Registrar Induction Session Welcome to GTD David Beckett

Registrar Induction Session Welcome to GTD David Beckett, Chief Executive Dawn Sewards, Head of Governance Dr Zubair Ahmad, GPST Training Lead - GTD Dianne Hill Operations Manager

Our Philosophy for Patient Care Patient Experience We put patients and their families at the centre of all we do Partnership We work together with individuals and the local community Quality Delivering evidence based care to agreed standards of excellence Continuity Focussing on delivering a seamless patient journey Innovation Developing innovative solutions to improve services
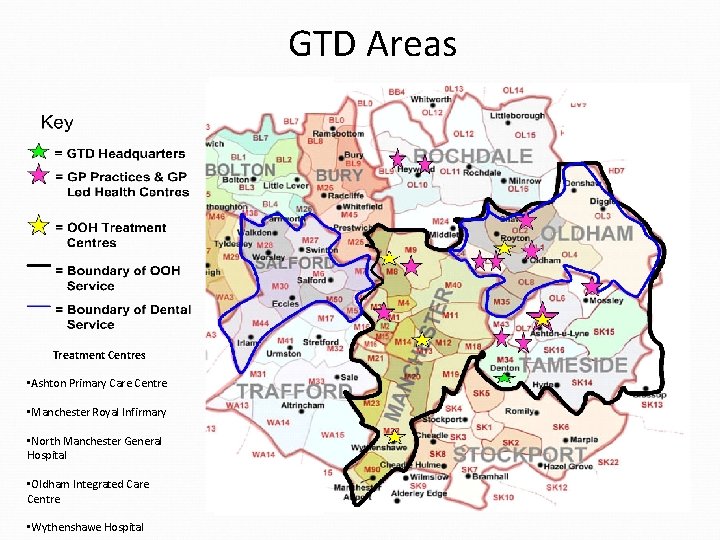
GTD Areas Treatment Centres • Ashton Primary Care Centre • Manchester Royal Infirmary • North Manchester General Hospital • Oldham Integrated Care Centre • Wythenshawe Hospital
GTD Area expansion 01. 10. 13
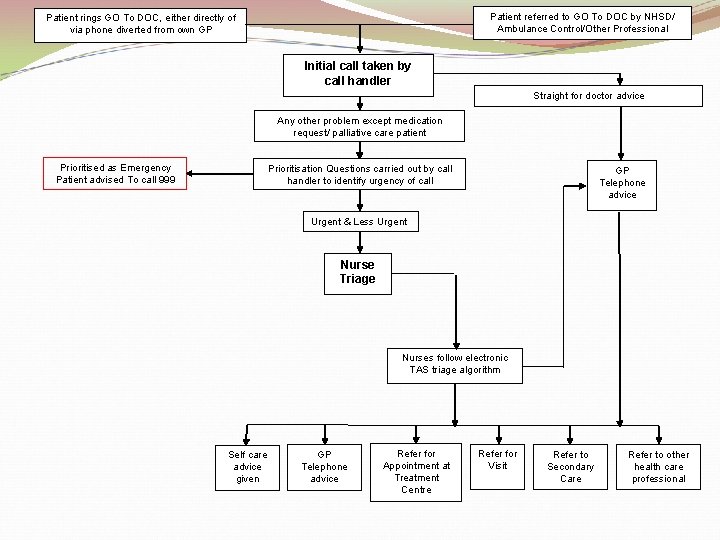
Patient referred to GO To DOC by NHSD/ Ambulance Control/Other Professional Patient rings GO To DOC, either directly of via phone diverted from own GP Initial call taken by call handler Straight for doctor advice Any other problem except medication request/ palliative care patient Prioritised as Emergency Patient advised To call 999 Prioritisation Questions carried out by call handler to identify urgency of call GP Telephone advice Urgent & Less Urgent Nurse Triage Nurses follow electronic TAS triage algorithm Self care advice given GP Telephone advice Refer for Appointment at Treatment Centre Refer for Visit Refer to Secondary Care Refer to other health care professional
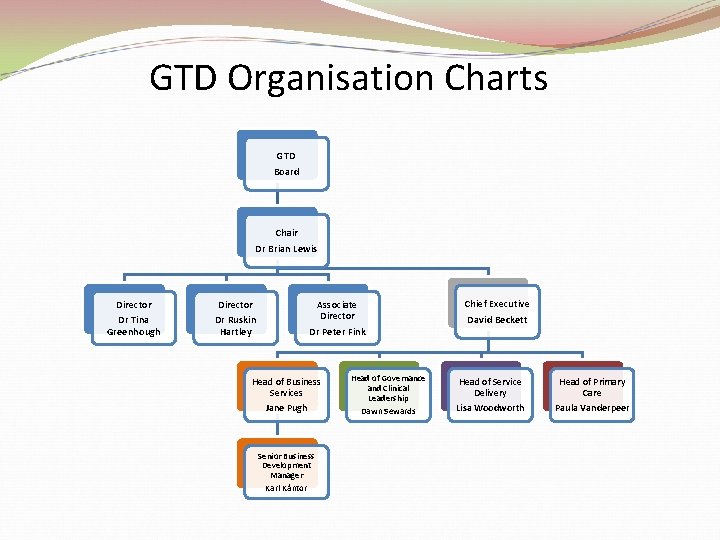
