Respiratory adjustments in special conditions By Dr MB

Respiratory adjustments in special conditions By Dr. MB. Bhat. .

In muscular exercise In Heavy exercise body’s metabolism increases about 2000% above normal (compare to high fever it increases only about 100% above normal) u Energy store available in the body at this high level activities is only for 20 seconds. u For sustaining exercise extra fuel & O 2 should be supplied by Respiration & CVS adjustments. u O 2 consumption increases proportionaly to severity of exercise up to a maximum level u

Increased O 2 consumption during exercise is achieved by – 1. Increased pulmonary ventilation 2. Increased O 2 diffusion capacity of lungs (from normal 250 to 4000 ml/min) u [same time CO 2 diffusion capacity also increases from 200 to 8000 ml/min)

Factors increasing pulmonary ventilation u In moderate exercise –by increased depth of respiration u In severe exercise –by increased depth & rate of respiration.
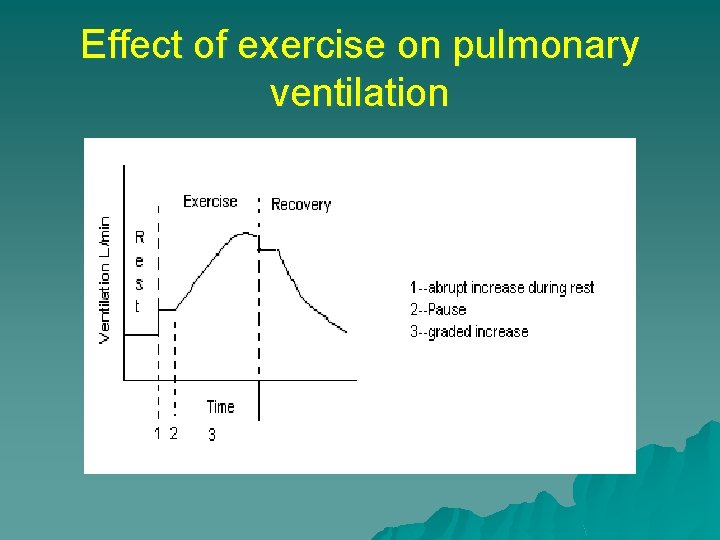
Effect of exercise on pulmonary ventilation

u u u u u Pulmonary ventilation shows – With exercise -Abrupt increase –during on-set of exercise (just before the exercise commence) Followed by a brief pause Graded increase –during exercise proportionate with grade of exercise Cessation of exercise – Abrupt slight decrease –immediately after cessation of exercise Followed by a brief pause Followed by graded decline to pre-exercise level

Abrupt increase with on-set of exercise due to stimulation of respiratory center by -1. 2. 3. Anticipatory response – Psychic stimuli coming from higher center (From limbic system) Pyramidal tract impulses via some collaterals Afferent impulses from proprioceptors of muscle, tendon & joints via collateral of dorsal column tracts (Lovan reflex)

u 1. 2. 3. 4. 5. 6. The graded increase is due to stimulation of respiratory center by – Increase in temperature Increase sensitivity of the respiratory center to the CO 2 (fluctuation of arterial PCO 2 is increased even though the mean arterial PCO 2 remain same) O 2 (even though arterial PO 2 in not decreased) Humeral effect (even though blood p. H, PCO 2 & PO 2 remain constant during moderate exercise) Increase in plasma K+ level In vigorous exercise all the above + Lactic acid

Cessation of exercise u Abrupt decrease – due to stoppage of impulses bombarding respiratory center (but not coming back to basal level) u Graded decline – due to lactic acedemia -- due to O 2 debt –last as long as 90 minutes u Magnitude of O 2 debt – amount by which O 2 exceeds basal consumption from the end of exertion until return to basal level

u 1. 2. 3. u u u Extra O 2 during this period is used for – Combine with muscle myoglobin Resynthesis of ATP & Phosphocreatine Removalof lactic acid Fate of lactic acid – 80% converted to glycogen in the liver 20% is metabolized to CO 2 & water During strenuous exercise because of O 2 debt the RQ rise to 2. After cessation because of repayment of O 2 debt the RQ falls to 0. 5

Hypoxia Oxygen deficiency at tissue level is known as hypoxia

Classification of hypoxia 1. 2. 3. 4. Hypoxic hypoxia or Arterial hypoxia Anemic hypoxia Stagnant hypoxia or Ischemic hypoxia or Hypo kinetic hypoxia Histotoxic hypoxia

