Research shows that the incidence of epilepsy is







































- Slides: 47


� Research shows that the incidence of epilepsy is higher in the elderly. � Epilepsy was believed to be predominantly a childhood disorder. � Epilepsy is the most common serious neurological disorder in the elderly after stroke and dementia.

US census projections � 147 percent increase in the over 65 years old population between 2000 -2050 � Only 49 percent in population over the same period.

� Elderly people with epilepsy are a large but neglected group. � In a postal survey 25% of general practitioners were unaware that epilepsy commonly manifests for first time in elderly.


� The prevalence and incidence of epilepsy are highest in later life!! � Approximately � 25% 7% of seniors have epilepsy. of new cases occur in elderly

� 5· 15 per 1000 people. � Children � 5– 9 years: 3· 16 � 10– 14 years: 4· 05 � Elderly � 65– 69 years : 6· 01 � 70– 74 years : 6· 53 � 75– 79 years : 7· 39 � 80– 84 years : 7· 54 � 85 years and older : 7· 73

� 80· 8 per 100 000 people � children � 5– 9 years: 63· 2 � 10– 14 years : 53· 8 � Elderly � 65– 69 years: 85· 9 � 70– 74 years: 82· 8 � 75– 79 years: 114· 5 � 80– 84 years: 159 �� 85 years: 135· 4

� PROVOKED SEIZURES � UNPROVOKED SEIZURES.

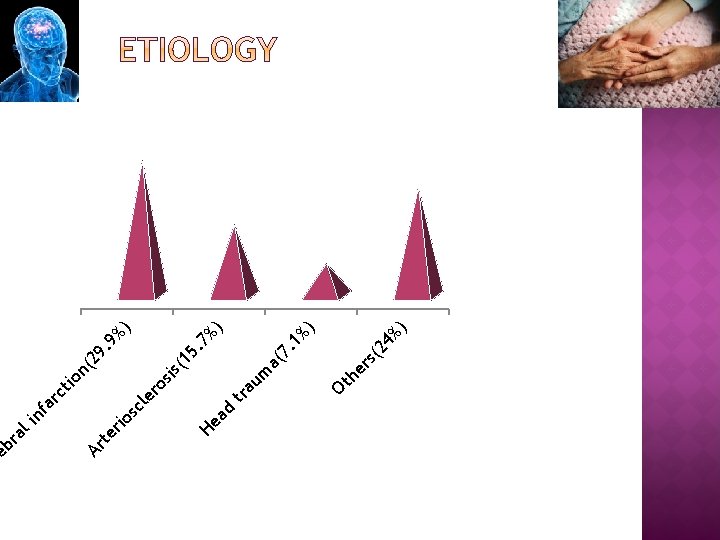
He a d ) 24 % s( he r Ot 1% ) 7. m a( au tr . 7 %) 15 is( ro s ) 9% 9. n( 2 rc tio le sc io nf a li er Ar t re br a

� Stroke is the leading cause of new-onset epilepsy in elderly 8% of patients will hemorrhagic stroke will develop seizures within two weeks � 5% of patients with ischemic stroke will develop seizures with in 2 weeks. � � Post-stroke epilepsy usually develops within 3 – 12 months � However, can still occur many years later

� 10– 20% � Less of all epilepsy in older people. appreciated is the evidence suggesting that dementia may develop with greater frequency elderly with chronic and established epilepsy.

� Post-traumatic epilepsy is common in elderly � Head injury, mostly from falls, causes up to 20% of epilepsy in the elderly. � Increased risk of subdural hemorrhage, especially with anticoagulants or platelet inhibitors. � Factors that increase risk of post-traumatic epilepsy � Loss of consciousness � Post-traumatic amnesia > 24 hrs. � Skull fracture, brain contusion and subdural hematoma.

� Seizures may be the presenting feature of tumors at any age. � The most common tumors causing seizures are gliomas, meningiomas and metastases.

� Seizures may be the first presentation of metastatic disease � In one study 43% of those presenting with seizures from metastases had no previous systemic diagnosis of cancer.

� Acute symptomatic seizures. � Often a reversible cause. � By definition, these are not epilepsy.

� Common causes � � acute alcohol withdrawal metabolic and electrolyte disturbances Hyponatremia Hypocalcemia Hypomagnesemia � Infections systemic CNS. � Drugs - commonly prescribed to elderly. Tramadol Antipsychotics Antidepressants (particularly tricyclics) Antibiotics(quinolones and macrolide) Theophylline, levodopa, thiazide diuretics and even the herbal remedy, ginkgo biloba

� The presentation of epilepsy in old age is often less specific. � It may take time before a firm diagnosis can be reached. � Under diagnosis and misdiagnosis are common.

