Resident Physics Lectures Christensen Chapter 4 Basic Interactions

Resident Physics Lectures • Christensen, Chapter 4 Basic Interactions Between X-Rays and Matter, Grid Attenuation and Filtration George David Associate Professor Medical College of Georgia Department of Radiology

Photons atoms interations • What happen when photons interact with human tissue?

Photon Phate * • absorbed ¨ completely removed from beam ¨ ceases to exist • scattered ¨ change in direction ¨ no useful information carried ¨ source of noise • Nothing ¨ Photon passes unmolested X
Image Noise Example Caution! Image Noise

Basic Interactions • Coherent Scattering • Compton Scattering • Photoelectric Effect • Pair Production • Photodisintegration

What is important in this lecture • How the interaction happen? • When happen? • The interaction affect on the image quality?
Interaction depends on • Photon energy e. v • Atom atomic number Z ~ + + ~ - -
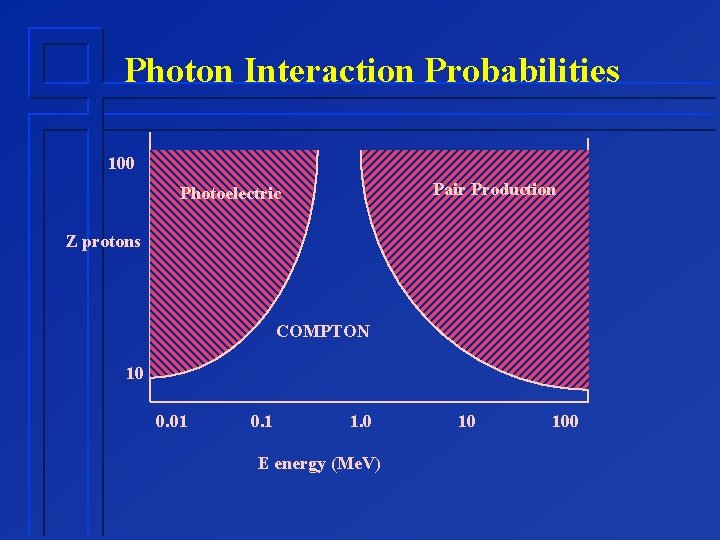
Photon Interaction Probabilities 100 Pair Production Photoelectric Z protons COMPTON 10 0. 01 0. 1 1. 0 E energy (Me. V) 10 100

Basic Interactions • Coherent Scattering D • Compton Scattering D • Photoelectric Effect D • Pair Production T • Photodisintegration T • D=Diagnostic radiology • T=Treatment radiology
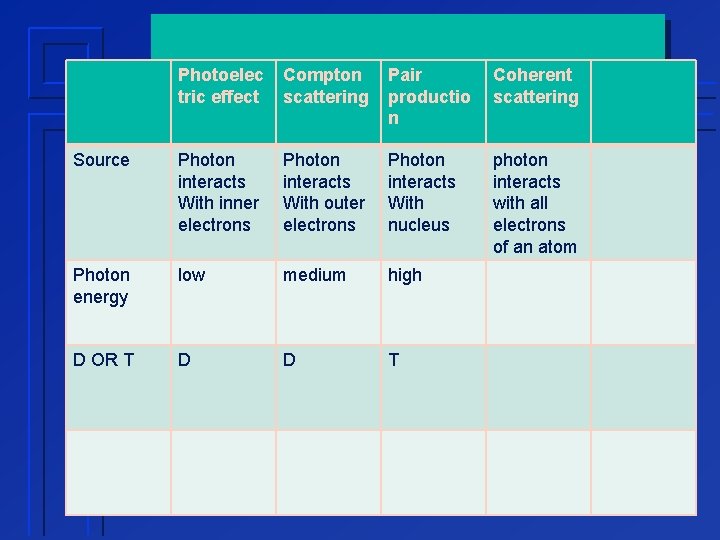
Photoelec tric effect Compton scattering Pair productio n Coherent scattering Source Photon interacts With inner electrons Photon interacts With outer electrons Photon interacts With nucleus photon interacts with all electrons of an atom Photon energy low medium high D OR T D D T

Coherent Scattering • Also called ¨unmodified scattering ¨classical scattering • Types ¨Thomson » photon interacts with single electron ¨Rayleigh » photon interacts with all electrons of an atom

Coherent Scattering • Change in direction • No change in ¨ energy ¨ frequency ¨ wavelength • No ionization • Contributes to scatter as film fog • Less than 5% of interactions ¨ insignificant effect on image quality compared to other interactions

*** • • Pair Production Process high energy photon interacts with nucleus photon disappears electron & positron (positive electron) created energy in excess of 1. 02 Me. V given to electron/positron pair as kinetic energy. - + ~ + + ~ - -
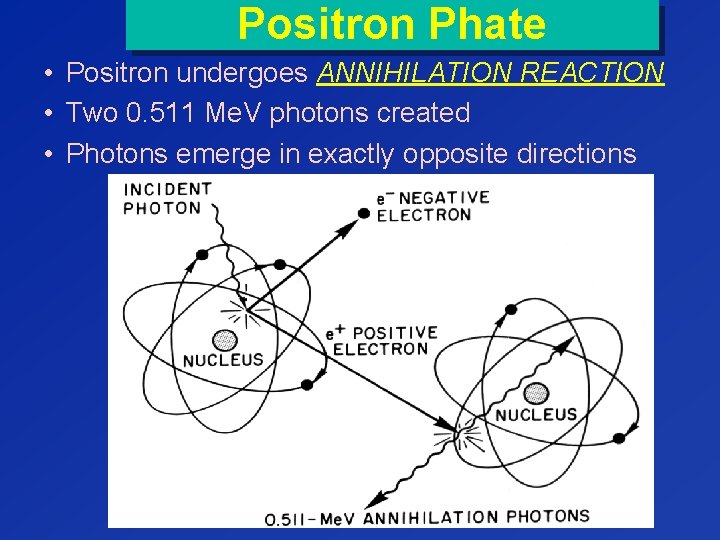
Positron Phate • Positron undergoes ANNIHILATION REACTION • Two 0. 511 Me. V photons created • Photons emerge in exactly opposite directions

