Renal System Functional unit is the Nephron Kidneys






- Slides: 29

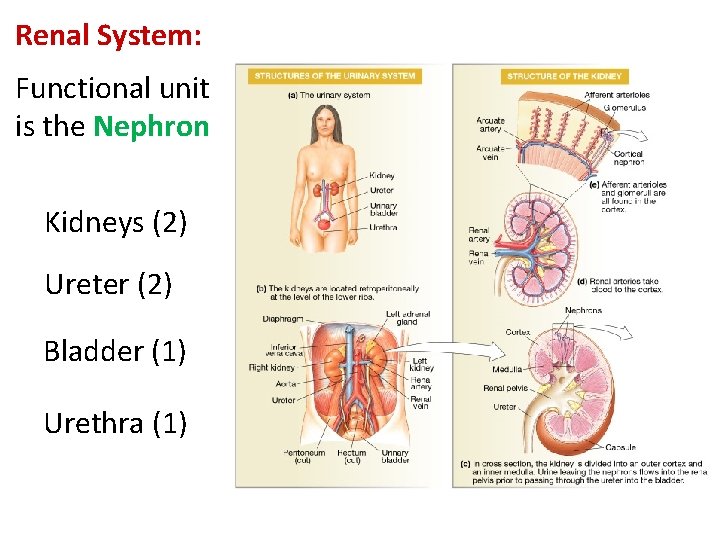
Renal System: Functional unit is the Nephron Kidneys (2) Ureter (2) Bladder (1) Urethra (1)

Functions of the Renal System 1) Regulates ECF volume: a) Regulates Osmolarity: b) Regulates Ion Balance: 2) Regulates p. H of body fluids:

Functions of Renal System (cont. ) 3) Eliminates Metabolic Waste: 4) Removes Foreign Substances: 5) 2 o Endocrine gland: a) Erythropoietin b) Renin

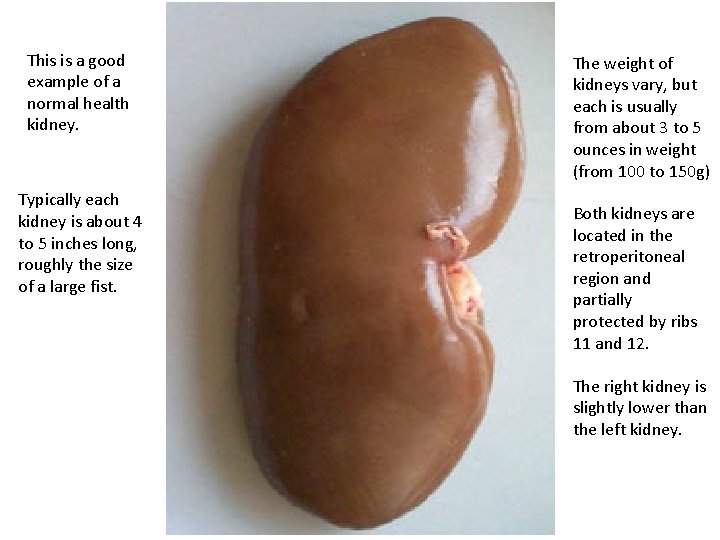
This is a good example of a normal health kidney. Typically each kidney is about 4 to 5 inches long, roughly the size of a large fist. The weight of kidneys vary, but each is usually from about 3 to 5 ounces in weight (from 100 to 150 g) Both kidneys are located in the retroperitoneal region and partially protected by ribs 11 and 12. The right kidney is slightly lower than the left kidney.

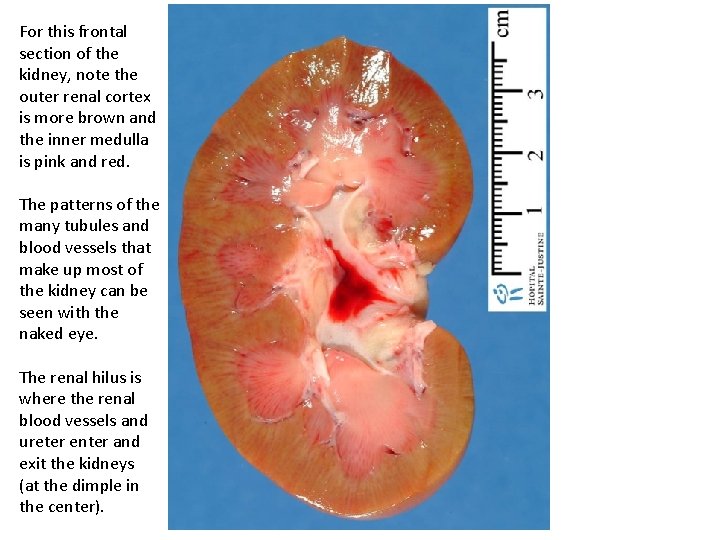
For this frontal section of the kidney, note the outer renal cortex is more brown and the inner medulla is pink and red. The patterns of the many tubules and blood vessels that make up most of the kidney can be seen with the naked eye. The renal hilus is where the renal blood vessels and ureter enter and exit the kidneys (at the dimple in the center).

