Rehabilitation of Spinal Cord Injury Dr Shereen Fawaz

Rehabilitation of Spinal Cord Injury Dr. Shereen Fawaz, Ph. D, MRCP Lecturer of Physical Medicine, Rheumatology & Rehabilitation, Ain Shams university 1 Dr. Shereen Fawaz

Intended Anatomy of the spine Functional Types Learning Outcomes: neuroanatomy of SCI Clinical and functional Assessment of SCI Complications Management of Spinal cord injury and Rehabilitation of SCI 2 Dr. Shereen Fawaz
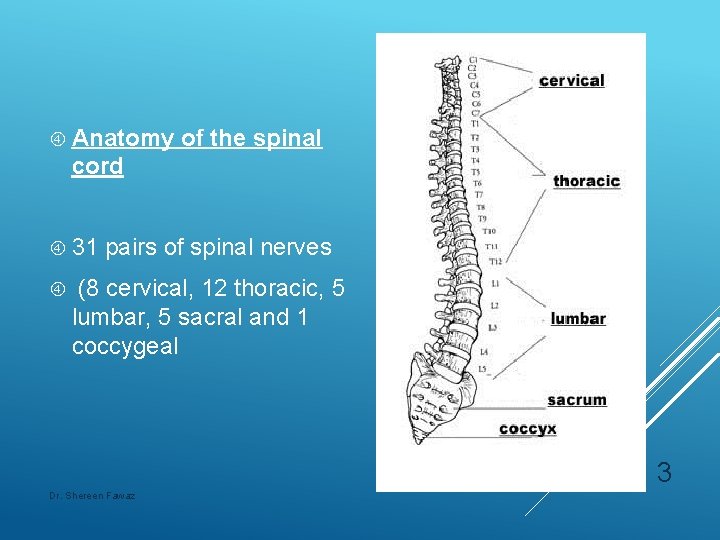
Anatomy of the spinal cord 31 pairs of spinal nerves (8 cervical, 12 thoracic, 5 lumbar, 5 sacral and 1 coccygeal 3 Dr. Shereen Fawaz
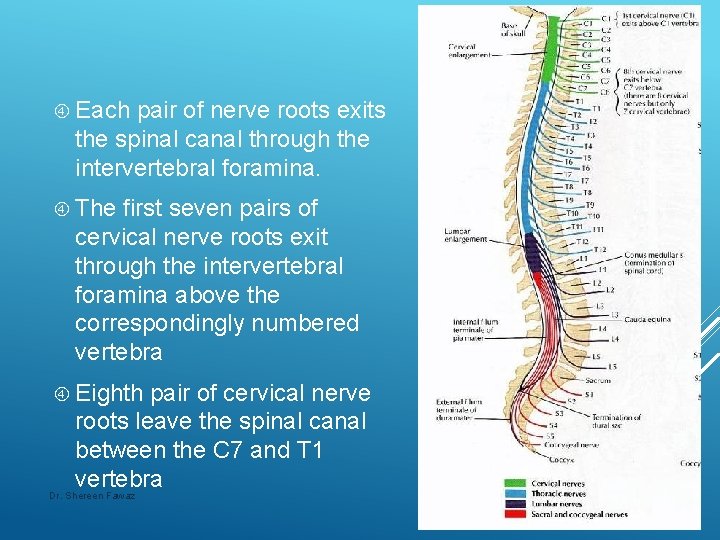
Each pair of nerve roots exits the spinal canal through the intervertebral foramina. The first seven pairs of cervical nerve roots exit through the intervertebral foramina above the correspondingly numbered vertebra Eighth pair of cervical nerve roots leave the spinal canal between the C 7 and T 1 vertebra Dr. Shereen Fawaz 4
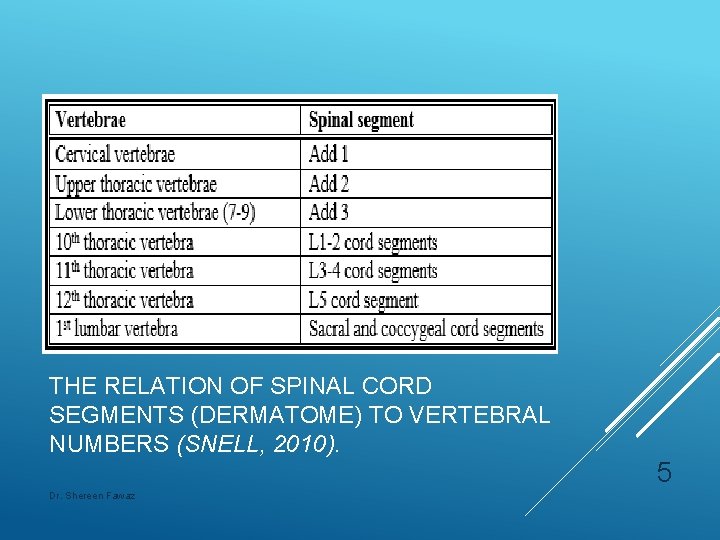
THE RELATION OF SPINAL CORD SEGMENTS (DERMATOME) TO VERTEBRAL NUMBERS (SNELL, 2010). Dr. Shereen Fawaz 5
Arterial Blood Supply of the spinal Cord; Anterior Spinal Artery: One anterior and two posterior branches arise from each vertebral artery. Posterior Spinal Artery: from the vertebral arteries. posterior one-third of the spinal cord. 6 Dr. Shereen Fawaz

The autonomic nervous system: • Sympathetic • Parasympathetic. Mainly located in the lateral funiculi and end in the preganglionic sympathetic and parasympathetic neurons located in the brainstem and at the levels of T 1–L 2 and S 2–S 4. 7 Dr. Shereen Fawaz
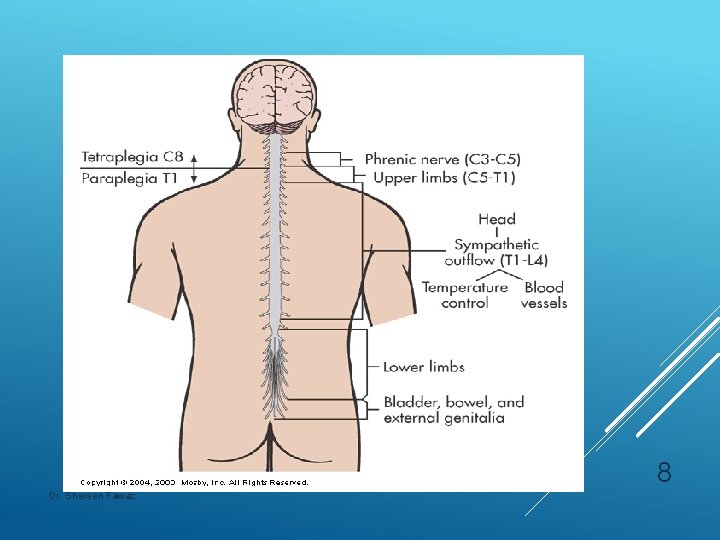
8 Dr. Shereen Fawaz

TYPES OF SCI Traumic Non traumatic 1. Cervical 1. Motor Neuron Diseases 2. Thoracic 2. Spondylotic Mylopathies 3. Lumbar 3. 4. Sacral Infectious and Inflammatory diseases 5. Multiple 4. Neoplastic 6. Non specified 5. Vascular Disorders 6. Toxic and metabolic conditions 7. Congenital disorders (SCIWRA) Dr. Shereen Fawaz 9
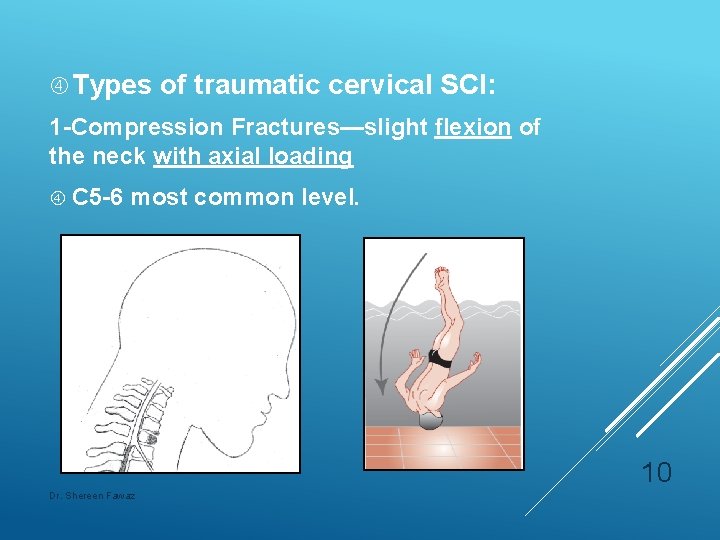
Types of traumatic cervical SCI: 1 -Compression Fractures—slight flexion of the neck with axial loading C 5 -6 most common level. 10 Dr. Shereen Fawaz

