REGULATION OF BLOOD PRESSURE DR RASHMI MISHRA Regulation

REGULATION OF BLOOD PRESSURE DR RASHMI MISHRA

Regulation of Blood Pressure v. Arterial B. P. Is controlled by several mechanism which under physiological condition maintain the normal mean arterial pressure which has a narrow range 95 -100 mm of Hg.
REGULATION OF ARTERIAL BLOOD PRESSURE Immediate mechanism ■ Short term mechanism ■ Long term mechanism ■ 02/16/16
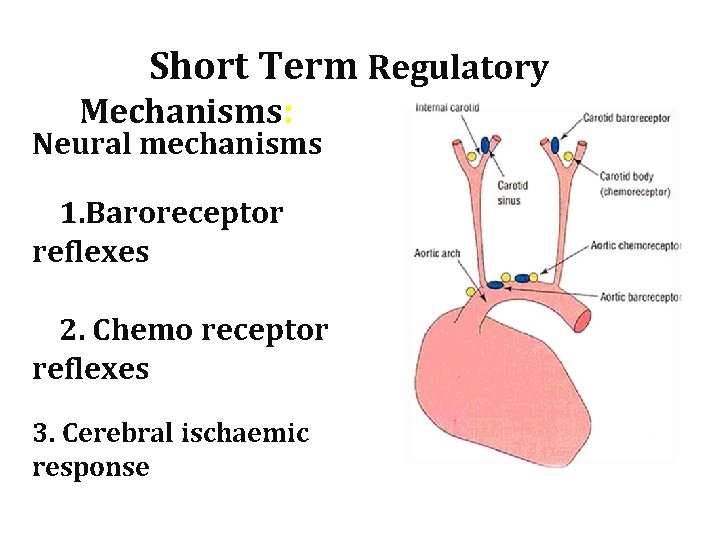
Short Term Regulatory Mechanisms: Neural mechanisms 1. 1. Baroreceptor reflexes 2. 2. Chemo receptor reflexes 3. Cerebral ischaemic response 02/16/16
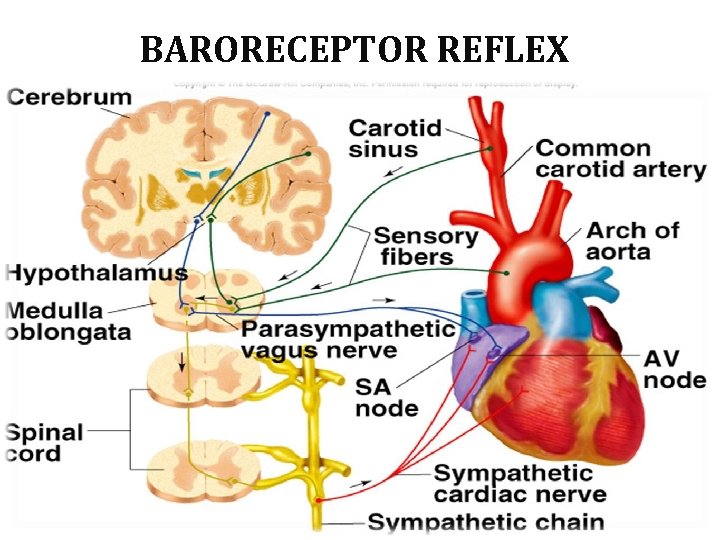
BARORECEPTOR REFLEX 02/16/16
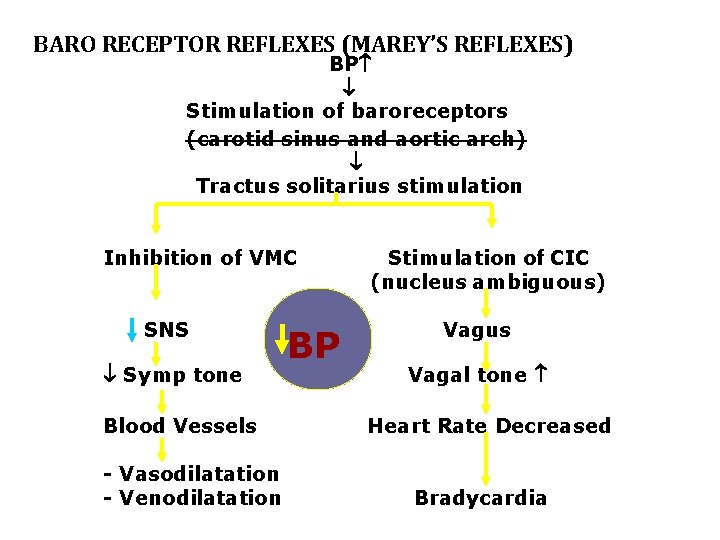
BARO RECEPTOR REFLEXES (MAREY’S REFLEXES) BP Stimulation of baroreceptors (carotid sinus and aortic arch) Tractus solitarius stimulation Inhibition of VMC SNS Symp tone Blood Vessels - Vasodilatation - Venodilatation BP Stimulation of CIC (nucleus ambiguous) Vagus Vagal tone Heart Rate Decreased Bradycardia
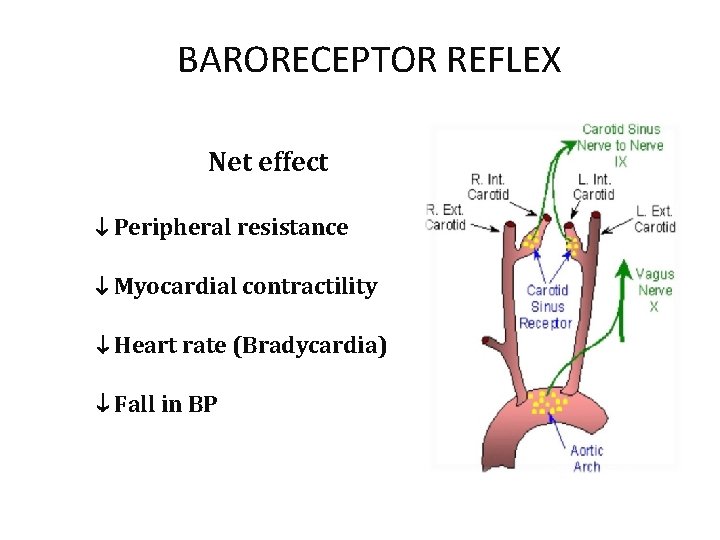
BARORECEPTOR REFLEX Net effect Peripheral resistance Myocardial contractility Heart rate (Bradycardia) Fall in BP 02/16/16


