Renal Review Ana Ivkovic and Rahul Dave Kidney











![PAH n n Used to measure RPF Effective RPF = ([U]PAH x V) / PAH n n Used to measure RPF Effective RPF = ([U]PAH x V) /](https://slidetodoc.com/presentation_image/2020f2a747d9965b7815337b5e52dde8/image-13.jpg)
























![Aldosterone secretion: n n Increased by ACTH, Angiotensin II, high plasma [K+], cases of Aldosterone secretion: n n Increased by ACTH, Angiotensin II, high plasma [K+], cases of](https://slidetodoc.com/presentation_image/2020f2a747d9965b7815337b5e52dde8/image-41.jpg)



















![Buffering Mechanisms [HCO 3 -] = 24 p. H = 6. 1 + log Buffering Mechanisms [HCO 3 -] = 24 p. H = 6. 1 + log](https://slidetodoc.com/presentation_image/2020f2a747d9965b7815337b5e52dde8/image-61.jpg)










- Slides: 74

Renal Review Ana Ivkovic and Rahul Dave

Kidney functions n n n Primary: water regulation and electrolyte balance-homeostasis The renal system functions to maintain the intravascular volume (of body fluids) Other: Endocrine: renin, erythropoieten, calcitriol ¨ Liver-like fxns: glucose synthesis ¨

Basic Concepts n Excretion = Filtration - Reabsorption + Secretion ¨ Filtration: Bowman’s capsule ¨ Reabsorption: Peritubular capillaries ¨ Secretion: Peritubular capillaries

Measuring Fluid Compartments Total Body Water = 60% total body weight 2/3 = ICF 1/4 = Plasma 1/3 = ECF 3/4 = Interstitial Fluid §Total Body Water: varies with fat § 20 -40 -60 Rule §ICF high in K and Mg; ECF high in Na, Cl §Plasma high in protein; interstitial fluid low in protein-Gibbs Donnan (neg. charged prots attract more pos. charge) §Smallest compartment (plasma) most important (intravascular volume that is controlled by kidney)

Osmolarity and Oncotic Pressure n n n Normal plasma osmolarity = 285 -290 m. Osm/L Tightly controlled Osmolarity vs. Osmolality Osmolarity = mmol solute/L solution ¨ Osmolality = mmol solute/kg h 2 O ¨ n Reflection coefficient: 0 = ineffective osmolyte (urea, ethanol--freely permeable) ¨ 1 = effective osmolyte (Na, K, glucose w/o insulin; “draw” water) ¨ n Oncotic Pressure: the fraction of plasma osmolarity that is due to plasma proteins

Tonicity vs. Osmolarity n Osmolarity ¨ n Describes the osmotic properties of a solution Tonicity Refers to the osmotic effect on the volume of a cell ¨ Ex: hypotonic soln--water moves in, cell swell ¨ n Isosmotic solns not necessarily isotonic (has to do w/ concept of reflection coefficient--ex of urea solution and RBC)

Darrow-Yanet Diagrams--Think Logically! n n n All volume disturbances originate in the ECF compartment Changes in the ICF compartment are in response to changes in the ECF “hyposmotic contraction” refers to the volume of fluid that remains

Volume contractions n n Diarrhea, vomiting, loss of blood--isosmotic volume contraction Diaphoresis (sweating), dehydration-hyperosmotic contraction Remember that sweat is hyposmotic Addison’s disease (lack of aldosterone)-hyposmotic volume contraction

Volume expansions (rarer) n n n Isotonic volume expansion (isotonic saline IV): ECF expands, ICF doesn’t change Hypertonic volume expansion: ECF osmolarity increases, draws fluid from ICF Hypotonic volume expansion: ECF osmolarity decreases, adds fluid to ICF (examples: psychogenic polydipsia, SIADH)