GTD Organisation Charts GTD Board Chair Dr Brian Lewis Director Dr Tina Greenhough Director Dr Ruskin Hartley Associate Director Dr Peter Fink Head of Business Services Jane Pugh Senior Business Development Manager Karl Kántor Head of Governance and Clinical Leadership Dawn Sewards Chief Executive David Beckett Head of Service Delivery Lisa Woodworth Head of Primary Care Paula Vanderpeer
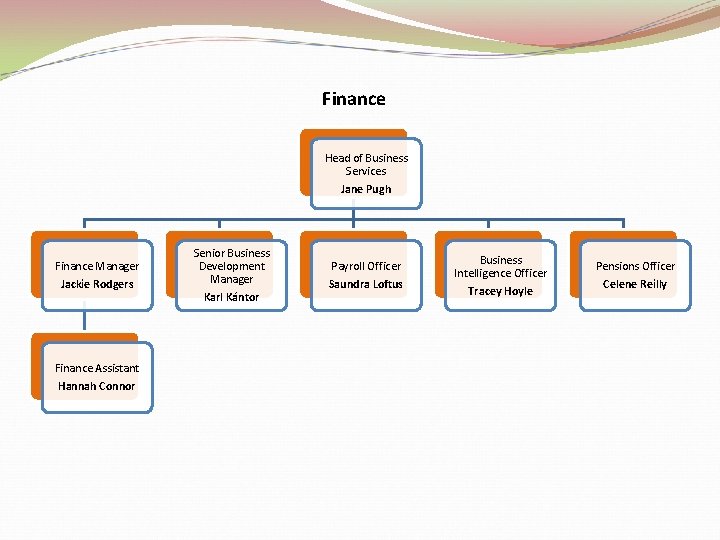
Finance Head of Business Services Jane Pugh Finance Manager Jackie Rodgers Finance Assistant Hannah Connor Senior Business Development Manager Karl Kántor Payroll Officer Saundra Loftus Business Intelligence Officer Tracey Hoyle Pensions Officer Celene Reilly
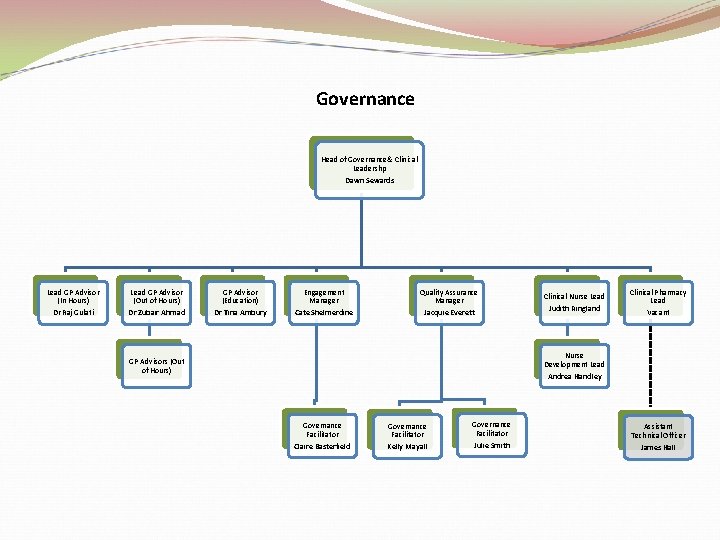
Governance Head of Governance& Clinical Leadershp Dawn Sewards Lead GP Advisor (In Hours) Dr Raj Gulati Lead GP Advisor (Out of Hours) Dr Zubair Ahmad GP Advisor (Education) Dr Tina Ambury Engagement Manager Cate Shelmerdine Quality Assurance Manager Jacquie Everett Clinical Nurse Lead Judith Ringland Clinical Pharmacy Lead Vacant Nurse Development Lead Andrea Handley GP Advisors (Out of Hours) Governance Facilitator Claire Basterfield Governance Facilitator Kelly Mayall Governance Facilitator Julie Smith Assistant Technical Officer James Hall
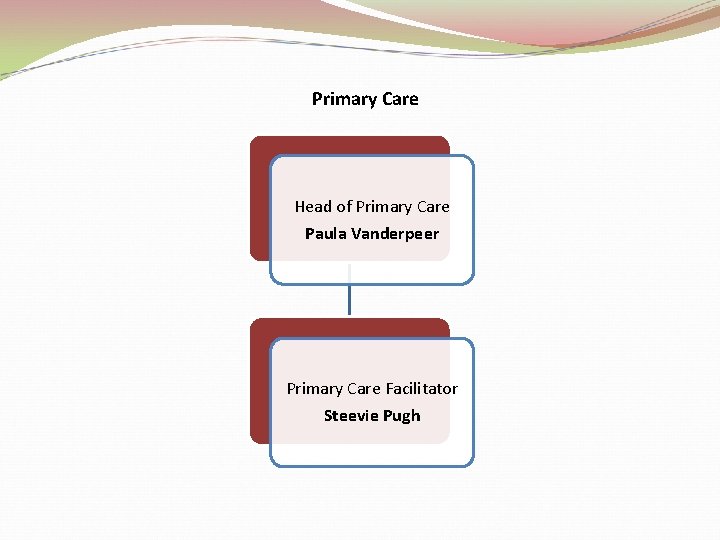
Primary Care Head of Primary Care Paula Vanderpeer Primary Care Facilitator Steevie Pugh
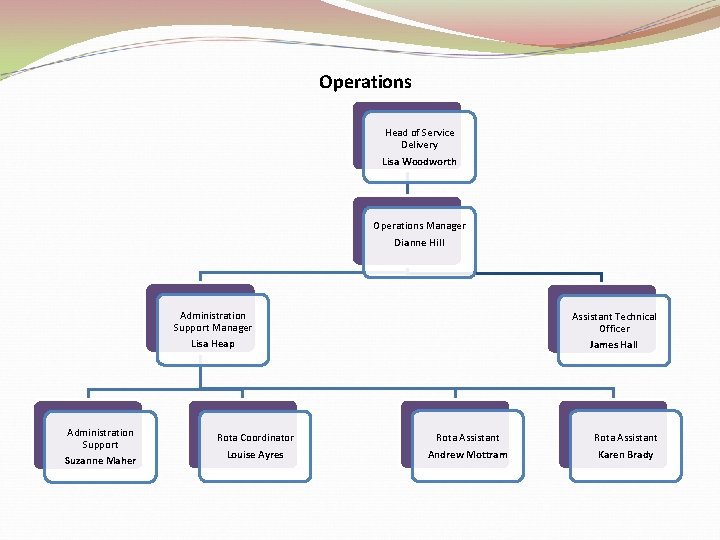
Operations Head of Service Delivery Lisa Woodworth Operations Manager Dianne Hill Administration Support Manager Lisa Heap Administration Support Suzanne Maher Rota Coordinator Louise Ayres Assistant Technical Officer James Hall Rota Assistant Andrew Mottram Rota Assistant Karen Brady