� 70% of seizures are of focal onset. � Focal or complex partial seizures �Memory lapses, �Episodes of confusion �Periods of inattention �Apparent syncope. � Late onset idiopathic generalized epilepsy cases are occasionally seen.

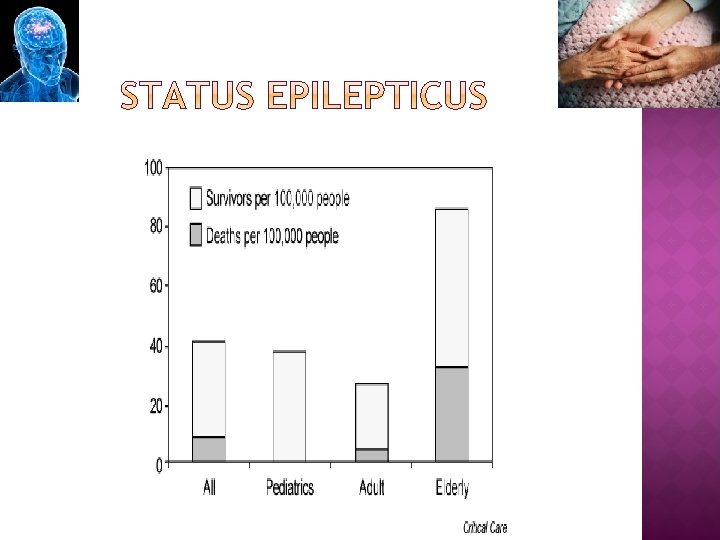
Status epilepticus (SE) is a serious condition of prolonged or repetitive seizures. � The annual incidence is 86/100, 000 > 60 Yrs. � It is almost twice that of the general population. �Over half of patients with SE do not have a diagnosis of epilepsy and often it is precipitated by an acute illness.


Cerebrovascular accident (CVA) 21% � Remote symptomatic (mainly previous CVA) 21% � Low anticonvulsant drug concentrations 21% � Hypoxia 17% � Metabolic 14% � Alcohol 11% � Tumor 10% � Infection 6% � Anoxia 6% � Hemorrhage 5% � CNS infection 5% � Trauma 1% � Idiopathic 1% � Other 1% �

� NCSE accounts for about 4 -20% of all cases of SE. � Only one third of the patients with NCSE had a history of epilepsy. � High mortality of about 50%. � Veterans Affairs studies found that 65% of the patients with NCSE died within 30 days of an episode compared to 27% of patients with GCSE.

� Impairment of cognition, Behavioral change. � Psychomotor retardation � Agitation or excitation � Subtle facial or limb twitches � Aphasia, echolalia, confabulation � Head or eye deviation � Automatisms � Autonomic disturbance

SEIZURE OR NOT A SEIZURE

�Neurological � Transient ischemic attack � Transient global amnesia � Migraine � Narcolepsy � Restless legs syndrome �Cardiovascular � Vasovagal syncope � Orthostatic hypotension � Cardiac arrhythmias � Structural heart disease � Carotid sinus syndrome

�Endocrine/metabolic � Hypoglycaemia � Hyponatraemia � Hypokalaemia � Sleep disorders � Obstructive sleep apnea � Hypnic jerks � Rapid eye movement sleep disorders � Psychological � Non-epileptic psychogenic seizures


� Diagnosing epilepsy can be more difficult and more time consuming in elderly. �Atypical presentation. �Potential mimics �Higher prevalence of comorbidities

� Only 24% of patients were initially diagnosed with epilepsy when they presented to their health care providers. � It took a mean of 19 months from the time the seizures began to the time epilepsy was correctly diagnosed.

� History � Clinical Exam � Investigations: �Blood work full blood count, renal function testing, serum electrolytes, and random blood glucose. 1 �EKG, Holter monitoring and tilt table in some cases. �Chest X ray �EEG �Neuroimaging studies

� Provoked seizures - treat the underlying cause. � Unprovoked treatment. Seizures - antiepileptic drug


� Start treatment after a single unprovoked seizure ? Remains controversial.

� Older people who present with a first unprovoked seizure are more likely to develop seizure recurrence than are younger adults. � Cause identified in more than 60% of elderly people with epilepsy.