2 -Flexion-Rotation Mostly Injuries with unilateral facet dislocation. Unstable if the PLL disrupted. Vertebral body less than 50% displaced n x- ray. 11 Dr. Shereen Fawaz
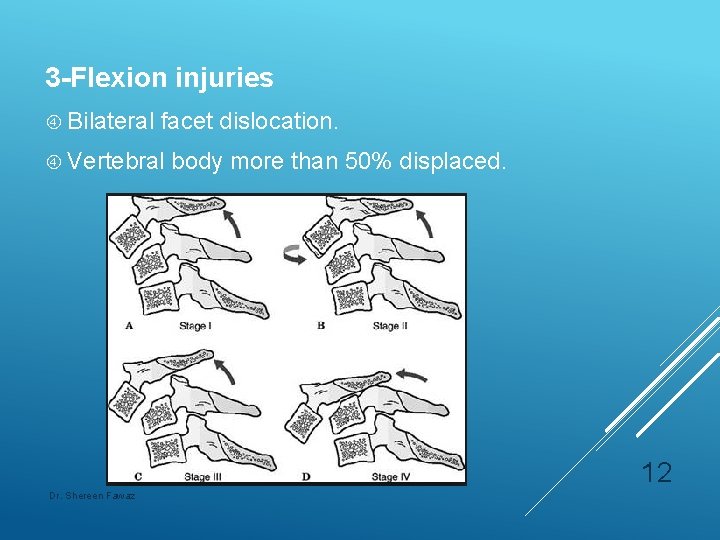
3 -Flexion injuries Bilateral facet dislocation. Vertebral body more than 50% displaced. 12 Dr. Shereen Fawaz
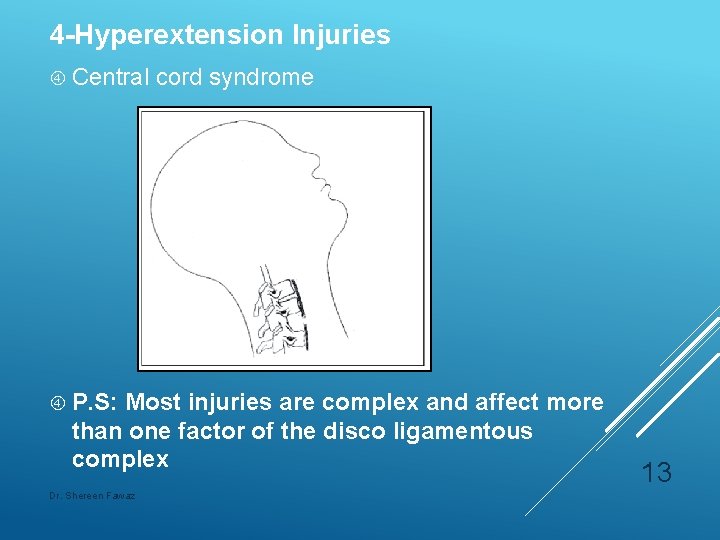
4 -Hyperextension Injuries Central cord syndrome P. S: Most injuries are complex and affect more than one factor of the disco ligamentous complex Dr. Shereen Fawaz 13

SCIWORA Common in children and older adults Mostly hyperextension injury causing acute central cord syndrome 14 Dr. Shereen Fawaz
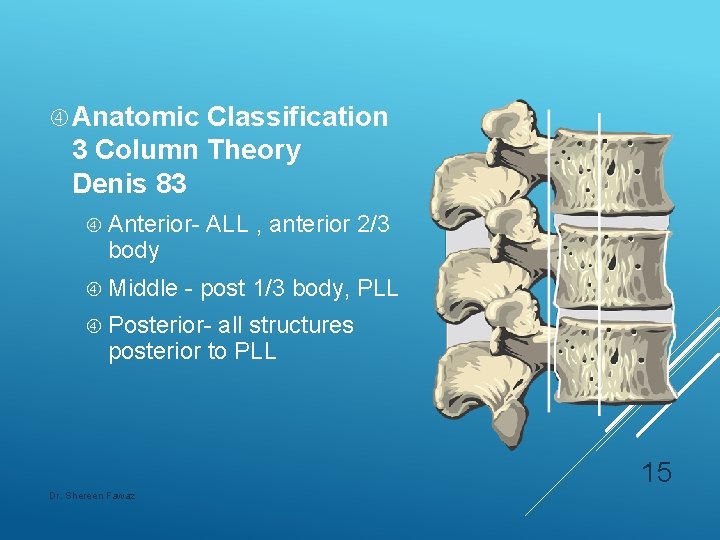
Anatomic Classification 3 Column Theory Denis 83 Anterior- body Middle ALL , anterior 2/3 - post 1/3 body, PLL Posterior- all structures posterior to PLL 15 Dr. Shereen Fawaz

n Middle column is the primary determinant of mechanical stability of the thoracolumbar region of the spine. n Middle column fracture is unstable fracture n Anterior column fracture is a stable fracture n Posterior column fracture is a stable fracture n Any 2 column fracture is an unstable fracture 16 Dr. Shereen Fawaz

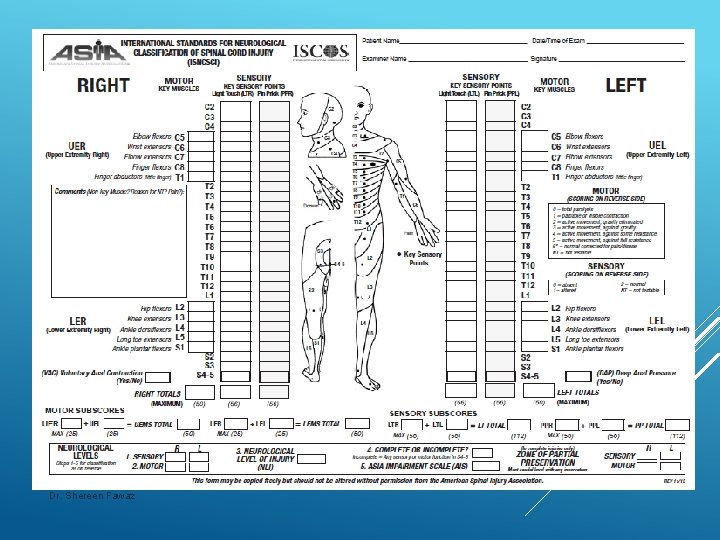
Clinical Evaluation of Chronic SCI 1. History 2. Physical Examination include: cardiac, chest, abdominal and musculoskeletal (Joints ROM), Pain assessment, . . etc 3. Neurological Examination for associated injuries e. g TBI. . 4. ASIA score for spinal cord Injury (2016) 17 Dr. Shereen Fawaz
18 Dr. Shereen Fawaz

19 Dr. Shereen Fawaz

Classification according to ASIA is based on four components: Neurologic Complete ASIA level of lesion or incomplete lesion Impairment Scale Grade Zone of partial preservation (ZPP) for complete lesions 20 Dr. Shereen Fawaz

21 Dr. Shereen Fawaz

ASIA Impairment Scale (AIS) (2016): A = Complete. No sensory or motor function is preserved in the sacral segments S 4 -5. B = Sensory Incomplete. Sensory but not motor function is preserved below the neurological level and includes the sacral segments S 4 -5 (light touch or pin prick at S 4 -5 or deep anal pressure) AND no motor function is preserved more than three levels below the motor level on either side of the body. Dr. Shereen Fawaz 22

C = Motor Incomplete. Motor function is preserved at the most caudal sacral segments for voluntary anal contraction (VAC) OR the patient meets the criteria for sensory incomplete status (sensory function preserved at the most caudal sacral segments (S 4 -S 5) by LT, PP or DAP), and has some sparing of motor function more than three levels below the ipsilateral motor level on either side of the body. (This includes key or non-key muscle functions to determine motor incomplete status. ) For AIS C – less than half of key muscle functions below the single NLI have a muscle grade ≥ 3. Dr. Shereen Fawaz 23

D = Motor Incomplete. Motor incomplete status as defined above, with at least half (half or more) of key muscle functions below the single NLI having a muscle grade ≥ 3. 24 Dr. Shereen Fawaz

E = Normal. If sensation and motor function as tested with the ISNCSCI are graded as normal in all segments, and the patient had prior deficits, then the AIS grade is E. Someone without an initial SCI does not receive an AIS grade. Using ND: To document the sensory, motor and NLI levels, the ASIA Impairment Scale grade, and/or the zone of partial preservation (ZPP) when they are unable to be determined based on the examination results. 25 Dr. Shereen Fawaz

ASIA MYOTOMES C 5 – Elbow flexors L 2 – Hip flexion C 6 – Wrist extensors L 3 – Knee extension C 7 – Elbow extension L 4 – Ankle dorsiflexion C 8 – Finger flexors L 5 – Long toe extension T 1 – 5 th digit abduction S 1 – Ankle plantar flexion 26 Dr. Shereen Fawaz