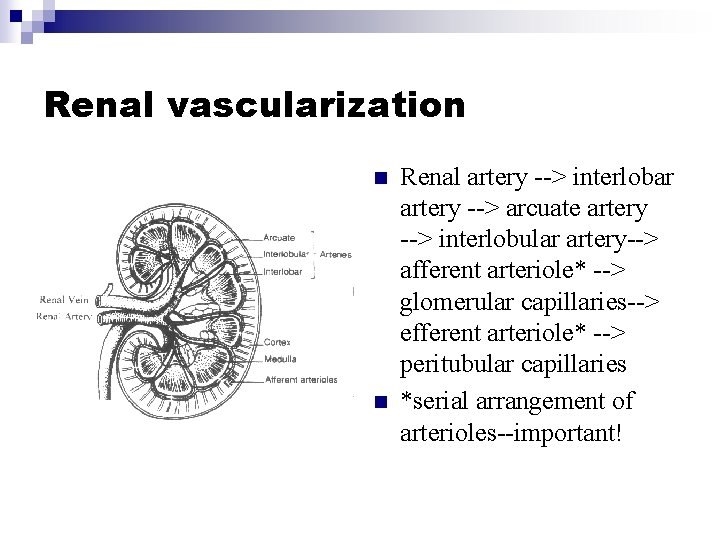
Renal vascularization n n Renal artery --> interlobar artery --> arcuate artery --> interlobular artery--> afferent arteriole* --> glomerular capillaries--> efferent arteriole* --> peritubular capillaries *serial arrangement of arterioles--important!

Juxtamedullary vs. Superficial Nephron n JMN has long Loop of Henle Generates a concentrated urine JMNs are what we lose with age

Renal Clearance and Blood Flow n n n n C. O. = 5. 2 L/min RBF = 1. 2 L/min (20% of cardiac output) RPF =. 66 L/min (plasma = 55% of blood); also equal to the clearance of PAH (filtered and secreted) GFR = Clearance of inulin or creatinine Inulin is filtered but not secreted or reabsorbed Creatinine clearance a slight overestimate of GFR because it is partly secreted (GFR = 0. 9 X Ccreatinine) Filtration Fraction = GFR/RPF, normally 20%
![PAH n n Used to measure RPF Effective RPF UPAH x V PAH n n Used to measure RPF Effective RPF = ([U]PAH x V) /](https://slidetodoc.com/presentation_image/2020f2a747d9965b7815337b5e52dde8/image-13.jpg)
PAH n n Used to measure RPF Effective RPF = ([U]PAH x V) / [P]PAH = CPAH

Clearance Ratio n n CR = Cx/Cin If CR = 1, substance “x” is only being filtered If CR < 1, substance “x” is being reabsorbed If CR > 1, substance “x” is being secreted

GFR: A. B. C. D. E. F. G. Is dependent on hydrostatic pressure inside glomerular capillaries Depends on the oncotic pressure inside glomerular capillaries Is equal to the clearance of inulin Under normal conditions, is rarely dependent on the oncotic pressure inside Bowman’s space Creatinine is used to calculate it Three of the above All of the above

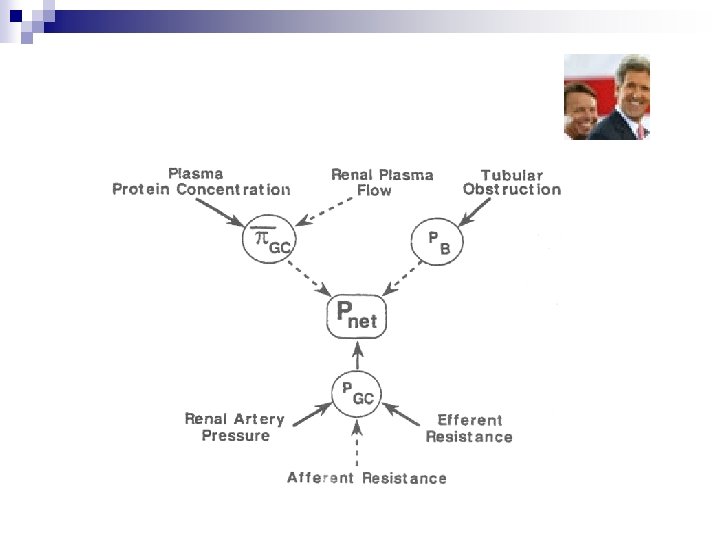
Starling’s Forces of capillary exchange n n GFR = Kf (PGC - PBS - ∏GC) Hypoalbuminemia increases GFR PBS: low unless obstruction present (kidney stones increase GFR) Basement membrane has fixed negative charge--> neg. charged prots can’t get across --> oncotic pressure in Bowman’s space = 0

Cont’d n n n Hydrostatic Pressure is high and relatively constant (due to serial arterioles) Oncotic Pressure increases along length of glomerular capillary (as more fluid is filtered out) Filtration occurs upstream while reabsorption occurs downstream Q: why does a low GFR result in increased reabsorption? A: more time to filter --> oncotic pressure increases