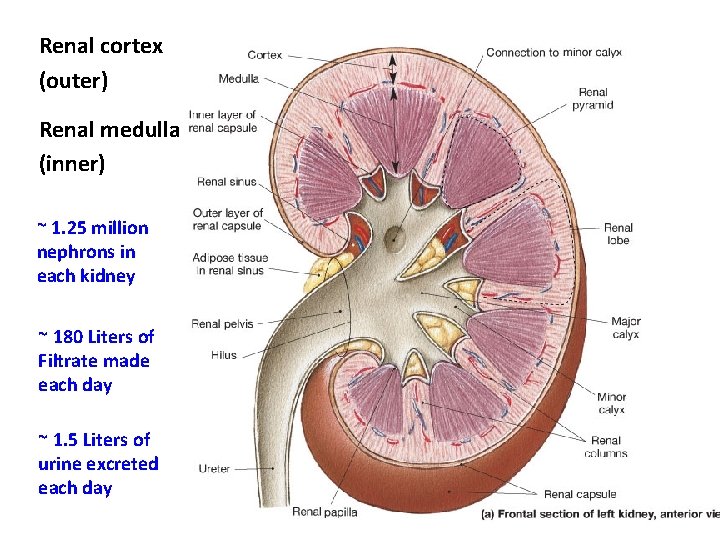
Renal cortex (outer) Renal medulla (inner) ~ 1. 25 million nephrons in each kidney ~ 180 Liters of Filtrate made each day ~ 1. 5 Liters of urine excreted each day

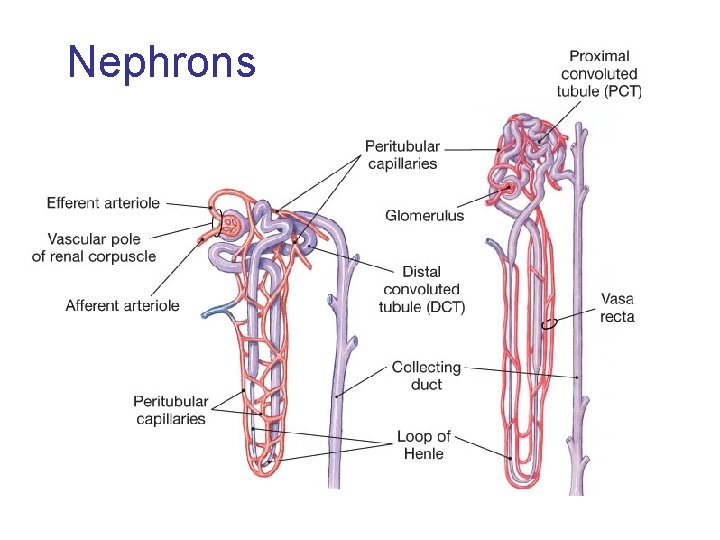
Nephrons

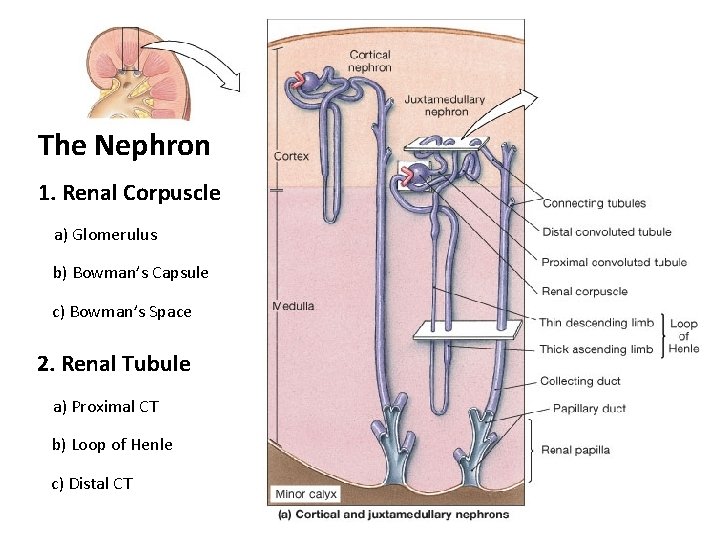
In the Human Renal System ~85% are Cortical nephrons – Renal corpuscle located higher in cortex. – Shorter loop of Henle. – *Peritubular Capillaries at Loop of Henle ~15% are Juxtamedullary nephrons – Renal corpuscle closer to medulla. – Loop of Henle extends deep into medulla. – *Vasa Recta Capillaries at Loop of Henle