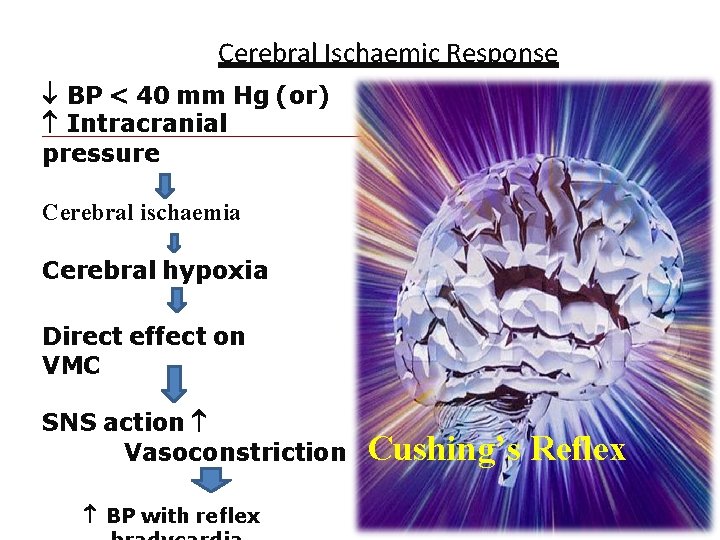
Cerebral Ischaemic Response BP < 40 mm Hg (or) Intracranial pressure Cerebral ischaemia Cerebral hypoxia Direct effect on VMC SNS action Vasoconstriction 02/16/16 BP with reflex Cushing’s Reflex

