Rectum lecture 2 Partial Rectal prolapseMucosal The mucous


















- Slides: 24

Rectum lecture 2

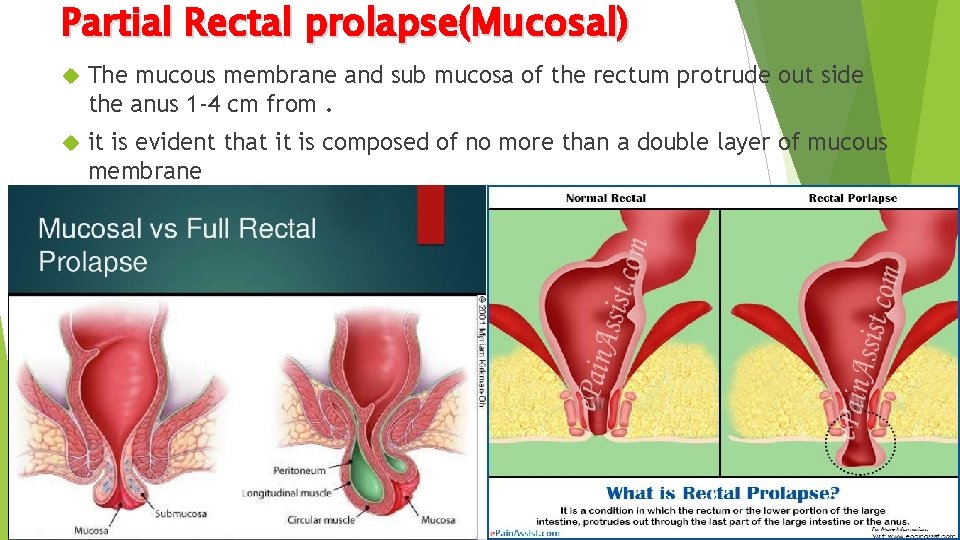
Partial Rectal prolapse(Mucosal) The mucous membrane and sub mucosa of the rectum protrude out side the anus 1 -4 cm from. it is evident that it is composed of no more than a double layer of mucous membrane

Aetiology: In infant The absence of normal sacral curve predispose to rectal prolapse in infant. In children : Start after of attack of diarrhea. Loss of fat in the ischo rectal fossa due to loss of weight. It may be associated with cystic fibrosis. Neurological cause and mal development of pelvis. In adult Start as third degree hemorrhoid (mucohaemorrhoidal prolapse) In a female due to torn perineum. In male, straining during micturition. May fellow operation of fistula in ano ( damage large portion of muscle).

Treatment : Infant and young children : Digital re position Submucosal injection 5% phenol in almond oil. or banding by rubber band(If digital repositioning fails after a 6 -week trial) Adult : Local treatments: Submucosal injections of phenol in almond oil the application of rubber bands are sometimes successful in cases of mucosal prolapse. Excision of prolapsed mucosa : When the prolapse is unilateral, the redundant mucosa can be excised or if circumferential, an (endoluminal stapling) technique.

Complete Rectal prolapse Complete Contain rectal prolapse (procendentia) is Less common. all layer of rectal wall. More common in the women, It is more than 4 cm and commonly as much as 10– 15 cm in length Examination between thumb and finger feels consist more than double layer. And thicker than mucosal prolapse Some time part of peritoneal pouch contain small bowel with gurgle can be felt.

Any prolapse over 5 cm in length will contain anteriorly, between its layers, a pouch of peritoneum. When large, the peritoneal pouch may contain small intestine or bladder. The anal sphincter is characteristically patulous and gapes widely on straining to allow the rectum to prolapse. Complete prolapse is uncommon in children but may occur as a result of malnutrition. In adults, it can occur at any age, but it is more common in the elderly. Women are affected six times more often than men. In approximately 50% of adults, fecal incontinence is also a feature. Complications of rectal prolapse include rectal ulceration and bleeding, incontinence and even incarceration with strangulation of the rectum