The Nephron 1. Renal Corpuscle a) Glomerulus b) Bowman’s Capsule c) Bowman’s Space 2. Renal Tubule a) Proximal CT b) Loop of Henle c) Distal CT

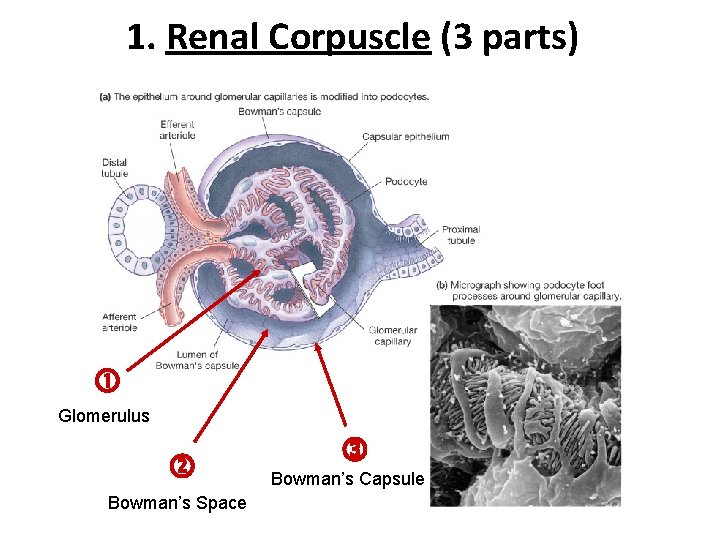
1. Renal Corpuscle (3 parts) Glomerulus Bowman’s Space Bowman’s Capsule

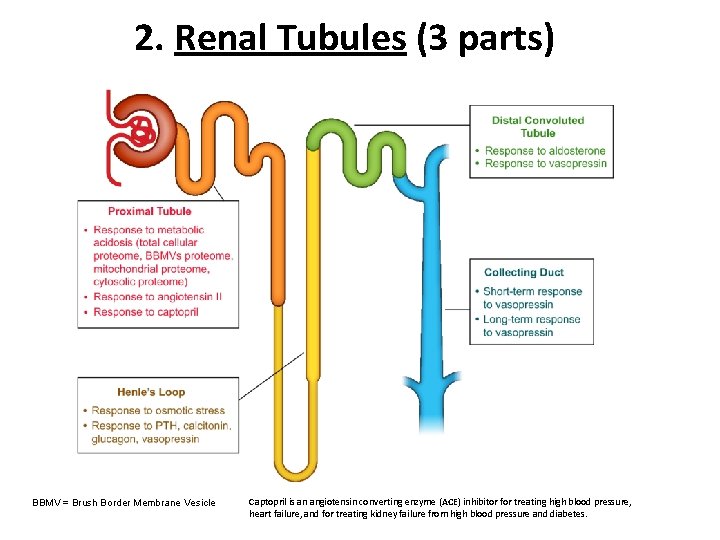
2. Renal Tubules (3 parts) BBMV = Brush Border Membrane Vesicle Captopril is an angiotensin converting enzyme (ACE) inhibitor for treating high blood pressure, heart failure, and for treating kidney failure from high blood pressure and diabetes.

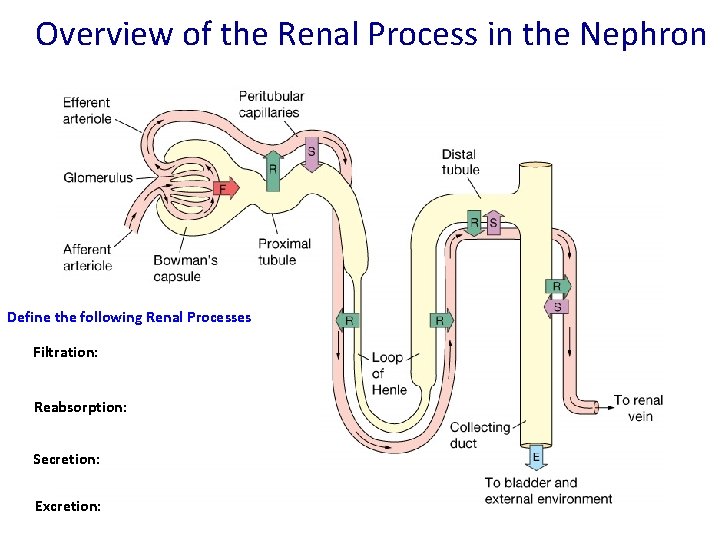
Overview of the Renal Process in the Nephron Define the following Renal Processes Filtration: Reabsorption: Secretion: Excretion:

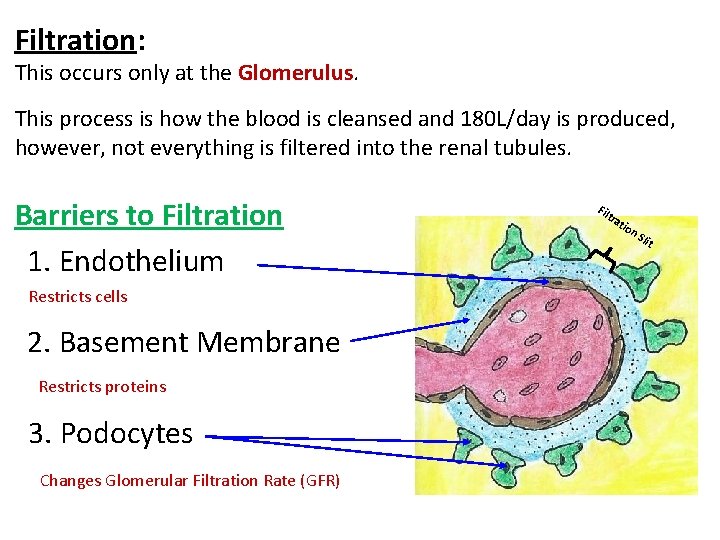
Filtration: This occurs only at the Glomerulus. This process is how the blood is cleansed and 180 L/day is produced, however, not everything is filtered into the renal tubules. Barriers to Filtration 1. Endothelium Restricts cells 2. Basement Membrane Restricts proteins 3. Podocytes Changes Glomerular Filtration Rate (GFR) Fil tra t ion Sli t

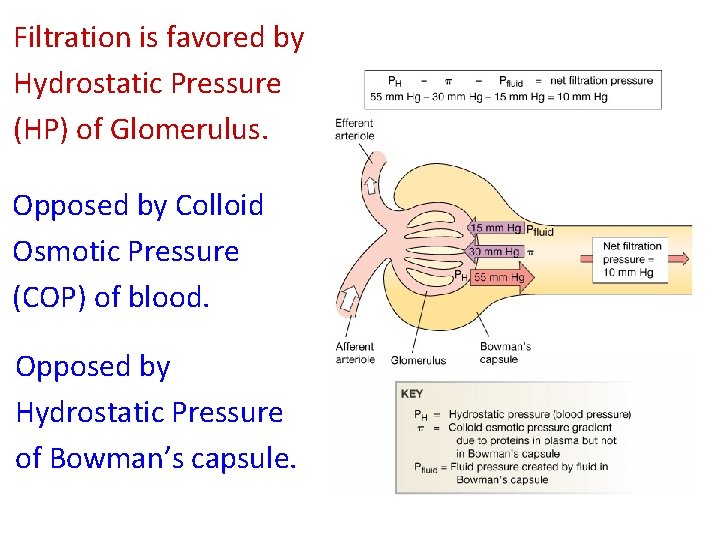
Filtration is favored by Hydrostatic Pressure (HP) of Glomerulus. Opposed by Colloid Osmotic Pressure (COP) of blood. Opposed by Hydrostatic Pressure of Bowman’s capsule.

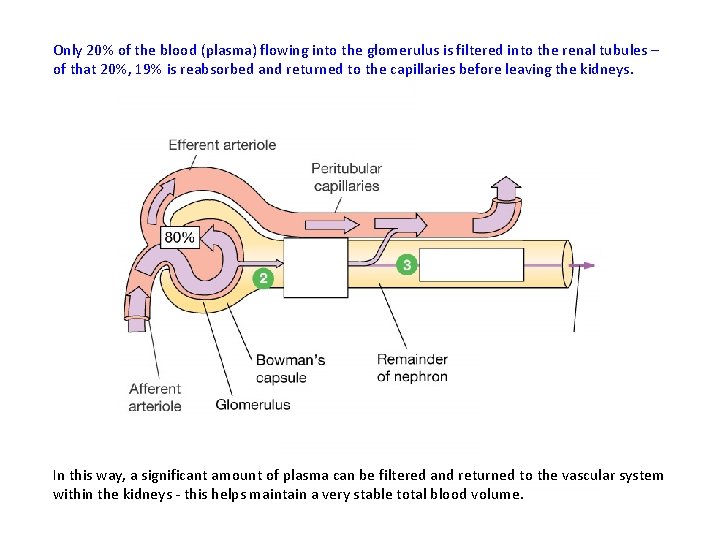
Only 20% of the blood (plasma) flowing into the glomerulus is filtered into the renal tubules – of that 20%, 19% is reabsorbed and returned to the capillaries before leaving the kidneys. In this way, a significant amount of plasma can be filtered and returned to the vascular system within the kidneys - this helps maintain a very stable total blood volume.

