Recognition of a Sick Child Aims of Assessment











































- Slides: 50


Recognition of a Sick Child

Aims of Assessment LIFE THREATENING Potentially Life Threatening Not Life Threatening

Clinical Parameters Interact! • Whatever the cause and whichever the organ system involved, the clues to recognition of serious and deteriorating physiology can be found in just 3 clinical parameters • ABNORMAL BEHAVIOR • ABNORMAL RESPIRATION • ABNORMAL CIRCULATION

In every Sick / Potentially Sick Child • ASK • Behavior, Feeding, Urine output • LOOK • Appearance, Breathing, Circulation, others • LISTEN • Speech, Cry, Breathing, MOTHER

In every Sick / Potentially Sick Child • FEEL • Pulses, Warmth, Extremities • SMELL • MEASURE • HR, RR, BP, TEMP, • O 2 Saturation, Blood Sugar

Equipment for Assessment LOOK LISTEN FEEL MEASURE

Question Interact! • What would be three main things you would ask to rapidly assess a sick child?

Step 1 - Ask BEHAVIOR FEEDING URINE OUTPUT

Step 2 – Look…. . Appearance • Behaviour • Look/Gaze - Not playful, Lethargic • Anxious – hypoxic • Interactivity • No / decreased Interactions with parents, surroundings • Consolability • Consolable, not consolable

Step 2 – Look…. . Appearance • Posture and Tone • Limp, stiff, curled up, neck retraction • Feeding well, Not feeding • Pain facies • Is the infant/child in moderate to severe pain?

Look…. . Breathing Interact!

What are other Respiratory LOOK Signs that are Important? • RATE: Fast or Slow • TYPE: Thoraco-abd, Abd or Thoracic • REGULARITY/RHYTHM • RETRACTIONS: Mild, Moderate or Severe

Look…. . Circulation • Diaphoresis: excessive sweating • Mottling of skin • Colour: cyanosis present/absent, peripheral/central

Look…. . Others • Bleeding • Fractures/ deformities • Rashes

Listen • Cry • Respiratory Sounds • Speech • Mother’s concerns

Stridor Interact!

Wheeze Interact!

Grunt Interact!

Recognition of the Seriously Ill Child - Efficacy of Breathing Interact! • A silent chest is a pre-terminal sign

Step 4 - Feel • PULSES: Peripheral and central • SKIN: Warmth, Turgor. Cold and sweaty palms and soles usually indicate poor perfusion • CFT • EXTREMITIES: injuries / fractures / hematomas

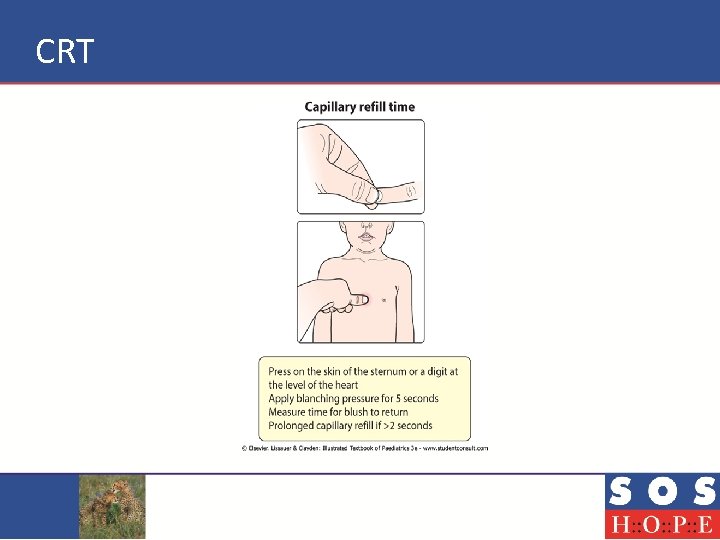
How do you Assess Capillary Refill Time? Interact! • • • Where? How long? Position of limb? Normal? Physiological causes of prolonged CRT?

