Recognition and prevention of deterioration using the ABCDE

Recognition and prevention of deterioration using the ABCDE approach Version: Jan 2016

Learning outcomes This lecture should enable you to: • discuss the importance of early recognition and the treatment of a deteriorating patient in order to prevent cardiac arrest • state how to assess a patient using the ABCDE approach • identify causes of cardiac arrest and the measures used to prevent them
Chain of Prevention Assists in preventing: • • deterioration cardiac arrests and deaths admissions to ICU inappropriate resuscitation attempts

Standard 9 Recognising and Responding to Clinical Deterioration in Acute Health Care • establish recognition and response systems • IHCA reporting is rare in the literature • recognising clinical deterioration escalate care • range between 1 and 5 events per 1, 000 hospital admissions • responding to clinical deterioration • survival to hospital discharge most common range being between 15% and 20% – (or 0. 175 events/bed annually) • VF/VT is present in only 25– 35% of IHCAs and 60 -70% OHCAs – many develop VF during arrest
Early recognition of the deteriorating patient Common factors seen in cardiac arrests: • most arrests are predictable • deterioration in up to 80% of patients prior to cardiac arrest • tachypnoea early sign - hypotension often later • hypoxaemia and hypotension common pre-arrest in review of arrested patients
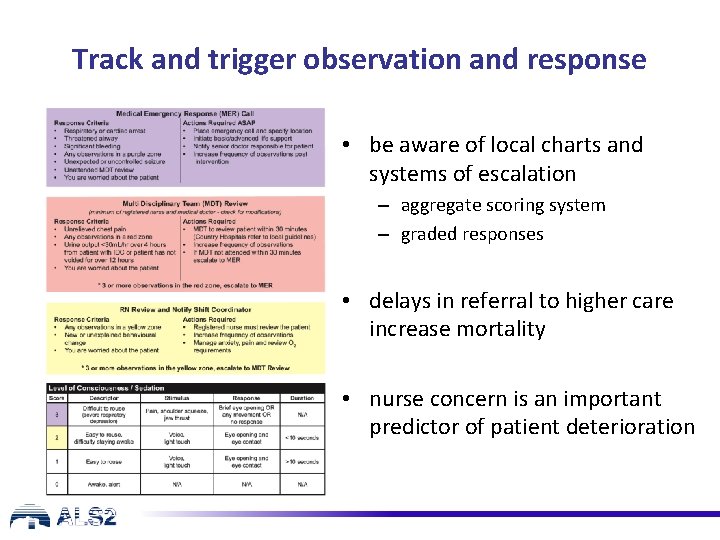
Track and trigger observation and response • be aware of local charts and systems of escalation – aggregate scoring system – graded responses • delays in referral to higher care increase mortality • nurse concern is an important predictor of patient deterioration
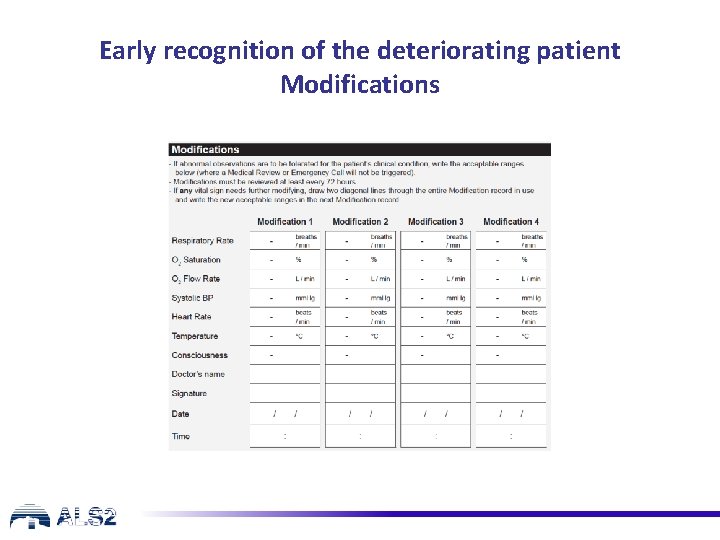

Early recognition of the deteriorating patient Modifications

Causes of deterioration and cardiorespiratory arrest • Airway obstruction • Breathing problems • Circulation problems

The ABCDE approach to the deteriorating patient Airway Breathing Circulation Disability Exposure

ABCDE approach Underlying principles: • • • complete a prompt initial assessment treat life-threatening problems as they are found call for help early use all members of the team assess response to treatment/interventions effective communication – e. g. ISBAR

ABCDE approach • • personal safety first impression – ‘do they look unwell? ’ assess from afar - ‘how are you? ’ core physiological observations included: – respiratory rate, oxygen saturation, heart rate, blood pressure, temperature and level of consciousness – ECG monitor

ABCDE approach Airway Causes of airway obstruction: • CNS depression • foreign body – solid – blood – vomit • direct trauma • • • infection inflammation laryngospasm bronchospasm blocked tracheostomy

