Regional Accountable Entity Webinar Orientation for Providers March

Regional Accountable Entity Webinar Orientation for Providers March 28 & 30, 2018
Introducing RAE Rocky Mountain Health Plans (RMHP) is the Regional Accountability Entity (RAE) for Region 1 (all of Western Colorado and Larimer County). The RAE is a contract awarded by the Colorado Department of Health Care Policy and Financing (Department) for the Accountable Care Collaborative (ACC) Phase II. The RAE for Region 1 includes: The services previously performed by RMHP as the Regional Care Collaborative Organization (RCCO), including the primary care medical provider network and care coordination services. The services previously performed by the regional Behavioral Health Organization (BHO), including managing covered services under the Medicaid Capitated Behavioral Health Benefit. The Western Colorado payment reform initiative known as RMHP Prime. Additional services to support whole person care, including activities to address social determinants of health. Note: With the transition to the RAE, the terms RCCO and BHO will no longer be used. Slide 2 rmhpcommunity. org

RMHP PRIME WITH ACC PHASE II RMHP Prime continues with the Accountable Care Collaborative Phase II. o RMHP Prime counties: Garfield, Gunnison, Mesa, Montrose, Pitkin, and Rio Blanco. o The Department continues to pay RMHP a fixed global payment for physical health services provided to RMHP Prime Members are individuals who enroll in RMHP Prime based on county of residence and Health First Colorado eligibility. Eligible adults and children with a disability status are enrolled by the Department into RMHP Prime. o Primary care providers participating in RMHP Prime will continue to receive risk adjusted monthly global payments for attributed RMHP Prime Members. With the changes to the RAE, for RMHP Prime Members, RMHP is responsible for the physical health services historically covered under RMHP Prime, and the behavioral health services covered under the Capitated Behavioral Health Benefit. 3 rmhpcommunity. org

CHANGES FOR MEMBERS
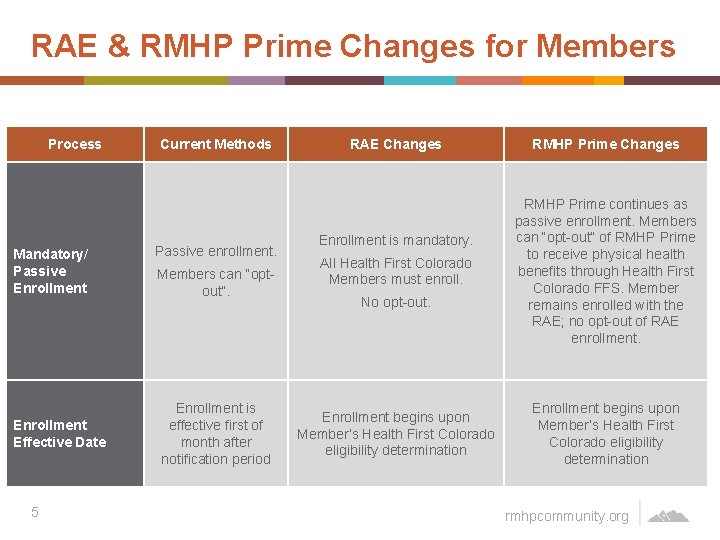
RAE & RMHP Prime Changes for Members Process Mandatory/ Passive Enrollment Effective Date 5 Current Methods Passive enrollment. Members can “optout”. Enrollment is effective first of month after notification period RAE Changes Enrollment is mandatory. All Health First Colorado Members must enroll. No opt-out. Enrollment begins upon Member’s Health First Colorado eligibility determination RMHP Prime Changes RMHP Prime continues as passive enrollment. Members can “opt-out” of RMHP Prime to receive physical health benefits through Health First Colorado FFS. Member remains enrolled with the RAE; no opt-out of RAE enrollment. Enrollment begins upon Member’s Health First Colorado eligibility determination rmhpcommunity. org
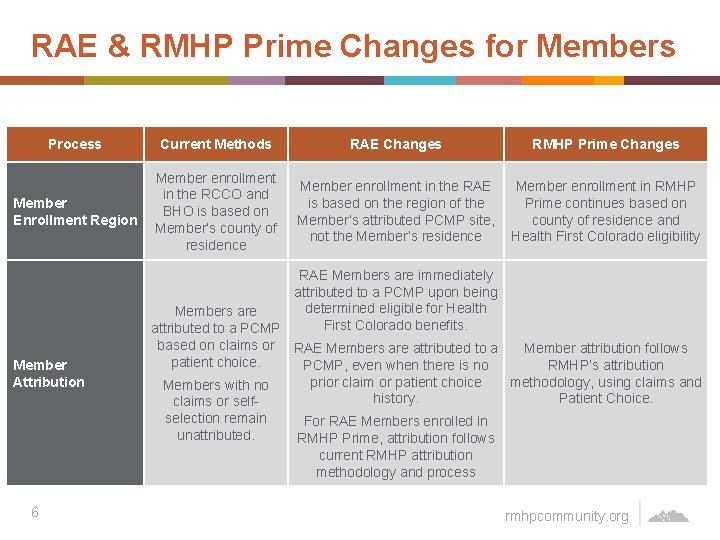
RAE & RMHP Prime Changes for Members Process Current Methods Member Enrollment Region Member enrollment in the RCCO and BHO is based on Member’s county of residence Member Attribution RAE Members are immediately attributed to a PCMP upon being determined eligible for Health Members are First Colorado benefits. attributed to a PCMP based on claims or RAE Members are attributed to a Member attribution follows patient choice. RMHP’s attribution PCMP, even when there is no methodology, using claims and prior claim or patient choice Members with no Patient Choice. history. claims or selfselection remain For RAE Members enrolled in unattributed. RMHP Prime, attribution follows current RMHP attribution methodology and process 6 RAE Changes RMHP Prime Changes Member enrollment in the RAE Member enrollment in RMHP is based on the region of the Prime continues based on Member’s attributed PCMP site, county of residence and not the Member’s residence Health First Colorado eligibility rmhpcommunity. org

