Referral Coordination Primary Care Community Based Resources June

Referral Coordination: Primary Care & Community. Based Resources June 21, 2016 8: 00 am – 9: 00 am
We Want To Hear From You! Type questions into the Questions Pane at any time during this presentation

Patient-Centered Primary Care Institute History and Development • Launched in 2012 • Public-private partnership • Broad array of technical assistance for practices at all stages of transformation – Learning Collaboratives – Website (www. pcpci. org) – Webinars & Online Learning • Ongoing mechanism to support practice transformation and quality improvement in Oregon

PCPCH Model of Care Oregon’s PCPCH Model is defined by six core attributes, each with specific standards and measures • Access to Care – “Be there when we need you” • Accountability – “Take responsibility for us to receive the best possible health care” • Comprehensive Whole Person Care – “Provide/help us get the health care and information we need” • Continuity – “Be our partner over time in caring for us” • Coordination and Integration – “Help us navigate the system to get the care we need safely and timely manner” • Person and Family Centered Care – “Recognize we are the most important part of the care team, and we our responsible for our overall health and wellness” Read more: http: //primarycarehome. oregon. gov

Introduce Presenter David Ross Katie Unger Oregon Pediatric Improvement Partnership

Learning Objectives To understand some key concepts and considerations related to: 1. Collecting and managing community-based resource lists 2. Effective referrals 3. Referral tracking 4. Encouraging effective communication and coordination AFTER the referral is made

Why this topic? • A Medical Home strives to be the hub for all care patients receive – A fundamental distinction between a Patient Centered Primary Care Home and a more historically typical Primary Care Provider A successful medical home sees it as one of their roles to manage their patient population and understand the full set of services that they are receiving. 7
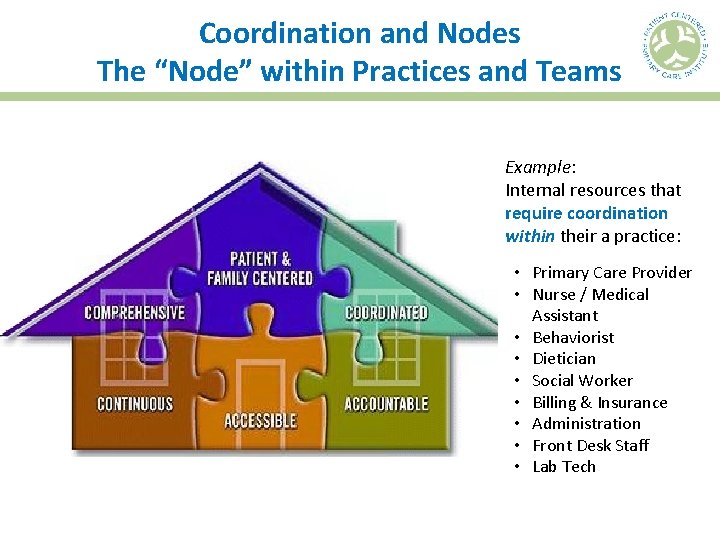
Coordination and Nodes The “Node” within Practices and Teams Example: Internal resources that require coordination within their a practice: • Primary Care Provider • Nurse / Medical Assistant • Behaviorist • Dietician • Social Worker • Billing & Insurance • Administration • Front Desk Staff • Lab Tech
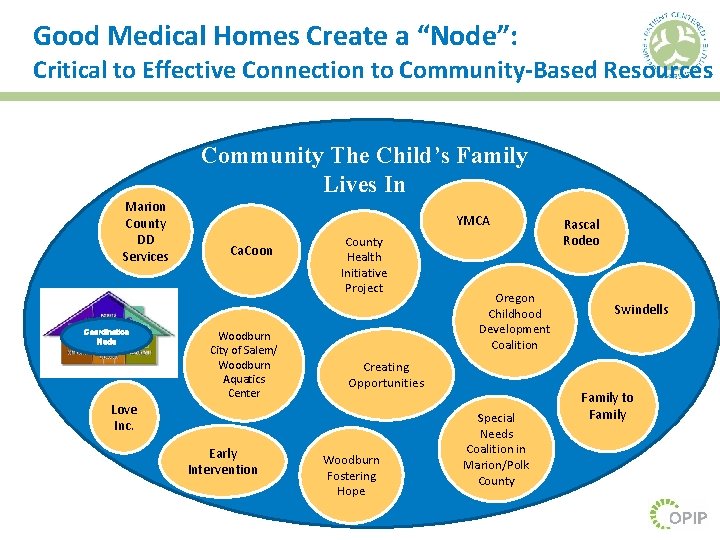
Good Medical Homes Create a “Node”: Critical to Effective Connection to Community-Based Resources Community The Child’s Family Lives In Marion County DD Services Coordination Node Love Inc. YMCA Ca. Coon Woodburn City of Salem/ Woodburn Aquatics Center Early Intervention County Health Initiative Project Oregon Childhood Development Coalition Creating Opportunities Woodburn Fostering Hope Special Needs Coalition in Marion/Polk County Rascal Rodeo Swindells Family to Family

