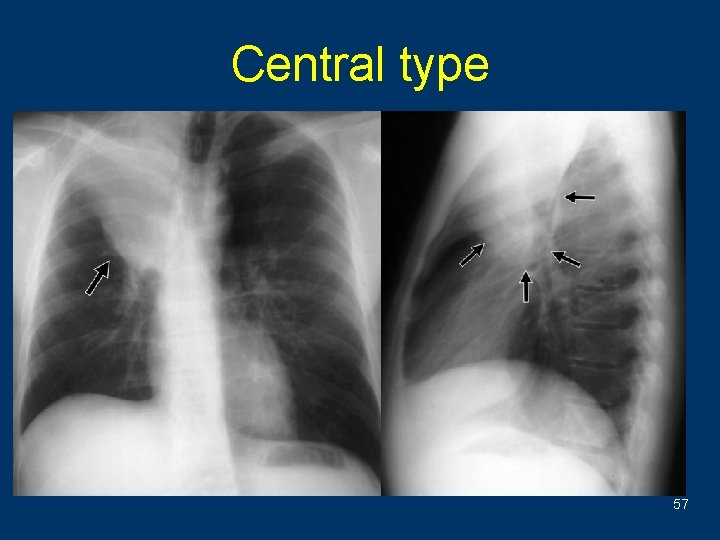
Central type 57

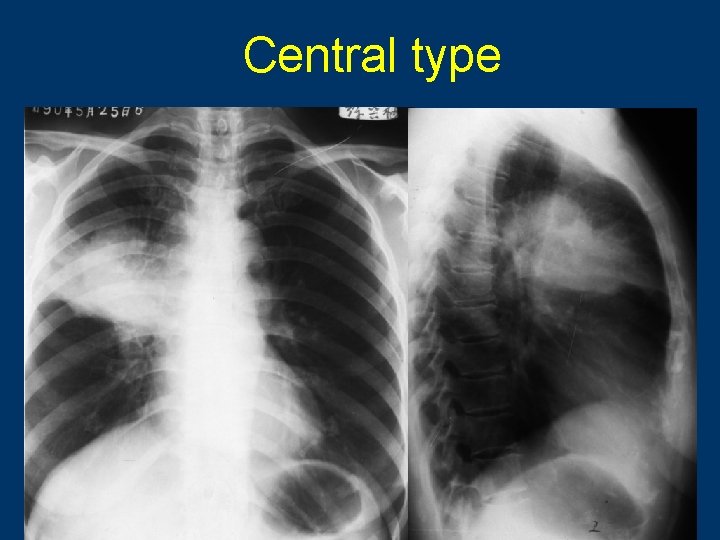
Central type 58

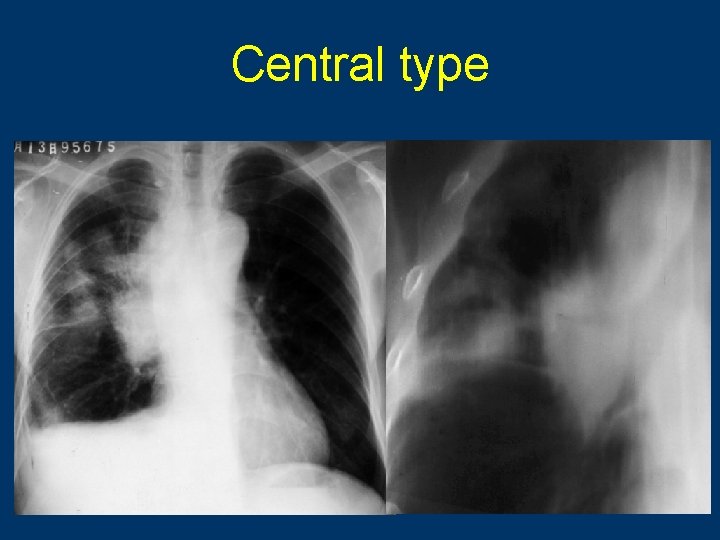
Central type 59

Central type 60

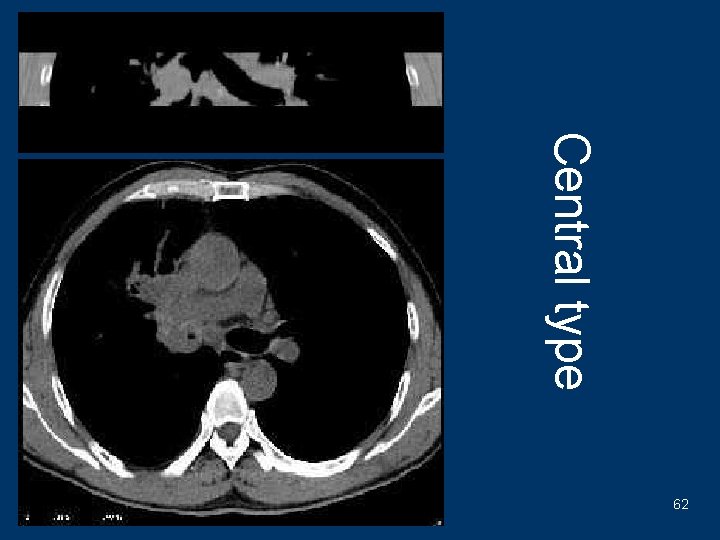
Central type--CT findings l Bronchial wall thick l Endobronchial nodules l Extrabronchial mass l Bronchial Obstruction l Atelectasis l Obstructive pneomonitis l Hilar and mediastinal metastasis l Remote metastasis 61

