Relationship Between the Chronic Care Model and Diabetes

Relationship Between the Chronic Care Model and Diabetes Outcomes Laurie Hurowitz, Ph. D, Benjamin Littenberg, MD, and Charles D. Mac. Lean, MDCM General Internal Medicine, College of Medicine Academy. Health, Boston, MA, June 28, 2005

Context: Chronic Illness Care • Current health care services are designed to deliver acute care • Need to redesign health care to deliver: – more effective preventive services – more effective services to those with one or more chronic illnesses

The Chronic Care Model (CCM) Community Resources & Policies Organization of Care Health System Organization Delivery System Design Decision Support Clinical Information Systems Self-Management Support Informed, Activated Patient Productive Interactions Functional and Clinical Outcomes Prepared, Proactive Practice Team

Current Research CCM & Outcomes • Most research has focused on elements of the CCM and outcomes, and not the model as a whole. • Clinical Tool: Assessment of Chronic Illness Care – pre/post measure, sensitive to organizational change.

Research Question What is the relationship between primary care practice organization across all components of the Chronic Care Model and glycemic control for patients with diabetes?

Methods • Design - Cross-sectional, observational study • Subjects - Adults diagnosed with diabetes in care in primary care practices in a rural VT, NH, and NY. • 2 measures

Predictor Measure The Assessment of Diabetes Care, adapted from the Assessment of Chronic Illness Care version 3. 5 (organizational change - organizational status) • 33 prompts/stems • 12 -point response scale – descriptors provided • Subscale scores (0 -11); overall score is average (0 -11) • Practice average – average across all practitioners Higher scores are associated with greater conformance with the CCM.

Sample Item Subscale: Overall System of Health Care Overall Goals for Diabetes Care (circle one) : 0 1 2 Do not exist. 3 4 5 6 7 8 9 10 11 Exist but are not Are measurable, reviewed actively reviewed. and reviewed. routinely, and incorporated into plans for improvement.

