Recommended Practices to Maximize Reimbursement ColoRectal Bundle Sunil

Recommended Practices to Maximize Reimbursement: Colo-Rectal Bundle Sunil (Sunny) Eappen, MD, Chief Medical Officer and Chief of Anesthesia Massachusetts Eye & Ear Fleurette (Flo) Kiokemeister, RN, MSN Project Manager for the Perioperative Surgical Home/ERAS/ RRP Advocate Lutheran General
Agenda Case Study Client logo placeholder Getting Started Information Governanc e/ Steering Committee Clinical Redesign

Advocate Lutheran General Hospital 638 – bed hospital Level 1 Trauma Center Tertiary care referral hospital 1, 303 physician representing 51 specialties and subspecialties 25 operating rooms / over 19, 000 surgeries per year Part of Advocate Health Care, Illinois’ largest health care system and one of the nation’s top 10 health care systems 3
What is the Main Goal? Client logo placeholder The main goal is to enhance value while achieving the Triple Aim: a better patient experience, better health outcomes and lower costs

Specific Goals and Objectives Client logo placeholder Provide a portal of entry to perioperative care Ensure continuity of coordinated care throughout the surgical experience Reduce • • Cost of care LOS Complication rates Readmissions Promote optimal patient safety Standardization using evidence based practices and research Improve the patient and caregiver experience and satisfaction Provide quality and improvement measures demonstrating success and outcomes
Perioperative Surgical Home: Who, Where, When, How Multidepartmental Initiative Continuity of Care Throughout Surgical Experience Surgic al Home Transform Surgical Care Developing a Standardized Set of Evidenced Based Protocols 6

Getting Started

First Step: The Most Important One Assemble anesthesia champions Select 1 surgical service line • High Cost / High Complexity / High Volume Procedure with ERAs protocol • Enthusiastic surgeons Obtain senior leadership support • Allocate money and support personnel Obtain benchmark data on performance 8
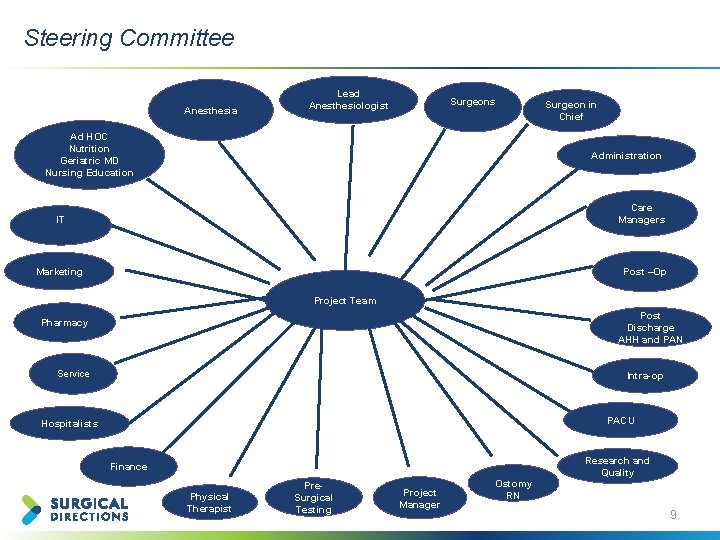
Steering Committee Anesthesia Lead Anesthesiologist Surgeons Ad HOC Nutrition Geriatric MD Nursing Education Surgeon in Chief Administration Care Managers IT Marketing Post –Op Project Team Post Discharge AHH and PAN Pharmacy Service Intra-op PACU Hospitalists Finance Physical Therapist Pre. Surgical Testing Project Manager Ostomy RN Research and Quality 9
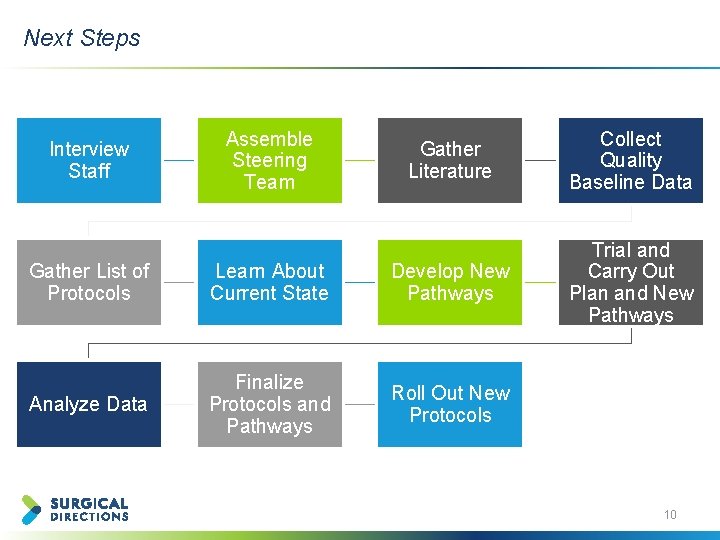
Next Steps Interview Staff Assemble Steering Team Gather Literature Collect Quality Baseline Data Trial and Carry Out Plan and New Pathways Gather List of Protocols Learn About Current State Develop New Pathways Analyze Data Finalize Protocols and Pathways Roll Out New Protocols 10

