RENAL TRANSPLANTATION INTO HIGH RISK HIGHLY SENSITIZED RECIPIENTS


























- Slides: 44

RENAL TRANSPLANTATION INTO HIGH RISK, HIGHLY SENSITIZED RECIPIENTS: A SINGLE CENTER EXPERIENCE Randy Hennigar Ph. D, MD Director, Nephropathology and Electron Microscopy Emory University Hospital Atlanta , GA

Incidence of C 4 d in Renal Transplant Population: Emory University Hospital (EUH) • Objective: To gain more information about the role of antibody mediated rejection in the renal transplant population @ EUH. • Method: From Nov 2003 to Mar 2005, a total of 313 consecutive biopsies (252 tx patients) were screened for C 4 d deposition. Bxs were performed for renal dysfunction.

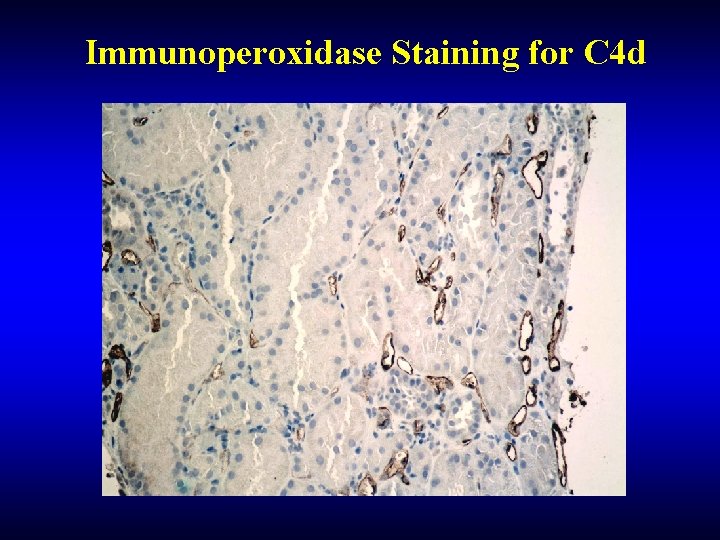
Immunoperoxidase Staining for C 4 d

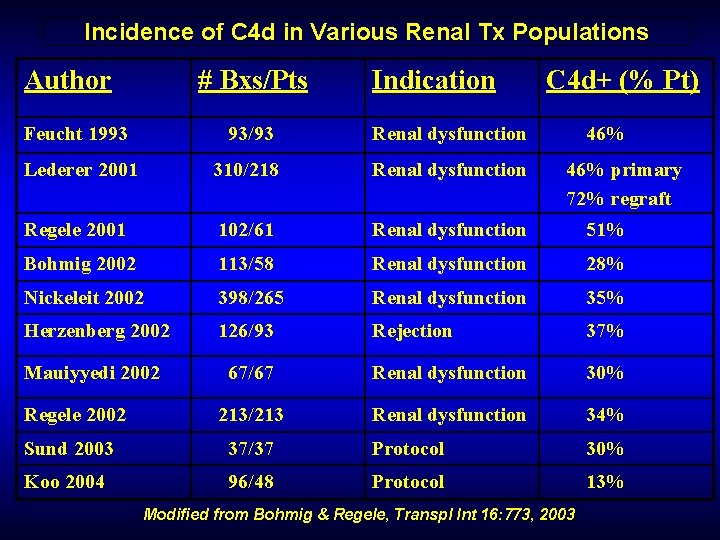
Incidence of C 4 d in Various Renal Tx Populations Author # Bxs/Pts Indication C 4 d+ (% Pt) Feucht 1993 93/93 Renal dysfunction Lederer 2001 310/218 Renal dysfunction Regele 2001 102/61 Renal dysfunction 51% Bohmig 2002 113/58 Renal dysfunction 28% Nickeleit 2002 398/265 Renal dysfunction 35% Herzenberg 2002 126/93 Rejection 37% Mauiyyedi 2002 67/67 Renal dysfunction 30% 213/213 Renal dysfunction 34% Regele 2002 46% primary 72% regraft Sund 2003 37/37 Protocol 30% Koo 2004 96/48 Protocol 13% Modified from Bohmig & Regele, Transpl Int 16: 773, 2003

Incidence of C 4 d in Renal Transplant Population @ EUH • Results: 23 of 252 pts (9%) were positive, using the criteria of Nickeleit and Mihatsch (Nephrol Dial Transpl 18: 2232 -2239, 2003). • Conclusion: The incidence of C 4 d deposition (and presumably antibody-mediated rejection) among the kidney transplant population at EUH appears less prevalent than that reported in the literature.