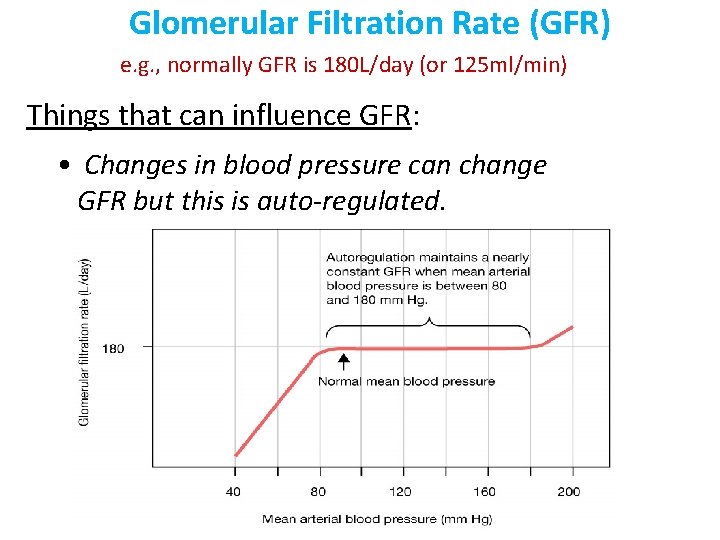
Glomerular Filtration Rate (GFR) e. g. , normally GFR is 180 L/day (or 125 ml/min) Things that can influence GFR: • Changes in blood pressure can change GFR but this is auto-regulated.