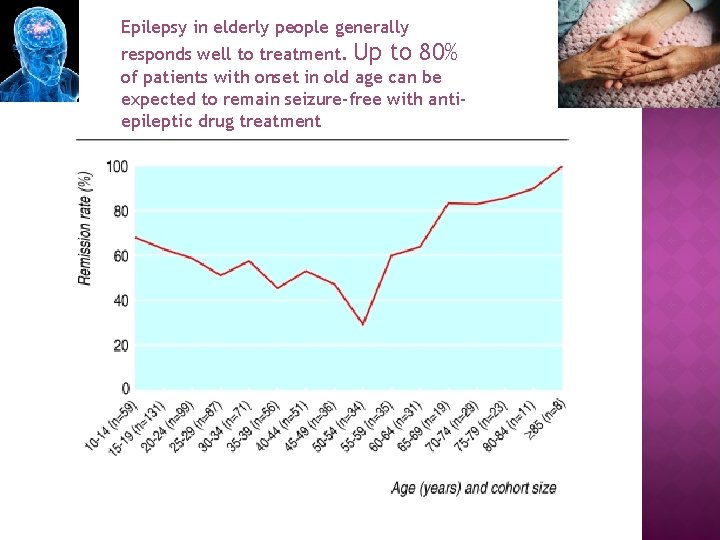
Epilepsy in elderly people generally responds well to treatment. Up to 80% of patients with onset in old age can be expected to remain seizure-free with antiepileptic drug treatment

� Treatment decisions have to be made Cautiously. �Elderly are more susceptible to the adverse effects of drugs than their younger counterparts �The pharmacokinetics and pharmacodynamics of antiepileptic drugs differ in old age �Drug-drug interactions

Pharmacokinetic and pharmacodynamic alteration of aging. � Decreased Drug absorption � Delayed esophageal emptying � Altered gastric p. H � Delayed gastric emptying � Increased intestinal transit time � Drug distribution � Decreased albumin and decreased of protein binding � Decreased body fat Metabolism and excretion. � Decreased hepatic metabolism � Decreased renal clearance

� Reasonable to assume that antiepileptic treatment will be life-long. � Ideal AED choice �Most likely achieves seizure freedom with the fewest side effects. �Be well tolerated, have a limited side-effect profile. �Easy dosing. �Free of troublesome drug–drug interactions. � ‘Start low and go slow'

� Very narrow evidence based data is available for managing newly-diagnosed epilepsy in the elderly � Even less information is available on newer drugs, such as levetiracetam or oxcarbazepine, in elderly populations.

Older AEDs � Benzodiazepines � Acute use � Status epilepticus � Idiosyncratic reactions, psychosis and sedation � Phenobarbital � Broad spectrum � Once-daily dosing Significant adverse event profile � Requires very slow dose titration � Phenytoin � Acute use � Status epilepticus � 'Zero-order' kinetics, so care is needed in making dose changes � Enzyme inducer � Interacts with digoxin and warfarin � Carbamazepine � Effective in partial-onset seizures � Enzyme inducer so interacts with other AEDs, some antibiotics and warfarin � Hyponatremia can occur, especially with diuretics � Sodium valproate � Effective in generalized-onset seizures � Enzyme inhibitor. . � Few interactions Ataxia and tremor may be troublesome in elderly � Reversible extrapyramidal symptoms

NEWER AEDS � � � Lamotrigine (Lamictal) � Effective in partial-onset seizures and generalized seizures. Mood stabilizer � Requires slow-dose titration to avoid serious allergic rash. � Very slow titration especially in patients already taking sodium valproate Oxcarbazepine (Trileptal) � Few interactions. Well tolerated � Hyponatremia can occur, especially with diuretics Levetiracetam (Keppra) � Inert metabolites � Lack of drug interactions � Mood and behavioral disturbances occur occasionally Topiramate (Topamax) � Seizures and migraine prophylaxis. � Requires slow dose titration � Can cause weight loss and cognitive problems. Zonisamide (Zonegran) � Better side effect profile compared to Topamax.

NEWER AEDS � � � Gabapentin (Neurontin) � Also used for neuropathic pain. Limited efficacy in epilepsy. � Can be used in liver dysfunction � Can cause dizziness, sedation and weight gain Pregabalin (lyrica) � Also Used for neuropathic pain � Can be used in liver dysfunction � Lack of drug interactions � Can cause dizziness and weight gain, motor and cognitive slowing Lacosamide (Vimpat) � Partial Epilepsy � Increased risk of PR interval elongation on electrocardiogram. � Contraindicated in second- and third-degree AV block

� Comorbidities of in elderly patients add to the diagnostic challenge and also complicate the treatment options � Polypharmacy make them susceptible to drug interactions. � A survey of elderly nursing home residents found that 49% of residents receiving AEDs were prescribed six or more medications. � Adherence may not be as good in elderly patients with epilepsy.

�Surgery �VNS

Development of epilepsy is common in later life. � The number of elderly with epilepsy will rise further. placing an increasing burden on healthcare resources � Epilepsy can have a profound physical and psychological impact in old age, with a substantial negative effect on quality of life � Be aware of Mimics � Most elderly people with epilepsy can remain seizurefree with appropriate treaments. � Attention should be paid to side effects and potential for drug-drug interactions �
