Recurrent miscarriage DR shatha sami FICOG CABCOG Recurrent

Recurrent miscarriage DR. shatha sami FICOG CABCOG

Recurrent miscarriage � Definition : ≥ 3 consecutive losses of clinically recognized pregnancies < 20 week gestation �Ectopic, molar, and biochemical pregnancies not included. • Primary recurrent pregnancy loss" refers to couples that have never had a live birth, • “Secondary RPL" refers to those who have had repetitive losses following a successful pregnancy

Epidemiology ▫ Spontaneous abortion: 10 -15% of all clinically recognised pregnancies ▫ 2 consecutive miscarriage : 2% risk of 3 consecutive miscarriage: 1% of all women

Causes Unexplained 43% Endocrine 20% Autoimmune 20% Anatomical 16% Genetic Infectious 3. 5% 0. 5%

Causes • Idiopathic in 40 -50% of cases • Easier to divide into 1 st or 2 nd trimester losses • 1 st trimester losses ▫ ▫ ▫ PCOS (Polycystic ovary syndrome) APS (Antiphospholipid syndrome) Chromosomal abnormalities Endocrine disorders (untreated DM, thyroid disease) Uterine abnormalities �Submucous fibroid �Subseptate uterus

• 2 nd trimester losses ▫ ▫ Cervical incompetence Asherman syndrome (intrauterine synechiae) Bacterial vaginosis Uterine abnormalities �Congenital – bicornuate, septate, subseptate, hypoplasia �Myomas ▫ Thrombophilias • Others – SLE, hyperprolactinaemia

Polycystic ovary syndrome (PCOS) • Criteria for diagnosis (ROTRDAM CRITERIA) • Presence of at least 2 of the following 3 criteria: ▫ Polycystic ovaries �≥ 12 follicles in each ovary (<10 mm (2 -9 mm in diameter)) and/or �Ovarian volume > 10 cm 3 ▫ Oligomenorrhea and/or anovulation ▫ Clinical and/or biochemical hyperandrogenism

Antiphospholipid syndrome (APS) • Most important treatable cause of recurrent miscarriage • Antiphospholipid antibodies: • approximately 3% of recurrent miscarriage • (Anticardiolipin, Lupus anticoagulant) • APA likely induce microthrombi at the placentation site. • Altered vascularity affects developing embryo, induces abortion

Chromosomal abnormalities Karyotyping • 70% of all early spontaneous abortions (<14 weeks) • have chromosomal abnormalities. • Most are autosomal trisomies (50%). • 2 to 4% of couples with RPL will have some form of • chromosomal abnormality on karyotyping. • Most are balanced translocations.
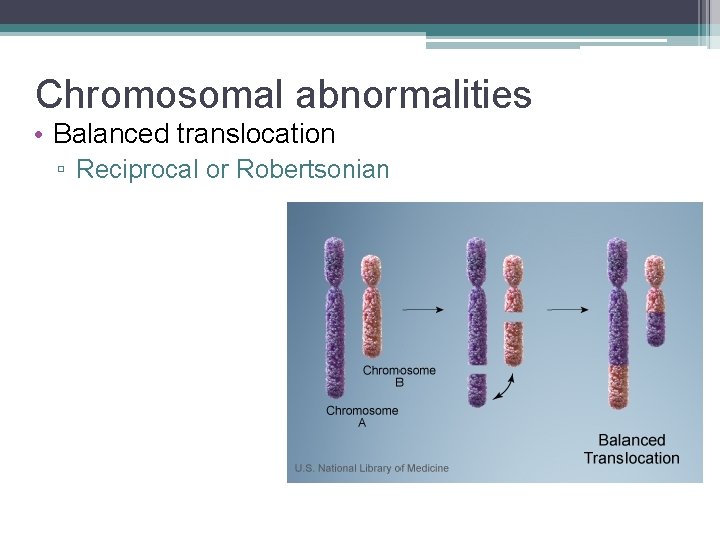
Chromosomal abnormalities • Balanced translocation ▫ Reciprocal or Robertsonian
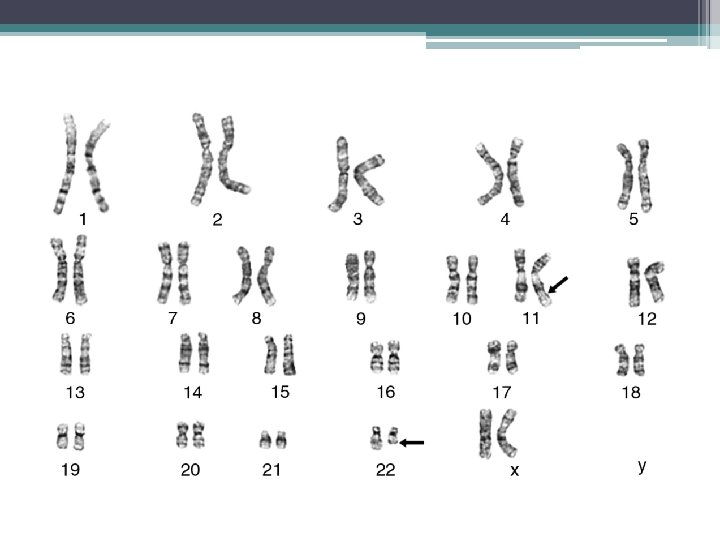
Chromosomal abnormalities