Pair Production • Threshold energy for occurrence: 1. 02 Me. V » energy equivalent of rest mass of 2 electrons • Threshold is above diagnostic energies ¨ does not occur in diagnostic radiology - + ~ + + ~ - -

* Photodisintegration • photon causes ejection of part of atomic nucleus • ejected particle may be ¨neutron ¨proton ¨alpha ¨particle cluster ~ + + ~ ? - -

Photodisintegration • Threshold photon energy for occurrence ¨nuclear binding energy » typically 7 -15 Me. V • Threshold is above diagnostic energies ¨does not occur in diagnostic radiology

** Photoelectric Effect • photon interacts with bound (inner-shell) electron • electron liberated from atom (ionization) • photon disappears Photon in - Electron out

PHOTOELECTRIC EFFECT
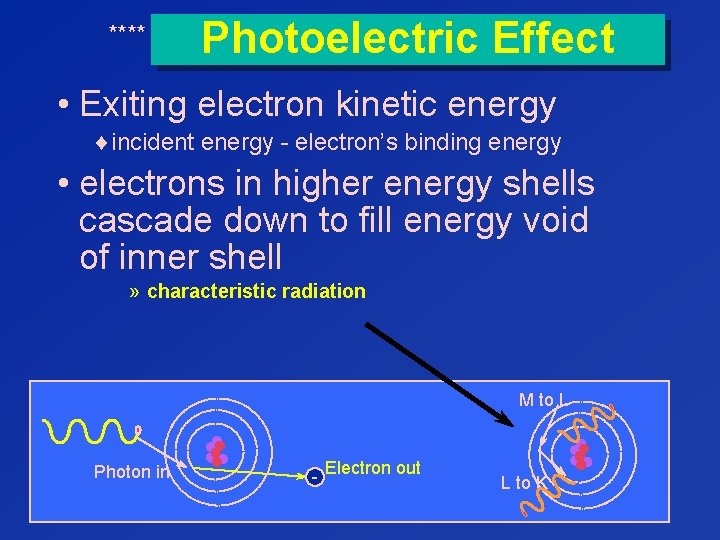
**** Photoelectric Effect • Exiting electron kinetic energy ¨incident energy - electron’s binding energy • electrons in higher energy shells cascade down to fill energy void of inner shell » characteristic radiation M to L Photon in - Electron out L to K

Photoelectric Interaction Probability • inversely proportional to cube of photon energy ¨low energy event • proportional to cube of atomic number • more likely with inner (higher) shells ¨tightly bound electrons 1 P. E. ~ -----energy 3 P. E. ~ Z 3

Photoelectric Effect • Interaction much more likely for ¨low energy photons ¨high atomic number elements 1 P. E. ~ -----energy 3 P. E. ~ Z 3

Photoelectric Effect • Photon Energy Threshold ¨ > binding energy of orbital electron • binding energy depends on ¨ atomic number » higher for increasing atomic number ¨ shell » lower for higher (outer) shells • most likely to occur when photon energy & electron binding energy are nearly the same

Photoelectric Threshold • Binding Energies ¨K: 100 ¨L: 50 ¨M: 20 Photon energy: 25 A Photon in B Photon energy: 22 1 P. E. ~ -----energy 3 Which photon has a greater probability for photoelectric interactions with the m shell?

Photoelectric Threshold 1 P. E. ~ -----energy 3 • Photoelectric interactions decrease with increasing photon energy BUT …

** Photoelectric Threshold • When photon energies just reaches binding energy of next (inner) shell, photoelectric interaction now possible with that shell ¨ shell offers new candidate target electrons Interaction Probability L-shell interactions possible L-shell binding energy K-shell binding energy Photon Energy K-shell interactions possible

Photoelectric Threshold • causes step increases in interaction probability as photon energy exceeds shell binding energies Interaction Probability L-edge K-edge Photon Energy

** Characteristic Radiation • Occurs any time inner shell electron removed • energy states ¨orbital electrons seek lowest possible energy state » innermost shells M to L L to K

** Characteristic Radiation • electrons from higher states fall (cascade) until lowest shells are full ¨characteristic x-rays released whenever electron falls to lower energy state M to L characteristic x-rays L to K
Characteristic Radiation • only iodine & barium in diagnostic radiology have characteristic radiation which can reach film-screen

Photoelectric Effect Why is this important? • photoelectric interactions provide subject contrast ¨ variation in x-ray absorption for various substances • photoelectric effect does not contribute to scatter • photoelectric interactions deposit most beam energy that ends up in tissue ¨ always use highest k. Vp technique consistent with imaging contrast requirements

*** Compton Scattering • Source of virtually all scattered radiation • Process ¨incident photon (relatively high energy) interacts with free (loosely bound) electron ¨some energy transferred to recoil electron » electron liberated from atom (ionization) ¨emerging photon has » less energy than incident » new direction Photon in Electron out (recoil electron) Photon out

Compton Scattering • What is a “free” electron? ¨low binding energy » outer shells for high Z materials » all shells for low Z materials Electron out (recoil electron) Photon in Photon out

