Regulation of calcitonin secretion Elevation of blood calcium

Regulation of calcitonin secretion • Elevation of blood calcium – Response greater in male – Affected by age • Declines as one ages • Secretion by GI tract – Gastrin • Stimulator of acid secretion – Cholecystokinin

• Response to calcium – Calcium receptors • Increased calcium, increased calcitonin secretion

Physiological roles • Bone mineral metabolism – Prevention of hypercalcemia • After meals – Mineralization of bones in neonates – Protection against calcium loss • Pregnancy • Lactation

• Satiety factor – Regulation of food intake • Inhibition of calcium-induced hunger • Vitamin D regulation – Stimulation of vitamin D metabolism • Direct stimulation • Decreased blood calcium level

Mechanism of action • Receptors for calcitonin – Skeletal tissue, kidneys, and Leydig cells • Coupled with adenylate cyclase • Coupled with different types of G proteins – Gs, Gi, and Gq – Depending on the cell cycle – Trigger different responses (activation of different sigaling pathway)
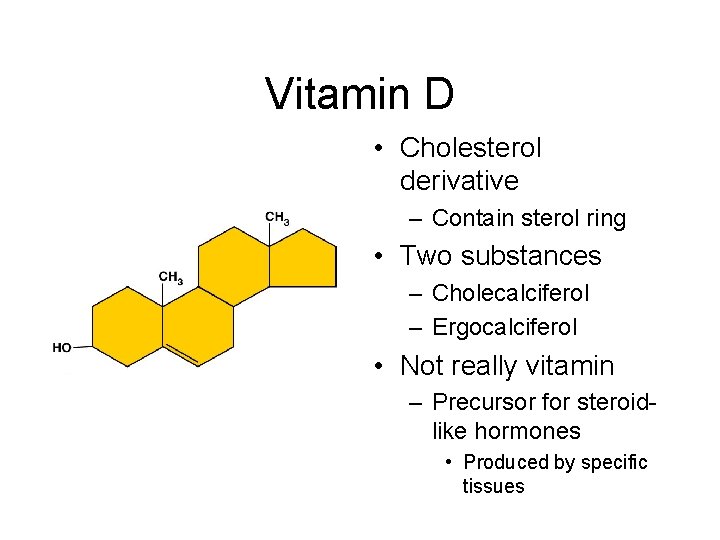
Vitamin D • Cholesterol derivative – Contain sterol ring • Two substances – Cholecalciferol – Ergocalciferol • Not really vitamin – Precursor for steroidlike hormones • Produced by specific tissues
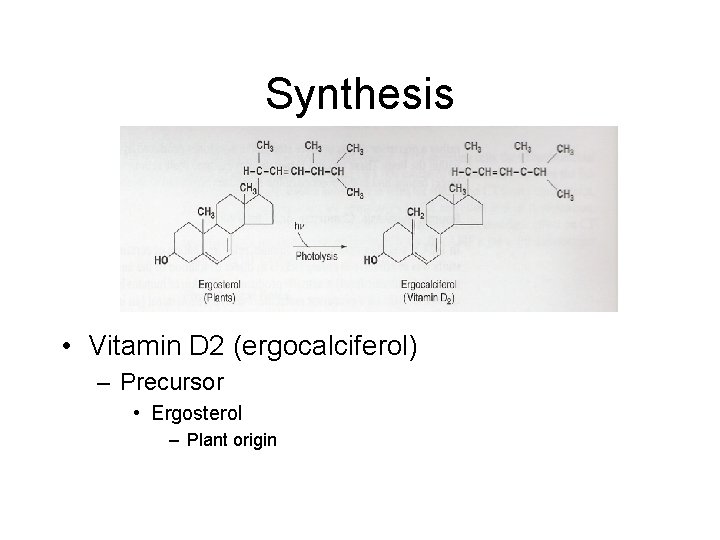
Synthesis • Vitamin D 2 (ergocalciferol) – Precursor • Ergosterol – Plant origin