Emory University Hospital: Renal Transplant Center Activity (2004) Deceased donor txs = Living donor txs = Total = 111 (74%) 39 (26%) 150 Tx rate among waitlist pts = 0. 3 From: The Scientific Registry of Transplant Recipients

Emory University Hospital: Transplant Recipient Characteristics (2004) Ethnicity/race of waitlist pts (end of 2004): EUH(%) African-American White Hispanic/Latino Asian Other 63 32 2 3 <1 USA average(%) 36 39 16 8 1 From: The Scientific Registry of Transplant Recipients

Emory University Hospital: Transplant Recipient Characteristics (2004) Ethnicity/race of tx patients (deceased donors): EUH(%) African-American White Hispanic/Latino Asian Other 52 45 1 2 0 USA average(%) 30 49 14 6 2 From: The Scientific Registry of Transplant Patients

Panel Reactive Antibodies (PRA) • A screening mechanism to determine the HLA antibody profile of potential transplant recipients. • Periodic screening (monthly/quarterly) of recipient sera with a panel of HLA-typed cells. • Sensitization of the recipient is expressed as the percentage of serum reactivity with the total panel. Typically, high PRA is indicative of a highly sensitized recipient- one who is at risk for early graft loss.

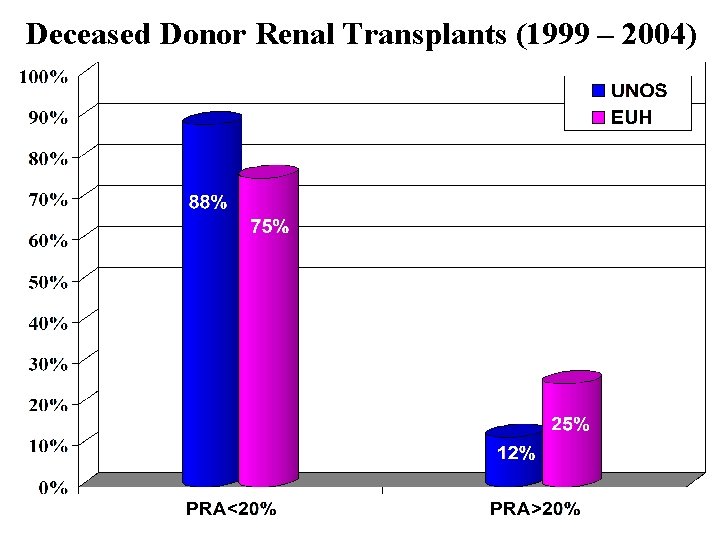
Deceased Donor Renal Transplants (1999 – 2004)

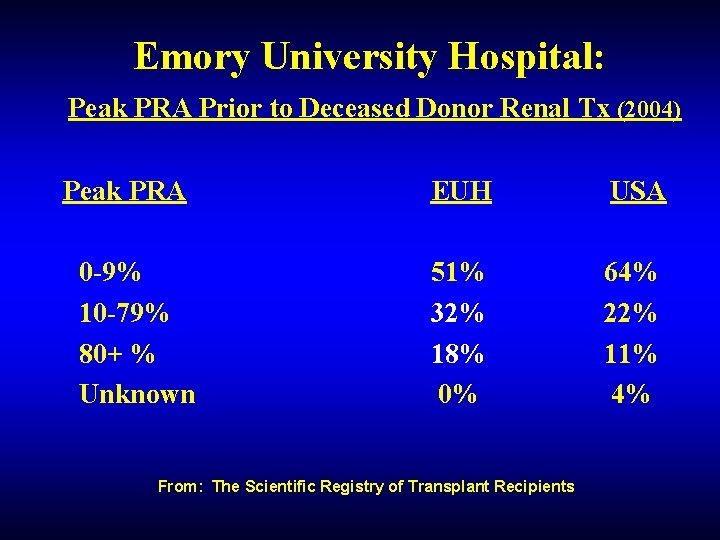
Emory University Hospital: Peak PRA Prior to Deceased Donor Renal Tx (2004) Peak PRA 0 -9% 10 -79% 80+ % Unknown EUH USA 51% 32% 18% 0% 64% 22% 11% 4% From: The Scientific Registry of Transplant Recipients