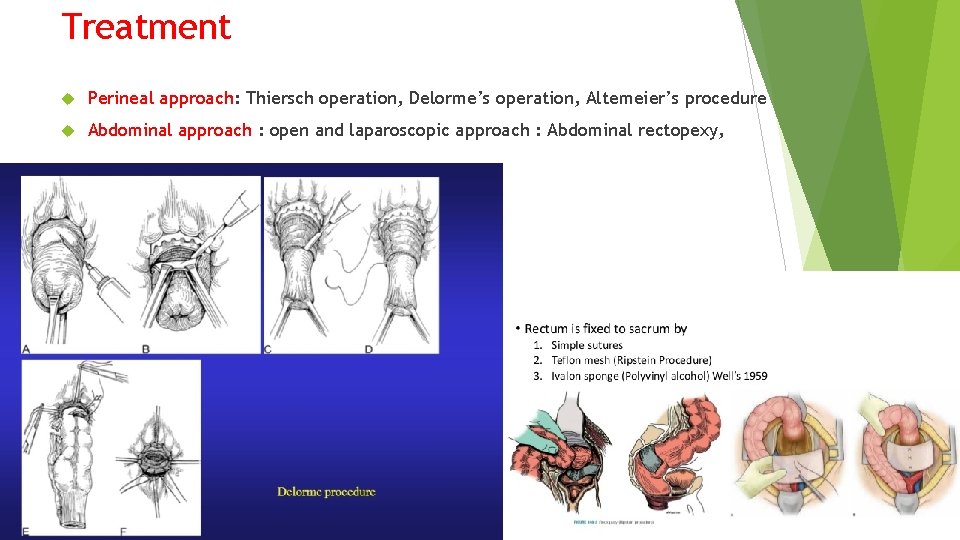
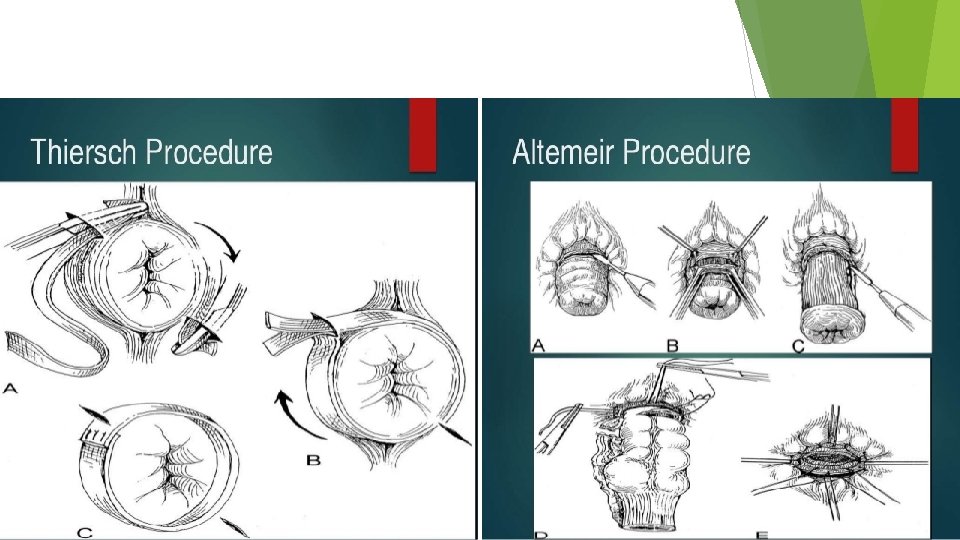
Treatment Perineal approach: Thiersch operation, Delorme’s operation, Altemeier’s procedure Abdominal approach : open and laparoscopic approach : Abdominal rectopexy,


Proctitis The patient is usually middle-aged and complains of defaecatory frequency with the passage of loose motions, often with blood mixed in the stools. Inflammation is sometimes limited to the rectum; in other cases, it is associated with a similar condition in the colon (proctocolitis). The inflammation can be acute or chronic. Although the patient has a frequent, intense desire to defaecate, the amount of faeces passed at any time is small. Acute proctitis is usually accompanied by malaise and pyrexia. Sigmoidoscopic examination : shows inflamed mucous membrane without ulcer of the rectum extend 12. 5 up to 15 cm from the anus. the mucosa above normal.