RAE & RMHP Prime Changes for Members Process Member Re-Attribution 7 Current Methods RAE Changes On a quarterly basis the Department runs a re-attribution process to identify new Member/PCMP attributions and to change Member/PCMP attributions, based on claims during the most recent 12 months Every 6 months the Department will run a re-attribution process to attribute RAE Members to PCMPs based on claims during the most recent 18 months. RMHP Prime Changes RMHP determines attribution If the Member’s new attributed each month PCMP is in a different region, the Member’s RAE will change to the PCMP’s region. For RAE Members in RMHP Prime, re-attribution follows RMHP’s current process rmhpcommunity. org

CHANGES FOR PCMPs
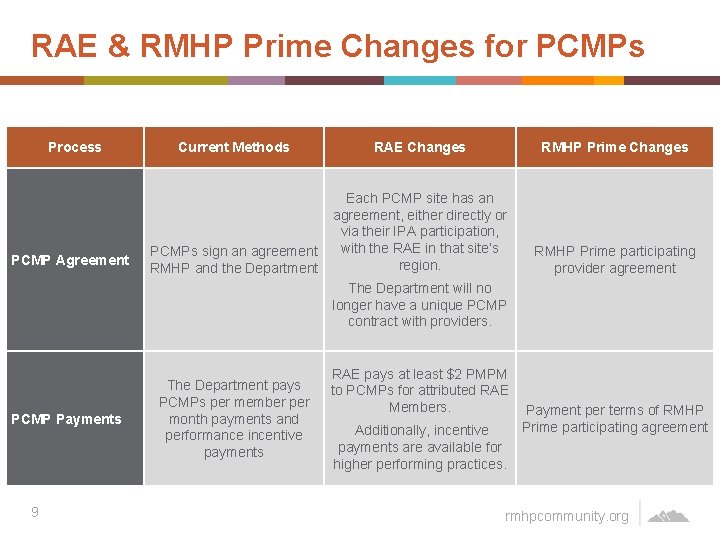

RAE & RMHP Prime Changes for PCMPs Process PCMP Agreement PCMP Payments 9 Current Methods RAE Changes RMHP Prime Changes Each PCMP site has an agreement, either directly or via their IPA participation, PCMPs sign an agreement with the RAE in that site’s region. RMHP and the Department The Department will no longer have a unique PCMP contract with providers. The Department pays PCMPs per member per month payments and performance incentive payments RMHP Prime participating provider agreement RAE pays at least $2 PMPM to PCMPs for attributed RAE Members. Payment per terms of RMHP Prime participating agreement Additionally, incentive payments are available for higher performing practices. rmhpcommunity. org
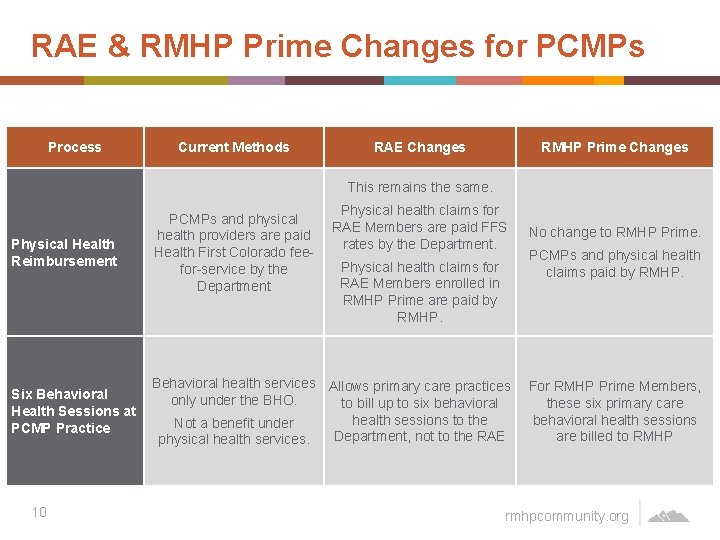

RAE & RMHP Prime Changes for PCMPs Process Current Methods RAE Changes RMHP Prime Changes This remains the same. Physical health claims for RAE Members are paid FFS rates by the Department. Physical Health Reimbursement PCMPs and physical health providers are paid Health First Colorado feefor-service by the Department Six Behavioral Health Sessions at PCMP Practice Behavioral health services Allows primary care practices For RMHP Prime Members, only under the BHO. to bill up to six behavioral these six primary care health sessions to the behavioral health sessions Not a benefit under Department, not to the RAE are billed to RMHP physical health services. 10 Physical health claims for RAE Members enrolled in RMHP Prime are paid by RMHP. No change to RMHP Prime. PCMPs and physical health claims paid by RMHP. rmhpcommunity. org