• Vitamin D 3 (cholecalciferol) – Produced by skin • 7 -dehydrocholesterol – UV light as energy source (thermal isomerization) – Production of inert metabolites (lumisterol and tachysterol) when exposed to sun for a prolonged period – Transported into the blood • Vitamin D 3 only • Binding protein – Transcalciferin
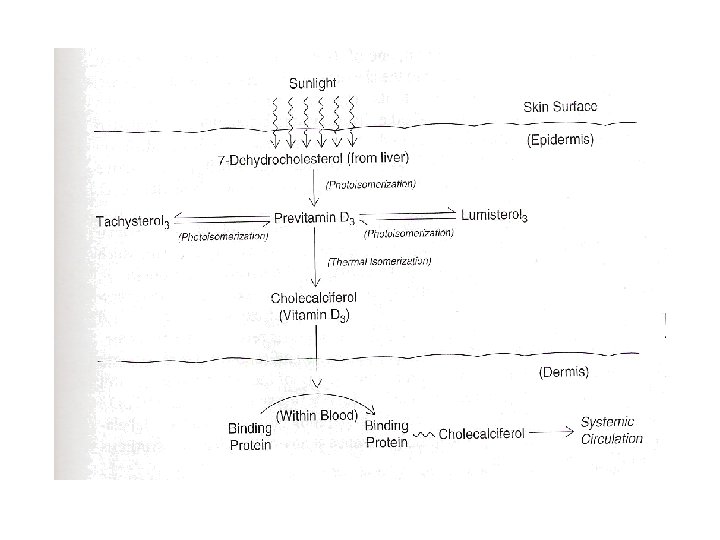
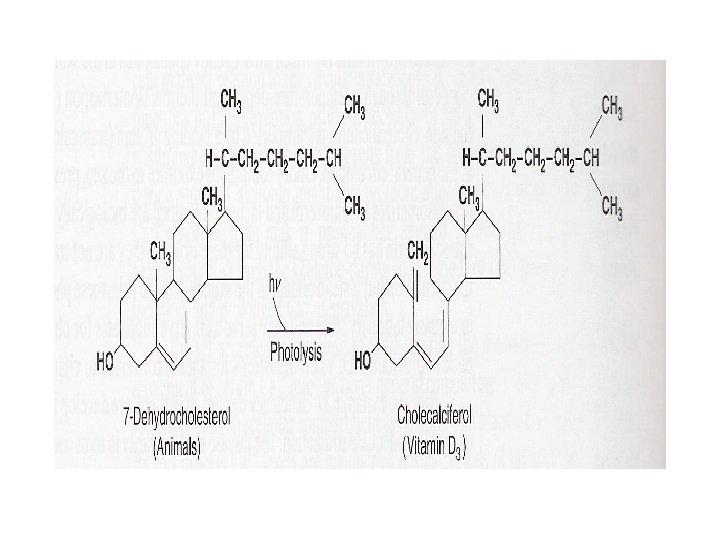

• Vitamin D 3 – Requires further conversion • 25 -hydroxyvitamin D 3 – Liver • 1, 25 -dihydroxyvitamin D 3 – Kidneys – Hormonal form of vitamin D 3 – Bound to plasma protein (transcalciferin) • 24, 25 -dihydroxyvitamin D 3 – Inactive form in mammals – Kidneys and other organs • 1, 24, 25 -trihydroxyvitamin D 3 – Unknown origin and function
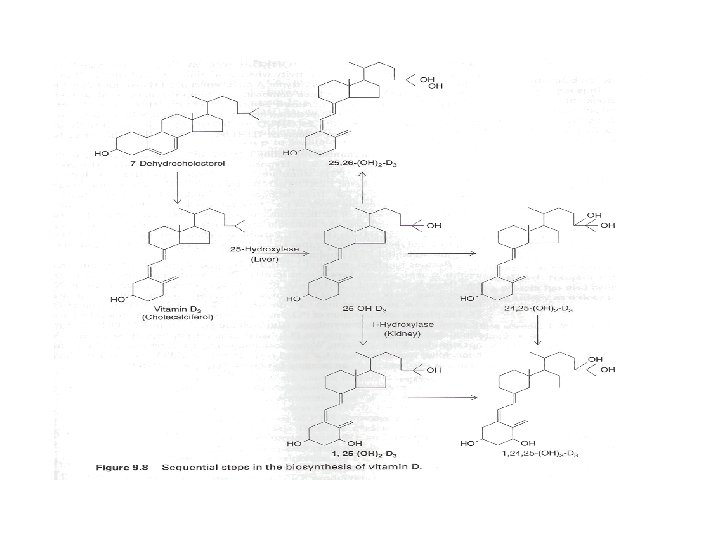

Vitamin D metabolism • Blood calcium level – Production of 1, 25 dihydroxyvitamin D 3 • Increased when low blood calcium level • Decreased when high blood calcium level • Regulated by PTH • Production of 24, 25 dihydroxyvitamin D 3 – Increased when 1, 25 dihydroxyvitamin D 3 decreases • Inhibited by PTH

• Activity of renal 1 alpha-Ohase – Regulation • Vitamin D level (inverse) • PTH (stimulation) – Inhibited by 1, 25 dihydroxvitamin D 3 • Increased phosphate excretion (stimulation) – PTH-induced

• Conversion of 25 -hydroxyvitamin D to 24, 25 dihydroxyvitamin D – Inactivation of 25 -hydroxyvitamin D • Secretion of 1, 25 dihydroxyvitamin D 3 – Hormonal regulation • Insulin • GH • Prolactin

