Respiration Control of Breathing Dynamics of Breathing ExternalInternal

Respiration Control of Breathing Dynamics of Breathing External/Internal Respiration Gas Transport in Blood
![Control of Breathing PRIMARY MECHANISM [CO 2] and [H+] (including all ways that they Control of Breathing PRIMARY MECHANISM [CO 2] and [H+] (including all ways that they](http://slidetodoc.com/presentation_image_h2/3a96706640e014851091d9d5ef0277a0/image-2.jpg)
Control of Breathing PRIMARY MECHANISM [CO 2] and [H+] (including all ways that they are carried) within the blood are the primary stimuli that affect a person’s breathing rate/depth. (For simplicity’s sake, in Bio 12, we will assume that an increase in breathing rate is accompanied by an increase in breathing depth, and vice versa). • CO 2 and H+ levels in the blood (including all ways that they are carried) are detected by chemoreceptors (chemical-sensitive nerve endings) in the Respiratory Center of the MEDULLA OBLONGATA in the brainstem (top of spinal cord). • The Medulla Oblongata is the part of the brain that controls the body’s organ systems. (p. 334 -335) • The respiratory center is a cluster of nerve cells that trigger inspiration through automatic, rhythmic discharges. •
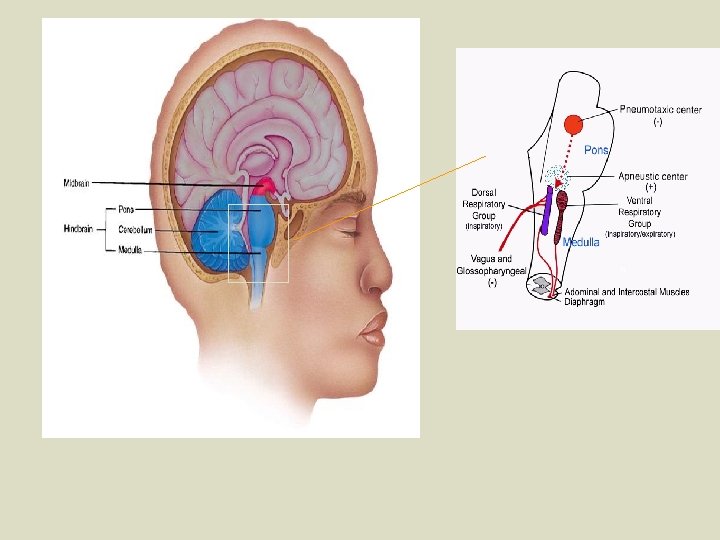
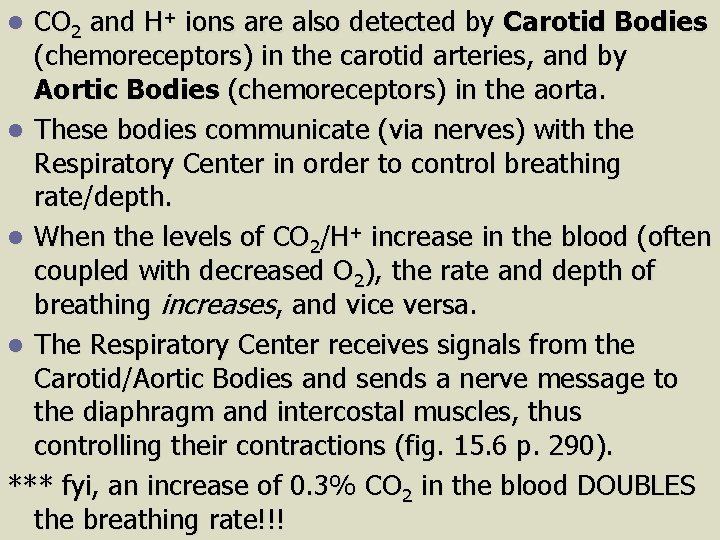
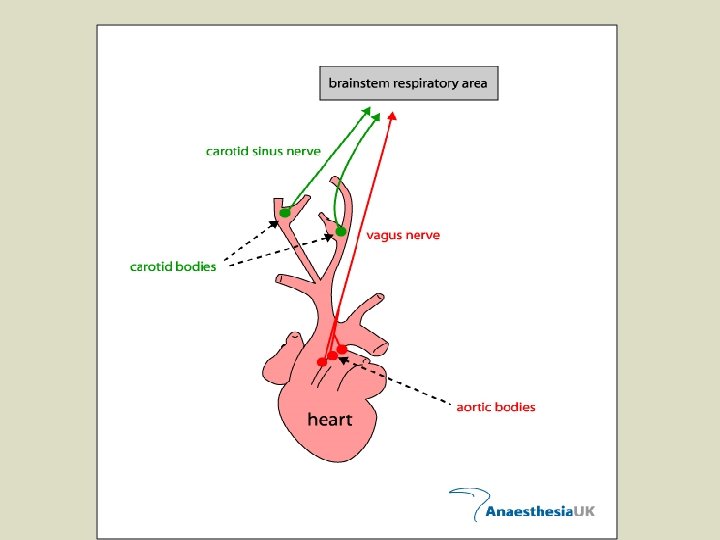