GP REGISTRAR OOH INDUCTION GUIDE Dr Zubair Ahmad FRCGP GP Trainer GP advisor and GPST Training Lead GTD

Learning Objectives & Outcomes History of OOH Care Today Registrar Training OOH What it involves How to register How to book sessions The Art of Telephone Triage Role Play / Scenarios Questions & feedback

History of OOH Doctors were private practitioners, responsible for their own client list Charged accordingly Night Journey & Consultation 4 s 6 d (1855) = £ 192. 02 (2007) Excluding treatment Often payment in kind Public Insurance ‘Poor Law’ National Insurance Act (1911) Ref: P 116 The Evolution of British General Practice 1850 -1948, Anne Digby

History of OOH – Birth of the NHS 1948 – Birth of the NHS Named GP personally and legally responsible for patient care 24 hours / day Managed either by personal lists, or rotas within practices Demand increased over the years GPs on call 5 or more nights / week 1964 – 39% 1977 – 9 %

Growth of Cooperatives 1980’s saw increased use of deputising services and cooperatives Amendments to GMS mid 90 s facilitated this Venue of consultation Changes to visiting fees Shift to co-ops lead to: Greater use of Primary Care Centres The increased role of telephone for triage Decreased exposure to OOH work

Carson report & n. GMS ‘Raising Standards for Patients: New Partnerships in OOH Care’ David Carson October 2000 Single point of access for patients Build infrastructure to meet proposed QRs Share information Record calls Assure Quality n. GMS contract allowed GPs to opt-out (April 2004) National Quality Requirements (1 January 2005) Standards for Better Health (1 June 2005)

Quality Requirements Regularly report to PCT Send details of consultation to registered practice by 8 am ‘Special notes’ system Regularly audit sample of contacts Regularly audit patient experience Operate NHS compliant complaints procedure

st Introduced 1 January 2005 Manage fluctuating demand Initial Call Telephone Clinical assessments F 2 F Clinical Assessments Ensure appropriate clinician treats patient’s needs, in appropriate venue (inc HV) F 2 F Consultation Interpretation services & services for hearing/vision impaired

How is it organised? CCG separate commissioner and provider role Numerous providers GPs who haven’t opted out (usually coops) Not-for-profit orgs /For profit orgs (APMS) PCTs providing their own service (PCTMS) Others

OOH Training ‘…the generalist role of the GP should be maintained and that newly accredited GPs will be expected to have demonstrated their ability to perform competently in OOH primary care’ OOH Training for GP Speciality Registrars, Position Paper COGPED 2007

Why does a GPST require to have an experience in OOH Out of Hours experience is viewed by the Deanery, and the RCGP, as an important and necessary educational component of the GP Specialty training year. The skills developed in this are part of the competences that will need to be present in order for your trainer to sign the Trainer’s report.