Delayed or Intermediate Mechanism Capillary fluid shift phenomenon: Whenever there is an increase in blood pressure more fluid is filtered through the capillary wall into the interstitial space. Blood volume decreases and so BP itself decreases. Reverse changes take place when BP falls. 02/16/16
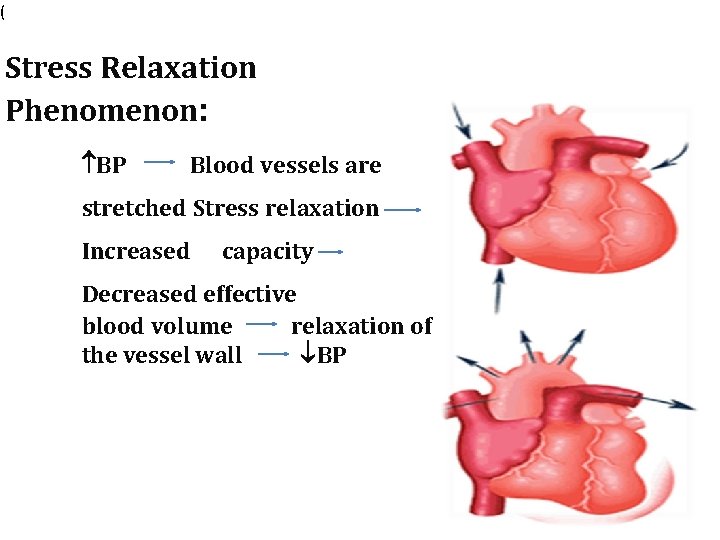
( Stress Relaxation Phenomenon: BP Blood vessels are stretched Stress relaxation Increased capacity Decreased effective blood volume relaxation of the vessel wall BP 02/16/16

REVERSE STRESS RELAXATION q When the B. P. is low due to stress on the vessels walls and tries to restore it back to normal. q This mechanism can correct up to 15% change in blood volume below normal.

Long term Regulatory Mechanisms: All the mechanisms that tend to alter the blood volume participate in long term regulatory mechanisms 02/16/16

RENAL BODY FLUID SYSTEM FOR ARTERIAL PRESSURE CONTROL § The renal body fluid system corrects the B. P. by causing appropriate changes in the Blood volume through diuresis and natriuresis. §WHEN B. P RISES TOO HIGH- The kidney excrete increased quantities of sodium and water because of pressure diuresis respectively. § As a result of increased renal excretion. §The extracellular fluid volume and blood volume both decrease until B. P return to normal and the kidney excrete normal amount of sodium in water.

Increases B. P. (Large intake of Water & Salt) Increased excretion of salt & water by Kidney Decreased in Extracellular fluid & blood volume Decreased venous return to Heart Decreased Cardiac output Decreases B. P.

WHEN THE B. P. FALLS TOO LOW • The Kidney reduces the rate of sodium and water excretion and over a period of hours to day. • If the person drinks enough water and eats enough salt to increases blood volume the B. P. will return to previous level.
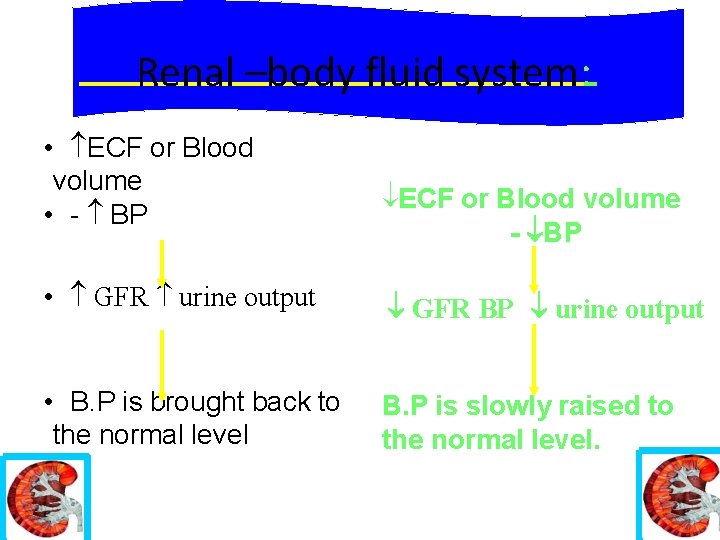
Renal –body fluid system: • ECF or Blood volume • - BP ECF or Blood volume - BP • GFR urine output GFR BP urine output • B. P is brought back to the normal level B. P is slowly raised to the normal level. 02/16/16

Indirect Mechanism When B. P. & extracellular fluid decreases, Renin secreted from kidney is increased it converts Angiotensinogen into Angiotensin I , this is converted into Angiotensin II by ACE(Angiotensin converting enzyme). Angiotensin II act in 2 ways to restore the B. P. : - 1) This causes constriction of arteriole in the body, so the peripheral resistance is increased and B. P. raised, in addition Angiotensin II causes constriction of afferent arteriole in the kidneys so the glomerular filtrate reduces. This return in the retention of water and salt, increase ECF volume to normal volume, this in turn increases the BP to the normal level.

