Rehabilitation of patients with rheumatic diseases Dr Demet

Rehabilitation of patients with rheumatic diseases Dr. Demet Demircioğlu

General information Rheumatic conditions adversely affect patients’ lives. Dealing with chronic pain, stiffness, and fatigue, limitations in daily activities and restricted participation in society are some of the challenges that these patients face. Rheumatic diseases are a burden for the health care system and society and lead to decreased productivity and financial loss. Pharmacological means alone rarely offer long-term remission for these chronic disorders and rehabilitative measures are incorporated in treatment protocols.
Rheumatic diseases Adversely affect patient’s wellbeing Rheumatic and Musculoskeletal Diseases Burden for society and health care system Lead to financial loss and productivity Require multidisciplinary approach

Medical rehabilitation • Rehabilitation manages disease consequences, the most important being pain, fatigue, joint stiffness, deformity and aims alongside medical treatment to restore completely the physical, medical, emotional, social, economic and vocational potential of the individual. • Rheumatologists, having a key position in patient management need to know the advantages and limitations of rehabilitation modalities. • The majority of rehabilitative interventions require time and changes in patient’s behavior and level of motivation.

Rehabilitation structured approach • • • Goal of intervention and appropriate measures must be defined. Rehabilitation plan should be developed in cooperation with the patient. The World Health International Classification of Functioning, Disability and Health (ICF) is a very good tool for measuring health and disability at both individual and population level. It has two parts with two components each : Functioning and disability part which contains - body functions and structures; activities and participation Contextual factors part with - environmental factors and personal factors.

Evolution of rehabilitation in rheumatology Splinting and mobilization with assistive devices to promote function were applied frequently in the forties after steroids introduction. Joint replacements and post-operative rehabilitation protocols bloomed in the sixties and seventies Incorporation of dynamic exercises and functional activities earlier in the disease process occurred the eighties; the impact of isometric and low-intensity isotonic exercise on immune response and function was also evaluated. Increase of research in evaluation of various intensities, frequencies, and modes of exercises on patient outcomes ensued arrival of DMARD-s in the market 1940 1950 1960 1970 1980 1990

Rehabilitation in rheumatology • • In the twenty first century the public health perspective of promoting physical activity for improving the quality of life, function, and participation of patients is embraced. Research focus is on investigating the impact of weight-bearing activities of various intensities on joint integrity in light of radiological advancements and advent of modern biologic therapies.

Rehabilitation modalities in rheumatology Total/Local body rest. Bed rest is practical but should not be applied for more than four days especially in the elderly. Manual therapy Massage

Rehabilitation modalities in rheumatology Exercise therapy Range of motion (Ro. M) and flexibility exercises– help preserve joint movements and are passive when performed by the physiotherapist or active when there’s patient involvement. Isometric/static exercises – muscle contractions here achieved without joint movement and lengthening or shortening of muscle fibers; they can be generated with the help of a fixed object like the hand of therapist, a belt, small ball or elastic band. Isometric exercises increase strength and resistance and are easy and safe to be performed by patients with inflammatory arthritis. Isotonic/dynamic exercises – involve changes in the muscle fiber length through their lengthening (essentric) or shortening (concentric); nearby joints move through full Ro. M. Aerobic conditioning / strengthening exercises – moderate intensity exercises are effective (70 -80% max heart rate = 220 - age) and include walking, running, cycling, swimming and stair climbing. Aquatic exercises

Exercises in rheumatology • • • Exercise therapy represent the foundation of rheumatic conditions rehabilitative management. Involves repeating planned and structured physical activities in order to improve or preserve components of physical fitness. Exercise programs for patients with rheumatic diseases usually involve the combination of exercises which increase cardio pulmonary fitness, strengthen muscles and enhance flexibility with training for specific movement patterns or daily activities, education and spare time activities.

Exercises in rheumatology Cardiopulmonary fitness exercises: Public health recommendations for older adults can be utilized. They involve completing moderate intense aerobic activities (cardiac and respiratory rate is increased, with or without sweating, while the person can talk normally ) like walking, running, aerobic dancing for at leas 30 min/5 days per week, or high intensity exercises (higher heart and respiratory rate, sweating and the person can speak only short sentences) for 20 min/3 days per week. Exercises for increasing muscle strength 8 -10 exercises to increase muscle strength with 8 -12 repetitions each should to be performed at least 2 times per week. Exercises should focus on damaged structures and should be proceeded by a 5 -10 min warm up with Ro. M exercises. Flexibility and balance exercises Flexibility exercises aim to keep Ro. M within physiologic limits. They should involve the most used joints and are especially important when local inflammation in present or for contracture prevention. They should be performed preferentially every day or minimally three times per week. Balance exercises reduce falling risk.