Information Retrieval is Challenging Information Needed: How Best To Obtain: EHR Nomenclature to Schedule Financial – Cost Per Case Hospital Financial System ICD 10 L. O. S. NSQIP Database Quality SSI DVT Crimson NSQIP HCAHP Press-Ganey/NRC 11
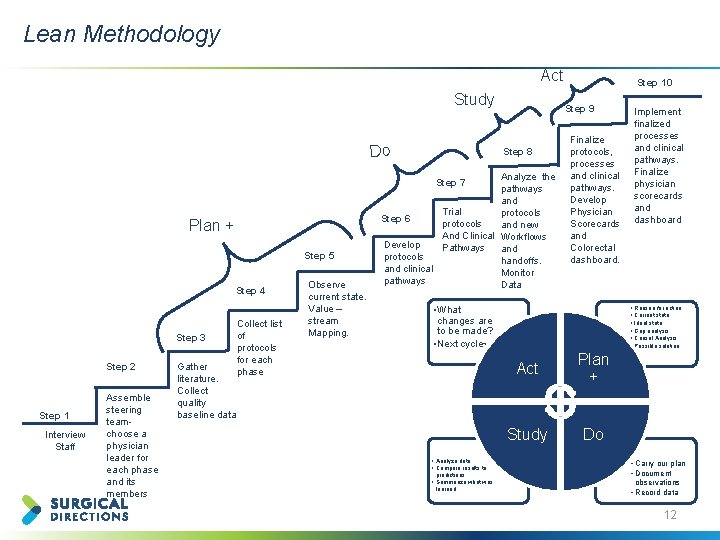
Lean Methodology Act Study Do Step 9 Step 8 Analyze the pathways and Trial protocols Step 6 protocols and new And Clinical Workflows Develop Pathways and protocols handoffs. and clinical Monitor pathways Data Step 7 Plan + Step 5 Step 4 Step 3 Step 2 Step 1 Interview Staff Assemble steering teamchoose a physician leader for each phase and its members Gather literature. Collect quality baseline data Collect list of protocols for each phase Observe current state. Value – stream Mapping. Step 10 Finalize protocols, processes and clinical pathways. Develop Physician Scorecards and Colorectal dashboard. • What changes are to be made? • Next cycle? • Analyze data • Compare results to predictions • Summarize what was learned Implement finalized processes and clinical pathways. Finalize physician scorecards and dashboard • • • Act Plan + Study Do Reason for action Current state Ideal state Gap analysis Causal Analysis Possible solution • Carry our plan • Document observations • Record data 12

How Did We Educate Ourselves? ASA Learning Collaborative Attend Conferences Literature Reviews Networking ERAS Project Management Group 13
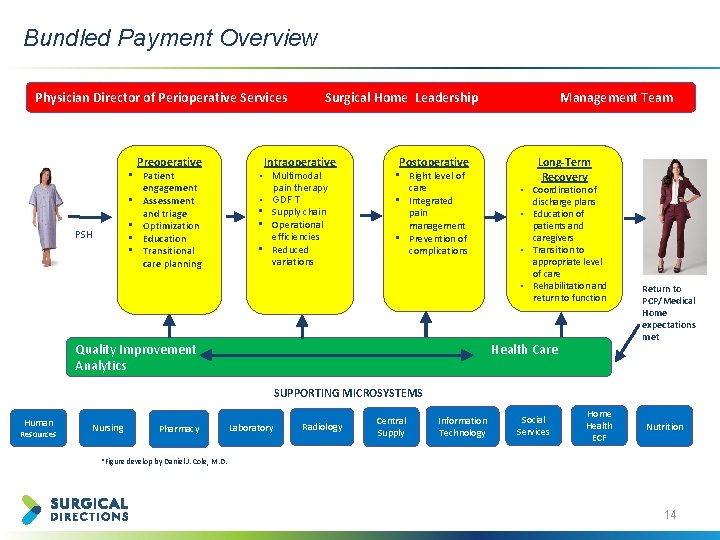
Bundled Payment Overview Physician Director of Perioperative Services Preoperative • Patient engagement • Assessment and triage • Optimization • Education • Transitional care planning PSH Surgical Home Leadership Intraoperative • Multimodal pain therapy • GDFT • Supply chain • Operational efficiencies • Reduced variations Management Team Postoperative • Right level of care • Integrated pain management • Prevention of complications Long-Term Recovery • • Quality Improvement Analytics Coordination of discharge plans Education of patients and caregivers Transition to appropriate level of care Rehabilitation and return to function Health Care Return to PCP/Medical Home expectations met SUPPORTING MICROSYSTEMS Human Resources Nursing Pharmacy Laboratory Radiology Central Supply Information Technology Social Services Home Health ECF Nutrition *Figure develop by Daniel J. Cole, M. D. 14

Perioperative Phase: Surgeons’ Office, PST and the Perioperative Optimization Clinic for Risk Reduction
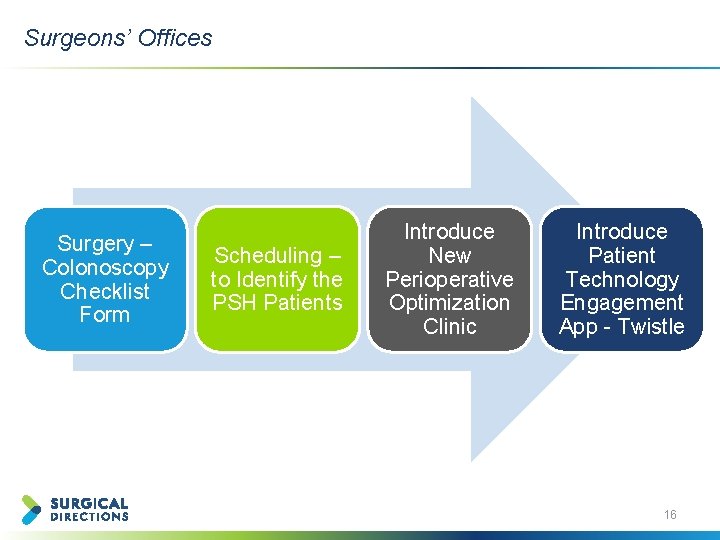
Surgeons’ Offices Surgery – Colonoscopy Checklist Form Scheduling – to Identify the PSH Patients Introduce New Perioperative Optimization Clinic Introduce Patient Technology Engagement App - Twistle 16

