Regulation of Cardiac Output Chris Hague Ph D






![Cardiac Electrophysiology + Na Na+ K+ Ca 2+ K+ Ion [EC] (m. M) [IC] Cardiac Electrophysiology + Na Na+ K+ Ca 2+ K+ Ion [EC] (m. M) [IC]](https://slidetodoc.com/presentation_image/377744d4b33cf2edfd27d205025bf85c/image-12.jpg)

![Cardiomyocyte Contraction increased [Ca 2+]i through Ca 2+ channels Ca 2+ spread by transverse Cardiomyocyte Contraction increased [Ca 2+]i through Ca 2+ channels Ca 2+ spread by transverse](https://slidetodoc.com/presentation_image/377744d4b33cf2edfd27d205025bf85c/image-17.jpg)




- Slides: 26

Regulation of Cardiac Output Chris Hague, Ph. D chague@u. washington. edu Technical Advisor: Seth Goldenberg, Ph. D

Outline 1. Function and Anatomy of the Heart 2. Cardiac Output, Afterload and Preload 3. Excitation-contraction coupling 4. Frank-Starling and Venous Return 5. Autonomic Regulation of Cardiac Output

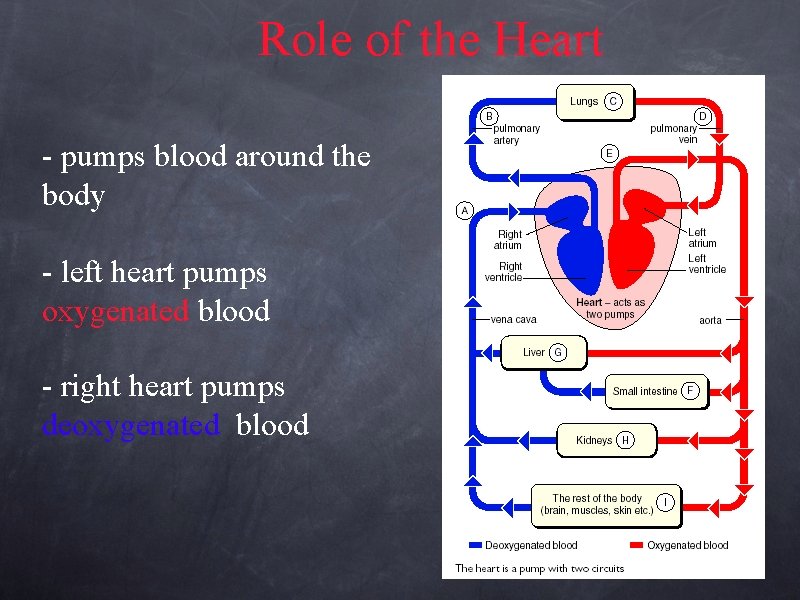
Role of the Heart - pumps blood around the body - left heart pumps oxygenated blood - right heart pumps deoxygenated blood

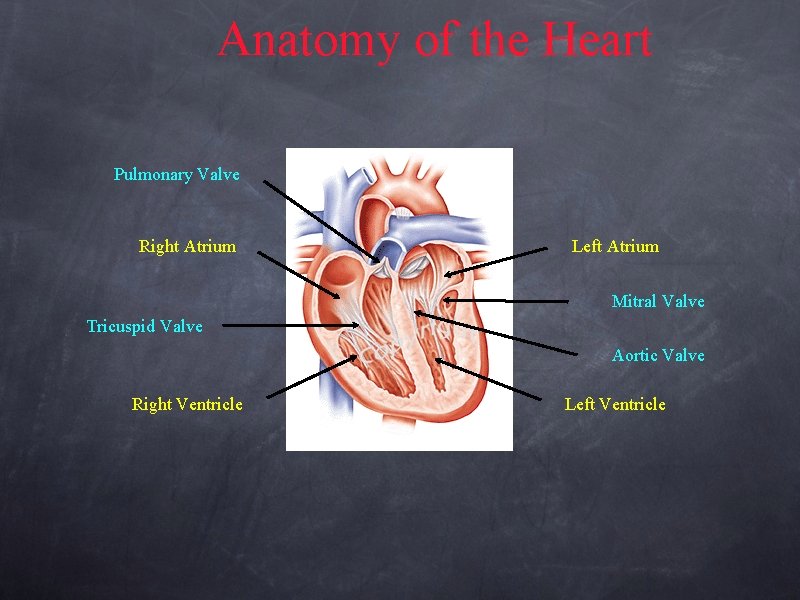
Anatomy of the Heart Pulmonary Valve Right Atrium Left Atrium Mitral Valve Tricuspid Valve Aortic Valve Right Ventricle Left Ventricle