Referral Tracking in the Oregon PCPCH Standards Standard 5. E Referral & Specialty Care Coordination (NOT a must pass standard) • 5. E. 1 - PCPCH tracks referrals to consulting specialty providers ordered by its clinicians, including referral status and whether consultation results have been communicated to patients and/or caregivers and clinicians • 5. E. 2 - PCPCH demonstrates active involvement and coordination of care when its patients receive care in specialized settings (hospital, SNF, long term care facility) • 5. E. 3 - PCPCH tracks referrals and cooperates with community service providers outside the PCPCH, such as dental, educational, social service, foster care, public health, nontraditional health workers and pharmacy services
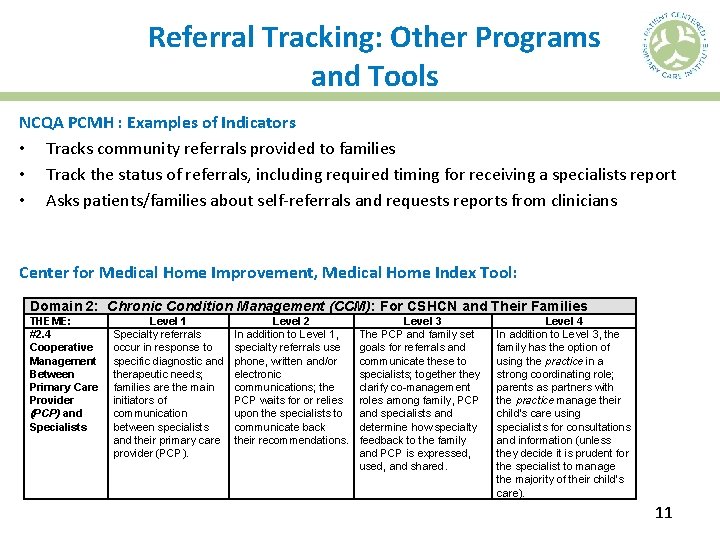

Referral Tracking: Other Programs and Tools NCQA PCMH : Examples of Indicators • Tracks community referrals provided to families • Track the status of referrals, including required timing for receiving a specialists report • Asks patients/families about self-referrals and requests reports from clinicians Center for Medical Home Improvement, Medical Home Index Tool: Domain 2: Chronic Condition Management (CCM): For CSHCN and Their Families THEME: #2. 4 Cooperative Management Between Primary Care Provider (PCP) and Specialists Level 1 Specialty referrals occur in response to specific diagnostic and therapeutic needs; families are the main initiators of communication between specialists and their primary care provider (PCP). Level 2 In addition to Level 1, specialty referrals use phone, written and/or electronic communications; the PCP waits for or relies upon the specialists to communicate back their recommendations. Level 3 The PCP and family set goals for referrals and communicate these to specialists; together they clarify co-management roles among family, PCP and specialists and determine how specialty feedback to the family and PCP is expressed, used, and shared. Level 4 In addition to Level 3, the family has the option of using the practice in a strong coordinating role; parents as partners with the practice manage their child's care using specialists for consultations and information (unless they decide it is prudent for the specialist to manage the majority of their child's care). 11

Developing and Maintaining a List of Community-Resources Key Considerations and Examples from Practices

Developing and Maintaining a List of Community-Resources Goal - Create an inventory of the community-based resources in your area that meet the needs of your patient population, and that you would feel comfortable sending families to. BUT HOW? !?