Endocrine factors • Usually DM or thyroid disease • Well-controlled DM and treated thyroid dysfunction are not risk factors for recurrent miscarriage
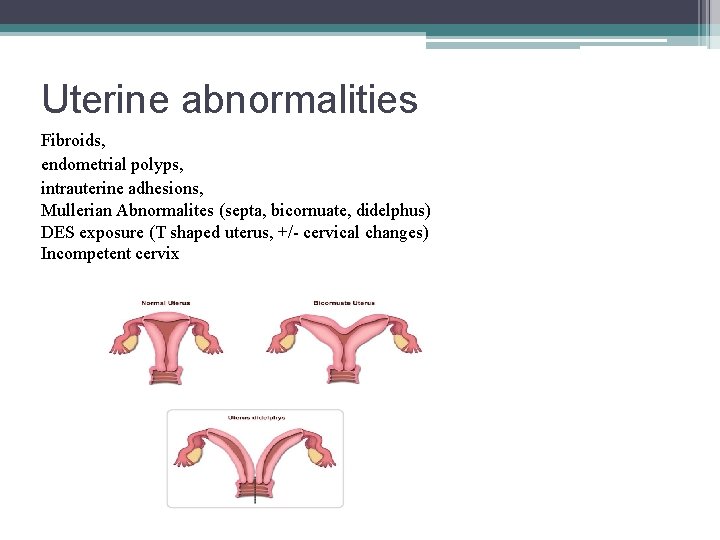
Uterine abnormalities Fibroids, endometrial polyps, intrauterine adhesions, Mullerian Abnormalites (septa, bicornuate, didelphus) DES exposure (T shaped uterus, +/- cervical changes) Incompetent cervix
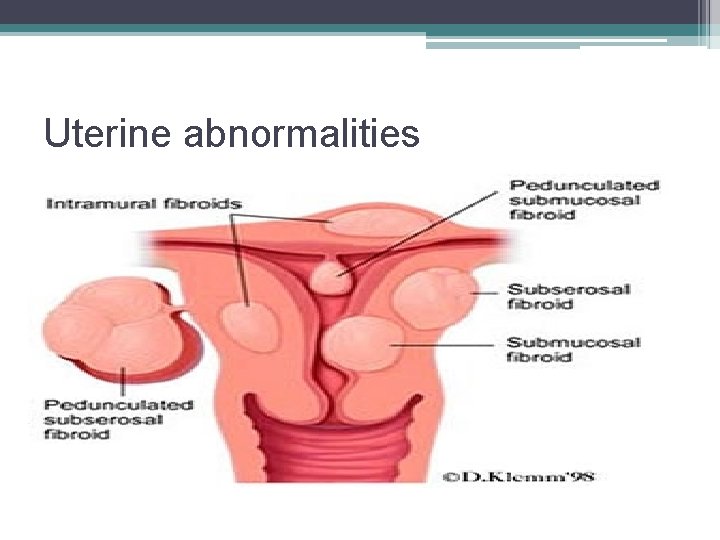
Uterine abnormalities

Cervical incompetence • Diagnosis is clinical, usually based on history ▫ Miscarriage � 2 nd-trimester miscarriage �Subsequent miscarriages are usually earlier �Preceded by spontaneous rupture of membranes �Bulging membranes through the cervix prior to onset of labour �Painless and progressive cervical dilatation �Fetus alive during miscarriage ▫ History of cervical surgery (cone biopsy, LLETZ) • No satisfactory objective test
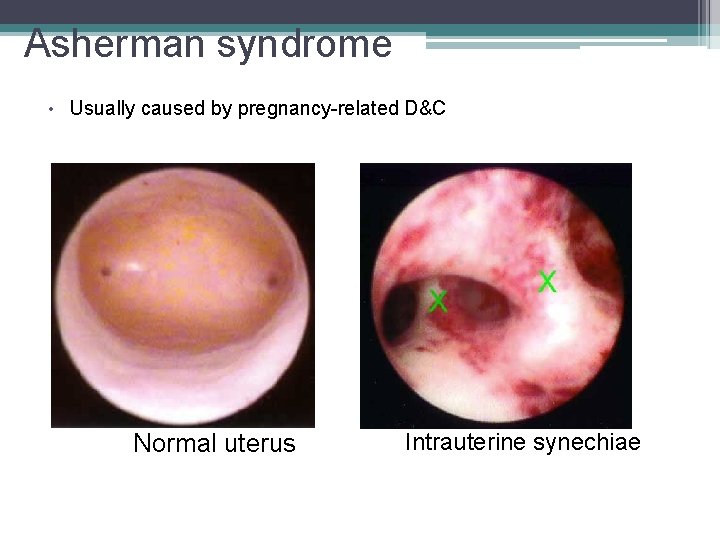
Asherman syndrome • Usually caused by pregnancy-related D&C Normal uterus Intrauterine synechiae

Bacterial vaginosis • Presence of BV in the first trimester ▫ Reported as a risk factor for 2 nd-trimester miscarriage or preterm delivery. • A RCT reported that treatment of BV early in the 2 ndtrimester with oral clindamycin significantly reduces the incidence of second-trimester miscarriage and preterm birth in the general population. • No data to assess the role of antibiotic therapy in women with a previous second-trimester miscarriage.