Compton Scattering • Incident photon energy split between electron & emerging photon • Fraction of energy carried by emerging photon depends on ¨incident photon energy ¨angle of deflection » similar principle to billiard ball collision Photon in Electron out (recoil electron) Photon out

Compton Scattering Probability of Occurrence • independent of atomic number (except for hydrogen) • Proportional to electron density (electrons/gram) ¨ fairly equal for all elements except hydrogen (~ double)
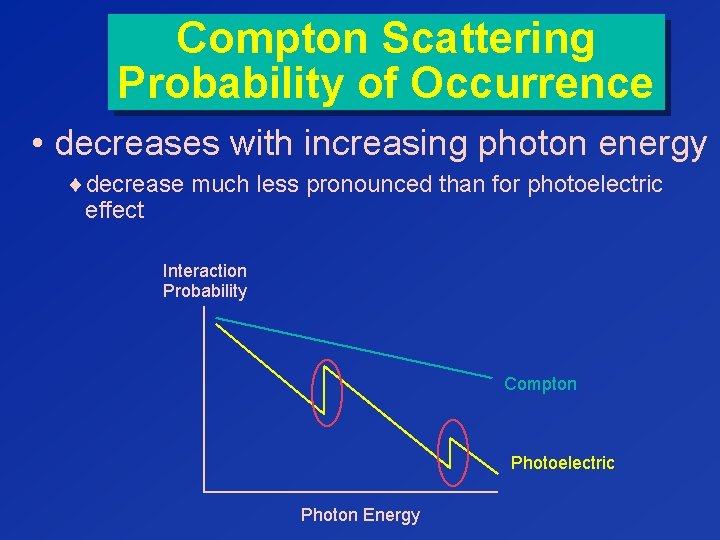
Compton Scattering Probability of Occurrence • decreases with increasing photon energy ¨decrease much less pronounced than for photoelectric effect Interaction Probability Compton Photoelectric Photon Energy
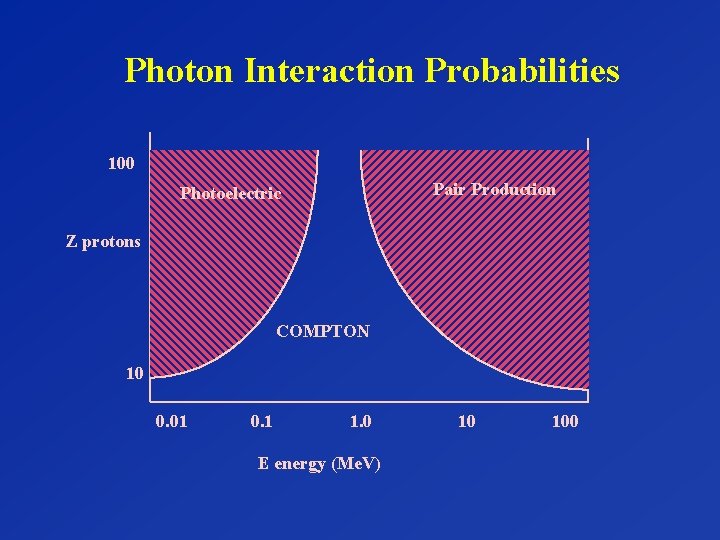
Photon Interaction Probabilities 100 Pair Production Photoelectric Z protons COMPTON 10 0. 01 0. 1 1. 0 E energy (Me. V) 10 100

Resident Physics Lectures • Christensen, Chapter 5 Attenuation George David Associate Professor Medical College of Georgia Department of Radiology
Beam Characteristics • Quantity ¨number of photons in beam 1, 2, 3, . . . ~ ~ ~
Beam Characteristics • Quality ¨energy distribution of photons in beam 1 @ 27 ke. V, 2 @ 32 ke. V, 2 at 39 ke. V, . . . ~ ~ ~ ~
Beam Characteristics • Intensity ¨weighted product of number and energy of photons ¨depends on 324 m. R » quantity » quality ~ ~ ~ ~

Beam Intensity • Can be measured in terms of # of ions created in air by beam • Valid for monochromatic or for polychromatic beam 324 m. R ~ +

Attenuation Coefficient • Parameter indicating fraction of radiation attenuated by a given absorber thickness • Attenuation Coefficient is function of ¨ absorber ¨ photon energy

Linear Attenuation Coef. • Why called linear? ¨ distance expressed in linear dimension “x” • Formula N = No e -mx where N = number of incident photons o N = number of transmitted photons e = base of natural logarithm (2. 718…) m = linear attenuation coefficient (1/cm); property of N N o energy material x = absorber thickness (cm) x

Linear Attenuation Coef. Larger Coefficient = More Attenuation • Units: 1 / cm ( or 1 / distance) • Properties N = No e - m x ¨ reciprocal of absorber thickness that reduces beam intensity by e (~2. 718…) » ~63% reduction » 37% of original intensity remaining ¨ as photon beam energy increases » penetration increases / attenuation decreases » attenuating distance increases » linear attenuation coefficient decreases • Note: Same equation as used for radioactive decay

Polychromatic Radiation • X-Ray beam contains spectrum of photon energies ¨highest energy = peak kilovoltage applied to tube ¨mean energy 1/3 - 1/2 of peak » depends on filtration

X-Ray Beam Attenuation • reduction in beam intensity by ¨absorption (photoelectric) ¨deflection (scattering) • Attenuation alters beam ¨quantity ¨quality » higher fraction of low energy photons removed » Beam Hardening Lower Energy Higher Energy