SAMPLE: Surgery – Colonoscopy Checklist Form 17

Perioperative Optimization Clinic (POC) Multidisciplinary Clinic: “One Stop Shopping” Concept • Hospitalist • Anesthesiologist • Nurses Additional Clinicians – AD HOC • Discharge Consultant • Nutritionist • Skilled Nursing Home Rep or Home Health • Ostomy Nurse 18

Opportunities of the POC Develop Preoperative Risk Assessment for all surgical patients • Preoptimize patient 2 -3 weeks before surgery Serve as home base for patient and point of contact before and after surgery Allow for proactive planning for post-discharge and transitional care • Active follow-up with high-risk patients Patients will be well prepared for discharge before admission Patients will be educated on postop expectations and their healing process 19
POC Requires Support From… Administration Building Blocks Anesthesiologists Primary Care MDs/Hospitalists Surgeons (some) Staff Goal is Standardization 20

Anchors of Best Practice in Preoperative Preparation • Benchmark cost/patient preparation <$50/patient • RN’s is the POC manages patient preparation, education, and clearance processes • Charts completed at least 3 -5 days prior to day of surgery • Surgeon’s office supplies timely H&P, Orders, Consents and faxes to POC • Anesthesia assists in the POC with patient preparation/clearance –Developing Preparation Algorithms –Staffing POC most common only with physician-extender/hospitalist (relationship) • Seamless, efficient paperwork or use of IT system 21

What Elements Are Needed to Create A Successful POC Center? • Accurate surgical scheduling • Immediate triage-as soon as patient scheduled for surgery Tool Box • Pre-registration (telephone screen completed within 2448 hrs. of scheduling for surgery) • Pre-op Order sets for surgeon and or anesthesia- future orders completed for surgery • History tool (more complete triage) • Lab/EKG on-site • Matrix for labs required for surgery 22

What Elements Are Needed to Create A Successful POC Center? • MD/DO Review of all abnormal tests (Hospitalist/Anesthesiologist) Tool Box • Medications to hold with updated list (250 plus) prior to surgery • Communication with Primary and Surgeon’s Office (after visit within 72 hours) • Hospitalists/charge capture • Tracking form for all patients- who were identified as high risk • Evening before phone call /scripted instructionsautomated reminders from APP • Incomplete chart summary performed 2 -3 days before surgery 23
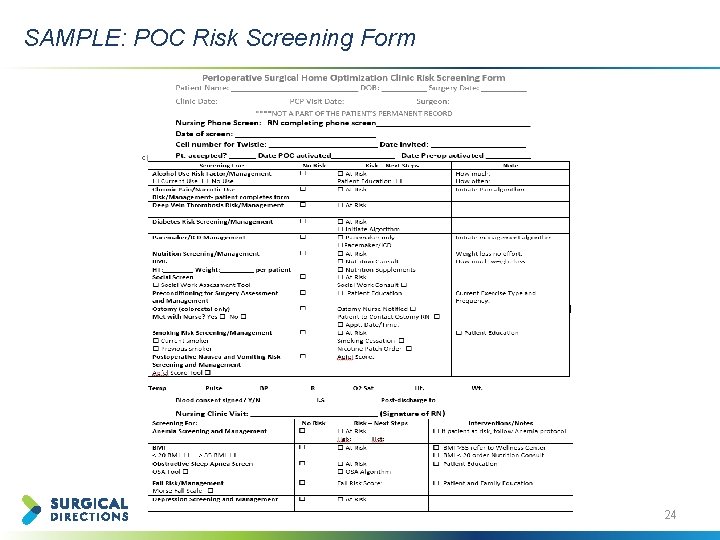
SAMPLE: POC Risk Screening Form 24
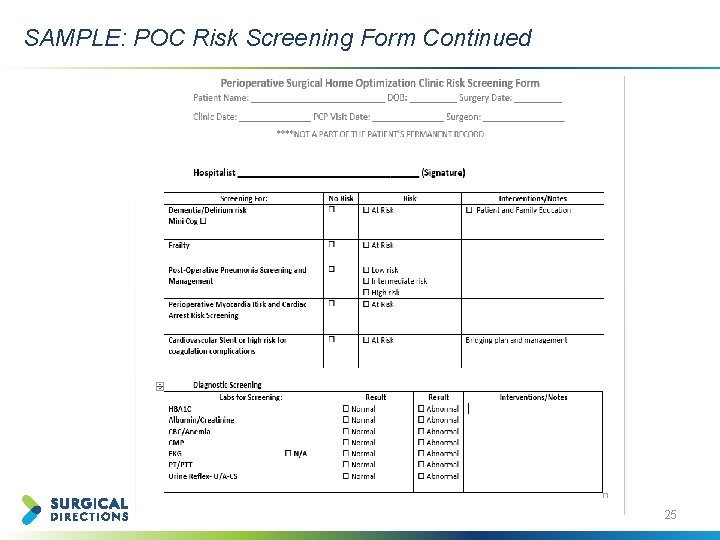
SAMPLE: POC Risk Screening Form Continued 25
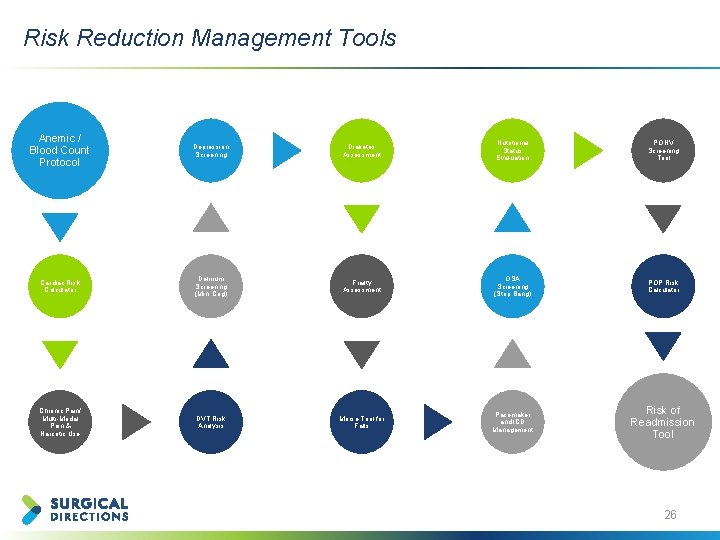
Risk Reduction Management Tools Anemic / Blood Count Protocol Depression Screening Diabetes Assessment Nutritional Status Evaluation PONV Screening Tool Cardiac Risk Calculator Delirium Screening (Mini Cog) Frailty Assessment OSA Screening (Stop Bang) POP Risk Calculator Chronic Pain/ Multi-Modal Pain & Narcotic Use DVT Risk Analysis Morse Tool for Falls Pacemaker and ICD Management Risk of Readmission Tool 26
Additional Screening Tools in Clinic Alcohol Use Smoking Cessation Social Screen Preconditionin g / Exercise 27