27 Dr. Shereen Fawaz

When to Test Non-Key Muscles: In a patient with an apparent AIS B classification, non-key muscle functions more than 3 levels below the motor level on each side should be tested to most accurately classify the injury (differentiate between AIS B and C). 28 Dr. Shereen Fawaz
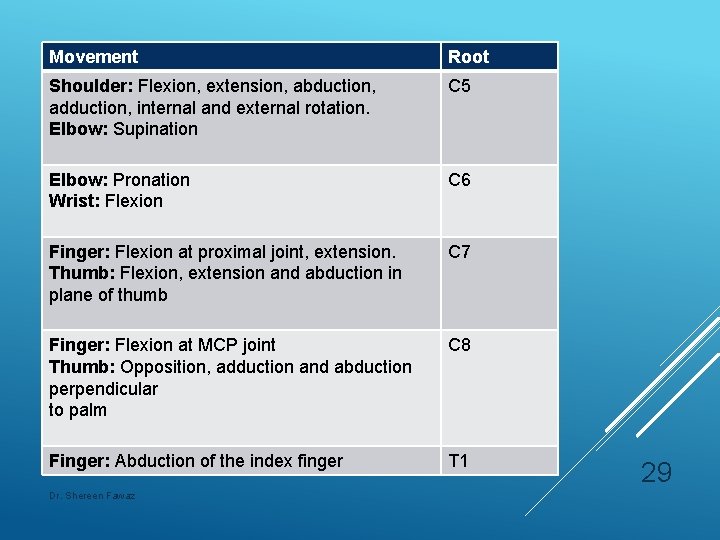
Movement Root Shoulder: Flexion, extension, abduction, adduction, internal and external rotation. Elbow: Supination C 5 Elbow: Pronation Wrist: Flexion C 6 Finger: Flexion at proximal joint, extension. Thumb: Flexion, extension and abduction in plane of thumb C 7 Finger: Flexion at MCP joint Thumb: Opposition, adduction and abduction perpendicular to palm C 8 Finger: Abduction of the index finger T 1 Dr. Shereen Fawaz 29
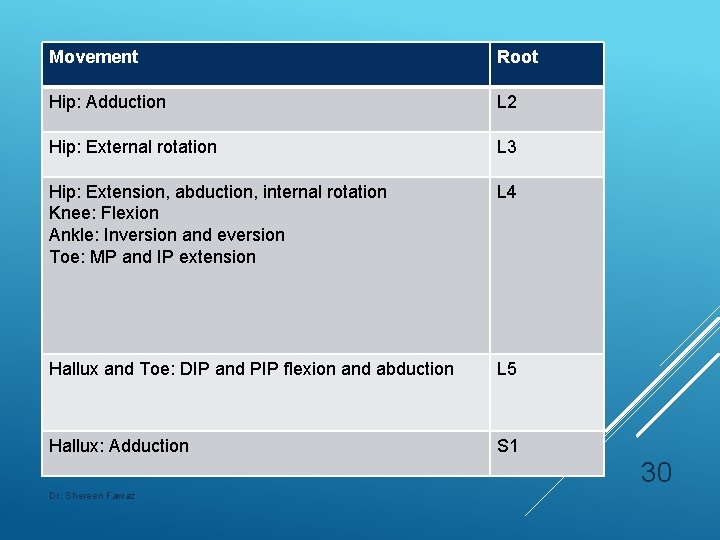
Movement Root Hip: Adduction L 2 Hip: External rotation L 3 Hip: Extension, abduction, internal rotation Knee: Flexion Ankle: Inversion and eversion Toe: MP and IP extension L 4 Hallux and Toe: DIP and PIP flexion and abduction L 5 Hallux: Adduction S 1 30 Dr. Shereen Fawaz

Sensory 0 Grading = Absent 1 = Altered, either decreased/impaired sensation or hypersensitivity 2 = Normal NT = Not testable 31 Dr. Shereen Fawaz
Level of Lesion: Neurological level of lesion: The most caudal spinal cord segment with normal sensory and motor function. Sensory level: The most caudal spinal cord segment with normal (2/2) sensory function for light touch and pain (Pin Prick). Motor level: The most caudal key muscle group that is graded three-fifths or greater with the segments above graded five-fifths in strength. 32 Dr. Shereen Fawaz

Steps in Classification The following order is recommended for determining the classification of individuals with SCI. 1. Determine sensory levels for right and left sides. The sensory level is the most caudal, intact dermatome for both pin prick and light touch sensation. 33 Dr. Shereen Fawaz

2. Determine motor levels for right and left sides. Defined by the lowest key muscle function that has a grade of at least 3 (on supine testing), providing the key muscle functions represented by segments above that level are judged to be intact (graded as a 5). Note: in regions where there is no myotome to test, the motor level is presumed to be the same as the sensory level, if testable motor function above that level is also normal. 34 Dr. Shereen Fawaz
3. Determine the neurological level of injury (NLI) This refers to the most caudal segment of the cord with intact sensation and antigravity (3 or more) muscle function strength, provided that there is normal (intact) sensory and motor function rostral respectively. The NLI is the most cephalad of the sensory and motor levels determined in steps 1 and 2. 35 Dr. Shereen Fawaz

4. Determine whether the injury is Complete or Incomplete. (i. e. absence or presence of sacral sparing) If voluntary anal contraction = No AND all S 4 -5 sensory scores = 0 AND deep anal pressure = No, then injury is Complete. Otherwise, injury is Incomplete. 36 Dr. Shereen Fawaz

Determine ASIA Impairment Scale (AIS) Grade: 1 If Is injury Complete? yes- determine ZPP 2 - If No, determine B-C-D-E 37 Dr. Shereen Fawaz