The Cardiac Cycle events that occur from beginning of one heartbeat to beginning of next heartbeat consists of 2 periods: Diastole: relaxation, heart fills with blood (BP ~ 80 mm Hg) Systole: contraction, blood is ejected (BP ~ 120 mm Hg)

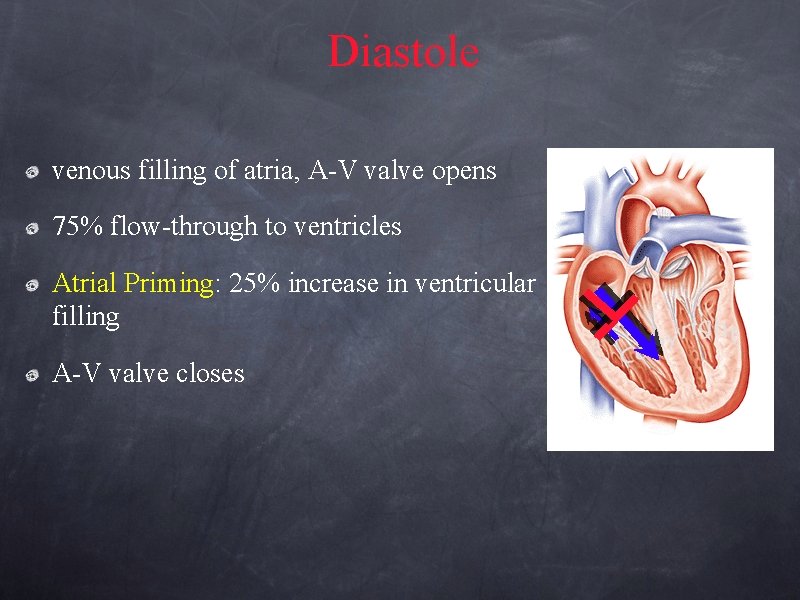
Diastole venous filling of atria, A-V valve opens 75% flow-through to ventricles Atrial Priming: 25% increase in ventricular filling A-V valve closes

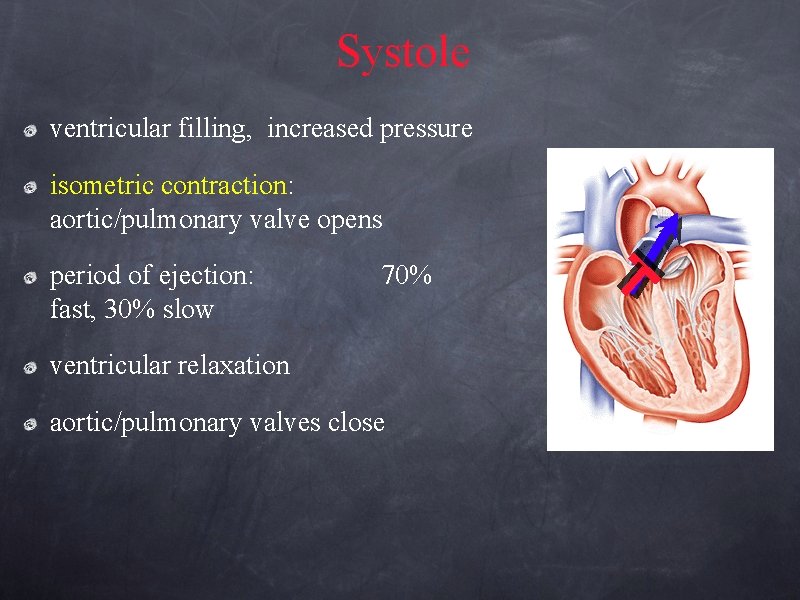
Systole ventricular filling, increased pressure isometric contraction: aortic/pulmonary valve opens period of ejection: fast, 30% slow 70% ventricular relaxation aortic/pulmonary valves close