CO 2 and H+ ions are also detected by Carotid Bodies (chemoreceptors) in the carotid arteries, and by Aortic Bodies (chemoreceptors) in the aorta. l These bodies communicate (via nerves) with the Respiratory Center in order to control breathing rate/depth. l When the levels of CO 2/H+ increase in the blood (often coupled with decreased O 2), the rate and depth of breathing increases, and vice versa. l The Respiratory Center receives signals from the Carotid/Aortic Bodies and sends a nerve message to the diaphragm and intercostal muscles, thus controlling their contractions (fig. 15. 6 p. 290). *** fyi, an increase of 0. 3% CO 2 in the blood DOUBLES the breathing rate!!! l
![SECONDARY MECHANISM [O 2] (in both ways that it is carried) in the blood SECONDARY MECHANISM [O 2] (in both ways that it is carried) in the blood](http://slidetodoc.com/presentation_image_h2/3a96706640e014851091d9d5ef0277a0/image-6.jpg)
SECONDARY MECHANISM [O 2] (in both ways that it is carried) in the blood is detected by the same chemoreceptors in the Respiratory Center, and Carotid and Aortic Bodies. o Oxygen levels usually have little effect on breathing rate/depth unless there exists an extreme deficiency. o Cases could be: High Altitudes, CO poisoning, extreme blood loss. o o The Carotid/Aortic Bodies detect the extreme O 2 deficiency and signal the Respiratory Center to increase the rate/depth of breathing (again, low O 2 is usually coupled with high CO 2/H+, but not necessarily in extreme cases – some anaerobic respiration may not produce as much CO 2 as a byproduct). Hyperventilation lowers CO 2 levels to below normal increases blood p. H constricts blood vessels in brain lowers O 2 levels in brain faint. Breathing into paper bag? Increases CO 2 levels to keep p. H nearer to normal…