AFFERENT AND EFFERENT ARTERIOLES ARE THE MAJOR SITES OF REGULATED RESISTANCE IN THE RENAL VASCULATURE: Glomerular capillary is unique: 2 sites of vasoconstriction

Autoregulation n Myogenic Mechanism (Bayless): intrinsic reflex mechanism of smooth muscle; increased pressure causes vasoconstriction Tubuloglomerular feedback: macula densa senses increased filtered load of Na. Cl--> sends signals to afferent arteriole to vasoconstrict, thereby decreasing the filtered load (by decreasing GFR back to normal) Both processes serve to keep RBF and GFR constant

Sympathetic Innervation n n There is no parasympathetic input to the kidneys Sympathetic innervation of the afferent and efferent arterioles is the major regulator of RBF and GFR Vasoactive compounds also act on afferent and efferent arterioles: NE, Angiotensin II, Endothelin--> constrict; Ach, NO, PGs, etc --> dilate Low vs. severe sympathetic drive--examples of exercise and hemorrhage

Urine formation n n Ultrafiltration of plasma Reabsorption of H 2 O and solutes from tubular fluid Active and passive processes Transcellular and paracellular (lateral space) transport; latter occurs in proximal tubule due to leaky tight junctions--> ions pass, followed by H 2 O In collecting duct tight jxns are very tight and do not allow passage of water, proteins, or solutes

Solute Regulation in Nephron Segments

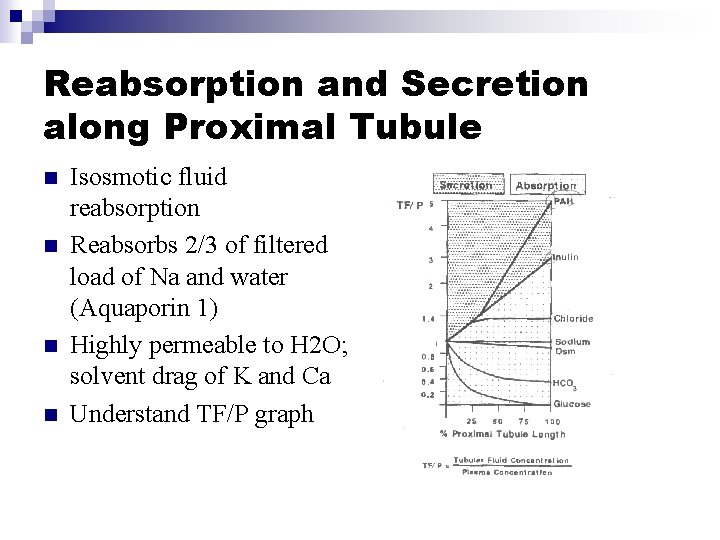
Reabsorption and Secretion along Proximal Tubule n n Isosmotic fluid reabsorption Reabsorbs 2/3 of filtered load of Na and water (Aquaporin 1) Highly permeable to H 2 O; solvent drag of K and Ca Understand TF/P graph

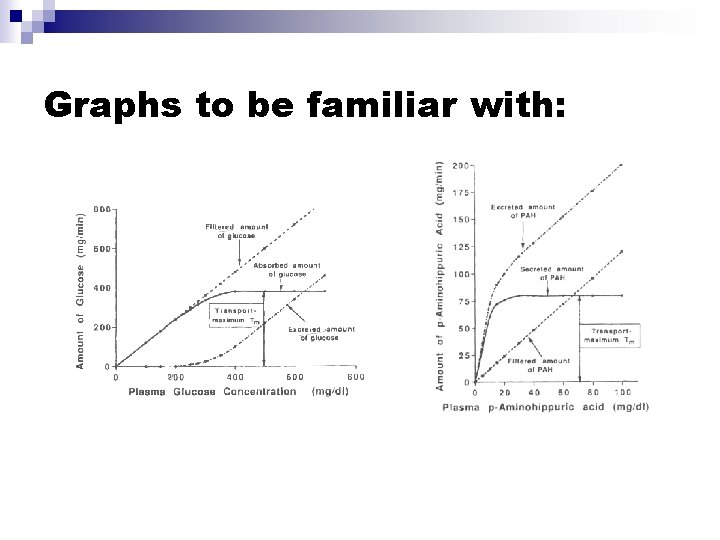
Upper Segment of PT n n n Na cotransported along with bicarb, glc, amino acids, phosphate (luminal membrane) H+ secreted as counter-transport with Na (luminal membrane) Sodium bicarbonate is reabsorbed (basolateral membrane) Under normal conditions, reabsorption will increase as plasma [gluc] increases Once plasma [gluc] reaches a certain level, all glucose carriers in the PT will be saturated, leaving some glucose behind Tm of SGLT-2 (sodium coupled) is 200 g/dl, which is exceeded in diabetics; osmotic diuresis results