Physiological roles • Absorption of calcium – Intestine • Increased phosphate translocation • Increased calcium transport – From mucosa to serosa via cytosolic calcium binding protein – Bones • Paradox – Essential for normal bone growth – Causes demineralization

• Absorption of calcium – Kidneys • Tubular reabsorption • Retention of phosphate by proximal tubule

• Regulation of PTH secretion – Negative feedback • Long-feedback system – Blood calcium level • Short-feedback system – 1, 25 dihydroxyvitamin D 3
• Proliferation and differentiation of cells – Hematopoetic stem cells – Keratinocytes – Myoblasts • Immune reaction

Mechanism of action • Receptor – Nuclear receptor • Similar to steroid receptor – Ligand binding domain – DNA binding domain • Interaction with hormone responsive element – VDRE • Delayed action (2 hours) – Protein synthesis
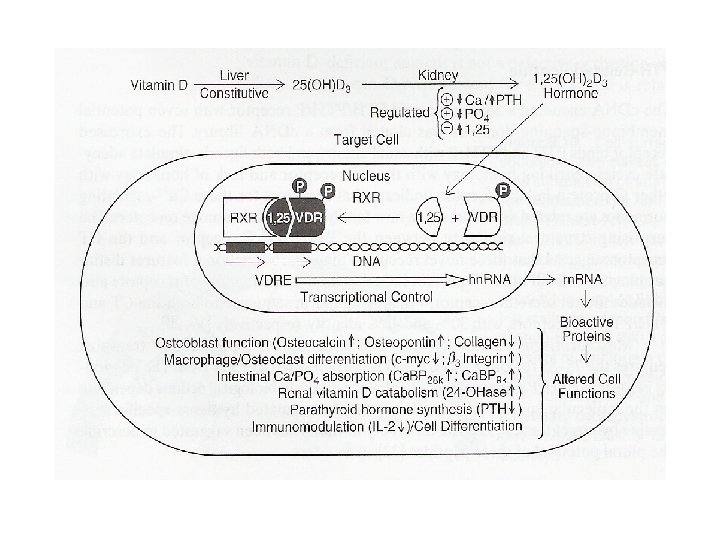

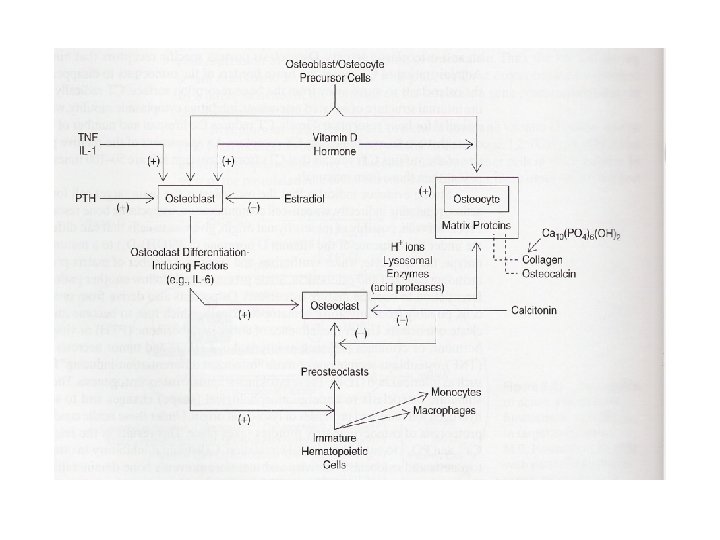
Hormonal integration in calcium homeostasis • Calcitonin – Inhibition of PTH and vitamin D action on osteoclasts • Not on osteoblasts

Hormonal integration in calcium homeostasis • Calcitonin – Inhibition of bone resorption by multinucleated osteoclast • Alteration of morphology • Activity of osteoclast activity – Reduced lysosomal enzyme release • Stimulates detachment of osteoclasts • Inhibit motility • Reduction of lifespan

• PTH – Elevation of blood calcium level • c. AMP mediated • Stimulation of osteoclast activity • Inhibition of osteoblast activity – Osteoblast • Target cells • Indirectly affect osteoclast function

• PTH – Stimulates secretion of osteoclast differentiationinducing factors • Cytokines – IL-6 – Increased differentiation of precursor cells into multinucleated osteoclasts • Morphological changes • Secretion of lysosomal contents • Result in increased release of calcium and phosphate

• Regulation – Short-term • Parathyroid gland – PTH – Long-term • Kidney – 1, 25 -dihydrovitamin D • Intestinal calcium absorption • Decreased skeletal calcium turn-over

• Other hormones – Estrogens • Crucial for maintenance of bone density in women – Inhibition of IL-6 secretion – GH • Greater bone mass in African-Americans
- Slides: 28