Half Value Layer (HVL) N = No e -mx • absorber thickness that reduces beam intensity by exactly half • Units of thickness • value of “x” which makes N equal to No / 2 HVL =. 693 / m

Half Value Layer (HVL) • Indication of beam quality • Valid concept for all beam types ¨ Mono-energetic ¨ Poly-energetic • Higher HVL means ¨ more penetrating beam ¨ lower attenuation coefficient

Factors Affecting Attenuation • Energy of radiation / beam quality ¨higher energy » more penetration » less attenuation • Matter ¨density ¨atomic number ¨electrons per gram ¨higher density, atomic number, or electrons per gram increases attenuation
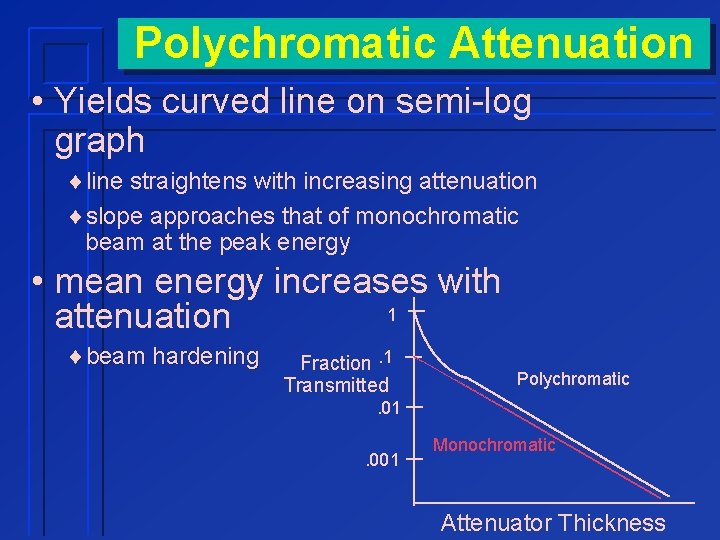
Polychromatic Attenuation • Yields curved line on semi-log graph ¨line straightens with increasing attenuation ¨slope approaches that of monochromatic beam at the peak energy • mean energy increases with 1 attenuation ¨beam hardening Fraction. 1 Transmitted Polychromatic . 01. 001 Monochromatic Attenuator Thickness

Photoelectric vs. Compton • Fractional contribution of each determined by ¨photon energy ¨atomic number of absorber • Equation m = mcoherent + m. PE + m. Compton Small

Photoelectric vs. Compton • As photon energy increases m = mcoherent + m. PE + m. Compton ¨ Both PE & Compton Interaction decrease Probability ¨ PE decreases faster » Fraction of m that is Compton increases » Fraction of m that is PE decreases Compton Photoelectric Photon Energy

Photoelectric vs. Compton m = mcoherent + m. PE + m. Compton • As atomic # increases ¨Fraction of m that is PE increases ¨Fraction of m that is Compton decreases
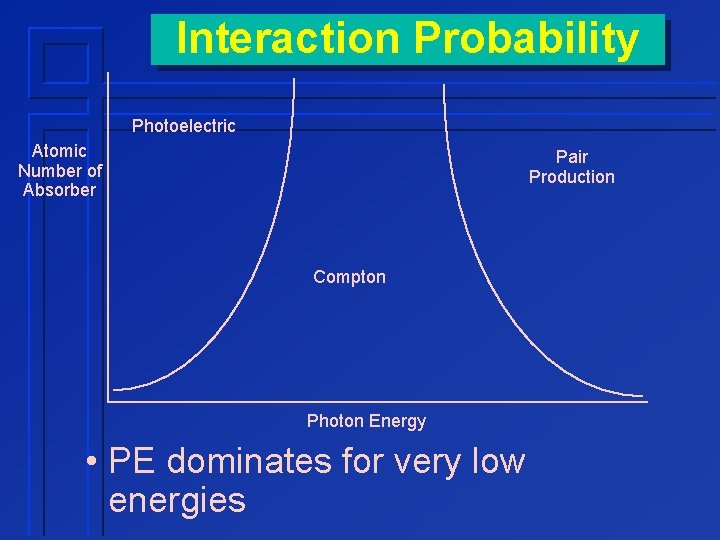
Interaction Probability Photoelectric Atomic Number of Absorber Pair Production Compton Photon Energy • PE dominates for very low energies
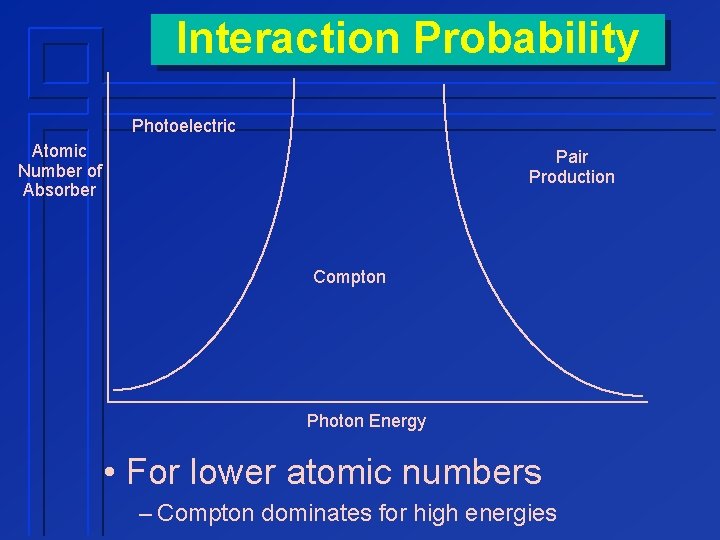
Interaction Probability Photoelectric Atomic Number of Absorber Pair Production Compton Photon Energy • For lower atomic numbers – Compton dominates for high energies
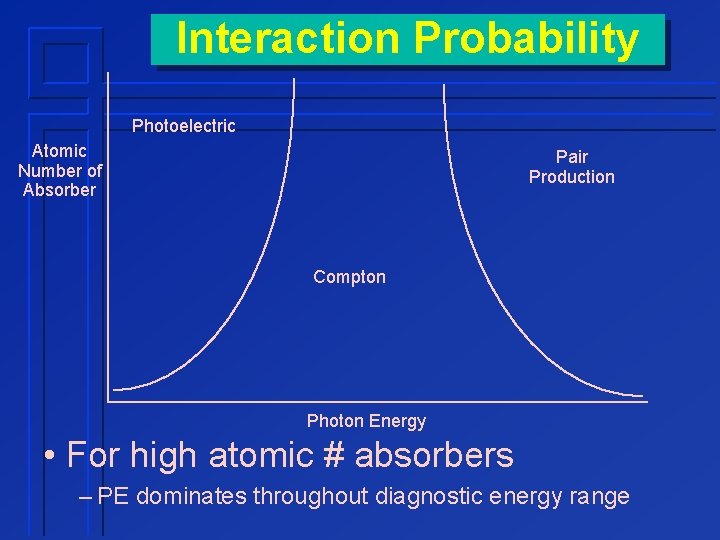
Interaction Probability Photoelectric Atomic Number of Absorber Pair Production Compton Photon Energy • For high atomic # absorbers – PE dominates throughout diagnostic energy range

