Recognition of Virus Growth in Cell Cultures 1










- Slides: 13


Recognition of Virus Growth in Cell Cultures: 1) Cytopathic effects: Many viruses kill the cells in which they replicate, some times with characteristic appearances or cytopathic effects (CPE). These effects occur in the host as well as in cell cultures and are often useful in the diagnostic laboratory. These include: (a) Cell lysis. (b) Changes in cell morphology: e. g. Cell fusion and Cell rounding. (c) Cell transformation. (d) Plaque Formation. Some viruses may be detected macroscopically by their ability to form plaques in monolayer cells under solid medium. A plaque is a focus of virus infected cells which doesn't take up the vital stain (neutral red) and thus appears as a clear area against a background of stained viable cells. (e) Inclusion bodies.

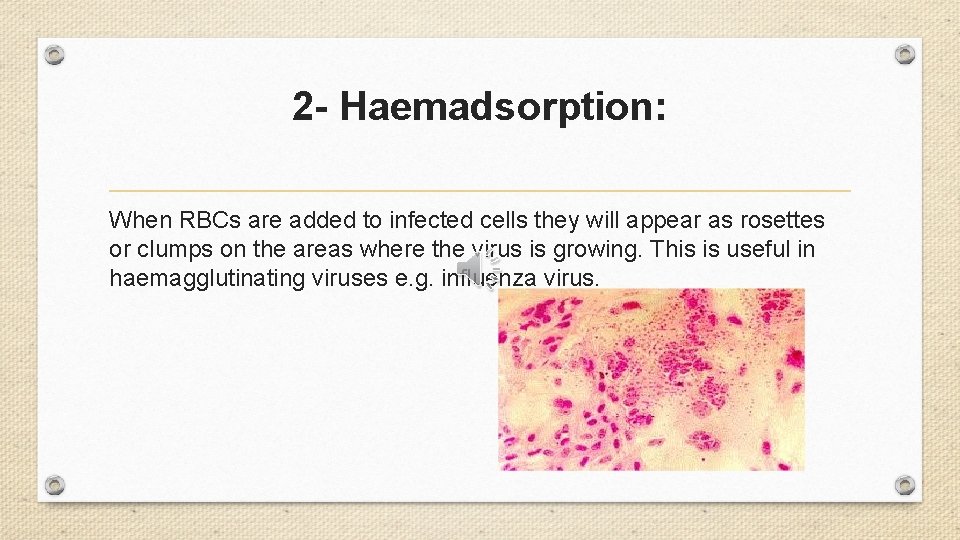
2 - Haemadsorption: When RBCs are added to infected cells they will appear as rosettes or clumps on the areas where the virus is growing. This is useful in haemagglutinating viruses e. g. influenza virus.

3 - Direct immuonoflouresence (IF): Infected cell sheets on cover slips or microtiter plates are treated with fluorescein labeled specific antibody and examined for positive fluorescence.

4 - Detection of viral antigens by serology: • Soluble antigens which diffuse in the nutrient medium or those released after freezing and thawing of tissue culture cells, can be detected by any serologic method including:

Complement fixation: This is an antigen antibody reaction that occurs in the presence of a third component known as the complement. The antigen unites with its specific antibody and the resulting complex fixes the complement. Indicator system formed of sheep RBCs coated with their antibody is used. If there is antigen antibody reaction complement is fixed and no heamolysis of RBCs occurs. If the sample is negative i. e. no antigen antibody reaction occurred, the complement is free and causes heamolysis of RBCs.

Haemagglutination: Some viruses e. g. influenza, mumps, adeno and yellow fever virus can cause agglutination of RBCs (passive heamagglutination test). This test is used for detection and titration of heamagglutinatig viruses in cultures.

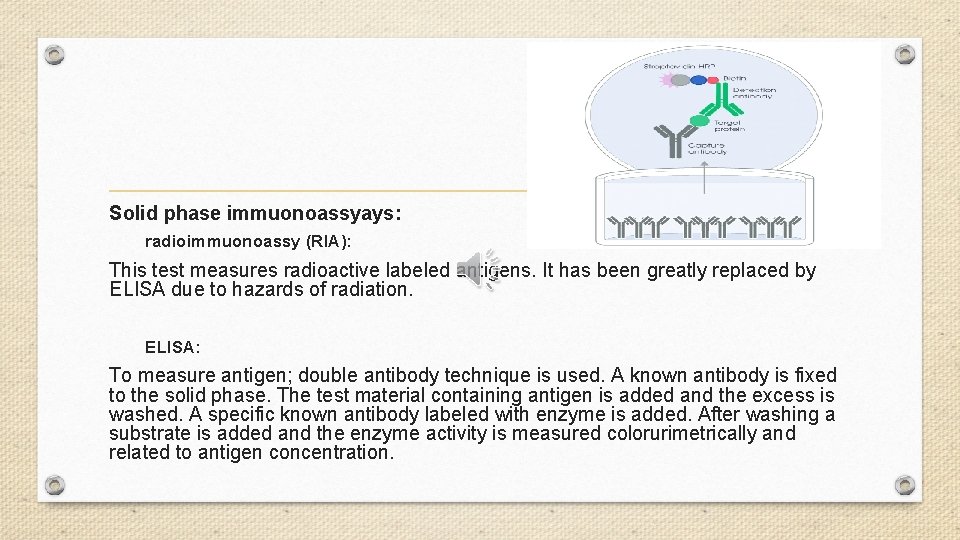
Solid phase immuonoassyays: radioimmuonoassy (RIA): This test measures radioactive labeled antigens. It has been greatly replaced by ELISA due to hazards of radiation. ELISA: To measure antigen; double antibody technique is used. A known antibody is fixed to the solid phase. The test material containing antigen is added and the excess is washed. A specific known antibody labeled with enzyme is added. After washing a substrate is added and the enzyme activity is measured colorurimetrically and related to antigen concentration.