Synchronicity of Systems!!! l The respiratory center responds to a variety of nervous and chemical signals, adjusting the rate/depth of breathing accordingly. l Control of breathing is only effective if it is synchronized with the circulatory system. l eg. During exercise, cardiac output is aligned with the increased breathing rate, thus enhancing the O 2 supply and CO 2 removal. l Ie. As breathing rate increases, heart rate increases, and vice versa.

Dynamics of Breathing -- Inhalation l l l The respiratory center signals the diaphragm and the external intercostal (rib) muscles to contract. This forces the normally ‘dome-shaped’ diaphragm to push downward and ‘flatten out’, while the external intercostals move the ribcage up and out. Note: during ‘rest’ (normalcy), only the diaphragm contracts; the external intercostals contract during stressful/exertive situations. Nevertheless, both of these contractions and consequential movements serve to increase the size of the thoracic cavity. Since the lungs are attached to the diaphragm and the intercostals/ribs by pleural membranes, the contraction of each increases the size of the lungs (ie. the increase in the size of the thoracic cavity ‘pulls the lungs open’. As the lungs increase in volume, so too do the alveoli.

As the lungs open up (alveoli too!), the air pressure within them decreases. In fact, the air pressure within the lungs decreases to a point where it is less than atmospheric air pressure (ie. the air pressure outside the body). l A notable pressure gradient has now been created and air flows from a region of higher pressure (outside of body) to a region of lower pressure (inside lungs/alveoli). l Result: Air rushes into lungs/alveoli (ie. Air is pulled into the alveoli, not pushed). l Negative pressure breathing (not Positive pressure breathing) l Fig. 15. 7 a p. 291.
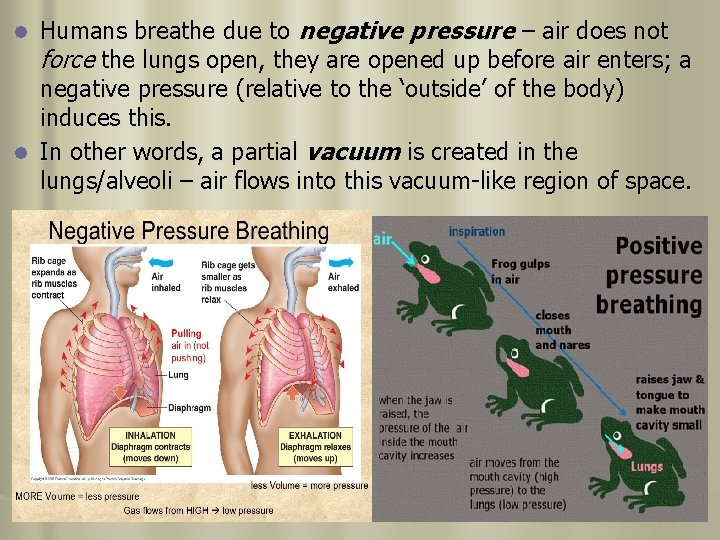
Humans breathe due to negative pressure – air does not force the lungs open, they are opened up before air enters; a negative pressure (relative to the ‘outside’ of the body) induces this. l In other words, a partial vacuum is created in the lungs/alveoli – air flows into this vacuum-like region of space. l
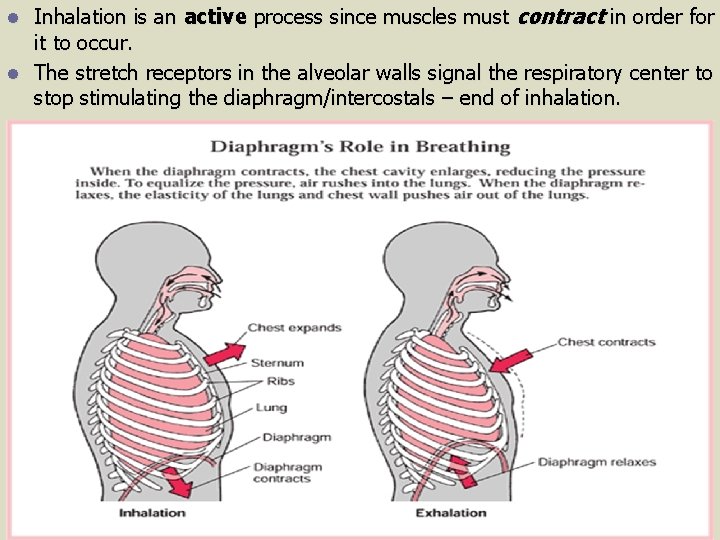
Inhalation is an active process since muscles must contract in order for it to occur. l The stretch receptors in the alveolar walls signal the respiratory center to stop stimulating the diaphragm/intercostals – end of inhalation. l

Dynamics of Breathing -- Exhalation l Upon ceased stimulation from the respiratory center, the diaphragm and the intercostals relax and return to their resting positions: l The diaphragm resumes its dome shape by pushing back upward; l The external intercostals relax, dropping the ribcage down and inward. See fig. 15. 7 b p. 291. l Both of these actions serve to decrease the size of the thoracic cavity, decrease the size of the lungs (the lungs recoil), and increase the air pressure in the lungs to greater than that of atmospheric air.

l Air flows from a region of higher pressure (the lungs/alveoli) to a region of lower pressure (the ‘outside’ of the body). l Exhalation is a passive process in that it simply involves the relaxation of muscles. l That said, exhalation, at times, may be active in nature when breathing is deeper and/or more rapid (eg. during exercise). l Internal intercostal muscle contractions can FORCE the ribcage down and in with more vigor; l Contraction of abdominal muscles can push diaphragm upwards with more force. l Thus, more air might be expelled at a faster rate.