Treatment in non specific 5 -ASA Prednisolone retention enema. Oral steroid in resistant cases Milk excluded from the diet.

Ulcerative proctocolitis : This may be part of ulcerative colitis. Proctitis due to crohn disease : The rectum can effected by the disease. Sigmoidoscopy revealed patchy ulceration rather confluent , there may be fissuring rather ulceration; cobble stone appearance. Rectal cronhs disease associated with severe perineal fistulation. Skip lesion also present. Radiation proctitis Radiation therapy is used in the treatment of cervical, prostate and rectal cancers. It can produce acute radiation proctitis with bleeding, pain, diarrhoea and defaecatory frequency. Most symptoms settle within a few weeks, but some patients develop chronic proctitis with symptoms appearing months or even decades after the radiation exposure.

Proctitis due to specific infections Ø Clostridium difficile : pseudomembranous colitis , follow broad spectrum antibiotic. Bacillary dysentery : acute purulent proctocolitis. dx swab from mucous membrane. proctoscopy painful Amoebic dysentery: infection is chronic , proctoscopy is not painful Amoebic granuloma : Present as mass in the recto sigmoid. The lesion is mistaken for a carcinoma.

Tuberculous Proctitis : this is always associated with active pulmonary tuberculosis , ulceration of the anus. Sub mucous rectal abscess raptured leave an ulcer with undermined edge. Hypertrophic ulcer in the rectum is associated with Tuberculous peritonitis , Tuberculous Salpingitis. . Dx by endoscopic biopsy. Gonococcal proctitis : is sexual transmitted disease. in female direct spread from the vulva. In acute stage the mucosa id hyperemic with thick pus. The diagnosis is established by bacteriological examination. Treatment is specific for gonococcal infection. Lymphogranuloma inguinale : Is sexual transmitted disease , but in female the mode of spread of infection from the cervix via lymphatic to the para rectal lymph nodes. Dx is suspected when there is inguinal lymph node enlargement. Proctoscopy the same for gonococcal infection Treatment : oxytetracyclin , streptomycin, co-trimoxazole.

Proctitis : due to Primary syphilis: AIDS Rectal bilharziasis : by Schistosoma mansoni common In Egypt. Proctitis due to herbal enema : common in Africa (pepper , bark, ginger ) Severe proctitis. proctoscopy complete gelatinous cast of the mucous membrane of the rectum Treatment : streptomycin , morphine. Temporary colostomy me be needed.

Rectal evacuation disorder (RED) Symptoms consist of a difficulty in emptying despite persistent straining and a feeling of incompleteness in the process. Rectal intussusception is often a component of RED whereby the rectal wall in folds on itself to produce an internal prolapse during straining. Solitary rectal ulcer syndrome may also be another associated manifestation of RED. Classically, SRUS takes the form of an ulcer on the anterior wall of the rectum, situated around 8 cm from the anal verge. In this form, it can be mistaken for rectal carcinoma or inflammatory bowel disease, It may heal, leaving a polypoid appearance Histology will confirm the diagnosis

The condition is difficult to treat. Symptomatic relief from bleeding and discharge may sometimes be achieved by controlling any associated straining with recoordination of defecation using biofeedback therapy. Trans anal stapled resection of the intussusception (STARR procedure) or resuspension of the rectum by abdominal rectopexy may be beneficial. In rare cases, rectal excision may be required

Benign tumor of the rectum Rectal Polyp In the rectum and sigmoid is the most common site ( adenomatous polyp). Polyps are described in terms of their appearance (pedunculated, sessile, flat) or histological composition (tubular, villous, tubulovillous). Adenomatous type has the tendency to be malignant sp. Size >1 cm , follow up increasing size , sessile rather than pedunculated If more than one polyp , total colonoscopy examination , to exclude malignancy. (no rectal tumor removed until resection of the proximal part otherwise implantation tumor cell in the rectal wound). Most of then treated by endoscopic excision , rarely rectal excision.