Assessment of Spinal Shock After severe SCI, there is a state of complete spinal areflexia. The spinal shock is classically evaluated by bulbocavernosus reflux S 3 -4 During the shock stage, no determination can be made regarding the completeness of the lesion. After 24 -48 hours, most patients emerge fro spinal shock, if still no sacral function the lesion is termed complete. 38 Dr. Shereen Fawaz
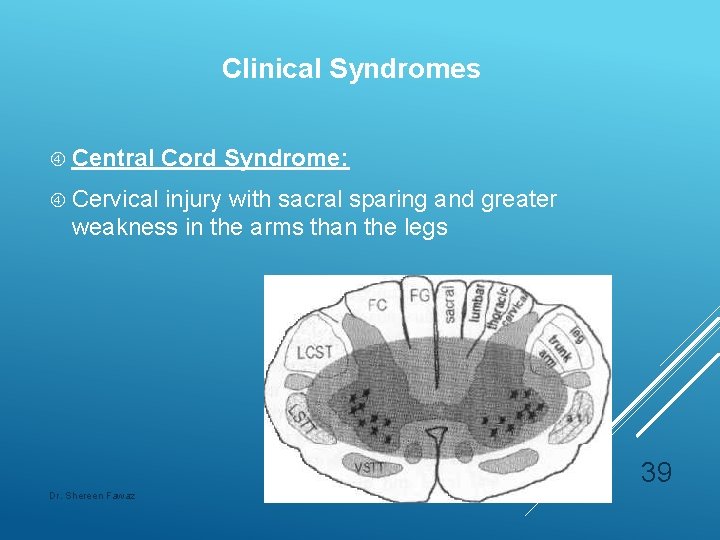
Clinical Syndromes Central Cord Syndrome: Cervical injury with sacral sparing and greater weakness in the arms than the legs 39 Dr. Shereen Fawaz
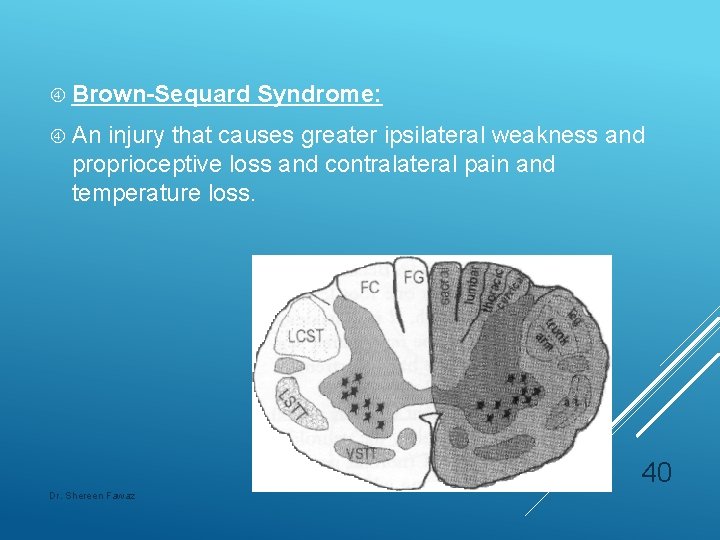
Brown-Sequard Syndrome: An injury that causes greater ipsilateral weakness and proprioceptive loss and contralateral pain and temperature loss. 40 Dr. Shereen Fawaz
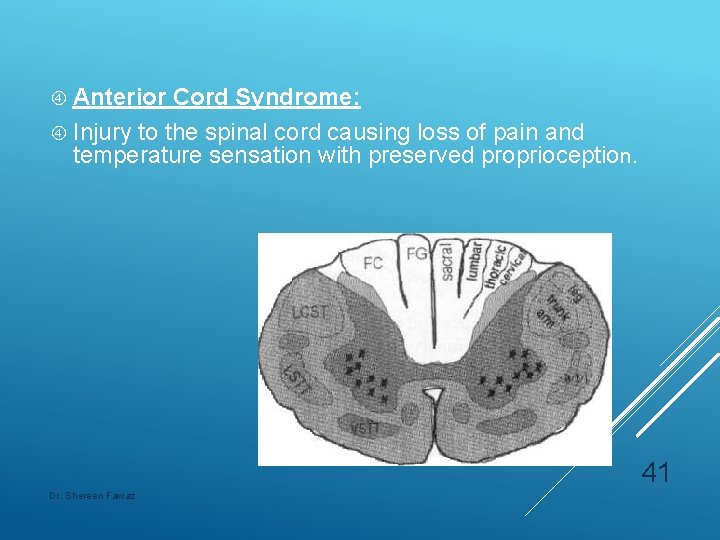
Anterior Cord Syndrome: Injury to the spinal cord causing loss of pain and temperature sensation with preserved proprioception. 41 Dr. Shereen Fawaz
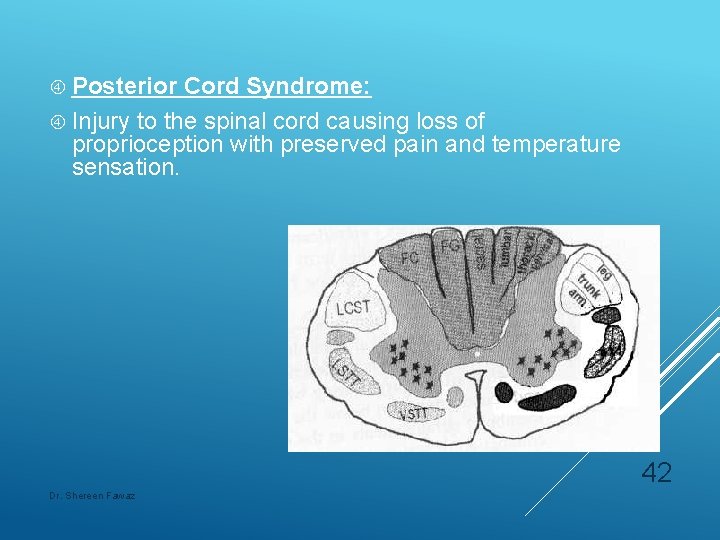
Posterior Cord Syndrome: Injury to the spinal cord causing loss of proprioception with preserved pain and temperature sensation. 42 Dr. Shereen Fawaz
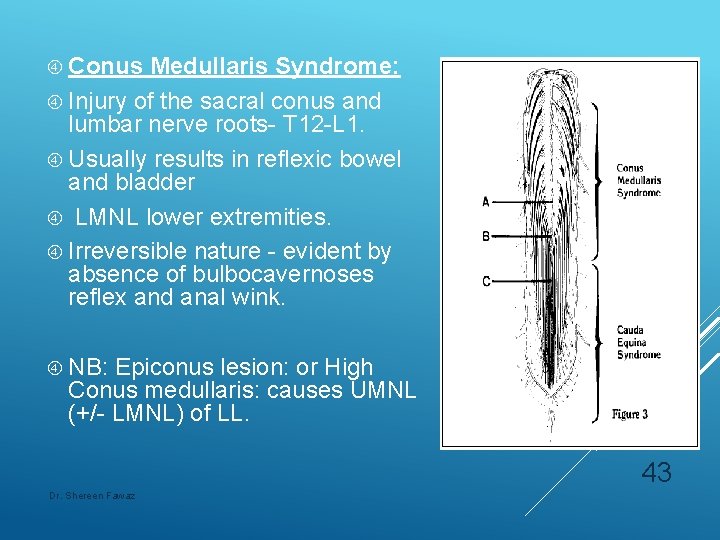
Conus Medullaris Syndrome: Injury of the sacral conus and lumbar nerve roots- T 12 -L 1. Usually results in reflexic bowel and bladder LMNL lower extremities. Irreversible nature - evident by absence of bulbocavernoses reflex and anal wink. NB: Epiconus lesion: or High Conus medullaris: causes UMNL (+/- LMNL) of LL. 43 Dr. Shereen Fawaz

Cauda Equina Syndrome: Injury to the lumbosacral nerve roots within the neural canal. Areflexic bowel and bladder and lower limbs. Injury to nerve rootlets has better prognosis. Functional assessment of SCI FIM SCIM 44 Dr. Shereen Fawaz

Investigations CT MRI NCV and EMG MEP, Inv. ss. EP for complications associated with SCI 45 Dr. Shereen Fawaz

Complications following SCI T 6 and above: Individuals with SCI are considered to be at risk of: 1. Autonomic Dysreflexia 2. Orthostatic Hypotension If lesion above T 8: Patient cannot regulate and maintain normal body temperature (Poikilothermia) 46 Dr. Shereen Fawaz
CARDIOVASCULAR COMPLICATIONS FOLLOWING SCI Direct 1 - Orthostatic Hypotension Ø 2 - Cardiac arrhythmias Ø 3 -Autonomic dysreflexia Indirect 1 - Venous thromboembolism Reduced cardiovascular fitness and altered exercise capacity Lipid abnormalities, insulin resistance and hyperinsulinemia 47 Dr. Shereen Fawaz

1 -ORTHOSTATIC HYPOTENSION Lack of sympathetic outflow, triggered by tilt of patient > 60 degrees Normal Mechanism • Upright position → ↓ BP→ + Carotid body baroreceptors sense → ↑ sympathetic outflow. 48 Dr. Shereen Fawaz

Resultant Symptoms 1. Hypotension 2. Tachycardia 3. Patient can lose consciousness Treatment 1. Reposition—Trendelenburg/daily tilt table/recliner wheelchair 2. Elastic Stocking/Abdominal Binder/Ace wrap LE 49 Dr. Shereen Fawaz
3. Add Salt/Meds: Salt Tablets 1 gram QID Florinef® (mineralocorticoid): 0. 05– 0. 1 mg QD Ephedrine (alpha agonist): 20– 30 mg QD– QID)→AD 4. Fluid resuscitation: monitor for neurogenic pulmonary edema P. S: Orthostasis ↓ with time → ↑ spinal postural reflexes. (VC → ↑circulation) Dr. Shereen Fawaz 50

2 - Autonomic dysreflexia Onset: After spinal shock, first 6 months– 1 year Cause: Noxious stimulus below the level of the →↑ sympathetic discharge Most commonly: Bladder distension, blocked catheter Fecal impaction , Pressure ulcers Ingrown toenails, Urinary tract infections 51 Dr. Shereen Fawaz

Mechanism: Noxious stimuli—Increases sympathetic reflex spinal release → Regional VC →↑ PR → ↑ CO → ↑ BP →Carotid body responds to HTN causing reflex bradycardia (dorsal motor nucleus of the vagus nerve) 52 Dr. Shereen Fawaz

Symptoms: Headache, Flushing Piloerection Sweating above level of SCI Blurry vision (pupillary dilation) Nasal Congestion 53 Dr. Shereen Fawaz

Treatment: Sit patient up Identify and remove noxious stimulus Nitroglycerine—to control BP— 1/150 sublingual, once noxious stimulus corrected Procardia®: 10 mg chew and swallow Hydralazine: Clonidine: ICU 10– 20 mg IM/IV 0. 3– 0. 4 mg - Nipride 54 Dr. Shereen Fawaz

3 -Cadriac arrhythmias (esp in quadriplegics and high paraplegics) Bradycardia Peaks: 2 -3 weeks after injury PPFs : overstimulation e. g tracheal intubation, defecation Tachycardia Asystole 55 Dr. Shereen Fawaz

4 - Deep Venous Thrombosis (DVT) Predisposing Factors Virchow’s Triad: Venous stasis/intimal injury/hypercoagulability E. g LE fractures- Obesity 56 Dr. Shereen Fawaz

Incidence Ranges 47%– 100% More in complete SCI More in tetraplegics 20% of calf vein thrombi extend proximally Onset Mostly first 2 weeks after SCI Incidence decreases after 12 weeks post SCI 57 Dr. Shereen Fawaz