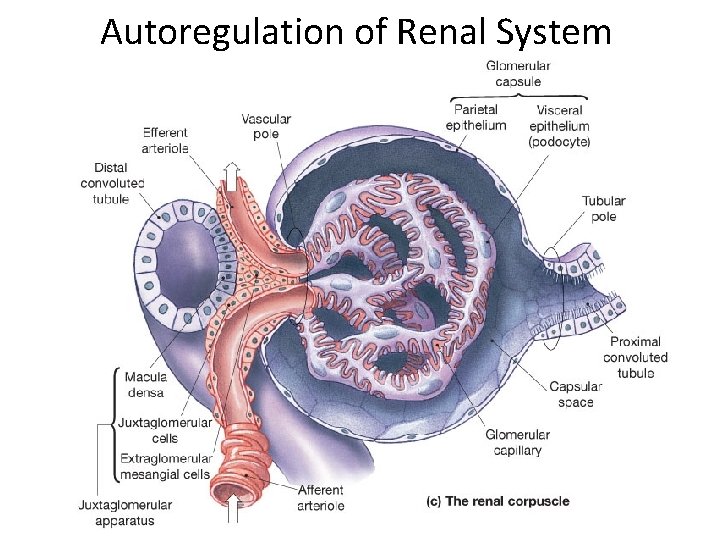
Autoregulation of Renal System

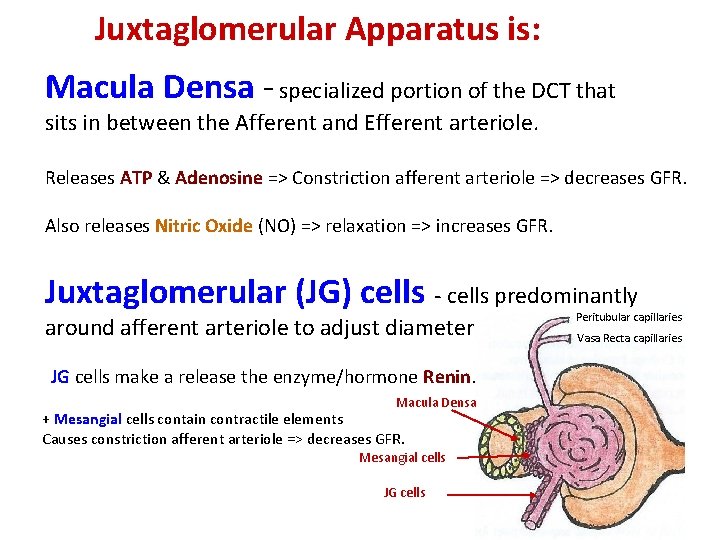
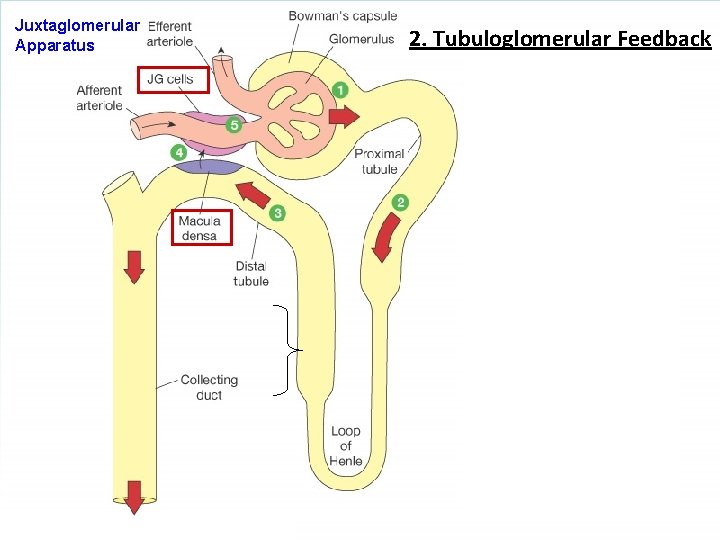
Juxtaglomerular Apparatus is: Macula Densa - specialized portion of the DCT that sits in between the Afferent and Efferent arteriole. Releases ATP & Adenosine => Constriction afferent arteriole => decreases GFR. Also releases Nitric Oxide (NO) => relaxation => increases GFR. Juxtaglomerular (JG) cells - cells predominantly around afferent arteriole to adjust diameter. JG cells make a release the enzyme/hormone Renin. Macula Densa + Mesangial cells contain contractile elements Causes constriction afferent arteriole => decreases GFR. Mesangial cells JG cells Peritubular capillaries Vasa Recta capillaries

Autoregulation of the Nephron 1. Myogenic Stretch 2. Tubuloglomerular Feedback 1. Myogenic Stretch If ↑ blood pressure in afferent arteriole, this stretches smooth muscle and it contracts in response, thus vasoconstricts in response. o This decreases blood flow, o which decreases pressure, o which decreases GFR.

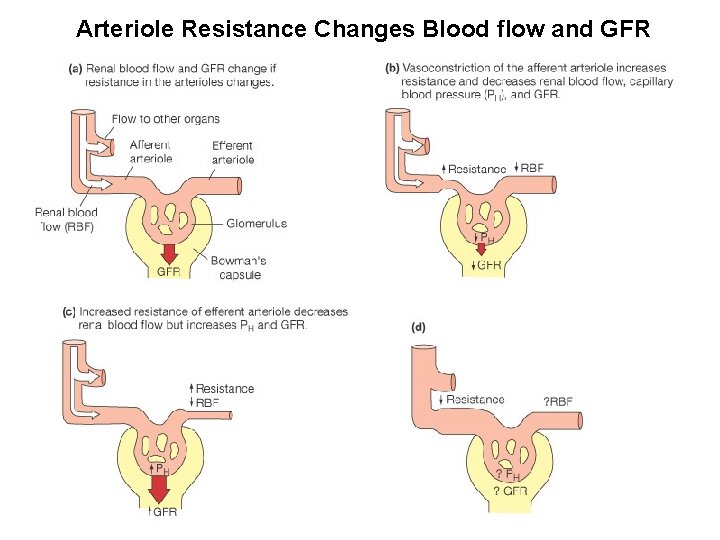
Arteriole Resistance Changes Blood flow and GFR

Juxtaglomerular Apparatus 2. Tubuloglomerular Feedback

• ANS-Sympathetic Modulation Both Afferent and Efferent Arterioles are innervated by SYM neurons. NE binds to receptors on smooth muscle, causing vasoconstriciton. e. g. , if hemorrhage or dehydration, ↑ Sym, vasoconstriction, ↓GFR, conserves fluid volume. • Hormones – Angiotensin II – vasoconstrictor. – Prostaglandins – vasodilator.

