Reprocessing Flexible Endoscopes Whats New William A Rutala

Reprocessing Flexible Endoscopes: What’s New William A. Rutala, Ph. D. , M. P. H. Director, Hospital Epidemiology, Occupational Health and Safety Program, UNC Health Care; Professor of Medicine, Director, Statewide Program for Infection Control and Epidemiology, University of North Carolina (UNC) at Chapel Hill, NC, USA

DISCLOSURES l l Consultation and Honoraria n ASP (Advanced Sterilization Products), Clorox Honoraria n 3 M Grants n CDC, CMS No funds from Medivator, session sponsor

Reprocessing Flexible Endoscopes Objectives Risks associated with reprocessing flexible endoscopes l Causes of contamination and infection l Gaps in current reprocessing standards l Establish scientific rationale and evidence requirements for enhancing safe practices l

Reprocessing Flexible Endoscopes Topics l l l l Risks associated with reprocessing flexible endoscopes Audits-cleaning (ATP) and microbiological sampling Outbreaks when no reprocessing deficiencies identified Patient notification after failure to follow guidelines Endoscopes reprocessed if unused at 5 days Human papilloma virus C. difficile spores Biofilms Unsafe injection practices Reprocessing steps performed in compliance with guidelines AERs Newer high-level disinfectants Fecal transplants

Reprocessing Flexible Endoscopes Objectives l Risks associated with reprocessing flexible endoscopes n Margin of safety and evidence of transmission, patient notification Causes of contamination and infection l Gaps in current reprocessing standards l Establish scientific rationale and evidence requirements for enhancing safe practices l
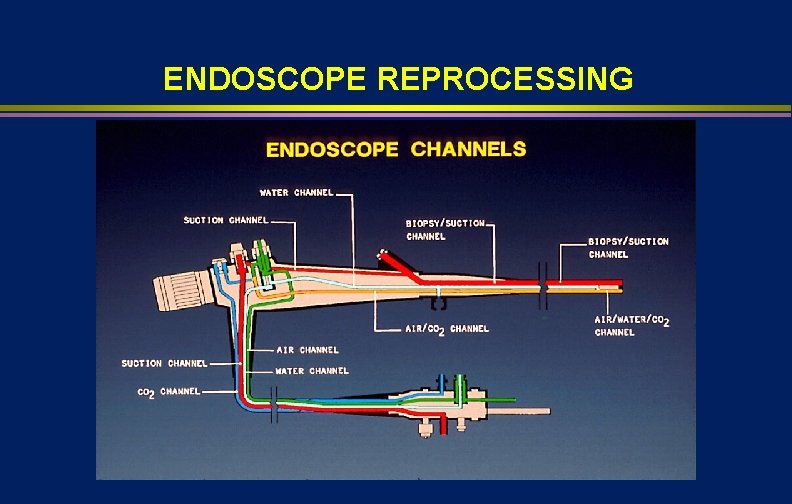
ENDOSCOPE REPROCESSING

Disinfection and Sterilization EH Spaulding believed that how an object will be disinfected depended on the object’s intended use. CRITICAL - objects which enter normally sterile tissue or the vascular system or through which blood flows should be sterile. SEMICRITICAL - objects that touch mucous membranes or skin that is not intact require a disinfection process (high-level disinfection [HLD]) that kills all microorganisms but high numbers of bacterial spores. NONCRITICAL -objects that touch only intact skin

ENDOSCOPES l l l Widely used diagnostic and therapeutic procedure (1122 million GI procedures annually in the US) GI endoscope contamination during use (109 in/105 out) Semicritical items require high-level disinfection minimally Inappropriate cleaning and disinfection has lead to cross-transmission In the inanimate environment, although the incidence remains very low, endoscopes represent a significant risk of disease transmission

Endoscope Reprocessing: Current Status of Cleaning and Disinfection l Guidelines n Multi-Society Guideline, 12 professional organizations, 2011 n Centers for Disease Control and Prevention, 2008 n Society of Gastroenterology Nurses and Associates, 2010 n AAMI Technical Information Report, Endoscope Reprocessing, In preparation n Food and Drug Administration, 2009 n Endoscope Reprocessing, Health Canada, 2010 n Association for Professional in Infection Control and Epidemiology, 2000

MULTISOCIETY GUIDELINE ON REPROCESSING GI ENDOSCOPES, 2011 Petersen et al. ICHE. 2011; 32: 527

ENDOSCOPE REPROCESSING Multi-Society Guideline on Endoscope Reprocessing, 2011 l l l PRECLEAN-point-of-use (bedside) remove debris by wiping exterior and aspiration of detergent through air/water and biopsy channels; leak test CLEAN-mechanically cleaned with water and enzymatic cleaner HLD/STERILIZE-immerse scope and perfuse HLD/sterilant through all channels for exposure time (>2% glut at 20 m at 20 o. C). If AER used, review model-specific reprocessing protocols from both the endoscope and AER manufacturer RINSE-scope and channels rinsed with sterile water, filtered water, or tap water. Flush channels with alcohol and dry DRY-use forced air to dry insertion tube and channels

Disinfection and Sterilization EH Spaulding believed that how an object will be disinfected depended on the object’s intended use. CRITICAL - objects which enter normally sterile tissue or the vascular system or through which blood flows should be sterile. SEMICRITICAL - objects that touch mucous membranes or skin that is not intact require a disinfection process (high-level disinfection [HLD]) that kills all microorganisms but high numbers of bacterial spores. NONCRITICAL -objects that touch only intact skin


Critical Items Sterilization-Huge Margin of Safety l l l Huge margin of safety associated with sterilization of critical items Surgical instrument contaminated with <100 microorganisms Decontamination by washer-disinfector eliminates >5 logs (or 100, 000 fold reduction) Sterilization processes inactivate 12 logs of spores (or 1, 000, 000 spores) Unlikely sterilized instrument will transmit infection when compliant with recommendations

FEATURES OF ENDOSCOPES THAT PREDISPOSE TO DISINFECTION FAILURES l l l Require low temperature disinfection Long narrow lumens Right angle turns Blind lumens May be heavily contaminated with pathogens, 109 Cleaning (4 -6 log 10 reduction) and HLD (4 -6 log 10 reduction) essential for patient safe instrument

GI Endoscopes HLD-Narrow Margin of Safety l l l Narrow margin of safety associated with highlevel disinfection of semicritical items Instrument contaminated with 1, 000, 000 microorganisms Cleaning eliminates ~5 logs (or 100, 000 fold reduction) High-level disinfection process inactivates ~ 5 logs of microbes (100, 000 fold) Likely exposed to previous patient’s pathogens if reprocessing protocol is not followed precisely
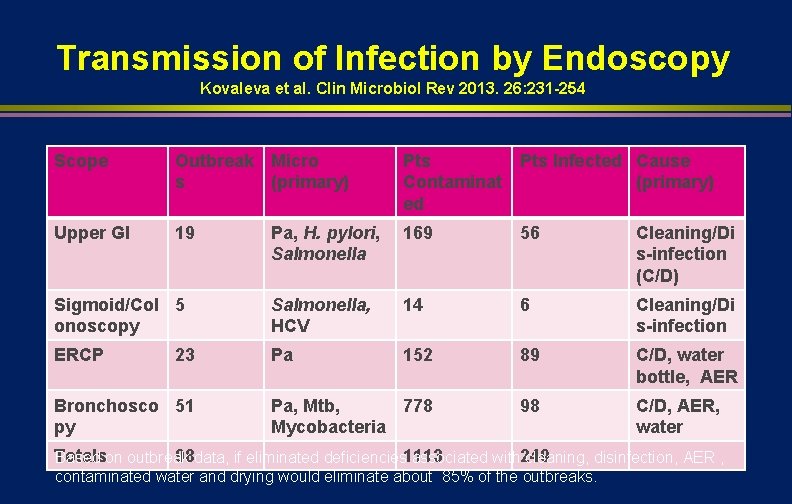
Transmission of Infection by Endoscopy Kovaleva et al. Clin Microbiol Rev 2013. 26: 231 -254 Scope Outbreak Micro s (primary) Pts Infected Cause Contaminat (primary) ed Upper GI 19 Pa, H. pylori, Salmonella 169 56 Cleaning/Di s-infection (C/D) Sigmoid/Col 5 onoscopy Salmonella, HCV 14 6 Cleaning/Di s-infection ERCP Pa 152 89 C/D, water bottle, AER Pa, Mtb, 778 Mycobacteria 98 C/D, AER, water 23 Bronchosco 51 py Totals 98 data, if eliminated deficiencies 1113 Based on outbreak associated with 249 cleaning, disinfection, AER , contaminated water and drying would eliminate about 85% of the outbreaks.

TRANSMISSION OF INFECTION l Gastrointestinal endoscopy n n n l Bronchoscopy n n l >150 infections transmitted Salmonella sp. and P. aeruginosa Clinical spectrum ranged from colonization to death (~4%) ~100 infections transmitted M. tuberculosis, atypical Mycobacteria, P. aeruginosa Endemic transmission may go unrecognized (e. g. , inadequate surveillance, low frequency, asymptomatic infections)

Endoscope Reprocessing, Worldwide l Worldwide, endoscopy reprocessing varies greatly India, of 133 endoscopy centers, only 1/3 performed even a minimum disinfection (1% glut for 2 min) n Brazil, “a high standard …occur only exceptionally” n Western Europe, >30% did not adequately disinfect n Japan, found “exceedingly poor” disinfection protocols n US, 25% of endoscopes revealed >100, 000 bacteria n Schembre DB. Gastroint Endoscopy 2000; 10: 215

Nosocomial Infections via GI Endoscopes l Infections traced to deficient practices n Inadequate cleaning (clean all channels) n Inappropriate/ineffective disinfection (time exposure, perfuse channels, test concentration, ineffective disinfectant, inappropriate disinfectant) n Failure to follow recommended disinfection practices (tapwater rinse) n Flaws and complexity in design of endoscopes or AERs




Reprocessing Flexible Endoscopes Objectives Risks associated with reprocessing flexible endoscopes l Causes of contamination and infection l n Complex device/complex reprocessing Gaps in current reprocessing standards l Establish scientific rationale and evidence requirements for enhancing safe practices l

FEATURES OF ENDOSCOPES THAT PREDISPOSE TO DISINFECTION FAILURES l l l Require low temperature disinfection Long narrow lumens Right angle turns Blind lumens May be heavily contaminated with pathogens, 109 Cleaning (4 -6 log 10 reduction) and HLD (4 -6 log 10 reduction) essential for patient safe instrument

Multi-Society Guideline for Reprocessing Flexible Gastrointestinal Endoscopes, 2011 l Transmission categorized as: n Non-endoscopic and related to care of intravenous lines and administration of anesthesia or other medications u. Multidose vials u. Reuse of needles and syringes u. Intravenous sedation tubing n Endoscopic and related to endoscope and accessories u. Failure to sterilize biopsy forceps between patients u. Lapses in reprocessing tubing used in channel irrigation

HCV from Unsafe Injection Practices at an Endoscopy Clinic in Las Vegas, 2007 -2008 Fischer et al. Clin Infect Dis. 2010; 51; 267 l l Background-in January 2008, 3 persons with acute HCV underwent endoscopy at a single facility in Nevada. Method-reviewed clinical and laboratory data Results- 5 additional cases of HCV were identified and quasispecies analysis identified two clusters. 7/38 (17%) who followed source patient were HCV infected. Reuse of syringes on single patients with use of single-use propofol vials for multiple patients was observed. Conclusion- patient-to-patient transmission of HCV resulted from contamination of single-use medication vials that were used for multiple patients during anesthesia administration. The resulting notification of >50, 000 persons was the largest of its kind in US health care.
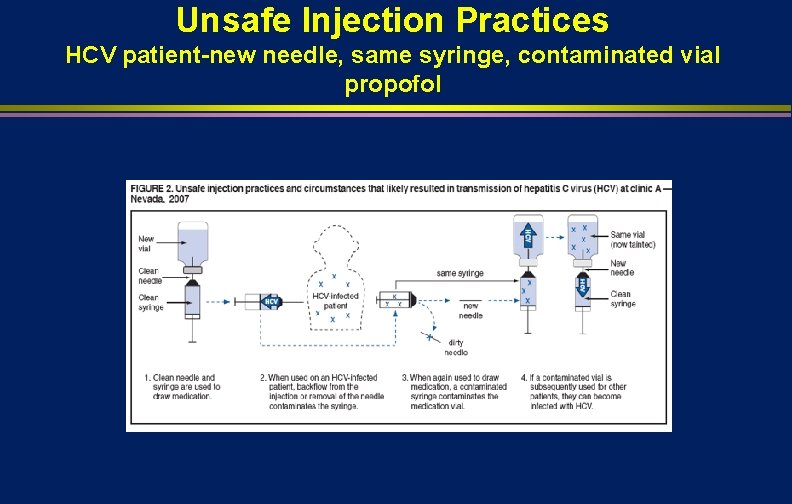
Unsafe Injection Practices HCV patient-new needle, same syringe, contaminated vial propofol

SAFE INJECTION PRACTICES

Endoscope Reprocessing Methods Ofstead , Wetzler, Snyder, Horton, Gastro Nursing 2010; 33: 204

Endoscope Reprocessing Methods Ofstead , Wetzler, Snyder, Horton, Gastro Nursing 2010; 33: 204 Performed all 12 steps with only 1. 4% of endoscopes using manual versus 75. 4% of those processed using AER
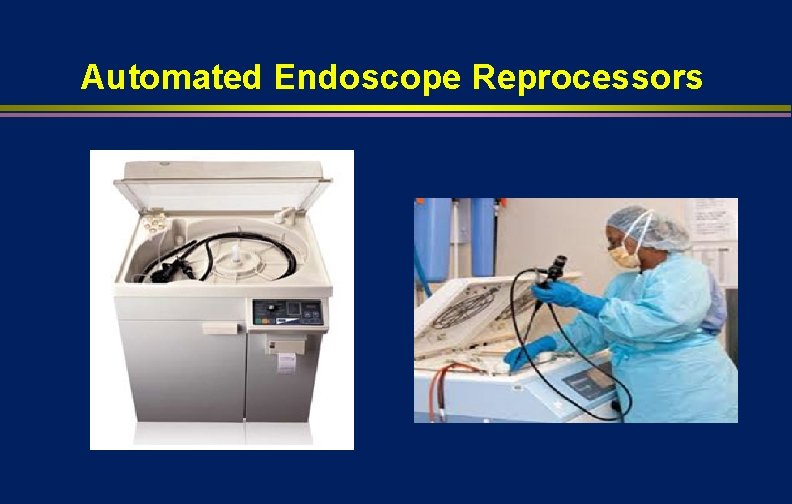
Automated Endoscope Reprocessors

Automated Endoscope Reprocessors (AER) l l l Manual cleaning of endoscopes is prone to error. AERs can enhance efficiency and reliability of HLD by replacing some manual reprocessing steps AER Advantages: automate and standardize reprocessing steps, reduce personnel exposure to chemicals, filtered tap water, reduce likelihood that essential steps will be skipped AER Disadvantages: failure of AERs linked to outbreaks, may not eliminate precleaning BMC Infect Dis 2010; 10: 200 Problems: incompatible AER (side-viewing duodenoscope); biofilm buildup; contaminated AER; inadequate channel connectors; used wrong set-up or connector MMWR 1999; 48: 557 Must ensure exposure of internal surfaces with HLD/sterilant

Automated Endoscope Reprocessors Gastro Endoscopy 2010; 72: 675 l l l All AERs have disinfection and rinsing cycles; some detergent cleaning; alcohol flush and/or forced-air drying Additional features may include: variable cycle times; printed documentation; HLD vapor recovery systems; heating; automated leak testing; automated detection of channel obstruction, MEC Not all AERs compatible with all HLDs or endoscopes; some models designed with specific HLDs Some AERs consume and dispose of HLD and other reuse HLD Some AERs have an FDA-cleared cleaning claim (eliminates soil and microbes equivalent to optimal manual cleaning-

Automated Endoscope Reprocessors with Cleaning Claim (requires procedure room pre-cleaning) Medivator Advantage Plus Endoscope Reprocessing System Evo-Tech (eliminates soil and microbes equivalent to optimal manual cleaning. BMC ID 2010; 10: 200)

ENDOSCOPE REPROCESSING: CHALLENGES NDM-Producing E. coli Associated ERCP MMWR 2014; 62: 1051 NDM-producing E. coli recovered from elevator channel

CHALLENGES NDM-Producing E. coli Associated ERCP MMWR 2014; 62: 1051 l l l March-July 2013, 9 patients with cultures for New Delhi Metallo-ß-Lactamase producing E. coli associated with ERCP History of undergoing ERCP strongly associated with cases NDM-producing E. coli recovered from elevator channel No lapses in endoscope reprocessing identified Hospital changed from automated HLD to ETO sterilization Due to either failure of personnel to complete required process every time or intrinsic problems with these scopes (not altered reprocessing)

CHALLENGES NDM-Producing E. coli Associated ERCP MMWR 2014; 62: 1051 l Recommendations n n Education/adherence monitoring u. Certification/competency testing of reprocessing staff Enforcement of best practices-preventive maintenance schedule Improved definition of the scope of the issue and contributing factors Development of innovative approaches to improve and assess the process u. Systematic assessment of the ability of AERs/technicians to clean/disinfect scopes u. Disinfection evaluation testing that relates to risk of

DECREASING ORDER OF RESISTANCE OF MICROORGANISMS TO DISINFECTANTS/STERILANTS Most Resistant Prions Spores (C. difficile) Mycobacteria Non-Enveloped Viruses (norovirus, polio, HPV, parvo) Fungi Bacteria (MRSA, VRE, Acinetobacter) Most Susceptible Enveloped Viruses
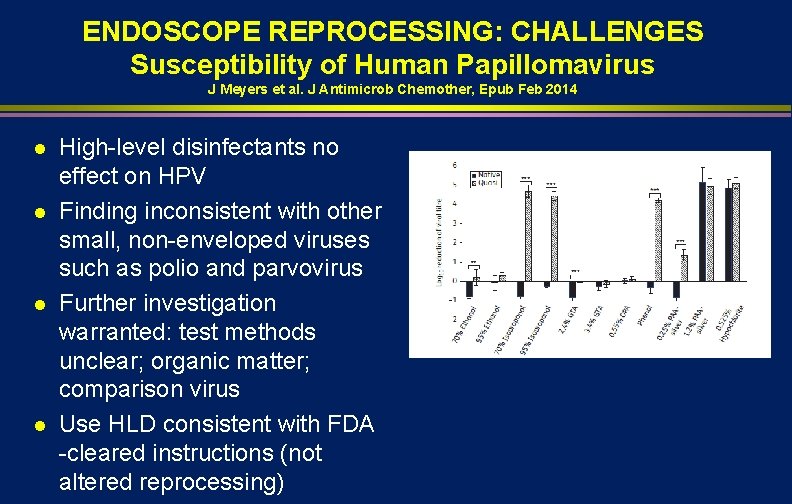
ENDOSCOPE REPROCESSING: CHALLENGES Susceptibility of Human Papillomavirus J Meyers et al. J Antimicrob Chemother, Epub Feb 2014 l l High-level disinfectants no effect on HPV Finding inconsistent with other small, non-enveloped viruses such as polio and parvovirus Further investigation warranted: test methods unclear; organic matter; comparison virus Use HLD consistent with FDA -cleared instructions (not altered reprocessing)