Health & Social Care Act 2012 “The role of GP’s has changed – now both providers and clinical commissioners responsible for population health” “Clinical Commissioning about Patients not about GPs” “General Practice has changed – both in-hours and out of hours” “The Urgent Care Landscape has changed” “Biggest change NHS management programme ever” “Just being a GP/Doctor is not enough” – “Strategic Challenge” Understanding the wider urgent care system a key COMPETENCY

What are Out of Hour Sessions? These are sessions where you shadow a GP providing medical care or telephone triage and advice. According to your experience and confidence you will be either seeing patients yourself or sitting in with the GPs consulting. You will always be supervised and supported even during telephone consultations where you will have adequate training.

Out of Hours for Pennine GPST’s Out of hours is a mandatory component of GPST training and you must demonstrate competence to your educational supervisor to allow a CCT to be issued. OOH is defined as work undertaken between 18. 30 and 0800 Monday to Friday, all day Saturday, Sunday and Bank Holidays.

Why do I have to do these? Simple answer: It’s a training requirement. But it’s much more than that, as a Trained GP you will be providing Out of Hours services in some capacity or the other. They are an excellent training tool, as you learn in a supervised environment to identify learning needs and put your skills into practice. Also when you have qualified, the experience gained is invaluable as Out of Hours sessions are a good way to supplement your income.

In addition: You don’t get paid extra for doing these sessions as a trainee, but you can claim for the mileage incurred travelling from your home address to the base station and back on a public transport rate (23 pence a mile – see further guidance on mileage claims guidance in 2009 -pennine GPVTS website ). Of course you are human and like most doctors you may not be particularly enamoured with doing on-call. However you are paid a significant uplift in your salary for on-call and so cannot opt out. You must do out of hours to complete your work place based assessments for the MRCGP.

Moreover… High profile cases and reviews of OOHs • Need for future GP to be fit for purpose • COMPETENT and CONFIDENT • Reviewed – November 2010 • It is mandatory that GP ST 2/3 maintain a portfolio of evidence of achieved competencies and experience

OOH Educational Supervision This is the responsibility of your practice GP Trainer who will undertake overall supervision and management of your out of hours experience. You will need to provide your Trainer with portfolio evidence and formative feedback from your Clinical Supervisor(s) at your OOH provider. We would recommend you do this using the 'Record Of Out Of Hours Session' form as well as the out of hours session learning Log entry in your e-Portfolio under curriculum statement 7, Care of acutely ill People

OOH Clinical Supervision Clinical Supervisors in OOH will complete a record of the session, using the OOH session record sheet, which the GPST must share with the Trainer as evidence of attendance. GPSTs may choose to use an OOH encounter to submit formal case-based discussion

Documenting OOH experience in the e-portfolio GPSTs should record each of their OOH sessions in their e-portfolio. Each entry has to be tagged before filing against at least one curriculum statement heading. Normally in the case of an OOH session this would be curriculum statement 7: Care of Acutely Ill People. All OOH sessions entered into the e-portfolio must be ‘shared’ with the Trainer who may choose to ‘validate’ some of these as contributing to workplace-based assessment. In this case, the entry will also be tagged against one of the twelve professional competency areas.

At the end of the training programme, the Trainer will search for all OOH sessions in the ‘shared entries’ in the e -portfolio (there is a filter facility for this) ensuring that the requisite number have been completed. A declaration is then completed which will appear in the ‘progress to CCT’ section of the e-portfolio.

How many sessions do I have to do? an ST 3 needs to do 72 hours of OOH activity (minimum 12 sessions) The minimum total amount of documented GP OOH activity for a ST 1/2 in a 6 month WTE GP Post is 36 hours (minimum 6 sessions)

OUT OF HOURS EXPECTATIONS – Deanery Guidance The number and frequency of OOH sessions to be completed whilst working in a training practice is defined in Form B for each post. This is usually, but not always, at least one session in a 4 week period. Leaving this until later might reduce your opportunities to complete a sufficient number of sessions toward the end of your post and create problems when an ARCP panel assesses your portfolio. Complete approximately 1 session per month of GP placement of out of hours care with a clinical supervisor at GTD during your 3 years on the scheme (most GPSTs will have to do between 14 and 18 sessions in total).

Types of OOH sessions GPST needs to cover all aspects of OOH care i. e. Telephone triage, emergency clinic sessions and home visiting.

THE GTD PATIENT PATHWAY Type of Shift (Triage, Treatment centre, Mobile)

There needs to be an appropriate balance between telephone consultations and face to face consultations in your out of hours experience. As a guide it might be considered that between a third of your out of hours sessions should focus on telephone consulting. This might vary depending on how much telephone consulting is experienced in the practice in normal hours and the rate of competency progression.