Diagnosis Venogram is the Gold Standard Venous Doppler is used as a screening test for lower extremity DVTs Impedance Plethysmography—accurate in assessment of DVTs above the calf Complications: Pulmonary Embolism (PE) leading cause of death in acute SCI 58 Dr. Shereen Fawaz

Pulmonary Embolism Symptoms Pleuritic chest pain Dyspnea Fever, hemoptysis Tachycardia Hypoxemia 59 Dr. Shereen Fawaz

Physical Examination 1. Increased S 2 sound: severe pulmonary HTN → cor pulmonale. → Right heart failure 2. Dullness at bases of lungs Diagnosis (PE) ECG: Right Axis Deviation, Right Bundle Branch Block (RBBB): —if massive PE ABG: —decreased Chest X-ray: wedge shaped opacity Perfusion Gold PO 2 (PO 2 drops severely) lung scan: VQ mismatched Standard: CT Pulmonary arteriogram Dr. Shereen Fawaz 60

Treatment (PE) O 2 Heparin Vasopressor Surgical to treat shock Treatment Embolectomy 61 Dr. Shereen Fawaz

Post phlebitic syndrome (late complication of DVT) Distal venous hypertension (residual obstruction of outflow—incompetent valve) Swelling, Pigmentation Exercise induced pain Ulceration Long standing autonomic dysreflexia Treatment: Elastic Dr. Shereen Fawaz stockings, elevation massage, ROM exercises 62

Prophylaxis Treatment and Prevention of DVT (12 weeks) • External intermittent pneumatic compression devices • Enoxaparin- (LMWH) – Dose 40 mg SQ BID – Not used in patients with active bleeding or coagulopathy • Thigh-high graded compression stockings (TEDS)—alone, adjuvant ttt Dr. Shereen Fawaz 63

Therapeutic Anticoagulation for DVT: 1 - Unfractionated Heparin 2 - Low molecular Weight Heparin: 1. 5 unit/kg, average 80 every 12 hours 3 - Start Warfarin after 3 days, target INR 2 -3 64 Dr. Shereen Fawaz

4 -NOACS: non vitamin K oral anticoagulants. The direct factor Xa (FXa) inhibitors: • Rivaroxaban (R/ xarelto-Rivarospire): 20 mg/ bd- 21 days then once • Apixaban (R/Eliquis): 10 mg / bd for 7 days, then 5 mg/bd for 6 months, then 2. 5 mg / bd for another 6 month • Edoxaban The direct thrombin inhibitor: dabigatran (R/ Pradaxa). 65 Dr. Shereen Fawaz

Neurogenic Bladder Neural Control of Micturition Central Pathways Parietal lobes and the thalmus: receive and coordinate detrusor afferent stimuli Frontal lobes and basal ganglia: inhibit voiding Pontine Micturition center: coordinates urethral relaxation and detrusor contraction 66 Dr. Shereen Fawaz

Peripheral Pathways 1. Urine storage: sympathetic control (inhibiting detrusor contraction and increasing sphincter tone) 2. Urine voiding: parasympathetic (detrusor contractor and relaxation of sphincter tone). 67 Dr. Shereen Fawaz
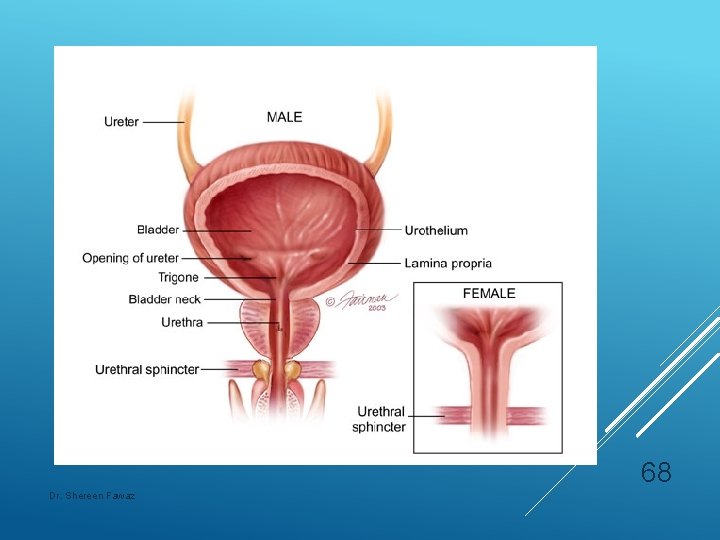
68 Dr. Shereen Fawaz

Urethral sphincter: • Proximal urethral: smooth muscle – alpha 1 receptor→sympathetic stimulation - T 11 to L 2. • Distal urethral: striated muscle → cholinergic somatic stimulation - S 2 to S 4. 69 Dr. Shereen Fawaz
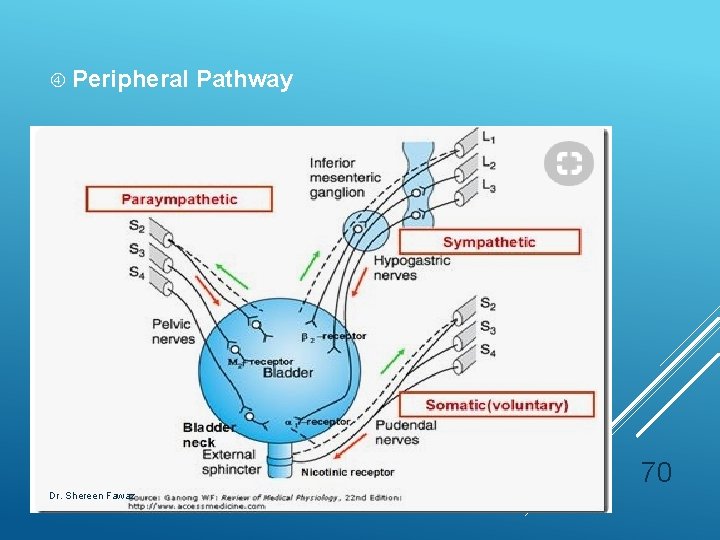
Peripheral Pathway 70 Dr. Shereen Fawaz
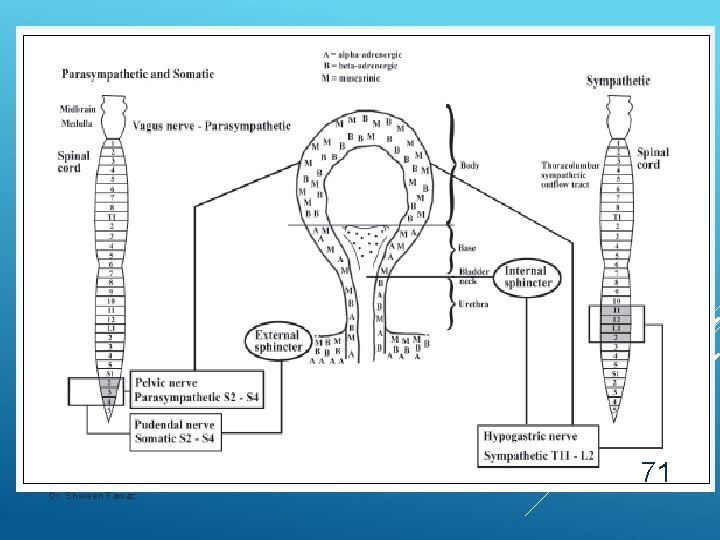
71 Dr. Shereen Fawaz
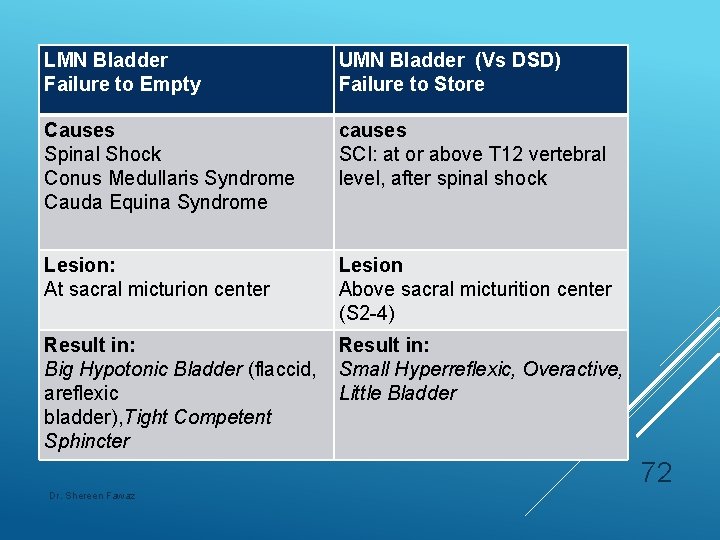
LMN Bladder Failure to Empty UMN Bladder (Vs DSD) Failure to Store Causes Spinal Shock Conus Medullaris Syndrome Cauda Equina Syndrome causes SCI: at or above T 12 vertebral level, after spinal shock Lesion: At sacral micturion center Lesion Above sacral micturition center (S 2 -4) Result in: Big Hypotonic Bladder (flaccid, areflexic bladder), Tight Competent Sphincter Result in: Small Hyperreflexic, Overactive, Little Bladder 72 Dr. Shereen Fawaz