ERAS (What) A multimodal perioperative care pathway designed to achieve early recovery for patients undergoing major surgery by minimizing organ dysfunction and reducing the profound stress response brought on by surgery 28

Components of ERAS for Colorectal Education and prehabilitation of patient Clear fluids and a carbohydrate beverage up to 2 -3 hours prior to surgery Narcotic sparing, multimodal pain therapy Goal directed IV fluid therapy GDFT Active intraoperative warming Routine administration of prophylactic antiemetic Minimally invasive surgical technique No drains or nasogastric tubes Early ambulation and enteral nutrition 29

Intra-Operative Phase POCU, OR, PACU
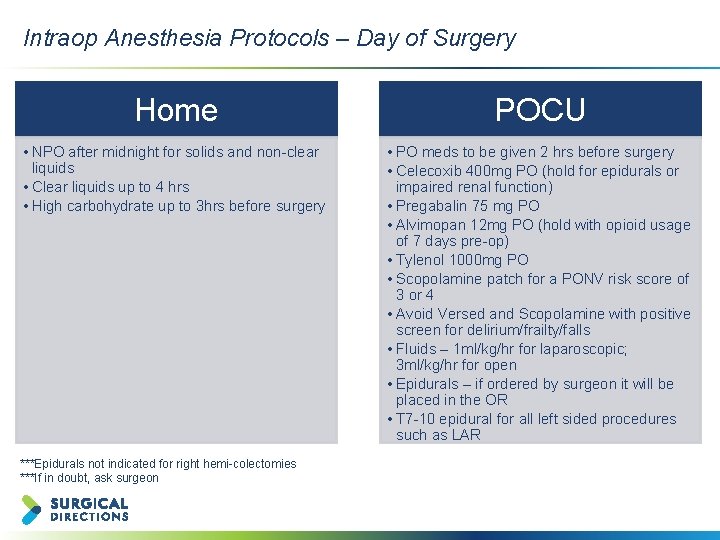
Intraop Anesthesia Protocols – Day of Surgery Client logo placeholder Home POCU • NPO after midnight for solids and non-clear liquids • Clear liquids up to 4 hrs • High carbohydrate up to 3 hrs before surgery • PO meds to be given 2 hrs before surgery • Celecoxib 400 mg PO (hold for epidurals or impaired renal function) • Pregabalin 75 mg PO • Alvimopan 12 mg PO (hold with opioid usage of 7 days pre-op) • Tylenol 1000 mg PO • Scopolamine patch for a PONV risk score of 3 or 4 • Avoid Versed and Scopolamine with positive screen for delirium/frailty/falls • Fluids – 1 ml/kg/hr for laparoscopic; 3 ml/kg/hr for open • Epidurals – if ordered by surgeon it will be placed in the OR • T 7 -10 epidural for all left sided procedures such as LAR ***Epidurals not indicated for right hemi-colectomies ***If in doubt, ask surgeon
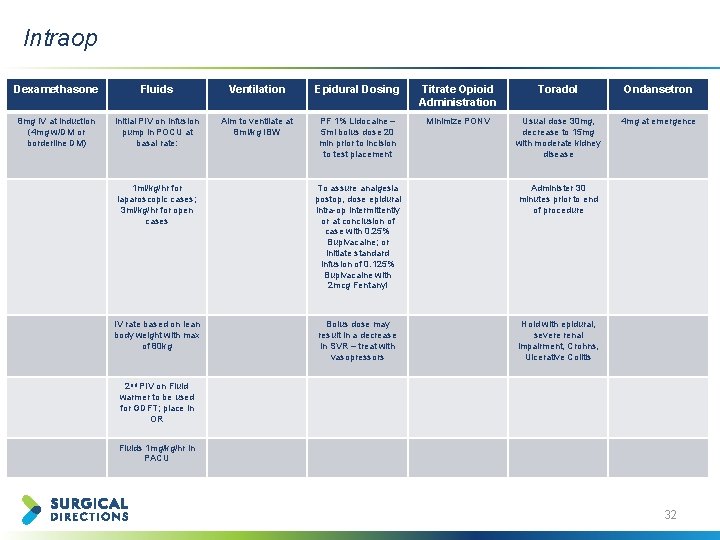
Intraop Dexamethasone Fluids Ventilation Epidural Dosing Titrate Opioid Administration Toradol Ondansetron 8 mg IV at induction (4 mg w/DM or borderline DM) Initial PIV on infusion pump in POCU at basal rate: Aim to ventilate at 8 ml/kg IBW PF 1% Lidocaine – 5 ml bolus dose 20 min prior to incision to test placement Minimize PONV Usual dose 30 mg, decrease to 15 mg with moderate kidney disease 4 mg at emergence 1 ml/kg/hr for laparoscopic cases; 3 ml/kg/hr for open cases To assure analgesia postop, dose epidural intra-op intermittently or at conclusion of case with 0. 25% Bupivacaine; or initiate standard infusion of 0. 125% Bupivacaine with 2 mcg Fentanyl Administer 30 minutes prior to end of procedure IV rate based on lean body weight with max of 80 kg Bolus dose may result in a decrease in SVR – treat with vasopressors Hold with epidural, severe renal impairment, Crohns, Ulcerative Colitis 2 nd PIV on Fluid warmer to be used for GDFT; place in OR Fluids 1 mg/kg/hr in PACU 32