What is Cardiac Output? Cardiac output = Stroke Volume X Heart Rate OR CO = SV x HR Stroke Volume: blood volume ejected by ventricles/beat Heart Rate: heart beats/min

Preload/Afterload determinants of stroke volume Preload: tension on ventricular muscle before contraction determined by left ventricular end diastolic volume Afterload: pressure against which ventricles pump blood determined by total peripheral resistance

Excitation-Contraction Coupling generation of rhythmical electrical impulses sinus (or sinoatrial) node propagation of impulses throughout the heart internodal pathways A-V node A-V bundle Purkinje fibers

Generation of cardiac rhythmicity Sinus node: small specialized muscle in right atrium controls heart rate “spontaneous” action potential
![Cardiac Electrophysiology Na Na K Ca 2 K Ion EC m M IC Cardiac Electrophysiology + Na Na+ K+ Ca 2+ K+ Ion [EC] (m. M) [IC]](https://slidetodoc.com/presentation_image/377744d4b33cf2edfd27d205025bf85c/image-12.jpg)
Cardiac Electrophysiology + Na Na+ K+ Ca 2+ K+ Ion [EC] (m. M) [IC] (m. M) Eq. Potential Na+ 145 10 50 m. V K+ 4 140 -90 m. V Ca 2+ 2 0. 0001 140 m. V

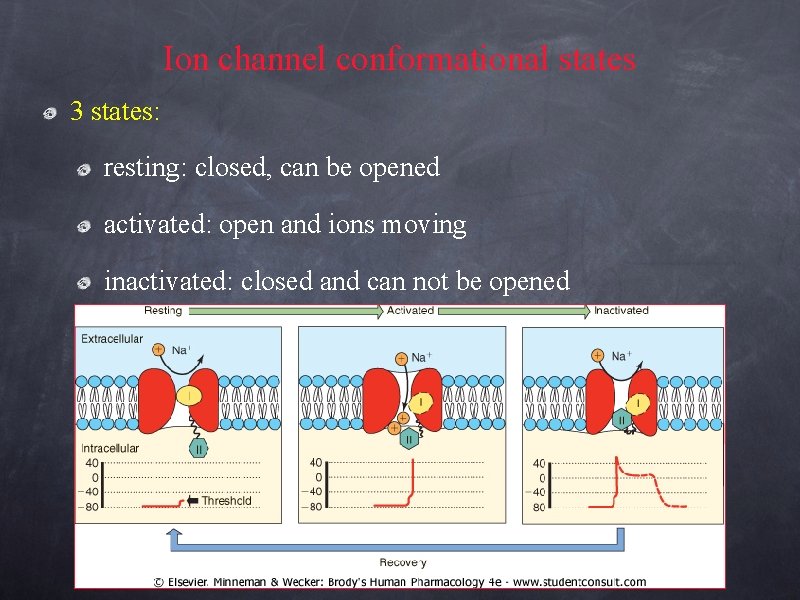
Ion channel conformational states 3 states: resting: closed, can be opened activated: open and ions moving inactivated: closed and can not be opened

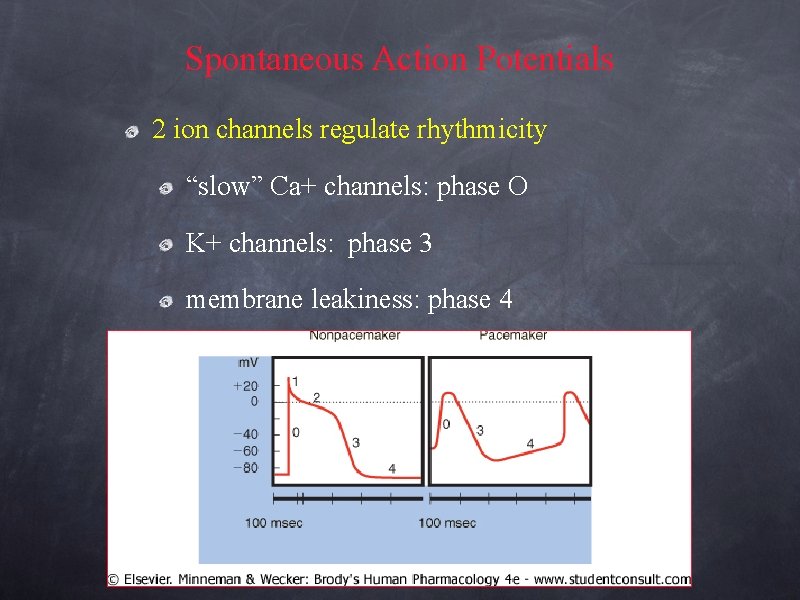
Spontaneous Action Potentials 2 ion channels regulate rhythmicity “slow” Ca+ channels: phase O K+ channels: phase 3 membrane leakiness: phase 4