Type of hypoxia Hypoxic Anemic Stagnant Histotoxic Oxygen content in the blood Reduced Normal Arterial PO 2 Reduced Normal Oxygen carrying capacity Normal Reduced Normal Hemoglobin saturation of blood Reduced Normal or normal Normal Rate of blood flow to tissue Normal Reduced Normal O 2 utilization by tissue Normal Reduced A-V O 2 difference More Reduced Cyanosis General Not occur Local & general Not occur Oxygen therapy useful not useful Not useful Useful Treatment oxygen with hyperbaric -- Not useful

Hypoxic hypoxia u Seen in -u Physiological condition – High altitude (alveolar PO 2 is decreased) u Pathological condition – Cardiorespiratory diseases (O 2 diffusion capacity is decreased)

High altitude Atmospheric pressure decreases in high altitude u Concentration of gases everywhere in the atmosphere is same u Whereas, partial pressure of the gas varies. u Also in the alveoli, the water vapor pressure is constant (47 mm Hg) u So PO 2 in alveoli = ATP – 47 X O 2 concentration (20% or 0. 2) u

u At 10, 000 ft (3000 m) alveolar PO 2 is 60 mm Hg –Hb saturation maybe normal u At 12, 000 ft (3700 m), mental irritability appears (first hypoxic symptom) u At 18, 000 ft (5500 m), hypoxic symptoms are severe u At 20, 000 ft (6100 m)consciousnes lost in 20 seconds & death occurs in 4 to 5 minutes (PO 2 is only 20 mm Hg)

Hypoxic symptoms at high altitude u u u u Less severe hypoxic symptoms – Acute mountain sickness -- Many individuals first arrive at high altitude develop “transient mountain sickness” –acute mountain sickness The syndrome develops 8 to 24 hours after arrival & last 4 to 8 days Symptoms of acute mountain sickness are – Mental symptoms --Irritability, mental aberrations such as impaired judgment, dis-orientation, excitement, drowsiness, loss of sense of time, loss of sensibility, Other systemic symptoms -- dulled pain & headache, breathlessness, dizziness, insomnia, fatigue, Cheyne-Stoke breathing is common during sleep –anorexia, nausea, vomiting, tachycardia, palpitation, retinal hemorrhage (after healing no visual defect);

u Severe hypoxic symptoms – u 1. Hypertension (proportionate to severity of chemoreceptor drive) u 2. High-altitude cerebral edema –due to low PO 2 –arteriolar dilation – increase capillary pressure –increase transudation of fluid into brain tissue u Due to Cerebral edema – ataxia, disorientation, in extreme case coma & death

u 3. High-altitude pulmonary edema –is a patchy edema of lungs due to pulmonary hypertension (due to low PO 2), Left atrial pressure is normal u Cough with pink frothy sputum u Increased pulmonary capillary pressure along with polycythemia cause increased right heart work & right ventricular hypertrophy.

Chronic mountain sickness (Monge’s disease) u Disease of long term residents at high altitude u These people develop –manifestation of superimposed pulmonary disease with -u Fatigue, reduced exercise tolerance, severe hypoxemia & polycythemia

Acclimatization (Increase altitude tolerance) Compensatory mechanisms develop over a period of time to tolerate high altitude u 1. 2. ‘Mechanisms are – Hyperventilation –due to hypoxic action through peripheral chemoreceptor Increased sensitivity to CO 2 (after 4 days) —due to --outward movement of HCO 3 from ; --active transport of H+ ions into CSF; --development of lactic acidosis in the brain All these decrease p. H in CSF that stimulate respiration through central chemoreceptor

u u 1. 2. 3. 4. 5. 6. 3. Polycythemia – dueto erythropoietin (within 2 to 3 days) – due to hypoxia –sustain as long as stay in high altitude Others – Increase number of capillaries in peripheral tissues Increase mitochondria Increase cytochrome oxidase in the tissue Increase myoglobin level Increase MBC (up to 200 L/min) as air is less dense Kidney secrete alkaline urine

Hypoxic hypoxia in pathological condition Lung failure (or) Gas-exchange failure – u Pulmonary fibrosis u V/Q imbalance –Shunt –Congenital heart diseases –Tetralogy of Fallot (Blue baby) – Right to left shunt u Pump failure (or) Ventilation failure – u Respiratory muscles fatigue u Mechanical defects cause atelectasis u Depression of respiratory center –by morphine & other drugs u

Atelectasis –Collapse of the alveoli u 1. 2. 3. Causes – Surfactant deficiency Obstruction of bronchus & bronchioles – alveoli beyond point of obstruction collapse –leading to more negative intrapleural pressure –pulls mediastinum towards affected side Pneumothorax –air in the interstitial space –intrapleural pressure equal to atmospheric pressure –Push the mediastinum towards normal side