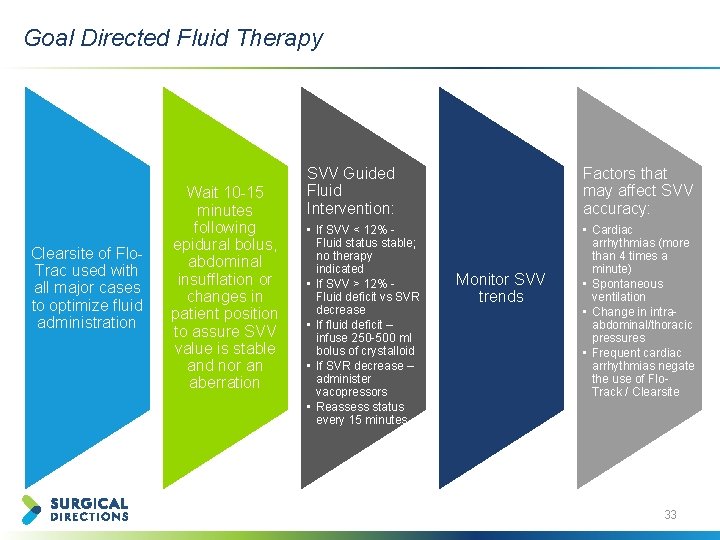
Goal Directed Fluid Therapy Clearsite of Flo. Trac used with all major cases to optimize fluid administration Wait 10 -15 minutes following epidural bolus, abdominal insufflation or changes in patient position to assure SVV value is stable and nor an aberration SVV Guided Fluid Intervention: Factors that may affect SVV accuracy: • If SVV < 12% Fluid status stable; no therapy indicated • If SVV > 12% Fluid deficit vs SVR decrease • If fluid deficit – infuse 250 -500 ml bolus of crystalloid • If SVR decrease – administer vacopressors • Reassess status every 15 minutes • Cardiac arrhythmias (more than 4 times a minute) • Spontaneous ventilation • Change in intraabdominal/thoracic pressures • Frequent cardiac arrhythmias negate the use of Flo. Track / Clearsite Monitor SVV trends 33

Post-Operative Delirium & Miscellaneous Avoid Versed in patient who screen positive for delirium/frailty/fall risk Give muscle relaxant at beginning of case and reverse at the end of case with as little reversal as needed OG tube removed at the end of the case; no NG tubes 34
Additional Intra-Op Identified Colorectal anesthesia and OR nursing team Colorectal SSI Bundle – July 2014 • Sage wipes the night before surgery – full body • Sage wipes the morning of surgery – site specific • Dedicated closing tray and changing gloves and gowns • Maintenance of Normothermia 35

Post-Op Phase
Post-Op Protocols No PICC line delays – Patient screened POD 1 to determine PICC line necessity All ostomy patients will be seen on POD 1; additional floor nursing staff trained to educate patients on ostomy care PT – all colorectal patients will be consulted on POD 1 Activity and early mobilization Early feeding and diet Early removal of Foley catheter Post-op analgesia Daily goals developed for patients 37

Readmission Prevention Tools

Education Video Links and Patient Engagement Provide Education Video Links Build patients’ expectations and prepare them for entire surgical experience Patient Technolog y Engageme nt App Twistle- used to remind patients pre-op and to monitor and surveillance patients up to 30 days post discharge Can be viewed on tablets 39