Key Considerations BEFORE Creating the List Valuable community resources lists are ones that fit within the context of how the practices plans to use this information. Who is the primary audience for the list? – Will it be a resource Providers go in and use ad hoc? Will Care Coordinators be the primary user? How will you categorize your resources? – How one person may categorize resources may not fit with how another person would catalog them (by Dx? by topic area? ) – A practice may duplicate organization links under multiple locations on the resource list as organizations may fall under multiple categories of ‘support’, but this may lead to cumbersome maintenance.

Key Considerations BEFORE Creating the List Who will maintain this list? – Care Coordinator? Referral Coordinator? Medical Assistant? Where will this document ‘live’? – Printed in a binder in a central location? On a shared drive? On an interactive web-based tool? How will it get updated? – Can multiple people update the list, or just the maintainer? What will be the workflow to pass information along about a closed or new resource? How often will it get reviewed? – Continually at QI/Staff meetings? Every 6 months? Annually?

Creating the List: Proposed Workflow It is important to outline your key considerations FIRST. Once you have those elements decided upon, it is time to create the list itself. • Creating an effective resource list requires more than just listing names and contact information. In order to collect the necessary information for a quality list, and also to establish effective communication between the resource and your practice, the following general workflow is recommended: Visual citation: Building the Community Foundation. May 2014. Agency for Healthcare Research and Quality, Rockville, MD. http: //www. ahrq. gov/professionals/prevention-chronic-care/improve/community/obesitypcpresources/obpcp 4. html

Step 1 - Identify the Resources in Your Community Approaches to Identifying Community Resources– • You may have a list to start with. If not, ask your staff to brainstorm a list of the community-based resources they use frequently. It is important to use a group process for this step to minimize the chances of missing resources. • Determine if a resource inventory or directory already exists in the community. – Check with your local health department, the hospital's education department, senior citizen centers, community action agencies, parks and recreation departments. Consider if a modification of an existing directory will work for you. • Look online. Search community and service specific headings, such as “children, nutrition, Salem OR” or “Autism services, children, Gresham OR”, This approach is most helpful in supplementing resource lists already created. • CRITICAL TO ANY APPROACH: ASK FAMILIES! – They are local ‘experts’ that utilize the resources. They may know of resources that you don’t, and may have insight to share about their experiences and knowledge of the resource. – There are many ways you could engage families around this topic, including reaching out to specific parents of children with special health care needs, focus groups with selected parents, or even a specific survey. Building the Community Foundation. May 2014. Agency for Healthcare Research and Quality, Rockville, MD. http: //www. ahrq. gov/professionals/prevention-chronic-care/improve/community/obesity-pcpresources/obpcp 4. html

Examples from Practices: Identify the Resources in Your Community Three Practices we have worked with have surveyed their families to understand resources families use. Approaches each Practice took: 1. Hosted a local organization who supports families to present at a Family Advisory Meeting and then asked families to share about other community organizations that they have utilized 2. Surveyed families that came in for flu clinic 3. Posted questions on their clinics Facebook page

Step 2. Contact Resources to Determine What They Offer - Assign the task of reaching out - It may help to divide the list among staff members and ask them to contact each resource - Collect common information from all resources -It would be best to conduct the follow up interviews in person if you are able. The ability to actually see the resource and not rely on a web site or professional photo to determine its cleanliness, professionalism, and value is helpful. "Good Morning (afternoon), I'm (name) calling from the (name of clinic), here in (name of community). We are trying to improve our understanding of resources in our community, so we can better coordinate and communicate with them in partnership with our patients. We are building a resource directory of all the resources here in (name of the community) that help with (insert topic). We'd like to learn more about (name of resource) and perhaps build a relationship with your organization. Who should I speak to? " Building the Community Foundation. May 2014. Agency for Healthcare Research and Quality, Rockville, MD. http: //www. ahrq. gov/professionals/prevention-chronic-care/improve/community/obesity-pcpresources/obpcp 4. html