Lung Air Capacity l l l The volume of air a human inhales and exhales with each breath is called tidal volume (avg. = 500 m. L). The maximum volume of air that can be inhaled/exhaled during forced breathing is known as vital capacity (avg. = 4 -5 L). The lungs are actually able to hold more air than the vital capacity, but since it is impossible to completely empty (and thus, collapse) the alveoli, a residual volume of air remains in the lungs after active expiration (avg. = 1. 2 L). This air plays no role in gas exchange. Certain respiratory disorders increase the residual volume of the lungs (more useless air = less chance to get useful air weak, short of breath, etc). Avg. total lung capacity = 6 L. See fig. 15. 5 p. 288
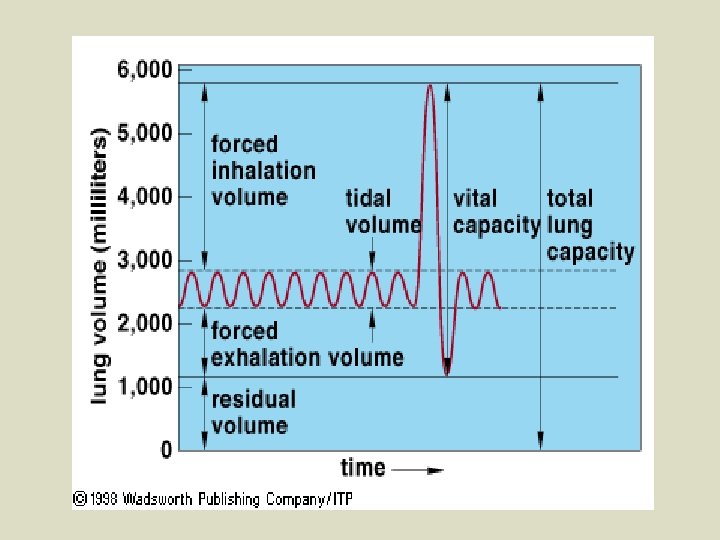

l Some inhaled air (in all people) never reaches the lungs; instead it fills the respiratory tract where there exists no gas exchange functioning l Known as ‘dead space’ air. l To increase the chances of inhaled air reaching the lungs, and exhaled air actually reaching the ‘outside’, it is better to breathe deeply – luckily, the medulla promotes this. l This idea is evident when getting a cramp while running (the cramp is indicative of anaerobic respiration taking place in certain muscles (usually the abs)) – it is better to exhale deeply to rid body of dead space air so that the next inhalations contain mainly ‘fresh’ air with a higher % of O 2.

External Respiration (Location: Lungs) Refers to the exchange of oxygen (O 2) and carbon dioxide (CO 2) between the alveoli and the blood in the alveolar (pulmonary) capillaries. l Recall that the two structures are, at most, 0. 2 µm apart and that each of them possess walls that are only one cell thick – excellent conditions for efficient exchange. l Transfer occurs via simple diffusion, but the gradient is based on gas pressures. l All gases exert pressure (directly proportional to their concentrations); each individual gas exerts its own partial pressure (PP). The PP of each gas sums to the overall gas pressure. l

l The PPO 2 in the alveoli (due to the inhalation of O 2 -laden air) is higher than the PPO 2 in the alveolar capillaries (due to the metabolism of O 2 throughout the body). l Because of this pressure gradient, O 2 flows from a region of higher PP (alveoli) to a region of lower PP (blood). l CO 2 also follows a pressure gradient, except that it moves from a higher PP in the alveolar capillaries to a lower PP in the alveoli for exhalation. l CO 2 is produced by cellular respiration (metabolism) by the body’s cells – high blood PPCO 2 l The PPCO 2 in inhaled air is very low.
Internal Respiration (Location: Body Cells) Gas exchange at the cellular level occurs between the blood in the capillaries and the ECF – the substances that enter the ECF eventually enter the cells via diffusion; the substances ‘waiting’ in the ECF to enter the blood diffused out of cells. l PPO 2 in blood > PPO 2 in ECF O 2 diffuses into ECF for eventual entry into cells. l PPCO 2 in ECF > PPCO 2 in blood CO 2 diffuses into blood (in order to reach lungs for exhalation). **Both external and internal respiration involve the movement of water and other substances as well (Capillary-Tissue exchange) – but here, in the Respiration Unit, we are focusing primarily on the driving force (gradient) behind the movement of gases. l

Transport of Gases in Blood OXYGEN: § Oxygen binds loosely and therefore reversibly to hemoglobin (Hb) in RBCs. § One Hb molecule can bind up to 4 O 2 molecules § Once this occurs, and it is saturated, it is referred to as oxyhemoglobin (Hb. O 2). § Hb + O 2 Hb. O 2 (at lungs) § Hb. O 2 Hb + O 2 (at cells) § Hb = Deoxyhemoglobin (purplish) whereas Hb. O 2 = Oxyhemoglobin (bright red). § Within the lung capillaries, 98% of O 2 joins Hb whereas 2% simply dissolves in the plasma (oxygen is fairly non-polar).