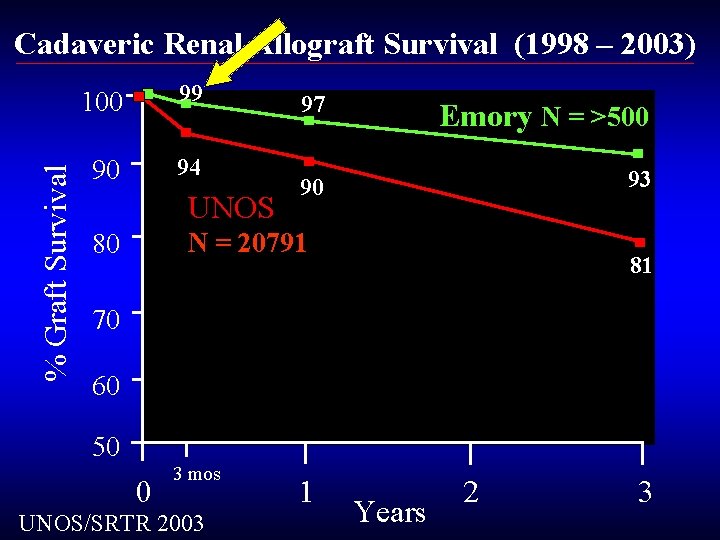
% Graft Survival Cadaveric Renal Allograft Survival (1998 – 2003) 100 99 90 94 UNOS 97 Emory N = >500 90 93 N = 20791 80 81 70 60 50 0 3 mos UNOS/SRTR 2003 1 Years 2 3



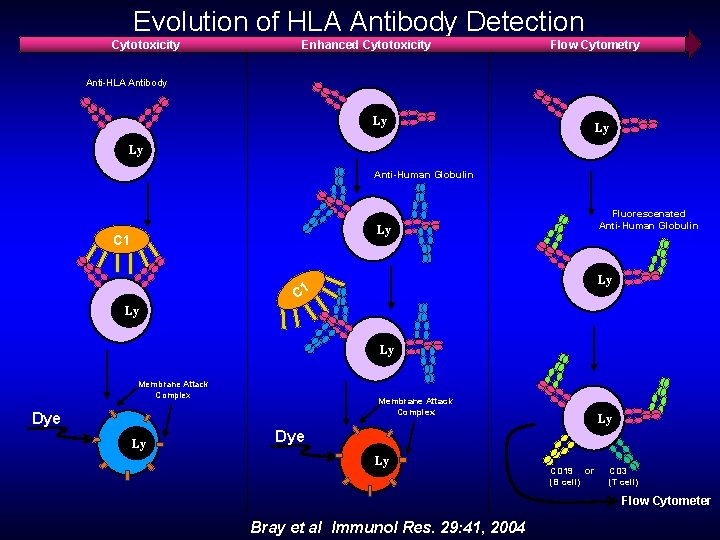
Evolution of HLA Antibody Detection Cytotoxicity Enhanced Cytotoxicity Flow Cytometry Anti-HLA Antibody Ly Ly Ly Anti-Human Globulin Fluorescenated Anti-Human Globulin Ly C 1 Ly Ly Membrane Attack Complex Dye Ly Ly Dye Ly CD 19 or (B cell) CD 3 (T cell) Flow Cytometer Bray et al Immunol Res. 29: 41, 2004

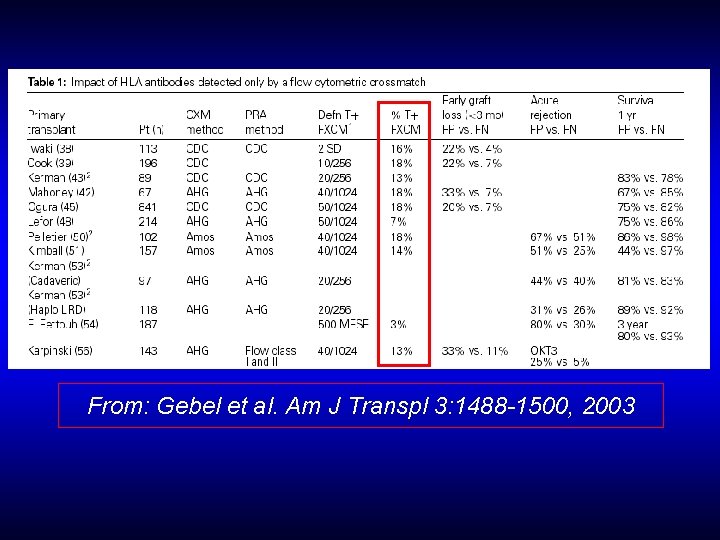
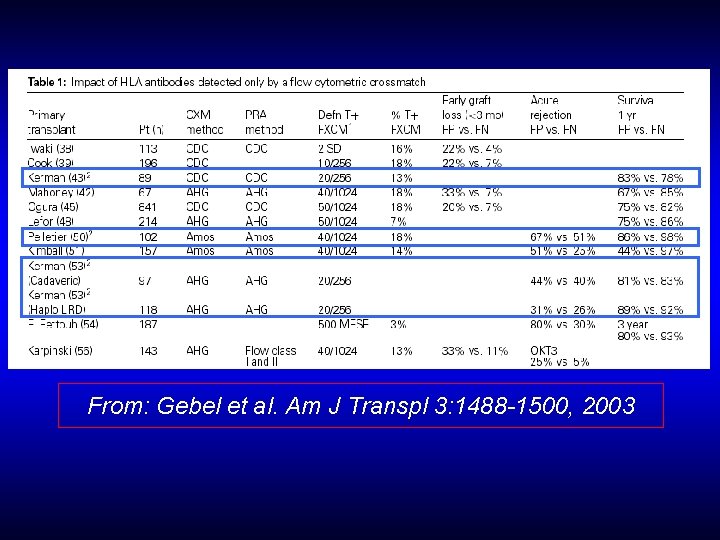
From: Gebel et al. Am J Transpl 3: 1488 -1500, 2003

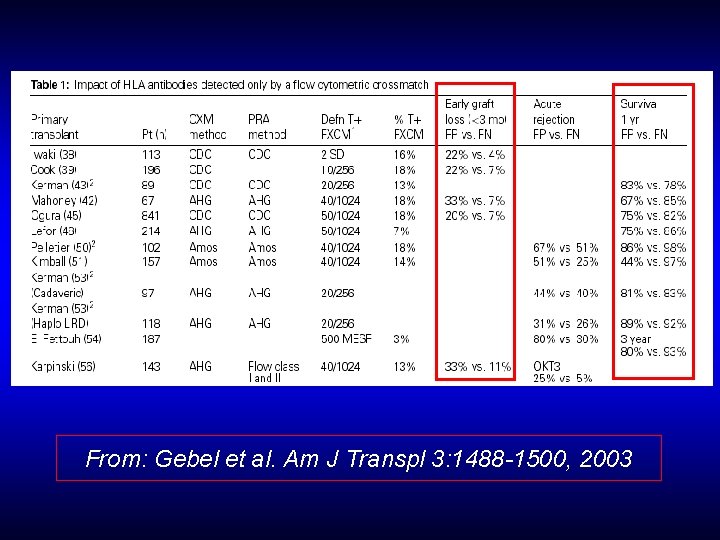
From: Gebel et al. Am J Transpl 3: 1488 -1500, 2003

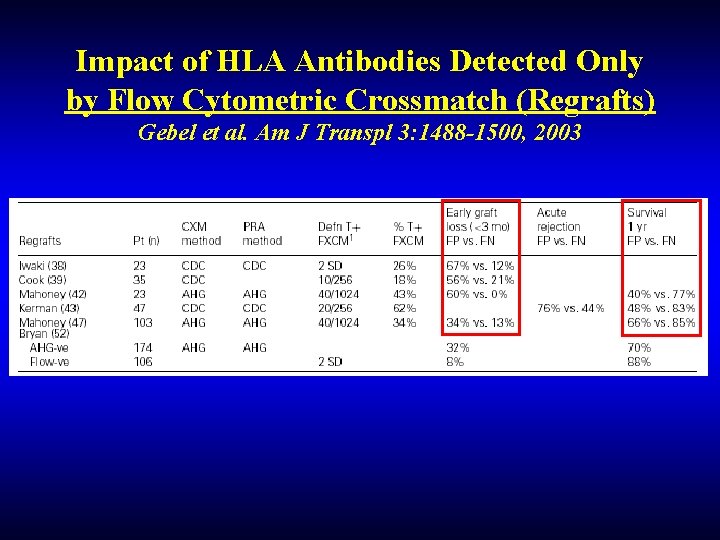
Impact of HLA Antibodies Detected Only by Flow Cytometric Crossmatch (Regrafts) Gebel et al. Am J Transpl 3: 1488 -1500, 2003

In 2002, of the >150 labs participating in the ASHI-CAP class I crossmatch surveys (MX 1 -A, B, C), only 68– 70% reported AHG augmented CDC and 47– 52% flow-based crossmatches.

From: Gebel et al. Am J Transpl 3: 1488 -1500, 2003

Perceived Pitfalls of Flow Cytometry Crossmatching (FCXM) • Too sensitive – Detection of low titer and noncomplementfixing antibodies of little or no clinical relevance • Would inappropriately deny a patient access to transplantion • Does not reliably predict poor clinical outcomes

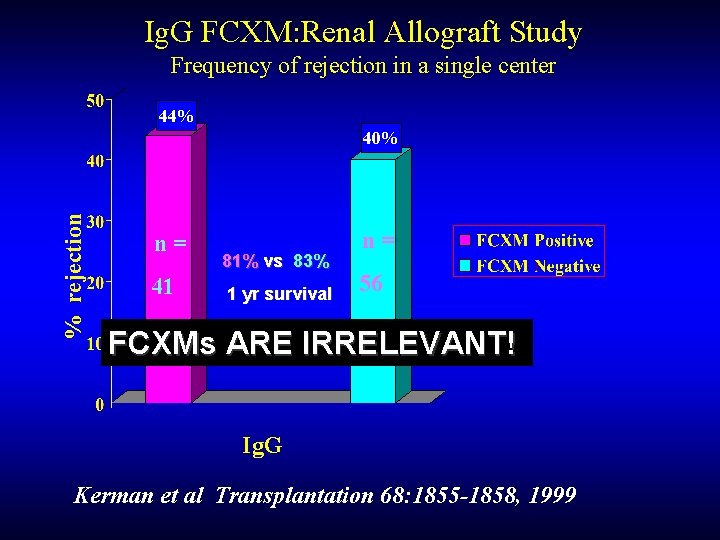
Ig. G FCXM: Renal Allograft Study Frequency of rejection in a single center 44% % rejection 40% n= 41 81% vs 83% 1 yr survival n= 56 FCXMs ARE IRRELEVANT! Ig. G Kerman et al Transplantation 68: 1855 -1858, 1999

In 2002, of the >150 labs participating in the ASHI-CAP class I crossmatch surveys (MX 1 -A, B, C), only 68– 70% reported AHG augmented CDC and 47– 52% flow-based crossmatches.

Panel Reactive Antibodies (PRA) • A screening mechanism to determine the HLA antibody profile of potential transplant recipients. • Periodic screening (monthly/quarterly) of recipient sera with a panel of HLA typed cells. • Sensitization of the recipient is expressed as the percentage of serum reactivity with the total panel. Typically, high PRA is indicative of a highly sensitized recipient- one who is at risk for early graft loss. • Historically, PRA has been antigen-nonspecific.

METHODS FOR ANTIBODY EVALUATION Antigen Non-Specific Antigen Specific Complement-dependent Cytotoxicity (CDC): - Direct CDC (Standard CDC) - Modifications Washes Extended Incubation Anti-human globulin (AHG-CDC) DTT / DTE ELISA - Yes / No - PRA % (I & II) - Specificity (I & II) Flow Cytometry (cells): - T cell / B cell - Pronase Multi-plex - Suspension Arrays - Protein Chips “Flow. PRA” Flow cytometry using microparticles (“beads”) - PRA % (I and II ) - Specificity (I & II)