CRT

Step 5 – Smell, which Conditions would Help? Interact! • DKA • IEM • POISONINGS

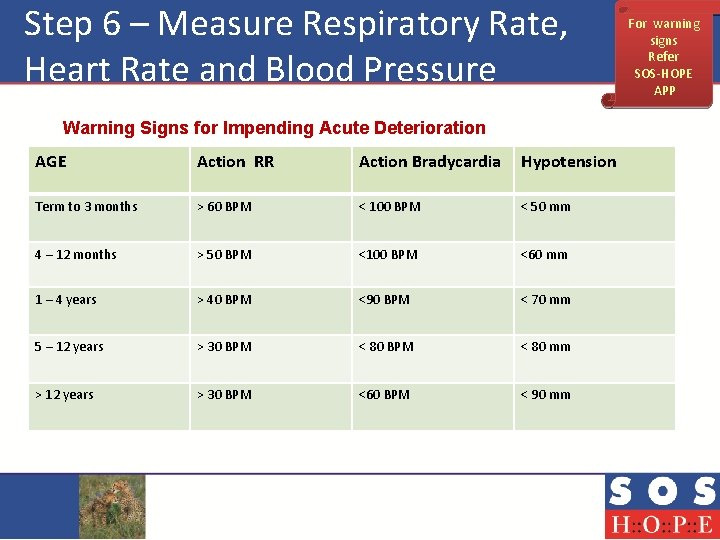
Step 6 – Measure Respiratory Rate, Heart Rate and Blood Pressure Warning Signs for Impending Acute Deterioration AGE Action RR Action Bradycardia Hypotension Term to 3 months > 60 BPM < 100 BPM < 50 mm 4 – 12 months > 50 BPM <100 BPM <60 mm 1 – 4 years > 40 BPM <90 BPM < 70 mm 5 – 12 years > 30 BPM < 80 mm > 12 years > 30 BPM <60 BPM < 90 mm For warning signs Refer SOS-HOPE APP

Measure • Temperature • Pulse Oximetry • Capillary Blood Glucose level

Key Values in Practice • • Pulse > 220/min consider SVT Cap refill > 2 seconds is not normal BP in kids > 1 year = 70 + (2 x age) RR > 60/min NB, > 50/min till 1 yr, > 40 /min till 5 yrs • Pulse oximetry < 92% In room air For key values Refer SOS-HOPE APP

Key Values in Practice For key values Refer SOS-HOPE APP • Blood Glucose • < 45 mg/dl on day 1 of life newborn • < 50 mg/dl after day 1 of life in newborn • Hypoglycemia in children - < 50 mg/dl of whole blood glucose • Hypothermia is diagnosed by identification of a core body temperature that is <35°C (95°F) • Heat stroke is defined as a core temperature ≥ 40°C (104°F) accompanied by central nervous system dysfunction in patients with environmental heat exposure

We Have Done a Rapid Assessment - 6 Steps 1. 2. 3. 4. 5. 6. Ask Look Listen Feel Smell Measure

From the Assessment we need to TRIAGE What is the meaning of TRIAGE

Triage Levels

When Would You Call It Triage Level 1 • BEHAVIOUR • RESPIRATION • CIRCULATION • ASK • LOOK • LISTEN • FEEL • SMELL • MEASURE

What to do? Severe Impairment of 1 or More Parameters • Unresponsive or altered consciousness or lethargic • HR < > NR +/- 2 SD , RR < > NR +/- 2 SD (Grossly abnormal) • Inadequate breathing • Moderate to severe respiratory distress/ marked stridor • Shock: CFT > 4 secs, BP lower than normal for age • Cyanosis • THIS IS AN EMERGENCY: ACT FAST! STABILIZE

When Would You Call It Triage Level 2 • BEHAVIOUR • RESPIRATION • CIRCULATION • ASK • LOOK • LISTEN • FEEL • SMELL • MEASURE

What to do? Mild-Moderate Impairment of 1 or More Parameters • Infant – unconsolable, not feeding, atypical behaviour • HR , RR outside NR for age • Mild-Moderate stridor • Mild distress • Capillary refill > 2 sec but < 4 sec • OBSERVE CLOSELY, TREAT, MAY DETERIORATE FAST!

When Would You Call It Triage Level 3 • BEHAVIOUR • RESPIRATION • CIRCULATION • ASK • LOOK • LISTEN • FEEL • SMELL • MEASURE

What to do? Mild or No Impairment of any Parameter • • • No history of recent behavior/appearance change HR & RR - normal for age/mildly deranged CFT < 2 sec BP in normal range for age THIS IS NON URGENT

Interact! There Always Exceptions in any Rule When would you triage a child more serious than he actually is?

Beware !! • Sick infant, < 3 months of age • Temp > 40 deg C or hypothermia • Suspected ingestion of unknown substance or unknown quantity of known substance • Severe pain

Beware !! • Any illness in a child with severe malnutrition • Burns: major - > 10% BSA &/or involving airway • Purpuric rashes, target lesions • Discordant Physical findings • MOTHER