Management of Urinary incontinence: History: Associated urinary symptoms such as frequency, urgency, and nocturia. Bladder Diary Severity: number of daily pads usage, its size Fluid intake (6 -8 glasses) Functional ability: access to bathroom, ambulation (needs assistance), transfer aids Questionnaires Examination: General, systemic, neurological 73 Dr. Shereen Fawaz

Investigations: Urinalysis and urine culture: infection, urinary stones. Ultrasound Pre- and post voidal assessment: measure the post voidal residuals (PVR): PVR: less than 100 over 65 years of age. Urodynamics: measure pressure in the bladder and the flow of urine. • Cystometry • Uroflometry Cystoscopy: to visualize the urethra and bladder. 74 Dr. Shereen Fawaz

AIMS & GOALS 1. EMPTY (no retention) 2. CAPACITY (storage) 3. DRY (continence) 4. SAFE (no complications) 75 Dr. Shereen Fawaz

Non pharmacological: A-Behavioral therapy: 1 - Avoid caffeinated beverages and alcohol 2 - Regulate fluid intake, minimizing evening intake – at least 2 hours before bed time. 3 - Bladder training: (timed voluntary voiding): Gradually increase the time between voids, each time by 30 mins, till reaching 4 -6 hours without leakage. 4 - Clean Intermittent Catheterization (CIC): 76 Dr. Shereen Fawaz

B-Pharmacological treatment of Neurogenic Bladder: A- UMN bladder, Failure to Store, DSD 1 -Anti. Cholinergics: ↑ capacity A- Non-selective: Oxybutynin (short acting )-(1 x 3), Dry mouth. . Tolterodine (Long acting)- (1 X 1), less side effects B- Selective: Solifinacin and Darifenacin (M 3 receptor antagonist). Dr. Shereen Fawaz 77

2 - Alpha-1 Adrenergic Antagonists ( in DSD): such as dibenzyline, terazosin, tamsulosin, alfuzosin, and doxazosin. 3 -B 3 -agonists: Mirabegron (R/Betmiga) A beta-3 adrenoceptor agonist, approved for the treatment of OAB. Dose: 25 mg and 50 mg once daily. Safe in patients over 65 and over 75. + Clean Intermittent Catheterization (CIC) 78 Dr. Shereen Fawaz

B- LMN Bladder (Failure to empty): 1 - Cholinergic agonists: Pyridostegmine, Mestinon 2 - Alpha-1 Adrenergic Antagonists : + CIC, Valsalva maneuver or crede maneuver 79 Dr. Shereen Fawaz
C-Rehabilitation: Pelvic muscle exercises (PME): Kegel exercises: Strengthen the muscular components of urethral support. 80 Dr. Shereen Fawaz
Biofeedback Identifying, controlling and coordinating the function of pelvic floor muscles Functional Vaginal training: electric stimulation weight training: Holding progressively weighted vaginal cones within the vagina by tightening the vaginal muscles. 81 Dr. Shereen Fawaz

Types of bladder Catheterization 1 - Indwelling Uretheral catheters: Most common Foley’s catheter, standard catheter sizes 16 F or 18 F. All indwelling catheters in the bladder kept for more than 2 weeks, become colonized with bacteria. 82 Dr. Shereen Fawaz
Bacterial colonization does not mean the patient has clinical bladder infection. Asymptomatic bacterial colonization is common and does not pose a health hazard. If bladder infection occurs, change the entire catheter and drainage system. Untreated symptomatic UTI → bacteremia → septicemia → Death. 83 Dr. Shereen Fawaz
2 - Suprapubic tubes Smaller catheters (14 F- 16 F) Once a month 3 - Self-intermittent Catheterization A pre-requisite- patient hand dexterity Best choice 4 -6 times per day Drain 400 -500 ml/time The best are short, rigid, plastic catheters 12 F-14 F most common (esp males) 84 Dr. Shereen Fawaz

Management of UTIs 1 - Asymptomatic UTIs Recurrent asymptomatic bacteriuria: not treated to avoid the development of resistant organisms 2 - Symptomatic UTIs Increase catheterization to reduce bacterial concentration Treat infection according to culture A Foley catheter may be necessary Dr. Shereen Fawaz 85
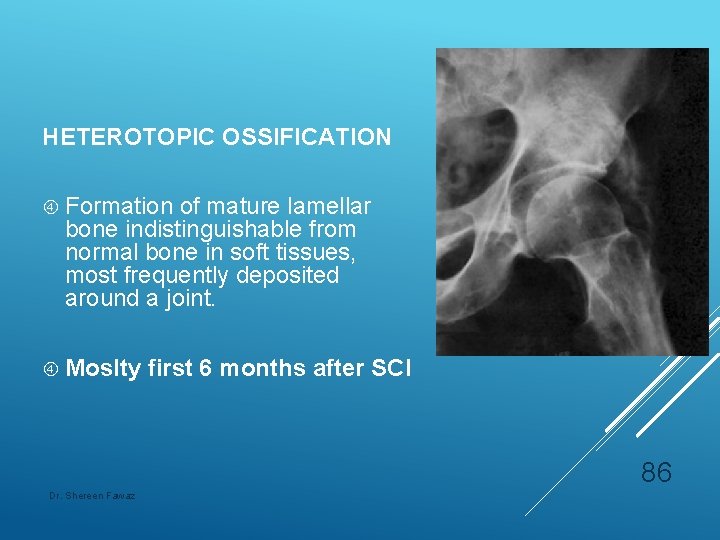
HETEROTOPIC OSSIFICATION Formation of mature lamellar bone indistinguishable from normal bone in soft tissues, most frequently deposited around a joint. Moslty first 6 months after SCI 86 Dr. Shereen Fawaz
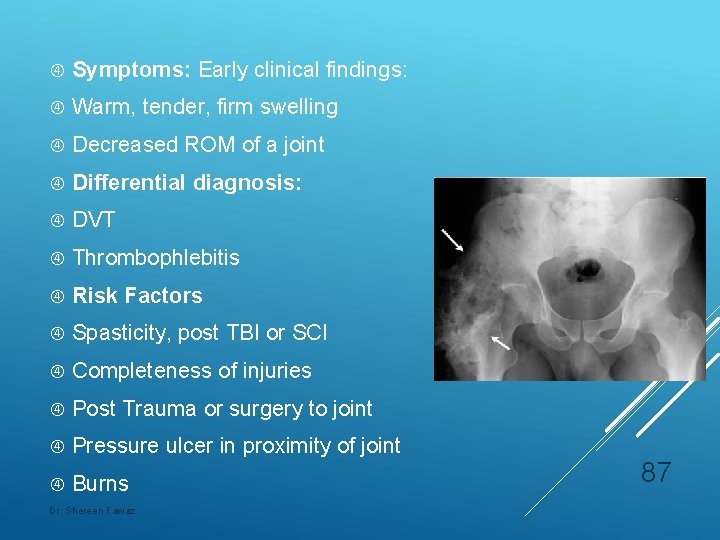
Symptoms: Early clinical findings: Warm, tender, firm swelling Decreased ROM of a joint Differential diagnosis: DVT Thrombophlebitis Risk Factors Spasticity, post TBI or SCI Completeness of injuries Post Trauma or surgery to joint Pressure ulcer in proximity of joint Burns Dr. Shereen Fawaz 87

Diagnosis: Within one week from onset triple phase bone scan Plain X-ray by at least 7– 10 days, usually after clinical signs are observed Bone Scan returns to normal as HO matures in 6– 18 months post injury Serum Alkaline Phosphatase: Increases at 2 weeks—exceeds normal levels at 3 weeks— peaks at 10 weeks—returns to normal after HO matures ESR, CRP and WBCs ↑ Doppler Dr. Shereen Fawaz U/S to rule out DVT 88
Treatment: ? ? ? Didronel® (etidronate disodium): 20 mg/Kg/day for 2 weeks then 10 mg/Kg/day for 10 weeks Biphosphonate immediately after diagnosis (Biphosphonates will do nothing for mature HO) Gently ROM through functional range—vigorous force should not be used as this may lead to further ectopic bone formation) Indocin®—Not commonly used in acute SCI Low dose radiation therapy 89 Dr. Shereen Fawaz
Surgery Excision of HO Excision Athroplasty of the joint CPM devices post-op NB: Surgery—Used when HO severely limits ROM impairing function—should only be planned after bone is mature: 12– 18 months post injury. Bone scan must be back to baseline and alkaline phosphatase should be back to normal Dr. Shereen Fawaz 90