Transmission of Cardiac Impulses Internodal pathways spread current around atrial muscle A-V node separates atria and ventricles delays spread of signal to ventricles has spontaneous activity (ectopic pacemaker) Purkinje fibers spreads impulse around ventricles

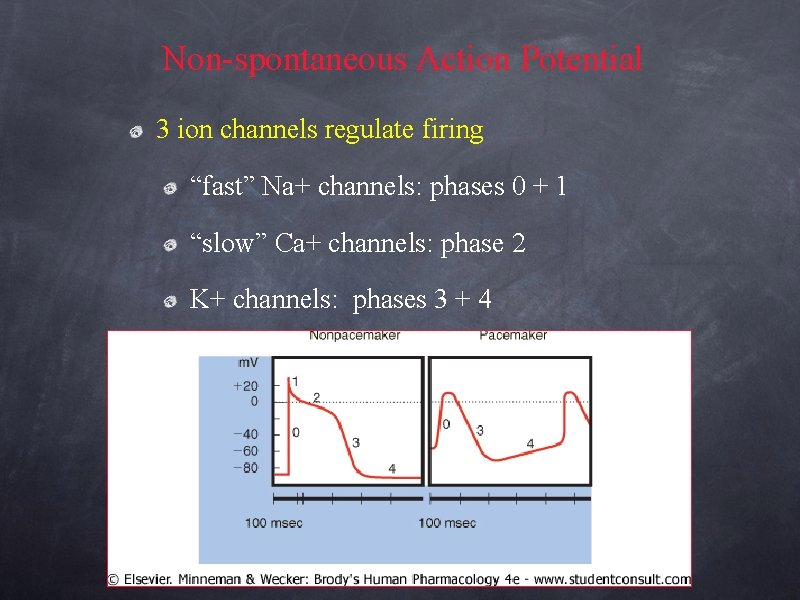
Non-spontaneous Action Potential 3 ion channels regulate firing “fast” Na+ channels: phases 0 + 1 “slow” Ca+ channels: phase 2 K+ channels: phases 3 + 4
![Cardiomyocyte Contraction increased Ca 2i through Ca 2 channels Ca 2 spread by transverse Cardiomyocyte Contraction increased [Ca 2+]i through Ca 2+ channels Ca 2+ spread by transverse](https://slidetodoc.com/presentation_image/377744d4b33cf2edfd27d205025bf85c/image-17.jpg)
Cardiomyocyte Contraction increased [Ca 2+]i through Ca 2+ channels Ca 2+ spread by transverse T-tubules opens ryanodine receptors on sarcoplasmic reticulum “ Ca 2+ induced Ca 2+ release” Ca 2+ binds to troponintropomyosin actin-myosin filament movement

Factors affecting Cardiac Output Frank-Starling Mechanism Autonomic Inputs sympathetic nervous system parasympathetic nervous system Cardiovascular disease

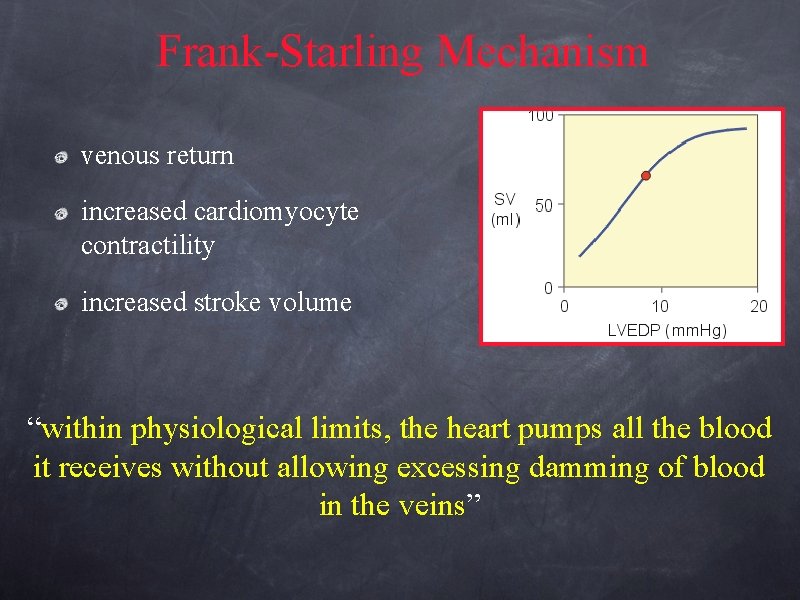
Frank-Starling Mechanism venous return increased cardiomyocyte contractility increased stroke volume “within physiological limits, the heart pumps all the blood it receives without allowing excessing damming of blood in the veins”