Twistle – Patient Engagement Platform (Pre and Post-Discharge Reminders) Reminders Cadence • Notifications 3 days and 1 day before clinic visit • Pre-op reminders send 7 days before surgery Reminder Content • Stop taking blood thinners • Arrive to pre-op dept. on 1 st floor • Bowel prep instructional video • SAGE wipes instructional video • NPO reminder • Clearfast or G. E. D. high carbohydrate drink reminder Post-Op Monitoring • Sent daily questions for the first 3 -5 days up to 30 days postdischarge • -HIPPA compliant • -Patients can send pictures • Alerts RN or surgeon if having any fever, hydrating, visit from Home Health RN • Follow-up appointment reminders for PCP and surgeon • Patient outcome questions 40

Post-Discharge Phase Home, Home with HH or ECF
Post-Discharge Developed handoff process • Care management to home health Identified 6 preferred PAN SNF’s Develop Protocols for colorectal patients • Patients with colostomy, lleostomy, open incision, closed incision In-services home health staff and 6 SNF’s on the PSH • Educated on ostomy care & protocols Implementation of Automated Patient Engagement System 42

Protocols…Before and After
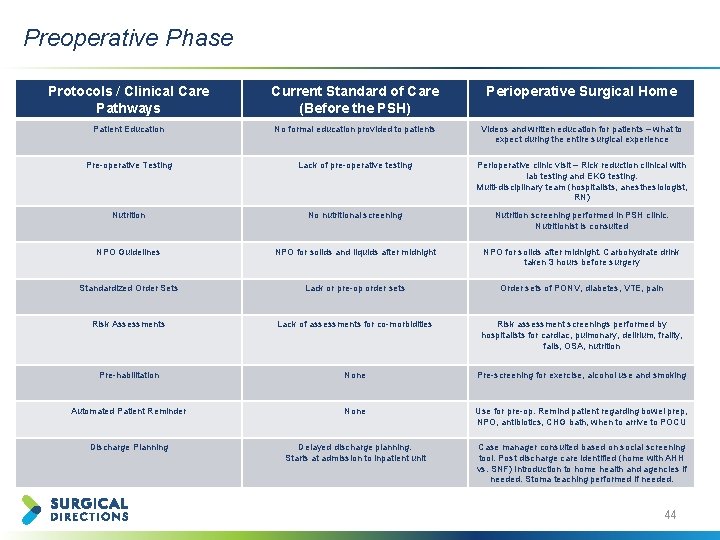
Preoperative Phase Protocols / Clinical Care Pathways Current Standard of Care (Before the PSH) Perioperative Surgical Home Patient Education No formal education provided to patients Videos and written education for patients – what to expect during the entire surgical experience Pre-operative Testing Lack of pre-operative testing Perioperative clinic visit – Rick reduction clinical with lab testing and EKG testing. Multi-disciplinary team (hospitalists, anesthesiologist, RN) Nutrition No nutritional screening Nutrition screening performed in PSH clinic. Nutritionist is consulted NPO Guidelines NPO for solids and liquids after midnight NPO for solids after midnight. Carbohydrate drink taken 3 hours before surgery Standardized Order Sets Lack or pre-op order sets Order sets of PONV, diabetes, VTE, pain Risk Assessments Lack of assessments for co-morbidities Risk assessment screenings performed by hospitalists for cardiac, pulmonary, delirium, frailty, falls, OSA, nutrition Pre-habilitation None Pre-screening for exercise, alcohol use and smoking Automated Patient Reminder None Use for pre-op. Remind patient regarding bowel prep, NPO, antibiotics, CHG bath, when to arrive to POCU Discharge Planning Delayed discharge planning. Starts at admission to inpatient unit Case manager consulted based on social screening tool. Post discharge care identified (home with AHH vs. SNF) Introduction to home health and agencies if needed. Stoma teaching performed if needed. 44
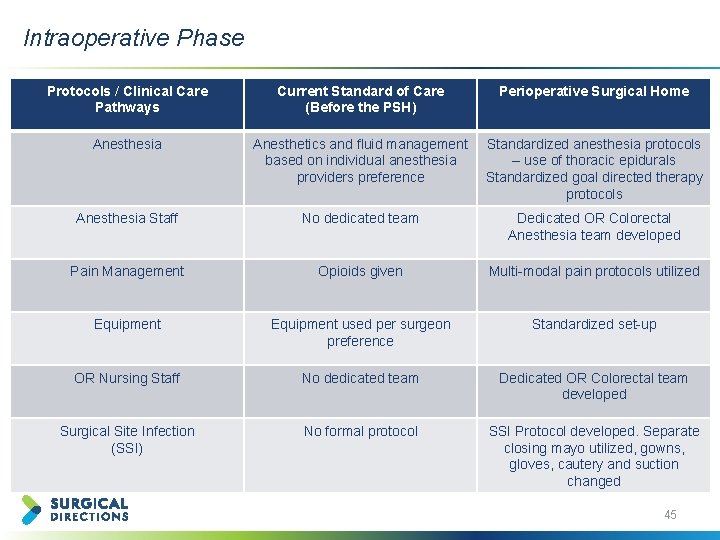
Intraoperative Phase Protocols / Clinical Care Pathways Current Standard of Care (Before the PSH) Perioperative Surgical Home Anesthesia Anesthetics and fluid management based on individual anesthesia providers preference Standardized anesthesia protocols – use of thoracic epidurals Standardized goal directed therapy protocols Anesthesia Staff No dedicated team Dedicated OR Colorectal Anesthesia team developed Pain Management Opioids given Multi-modal pain protocols utilized Equipment used per surgeon preference Standardized set-up OR Nursing Staff No dedicated team Dedicated OR Colorectal team developed Surgical Site Infection (SSI) No formal protocol SSI Protocol developed. Separate closing mayo utilized, gowns, gloves, cautery and suction changed 45