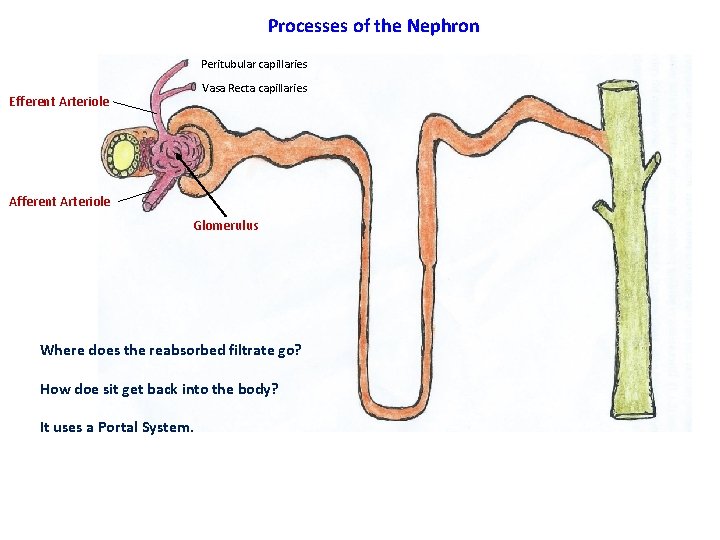
Processes of the Nephron Peritubular capillaries Vasa Recta capillaries Efferent Arteriole Afferent Arteriole Glomerulus Where does the reabsorbed filtrate go? How doe sit get back into the body? It uses a Portal System.

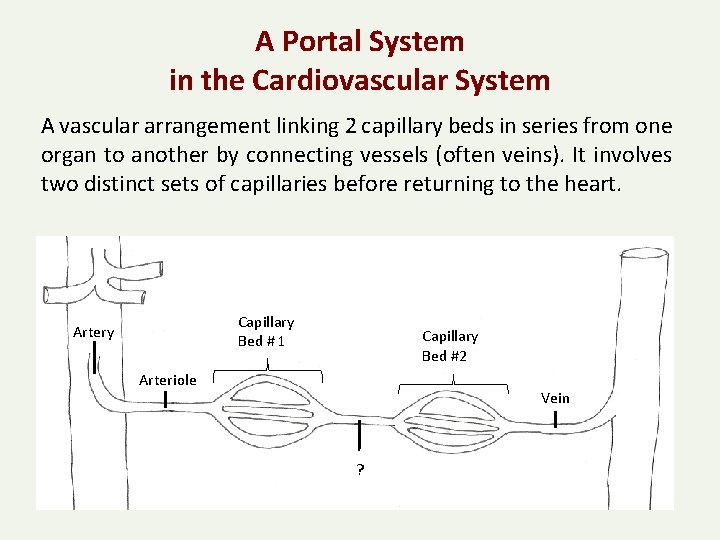
A Portal System in the Cardiovascular System A vascular arrangement linking 2 capillary beds in series from one organ to another by connecting vessels (often veins). It involves two distinct sets of capillaries before returning to the heart. Capillary Bed # 1 Artery Capillary Bed #2 Arteriole Vein ?

There are three (3) examples of Portal Systems in the Body: 1) Hepatic Portal System 2) Renal (Nephron) 3) Hypothalamic - Hypophyseal

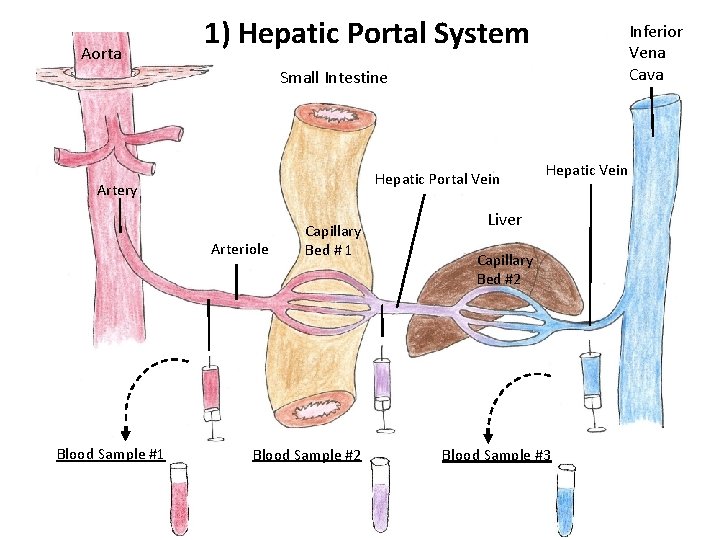
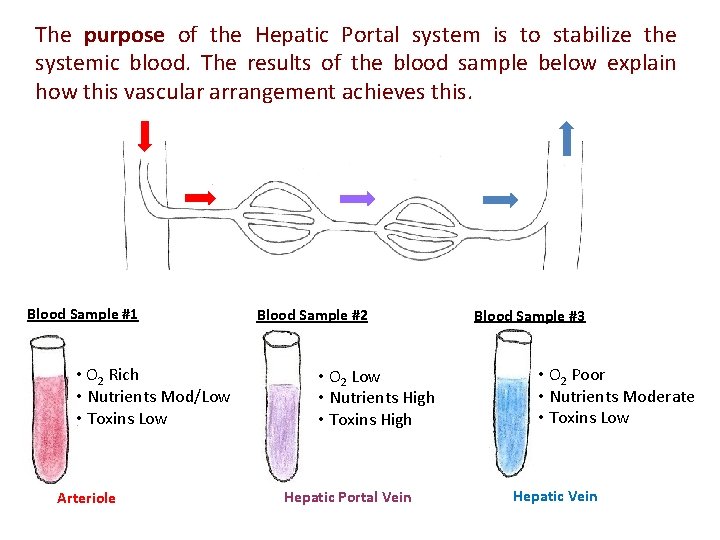
Aorta 1) Hepatic Portal System Inferior Vena Cava Small Intestine Hepatic Portal Vein Artery Arteriole Blood Sample #1 Capillary Bed # 1 Blood Sample #2 Hepatic Vein Liver Capillary Bed #2 Blood Sample #3