Attenuation & Density • Attenuation proportional to density ¨difference in tissue densities accounts for much of optical density difference seen radiographs • # of Compton interactions depends on electrons / unit path ¨which depends on » electrons per gram » density

Relationships • Density generally increases with atomic # ¨different states = different density » ice, water, steam • no relationship between density and electrons per gram • atomic # vs. electrons / gram ¨hydrogen ~ 2 X electrons / gram as most other substances ¨as atomic # increases, electrons / gram decreases slightly
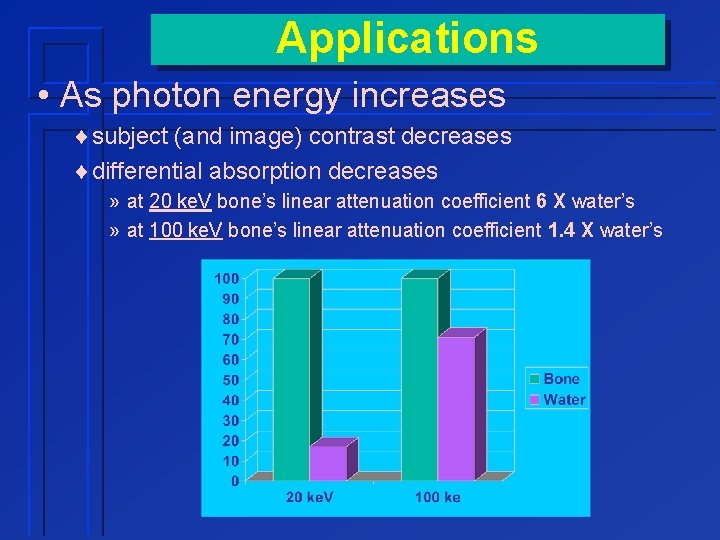
Applications • As photon energy increases ¨subject (and image) contrast decreases ¨differential absorption decreases » at 20 ke. V bone’s linear attenuation coefficient 6 X water’s » at 100 ke. V bone’s linear attenuation coefficient 1. 4 X water’s

Applications Photoelectric Pair Production Compton • At low x-ray energies ¨attenuation differences between bone & soft tissue primarily caused by photoelectric effect » related to atomic number & density
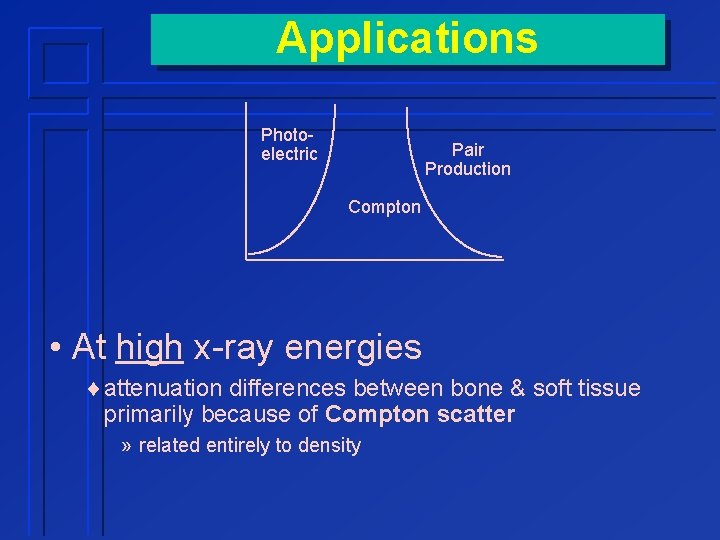
Applications Photoelectric Pair Production Compton • At high x-ray energies ¨attenuation differences between bone & soft tissue primarily because of Compton scatter » related entirely to density

Applications • Difference between water & fat only visible at low energies ¨effective atomic # of water slightly higher » yields photoelectric difference ¨electrons / cm almost equal » No Compton difference ¨Photoelectric dominates at low energy