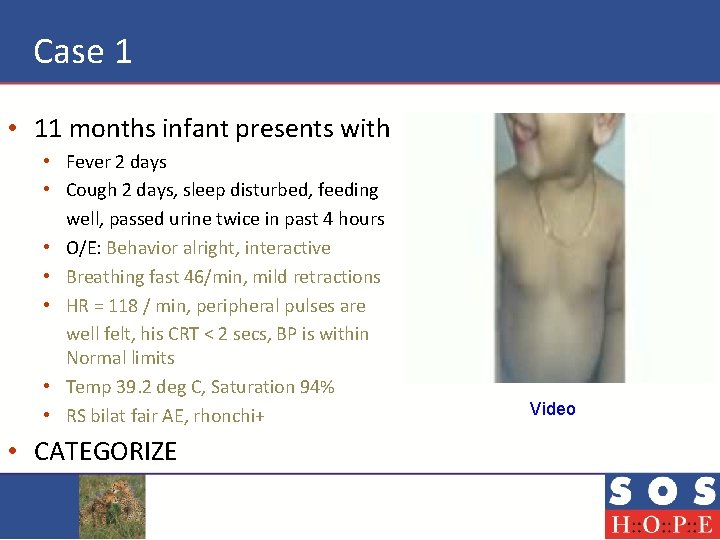
Case 1 • 11 months infant presents with • Fever 2 days • Cough 2 days, sleep disturbed, feeding well, passed urine twice in past 4 hours • O/E: Behavior alright, interactive • Breathing fast 46/min, mild retractions • HR = 118 / min, peripheral pulses are well felt, his CRT < 2 secs, BP is within Normal limits • Temp 39. 2 deg C, Saturation 94% • RS bilat fair AE, rhonchi+ • CATEGORIZE Video

Case 1 – Response • This child has got derangement of a mild nature of his breathing • Other parameters are within normal limits

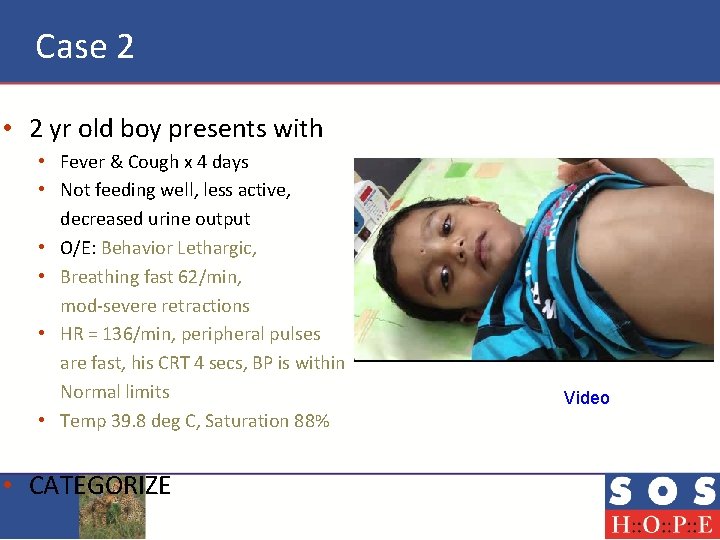
Case 2 • 2 yr old boy presents with • Fever & Cough x 4 days • Not feeding well, less active, decreased urine output • O/E: Behavior Lethargic, • Breathing fast 62/min, mod-severe retractions • HR = 136/min, peripheral pulses are fast, his CRT 4 secs, BP is within Normal limits • Temp 39. 8 deg C, Saturation 88% • CATEGORIZE Video

Case 2 - Response • This child is sicker than case # 1, he is hypoxemia, he also may have compensated shock • His categorization would be Urgent • Action ?

Case 3 • A 3 yr boy brought with • Vomiting & watery loose stools for 3 days, inactive & no urination for past 24 hours • O/E: Behavior – drowsy, reacting only to painful stimuli • Breathing fast 56/min with intermittent sighing breathing • HR = 176/min, peripheral pulses are feeble, his CRT > 5 secs, BP is un-recordable, • Temp 35. 6 deg, Saturation 82% • CATEGORIZE

Case 3 - Response • Measure his blood sugar. Found to be 20 mg/dl • This child is in decompensated shock, with probable acidosis, hypoxia, and hypothermia. He may be also in septic shock • His category would be Red

In Every Sick/Potentially Sick Child • ASK • Behavior, feeding, urine output • LOOK • Appearance, Breathing, Circulation, Others • LISTEN • Speech, Cry, Breathing, MOTHER • FEEL • Pulses, Warmth, Extremities • SMELL • MEASURE • HR, RR, BP, TEMP, O 2 SATN, Blood Sugar

In Every Sick / Potentially Sick Child CATEGORIZE 1. Emergency needing Resuscitation ACT 1. Stabilize & transfer 2. Potentially sick, can deteriorate fast 2. Stabilize & Observe closely 3. Non Urgent 3. Treat and Follow up

So it is very important to triage a sick child rapidly and either initiate stabilization or resuscitation depending on the severity

Basic Principles: III Children • Regardless of the aetiology → information required for assessment and management is the same for all children • Simple clinical tools are sufficient to recognize sick or potentially sick children • kids ‘can deteriorate quickly……so act in time’ Liverpool Primary Care Trust, Western Cheshire