ABCDE approach Airway Recognition of airway obstruction: • impaired vocalisation • difficulty breathing, distressed, choking • increased effort of breathing • see-saw respiratory pattern, accessory muscles • partial obstruction - noisy breathing – stridor, wheeze, gurgling • complete obstruction - silence
ABCDE approach Airway Treatment of airway obstruction: • airway opening – head tilt, chin lift, jaw thrust • simple adjuncts – oropharyngeal or nasal airway • advanced techniques – e. g. supraglottic airway device, tracheal tube • high flow oxygen

ABCDE approach Breathing Causes of breathing problems: decreased respiratory: • drive – CNS depression • effort – – muscle weakness/tiring nerve damage restrictive chest defect pain • lung disorders – – – – asthma infection acute exacerbation COPD pulmonary embolus pulmonary oedema pneumothorax haemothorax

ABCDE approach Breathing Recognition of breathing problems: • Look – respiratory rate, rhythm and depth, use of accessory muscles, cyanosis, chest deformity, conscious level • Listen – noisy breathing, breath sounds/silence • Feel – expansion, percussion note, tracheal position, surgical emphysema RATES approach • Respiratory Rate • Auscultate chest (listen) • Trachea • Effort of Breathing • Sp. O 2

ABCDE approach Breathing Treatment of breathing problems: • high flow oxygen – guided by Sp. O 2 (94 - 98% if measured) • support breathing if inadequate – e. g. bag-valve-mask, non-invasive ventilation • treat/consider underlying cause

ABCDE approach Circulation Causes of circulation problems: • hypovolaemia • blood/fluid loss • intravascular loss • cardiogenic • acute coronary syndromes • arrhythmias • valve disease • obstructive • emboli • pneumothorax • tamponade • distributive • septic shock • anaphylaxis • drugs/toxins • other • hypoxaemia • electrolyte/acid base abnormalities • anaemia • hyper/othermia • asphyxia

ABCDE approach Circulation Recognition of circulation problems: • • • shortness of breath syncope poor peripheral perfusion – capillary refill time pulse blood pressure – organ perfusion - chest pain, mental state, oliguria • bleeding, fluid losses
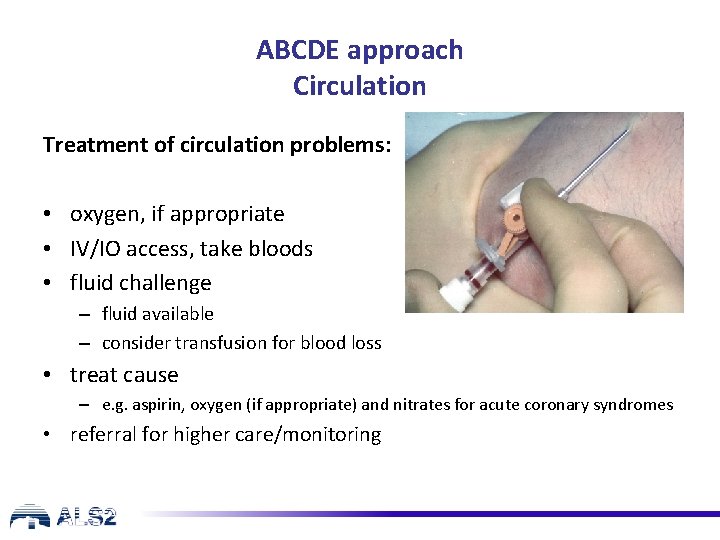
ABCDE approach Circulation Treatment of circulation problems: • oxygen, if appropriate • IV/IO access, take bloods • fluid challenge – fluid available – consider transfusion for blood loss • treat cause – e. g. aspirin, oxygen (if appropriate) and nitrates for acute coronary syndromes • referral for higher care/monitoring

ABCDE approach Disability Causes • hypoxia • drugs – prescribed – recreational • • hyper/hypoglycaemia intracranial haemorrhage cerebral hypo-perfusion hypothermia Recognition • AVPU and pupils initially then GCS later • bedside blood glucose • core temperature • check medication charts and notes

ABCDE approach Disability/Drugs/Diabetes Treatment • ABC treatment • oxygen if appropriate • treat underlying cause • achieve normoglycaemia • consider lateral position

ABCDE approach Exposure • remove clothes to enable examination – surface, orifice, extremity, cavity, drains • e. g. injuries, bleeding, rashes, bites and stings • avoid heat loss – record temperature • maintain dignity

Any questions?

Summary • early recognition of the deteriorating patient may prevent cardiac arrest • most patients have warning symptoms and signs before cardiac arrest • airway, breathing or circulation problems can cause cardiac arrest • use the ABCDE approach to recognise and treat patients at risk of cardiac arrest

Advanced Life Support Level 2 Course Slide set All rights reserved © Australian Resuscitation Council (June 2016)
- Slides: 26