Information to Collect Basic Organization Information - Name, Address, Phones, Website, Primary contact etc. Program Description – Purpose or mission of resource Description of ‘Typical User’ – Who do they see and not see Accessibility – Hours of operation and physical barriers Affordability – Cost, insurances accepted Continuity – Funding sources, years in operation etc. Communication – How will the resource communicate back to you? Do they have communication preferences from you? Feedback – Any considerations known about organization from providers or families Building the Community Foundation. May 2014. Agency for Healthcare Research and Quality, Rockville, MD. http: //www. ahrq. gov/professionals/prevention-chronic-care/improve/community/obesity-pcpresources/obpcp 4. html

Example in Practice: Contact Resources to Determine What They Offer In a ‘perfect world’ you could contact all resources to better understand, but in a busy primary care practice, you may need to take baby steps…. • Contact the top 20 resources you refer to • Then contact new resources as you become aware of them • Partner with parents to reach out to community resources as you go along Start small, make it manageable, and add incrementally

Step 3. Create a Resource Directory That Suits Your Clinic Once you have a list of all the resources, along with all the information you collected, you'll want to compile the information into a directory format that fits your office.

Example in Practice: Create a Resource Directory That Suits Your Clinic Woodburn Pediatrics uses an interactive tool called Free. Mind

Example in Practice: Create a Resource Directory That Suits Your Clinic Childhood Health Associates of Salem have built out an internal WIKI that all staff can view and maintain

Step 4. Invite Promising Resources To Visit the Clinic Invite the most likely referral organizations to visit your clinic to build relationships and credibility - Studies indicate that this could help mitigate clinician concerns – which tend to be cost, credibility of the resource, and convenience - Helps the community resource understand provider/practice concerns Building the Community Foundation. May 2014. Agency for Healthcare Research and Quality, Rockville, MD. http: //www. ahrq. gov/professionals/prevention-chronic-care/improve/community/obesity-pcpresources/obpcp 4. html

Examples from Practice: Invite Promising Resources To Visit the Clinic St. Luke’s Eastern Oregon Medical Associates hosted 15 community resources at their practice after clinic for a dinner meeting to learn about the services each entity provided and how they could partner together moving forward Example of attendants: Ca. Coon, WIC, Building Health Families, physical therapy, EI, Immunization Services and Childcare Resource and Referral

Creating Effective Referrals Key Considerations and Examples from Practices
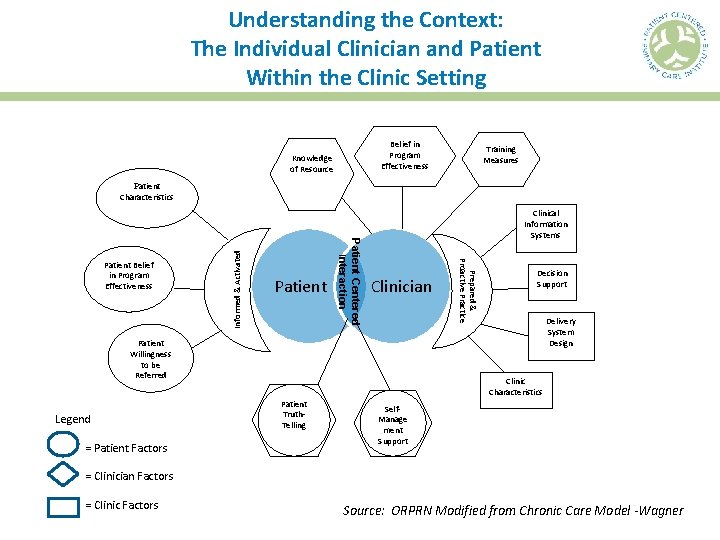
Understanding the Context: The Individual Clinician and Patient Within the Clinic Setting Belief in Program Effectiveness Knowledge of Resource Training Measures Clinical Information Systems Clinician Patient Willingness to be Referred Legend = Patient Factors = Clinician Factors = Clinic Factors Prepared & Proactive Practice Patient Centered Interaction Patient Belief in Program Effectiveness Informed & Activated Patient Characteristics Decision Support Delivery System Design Clinic Characteristics Patient Truth. Telling Self- Manage ment Support Source: ORPRN Modified from Chronic Care Model -Wagner