Flow Microparticles One Lambda www. onelambda. com

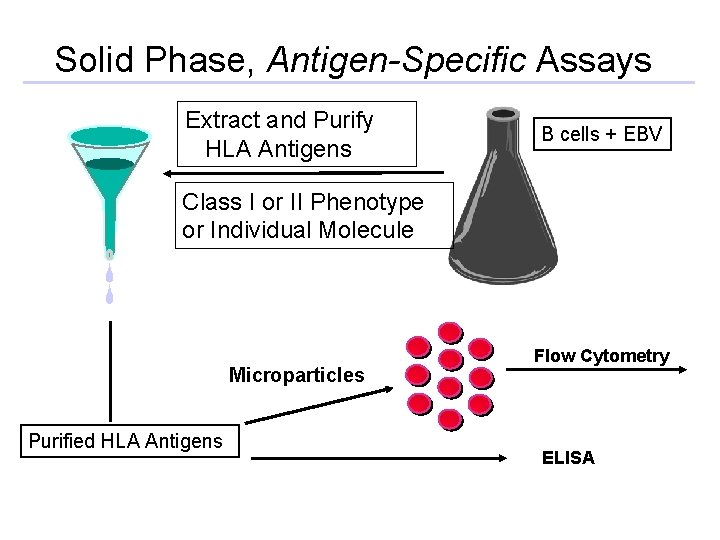
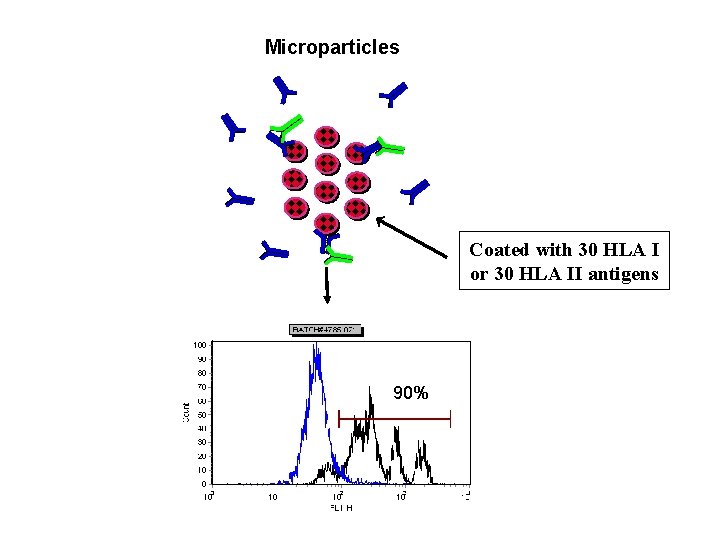
Solid Phase, Antigen-Specific Assays Extract and Purify HLA Antigens B cells + EBV Class I or II Phenotype or Individual Molecule Microparticles Purified HLA Antigens Flow Cytometry ELISA

Microparticles ELISA Coated with 30 HLA I or 30 HLA II antigens 90%

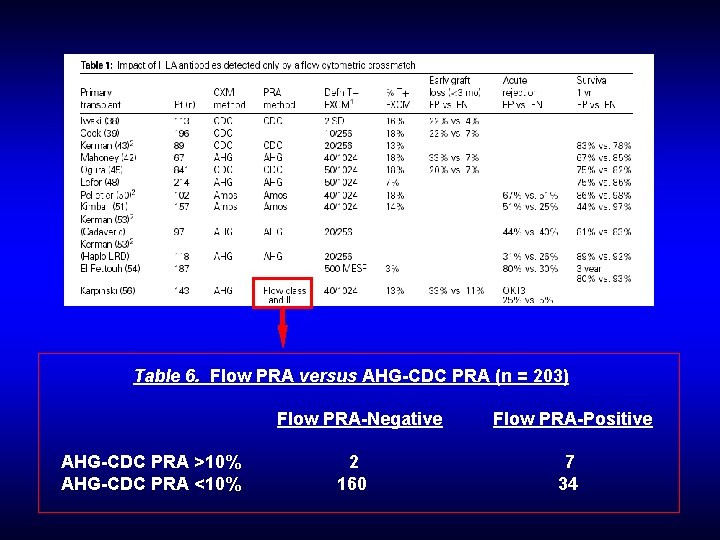
Table 6. Flow PRA versus AHG-CDC PRA (n = 203) Flow PRA-Negative AHG-CDC PRA >10% AHG-CDC PRA <10% 2 160 Flow PRA-Positive 7 34

PRA ANALYSIS BY DIFFERING METHODLOGIES POSITIVE NEGATIVE CDC 102 162 AHG-CDC 116 (+13%) 148 ELISA 127 (+10%) 137 Flow. PRA 139 (+10%) 125 Gebel and Bray, Transplantation 69: 1370 -1374, 2000.