Scatter Radiation • NO Socially Redeeming Qualities ¨no useful information on image ¨detracts from film quality ¨exposes personnel, public • represents 50 -90% of photons exiting patient

Abdominal Photons • ~1% of incident photons on adult abdomen reach film • fate of the other 99% ¨mostly scatter » most do not reach film ¨absorption

Scatter Factors • Factors affecting scatter ¨field size ¨thickness of body part ¨k. Vp An increase in any of above increases scatter.
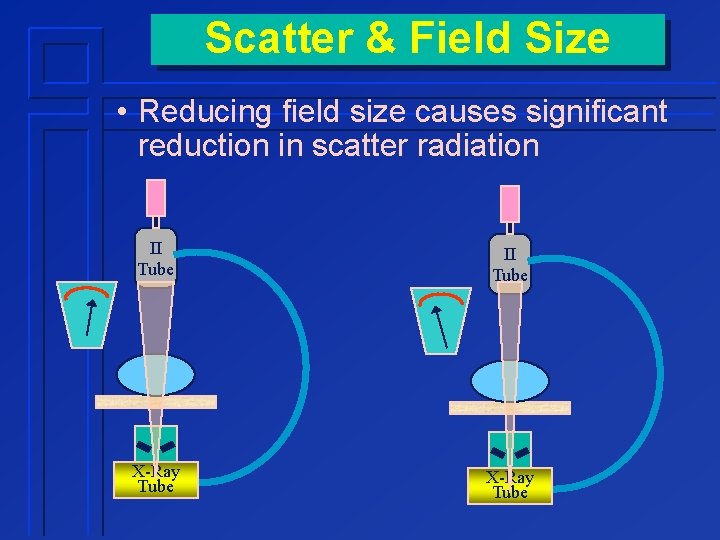
Scatter & Field Size • Reducing field size causes significant reduction in scatter radiation II Tube X-Ray Tube

Field Size & Scatter • Field Size & thickness determine volume of irradiated tissue • Scatter increase with increasing field size ¨initially large increase in scatter with increasing field size ¨saturation reached (at ~ 12 X 12 inch field) » further field size increase does not increase scatter reaching film » scatter shielded within patient

Thickness & Scatter • Increasing patient thickness leads to increased scatter but • saturation point reached ¨scatter photons produced far from film ¨shielded within body

k. Vp & Scatter • k. Vp has less effect on scatter than ¨ field size ¨ thickness • Increasing k. Vp ¨ increases scatter ¨ more photons scatter in forward direction

Scatter Management • Reduce scatter by minimizing ¨field size » within limits of exam ¨thickness » mammography compression ¨k. Vp » but low k. Vp increases patient dose » in practice we maximize k. Vp

Scatter Control Techniques: Grid • directional filter for photons • Increases patient dose
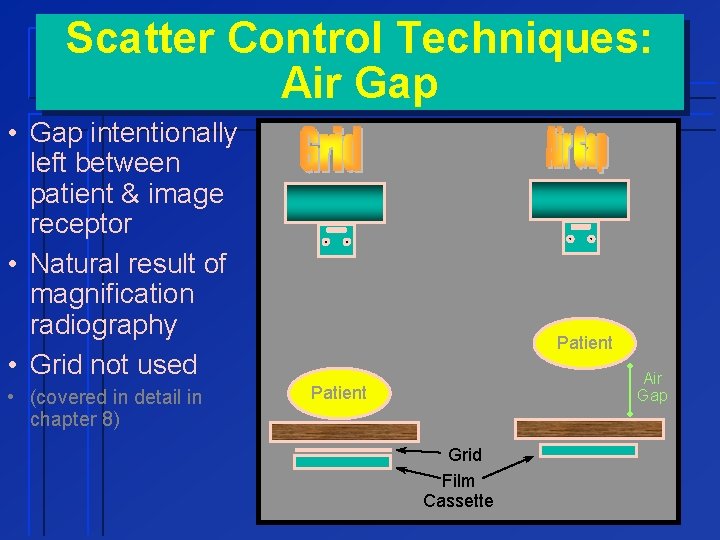
Scatter Control Techniques: Air Gap • Gap intentionally left between patient & image receptor • Natural result of magnification radiography • Grid not used • (covered in detail in chapter 8) Patient Air Gap Patient Grid Film Cassette

Resident Physics Lectures • Christensen, Chapter 8 Grids George David Associate Professor Department of Radiology Medical College of Georgia

Purpose • Directional filter for photons • Ideal grid Focal Spot “Good” photon ¨passes all primary photons » photons coming from focal spot ¨blocks all secondary photons » photons not coming from focal spot Patient “Bad” photon XGrid Film

Grid Construction • Lead ~. 05“ thick upright strips (foil) • Interspace ¨ material between lead strips ¨ maintains lead orientation ¨ materials » fiber » aluminum » wood Lead Interspace

Grid Ratio • Ratio of interspace height to width Lead Interspace h w Grid ratio = h / w

Grid Ratio • Expressed as X: 1 • Typical values 8: 1 to 12: 1 for general work 3: 1 to 5: 1 for mammography • Grid function generally improves with higher ratios h w Grid ratio = h / w