Direct immuonoflouresence (IF): It is an antigen antibody reactions in which we use fluorescein labeled antibodies. Fluorescein is a dye which emits greenish fluorescence under ultraviolet light (UV), and it can be tagged to immunoglobulin molecules. In this test, fluorescein labeled antibody is layered over the antigen fixed on a slide. The site where the antibody adheres to its specific antigen will be seen as apple green fluorescence.

Neutralization tests: Neutralization of the effects of virus on tissue culture by specific antisera can be used to identify the type of isolated virus (see below).

II. Indirect methods by: Serologic detection of antiviral antibodies: Serologic diagnosis of virus infections can be established by detecting a rising antibody titer to the virus or by detection of sero conversion (patient who was previously sero negative turns positive due to primary infection). The first sample should be collected early after disease onset, the second 1 -2 weeks later. If paired sera are not available or rapid diagnosis is needed, as in diagnosis of rubella in early pregnancy; detection of Ig. M antibodies to the virus is resorted to. The detection of Ig. M in a single serum sample indicates recent infection.

Serologic diagnosis is of value to: • Determine the type of infecting virus. • Diagnose viruses difficult to isolate or slow viral infections. • Differentiate acute or chronic infection (by antibody type; Ig. M is the main antibody in acute infection). • Differentiate active or convalescent infection (by detection of rising antibody titer in active infection). • Differentiate primary infection and reinfection: • Criteria for diagnosing Primary Infection: • A significant rise in titre of Ig. G/total antibody between acute and convalescent sera (a four-fold or greater increase in titre). • Presence of Ig. M. • Criteria for diagnosing re-infection/re-activation: • It is often very difficult to differentiate re-infection/re-activation from a primary infection. Under most circumstances, it is not important to differentiate between a primary infection and re-infection. However, it is very important under certain situations, such as rubella infection in the first trimester of pregnancy where primary infection is associated with a high risk of fetal damage whereas re-infection is not.

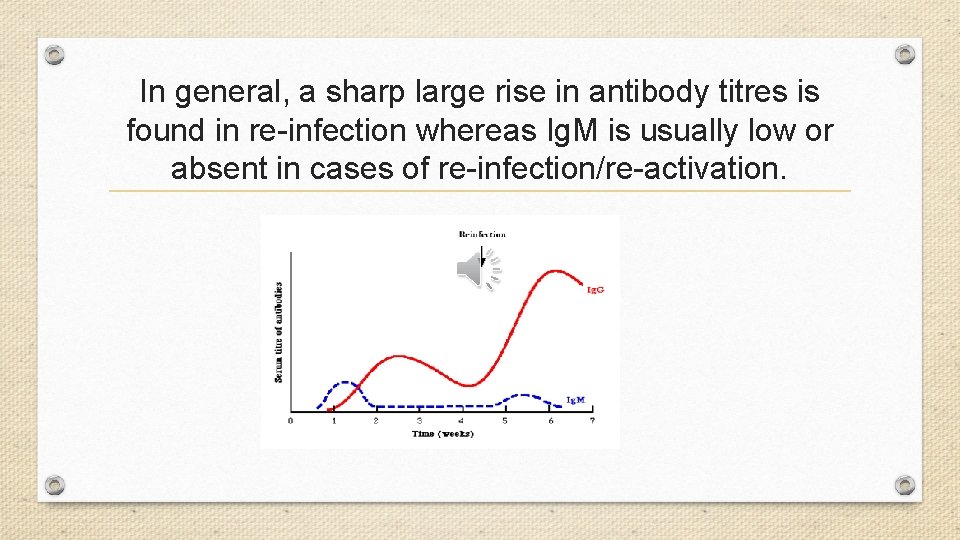
In general, a sharp large rise in antibody titres is found in re-infection whereas Ig. M is usually low or absent in cases of re-infection/re-activation.