Monitoring Endoscope Cleaning

Endoscope Cleaning Endoscope must be cleaned using water with detergents or enzymatic cleaners before processing. l Cleaning reduces the bioburden and removes foreign material (organic residue and inorganic salts) that interferes with the HLD or sterilization process. l Cleaning and decontamination should be done as soon as possible after the items have been l
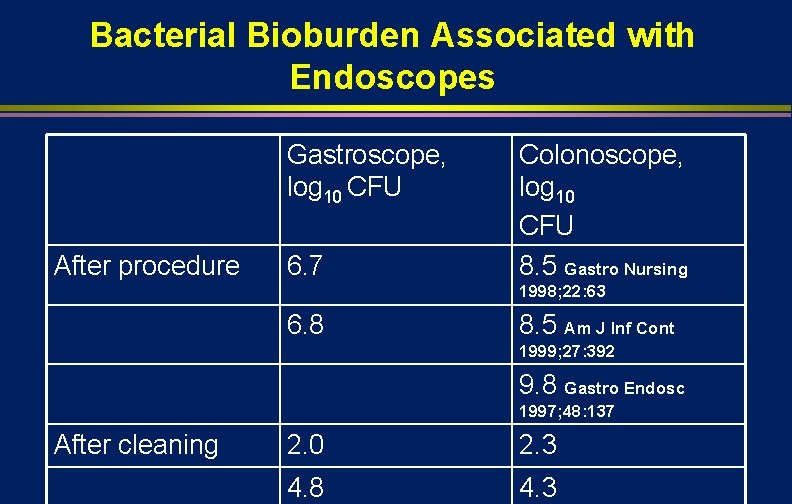
Bacterial Bioburden Associated with Endoscopes Gastroscope, log 10 CFU After procedure 6. 7 Colonoscope, log 10 CFU 8. 5 Gastro Nursing 1998; 22: 63 6. 8 8. 5 Am J Inf Cont 1999; 27: 392 9. 8 Gastro Endosc 1997; 48: 137 After cleaning 2. 0 2. 3 4. 8 4. 3
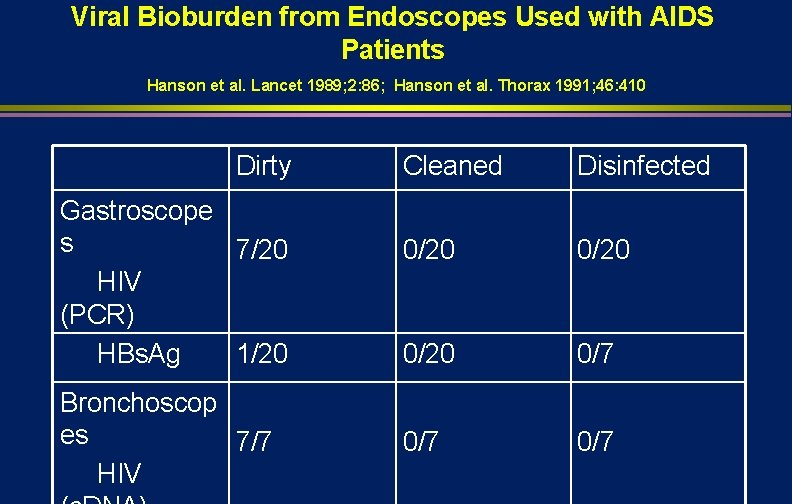
Viral Bioburden from Endoscopes Used with AIDS Patients Hanson et al. Lancet 1989; 2: 86; Hanson et al. Thorax 1991; 46: 410 Dirty Gastroscope s 7/20 HIV (PCR) HBs. Ag 1/20 Bronchoscop es 7/7 HIV Cleaned Disinfected 0/20 0/7 0/7

IS THERE A STANDARD TO DEFINE WHEN A DEVICE IS CLEAN? l l l There is currently no standard to define when a device is “clean”, cleanliness controlled by visual Potential methods: level of detectable bacteria; protein (6µg/cm 2); endotoxin; ATP; lipid This is due in part to the fact that no universally accepted test soils to evaluate cleaning efficiency and no standard procedure for measuring cleaning efficiency