Categorize and Develop Processes for Different Kinds of Referrals Different TYPES of Referrals Ø Medical Referrals Ø Community Based Referrals Recognize that with each, there may be different processes, different timelines, and different issues that need to be considered. 29

Referral Forms Why create a referral form? • Standardized effective and efficient coordination of care o Provides the information they need to efficiently process and proceed with the referral Ø Potentially avoiding redundant processes/ services o Provides PCP the opportunity to specify desired feedback materials, and clarify feedback mechanisms o Provides the opportunity to attain release of information authorization o Can serve as a decision support tool for effective communication with patients/families

A Medical Home Wants to be the Hub: Referrals Need to be Made in Way that Calls out “Hub” Function Referrals made in a way to ensure care coordination: – Care coordination requires two-way communication – In order to coordinate care, need information about the services received o Includes medical AND community based referrals – Examples: o Referral form to Early Intervention o Referral form to Ca. Coon o Referral form developed by the American Academy of Family Physicians 31

Example of a Referral Form to Early Intervention http: //www. ohsu. edu/xd/outreach/o ccyshn/programs-projects/upload/EIECSE-Referral_new-Med. Statement_11 -05 -2013. pdf 32

Example of a Referral Form to Ca. Coon Home Visiting https: //www. ohsu. edu/xd/outreac h/occyshn/programsprojects/upload/0_Ca. Coon. Universal Referral. Form_2012_0702. docx 33

Example of a Referral/Consultati on Request Form from AAFP http: //www. aafp. org/fpm/tool. Box/view. Too l. Type. htm? tool. Type. Id=26 34

Key Components in a Referral Form • Patient Demographic and Contact Information • Consent/authorization signature to share information • Clinical concern that has been identified leading to a referral • Information the PCP would like back from referred agency

Referral Forms: Within or Outside the EMR? Ideally, a practice would be able to build functionality of referral forms into their EMR to ensure its use and to streamline the referral process. DISCLAIMER: That said, in working with practices we know this may not be a realistic capacity for everyone. 36
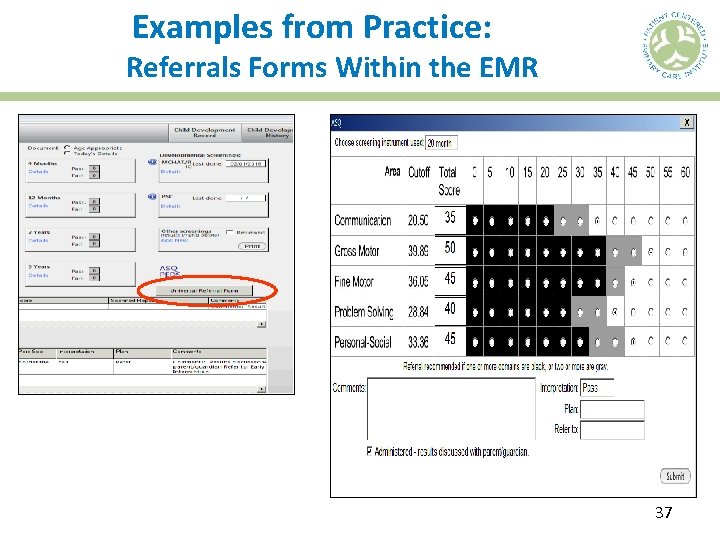
Examples from Practice: Referrals Forms Within the EMR 37