Asthma u Obstructive type of respiratory disease u Due to air way obstruction – due to u Air way hypersensitivity –due to – Allergy u Attack usually occurs in morning & also during exercise u Treatment – u β 2 adrenergic agonists u Administration of steroids

Emphysema Obstructive type of respiratory disease u Degenerative potentially fatal disease u Lungs are voluminous & inelastic with widespread destruction of alveolar walls & pulmonary capillaries u Most common cause heavy cigarette smoking u Smoking increase PAM which attracts leucocytes –which release protease enzymes & O 2 free radicals –destroy lung tissues u Smoking also decrease α 1 antitrypsin – which destroy protease enzymes u

Features of Emphysema 1. 2. 3. 4. 5. 6. 7. 8. 9. Barrel-shaped chest Work of breathing (both inspiration & expiration is laboured) Compliance (normal o. 25 to 0. 9 L/mm Hg) FRC (normal 3 L to 8 L) FVC duration (normal 4 to 8 second) FEV 1 (normal 3. 2 L to 0. 75 L) Physiological dead space (doubled) Physiological shunt O 2 diffusion capacity (1/5 th)

9. Arterial PO 2 (even goes to 50 mm Hg) 10. Arterial PCO 2 (goes up to 60 mm Hg) 11. Hb saturation (only 80 to 85%) 12. Plasma HCO 3 (compensatory acidosis) 13. Polycythemia (due to hypoxia) 14. Pulmonary hyperventilation 15. Right ventricular hypertrophy (Cor Pulmonale) Here respiratory drive is due to hypoxia. So O 2 treatment is not recommended

Anemic hypoxia u Seen in u Anemia –only in severe anemia; where Hb deficiency is marked (because in hypoxic condition increase 2, 3 -DPG level shift O 2 dissociation curve to right) u Carbon-monoxide poisoning

Stagnant hypoxia u Due to slowing of circulation u Local –vasoconstriction due to cold or obstruction to venous outflow; & peripheral circulatory failure u General – cardiac failure

Histotoxic hypoxia u Seen in cyanide poisoning u Cyanide inhibit cytochrome oxidase & other iron containing enzymes u Treatment –Administration of methylene blue or nitrates (oxidizing agents) u –oxidized Hb to methemoglobin which react with cyanide to form cyanmethemoglobin, a non-toxic compound u Hyperbaric O 2 therapy is useful

Cyanosis Bluish coloration of skin, nail beds, ear lobe, lips, fingers & mucus membrane due to presence of HHb >5 gm/dl u Local cyanosis or Peripheral cyanosis – seen in stagnant hypoxia due to exposure of cold, circulatory failure u Signs –patients may be cold & blue, peripheral pulses difficult to feel u Central cyanosis – seen in hypoxic hypoxia u Signs –patients extremities are warm & pulsatile, rapid blood flow, increase heart rate & pulse pressure and vasodilation u

u u 1. 2. 3. u Before cyanosis readily apparent; the Hb saturation of O 2 must fall below 80% & PO 2 45 mm Hg. Cyanosis does not occur in – Anemic hypoxia –due to low Hb content CO poisoning –COHb is cheery red Histotoxic hypoxia –O 2 utilization is less so HHb is also less High circulatory level of methemoglobin also produce discoloration of skin similar to cyanosis

O 2 therapy u Useful in treatment of u Hypoxic hypoxia (except in shunt condition) u Cyanosis u Only limited value in treatment of – u Anemic, Stagnant & Histotoxic hypoxia

Hyperbaric oxygen therapy u u u u u Exposure of O 2 with high pressure Advantage –markedly increase dissolved O 2 content in blood Used in treatment of – CO poisoning, Cyanide poisoning, Congenital cardiac disease (right to left shunt) Gas gangrene Very severe blood loss anemia Diabetic leg ulcers & other wounds that are slow to heal Rescue of skin flaps & grafts in which circulation is marginal, Primary treatment for decompression sickness & air embolism Radiation induced tissue injury

Oxygen toxicity Due to production of superoxide anions (O 2—)— oxygen free radicals & H 2 O 2, also – due to decrease surfactant production & lung macrophages in high PO 2. u Safe level –gas mixture contain O 2 <80% (can administer even 24 hours for years) u When gas mixture contain O 2 >80% to 100% (& 2 to 3 ATP) –can tolerate only up to 5 hours (Hyperbaric O 2 treatment) u When above administered >8 hours – respiratory irritation, sub-sternal distress, nasal congestion, sore throat & coughing u

u When exposed above >24 to 48 hours –cause lung damage, pulmonary edema, diminished vital capacity (due to absorption atelectasis), due CNS effect convulsion preceded by nausea, ringing in the ear & twitching of face u In children – u Bronchopulmonary dysplasia, Retrolental fibroplasia –formation of opaque vascular tissue in eyes (retinopathy of pre maturity)