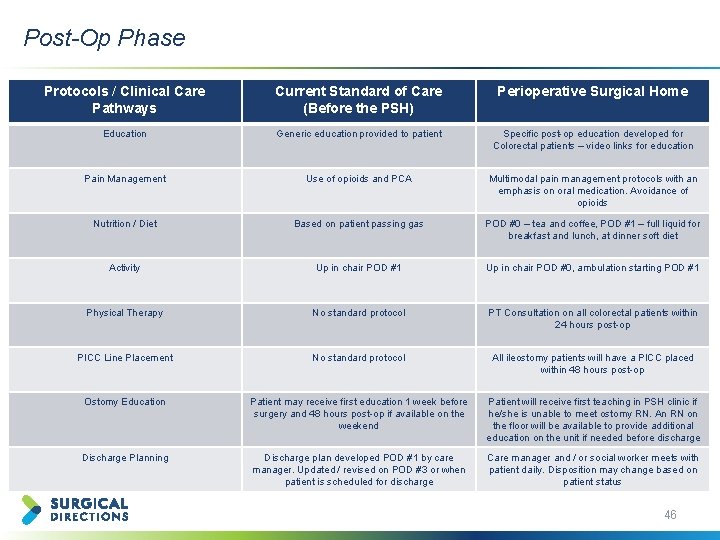
Post-Op Phase Protocols / Clinical Care Pathways Current Standard of Care (Before the PSH) Perioperative Surgical Home Education Generic education provided to patient Specific post-op education developed for Colorectal patients – video links for education Pain Management Use of opioids and PCA Multimodal pain management protocols with an emphasis on oral medication. Avoidance of opioids Nutrition / Diet Based on patient passing gas POD #0 – tea and coffee, POD #1 – full liquid for breakfast and lunch, at dinner soft diet Activity Up in chair POD #1 Up in chair POD #0, ambulation starting POD #1 Physical Therapy No standard protocol PT Consultation on all colorectal patients within 24 hours post-op PICC Line Placement No standard protocol All ileostomy patients will have a PICC placed within 48 hours post-op Ostomy Education Patient may receive first education 1 week before surgery and 48 hours post-op if available on the weekend Patient will receive first teaching in PSH clinic if he/she is unable to meet ostomy RN. An RN on the floor will be available to provide additional education on the unit if needed before discharge Discharge Planning Discharge plan developed POD #1 by care manager. Updated / revised on POD #3 or when patient is scheduled for discharge Care manager and / or social worker meets with patient daily. Disposition may change based on patient status 46
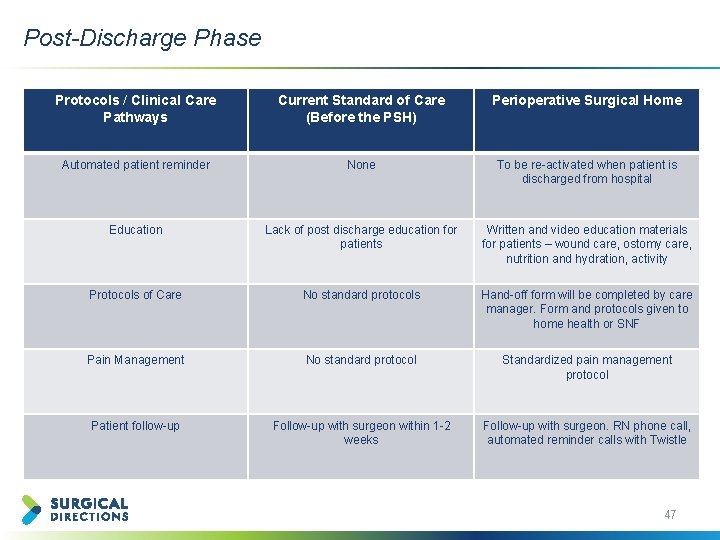
Post-Discharge Phase Protocols / Clinical Care Pathways Current Standard of Care (Before the PSH) Perioperative Surgical Home Automated patient reminder None To be re-activated when patient is discharged from hospital Education Lack of post discharge education for patients Written and video education materials for patients – wound care, ostomy care, nutrition and hydration, activity Protocols of Care No standard protocols Hand-off form will be completed by care manager. Form and protocols given to home health or SNF Pain Management No standard protocol Standardized pain management protocol Patient follow-up Follow-up with surgeon within 1 -2 weeks Follow-up with surgeon. RN phone call, automated reminder calls with Twistle 47
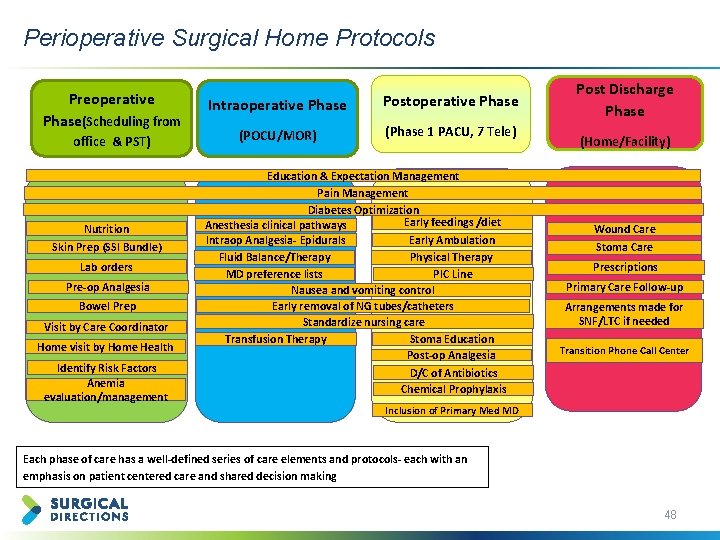
Perioperative Surgical Home Protocols Preoperative Phase(Scheduling from office & PST) Nutrition Skin Prep (SSI Bundle) Lab orders Pre-op Analgesia Bowel Prep Visit by Care Coordinator Home visit by Home Health Identify Risk Factors Anemia evaluation/management Intraoperative Phase Postoperative Phase (POCU/MOR) (Phase 1 PACU, 7 Tele) Education & Expectation Management Pain Management Diabetes Optimization Early feedings /diet Anesthesia clinical pathways Intraop Analgesia- Epidurals Early Ambulation Fluid Balance/Therapy Physical Therapy MD preference lists PIC Line Nausea and vomiting control Early removal of NG tubes/catheters Standardize nursing care Transfusion Therapy Stoma Education Post-op Analgesia D/C of Antibiotics Chemical Prophylaxis Post Discharge Phase (Home/Facility) Wound Care Stoma Care Prescriptions Primary Care Follow-up Arrangements made for SNF/LTC if needed Transition Phone Call Center Inclusion of Primary Med MD Each phase of care has a well-defined series of care elements and protocols- each with an emphasis on patient centered care and shared decision making 48
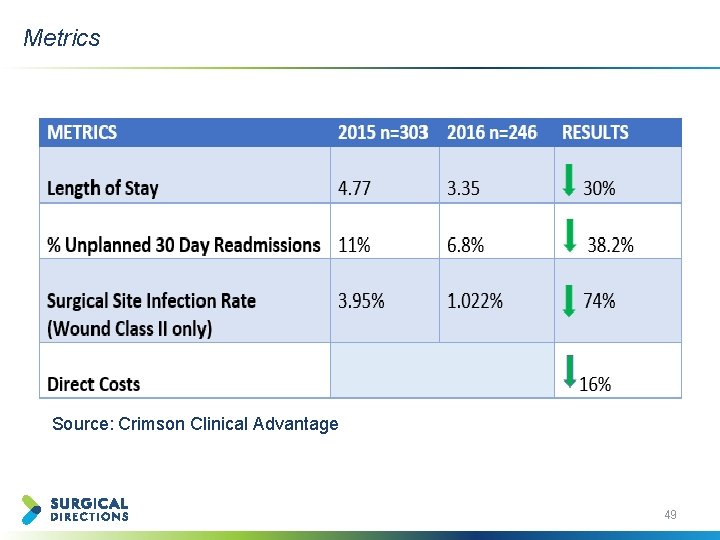
Metrics Source: Crimson Clinical Advantage 49