Next. Gen Workflow for Referral to EI Upon selecting Refer to EI in the form, Next. Gen will auto populate the Referral Form (located on the Developmental History tab) to include: • All demographics (that are documented in chart) • Provider Name • Dates • Concerning screening tool Still need to fill in the following fields: • Additional concerns for possible delays • The information you want BACK from EI • PARENT SIGNATURE • PROVIDER SIGNATURE

Tracking Referrals Key Considerations and Examples from Practices

Why Track Referrals? Ø To verify patients get connected to needed services § § Screenings are done to identify risks and concerns that should be followed up on Studies and anecdotal observations from providers indicate that MANY children never make it to referrals § § Note: not sure how this translates to the adult population It may be a long time before the patient comes in for another visit, making what may have been a small concern, a very large concern now 40

Key Consideration: Within or Outside the EMR? Ø This is one of the areas where practices experience the most frustration § § EMRs developed to help track claims Referrals are not claims – so requires innovative thinking and “work-arounds” • If choose to do within EMR, need staff that can help develop creative solutions Ø Observed that practices which are less invested in their EMRs for practice management and care management seem to have had an easier time with referral tracking, given they were already using non. EMR based processes 41

Approaches to Referral Tracking 1. Manually on spreadsheet 2. Create dummy code/EMR work arounds

Tiering Referrals • Practices have found great benefit in tiering their referrals for tracking – This allows support staff to prioritize their efforts as referral tracking can be time intensive and referral priority may defer based on patients needs Considerations- • • • Do cardiology and dermatology hold the same wait for referral tracking? Do referrals vary by patient? Could providers notify staff on the level of importance for tracking, if so – how?