ABOUT PAYMENT

Value Based Payment RMHP is dedicated to strengthening primary care. We reward high-quality, high-value care and reimburse through a payment structure designed to achieve better care, more efficient spending, and healthier communities. § RMHP is committed to supporting and continuing value-based payments. § RMHP recognizes that health care is complex, and resources are limited. § RMHP’s strategy is to provide maximum resources to the practices that assume the highest level of accountability for whole person care and that provide the highest level of access for RMHP Members. 12 rmhpcommunity. org
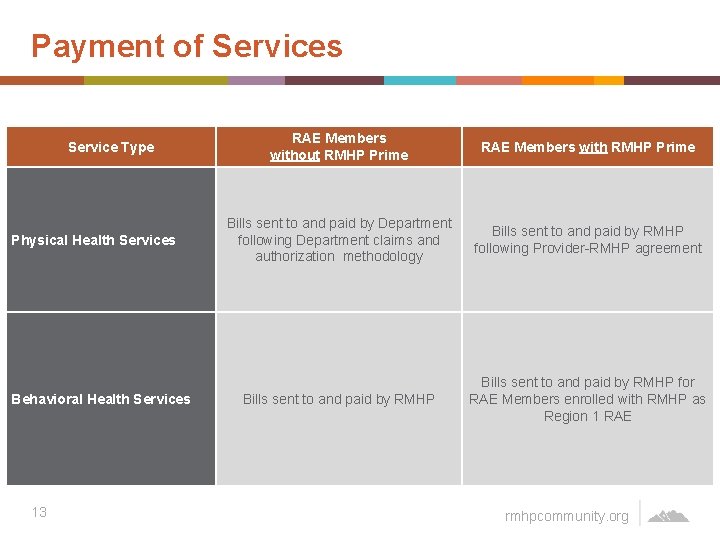
Payment of Services Service Type Physical Health Services Behavioral Health Services 13 RAE Members without RMHP Prime RAE Members with RMHP Prime Bills sent to and paid by Department following Department claims and authorization methodology Bills sent to and paid by RMHP following Provider-RMHP agreement Bills sent to and paid by RMHP for RAE Members enrolled with RMHP as Region 1 RAE rmhpcommunity. org
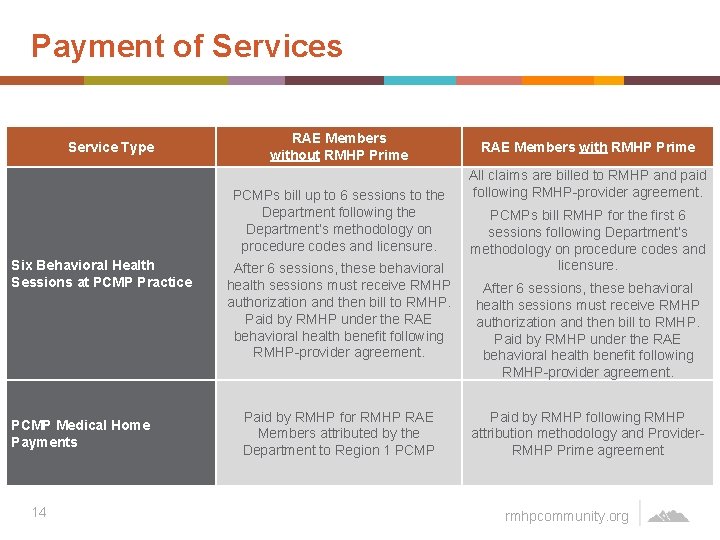
Payment of Services Service Type RAE Members without RMHP Prime PCMPs bill up to 6 sessions to the Department following the Department’s methodology on procedure codes and licensure. Six Behavioral Health Sessions at PCMP Practice PCMP Medical Home Payments 14 After 6 sessions, these behavioral health sessions must receive RMHP authorization and then bill to RMHP. Paid by RMHP under the RAE behavioral health benefit following RMHP-provider agreement. Paid by RMHP for RMHP RAE Members attributed by the Department to Region 1 PCMP RAE Members with RMHP Prime All claims are billed to RMHP and paid following RMHP-provider agreement. PCMPs bill RMHP for the first 6 sessions following Department’s methodology on procedure codes and licensure. After 6 sessions, these behavioral health sessions must receive RMHP authorization and then bill to RMHP. Paid by RMHP under the RAE behavioral health benefit following RMHP-provider agreement. Paid by RMHP following RMHP attribution methodology and Provider. RMHP Prime agreement rmhpcommunity. org