Outcome Measure Glycosylated hemoglobin, as measured by the A 1 C assay (A 1 C) Source: • adult patients diagnosed with diabetes • Practice average - baseline measure from the Vermont Diabetes Information System (VDIS) For patients with diabetes, lower A 1 Cs are associated with better clinical outcomes. Even small decreases are related to improving the burden of diabetes.
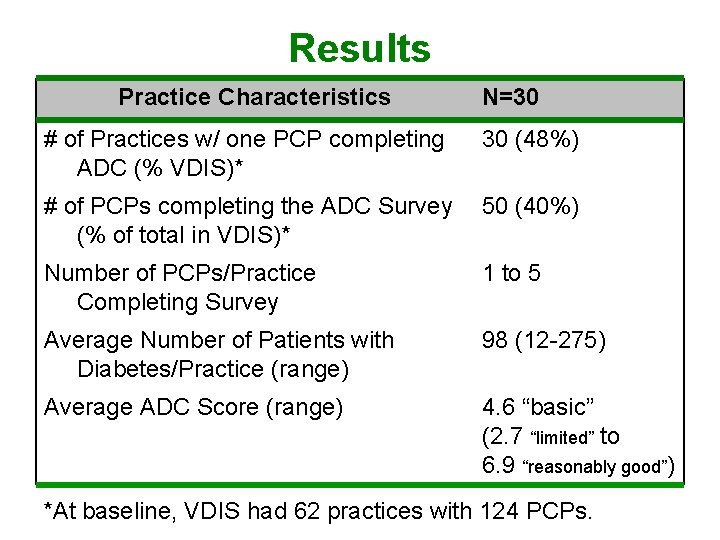
Results Practice Characteristics N=30 # of Practices w/ one PCP completing ADC (% VDIS)* 30 (48%) # of PCPs completing the ADC Survey (% of total in VDIS)* 50 (40%) Number of PCPs/Practice Completing Survey 1 to 5 Average Number of Patients with Diabetes/Practice (range) 98 (12 -275) Average ADC Score (range) 4. 6 “basic” (2. 7 “limited” to 6. 9 “reasonably good”) *At baseline, VDIS had 62 practices with 124 PCPs.
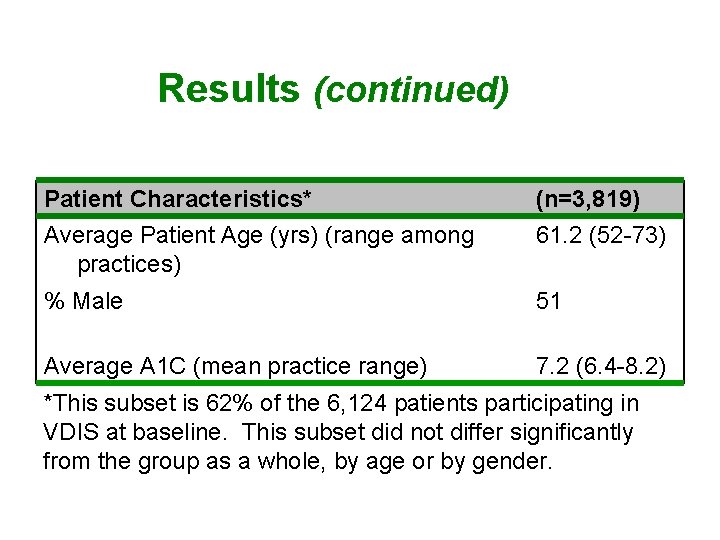
Results (continued) Patient Characteristics* (n=3, 819) Average Patient Age (yrs) (range among practices) 61. 2 (52 -73) % Male 51 Average A 1 C (mean practice range) 7. 2 (6. 4 -8. 2) *This subset is 62% of the 6, 124 patients participating in VDIS at baseline. This subset did not differ significantly from the group as a whole, by age or by gender.
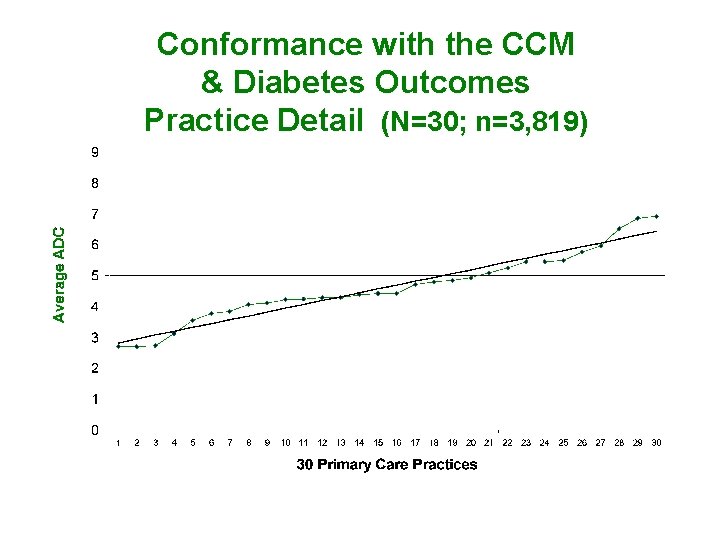
Conformance with the CCM & Diabetes Outcomes Practice Detail (N=30; n=3, 819)
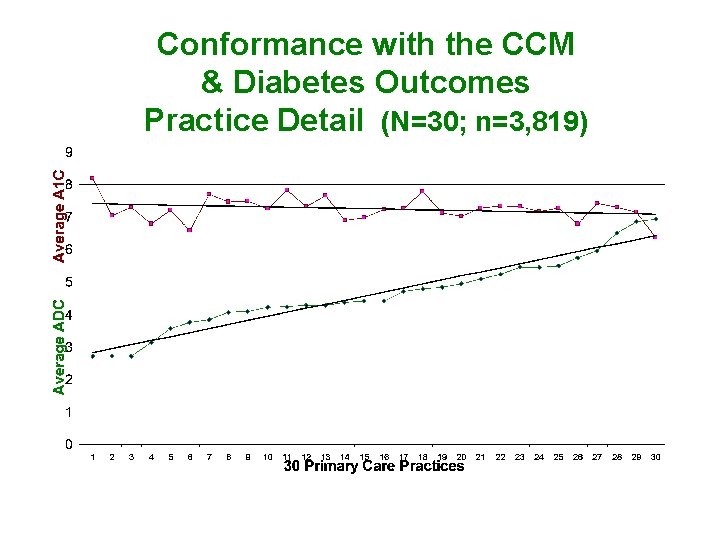
Conformance with the CCM & Diabetes Outcomes Practice Detail (N=30; n=3, 819)
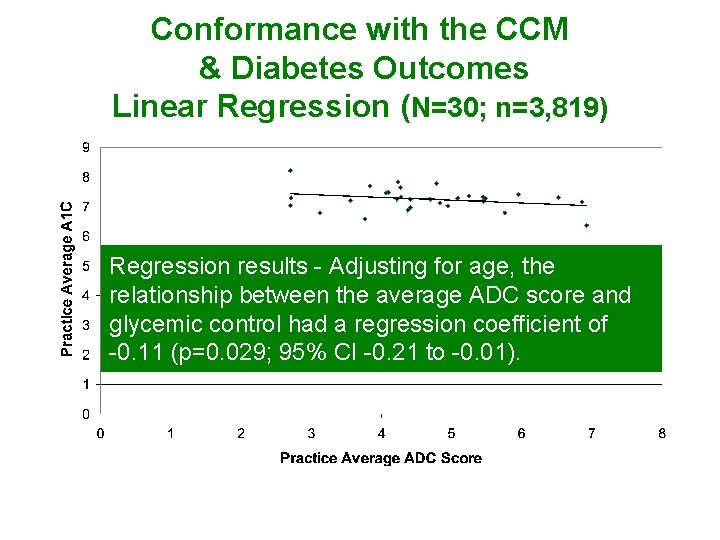
Conformance with the CCM & Diabetes Outcomes Linear Regression (N=30; n=3, 819) Regression results - Adjusting for age, the relationship between the average ADC score and glycemic control had a regression coefficient of -0. 11 (p=0. 029; 95% CI -0. 21 to -0. 01).