Central type 62

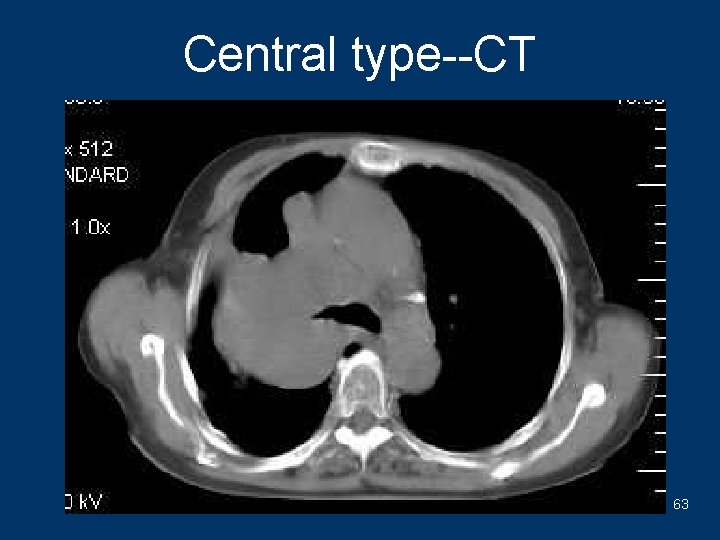
Central type--CT 63

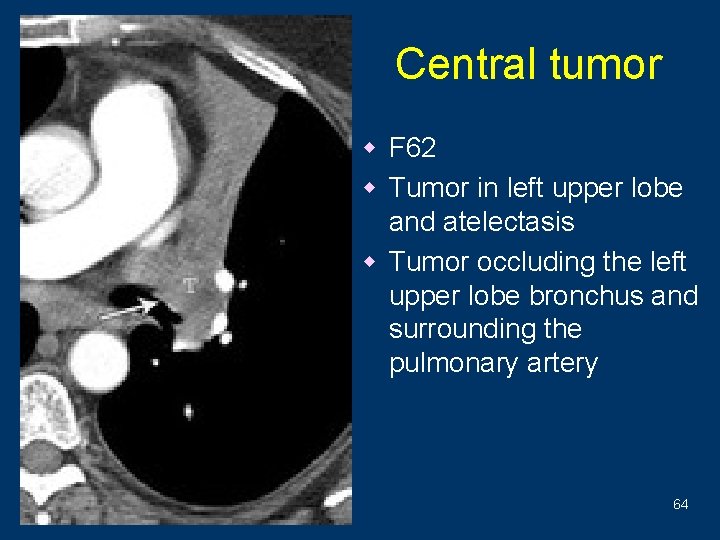
Central tumor w F 62 w Tumor in left upper lobe and atelectasis w Tumor occluding the left upper lobe bronchus and surrounding the pulmonary artery 64

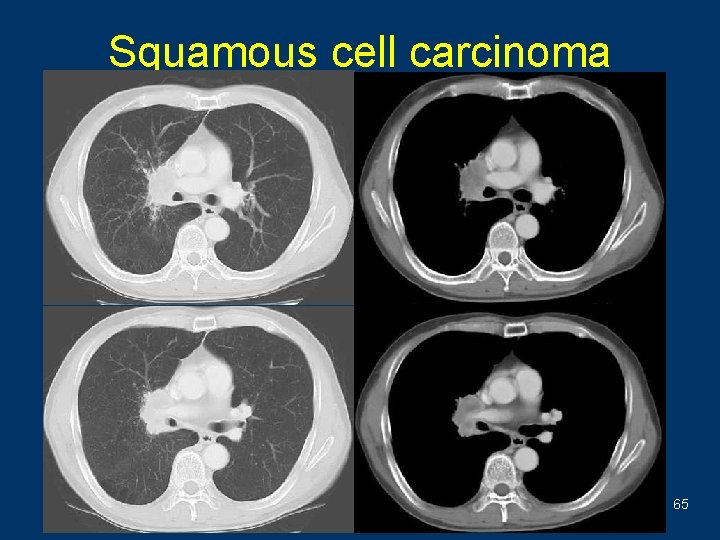
Squamous cell carcinoma 65

Peripheral type l Asymptomatic l Nodule and mass l Solitary pulmonary nodule l Spiculated appearance l Air bronchograms within a nodule l Cavitation with thick wall l Pleural indentation 66