Finally you should remember that some out of hours centres and some sessions tend to be busier than others. It may be the case that in order to demonstrate all the required competencies you might need to do more sessions than those specified in form B or more daytime "on call" activity

What about LTFT trainees? As for LTFTTs – yes they do the same number of sessions as FT - but pro rata over a longer time scale. So if they are working at 50% WTE they would do their nominal 6 sessions over a year.

What are the different types of sessions and what can I expect in these? As mentioned, there can be PCC, Mobile ( Home visits) or Telephone triage sessions. There are generally ample opportunities to discuss the cases with the trainers.

Primary Care Centre Sitting in surgeries or consulting under supervision, you can expect to see almost anything Its important to not forget that although they are usually not that complicated, there is no hard and fast rule. The trick is to develop the skills to deal with these safely. These cases may be given medication, referred to specialties or A&E or even given a review appointments.

Home Visits: It is best to arrive 10 minutes early at the base and go up to the Team leader and introduce yourself. They will direct you to your trainer and help you settle in. Then you set off with your trainer in a driven 4 x 4 / Car to do the home visits. You may be doing 6 -7 visits in a 6 hour session but the time is mainly taken in travelling ‘far and wide’. You will learn how to do home visits quickly and safely in an OOH setting with limited information. The patients can be given advice +/- meds, prescriptions or admitted to hospitals as needed. You will be expected to input the data on the laptop (extra ‘Brownie points’ for doing it while the car is on the move – saves time).

Telephone Triage: After having an induction session to the IT system, getting your Smart Card set up and the operating software ( Adastra), you may be ‘sitting in’ for the first session or two just listening to the GPs consult, but eventually you will be consulting and GPs will listen in (on the second headset or speaker phone), and will guide you through the process to a point where you will consult independently. You will be expected to consult safely, seek help when unsure and input data. The best advice I received was to actually pay attention during the listening in sessions, as this is a great opportunity to learn! Safety netting is ever more important in these sessions.

What should I take with me? Mobile kit and Doctors bag Already provided Be comfortable with its use Familiarise yourself with prescribing in general at OOH Please take the OOH record paperwork, fill these in as you go along and get your trainer to fill in their feedback and suggestions.

GPST Training OOH’s 1. Common Emergencies Chest pain, MI • CVA, collapse, fits • Acute Asthma /COPD • GI bleeds/Acute abdo • R. Colic/Pyeloneph/retent. • Ectopic, PID, Bld in Preg • Obstetric emergencies • Confus /Intox / psychotic • Allergy, anaphylaxis

GPST Training OOH’s 1. Common Emergencies …. . • ILL Child • Infectn. /Septica/ Meningiti • Ortho. / cord comp/Back P • Acute Eye pain/loss of V. • Sudden Death • Paed Emers. – Meningitis /croup/asthma/febrile con. /Gastro -enteritis. / dehydration / NAI • MH crises/Suicide Risk A. / MH Act sections • Basic Life Support • Emer Drugs & equipment

GPST Training OOH’s 2. Organisation of the NHS URGENT CARE/OOH’s - local & national • Processes local & national • Roles & responsibilities – GP practices, OOH’s providers and PCT’s • Impact of Emergencies & Health initiatives – procedures for e. g. CMO cascade, alerts • Outbreaks – infect dx, flu, / Winter bed crisis • Awareness of Communications OOH’s & IT systems (Connecting for Health- Best Practice Design) • Towards paperless systems OOH’s – on the telephone, at PCC or at home (via cars) ; NB decision support systems e. g CAS, NHS Pathways

GPST Training OOH’s 3. Appropriate Referrals • Aware of range of professionals & facilities • Courtesy, Effective Communications, prompt & appropriate referrals – clear documentation & follow up arrangements • Respect other roles & skills & work with ambulance / paramedics and others (cf ECPs , ENPs, Palliative Care staff, DNs)

GPR Training OOH’s 4. Communication & Consultation Skills • Telephone consultation skills • *Triage skills (cf Prioritisation / Streaming) • Understanding - Patient centred (models) – e. g bad news / absence of visual or non-verbal cues – limitations of telephone consultations • Team working – need for effective communication • *changes with NHS 111

GPR Training OOH’s 5. Individual Personal Time & Stress Management Time & workload management • PRODUCTIVITY (4 FTF; 2 -3 HV; 8 -10 TA / Hour) • Problem solving & prioritising • Difficulties of working antisocial & long hours – recognise their limitations • Strategies to manage stress, prevent burnout and maintain good health • Duties & responsibilities – health, safety and performance of colleagues

Standards for OOHs Care National Out of Hours Quality Requirements (13) • Initially Dec 2004 • Revised July 2006 (no changes) • For ALL Out of Hours providers