ABOUT ATTESTATION

RAE Primary Care Attestation The value-based payment model for PCMPs encompasses clear delineation of provider responsibilities and resources available for different levels of accountability and participation. These levels of accountabilities, called Tiers, impacts the resources available to the practice and activities the practice must demonstrate through ongoing assessments. Practices have the option to participate at the highest tier for which they qualify, or may choose to participate at a lower tier. Practices also may opt to identify a higher tier and work towards achieving that tier. Each practice site must complete the RAE Tier Attestation process. Complete and submit these documents to the RMHP Practice Transformation Team by April 16, 2018 o Practice Information Form o Attestation Tree Determination Submit documents by: • Mail: PO Box 10600 Grand Junction, CO 81502 • Email: practice. transformation 3@rmhp. org • Fax: 970 -244 -7827 16 rmhpcommunity. org

Tier 1 Description Comprehensive RMHP Population Health Partner Profile CPC+ participant Track 2 or PCMH Level 3/ Recognized Demonstration • Able to report a minimum of 6 CQMs from RMHP e. CQM Measurement Suite from a certified EMR Dashboard (FQHCs may report from the Azara registry) • Meet performance benchmarks on 6/6 measures (See Measurement Suite for benchmarks) • Performs satisfactorily (80%) on RMHP Tier 1 Assessment performed quarterly • Provides current documented Executed Care Compact with at least three major or critical specialties • Open to Medicaid Patients • Medicaid APM/ FQHC APM Score = (at least) 76 - 100% • Use of RMHP designated applications required for Reunion FQHCs and available to others 17 rmhpcommunity. org