2) Simultaneously, Angiotensin II stimulate zona glomerulosa of adrenal cortex to secrete aldosterone, This hormone increases the reabsorption of Na+ from renal tubules. Na+ is followed by water reabsorption resulting in increased ECF volume and the blood volume. It increases the B. P. to the normal level.
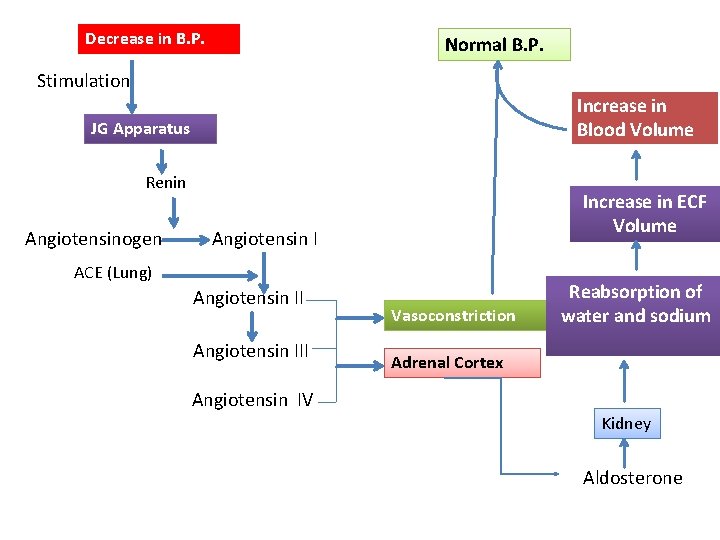
Decrease in B. P. Normal B. P. Stimulation Increase in Blood Volume JG Apparatus Renin Angiotensinogen Increase in ECF Volume Angiotensin I ACE (Lung) Angiotensin III Vasoconstriction Reabsorption of water and sodium Adrenal Cortex Angiotensin IV Kidney Aldosterone

Angiotensin III It increases the BP and stimulate adrenal cortex to secretes aldosterone. It has 100% Adrenal stimulating activity. And 40% vassopresor activity of Angiotensin II. Angiotensin IV It also has adrenal stimulating and vassopressor activities
HORMONAL REGULATIONS Catecholamines Mineralocorticocoid Glucocorticoid Thyroxine ADH Atrial Natriuretic Factor Nitric Oxide Histamine Angiotensin Serotonin 02/16/16

Local Mechanism for regulation of B. P. Ø Instead of renal, nervous and hormonal regulation some local substances regulates B. P. by vasoconstrictor and vasodilation Local Vasoconstrictors ØThey are derived from vascular endothelium. ØThese substances are called endothelium derived constricting factors (EDCF). ØTypes of EDCF – ET 1, ET 2, ET 3 are identified so far. Local Vasodilators Local vasodilators are of two types 1. Vasodilators of metabolic origin (eg. -CO 2, H+ ion, adenosine) 2. Vasodilator of endothelium (eg. - NO(nitric oxide)

Hypertension ❖ Defined as an elevation of systolic blood pressure ❖ Persistent hypertension very common ❖ 30% of people over 50 are hypertensive ❖ Never diagnosed on one reading ❖ Indication of cardiovascular disease ❖ Trauma ❖ Side effect of medication