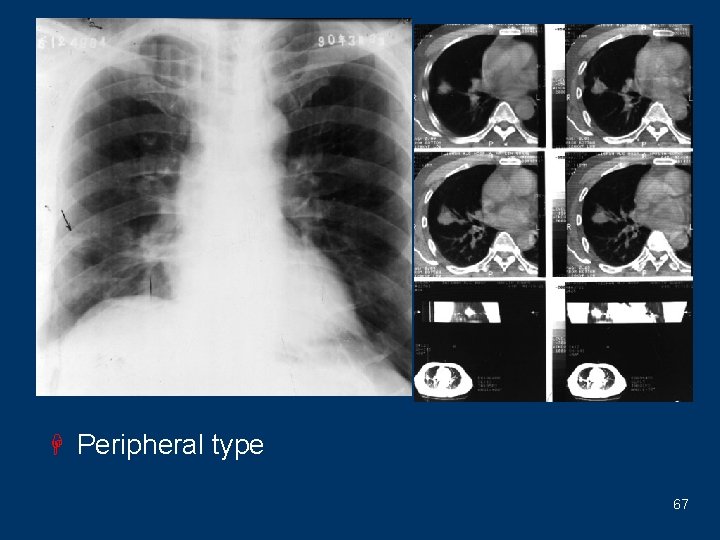
H Peripheral type 67

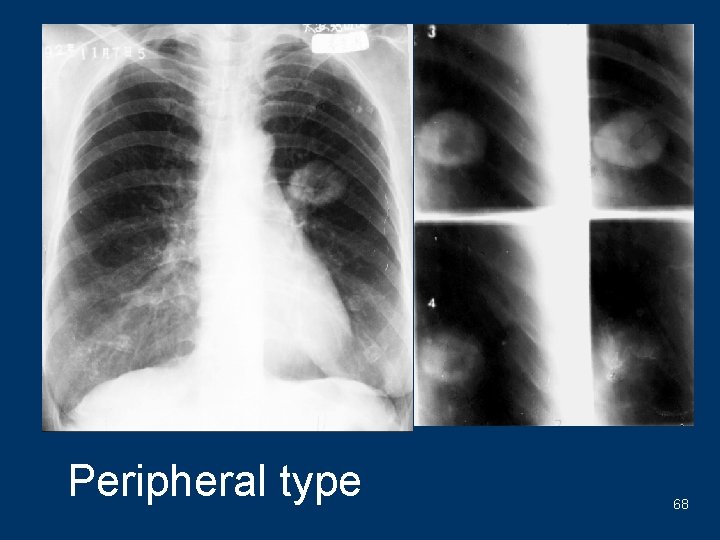
Peripheral type 68

Pancoast’s neoplasm w Henry Khunrath Pancoast, 1875 -1939, American w w w radiologist Also called superior sulcus neoplasm Occurs at extreme apex of lung in superior sulcus Typically invades chest wall and into neck Posterior extension may result in an involvement of roots of the brachial plexus with spread to spinal canal and vertebral bodies Anterior extension leads to involvement of the subclavian artery with invasion of trunks, division and cords of brachial plexus within interscalenic space and medial invasion of sympathetic stellate ganglion 69

Pancoast’s neoplasm w Is most often a pulmonary squamous cell carcinoma w Clinical manifestations are thoracic pain, Horner's syndrome, destruction of bone, atrophy of hand muscles and brachial plexopathy w Radiographs, an apical mass or an asymmetrical pleural thickening with irregularities sometimes associated with rib destruction w Enhanced CT and thin collimation and MRI are the preferred modalities for evaluating w if local tumor is not extensive and if there is no evidence of mediastinal or distant metastases, can be treated successfully with preoperative radiation therapy, followed by lobectomy and chest wall resection 70