l l l Hb binds more readily to oxygen at a relatively cooler temperature (370 C) and a higher p. H (7. 40) – conditions that exist in the lung capillaries (since they are ‘closer’ to the outside of the body). (See fig. 15. 9 p. 294) Once Hb has 1, 2, or 3 O 2 molecules bound to it, its ‘attraction’ (affinity) for the 2 nd, 3 rd, and 4 th molecule increases exponentially. Thus, all Hb molecules are saturated with O 2. Conditions at the cellular level are warmer (380 C) and more acidic (7. 38 p. H) than those in the lung capillaries. Hb tends to release an appreciable amount (~28%) of its O 2 in these conditions. The difference in the affinity of Hb for O 2 under different temp. /p. H conditions = the Bohr Shift.
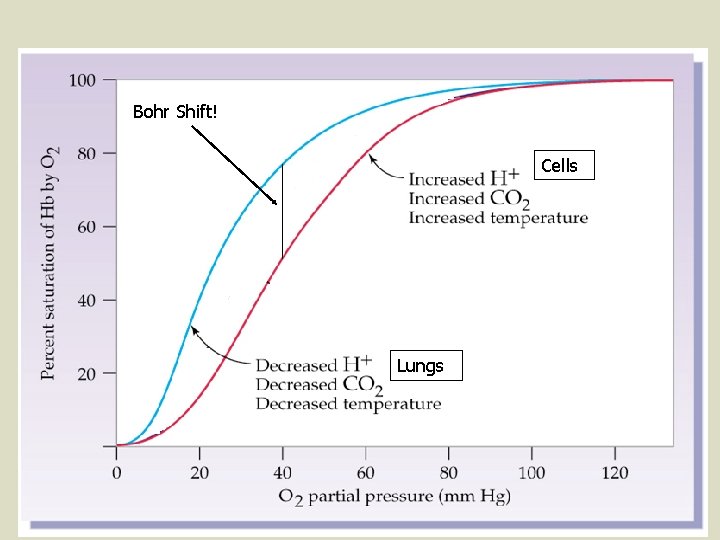
Bohr Shift! Cells Lungs

l During exercise, muscles heat up (increasing temperature) and produce lactic acid (decreasing p. H) which promotes Hb to give up even more of its O 2 to the cells (sometimes up to 75%). l INTERNAL SUFFOCATION – Carbon monoxide (CO) binds to Hb 200 x more readily than O 2. l Thus, oxygen is prevented from reaching the tissue cells on any RBC ‘infested’ with CO. l Therefore, the cells ‘suffocate’.

CARBON DIOXIDE (CO 2) ü CO 2 is transported through the blood in three ways: 1. 70% is transported as the bicarbonate ion (HCO 3 -) in the plasma (more on this in a moment). 2. 23% attaches directly to Hb to form carbaminohemoglobin (Hb. CO 2) @ TISSUES CO 2 + Hb Hb. CO 2 @ LUNGS The lower temp. /higher p. H in the lungs promotes CO 2 release by Hb. ü The higher temp. /lower p. H at the tissue cells promotes CO 2 uptake by Hb. 3. 7% simply dissolves in the plasma (as molecular CO 2). ü ** Silly Metaphor: Hb likes O 2 in the winter (O 2 is like a snowman) and hates O 2 at the beach. CO 2 is opposite…when Hb likes O 2, it hates CO 2, and vice versa…
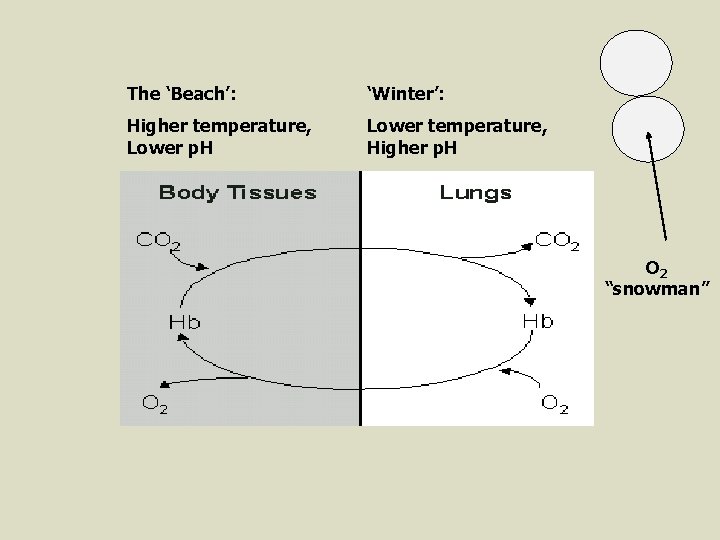
The ‘Beach’: ‘Winter’: Higher temperature, Lower p. H Lower temperature, Higher p. H O 2 “snowman”