Conclusions Patients who receive care in practices that conform to the Chronic Care Model have better glycemic control. This study lends support to the overall validity of the Chronic Care Model and its relationship to better outcomes for patients with diabetes.

References • Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness. JAMA 2002, Oct 9; 288(14): 1775 -9 and Part 2. JAMA 2992 Oct 16: 288(15): 1909 -14. • Bonomi AE, Wagner EH, Glasgow R, Vonkroff M. Assessment of chronic illness care: a practical tool for quality improvement. Health Services Research. 2002; 37(3): 791 -820. • Mac. Lean CD, Littenberg B, Gagnon M, Reardon M, Turner PD and Jordan C. The Vermont Diabetes Information System (VDIS): study design and subject recruitment for a cluster randomized trial of a decision support system in a regional sample of primary care practices. Clinical Trials. 2004; 1: 532 -544. • Shojania KG, Ranji SR, Shaw LK, Charo LN, Lai JC, Rushakoff RJ, Mc. Donald KM, Owens DK. Diabetes mellitus care. Closing the quality gap: a critical analysis of quality improvement strategies, Vol 2. Technical review 9, AHRQ Pub no. 04 -0051 -2. Rockville, MD. Sept 2004. • The Chronic Care Model and Clinical Tools. www. improvingchroniccare. org. • The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993; 329: 977 -986. • Wagner EH, Glasgow RE, Davis C, Bonomi AE, Provost L, Mc. Culloch D, Carver P, Sixta C. Quality improvement in chronic illness care: a collaborative approach. Jt Comm J Qual Improv 2001 Feb; 27(2): 63 -80.

How to Contact Us & Study Support For further information, please contact: Laurie. Hurowitz@uvm. edu This study was supported by the National Institute of Diabetes and Digestive and Kidney Disease (K 24 DK 068380 and R 01 DK 61167)
- Slides: 17