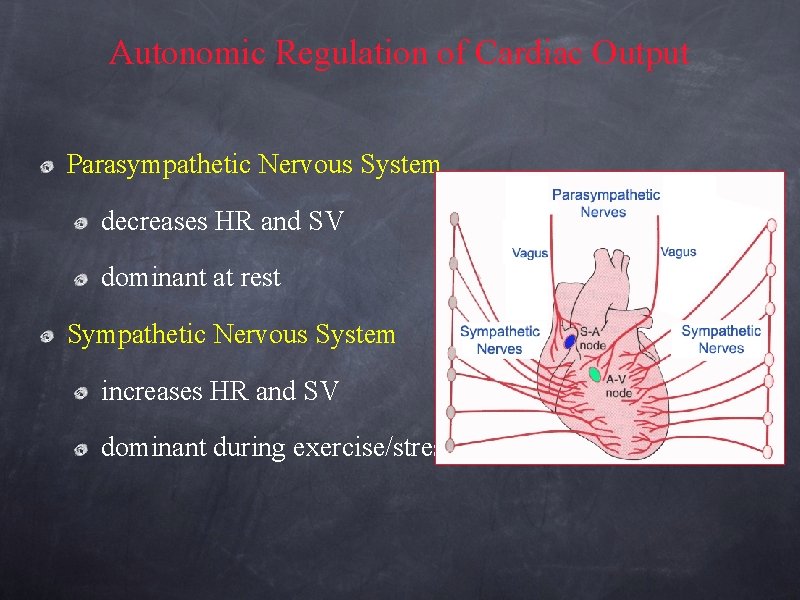
Autonomic Regulation of Cardiac Output Parasympathetic Nervous System decreases HR and SV dominant at rest Sympathetic Nervous System increases HR and SV dominant during exercise/stress