Bicarbonate Ion Transport of CO 2 l l l - - As mentioned previously, 70% of the cellular respirationproduced CO 2 is transported in the plasma (dissolved) as HCO 3 - acts as a blood buffer, in that it has the ability to neutralize acidic blood ‘contaminants’ or basic blood ‘contaminants’. Once CO 2 leaves cells and enters the ECF, the blood, and eventually the RBCs, it reacts with water to form carbonic acid (H 2 CO 3) which then dissociates to form HCO 3 - and H+. CO 2 + H 2 O H 2 CO 3 H+ + HCO 3 The RBC enzyme carbonic anhydrase along with the higher temperature at the cellular level work together to promote this reaction between CO 2 and water. Again, 70% of the CO 2 undergoes this reaction.

l l l Once formed, the HCO 3 - diffuse out of the RBCs (Cl- ions move into RBCs to balance the charge) and are carried in the plasma to the lungs. The H+ remain inside RBCs and are picked up by Hb (or else the p. H would severely drop – RBC membranes would be destroyed, blood proteins would be denatured, and vessel walls could be damaged) to form reduced hemoglobin (HHb), which is carried within RBCs to the lungs. H+ + Hb HHb (at tissues, within RBCs). Thus, Hb acts to buffer the blood and keep it at, or near, its optimal p. H. FYI: optimal blood p. H = 7. 4 due to the fact that HCO 3 - is a better base than it is an acid and that there is a much higher concentration of it in the blood than CO 2 and H 2 O (which, in combo, produce H 2 CO 3).

Once blood reaches the lungs, the HCO 3 - and H+ must be converted back to CO 2 and water so that the majority of the CO 2 can be exhaled. l At the lower temperature and higher p. H conditions in the lung capillaries, Hb gives up H+ (so that Hb can pick up O 2), HCO 3 - diffuses back into the RBC (Cl- ions diffuse back out), reacts with H+ to form H 2 CO 3, which then forms CO 2 and water; the CO 2 then diffuses into the alveoli from the blood. l Carbonic anhydrase helps again, but this time catalyzes the reverse reaction at the cooler temperature. H+ + HCO 3 - H 2 CO 3 CO 2 + H 2 O l
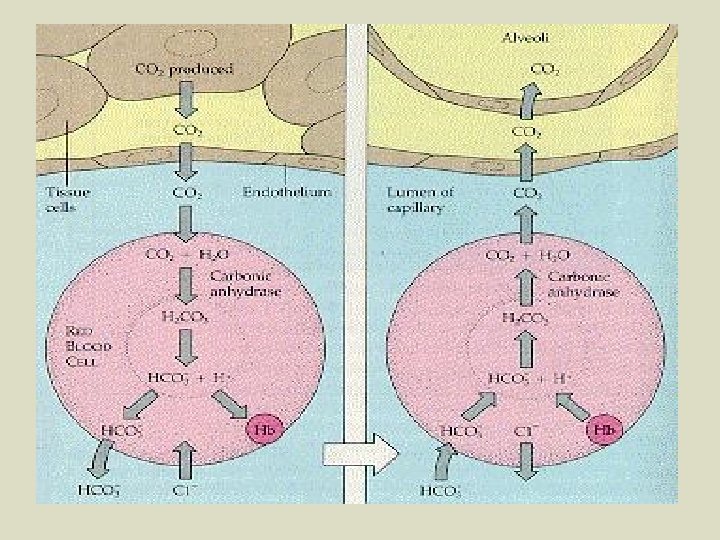

l See fig. 15. 8 p. 293 for summary diagram l Read pp. 295 -298 (for interest only) – Respiratory Disorders…including figs. 15. 10 p. 295 and 15. 11 p. 296.
- Slides: 30