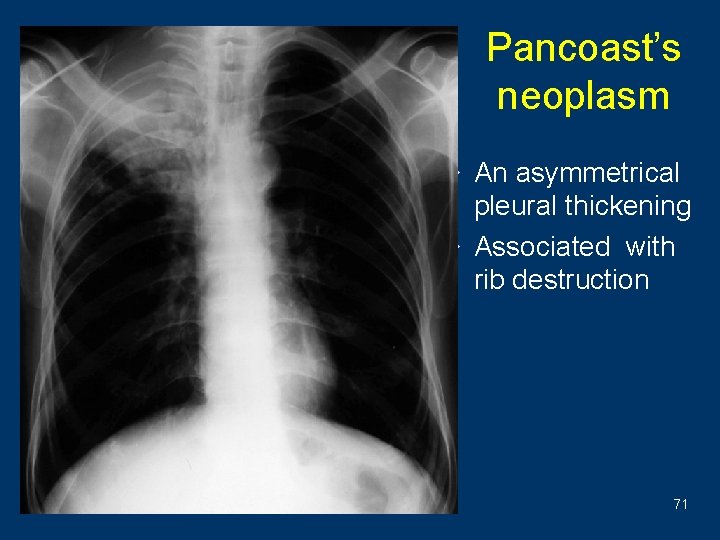
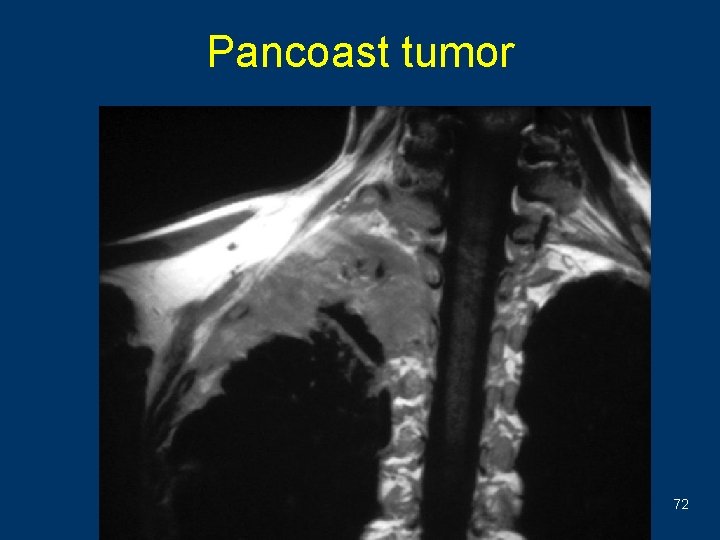
Pancoast’s neoplasm w An asymmetrical pleural thickening w Associated with rib destruction 71

Pancoast tumor 72

Peripheral type—CT w Nodule or mass w irregular or spiculated margin with distortion of adjacent vessels w Pseudocavitation (small, focal, low-attenuation regions within or surrounding the periphery of a nodule) w Cavitation have thick, irregular walls w Hilar metastasis w Mediastinal metastasis w Remote metastasis 73