Lines per Inch • # lead strips per inch grid width • Typical: 103 W 25. 4 Lines per inch = ------W+w w = thickness of interspace (mm) W = thickness of lead strips (mm) w
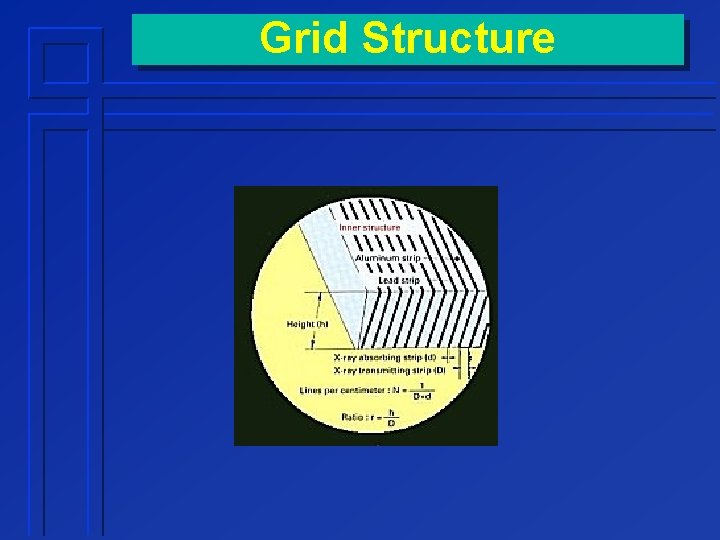
Grid Structure
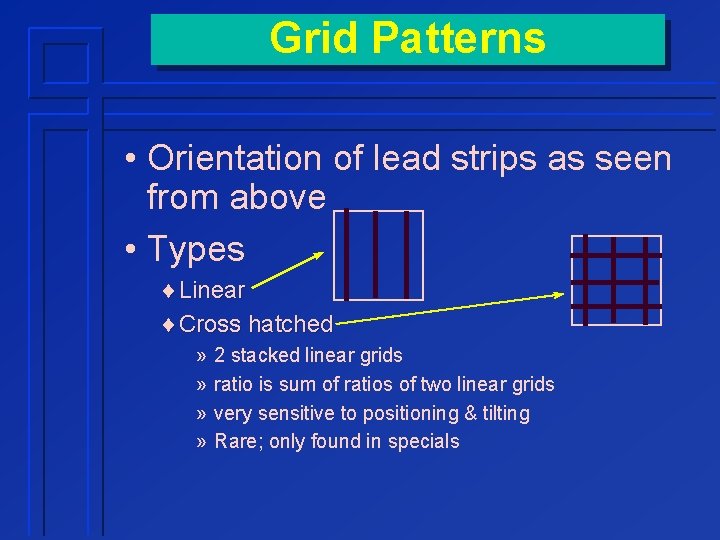
Grid Patterns • Orientation of lead strips as seen from above • Types ¨Linear ¨Cross hatched » » 2 stacked linear grids ratio is sum of ratios of two linear grids very sensitive to positioning & tilting Rare; only found in specials
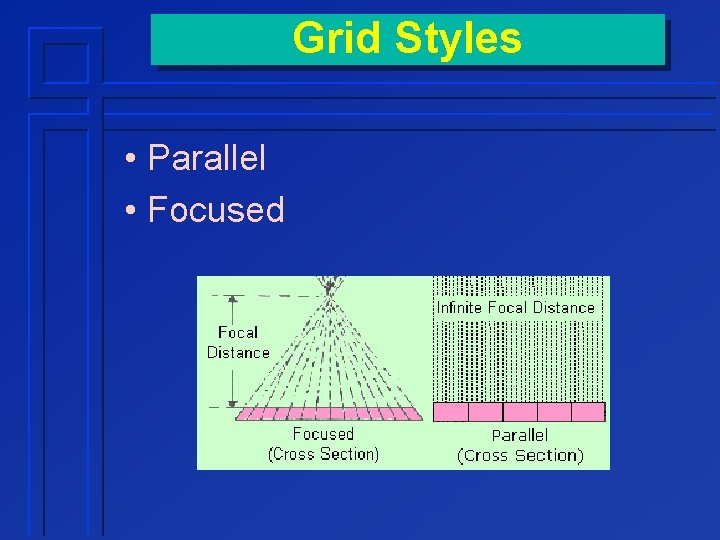
Grid Styles • Parallel • Focused
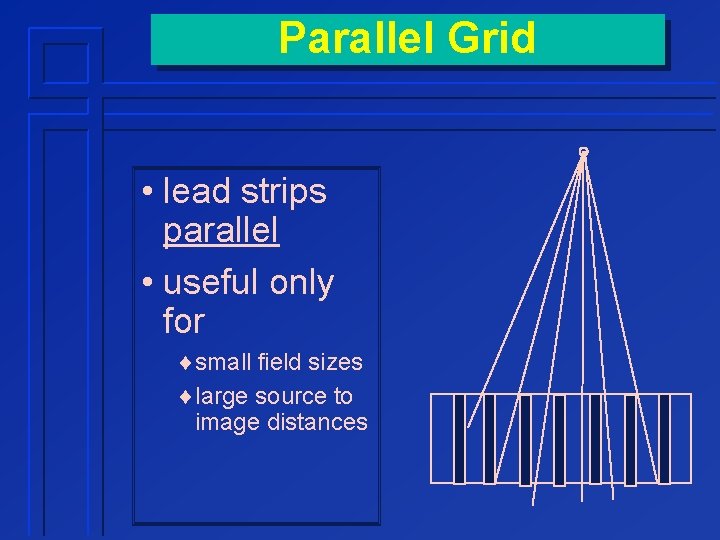
Parallel Grid • lead strips parallel • useful only for ¨small field sizes ¨large source to image distances
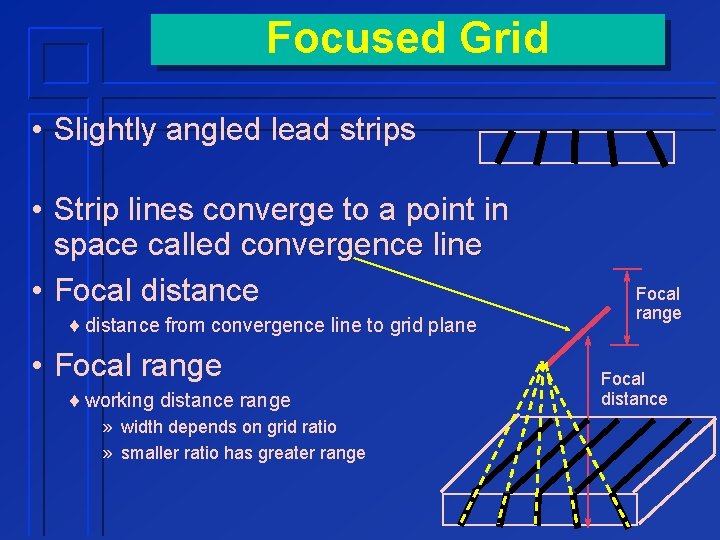
Focused Grid • Slightly angled lead strips • Strip lines converge to a point in space called convergence line • Focal distance ¨ distance from convergence line to grid plane • Focal range ¨ working distance range » width depends on grid ratio » smaller ratio has greater range Focal distance