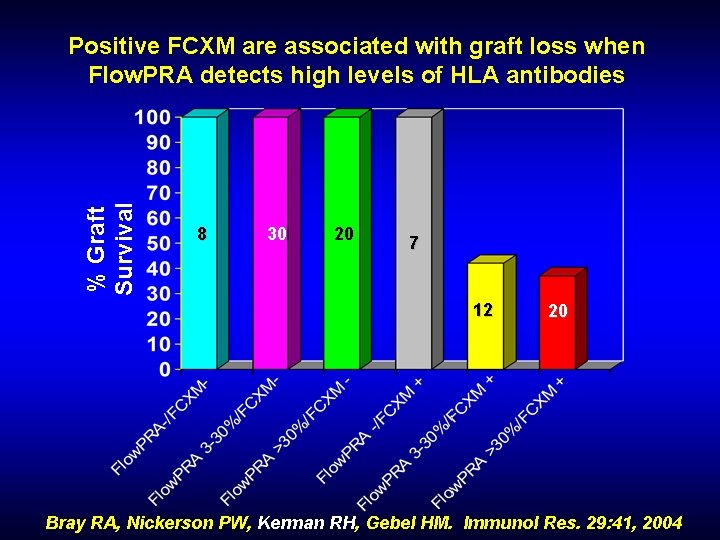
% Graft Survival Positive FCXM are associated with graft loss when Flow. PRA detects high levels of HLA antibodies 8 30 20 7 12 20 Bray RA, Nickerson PW, Kerman RH, Gebel HM. Immunol Res. 29: 41, 2004

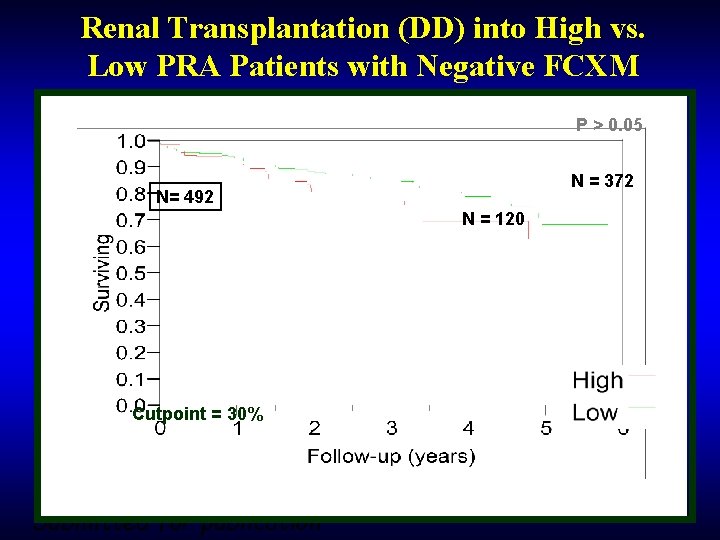
Renal Transplantation (DD) into High vs. Low PRA Patients with Negative FCXM P > 0. 05 N = 372 N= 492 N = 120 Cutpoint = 30% Submitted for publication

Antibody Paradigms - 2005 Screening Crossmatch Low Risk Antibody Negative Crossmatch Negative Antibody Negative Crossmatch Positive Antibody Positive Crossmatch Negative High Risk Antibody Positive Crossmatch Positive

PRA • PRA can be a qualitative and/or quantitative assessment of alloimmunization in transplant patients. • Optimally, PRA testing should identify the specificity of an antibody and provide the “transplantability” index of a patient. • More succinctly, PRA testing should correlate with the final crossmatch.

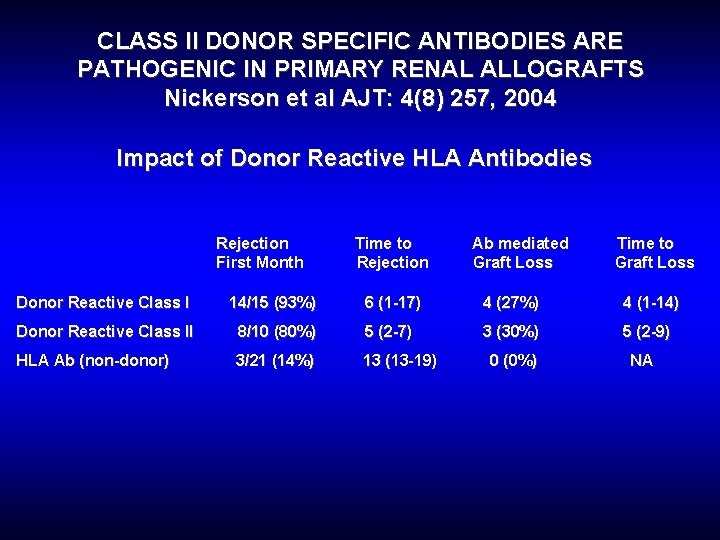
CLASS II DONOR SPECIFIC ANTIBODIES ARE PATHOGENIC IN PRIMARY RENAL ALLOGRAFTS Nickerson et al AJT: 4(8) 257, 2004 Impact of Donor Reactive HLA Antibodies Rejection First Month Time to Rejection Ab mediated Graft Loss Time to Graft Loss Donor Reactive Class I 14/15 (93%) 6 (1 -17) 4 (27%) 4 (1 -14) Donor Reactive Class II 8/10 (80%) 5 (2 -7) 3 (30%) 5 (2 -9) HLA Ab (non-donor) 3/21 (14%) 13 (13 -19) 0 (0%) NA