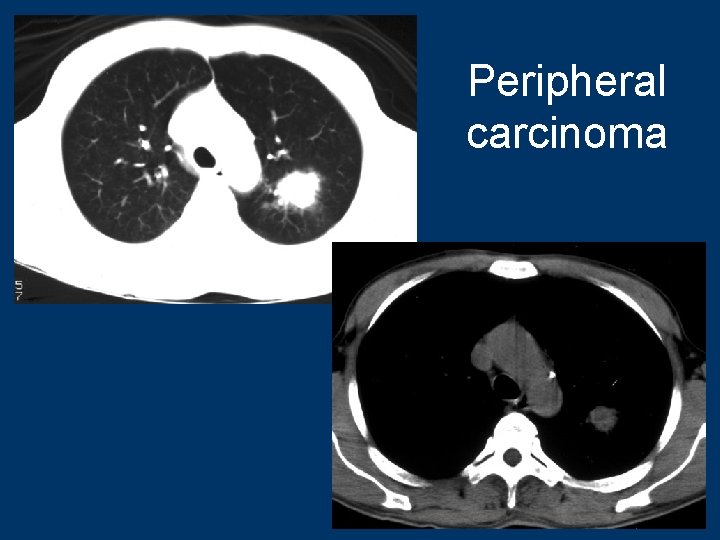
Peripheral carcinoma 74

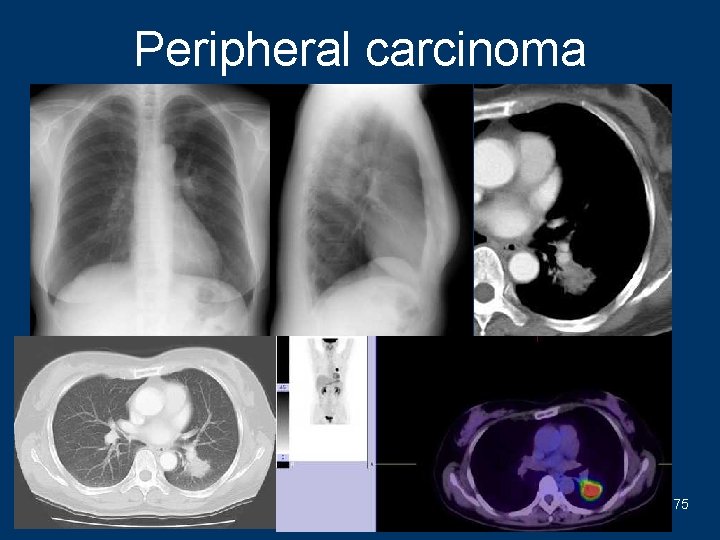
Peripheral carcinoma 75

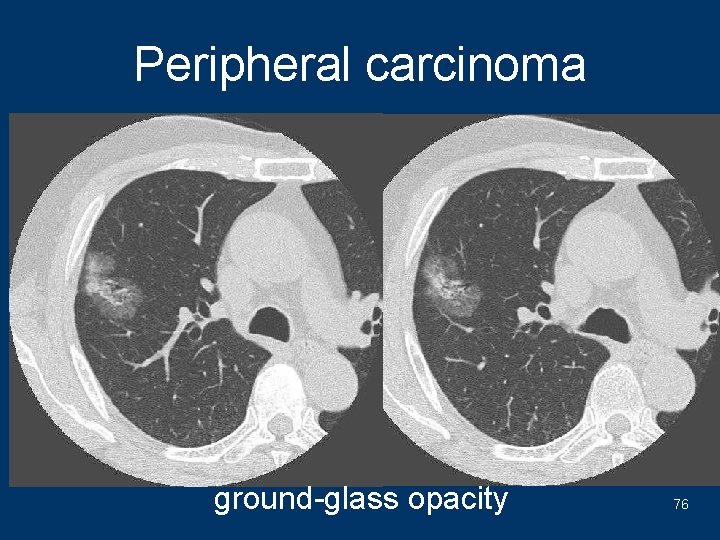
Peripheral carcinoma ground-glass opacity 76