Lower Segment of PT n n n Na. Cl reabsorbed transcellularly (1/3) and paracellularly (2/3); due to transepithelial voltage Amino Acids and Bicarbonate have been completely reabsorbed Glucose SGLT-1 (2 Sodium coupled) transporters move glucose against higher gradient

Thick Ascending Limb n n Reabsorbs 1/4 of filtered Na Has the Na-K-2 Cl cotransporter ¨ n n Inhibited by Furosemide (loop diuretic) Impermeable to water; tubular osmolarity decreases (“diluting segment”)--> separation of movement of water and solute Lumen becomes positively charged, causing paracellular transport of Na, K, Ca, and Mg

Early Distal Tubule/Collecting Duct n n Also impermeable to water (like TAL) Continues the dilution of urine; the “cortical diluting segment” Reabsorption of Na/Cl (cotransporter) Inhibited by Thiazide diuretics ¨ Thiazide diuretics unique in that they increase Ca++ reabsorption (Loop diuretics increase Ca++ excretion by diminishing Na. K 2 Cl + lumen effect)

Late Distal Tubule/Collecting Duct: fine tuning n n n n Principal cells--reabsorb Na, H 2 O, and secrete K+ Impermeable to water, except in presence of ADH (Vasopressin) ADH causes water channels to relocate to apical cell membrane (AQUAPORIN 2) Na (transcellularly) and Cl (paracellularly) are reabsorbed Aldosterone causes an increase in Na absorption and increases K secretion Spironolactone (K-sparing) blocks aldosterone; other K-sparing diuretics (Triamterene, Amiloride) act directly on the Na channel, independent of aldosterone Intercalated cells--secrete H+ through primary active transport exchange H+ out of cell for K+ into cell; K+ reabsorption ¨ possess carbonic anhydrase activity for bicarb reabsorption ¨

Miscellaneous Renal Stuff n n n Na+, Ca++ are never “secreted”; rather, fail to reabsorb Prostaglandins released during hypovolemic shock to increase RPF and prevent renal ischemia Aldosterone: promotes Na reabsorption and K secretion (via action on principal cells); also promotes H+ secretion (via action on intercalated cells)-->a link between volume and acid-base regulation Posm = 2[Na] + 2[Glucose] + [BUN] ADH: OSMOREGULATION ALDOSTERONE: Na+/VOLUME REGULATION

Genetic Defects that Target Tenal Transport Mechanisms n n Bartter’s Syndrome: defect in Na. K 2 Cl transporter Gettelman’s Syndrome: defect in Na/Cl cotransporter Liddel’s: defect in ENa. C (turned on) Pseudohypoaldosteronism: defect in ENa. C (turned off--> Na doesn’t get reabsorbed--> volume contraction

Graphs to be familiar with:

WATER BALANCE

n Urine flow rate is never zero n There is an inverse relationship between urine flow and osmolarity n Normal urine osmolarity ≈ 600 m. Osm/L ¨ Range = 50 - 1200!! (kidneys can concentrate urine up to 4 x the plasma concentration)

Control Mechanisms of Osmoregulation n Osmoreceptors Increase in plasma osm--> hypothalamus stimulated to release ADH (hypothalamic set point ≈ 285 m. Osm/L solution) ¨ Respond to < 2% change in plasma osmolarity ¨ Most important control in osmoregulation ¨ n Baroreceptors Respond to changes in Blood Pressure ¨ Require a 15 -20% change in BP before activation ¨

Disorders of Osmoregulation n Psychogenic Polydipsia, Hypothalamic/Central Diabetes Insipidus: low ADH n Nephrogenic Diabetes Insipidus: ineffective ADH (kidney unable to respond to ADH)