Exercises Can be performed under the supervision of a physical therapist By patients themselves after instruction Using community resources
Reabilitation modalities in rheumatology Physical modalities Superficial heat/cold therapy, Electrotherapy - uses electricity transmitted through surface electrodes to stimulate nerves and muscles and alleviate pain. Deep tissue heating/Ultrasound/ diathermy D

Reabilitation modalities in rheumatology Occupational therapy (learning joint protection and energy conservation methods) Making architectural changes Vocational rehabilitation and self management.
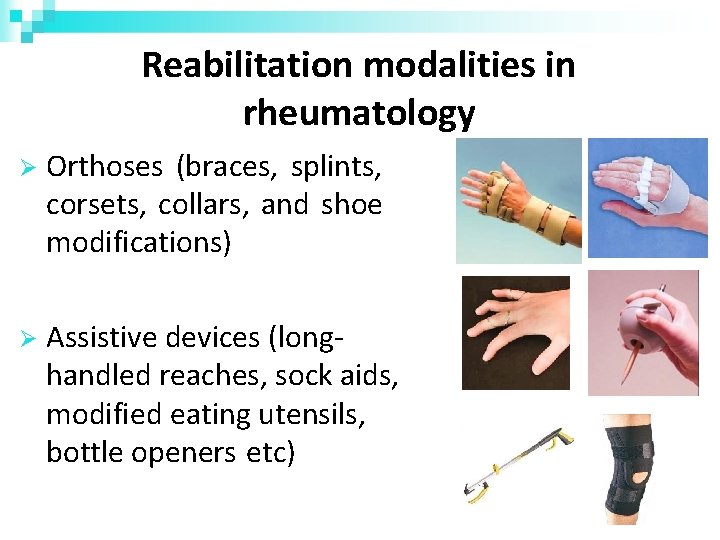
Reabilitation modalities in rheumatology Orthoses (braces, splints, corsets, collars, and shoe modifications) Assistive devices (longhandled reaches, sock aids, modified eating utensils, bottle openers etc)

Most important rehabilitative modalities Exercise, patient education programs, and self-management interventions are the best studied and the most effective measures producing moderate improvements in patients’ strength, pain, function, and modest (small to moderate improvements) results in mood, quality of sleep, sleep patterns, and psychological well-being.

Patient evaluation First step in every rehabilitation program is patient’s problem identification and correct diagnosis based on a comprehensive history, physical examination, laboratory and diagnostic evaluation. Patients’ evaluation includes : measuring Ro. M (through simple observation or goniometry), muscular strength (through observation or hand held dynamometers), gait, mobility and balance. There is primary, secondary and tertiary rehabilitation and different strategies are applied for specific pathologies.

Artriti Rheumatoid Arthritis is a chronic, systemic, autoimmune disease which: Affects 1 -2% of the population and results from the interplay of genetic and environmental factors It is 2 -3 times more common in women than in men and the highest incidence rate is observed between ages 40 and 60; autoantibodies are detected. Arthritis is erosive, symmetric, involving multiple peripheral joints, (mainly PIP, MCF, MTF joints and wrists); extra-articular manifestations are observed Causes pain, disability and loss of function Unresolved pathogenesis

Rheumatoid Arthritis medical treatment Treatment should start as soon as possible, aggressive management is preferred. Most utilized pharmacological agents include: NSAIDs are used to relieve pain and reduce minor inflammation but do not induce long term remission. Analgesics relieve pain. Glucocorticosteroids – are potent anti inflammatory drugs and are used to suppress the autoimmunity. Oral, intramuscular and intra-articular preparations are used. Disease Modifying Anti–rheumatic drugs/DMARDs (methotraxate + folic acid, hydroxychloroquine, sulfasalazine and leflunomide ) constitute the foundation of RA therapy and can be used alone or in combination. Biologics target molecules on cells of the immune system, joints, and the products that are secreted in the joint. Biologics used in RA include : TNF- α blockers: etanercept, adalimumab, infliximab, certolizuma; toclizumab, an IL-6 receptor monoclonal antibody, Rituximab (Rituxan) a B cell inhibitor; Abatacept a recombinant molecule which binds to CD 80 / CD 86 and prevents CD 28 mediated costimulation, Anakinra an IL-1 inhibitor, and Tofacitinib a JAK 1 and 3 inhibitor

Multidisciplinary Approach Appropriate pharmacologic therapy Pain control Management of osteoporosis Physiotherapy when inflammation is suppressed

Rehabilitation of Rheumatoid Arthritis During the active phase of Rheumatoid Arthritis or other inflammatory arthritis, measures to be taken include: Total body rest, splints and self management. Active and passive Ro. M exercises Isometric exercises Physical modalities - Cold therapy (ice packs, ice chips, ice massage, cryowraps) is applied to manage acute inflammation diminish swelling and lessen pain. Orthotics may also help in improving function and reducing pain.
Rehabilitation of Rheumatoid Arthritis Interventions on the subacute phase include: Increased repetitions of Ro. M exercises Progression from isometric to isotonic/dynamic exercises. Heat therapy and/or massage before stretching may limit muscle spasm and improve tissue flexibility. Ergonomic changes. Orthosis/ splinting. Aquatic therapy.