Audit Manual Cleaning of Endoscopes Establishing Benchmarks Alfa et al. Am J Infect Control 2012; 40: 860. Rapid Use Scope Test detects organic residuals: protein (<6. 4µg/cm 2); hemoglobin (<2. 2. µg/cm 2); and carbohydrate (<1. 2µg/cm 2) n Alfa et al. Am J Infect Control 2013; 41: 245 -248. If <200 RLUs of ATP, the protein, hemoglobin and bioburden (<4 -log 10 CFU/cm 2 [>106 per scope]) were achieved. n Alfa et al. Am J Infect Control 2014; 42: e 1 -e 5. 200 RLU adequate for ATP. n

Audit Manual Cleaning of Endoscopes l Issues for consideration n What is the clinical importance of <6. 4µg/cm 2 for protein and <4 log 10 CFU/cm 2 bioburden: that is, has it been related epidemiologically or clinically to decrease or increase risk of infection? n ATP may be related to markers (e. g. , protein) but markers may have no relationship to microbes/disease and providing patient safe instrument. n Ideally, validation of benchmarks should include correlation with patients’ clinical outcome. The CDC has suggested that sampling be done when there are epidemiological data that demonstrate risk (e. g. , endotoxin testing and microbial
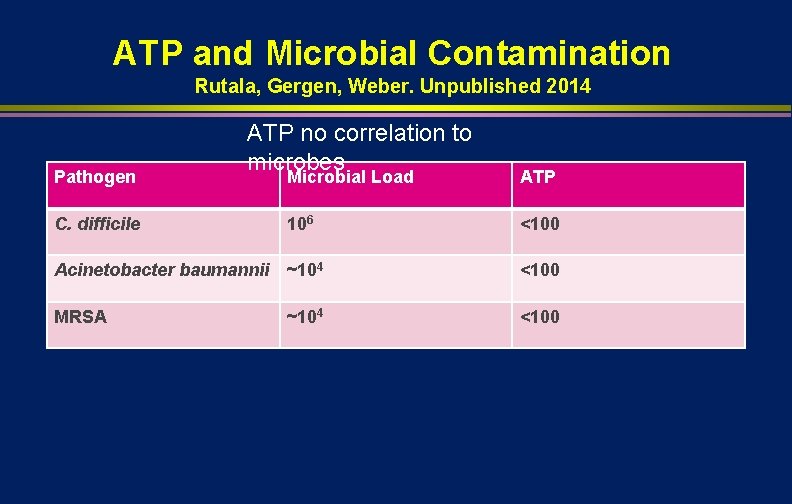
ATP and Microbial Contamination Rutala, Gergen, Weber. Unpublished 2014 Pathogen C. difficile ATP no correlation to microbes Microbial Load ATP 106 <100 Acinetobacter baumannii ~104 <100 MRSA <100 ~104

C. difficile: A GROWING THREAT
C. difficile spores

DECREASING ORDER OF RESISTANCE OF MICROORGANISMS TO DISINFECTANTS/STERILANTS Most Resistant Prions Spores (C. difficile) Mycobacteria Non-Enveloped Viruses (norovirus) Fungi Bacteria (MRSA, VRE, Acinetobacter) Most Susceptible Enveloped Viruses

C. difficile: MICROBIOLOGY AND EPIDEMIOLOGY l l l l l Gram-positive bacillus: Strict anaerobe, spore-former Colonizes human GI tract Increasing prevalence and incidence New epidemic strain that hyper-produces toxins A and B Causes virtually all cases of antibiotic-associated pseudomembranous colitis. Introduction of CDI from the community into hospitals High morbidity and mortality in elderly Inability to effectively treat fulminant CDI Absence of a treatment that will prevent recurrence of CDI

Disinfectants and Antiseptics C. difficile spores at 10 and 20 min, Rutala et al, 2006 l ~4 log 10 reduction (3 C. difficile strains including BI-9) Chlorine, 1: 10, ~6, 000 ppm chlorine (but not 1: 50, ~1, 200 ppm) n Chlorine, ~1, 910 ppm chlorine n Chlorine, ~25, 000 ppm chlorine n 0. 20% peracetic acid n 2. 4% glutaraldehyde n 2. 65% glutaraldehyde n 3. 4% glutaraldehyde and 26% alcohol n

Control Measures C. difficile l l No reports document the transmission of C. difficile by a GI endoscope. Current guidelines should be effective in preventing transmission via GI endoscope (i. e. , HLD such as glutaraldehyde and peracetic acid reliably kills C. difficile spores using normal exposure times)