BP is called Hypertension (Above 140/90 mm of Hg ) Primary (Essential 90%) 02/16/16 Secondary (10%)
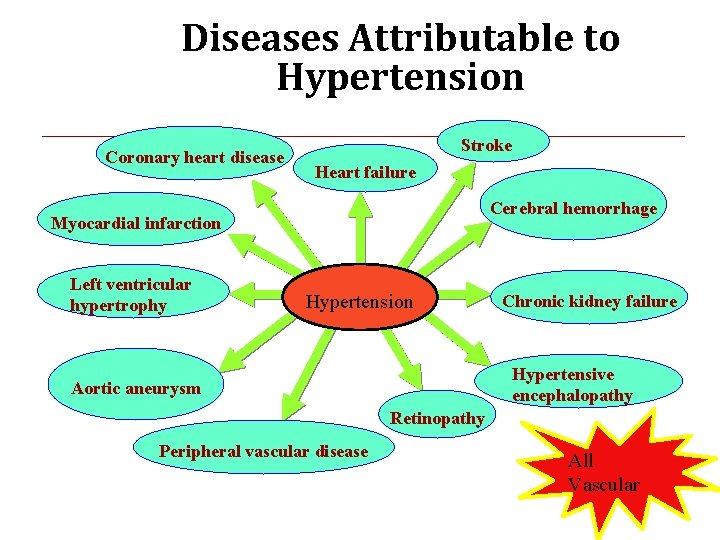
Diseases Attributable to Hypertension Coronary heart disease Stroke Heart failure Cerebral hemorrhage Myocardial infarction Left ventricular hypertrophy Hypertension Chronic kidney failure Hypertensive encephalopathy Aortic aneurysm Retinopathy Peripheral vascular disease All Vascular

Hypertension Predisposing factors: ■ ■ ■ Obesity Hereditary Alchoholism Stress Smoking Sedentary life 02/16/16

ØPrimary Hypertension : 90% of patients suffer from primary hypertension of which the cause is not known, But this is the type of hypertension which is treatable but not curable. - it is treated by antihypertensive drugs. ØSecondary Hypertension : -. This is the type of hypertension which is caused secondary to some disease. ØMalignant Hypertension : This is chronic hypertension which shows lesion in necrotic arterioles. - This condition is associated with Papilledema, Cerebral Manifestation & Renal Failure. - it is treated by antihypertensive drugs.

Secondary Hypertension Causes: ■ 1. Renal-Acute & Chronic Glomerulonephritis, Nephrotic syndrome ■ 2. Endocrine. Cushings, Conns, Thyrotoxicosis, Pheochromacytoma ■ 3. Vascular-Atherosclerosis Arteriosclerosis 02/16/16

Treatment of Hypertension Modification of lifestyle: ■Cessation of smoking. ■Moderation in alcohol intake. ■Weight reduction. ■Programmed exercise. ■Reduction in Na+ intake. ■Diet high in K+. ■Relaxation technique – Yoga, TM 02/16/16

Treatment of Hypertension ■ Medications: ■ Diuretics: � ■ Beta-blockers: � ■ Decrease HR. Calcium antagonists: � ■ Increase urine volume. Block Ca 2+channels. ACE inhibitors: Inhibit conversion to angiotensin II. � Angiotension II-receptor antagonists : � Block receptors. � 02/16/16

Prevention ■ ■ ■ ■ Reduce the risk of developing High Blood Pressure by making lifestyle changes…. . Eat a healthy , well balanced diet Reduce salt and fat intake Exercise regularly Stop smoking Reduce alcohol and caffeine consumption to recommended levels Reduce weight
Hypotension ❖ Defined in adults as a systolic pressure below 100 mm Hg ❖ Rarely treated in this country

q HYPOTENSION Ø A decrease in B. P. below the normal value of 90/60 mm of Hg. Ø Types 1. Primary Hypotension : - It is low B. P. that develops in the absence of any underlying disease & develops due to unknown cause. 2. Secondary Hypotension : - It is the hypotension that occurs due to some underlying disease which cause hypotensiona) Myocardial Infarction b) Hypoactivity of pituitary gland c) Hypoactivity of adrenal glands d) Nervous disorders e) Tuberculosis
BP is called Hypotension (Below 90/60 mm of Hg) 1. Hemorrhage 2. Dehydration 3. Vomiting 4. Diarrhea 5. Excessive sweating 6. Adissons disease 7. Hypothyroidism 02/16/16

Treatment of Hypotension � Treat the cause � Blood transfusion � I. V. Fluids � Vasoconstrictors 02/16/16
- Slides: 38