The purpose of the Hepatic Portal system is to stabilize the systemic blood. The results of the blood sample below explain how this vascular arrangement achieves this. Blood Sample #1 • O 2 Rich • Nutrients Mod/Low • Toxins Low Arteriole Blood Sample #2 • O 2 Low • Nutrients High • Toxins High Hepatic Portal Vein Blood Sample #3 • O 2 Poor • Nutrients Moderate • Toxins Low Hepatic Vein

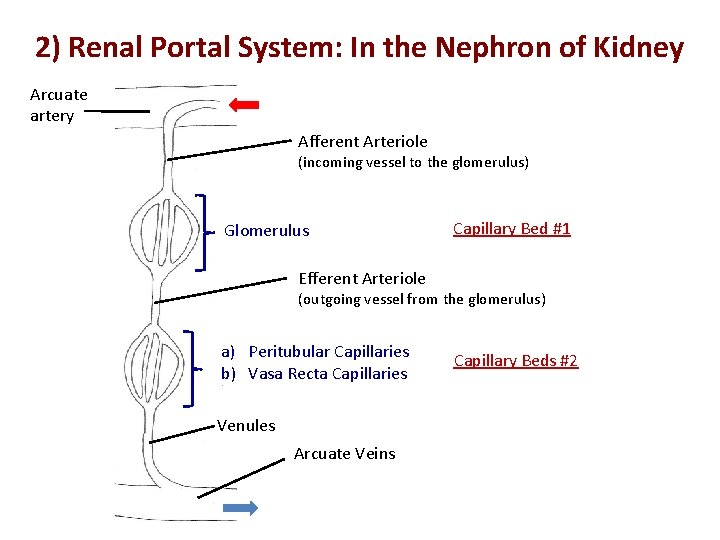
2) Renal Portal System: In the Nephron of Kidney Arcuate artery Afferent Arteriole (incoming vessel to the glomerulus) Glomerulus Capillary Bed #1 Efferent Arteriole (outgoing vessel from the glomerulus) a) Peritubular Capillaries b) Vasa Recta Capillaries Venules Arcuate Veins Capillary Beds #2

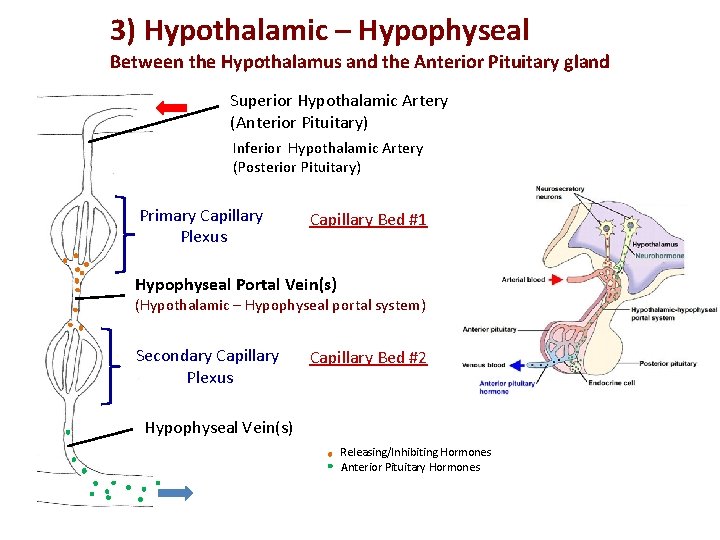
3) Hypothalamic – Hypophyseal Between the Hypothalamus and the Anterior Pituitary gland Superior Hypothalamic Artery (Anterior Pituitary) Inferior Hypothalamic Artery (Posterior Pituitary) Primary Capillary Plexus Capillary Bed #1 Hypophyseal Portal Vein(s) (Hypothalamic – Hypophyseal portal system) Secondary Capillary Plexus Capillary Bed #2 Hypophyseal Vein(s) Releasing/Inhibiting Hormones Anterior Pituitary Hormones