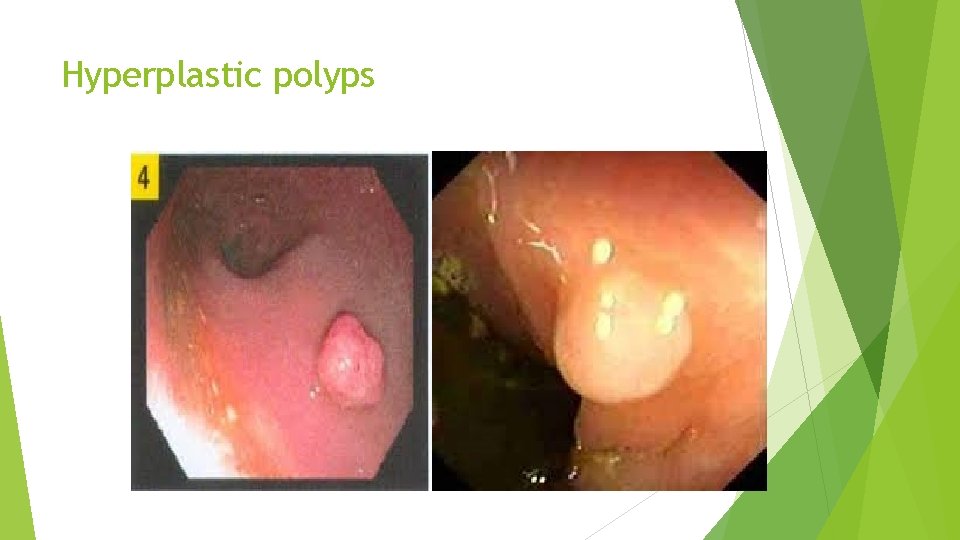
Hyperplastic polyps These are small, pinkish, sessile polyps, 2– 4 mm in diameter and frequently multiple. They are common and generally harmless Tubular adenomas q are the most common type of polyp. q They have the potential to turn malignant, particularly if over 1 cm in diameter. Serrated adenomas They are typically sessile lesions that have a distinct microscopic architecture and can give rise to cancers through an alternative ‘serrated’ pathway

Hyperplastic polyps

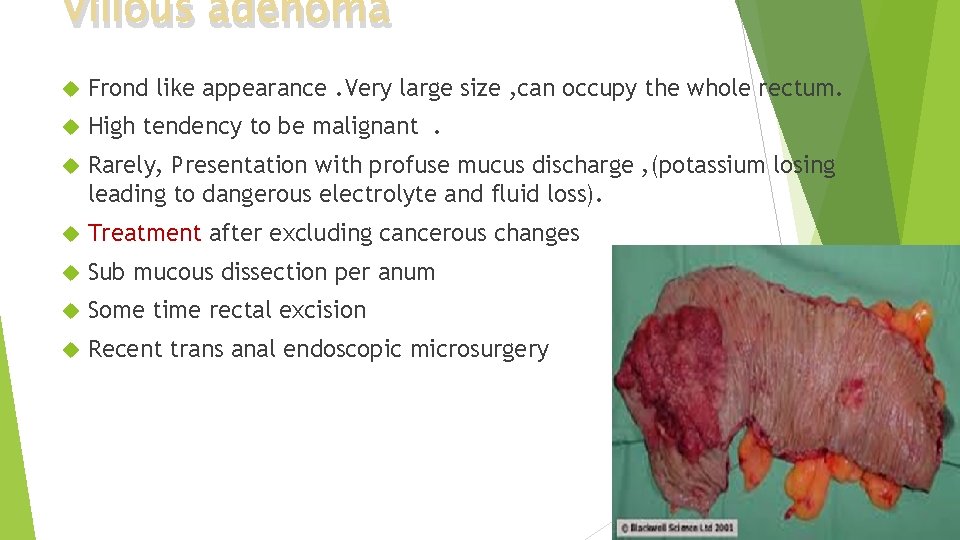
Villous adenoma Frond like appearance. Very large size , can occupy the whole rectum. High tendency to be malignant. Rarely, Presentation with profuse mucus discharge , (potassium losing leading to dangerous electrolyte and fluid loss). Treatment after excluding cancerous changes Sub mucous dissection per anum Some time rectal excision Recent trans anal endoscopic microsurgery