Complications Peripheral nerve entrapment Decreased ROM/loss of function/ankylosing HO overlying a bony prominence will directly predispose to pressure ulcer/skin breakdown secondary to poor positioning 91 Dr. Shereen Fawaz

Sexual dysfunction (UMNL): Better prognosis Management of Bowel Dysfunction in SCI: Gastric atony-ileus Metabolic complications (hypercalcemia) MSK complications: entrapments MSK pain Neuropathic pains (central or peripheral) 92 Dr. Shereen Fawaz

PULMONARY COMPLICATIONS OF SCI AND MANAGEMENT Restrictive and obstructive lung disease Atelectasis Bronchspasm, hypersecretion, nasal congestion (unopposed vagal tone) Pneumonia Assessment: Respiratory ABG, Dr. Shereen Fawaz rate, VC, pulse oximetry Chest x ray 93
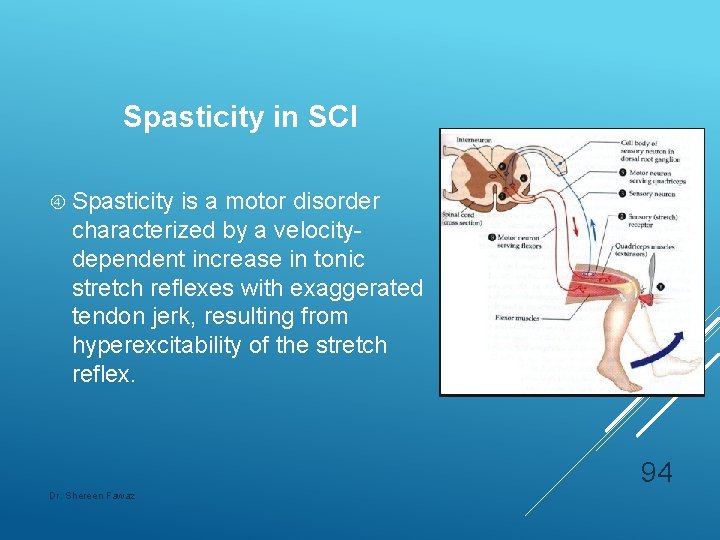
Spasticity in SCI Spasticity is a motor disorder characterized by a velocitydependent increase in tonic stretch reflexes with exaggerated tendon jerk, resulting from hyperexcitability of the stretch reflex. 94 Dr. Shereen Fawaz
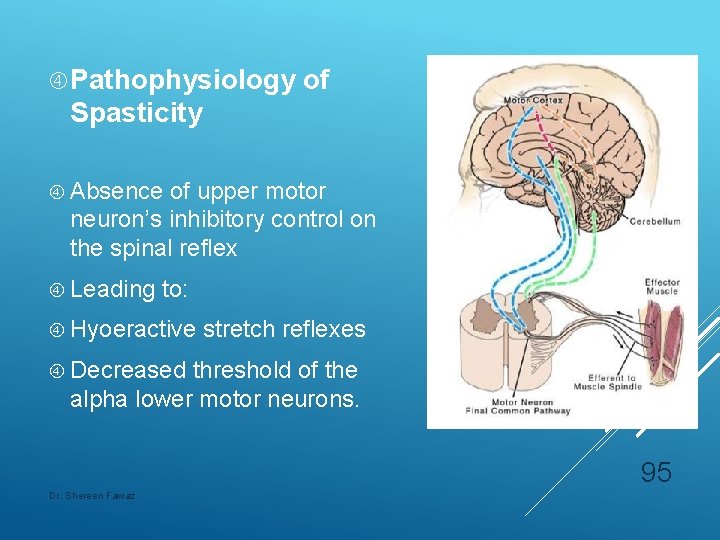
Pathophysiology of Spasticity Absence of upper motor neuron’s inhibitory control on the spinal reflex Leading to: Hyoeractive stretch reflexes Decreased threshold of the alpha lower motor neurons. 95 Dr. Shereen Fawaz
Clinical History: assessment: patient’s report. Examination: Tone: assessed by scores: e. g: Modified Ascworth scale. Power: MRC scale Tendon reflexes: exaggerated deep reflexes. Range of motion Posturing 96 Dr. Shereen Fawaz

Exacerbating factors: Any noxious stimulus: e. g UTI- stones-pain. Potential benefits: Increase stability in sitting and standing Prevent DVT Potential side effects: Increases pain, contractures, pressure sores Impair sleep 97 Dr. Shereen Fawaz

Treatment A- of spasticity: Non pharmacological: 1 - Eliminate noxious stimuli: e. g UTIs, bladder stones, constipation, hemorrhoids, skin irritation (pressure sores), ingrowing toe nails, Heterotopic ossification. 2 -Physiotherapy 3 -Therapeutic interventions. and Functional electric stimulation 4 -Casting 5 -Mental imagery 98 Dr. Shereen Fawaz

B-Pharmacological: 1 - Generalized Spasticity: Oral agents 2 -Regional Spasticity: Intrathecal baclofen or phenol nerve block 3 - Focal Spasticity Botulinum toxin and/or phenol block 99 Dr. Shereen Fawaz

Oral Agents: I- Centrally acting: A-Baclofen: GABA-b receptor agonist at the spinal level Half life: 6 -8 hours Dose : 5 -40 mg. 3 times daily Side effects: sedation, systemic muscle relaxation (incontinence, weakness). Avoid sudden withdrawal: hyperthermia, seizures and altered mental state. 100 Dr. Shereen Fawaz

B-Tizanidine (Sirdalud) Alpha 2 adrenergic agonist: Increases presynaptic inhibition of motor neurons, decreasing excitatory amino acids from spinal interneurons. Max. dose 24 mg daily Side effects: sedation, hypotension, bradycardia and drowsiness Contraindicated in patients on antihypertensive medications, prolongs QT interval) 101 Dr. Shereen Fawaz

C-Anticonvulsants: 1 - Benzodiazepines: Diazepam (R/Valium) Post-synaptic GABA-a receptor agonist, depresses the action of the CNS Dose Side effects: sedation, tolerance, dependence 2 - Gabapentin: (R/Neurontin) It’s structure similar to GABA, doesn’t act on its receptors Mechanism : relativelyunkown, act on voltagedependent Ca channels, inhibit Ca currents. Sideeffcts: somnolence, tremor and nystagmus 102 Dr. Shereen Fawaz

II- Peripherally acting: Dantrolene sodium: (R/Dantrelax) FDA approved Mechanism: Inhibit calcium release at the sarcoplasmic reticulum, uncoupling excitation and contraction. Side effects: general muscle weakness, liver dysfunction. Used as adjunct to other treatments. 103 Dr. Shereen Fawaz

C- Interventional treatments: 1 -Local injections: Botulinum toxin injections. Phenol/Alcohol injections. 2 -Intra. Thecal Baclofen pump D- Surgery: Rhizotomies, tenotomies and neurectomies. 104 Dr. Shereen Fawaz
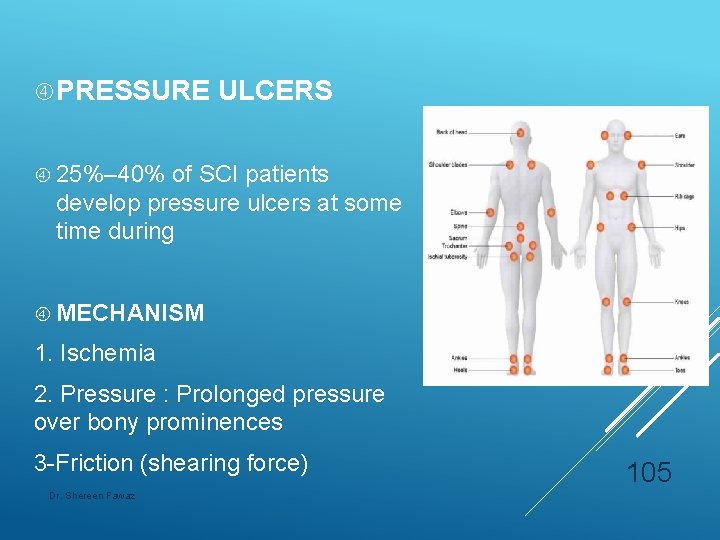
PRESSURE ULCERS 25%– 40% of SCI patients develop pressure ulcers at some time during MECHANISM 1. Ischemia 2. Pressure : Prolonged pressure over bony prominences 3 -Friction (shearing force) Dr. Shereen Fawaz 105
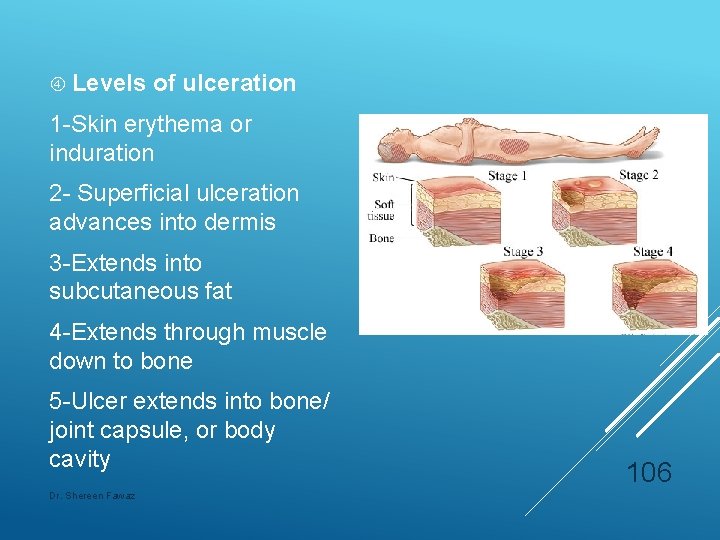
Levels of ulceration 1 -Skin erythema or induration 2 - Superficial ulceration advances into dermis 3 -Extends into subcutaneous fat 4 -Extends through muscle down to bone 5 -Ulcer extends into bone/ joint capsule, or body cavity Dr. Shereen Fawaz 106