Examples of Innovation Referral Tracking from Practices 44
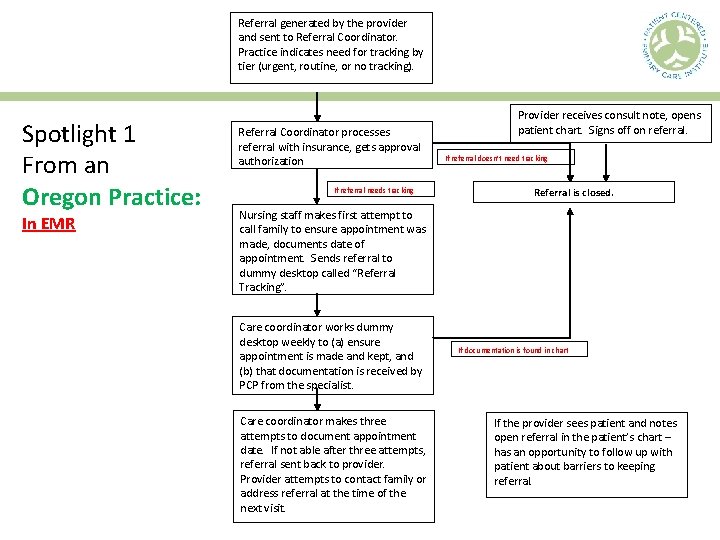
Referral generated by the provider and sent to Referral Coordinator. Practice indicates need for tracking by tier (urgent, routine, or no tracking). Spotlight 1 From an Oregon Practice: In EMR Referral Coordinator processes referral with insurance, gets approval authorization If referral needs tracking Provider receives consult note, opens patient chart. Signs off on referral. If referral doesn’t need tracking Referral is closed. Nursing staff makes first attempt to call family to ensure appointment was made, documents date of appointment. Sends referral to dummy desktop called “Referral Tracking”. Care coordinator works dummy desktop weekly to (a) ensure appointment is made and kept, and (b) that documentation is received by PCP from the specialist. Care coordinator makes three attempts to document appointment date. If not able after three attempts, referral sent back to provider. Provider attempts to contact family or address referral at the time of the next visit. If documentation is found in chart If the provider sees patient and notes open referral in the patient’s chart – has an opportunity to follow up with patient about barriers to keeping referral.
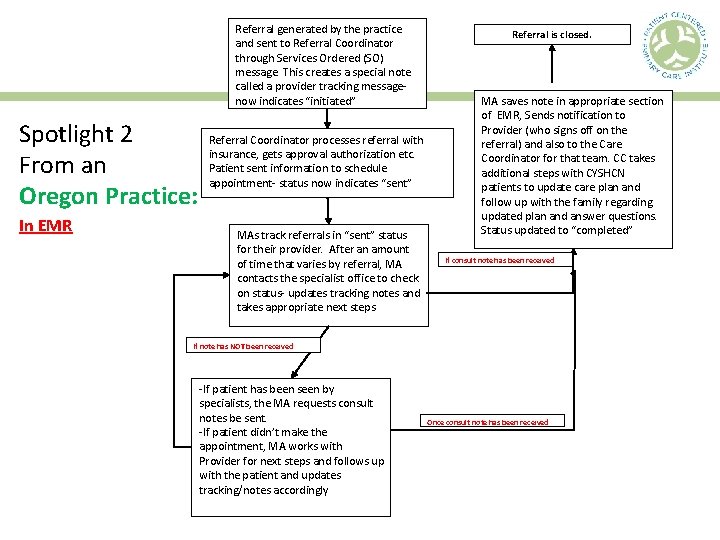
Referral generated by the practice and sent to Referral Coordinator through Services Ordered (SO) message. This creates a special note called a provider tracking message- now indicates “initiated” Spotlight 2 From an Oregon Practice: In EMR Referral Coordinator processes referral with insurance, gets approval authorization etc. Patient sent information to schedule appointment- status now indicates “sent” MAs track referrals in “sent” status for their provider. After an amount of time that varies by referral, MA contacts the specialist office to check on status- updates tracking notes and takes appropriate next steps Referral is closed. MA saves note in appropriate section of EMR, Sends notification to Provider (who signs off on the referral) and also to the Care Coordinator for that team. CC takes additional steps with CYSHCN patients to update care plan and follow up with the family regarding updated plan and answer questions. Status updated to “completed” If consult note has been received If note has NOT been received -If patient has been seen by specialists, the MA requests consult notes be sent. -If patient didn’t make the appointment, MA works with Provider for next steps and follows up with the patient and updates tracking/notes accordingly Once consult note has been received
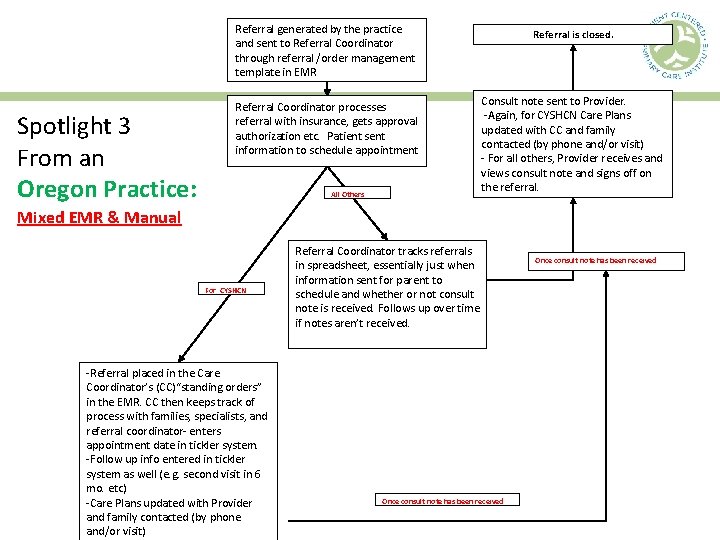
Referral generated by the practice and sent to Referral Coordinator through referral /order management template in EMR Spotlight 3 From an Oregon Practice: Referral Coordinator processes referral with insurance, gets approval authorization etc. Patient sent information to schedule appointment All Others Referral is closed. Consult note sent to Provider. -Again, for CYSHCN Care Plans updated with CC and family contacted (by phone and/or visit) - For all others, Provider receives and views consult note and signs off on the referral. Mixed EMR & Manual For CYSHCN -Referral placed in the Care Coordinator’s (CC)“standing orders” in the EMR. CC then keeps track of process with families, specialists, and referral coordinator- enters appointment date in tickler system. -Follow up info entered in tickler system as well (e. g. second visit in 6 mo. etc) -Care Plans updated with Provider and family contacted (by phone and/or visit) Referral Coordinator tracks referrals in spreadsheet, essentially just when information sent for parent to schedule and whether or not consult note is received. Follows up over time if notes aren’t received. Once consult note has been received