Tier 1 Description Comprehensive RMHP Population Health Partner Reimbursement Enhancement • RMHP RAE = Estimated $5 to $6 PMPM (contingent upon region-wide attestations and attribution) • Medicaid APM percent FFS Enhancement on the Department FFS = 3 - 4%+ (or as per Medicaid APM Score) or FQHC Value Based APM/ percent FFS reduction • Eligible for Department auto-attribution revenue for potential patients (Member outreach activities may be required) • Eligible for RMHP Community Integration Agreement to fund behavioral health, SDo. H and related services. Incentive Eligibility • Eligible for KPI Pool distributions – relative to TCR Resource Supplementation • Enhanced RMHP assistance in placing complex, resource intensive patients • Attribution and Feedback Reports • Eligible for Consultative Practice Transformation Resources • Eligible for Health Engagement Team/Community Health Worker resource • Eligible for RMHP designated applications with technical assistance • Eligible for $5 to $10 K bonus for AHCM screening participation 18 rmhpcommunity. org
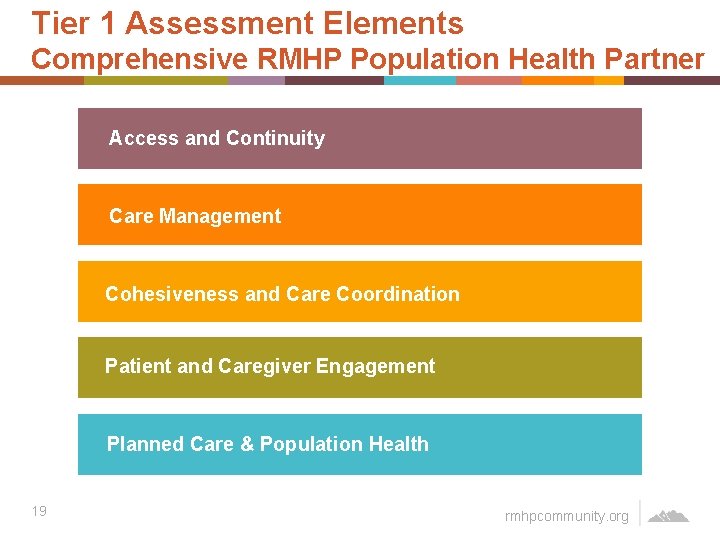
Tier 1 Assessment Elements Comprehensive RMHP Population Health Partner Access and Continuity Care Management Cohesiveness and Care Coordination Patient and Caregiver Engagement Planned Care & Population Health 19 rmhpcommunity. org

Tier 2 Description Advanced Participation Profile Masters 2 Graduate or CPC Classic Graduate or Current CPC+ Track 1 Participant Demonstration • Able to report minimum of 6 CQMs from the RMHP e. CQM Measurement Suite from a certified EMR Dashboard (FQHCs may report from the Azara registry) • Meet benchmark performance (CMS 70 th percentile) on 4/6 (See Measurement suite for Benchmarks) • Performs satisfactorily (80%) on RMHP Tier 2 Assessment performed quarterly • Provides current copy of Executed Care Compact with at least one major or critical specialty • Open to Medicaid patients. Equitable panel management processes permitted, with disclosure of tools and protocols to RMHP. Processes subject to review by RMHP. Current Medicaid attribution levels maintained at a minimum. • Medicaid APM/ FQHC APM Score = (at least) 51 - 75% 20 rmhpcommunity. org