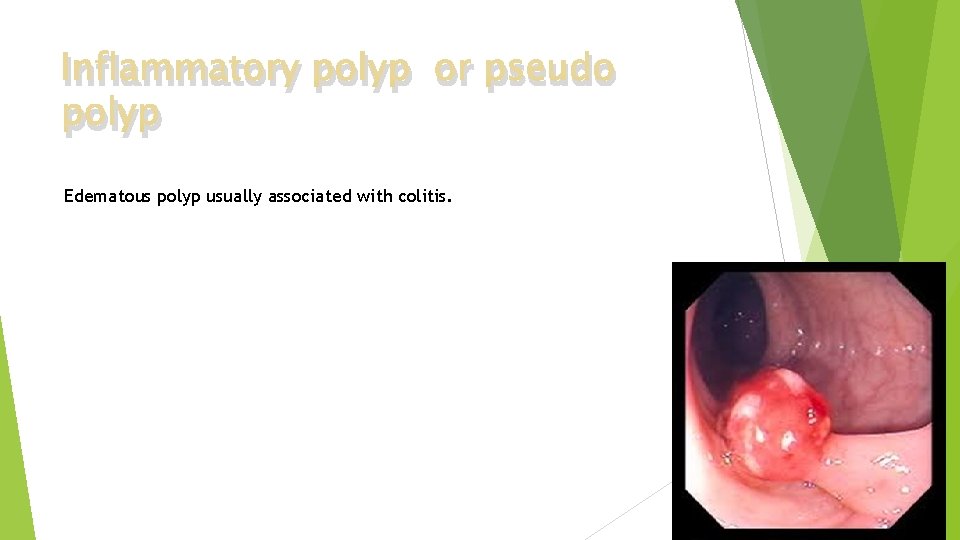
Inflammatory polyp or pseudo polyp Edematous polyp usually associated with colitis.

Juvenile polyp Bright red pedunculated (cherry tumor). Common in infant and children. Can cause bleeding , pain or prolapse Histology : large mucous filled spaces covered by smooth surfaces of thin rectal wall of cuboidal epithelium

Treatment of rectal polyps All polyps should be biopsied or removed for histological analysis to exclude cancer. A range of techniques can be used to remove rectal polyps, dependent on their size and location. The majority of polyps less than 1 cm in size are benign and are amenable to endoscopic polypectomy Polyps greater than 1 cm in size have a 10% chance of harboring a malignancy. Most polyps of 2 cm in size or less can be safely removed by endoscopic mucosal resection (EMR) Larger polyps are more difficult to remove by EMR and may require a transanal procedure, such as transanal endoscopic microsurgery (TEMS).

. Endometrioma : The focus of the ectopic endometrial tissue produces either a constricting lesion of the recto sigmoid or a tumour invading the rectum from the rectovaginal septum The neoplasm is mistaken is carcinoma is tumor invading the recto sigmoid or direct invasion from the rectovaginal septum. Sigmoidoscopy present with stricture with intact mucous membrane. Hormonal manipulation is the first-line therapy, but sometimes total abdominal hysterectomy and bilateral salpingo-oophorectomy and even bowel resection are required Haemangioma : Rare tumor In the lower part of the rectum. May cause fatal hemorrhage Selective angiography and embolization may be helpful, but excision of the rectum is sometimes required. Gastro intestinal stromal tumor : Smooth-muscle tumours of the rectum are rare. If the mitotic rate is high, and if there is variation in nuclear number, size