Benefits of Tracking Referrals • Get a better understanding of the care patients are receiving • It can inform your referral patterns and WHO you refer to as a Primary Care provider – You may find providers are referring out for services that you may be able to provide in your office – You may find that wait times differ for the same service at different entities or that some organizations are better at talking back to you about referrals

Encouraging Effective Communication and Coordination AFTER Referral is Made Key Considerations and Examples from Practices

Continuing Communication after Referral is Made Once a referral is made, the communication should not end… – Important to still communicate about: • When patients do and do NOT make appointments • Share information about ongoing treatment plans • If additional services or referrals need to be made to best meet the needs of the patient Best Practice – Invest the time in building relationships with the most frequent referring entities. This will allow you the rapport to follow up when there are concerns and understand the best communication strategies (who should I call and what is the right number)
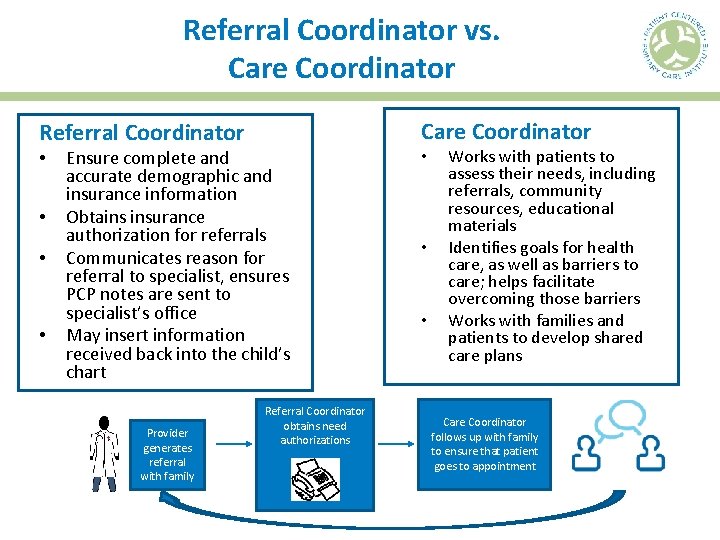
Referral Coordinator vs. Care Coordinator Referral Coordinator • • • Ensure complete and accurate demographic and insurance information Obtains insurance authorization for referrals Communicates reason for referral to specialist, ensures PCP notes are sent to specialist’s office May insert information received back into the child’s chart Provider generates referral with family • • Referral Coordinator obtains need authorizations Works with patients to assess their needs, including referrals, community resources, educational materials Identifies goals for health care, as well as barriers to care; helps facilitate overcoming those barriers Works with families and patients to develop shared care plans Care Coordinator follows up with family to ensure that patient goes to appointment

Spotlight from Illinois: Following-Up on Referrals When People are Making a Decision About Referral • A study showed people make a decision about a referral in the first 48 hours – Often get input from their social/support network • The practices in the Assuring Better Child Development (ABCD) project in Illinois were trying to get more people to access EI referrals Innovation Piloted: Ø Practice Care Coordinator followed up, by phone, the next day to see if parent/patients had any questions and to emphasize importance of referral Ø Provider and office staff reported increased access and increased patient satisfaction with the process 52
What Questions Do You Have? Type questions into the Questions Pane at any time during this presentation

Thanks! • Please feel free to reach out with any further questions – Katie Unger ungerk@ohsu. edu – David Ross rossda@ohsu. edu • Please complete post-webinar survey- your feedback is important to us!
- Slides: 54