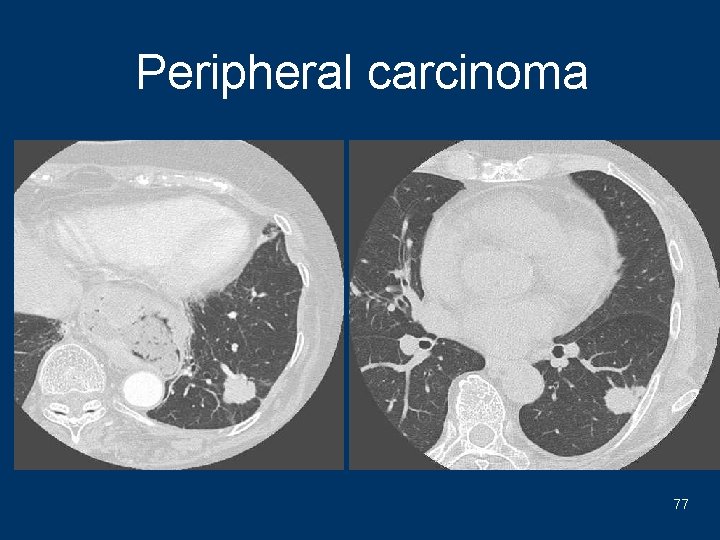
Peripheral carcinoma 77

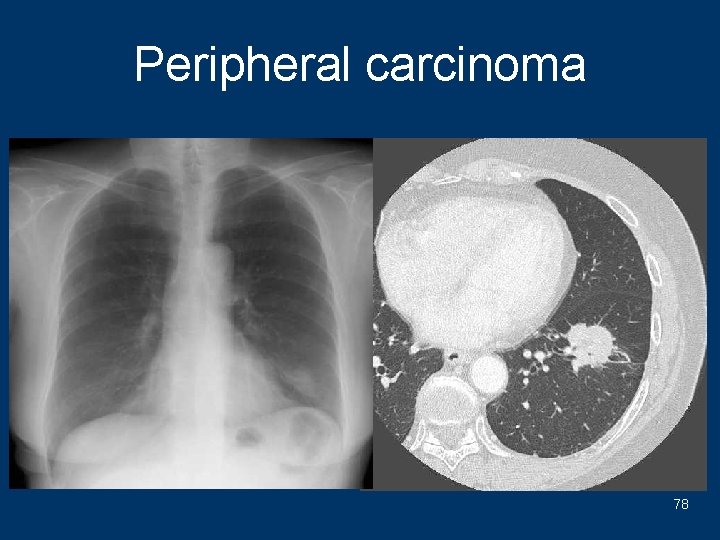
Peripheral carcinoma 78

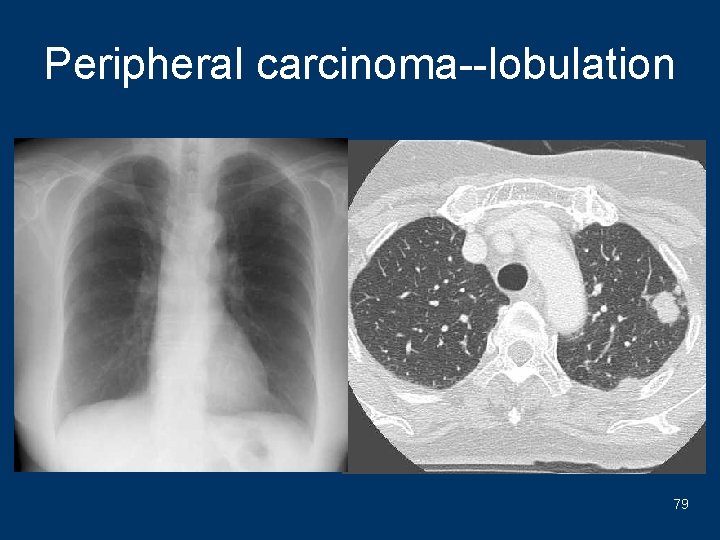
Peripheral carcinoma--lobulation 79

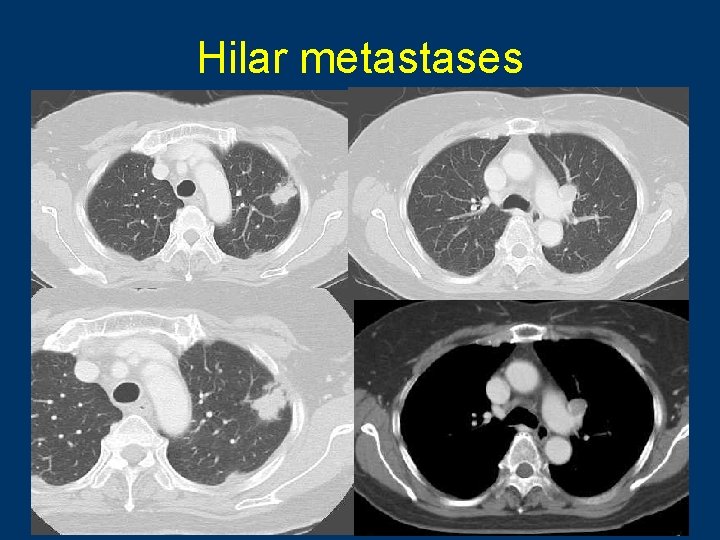
Hilar metastases 80

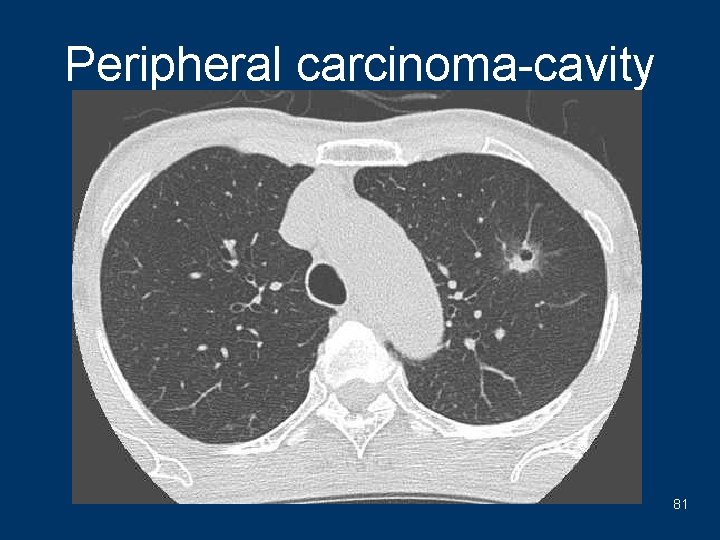
Peripheral carcinoma-cavity 81

Bronchioalveolar cell carcinoma w is a subtype of adenocarcinoma of the lung accounting for less than 5% of all lung cancers w Pathologically, it consists of a peripheral neoplasm in which the malignant cells use the surrounding alveolar walls as a scaffold w The cells produce mucus in such large amounts that expectoration of mucoid sputum may become a major presenting symptom 82

Bronchioloalveolar cell carcinoma w May present three distinct radiological patterns w The most common is a SPN, peripheral in location with ill-defined and hazy contours w On CT, the nodule frequently contains an air bronchogram and/or small bubble-like lucencies suggestive of pseudocavitation w Less characteristically, the nodule may appear homogeneously dense with irregular or spiculated contours, often associated with pleural retraction 83

Bronchioloalveolar cell carcinoma w The second pattern consists of lobar consolidation mimicking pneumonia, sometimes associated with nodules in the same lobe, other lobes or the contralateral lung. This reflects the presumed dissemination of the tumor through the tracheobronchial tree. The finding of a socalled angiogram sign may be seen on CT 84

Bronchioloalveolar cell carcinoma w The third pattern occurs in only a small minority of patients. It consists of multiple nodules scattered throughout both lungs, measuring 3 -10 mm in diameter, having very irregular margins, and only rarely appearing cavitated w Prognosis of bronchioloalveolar carcinoma when resected as a SPN is relatively good, whereas the prognosis of the large and disseminated lesions is very poor 85