National Quality Requirements One: performance reporting to PCT monthly Two: Report OOH consultations to patient’s own GP practice by 08: 00 next working day Three: Regular exchange of up-to-date information about patients with predefined needs e. g. Palliative care Four: Clinical audit of all who provide clinical service – (RCGP OOHs Clinical Audit Toolkit) (Urgent & Emergency Care Audit Toolkit 2011)

National Quality Requirements Five: Regular audit of patients’ experience of the service Six: Complaints procedure Seven: Capacity and contingency planning Eight: Telephone answering requirements Within 60 s including a recorded message Nine: Telephone Clinical Assessment 30 s, 20 min, 60 min

National Quality Requirements Ten: Face-to-face Clinical Assessment (walk ins) Eleven: Patients must be treated by clinician best equipped to meet their particular needs Twelve: Face-to-face consultations (Emer – 1 hr / Urgent – 2 hrs / Routine – 6 hrs) Thirteen: Providing services for people with language difficulties, impaired hearing or impaired sight

When should I start doing them? It’s generally advisable to start them fairly early in your GP placements. Leaving them for later will mean there won’t be an even spread and you won’t be able to show a good progression in your skills. Also with the CSA and other hurdles you may struggle to fit it all in. Also it might be difficult to get all the session slots including telephone triage sessions completed before the final ARCP deadline.

How should I log these in? Best to take the paper version of the document with you (link given) and when logging it in as an OOH session can upload the scan. Otherwise if there is time and you have access to a computer it can be done directly onto the e-portfolio with the supervisor, but there is no room for the supervisor feedback.

What do I do when I have finished the requisite number? Your educational supervisor will sign you off in your Eportfolio for the OOH sessions once you have completed the minimum number AND demonstrated all the OOH competencies (this may take more than the minimum number of OOH sessions). This should be no later than your final educational supervision meeting.

What if I want to cancel or if don’t turn up? Try to attend the sessions, as they will have been confirmed to the OOH care provider. Inform your Supervisor directly, especially if there is short notice and contact rota master well in time if you want to cancel so that the slot can be offered to others. If the GPST doesn’t turn up for the session, it should be communicated by the supervisor to the Programme Directors.

What if I have questions? There a lot of people to ask. Ask your colleagues especially ‘Older ST 3 s’, Supervisors, your Trainer and Programme Directors etc. Contact me: zubair. ahmad@nhs. net 07703 477969 (text only please)

Requirements Full time registrars must attend 12 OOH sessions during their GPR year The duration and frequency of these sessions may vary but normally a 4 -6 hr session is appropriate. Trainees should maintain a log of all Out of Hours sessions In order for registrars to gain a full range of OOH experience it is important that they book a range of OOH sessions

Other points to consider: GPSTs should regularly discuss their out of hours eportfolio entries with their trainers and get them to sign off their competencies. Remember it is your responsibility to sort out your OOH sessions! It will be the responsibility of the Educational Supervisor to determine if the criteria for OOH work have been met and ‘sign off’ this section at the final educational supervision meeting

Venues for Out of Hours Sessions Ashton Primary Care Centre Oldham Integrated Care Centre Manchester Royal Infirmary North Manchester General Hospital Wythenshawe Hospital

Competencies There are 6 generic competencies within the RCGP Curriculum section on “Care of Acutely Ill People” and registrars are expected to have demonstrated competence in each of these before your final review.

1. Ability to manage common medical, surgical and psychiatric emergencies in the out-of-hours setting Even caring for large numbers at gtd, no registrar will ever see every possible emergency. The training process must address this knowledge base theoretically, whatever the registrar’s OOH experience. 2. Understanding the organisational aspects of out of hours care A variety of experiences will help equip the registrar to function in any future situation 3. Ability to make appropriate referrals to hospitals and other professionals in the out-of-hours setting 4. Demonstration of communication skills required for out of hours care OOH care requires specific communication competencies eg. use of telephone consultations, operating with a lack of medical records, communicating with other doctors. 5. Individual personal time and stress management This is best accomplished by reflection on direct experience 6. Maintenance of personal security and awareness and management of the security risks to others

ADASTRA Adastra is a leading patient management system for unscheduled care Over 95% of Out-of-Hours GP services across the UK and ROI

ESSENTIAL POLICIES AND PROCEDURES OOH – Different, Riskier How to reduce risks Particular signpost: Palliative care, Safeguarding –Child and adult, Death, Failed encounters, Previous information, Doctor advice, Patients lacking capacity/refusing treatment Read up all the policy documents on GTD staff area website

Summary of next steps Complete the registration form (if not already done) Book your training via contact with Louise Ayres Book your first sessions nice and early! Please plan ahead and spread your sessions

Over to you. . . Questions so Far?

History of Telephone Triage From French – Trier (v. To Separate/Sort/Sift) Prioritising patients based on severity of condition Pioneered by French Military Surgeons during WWI

Telephone Invented by Alexander Graeme Bell First call: 10 th March 1876 “Mr Watson – Come here – I want to see you” First request for medical assistance!