Grid Cassette • Grid built into cassette front • Sometimes used for portables ¨formerly used in mammography • low grid ratios • focused

Ideal Grid • passes all primary radiation ¨Reality: lead strips block some primary Lead Interspace

Ideal Grid • block all scattered radiation ¨Reality: lead strips permit some scatter to get through to film Lead Interspace

Grid Performance Measurements • Primary Transmission (Tp) • Bucky Factor (B) • contrast improvement factor (K)

Resident Physics Lectures • Christensen, Chapter 6 Filters George David Associate Professor Department of Radiology Medical College of Georgia
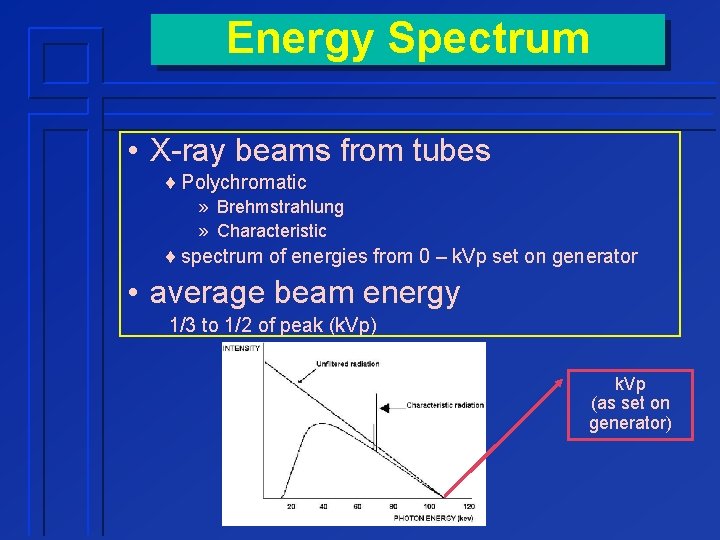
Energy Spectrum • X-ray beams from tubes ¨ Polychromatic » Brehmstrahlung » Characteristic ¨ spectrum of energies from 0 – k. Vp set on generator • average beam energy 1/3 to 1/2 of peak (k. Vp) k. Vp (as set on generator)

Unfiltered Beams • most energy deposited in first few centimeters of tissue ¨lowest energy photons selectively removed • energy of low energy photons ¨contributes to dose ¨does not contribute to image Patient » photons don’t reach film

Ideal Filtration • absorption characteristics ¨absorbs all low energy radiation ¨absorbs no high energy radiation • high atomic number desirable ¨increases photoelectric absorption of low energy photons

Filter’s Function • shape beam’s energy Filter spectrum • selectively attenuate low energy photons ¨less low energy radiation incident on patient ¨energy deposited in filter, not in patient Film
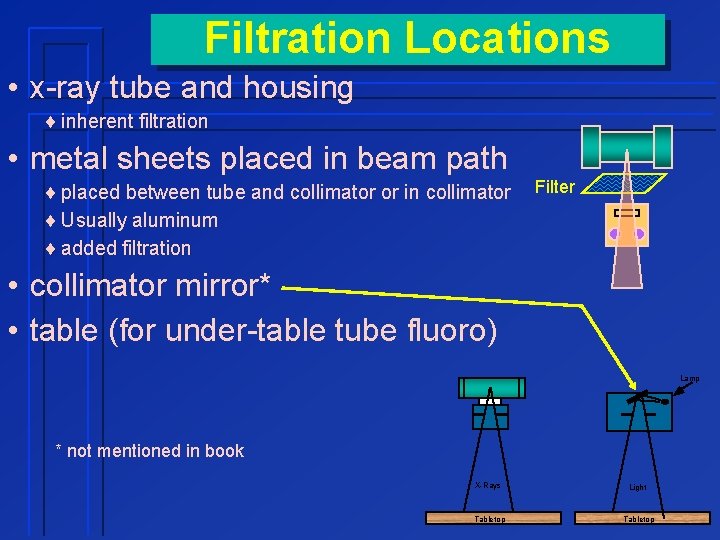
Filtration Locations • x-ray tube and housing ¨ inherent filtration • metal sheets placed in beam path ¨ placed between tube and collimator or in collimator ¨ Usually aluminum ¨ added filtration Filter • collimator mirror* • table (for under-table tube fluoro) Lamp * not mentioned in book X-Rays Light Tabletop
- Slides: 94