BIOFILMS Pajkos, Vickery, Cossart. J Hosp Infect 2004; 58: 224
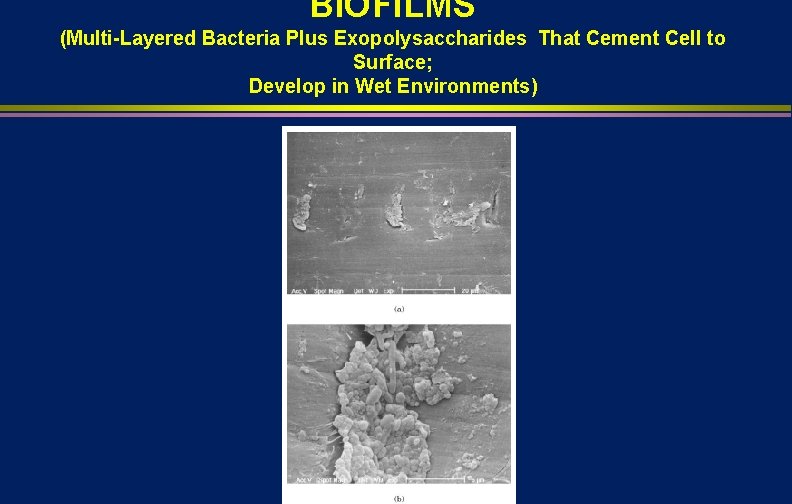
BIOFILMS (Multi-Layered Bacteria Plus Exopolysaccharides That Cement Cell to Surface; Develop in Wet Environments)

BIOFILMS (Multi-Layered Bacteria Plus Exopolysaccharides That Cement Cell to Surface; Develop in Wet Environments)

BIOFILMS l l l Bacteria residing within biofilms are many times more resistant to chemical inactivation than bacteria is suspension Does formation of biofilms within endoscopic channels contribute to failure of decontamination process? Not known Could be a reason for failure of adequate HLD processes but if reprocessing performed promptly after use and endoscope dry the opportunity for biofilm formation is minimal

Reprocessing Flexible Endoscopes Objectives Risks associated with reprocessing flexible endoscopes l Causes of contamination and infection l Gaps in current reprocessing standards l Establish scientific rationale and evidence requirements for enhancing safe practices l n New HLDs, TJC, AERs, reprocessing if unused for 5 -7 days, microbiologic sampling, fecal transplants

High-Level Disinfection of “Semicritical Objects” Exposure Time > 8 m-45 m (US), 20 o. C Germicide Concentration_____ Glutaraldehyde > 2. 0% Ortho-phthalaldehyde 0. 55% Hydrogen peroxide* 7. 5% Hydrogen peroxide and peracetic acid* 1. 0%/0. 08% Hydrogen peroxide and peracetic acid* 7. 5%/0. 23% Hypochlorite (free chlorine)* 650 -675 ppm Accelerated hydrogen peroxide 2. 0% Peracetic acid 0. 2% Glut and isopropanol 3. 4%/26% Glut and phenol/phenate** 1. 21%/1. 93%___ *May cause cosmetic and functional damage; **efficacy not verified

Resert. TM HLD l l High Level Disinfectant - Chemosterilant 2% hydrogen peroxide, in formulation n l p. H stabilizers Chelating agents Corrosion inhibitors Efficacy (claims need verification) n Sporicidal, virucidal, bactericidal, tuberculocidal, fungicidal HLD: 8 mins at 20 o. C l Odorless, non-staining, ready-to-use l No special shipping or venting requirements l Manual or automated applications l 12 -month shelf life, 21 days reuse l Material compatibility/organic material resistance *The (Fe, Accelerated Cu)? Hydrogen Peroxide technology and logo are the l property of Virox Technologies, Inc. Modified from G Mac. Donald.

ACCREDITING AGENCIES The Joint Commission/CMS l Recommendations for Improvement must be based on evidence-based guidelines n n n 7 -day endoscope reprocessing (challenged, removed from report) Storage Handling disinfected endoscopes with clean hands versus gloves (challenged, removed from report)