Hypercapnea u Occurs in – u Various forms of pump failure u Febrile state –For each 1 o. C rise in temperature, the CO 2 production by 13% u High carbohydrate food intake u Symptoms of large excess of CO 2 in blood –CO 2 narcosis – Depression of CNS –leads to confusion, diminished sensory activity, in extreme case – coma, respiratory depression & death

Hypocapnia u Occurs due to hyperventilation u Leads to – u Alkalosis u Vasoconstriction u Reduction in Cerebral blood flow (by 30%) u Cerebral ischemia –cause dizziness & parenthesis

Asphyxia u Existence of acute hypercapnia & hypoxia together due to closed airway breathing u Leads to improper aeration of blood u Occur in – u Drowning u Hanging u Pneumothorax

Effect of asphyxia Stage 1 –Stage of hyperpnoea – u duration 1 min u Features – u Rate & depth of respiration increased u Respiratory efforts are Violent u Dyspnea results u Initially both inspiratory & expiratory movements are increased u Later expiratory movements are more pronounced u Unconsciousness marked end of this stage u Cause –due to hypercapnea u

u u u Stage 2 –Stage of central excitation – duration 1 to 2 minutes Expiratory movements are still more pronounced with each expiration, the whole body enters into convulsion Saliva secretion & vomiting occurs Blood p. H decreases –acidosis (accumulation of lactic acid due to convulsion) Increased wide spread sympathetic stimulation Signs of central excitations appear – such as Increase heart rate & BP; Pupillary constriction (myosis) Exaggeration of reflexes Cause –hypercapnia, hypoxia & acidosis
u Stage 3 –Stage of central depression u Duration 2 to 3 minutes u Expiratory convulsion ceased u Replaced by slow deep spasmodic inspiration –individuals stretches out & open mouth wide as if gasping for breath (gasping type of breathing) u Signs of central depression appear – u Pupillary dilation (mydriasis) u Abolition of reflexes u Decreased HR & BP and vasodilation
As this stage is progressed interval between successive gasping longer u Cause –direct hypoxic effect on respiratory & other brain centers which is depressive. u Asphyxiated victim can still be saved by artificial respiration u Victim may develop ventricular fibrillation due to hypoxic myocardial damage & high circulatory catecholamine u If artificial respiration is not started – u At the end of 4 to 5 minutes of stage 3, the victim dies. u

Periodic breathing u When breathing is non-rhythmic & irregular, it is said to be periodic breathing u Two types u Cheyne-Stoke breathing –Regularly irregular type of periodic breathing u Biot’s breathing –Irregularly irregular type of periodic breathing
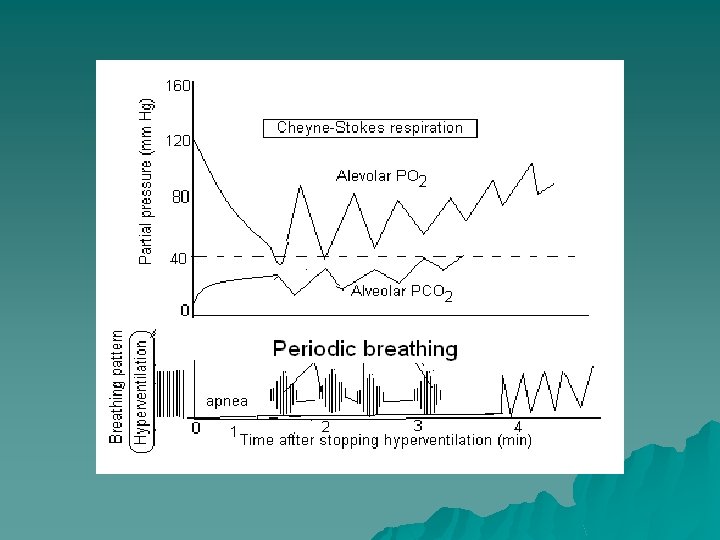
Cheyne-Stoke breathing Occurrence of waxing & waning type of respiration with a period of apnea in between last for few seconds to few minutes & then the cycle repeats 1. Physiological High altitude 2. After hyperventilation 3. In deep sleep 2. 4. In anesthetic condition 3. 5. Quite common u infants in healthy u 1. Pathological Congestive heart failure Uremia Elevating intracranial pressure