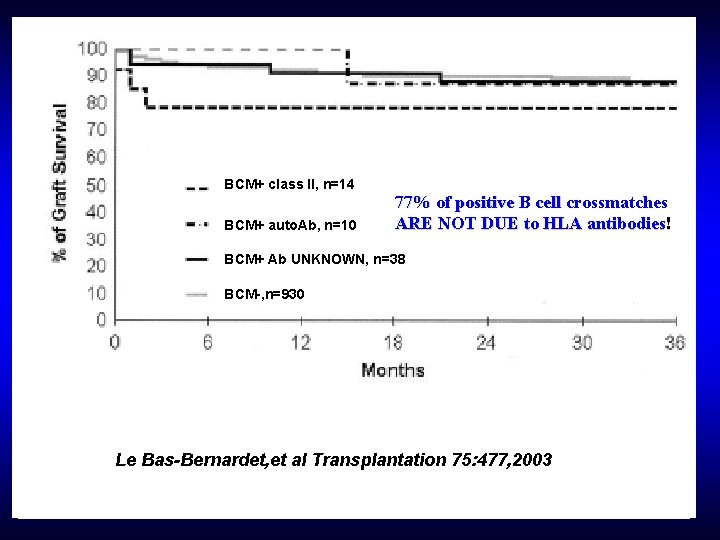
BCM+ class II, n=14 BCM+ auto. Ab, n=10 77% of positive B cell crossmatches ARE NOT DUE to HLA antibodies! BCM+ Ab UNKNOWN, n=38 BCM-, n=930 Le Bas-Bernardet, et al Transplantation 75: 477, 2003

Approaches Pharmacological Desensitization IVIG PP / IVIG Rituxan Transplant across a + crossmatch anticipating Immunosuppression Biological Identical Sibling Xenotransplantation Acceptable Mismatch - Detailed Antibody Analysis - Comprehensive PRA - Virtual Crossmatch

Acceptable Mismatches Putative Recipient: A 1, A 30; B 7, B 8 ; DR 11, 15 Antibodies - A 2, 23, 24, 68 Potential Donor: A 25, A 33; B 42, B 18; DR 12, DR 13

Strategic Approaches - Based on recognition that matching is not for everyone- 85% of DD Txs are mismatched. - Focus on appropriate mismatching rather than looking for an HLA “match”. - Requires detailed evaluation of the patient’s HLA antibodies. - Shifts emphasis to antibody evaluation and away from crossmatching to identify acceptable mismatches.

Desensitization Protocols Aren’t For Everyone - High Titer HLA Antibodies >512 - Refractory Specificities DR 52, DR 53 - Fragile Patients - Restricted to Living Donors - $$$$$$s

Recommendations to define the ‘non-sensitized’ patient: • Validate patient history for the lack of sensitizing events. • Confirm that a patient is nonsensitized using a solid phase assay documented to be more sensitive than CDC assays.

Recommendations to evaluate the ‘sensitized’ patient: • To optimize detection of low titer HLA antibodies, monitoring should be performed using sensitive solid-phase assays. • Monitoring should include evaluation for both antibodies to class I and class II HLA antigens. • A crossmatch test must be performed before transplantation using, as a minimum, an enhanced CDC technique. • The final crossmatch technique should be of equal sensitivity to the solid-phase assay used to screen for the presence of HLA antibody. • A B-cell crossmatch should be included in the final crossmatch. • Peak sera should be included in the final crossmatch. • Auto-crossmatches should be utilized to aid in the interpretation of allo-crossmatches.

END OF LECTURE