MULTISOCIETY GUIDELINE ON REPROCESSING GI ENDOSCOPES, 2011 Petersen et al. ICHE. 2011; 32: 527

Multi-Society Guideline for Reprocessing Flexible Gastrointestinal Endoscopes, 2011 l Unresolved Issues n Interval of storage after which endoscopes should be reprocessed before use u. Data suggest that contamination during storage for intervals of 7 -14 days is negligible, unassociated with duration, occurs on exterior of instruments and involves only common skin organisms u. Data are insufficient to proffer a maximal outer duration for use of appropriately cleaned, reprocessed, dried and stored endoscopes u. Without full data reprocessing within this interval may be advisable for certain situations (endoscope entry to otherwise sterile regions such as biliary tree, pancreas)
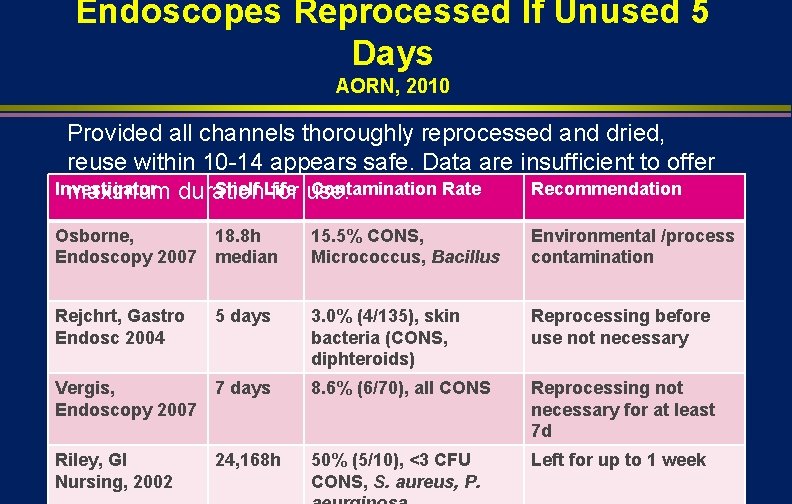
Endoscopes Reprocessed If Unused 5 Days AORN, 2010 Provided all channels thoroughly reprocessed and dried, reuse within 10 -14 appears safe. Data are insufficient to offer Investigator Shelf Life Contamination Rate Recommendation maximum duration for use. Osborne, Endoscopy 2007 18. 8 h median 15. 5% CONS, Micrococcus, Bacillus Environmental /process contamination Rejchrt, Gastro Endosc 2004 5 days 3. 0% (4/135), skin bacteria (CONS, diphteroids) Reprocessing before use not necessary Vergis, Endoscopy 2007 7 days 8. 6% (6/70), all CONS Reprocessing not necessary for at least 7 d Riley, GI Nursing, 2002 24, 168 h 50% (5/10), <3 CFU CONS, S. aureus, P. Left for up to 1 week

Multi-Society Guideline for Reprocessing Flexible Gastrointestinal Endoscopes, 2011 l Unresolved Issues n Optimal frequencies for replacement of: clean water bottles and tubing for insufflation of air and lens wash water, and waste vacuum canisters and suction tubing u. Concern related to potential for backflow from a soiled endoscope against the direction of forced fluid and air passage into clean air/water source or from tubing/canister against a vacuum into clean instruments n Microbiologic surveillance testing after reprocessing u. Detection of non-environmental pathogens indicator

Audit Manual Cleaning of Endoscopes Establishing Benchmarks l Lack of consensus regarding the clinical value of routine microbiological monitoring of endoscopes. We perform to assess the efficacy of reprocessing. n Alfa et al. Am J Infect Control 2012; 40: 233. Recommends a bioburden residual of <100 CFU/ml. n Beilenhoff et al. Endoscopy; 2007; 39: 175. ESGENA allows bioburden count of <20 CFU/ channel. n Heeg et al. J Hosp Infect; 2004; 56: 23. Contamination should not exceed 1 CFU/ml. Certain organisms should not be detected in any amount

Fecal Transplants for Refractory C. difficile Infection l l Criteria for eligibility -failed standard therapy, no contraindication to colonoscopy, confirmed C. difficile toxin positive, etc Self-identified donor-donor will respond to eligibility questions: no GI cancer, no metabolic disease, no prior use of illicit drugs, etc Donor Testing-Stool-C. difficile toxin, O&P, bacterial pathogen panel (Salmonella, Shigella, Giardia, norovirus, etc). Serum. RPR, HIV-1, HIV-2, HCV Ab, CMV viral load, HAV Ig. M and Ig. G, HBs. Ag, liver tests, etc Stool preparation-fresh sample into 1 liter sterile bottle, 500 ml saline added, vigorously shaking to liquefy, solid pieces

Reprocessing Flexible Endoscopes Objectives Risks associated with reprocessing flexible endoscopes l Causes of contamination and infection l Gaps in current reprocessing standards l Establish scientific rationale and evidence requirements for enhancing safe practices l

Conclusions l l l Endoscopes represent a nosocomial hazard. Narrow margin of safety associated with high-level disinfection of semicritical items. Guidelines must be strictly followed. AERs can enhance efficiency and reliability of HLD of endoscopes by replacing some manual reprocessing steps and reducing the likelihood that essential steps are not skipped Urgent need to better understand the gaps in endoscope reprocessing-CRE, C. difficile spores, HPV, biofilms, etc. Industry must support research to answer questions. Data are insufficient to recommend ATP monitoring Data suggest that contamination during storage for 7 -14 days

THANK YOU! www. disinfectionandsterilization. org

Endoscopes: Delayed Reprocessing and Drying l Delayed Reprocessing (GI Endoscopy 2011; 73; 853) n l Reprocess immediately after use; do not allow to sit idle and soiled for hours before being processed. If precleaning not initiated within an hour, soak in detergent before cleaning. Endoscope Drying (J Hosp Infect 2008; 68: 59) n Microbial contamination lower when stored in drying and storage cabinet.
- Slides: 72