Mechanisms to Concentrate Urine n Countercurrent Multiplication--creation of osmotic gradient Loop of Henle ¨ Generates a urine that is concentrated as high as 600 mosm/L ¨ n Urea recycling Medullary Collecting Duct ¨ Needed to increase the osmolar gradient from 600 to 1200 mosm/L ¨ Kidneys use urea to do osmotic work when in state of antidiuresis ¨ n Countercurrent exchange--vasa recta maintains the medullary insterstitial osmotic gradient set up by the countercurrent multiplier

Diuresis vs Antidiuresis n n n Understand the diagrams on p. 9 Water diuresis: most concentrated urine just before ascending limb and TAL; most dilute at end of CD Antidiuresis: most concentrated in lumen at level of renal papillae (in medulla); most dilute at TAL

SODIUM REGULATION

Renin, Angiotensin, Aldosterone n Renin secretion stimulated by: Decrease in effective circulating volume (decreased pressure at afferent arteriole) ¨ Increase in sympathetic nerve activity ¨ Tubuloglomerular feedback (decreased Na load sensed by macula densa, causing renin release) ¨ n Angiotensin II: Arteriolar constriction--> increases TPR ¨ Increases Aldosterone ¨ Increases ADH and thirst ¨ n Aldosterone causes: Na reabsorption at principal cells ¨ K secretion in CD ¨
![Aldosterone secretion n n Increased by ACTH Angiotensin II high plasma K cases of Aldosterone secretion: n n Increased by ACTH, Angiotensin II, high plasma [K+], cases of](https://slidetodoc.com/presentation_image/2020f2a747d9965b7815337b5e52dde8/image-41.jpg)
Aldosterone secretion: n n Increased by ACTH, Angiotensin II, high plasma [K+], cases of volume contraction Decreased by *ANP* and high plasma Na+ (feedback inhibition) ¨ ANP: OPPOSES RAAS; increases Na+ excretion during cases of volume expansion (cardiac myocytes are stretched) Note: Na+ alterations do not affect plasma osmolarity, rather they affect the effective circulating volume; H 2 O homeostasis and ADH determine plasma osmolarity

Aldosterone escape A protective mechanism during cases of abnormal aldosterone elevation (example of adrenal tumor); system becomes insensitive to aldosterone.

Renal Physiology Lectures 41 to 48 Rahul Dave’ (rdave 2@uic. edu)

I can’t go through everything in detail. Know the handout. My goal is to make this make sense to you, and orient your studying. Pay attention to major vs minor factors. Minor doesn’t mean less important to study, but helps you keep changes in perspective You need to memorize the regulation, etc … and understand the logic. It’s easy to talk yourself into something wrong.

Potassium Balance

K+ distribution and homeostasis n Plasma K is low … must be controlled well ¨ Determines membrane potential n Metabolic alkalosis causes hypokalemia (and vice -versa) n Rules of thumb: understand mechanisms ¨ Na and K go opposite

K+ Transport See diagrams in handout for cellular transport pathways in different sections

Regulation of K+ MAJOR FACTORS K+ itself (K promotes its own secretion) Aldosterone (Na+ excr. , K+ reabs. , H+ excr. ) MINOR FACTORS Tubular flow increases secretion ADH no net effect Alkalosis (acute) increases secretion Tubular Na+ increases secretion Insulin Increase reabsorption Epinephrine Decreases secretion (fight/flight)

Diuretics See diagrams of cell transport pathways

Control of Circulating Volume

n Small fraction of TBW … can’t detect it directly. Also, since detection and changes are indirect, the changes must occur slowly n Measured by BP (myogenic feedback) or [Na+] (tubuloglomerular) n Controlled by changing Na+

Volume Sensors & Effectors Baroreceptors … detect pressure n Central (Left atrium; carotid sinus) ¨ n ADH Na reabs; collecting duct permeability Intrarenal volume sensors Pressure: myogenic feedback ¨ Na (also K & Cl, maybe): tubuloglomerular ¨ n n Low ECF volume makes you thirsty Sympathetic overdrive (fight/flight) – conserve water & ↓ peripheral blood flow

Mechanisms Controlling ECF • Cardiac atria … secrete ANP … lowers GFR • Aortic Arch Baroreceptor … Sympathetic system • Macula Densa … Renin-Ang-Ald System • Hydrostatic/Oncotic pressure balance • Adrenal Cortex … hormones like aldosterone All of these affect Na+ balance!