Patient Satisfaction / Experience Satisfaction has also increased, since implementing the PSH with support from the Patient Engagement Technology support from Twistle. The following are a few of the questions that were asked 30 days after discharge: 50

Lessons Learned and Barriers Client logo placeholder Get everyone’s feedback early on current state to understand where opportunities and barriers exist Difficult to collect baseline data; found in multiple places: Midas, Crimson and Cerner • Procure data analyst to help with data collection and automate it Handoffs missing from discharge to post-discharge Inconsistencies in SNF ostomy care even after in-service by ostomy nurse Difficult to ensure protocols are being followed with patients that transition to a non. PAN SNF or a non-AHH. Care managers ensure the protocols are attached in EMR If patient is discharged early, based on the ERAS protocols, he or she has higher risk of readmission if patient is not managed properly post-discharge Need to monitor patient 30, 60 and 90 days post-discharge to determine if patient is back to normal activity Program is essential for bundled payments ****TIME
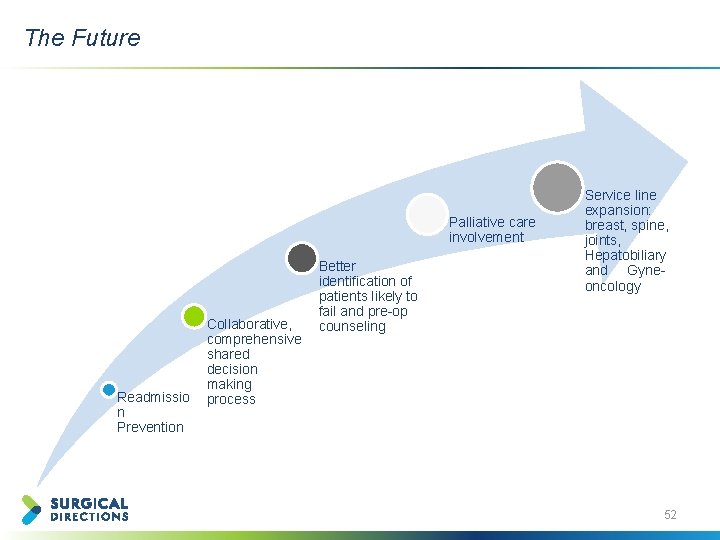
The Future Palliative care involvement Readmissio n Prevention Collaborative, comprehensive shared decision making process Better identification of patients likely to fail and pre-op counseling Service line expansion: breast, spine, joints, Hepatobiliary and Gyneoncology 52

Questions 53

Surgical Directions 541 N. Fairbanks Court Suite 2740 Chicago, IL 60611 T 312. 870. 5600 F 312. 870. 5601 www. Surgical. Directions. com
- Slides: 54