Thrombophillic Causes Factor V Leiden mutation (activated protein C resistance) most extensively studied. more common with 2 nd trimester abortion -definite risk factor for venous clotting in pregnancy, uncertain if treatment with heparin decreases risk of abortion -certainly require heparin for risk of VT during pregnancy

Management • Emotional aspect ▫ Lost of pregnancy – can be a devastating traumatic experience ▫ Can lead to anxiety, stress & depression ▫ May even lead to family problem divorce • Sensitivity is required in assessing and counselling couples ▫ Approach with sympathy and understanding ▫ DO NOT blame, make her feel at fault

Management • History and Physical Exam Focusing on: a) obstetrical hx- gestational ages, D&Cs, b) galactorrhea, thyroid symptoms c) autoimmune illnesses d) exposures to solvents, drugs, smoking e) family hx of RPL, genetic diseases, autoimmune diseases f) general physical exam with thyroid exam, breast exam g) complete pelvic exam with cultures
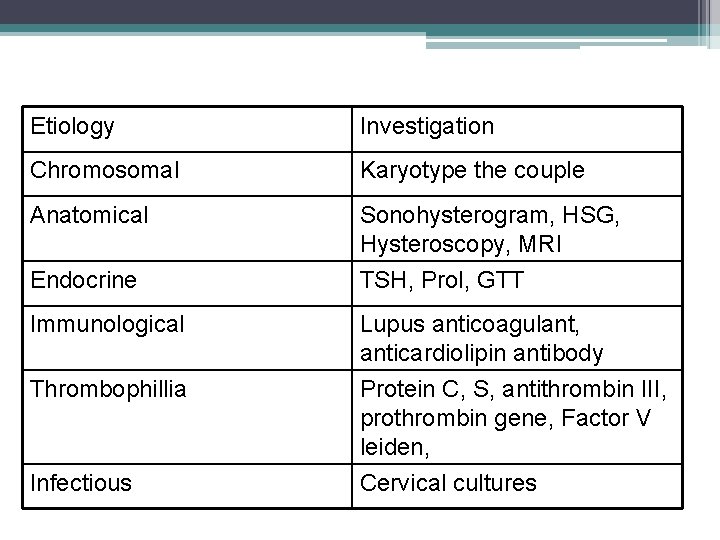
Etiology Investigation Chromosomal Karyotype the couple Anatomical Sonohysterogram, HSG, Hysteroscopy, MRI Endocrine TSH, Prol, GTT Immunological Lupus anticoagulant, anticardiolipin antibody Thrombophillia Protein C, S, antithrombin III, prothrombin gene, Factor V leiden, Cervical cultures Infectious
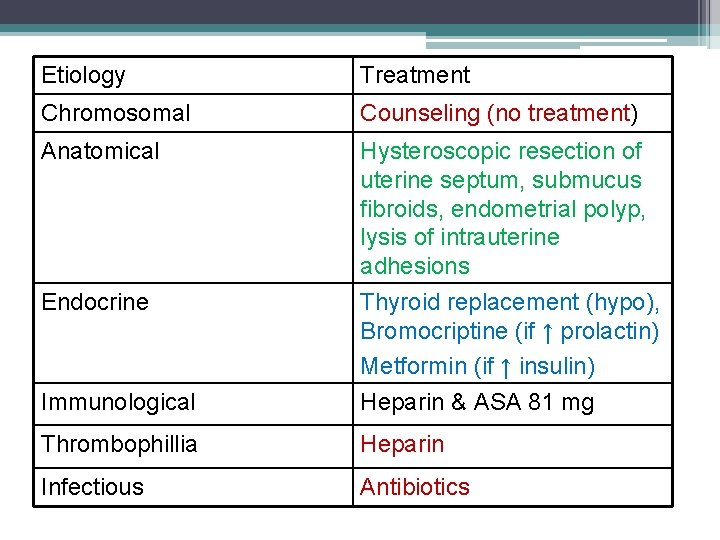
Etiology Treatment Chromosomal Counseling (no treatment) Anatomical Immunological Hysteroscopic resection of uterine septum, submucus fibroids, endometrial polyp, lysis of intrauterine adhesions Thyroid replacement (hypo), Bromocriptine (if ↑ prolactin) Metformin (if ↑ insulin) Heparin & ASA 81 mg Thrombophillia Heparin Infectious Antibiotics Endocrine

- Slides: 23