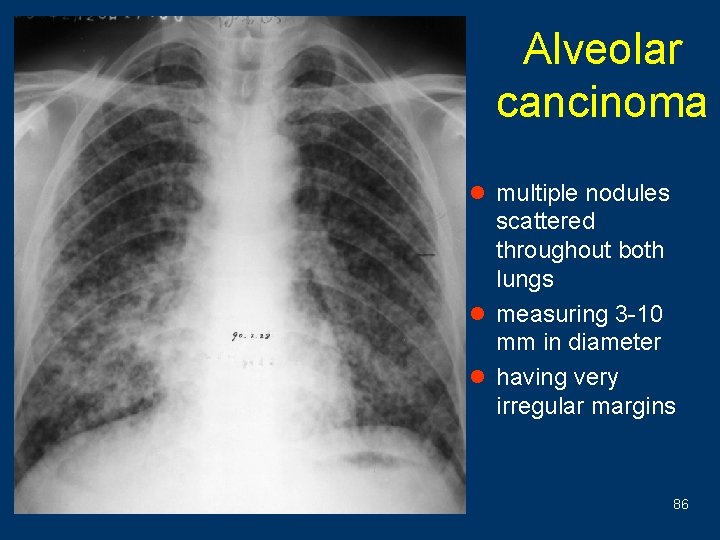
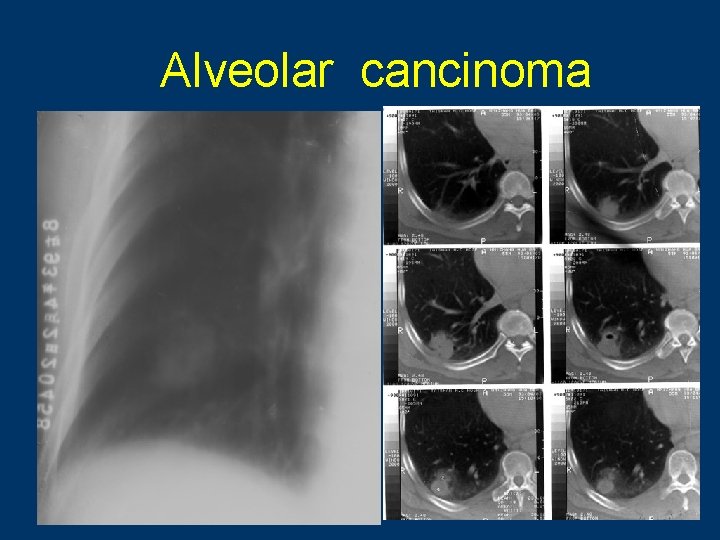
Alveolar cancinoma l multiple nodules scattered throughout both lungs l measuring 3 -10 mm in diameter l having very irregular margins 86

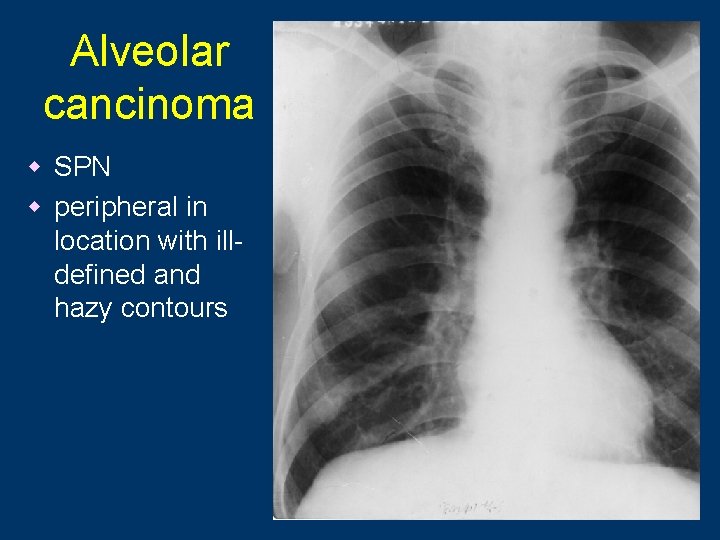
Alveolar cancinoma w SPN w peripheral in location with illdefined and hazy contours 87