Calcium and Phosphate Balance

Rules of Thumb: Ca 2+ Hitchhiking only takes you so far. But try to understand why & how these are true. In the PCT & TAL: Ca 2+ follows Na+ paracellularly In the DCT & CD: Ca 2+ is regulated by PTH

Rules of Thumb: PO 43 Try to understand why & how these are true. In the nephron it undergoes paracellular transport Controlled by PTH in the proximal tubule

PTH n Phosphate Trashing Hormone in urine Absorb (P) from gut & bone to incr. plasma (P) ¨ Excrete it in the urine n But Ca 2+ and PO 4 can’t be together ¨ n So if (P) is low, Ca 2+ is high, and vice-versa n PTH, not calcitonin, is a major controller of Ca 2+.

Vitamin D Synthesis n n This is a stupid detail, but winds up being tested sometimes (No promises about Hudson) Vit D is synthesized in liver & Kidney D (liver) 1 -OH-D (kidney) 1, 25 -OH-D You need Vitamin D to absorb Ca 2+ Think: Vit-D fortified milk

Acid-Base: Basics

Removing Acid or Base n Buffers Blood ¨ Intracellular ¨ n Lung ¨ “compensated state” seconds minutes hours n Kidneys days n Net acid excretion counts NH 4, Titratable Acid, HCO 3 - Titratable (weak) acids include lactic acid, ketone bodies, etc. ¨ Strong acids are secreted as their Na salts (eg, Na 2 SO 4) ¨
![Buffering Mechanisms HCO 3 24 p H 6 1 log Buffering Mechanisms [HCO 3 -] = 24 p. H = 6. 1 + log](https://slidetodoc.com/presentation_image/2020f2a747d9965b7815337b5e52dde8/image-61.jpg)
Buffering Mechanisms [HCO 3 -] = 24 p. H = 6. 1 + log ————— = 7. 4 0. 03 x P-CO 2 = 40 Know this and make sure you can calculate it!

Lung Mechanisms n CO 2 is an acid and gets blown out by respiration. ¨ So when you sprint, you develop lactic acidosis. This is metabolic acidosis. To get rid of the acid, you hyperventilate and breathe faster.

Kidney Mechanisms Mainly by HCO 3 H 2 O + CO 2 CA H 2 CO 3 HCO 3 - + H+

Kidney: HCO 3 n n Locations: look at cell diagrams Regulation ¨ Proximal tubule: follows Na+ (understand why) ¨ ¨ Na/H antiport. Whenever one H+ exits, a tubular HCO 3 - is used up to neutralize it. Also, to regenerate that H+, a HCO 3 is made, which is transported to the blood. Systemic Acidosis (in PCT, Henle, CD)

Kidney: H+ n H+ is usually tied to other ions n In the intercalated cell of collecting duct, there is a ATP-dependent H+ pump that secretes H+ n Upregulated by aldosterone

Nitrogen Removal (NH 3 or NH 4+) The mechanisms are complicated Know that H+ acidifies & traps NH 3 in the lumen (as NH 4+) K+ also regulates NH 4+ production … don’t worry (The mechanisms are important if you want to do really well)

Clinical Evaluation of Acid-Base Disorders the simple way …

Q 1. Acidosis or Alkalosis? n Remember compensation is never 100% n p. H < 7. 4 …. Acidosis n p. H > 7. 4 …. Alkalosis n p. H = 7. 4 …. . You’re fine (or … mixed)

Metabolic or Respiratory n If it’s acidosis (or alkalosis) look for the source of acid (or base) n HCO 3 < 24 HCO 3 > 24 metabolic n CO 2 > 40 CO 2 < 40 respiratory

Compensated or Uncompensated? Check with the formulas … Fig 43. 23 in Berne & Levy n I’m not sure whether he gave you these formulas. If he didn’t don’t worry. n Check the nomogram … ¨ It will tell you acute vs chronic.

Is it Mixed? Note that HCO 3 - and CO 2 move in opposite directions If they move in the same direction … you have a mixed disorder.

Clinical Causes … n Metabolic Acidosis: Diabetic ketoacidosis, diarrhea n Metabolic Alkalosis: antacid, vomiting (will loose Cl too) n Respiratory Acidosis: Hypoventiliation, pulmonary edema n Respiratory Alkalosis: Hyperventilation

Cell Diagrams You can find these in Costanzo, Hudson’s H/O or Berne & Levy. Best study tool: Draw these out yourself. Know them cold.

Stone Kidneys are cool …. Good luck ….