Rehabilitation of Rheumatoid Arthritis With stable disease patients should: Integrate dynamic strengthening exercises with resistance ones. Dynamic exercises can increase muscle strength, physical and aerobic capacity. Aerobic exercises (with 70%-80% max heart rate) should be started. Low-impact exercise, such as walking programs, aquatics, dance, and cycling, and dynamic exercises with resistance are the most commonly used exercises.

Osteoarthritis (OA) is a very common, slowly progressive joint disorder, whose symptoms typically start after age 40; women are more often affected by OA than men. It is called a degenerative joint disease or “wear and tear” arthritis. OA results from degenerative changes in the cartilage of weight-bearing joints (knee, hip and spine) and hands.

Osteoarthritis • • • OA likely begins with the breakdown of articular cartilage, which becomes ineffective, leaving the bones to rub against one another during movement. This process may be stimulated by high circulating levels of proinflammatory cytokines and cells. As OA progresses, the joint space narrows, causing bone-on-bone contact and spurring, ligament laxity and decreased strength around the joint can occur.

Osteoarthritis Rehabilitation Menaxhimi i osteoartritit perfshin aplikimin e: Dynamic strengthening exercises Core strengthening exercises Patient education Aerobic exercises – cycling, swimming Thermotherapy Parafin application for hand OA

Knee Osteoarthritis Rehabilitation Open-chain isometric exercises, such as quadriceps exercises, are used with progression to closed-chain weight-bearing exercises, such as mini-squats and step-ups. These exercises are effective and help reduce pain and improve function. Patients benefit from joint mobilization and manipulation procedures. Bracing, gait training, use of orthotics, and appropriate footwear. Thermotherapy may alleviate pain, enhance tissue extensibility, and reduce stiffness.

Systemic lupus erythematosus Studies of exercise in SLE are limited. Considering the fact that symptomatic coronary heart disease is a major cause of mortality a comprehensive cardiovascular pulmonary system review should be done along with exercises that enhance cardiovascular performance, such as biking, walking, and dynamic exercises at moderate intensity.

Ankylosing Spondylitis Ankylosing spondylitis is a systemic inflammatory disease of the sacroiliac and axial joints. It affects males more than females Starts in early adulthood Systemic features include fatigue, malaise and osteopenia. Patients have back pain. It results in reduced physical activity engagement, ankylosis, deformity and disability.

Ankylosing Spondylitis management Medical therapy Physical modalities, such as thermal therapy to relax soft tissues and prepare the patient for flexibility exercises, Manual therapy, Assistive and ambulatory devices, orthoses Exercise therapy Patient education

Exercise therapy in Ankylosing Spondylitis • • Posture/ core muscle strengthening exercises Ro. M exercises Flexibility & stretching exercises Exercises for strengthening hip – knee – spine muscles Exercises for pulmonary fitness Strengthening of Extensor muscles Aquatic therapy
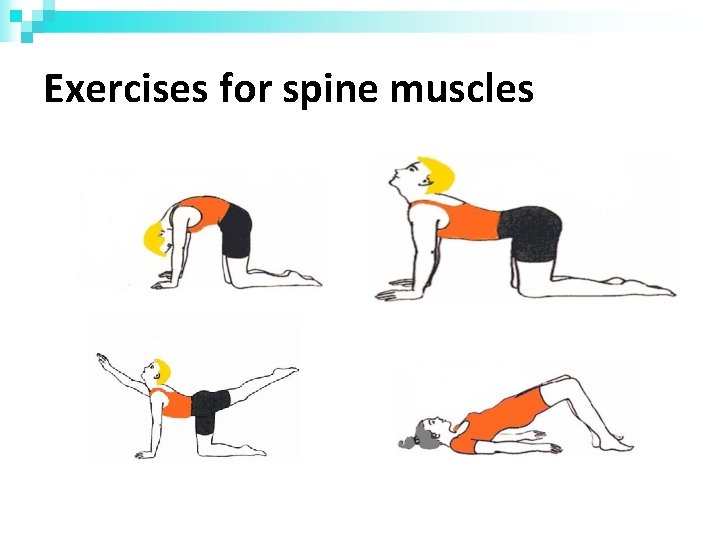
Exercises for spine muscles

Ankylosing Spondylitis rehabilitation • • Life style modification Exercises should be conducted on a regular basis (more than 3 times per week) Posture awareness Swimming Quit smoking Ergonomics Secondary osteoporosis evaluation

Conclusion Rehabilitation interventions comprise a large range of interventions. Selection of rehabilitation modalities for rheumatological disorders is influenced primarily on the disease state but is also dependent on other variables like disease severity, medication latency periods, comorbidities, disease severity, and patient preferences.
- Slides: 34