Biot’s breathing u Varying breathing time alternate with apnoeic periods of different lengths u Transition from periods of activity to apnea & back are abrupt u Occurs only in pathological conditions affect CNS –such as meningitis

Dyspnea u u 1. 2. 3. 4. Difficulty in breathing; where breathing becomes consciousness Causes – Reflex stimulation of respiratory centers either through central or peripheral or both chemoreceptors. Hypersensitivity of the Hering-Breuer reflex Hypoxic conditions Restriction of the action of the diaphragm or inter-costal

5. 6. 7. 8. 9. Acidosis Increased metabolism Nervous conditions such as emotional disturbance, neurasthenia, hysteria, encephalitis, cerebral tumor, cerebral hemorrhage or cerebral edema Various pulmonary diseases Cardiac Dyspnea –mitral stenosis

Effects of increased barometric pressure (Under water breathing) Ambient pressure increases by 1 ATP for every 10 m (33 ft) of depth in sea water or 10. 4 m of depth in fresh water u But work of breathing is increased as density of gas is increased u To overcome this, divers breath gas or air at increased pressure from pressurized chamber (Caisson chamber) u At high pressure, gases including inert gas equilibrium with body fluid & tissue increases diffusion & soluble capacity of gas u

u Among excess of gas content in the body -u Excess of O 2 can be utilized by the body u Excess of CO 2 can be expired out u Excess of N 2 pose problem u Total volume of N 2 in the body at sea level is one liter; whereas at 300 ft depth, 10 L u N 2 solubility is high in fatty tissue
![Decompression sickness [Dysbarism] [Caission disease] [Bent knee paralysis] Symptoms takes place to a diver, Decompression sickness [Dysbarism] [Caission disease] [Bent knee paralysis] Symptoms takes place to a diver,](http://slidetodoc.com/presentation_image_h/1786f8d1d192ff72bab7868cb0d16c20/image-53.jpg)
Decompression sickness [Dysbarism] [Caission disease] [Bent knee paralysis] Symptoms takes place to a diver, if he ascends rapidly from underwater to surface u In underwater breathing, due to high pressure, volume of gas equilibration (content) in body fluid & tissue is more. u In surface, as pressure is normal, excess gas equilibrates at high pressure begins to come out as bubbles. u

Small bubbles –no physiological disturbance u Formation of large bubbles (if ascends rapidly) –which when, u Coming out in the region of joints –Bends – pain around joints u Enter in pulmonary circulation –Chokes –a feeling of shortness of breath often accompanying cough u Enter coronary circulation –myocardial damage –heart attack u Enter in cerebral circulation –leads to neurological symptoms such as -u

Neurological symptoms are – u Parenthesis u Itching u Deafness u Impaired vision u Vestibular disturbance u Even stroke (Diver’s paralysis) u In extreme case patient may collapse & die u

Prevention – u Slow ascending has enough timeto prevent bubbles from being unduly large u Wearing SCUBA gear (Self-Contained Underwater Breathing Apparatus) u Treatment – u Recompression in a pressure chamber followed by slow decompression u Note – Half-time for elimination of N 2 – From blood is 2 minutes; from muscle 20 minutes & from fat 60 minutes. u

Artificial respiration u Useful in– u Acute asphyxia due to drowning u CO or other forms of gas poisoning u Electrocution u Anesthetic accidents

The purpose of giving artificial respiration is -u To maintain the gaseous interchange, the vitality of the nerve centers, as well as that of the heart. u It also helps to maintain circulation. u It is expected that after sometime, the respiratory centers will start functioning spontaneously. u During artificial respiration, the alternate inflation and deflation of lungs reflexly stimulate the respiratory centers, and revive the spontaneous respiration u

Methods of artificial respiration u I. Manual methods & u II. Instrumental methods

Manual methods u 1. 2. 3. 4. 5. The different types of manual methods are-Schafer’s method- Subject in prone position; Head tilted side; Operator-side by Holger-Nielsen method (Arm-lift back pressure method) –Subject in prone position, hands folded rested under head; Operator – head end Sylvester’s method —subject in supine position, Operator at head end Mouth-to-mouth method –better than others Eve’s rocking method

Instrumental methods Negative pressure breathing method – u By alternately compressing and relaxing the chest wall – u Drinker’s method u Bragg-Paul’s method u Positive-pressure breathing – u By introducing air or oxygen directly into the lungs – u Continuous inflation method u Intermittent inflation method u

END THANKS
- Slides: 62