Purpose of Telephone Triage Identify Immediately Life Threatening Conditions Provide advice Establish need for face-to-face consultation Establish venue for face-to-face consultation Facilitate access to other healthcare providers It is in fact a consultation Manage workload/workflow “Other”

What are the components of a good telephone consultation? A phone consult should allow a patient to tell the doctor what is wrong, it should include using a process to collect the relevant information to allow the doctor to come to a view of a differential, and should end with the patient being appropriately managed and knowing what to do next, and when What are the components?

Scenario (1) It’s Saturday afternoon You are the mother of a 3 year old child. Your daughter was sniffly yesterday, but was able to attend playgroup. On returning home, she had a bit of a temperature and didn’t eat her tea. You gave her calpol and she settled well. This morning she was hot, distressed and holding her right ear. You have given some more calpol to little effect, and you are worried she might have an ear infection.

Scenario (2) It’s Tuesday evening You are the son of an 83 year old man, who lives alone. For the past few weeks he has been forgetful at times, and unsteady on his feet. He suffers from Hypertension, and only takes Bendroflumethiazide and a Multivitamin. He is fiercely independent, and has refused any offer of home help. On visiting tonight, you are concerned that he is really quite confused and unable to care for himself. He has been sick a couple of times, and incontinent of urine.

Scenario (3) It’s 7 pm on Friday evening You are a 26 year old unemployed man with a history of drug abuse, currently clean and stable on 30 mg Methadone and 10 mg Diazepam 3 x daily. You have come down from Kent to Ashton to see a friend for the weekend. On getting off the coach it appears that someone has walked off with your bag, and your medication with it. All you have left is your wallet, mobile phone, and the clothes on your back. You have reported theft to the police, who suggested you call the OOH doctors.
Registrar 1

http: //www. gtdstaffarea. co. uk Username: Registrar Password: Registrar 1

Local services How to get details / access How to refer –Secondary care / intermediary care / PHCT

ANY QUESTIONS? (Before we move on to ‘how to book shifts’? )