Alveolar cancinoma 88

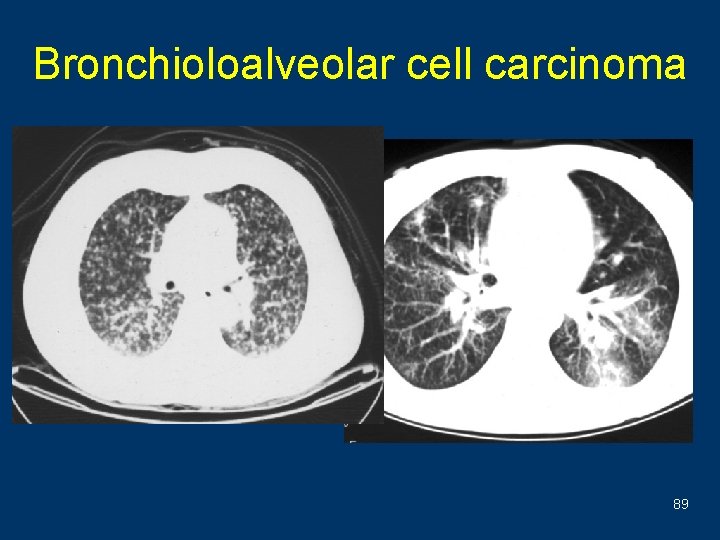
Bronchioloalveolar cell carcinoma 89

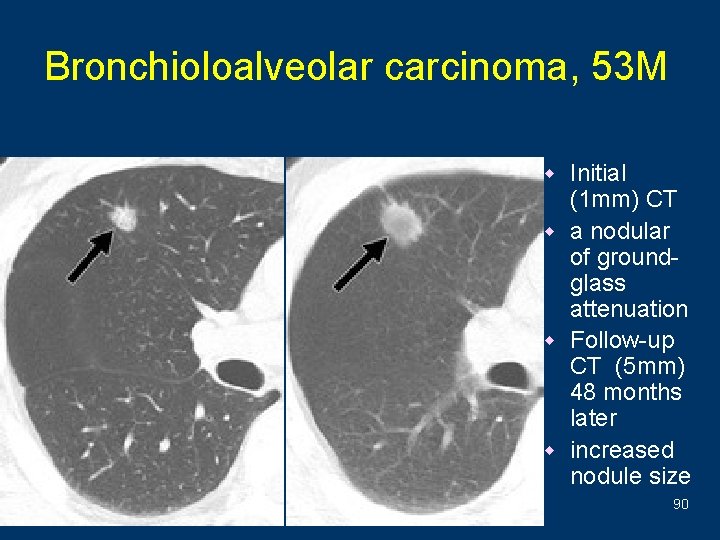
Bronchioloalveolar carcinoma, 53 M w Initial (1 mm) CT w a nodular of groundglass attenuation w Follow-up CT (5 mm) 48 months later w increased nodule size 90

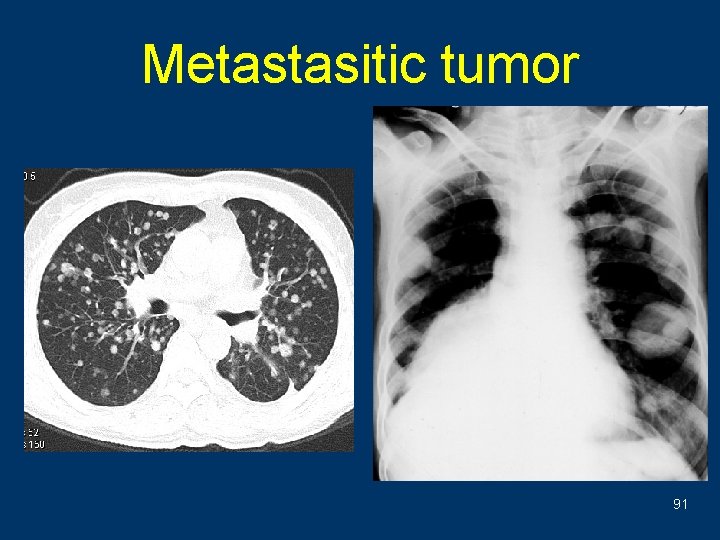
Metastasitic tumor 91

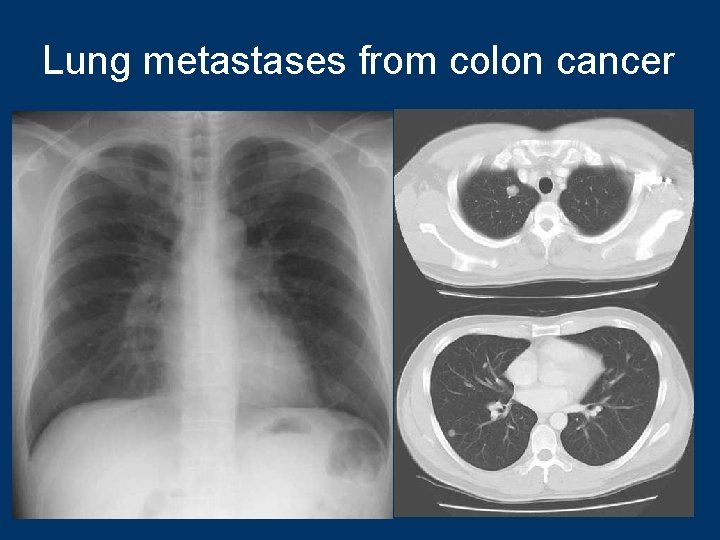
Lung metastases from colon cancer 92