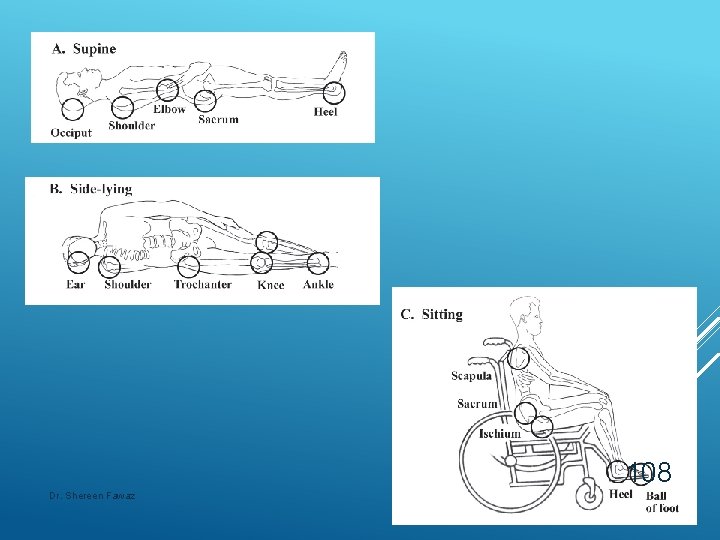
Common In Locations acute SCI patient lying supine: #1 Sacrum #2 Heels In chronic SCI patients the locations of ulcers are as follows: Ischial decubitus (30 %) Greater trochanter (20%) Sacrum (15%) Heels (10%) 107 Dr. Shereen Fawaz
108 Dr. Shereen Fawaz

Treatment of pressure sores: 1 - Relief the pressure 2 - keep it : clean, moist, and debrided. 3 - Infected wounds: Antibiotics according to culture 4 - Supplements: • Vit C 1 gm/d • Zinc sulphate, Copper, Arginine 5 -Increase protein intake 6 - Stages 3 & 4: surgical consultation and grafting 109 Dr. Shereen Fawaz
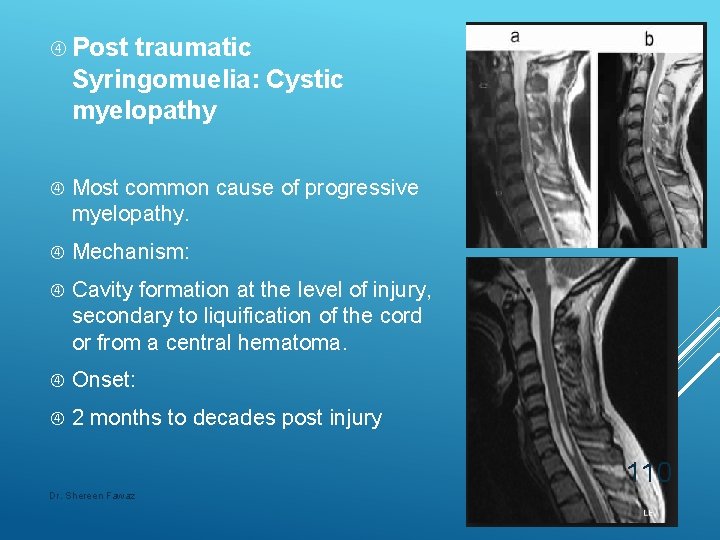
Post traumatic Syringomuelia: Cystic myelopathy Most common cause of progressive myelopathy. Mechanism: Cavity formation at the level of injury, secondary to liquification of the cord or from a central hematoma. Onset: 2 months to decades post injury 110 Dr. Shereen Fawaz
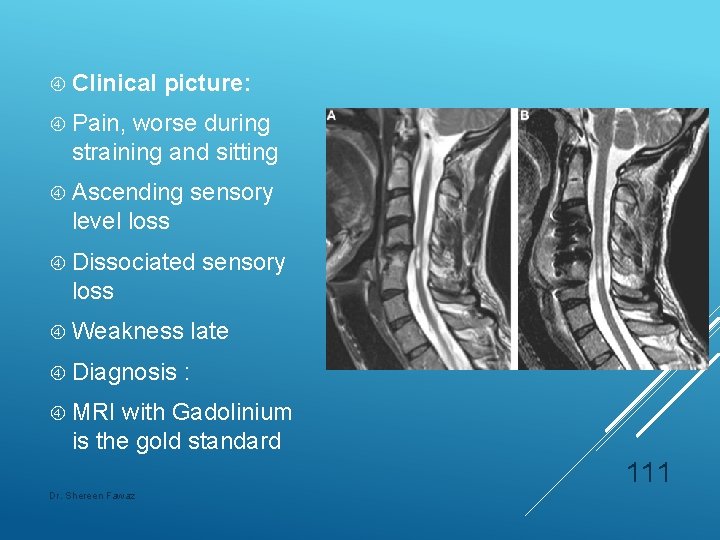
Clinical picture: Pain, worse during straining and sitting Ascending sensory level loss Dissociated sensory loss Weakness Diagnosis late : MRI with Gadolinium is the gold standard 111 Dr. Shereen Fawaz
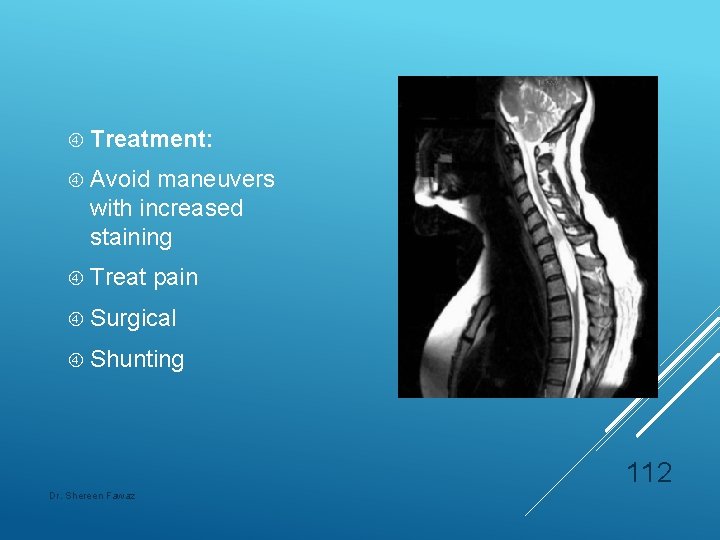
Treatment: Avoid maneuvers with increased staining Treat pain Surgical Shunting 112 Dr. Shereen Fawaz

Rehabilitation Motor: 1 -Physiotherapeutic intervention: A-Neurodevelopmental techniques (Bobath- Sensorymotor facilitation. Brunnstrom’s technique- PNF) B-Exercise: ROM- stretchingstrengthening exercises. 113 Dr. Shereen Fawaz

Balancing and proprioceptive training 114 Dr. Shereen Fawaz

C-Mental imagery D-Virtual reality 115 Dr. Shereen Fawaz

E-Body Weight Supported Treadmill Training F-Virtual 2 - Reality Occupational Therapy 116 Dr. Shereen Fawaz

3 -Functional Electrical Stimulation (FES) in SCI Uses: Cardiovascular conditioning program Increase muscle bulk strength and endurance Decrease risk of DVT Enhance brain plasticity and sensorimotor stimulation 117 Dr. Shereen Fawaz

4 -EMG-BF 5 -Robotic devices 6 - Magnetic stimulation: Transcranial (TMS) and Peripheral (PMS) 118 Dr. Shereen Fawaz

Dr. Shereen Fawaz 119
- Slides: 119