Tier 2 Description Advanced Participation Reimbursement Enhancement • RMHP RAE = Estimated $4 to $5 PMPM (contingent upon region-wide attestations and attribution) • Medicaid APM percent FFS Enhancement on the Department FFS = 2 - <3%+ (or as per Medicaid APM Score) or FQHC Value Based APM/ percent FFS reduction • Eligible for Department auto-attribution revenue for potential patients (Member outreach activities may be required) Incentive Eligibility • Eligible for KPI Pool distributions – relative to TCR Resource Supplementation • Attribution and Feedback Reports • Eligible for Practice Transformation Resources for NCQA PCMH recognition with application fee reimbursement • Eligible for Consultative Practice Transformation Resources • Eligible for Health Engagement Team/Community Health Worker resource • Eligible for RMHP designated applications with technical assistance • Eligible for $5 to $10 K bonus for AHCM screening participation 21 rmhpcommunity. org
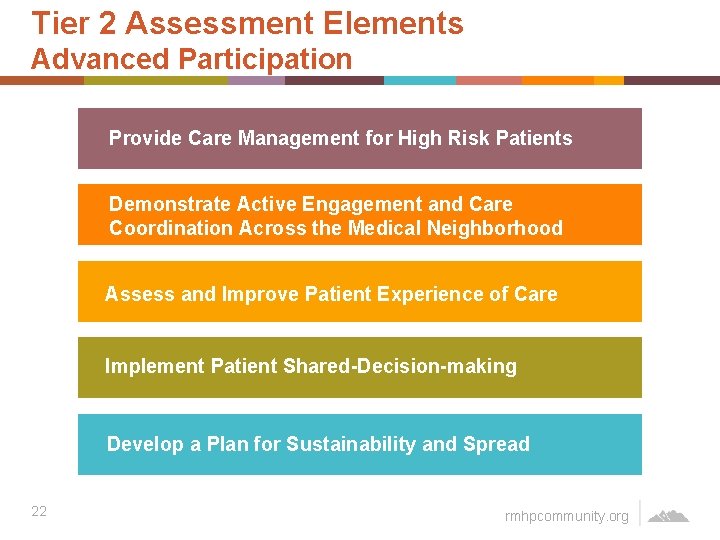
Tier 2 Assessment Elements Advanced Participation Provide Care Management for High Risk Patients Demonstrate Active Engagement and Care Coordination Across the Medical Neighborhood Assess and Improve Patient Experience of Care Implement Patient Shared-Decision-making Develop a Plan for Sustainability and Spread 22 rmhpcommunity. org

Tier 3 Description Foundations Participation Profile Graduate of RMHP Foundations or SIM (For Larimer County practices where RMHP practice transformation programs have been unavailable, other structured foundational work will be considered) Demonstration • Able to report minimum of 6 CQMs from the RMHP e. CQM Measurement Suite from a certified EMR Dashboard (FQHCs may report from Azara) • Meet benchmark performance (CMS 70 th percentile) on 2/6 (See Measurement suite for Benchmarks) • Performs satisfactorily (80%) on RMHP Tier 3 Assessment performed every 6 months • Open to Medicaid patients. Intermittent or limited availability for new Medicaid Members • Medicaid APM/ FQHC APM Score = (at least) 26 - 50% 23 rmhpcommunity. org

Tier 3 Description Foundations Participation Reimbursement Enhancement • RMHP RAE = Estimated $3 to $4 PMPM (contingent upon region-wide attestations and attribution) • Medicaid APM percent FFS Enhancement on the Department FFS = 1% - <2%+ (or as per Medicaid APM Score) or FQHC Value Based APM/ percent FFS reduction Incentive Eligibility • Eligible for KPI Pool distributions – relative to TCR Resource Supplementation • Attribution Reports • Feedback Reports upon request • Practice Transformation Resources with $10 K incentive for Masters 1 and Masters 2 successful program participation 24 rmhpcommunity. org
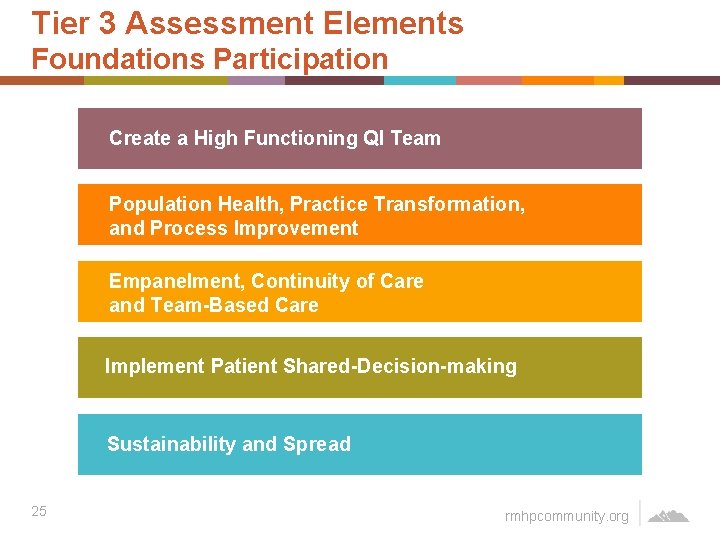
Tier 3 Assessment Elements Foundations Participation Create a High Functioning QI Team Population Health, Practice Transformation, and Process Improvement Empanelment, Continuity of Care and Team-Based Care Implement Patient Shared-Decision-making Sustainability and Spread 25 rmhpcommunity. org