How to book shifts Log in to www. gtdstaffarea. co. uk Username: Registrar Password: Registrar 1
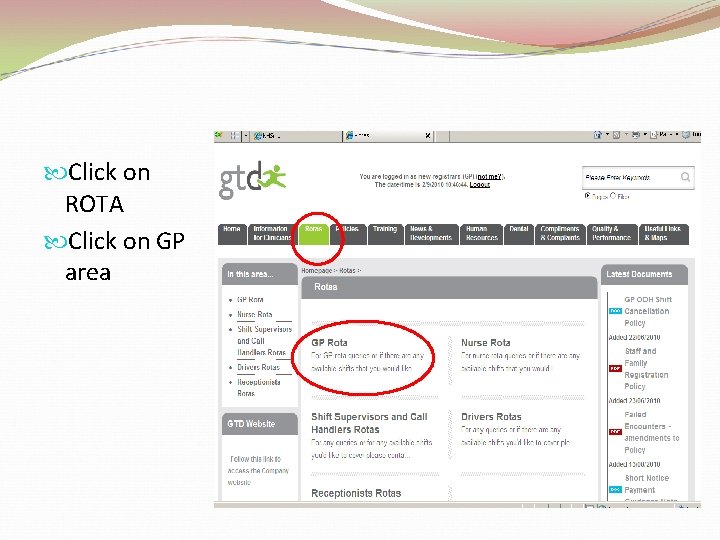
Click on ROTA Click on GP area
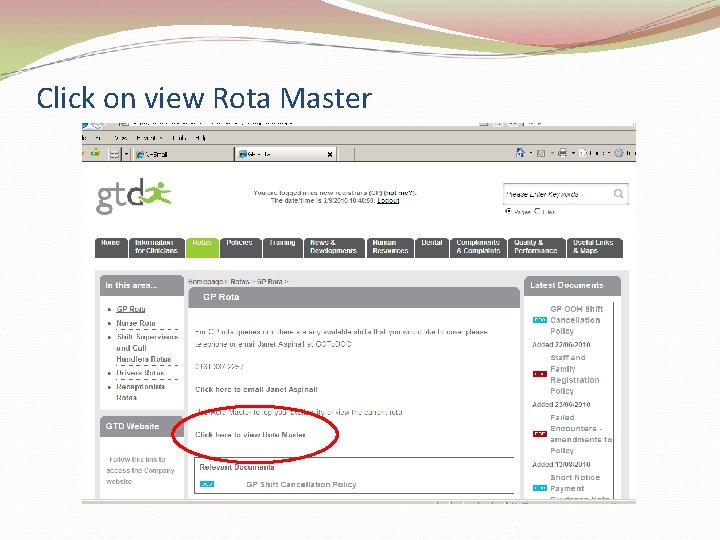
Click on view Rota Master
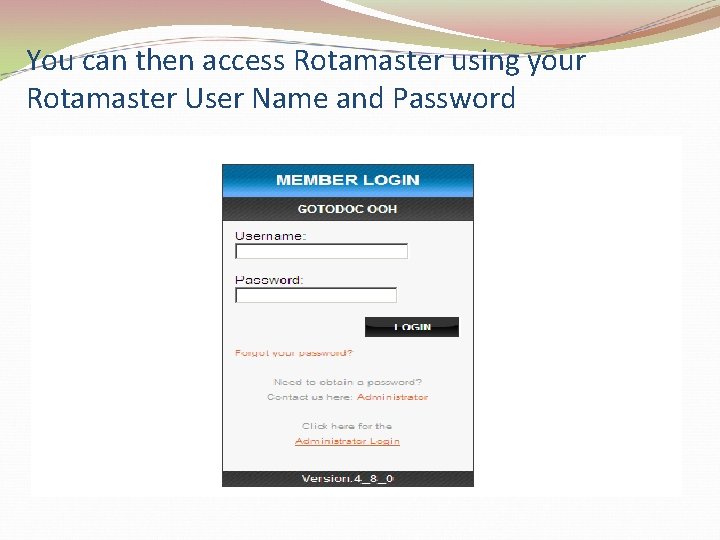
You can then access Rotamaster using your Rotamaster User Name and Password
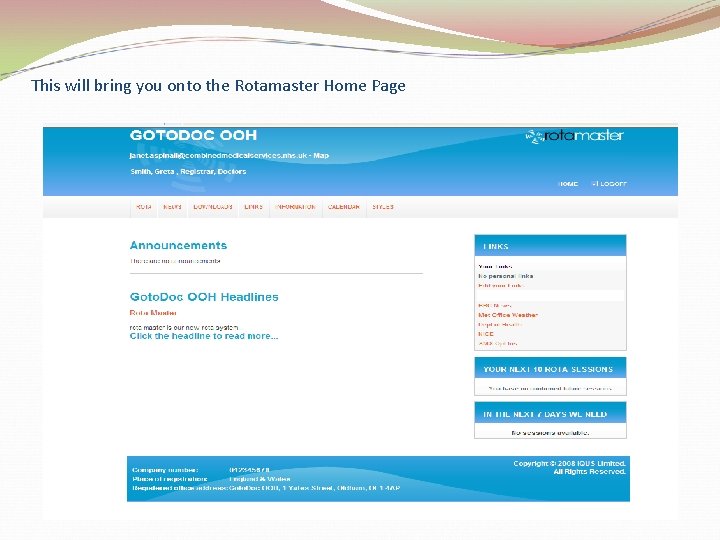
This will bring you onto the Rotamaster Home Page
To look for shifts you have to click on ‘click here for Registrar shifts, you will then need to check your Rota daily as all confirmed shifts will appear on here.
You can then see the available shifts which are available by base by clicking on each base tab

This then brings up any shifts which are available; to apply just tick in the box and press send, The email automatically goes to Louise Ayres who will then see: a. If the shift is still available b. If the doctor is OK to accept you on his shift. Just because you have applied for the shift, it does not guarantee you will get it Contact Details: Louise Ayres Email: Direct Line: Main Office: louise. ayres@nhs. net 0161 337 3466 0161 336 5958

GTD Registrar Shifts At the moment we have 37 working trainers. As we are an OOH provider the available shifts are: Weekday evening, weekend afternoons and evenings List of Treatment Centres available in your information pack with address, telephone numbers etc Shifts which have limited availability are: Weekend morning shifts including Bank holidays – this shift can be extremely busy and we do not want to compromise the service. On call shifts – the doctor only comes in at the last minute if another doctor cancels through sickness so he may not work the shift at all Weekday afternoons Overnight shifts

Cancelled Shifts We do have a cancellation policy for the doctors which states they must give 4 weeks notice which is adhered to except in certain circumstances, i. e. sickness, family emergencies The replacement doctor is not always a trainer so in this instance, the shift will have to be cancelled and you will be notified by email or a telephone call If we do have to cancel a shift, we will endeavour to give you plenty of warning and will try and offer you an alternative shift if possible, but this may not always be on the same day

Communication Confirmation of all shifts whether confirmed or declined will now be sent out to all registrars If the shift is declined an explanation can be obtained if necessary. Usually a shift has been declined as more than one registrar has applied for the shift. This should then make it clearer which shifts you are working. A weekly reminder of all shifts is also sent. By logging into rota master you will be able to also view your allocated shifts Once a month you will receive notification of the available shifts for the next

Frustrations Shift Cancellations If you (the registrar) has to cancel a shift, please give at least 48 hours notice so the doctor can be informed and maybe the shift could be filled by another registrar. Issues / queries Please ring if you have any issues so we can help – 0161 337 3466 between 08: 00 -16: 00 Mon-Fri Please contact us with any problems and we will try to resolve these straight away.
- Slides: 93