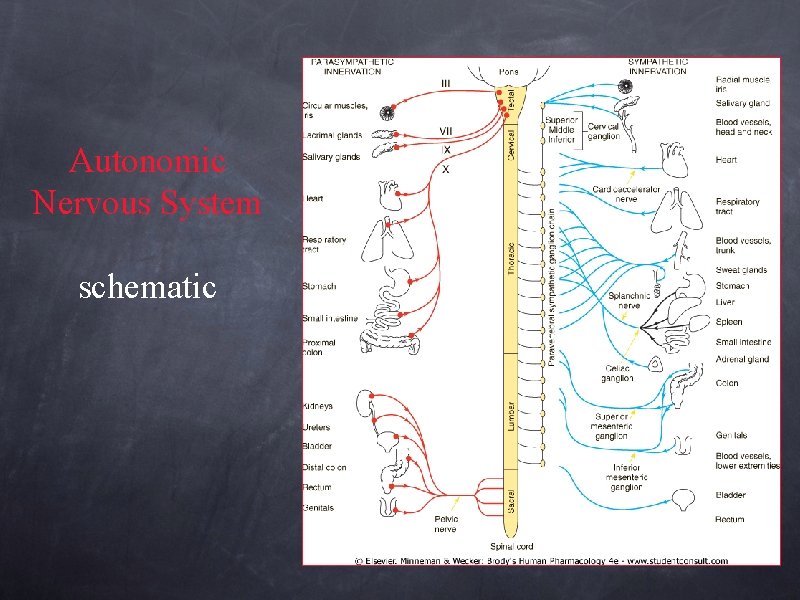
Autonomic Nervous System schematic

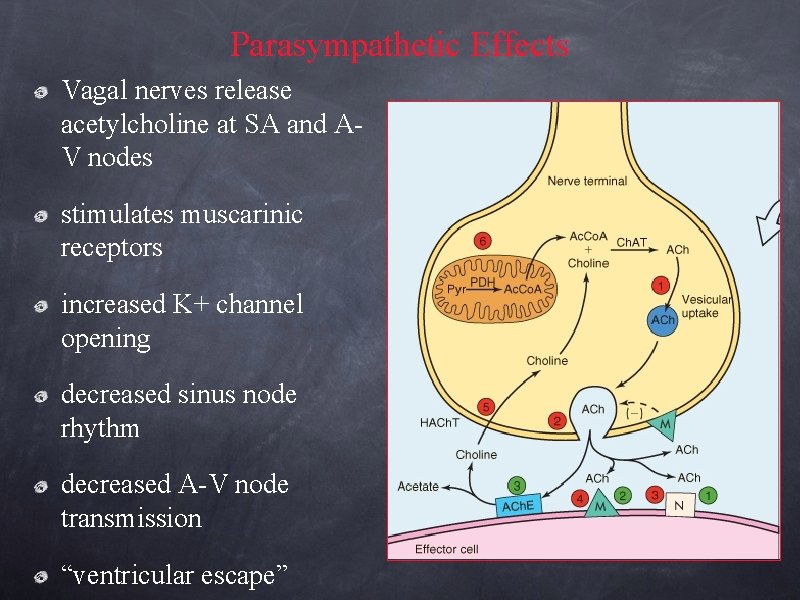
Parasympathetic Effects Vagal nerves release acetylcholine at SA and AV nodes stimulates muscarinic receptors increased K+ channel opening decreased sinus node rhythm decreased A-V node transmission “ventricular escape”

Sympathetic Effects Sympathetic nerves release norepinephrine throughout heart stimulates adrenergic receptors increased Ca+ and Na+ channel opening increased SA node rhythm increased A-V node transmission increased force of atrial and ventricular contraction

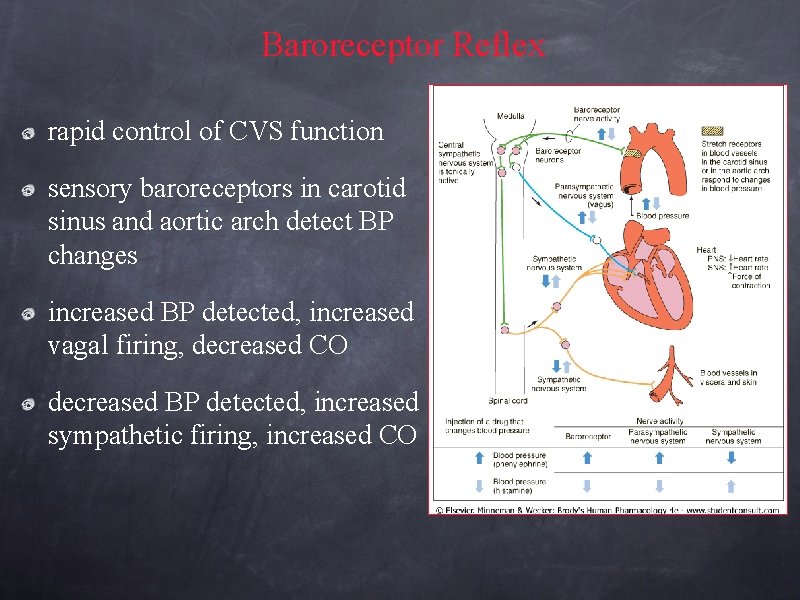
Baroreceptor Reflex rapid control of CVS function sensory baroreceptors in carotid sinus and aortic arch detect BP changes increased BP detected, increased vagal firing, decreased CO decreased BP detected, increased sympathetic firing, increased CO

Renin-Angiotensin System decreased BP causes release of renin from juxtaglomerular cells of kidney into blood renin cleaves angiotensin to angiotensin I angiotensin converting enzyme (ACE) converts Ang-I to Ang-II increases plasma olume and BP, increases O.

Diseases affecting cardiac output atherosclerosis: increased TPR, increased afterload coronary artery disease: decreased cardiac O 2 supply congestive heart failure: decreased stroke volume stroke renal disease diabetes