Tier 4 Description Basic Participation Profile No historical practice transformation work completed; may be engaged in RMHP Foundations or SIM Demonstration • None, or • Current involvement in Foundations or SIM • Medicaid APM/ FQHC APM Score = (at least) 0 - 25% 26 rmhpcommunity. org

Tier 4 Description Basic Participation Reimbursement Enhancement • RMHP RAE = $2 PMPM base program reimbursement. • Medicaid APM percent FFS Enhancement on the Department FFS = <1% or as per Medicaid APM Score or FQHC Value Based APM/ percent FFS reduction Incentive Eligibility • Eligible for KPI Pool distributions – relative to TCR Resource Supplementation • Attribution Reports • Feedback Reports upon request • Practice Transformation Resources with $10 K incentive for Foundations program participation 27 rmhpcommunity. org

Attestation Tree Determination In order to stay in Attested Tier, practice must demonstrate ALL of the following: Achieve ≥ 80% on appropriate assessment Achieve Medicaid APM scoring thresholds Submit 6 CQMs quarterly AND annually meet or exceed the 70 th percentile CMS benchmarks • • Tier 1 Assessment – quarterly Tier 2 Assessment – quarterly Tier 3 Assessment – semi-annually Tier 4 Assessment – none • • Tier 1 – Medicaid APM score of 76 -100% Tier 2 – Medicaid APM score of 51 -75% Tier 3 – Medicaid APM score of 26 -50% Tier 4 – Medicaid APM score of 0 -25% • Tier 1 – 6/6 e. CQMs must meet or exceed the 70 th percentile of the current CMS benchmarks Tier 2 – 4/6 e. CQMs must meet or exceed the 70 th percentile of the current CMS benchmarks Tier 3 – 2/6 e. CQMs must meet or exceed the 70 th percentile of the current CMS benchmarks Tier 4 – none • • • Be open to Medicaid • • 28 Tier 1 – Open to new Medicaid Tier 2 – Open with equitable panel management processes and tools applied in order to maintain current Medicaid attribution numbers (at a minimum). Attach processes and tools. Tier 3 – Limited, intermittent availability for new Medicaid patients Tier 4 – Not open to new Medicaid. rmhpcommunity. org
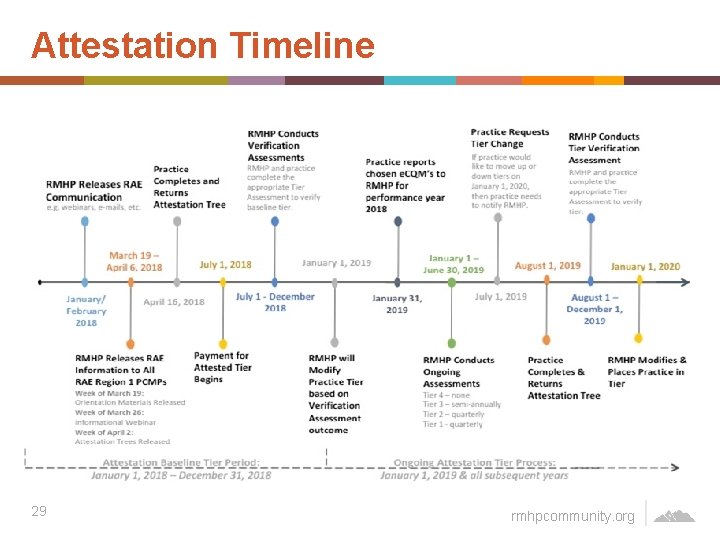
Attestation Timeline 29 rmhpcommunity. org

WE ARE HERE TO HELP

RESOURCES View HCPF-facilitated provider webinars and additional information at Visit RMHP’s community website at colorado. gov/pacific/hcpf/accphase 2 rmhpcommunity. org Email RMHP Community at Call RMHP Customer Service at support@rmhpcommunity. org 888 -282 -8801 31 rmhpcommunity. org
- Slides: 31